New Year begins with the “hottest time” for case management jobs
Case manager pipeline in long-term trouble
The nation’s healthcare expansion into population health models and moving payment away from fee-for-service toward pay for quality performance and financial stewardship has created an unprecedented need for experienced case managers, and their salaries are climbing, according to case management professionals and the 2015 Case Management Advisor Salary Survey.
“It’s the hottest time for case managers,” says Margaret Leonard, MS, RN-BC, FNP, vice president for medical management at MVP Healthcare in Schenectady, NY.
“We can’t find qualified candidates,” Leonard adds.
“I’ve been in this business since 1986, and the opportunity for case managers is unprecedented,” says Sandra L. Lowery, RN, BSN, CCM, CNLCP, president of CCMI Associates of Humboldt, AZ.
“It’s amazing to see the practice setting expanding in so many areas,” Lowery says. “Every day, I find a new avenue: We have case managers working on cruise ships, and in the Peace Corps.”
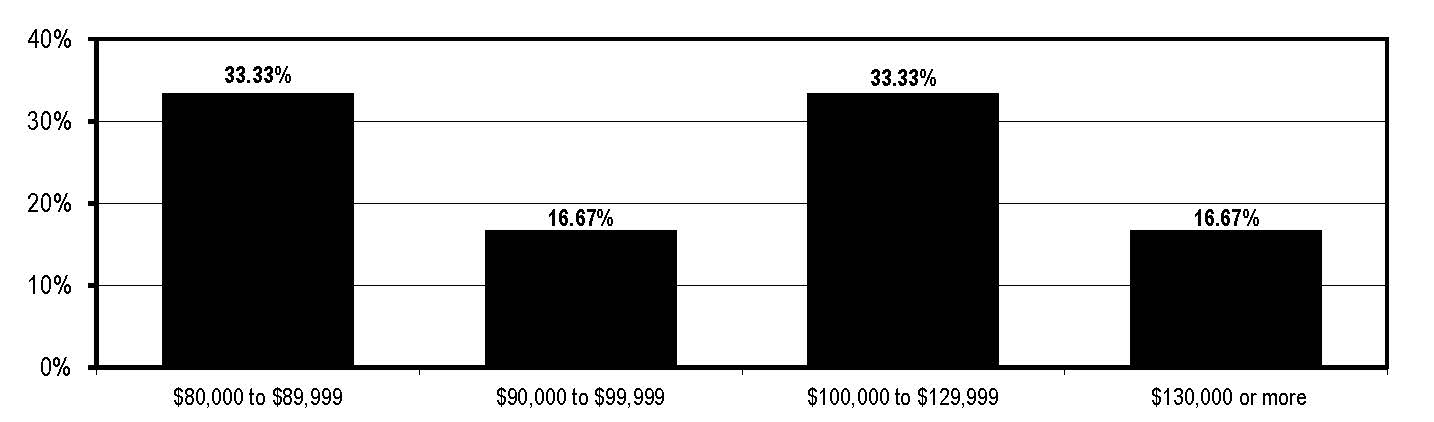
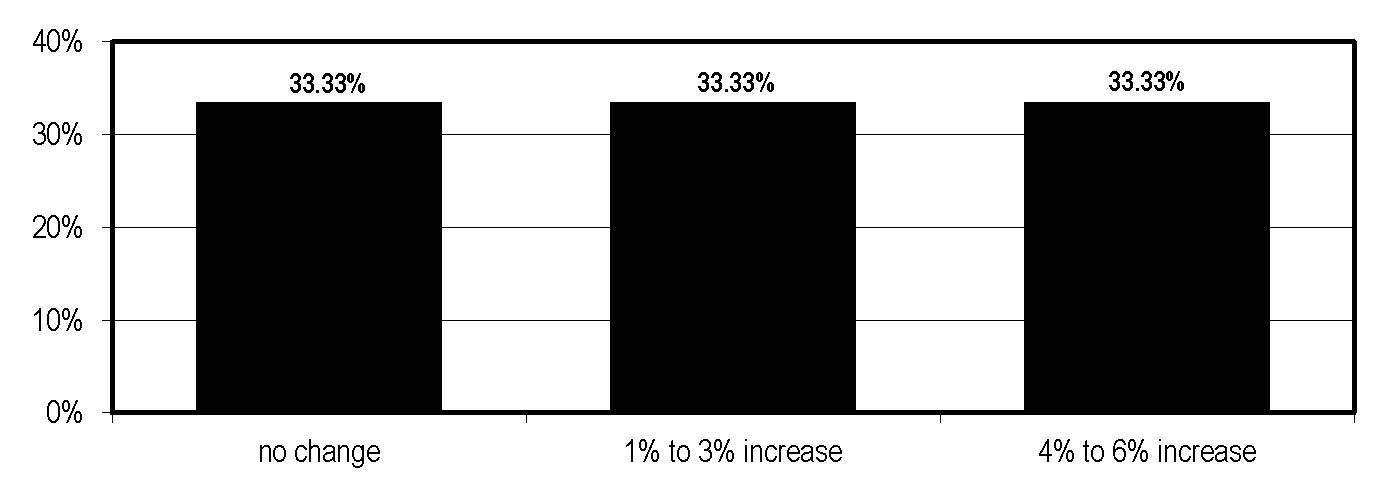
Case managers are well compensated, anecdotal evidence suggests: Respondents to Case Management Advisor’s 2015 Salary Survey report a median salary of $100,000 and annual raises that range between 1% and 6%.
Half of the people responding to the survey also say they have had an increase in the number of employees in the past year.
And they’re working a considerable amount of hours: No respondents had a 40-hour work week, and the range of hours worked rose to 65-plus.
“Across the board, generally speaking, case managers have a higher case load than they can handle most effectively,” Lowery says. “Either they work hard on those cases they can, or they put out fires and are not getting the outcomes they could produce.”
The survey does not ask about case managers’ backgrounds prior to moving into that role, but anecdotal evidence suggests this also is changing.
“We’re seeing a great deal of emphasis being put on pharmacists,” Leonard says. “They’re an important part of the team whether or not they are geared for or have the time to do care coordination.”
The case management job market is much different than it was a decade ago, with CMs moving into a variety of work settings other than hospitals and workers’ compensation offices, says LuRae Ahrendt, RN, CRRN, CCM, CLCP, rehab nurse case manager at Ahrendt Rehabilitation in Lawrenceville, GA.
“One of the things that is so interesting to me about case managers is that it’s unusual to have a practice area where so many different types of education and backgrounds are brought together under one umbrella,” Ahrendt explains. “There could be master’s level psychology majors, MSWs, and others.”
In Ahrendt’s field of rehab case management, there are more nurses and vocational counselors: “I love the fact that people’s individual licenses don’t define them,” she says.
The increase in demand for case managers is driven partly by the need to better coordinate care in an evolving healthcare world in which bad outcomes will cost providers.
“As we look at the evolution of healthcare, there are more and more studies that talk about how not only does healthcare case management change in a positive way the outcomes of individuals, but it also is shown to be cost effective,” Ahrendt says.
In the payer setting, there appears to be an increase in Medicare-Medicaid HMOs, which are hiring case managers to handle dual eligible populations, Lowery says.
“We’re also seeing an increase in special needs programs that need case managers, and the other area I see growth in is in the military,” she adds. “I almost always have someone in my program from the military who is encouraged to get certified.”
Population health disease management programs are growing under the Affordable Care Act (ACA), and they’re specifically targeting high-risk populations, Lowery says.
“A lot of case managers who have experience with analytics know what high risk is and how to identify it,” she explains. “What I do is nurse life care planning for case managers.”
This is a relatively recent professional career path for case managers, she notes.
“Attorneys have discovered that case managers have the necessary experience to develop life care plans for catastrophically injured populations,” Lowery says. “You develop life care plans for third-party lawsuits.”
For example, a person whose spinal cord or brain was injured in an auto accident will need some type of health and other assistance for life, she explains.
The person is suing a third party for damages, but it’s necessary to know what type of care they’ll need to sustain them for life, and case managers are the professionals who best can predict their care continuum needs, Lowery says.
While the need for case management professionals is growing, the pipeline is falling short.
“There are not enough people in the pipeline for case management,” Lowery says. “Where I don’t see shortages now, I definitely think we’re not growing enough.”
This is one of the reasons why more paraprofessionals are being hired to do case management work: Paraprofessionals, including occupational therapy assistants, medical technicians, and LPNs, are being hired for care management work — not because they don’t want a more qualified person, but the market doesn’t provide enough availability of staff, Lowery says.
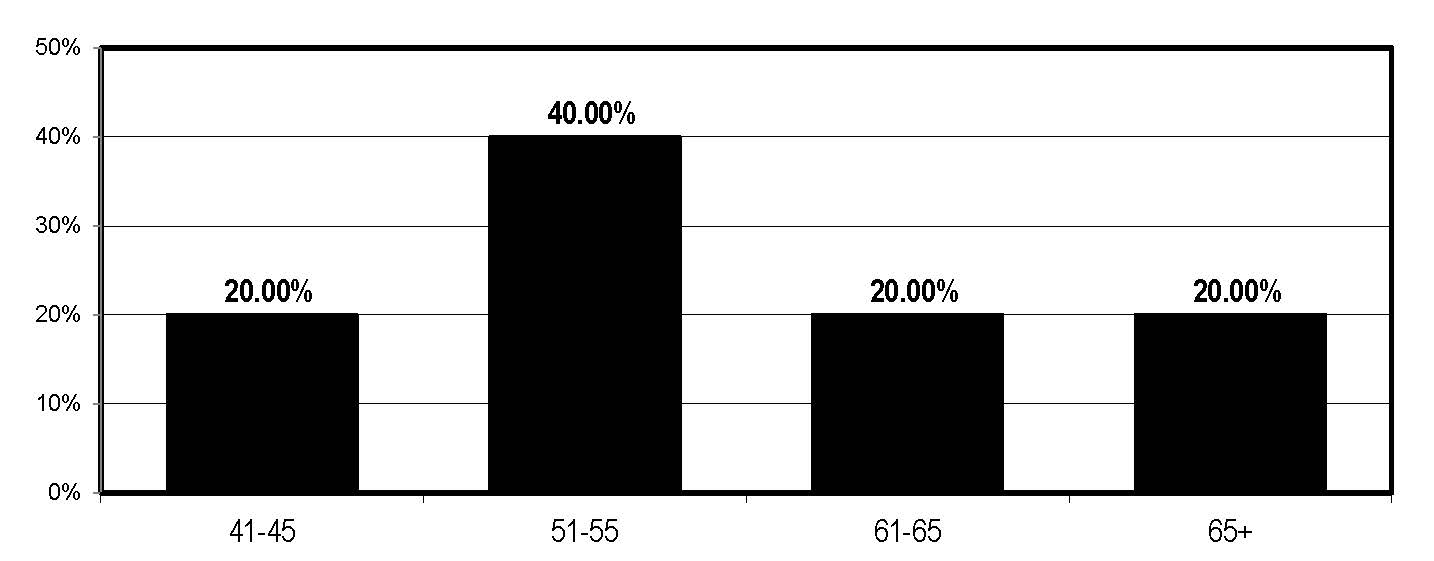
“The average age of case managers keeps increasing with boomers, and we’re well into our 50s now,” she adds. “This is not an entry level job, and it takes someone who has healthcare experience.”
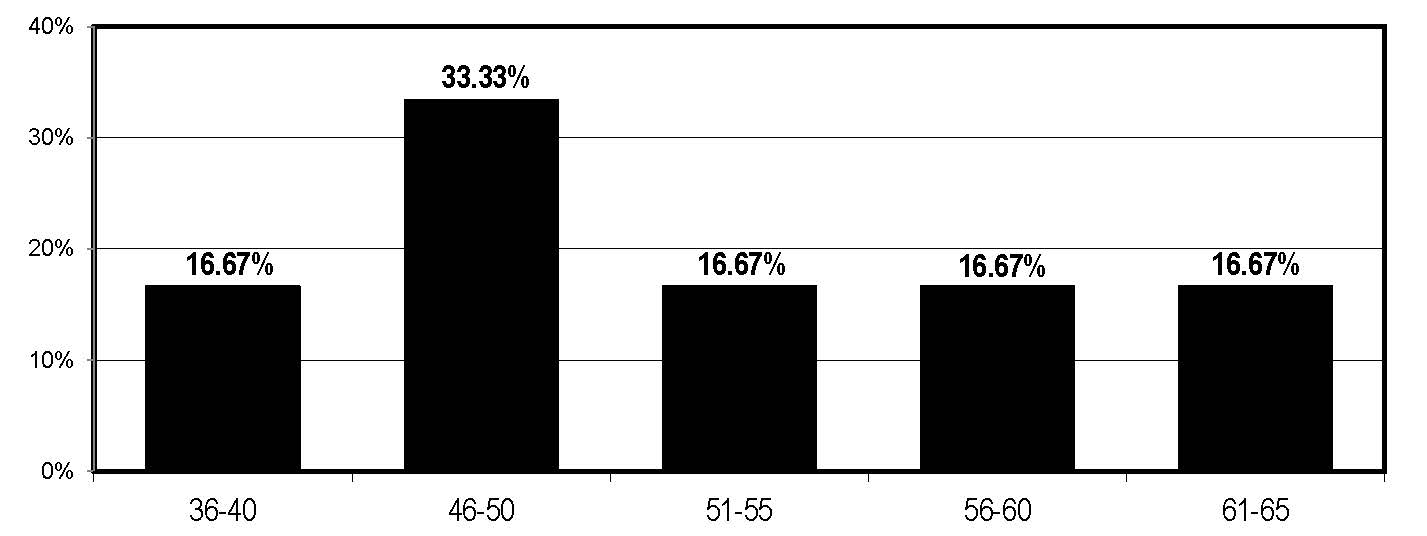
The Case Management Advisor 2015 Salary Survey suggests the same trend of aging CMs: Survey respondents were age 36 to 65, with most middle-aged, in their 40s and 50s.
There’s the conundrum: To become a fully qualified case manager, the job requires a professional healthcare background with some years or decades of experience, followed by case management training and, increasingly, credentialing.
“The job really needs someone with experience in doing case management,” Leonard notes. “It takes a lot of training, and in some cases we’re willing to make that investment for a new orientee.”
But the ideal case management employee is someone who understands what care coordination is and has some understanding of what patients' different needs are, she adds.
Ahrendt offers a solution to the CM pipeline problem, saying experienced case managers have a professional responsibility to mentor nurses and others who desire making a career change to case management.
“I’ve been mentoring nurses and rehab counselors,” Ahrendt says. “I do a lot of pediatric case management, and there’s a small number of people who do that, so I’ve taken a person under my wing to work with me.”
Knowing that her area has a huge deficit in bilingual pediatric case managers, she’s mentored a bilingual young woman she met through a professional conference. The woman — with Ahrendt’s guidance — is learning case management skills with a pediatric population.
“I live in a very diverse community, so having an individual who can work with non-English-speaking families with specialty in children is a gift to the community,” Ahrendt says. “Whether we like it or not, those of us moving into the middle years have a professional responsibility to mentor others.”
Experienced case managers can embrace mentoring for altruistic or even personal reasons, she observes. “I guess some of it is selfish on my part,” Ahrendt says. “I don’t know that I won’t need a case manager myself someday.”
While the bigger picture shows a serious gap between need for case managers in the future and the current pipeline, it also suggests that today’s case management professionals are well-positioned in their careers for decades to come.
“I do think the evolution of healthcare, whichever direction it goes, will continue to value the importance and impact of case management,” Ahrendt says.
In the last year, how has your salary changed?
What is your annual gross income?
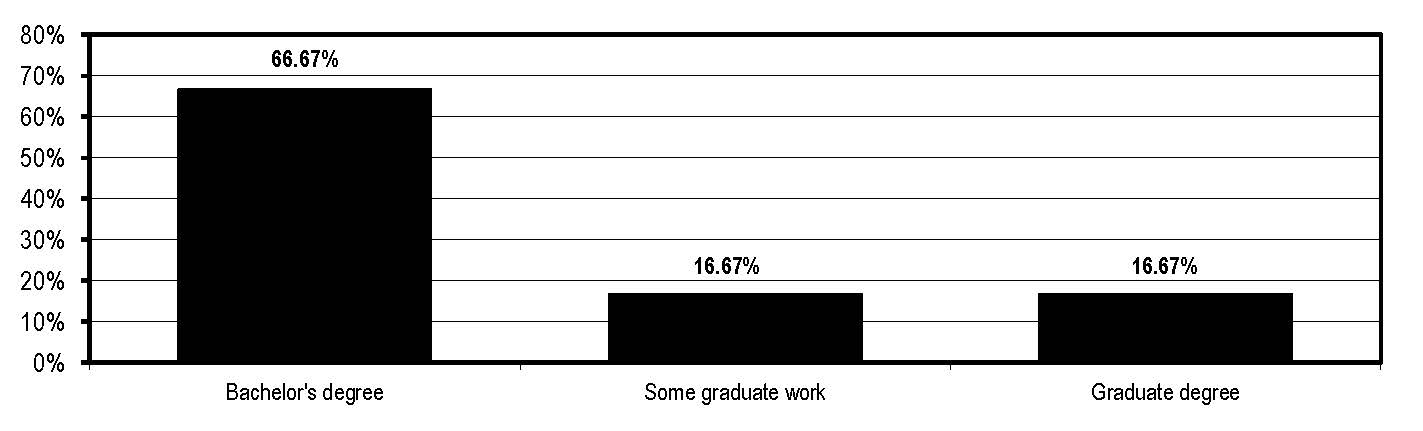
What is your highest degree?
What is your age?
How many hours a week do you work?
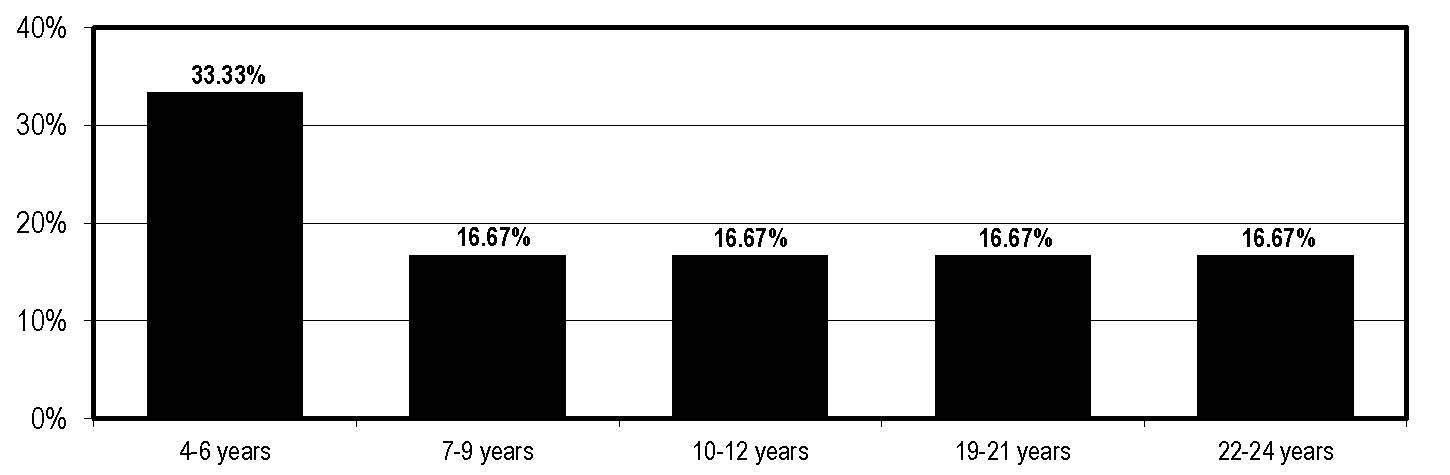
How long have you worked in case management?
 dddd
dddd
The nation’s healthcare expansion into population health models and moving payment away from fee-for-service toward pay for quality performance and financial stewardship has created an unprecedented need for experienced case managers, and their salaries are climbing.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.