Diagnosis and Management of Pediatric Concussions in the ED
February 1, 2016
Reprints
Authors
Akhila Pamula, MD, Resident Physician, Stanford/Kaiser Emergency Medicine Residency, Department of Emergency Medicine, Stanford School of Medicine, Stanford, CA
Calvin E. Hwang, MD, Kaiser Permanente Santa Clara Medical Center, Santa Clara, CA
N. Ewen Wang, MD, Professor of Emergency Medicine, Associate Director of Pediatric Emergency Medicine, Stanford School of Medicine, Stanford, CA
Peer Reviewer
Samuel H.F. Lam, MD, RDMS, Clinical Associate Professor of Emergency Medicine, University of Illinois at Chicago
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor), Dr. Skrainka (CME question reviewer), Ms. Wurster (nurse planner), Dr. Pamula (author), Dr. Hwang (author), Dr. Wang (author), Dr. Lam (peer reviewer), Ms. Coplin (executive editor) and Ms. Mark (executive editor) report no relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- Headache is the most commonly reported symptom of concussion, with immediate loss of consciousness occurring in < 10% of cases. Early symptoms of concussion may also include dizziness, amnesia to the event, confusion, nausea, and vomiting.
- Short-term predictors of prolonged symptoms include increased number of initial symptoms, older age (adolescent vs child), loss of consciousness and amnesia, and premorbid conditions including previous concussion, learning difficulties, and psychiatric illness.
- Regardless of age group, PECARN recommends a CT scan in any child who presents with a Glasgow Coma Scale < 15, altered mental status, signs of palpable or basilar skull fracture.
- In children older than 2 years of age, symptoms in which shared decision-making should be employed regarding CT imaging vs observation (either at home or in the ED) include history of vomiting, loss of consciousness, severe headache, or severe mechanism of injury.
- In children younger than 2 years of age, risk factors in which imaging should be considered include a nonfrontal scalp hematoma, abnormal activity according to the parents, or a severe mechanism of injury.
Head trauma is a common pediatric presentation in emergency departments (EDs). While traumatic brain injury can be a major cause of death and disability, most children have mild, non-life-threatening events. In recent years, there has been increased public awareness of mild traumatic brain injury, or “concussion,” and its sequelae in children. Children with a possible concussion frequently first present in the ED. Thus, its diagnosis, management, and aftercare are significant issues in the pediatric ED.
— Ann M. Dietrich, MD, FAAP
Definition
A wide variation exists in definitions for pediatric head injuries. For the purpose of this article, pediatric head trauma will be divided into three categories: mild head trauma, mild traumatic brain injury, and clinically important traumatic brain injury.1 Definitions for these three distinct entities can be found in Table 1. Diagnostic criteria for mild traumatic brain injury are listed in Table 2. The term concussion has been used interchangeably with mild traumatic brain injury, although a universally accepted definition still remains elusive. The current international definition of concussion, as determined by the Fourth International Conference on Concussion in Sport, has multiple components; it is defined as a brain injury induced by biomechanical forces resulting in short-lived impairment of neurologic function that resolves spontaneously. According to the definition, the acute clinical symptoms of concussion reflect a functional disturbance as opposed to a structural injury; therefore, no abnormality is seen on standard structural neuroimaging studies.2 Acute symptomology is thought to be related to transient axonal injury, alteration in cerebral blood flow, metabolic derangement, and microstructural change.
Table 1. Definition of Pediatric Head Trauma |
|||
|
Mild Head Trauma |
Mild Traumatic Brain Injury |
Clinically Important Traumatic Brain Injury |
|
|
Glasgow Coma Scale |
15 |
14-15 |
Usually < 14 |
|
Definition |
Age < 2 years: either a history or physical signs of blunt trauma to the skull or scalp in an infant or child who is alert or awakens to voice or light touch. Age > 2 years: head trauma resulting in a normal neurologic exam and no physical evidence of skull fracture |
Head trauma associated with disorientation, vomiting, or brief loss of consciousness |
Head trauma associated with the presence of intracranial injury on CT imaging that warrants surgical intervention, intubation for management, hospitalization for > 48 hours, or death |
|
Adapted from: Schutzman S. Minor head trauma in infants and children: Management. In: Post TW, ed. UpToDate. Waltham, MA: UpToDate. Available at: http://www.uptodate.com/contents/minor-head-trauma-in-infants-and-children-evaluation. Accessed Aug. 8, 2015. |
|||
Table 2. Diagnostic Criteria for Mild Traumatic Brain Injury |
|
A patient with mild traumatic brain injury has had a traumatically induced physiologic disruption of brain function, as manifested by 1 or more of:
|
|
Adapted from the Mild Traumatic Brain Injury Committee of the American Congress of Rehabilitation Medicine |
Epidemiology
More than 600,000 cases of pediatric head trauma present to EDs annually.3 Males in early adolescence are at the highest risk for concussion. Falls are the most common cause in children younger than 10 years of age. Sports-related concussions are the most common cause in children ages 10 years and older.4
Clinical Manifestations
Concussions cause a constellation of functional symptoms in the absence of structural damage. Symptoms can begin with the trauma or in the subsequent 24-48 hours and may evolve slowly over days to weeks. (See Table 3.) Headache is the most commonly reported symptom. Immediate loss of consciousness occurs in < 10% of cases. Early symptoms of concussion may also include dizziness, amnesia to the event, confusion, nausea, and vomiting. The incidence of post-traumatic dizziness or vertigo, thought to be caused by direct injury to the cochlear, labyrinthine, or vestibular structures, has not been well-characterized in the literature.5
Table 3. Concussion Symptom Checklist |
|||
|
Physical |
Cognitive |
Emotional |
Sleep |
|
|
|
|
|
Adapted from: Centers for Disease Control and Prevention. Acute Concussion Evaluation (ACE). Available at: http://www.cdc.gov/headsup/pdfs/providers/ace_ed-a.pdf. Accessed July 30, 2015. |
|||
Over the next hours to days, patients may develop mood or cognitive disturbance, light and noise sensitivity, and sleep disturbance. Occasionally, there may be transient cortical neurologic deficits, including cortical blindness, global amnesia, and slurred or incoherent speech, thought to be due to vascular hyperreactivity, a migraine-equivalent phenomenon.3 A surprisingly large percentage of patients can have continued symptoms for months, which can result in a phenomenon known as post-concussive syndrome described later in this article.
Short-term predictors of prolonged symptoms vary across studies but appear to include increased number of initial symptoms, older age (adolescent vs child), loss of consciousness and amnesia, and premorbid conditions including previous concussion, learning difficulties, and psychiatric illness.6 Interestingly, family history of headaches or migraines is not a predictor identified in the literature.
ED Evaluation
In the ED, all patients with head trauma should have a full medical assessment with a thorough history from both the patient and witnesses to the event. This includes number of previous concussions or head injuries and the dates they occurred. The physical exam should pay special attention to the head, neck, and neurologic exam, including mental status, gait, balance, and evidence of associated extracranial injury. Management of serious brain injury, cervical spine injuries, and major trauma are outside the scope of this article.
Diagnosis — Ruling Out Clinically Important Brain Injury
The differential diagnosis for a concussion includes intracranial injuries such as a contusion, hemorrhage, or edema. Ultimately, the diagnosis of a concussion can be made only after the exclusion of these more serious, structural brain injuries. Thus, a common diagnostic dilemma in children with head trauma is the decision to obtain computed tomography (CT) imaging, an imaging modality both highly sensitive and specific for the detection of epidural and subdural bleeds, and subarachnoid hemorrhages. However, as practitioners and families have become increasingly aware of the possible long-term sequelae of ionizing radiation, researchers have developed algorithms to help guide practitioners in imaging children with head trauma.7
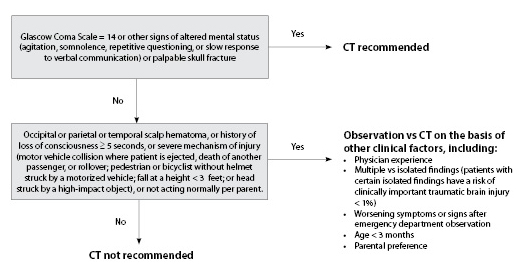
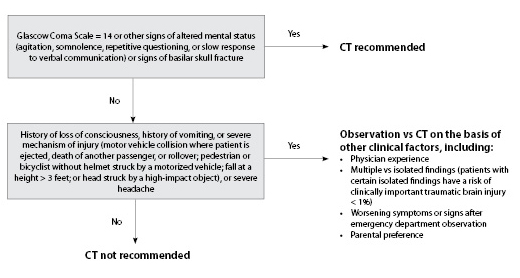
The Pediatric Emergency Care Applied Research Network (PECARN) consortium produced the largest study to date that derived and validated a clinical prediction rule to identify children with very low risk for clinically important traumatic brain injury who, therefore, do not require CT imaging.8 The study population included a combined 42,412 children in the derivation and validation populations. Of note, 10,718 children were younger than 2 years of age. Clinically important traumatic brain injury was defined as brain injury resulting in any of the following: death from traumatic brain injury, brain injury requiring neurosurgical intervention, intubation for more than 24 hours for the brain injury, and/or hospital admission of at least 2 days. Figure 1 describes the PECARN algorithm. Children are divided into two categories: those between the ages of 2 and 18 years and those younger than 2 years of age. Regardless of age group, a CT scan is recommended in any child who presents with a Glasgow Coma Scale (GCS) < 15 (see Table 4), altered mental status, or signs of palpable or basilar skull fracture. Severe mechanism of injury is defined as a fall greater than the child's height (typically < 3 feet for children younger than 2 years of age and > 5 feet for children older than 2 years of age); a motor vehicle collision with ejection, rollover, or fatality; a bike/pedestrian vs vehicle accident in which the patient was not wearing a helmet; or being struck by a high-impact object.
Figure 1. PECARN Algorithm for Imaging Children with Head Trauma |
|
Suggested Algorithm for Children Younger than Age 2 Years |
 |
|
Suggested Algorithm for Children Older than Age 2 Years |
 |
|
Adapted from: Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically important brain injuries after head trauma: A prospective cohort study. Lancet 2009;374:1160-1170. |
Table 4. Glasgow Coma Scale (Infant GCS in Italics) |
|||
|
Eyes |
Verbal |
Motor |
|
|
1 |
No response |
No response |
No response |
|
2 |
Open to pain |
Incomprehensible sounds Moans to pain |
Extension posturing (decerebrate) |
|
3 |
Open to speech |
Inappropriate words Cries to pain |
Flexion posturing (decorticate) |
|
4 |
Spontaneously open |
Confused Irritable |
Withdraws to pain |
|
5 |
Oriented Coos, babbles, smiles, interacts |
Localizes to pain Withdraws to touch |
|
|
6 |
Spontaneous movement |
||
In children older than 2 years of age, symptoms in which shared decision-making should be employed regarding CT imaging vs observation (either at home or in the ED) include history of vomiting, loss of consciousness, severe headache, or severe mechanism of injury. Recent studies have demonstrated that isolated brief loss of consciousness and minimal vomiting are rarely associated with clinically important traumatic brain injury.9
In children younger than 2 years of age, risk factors in which imaging should be considered include a non-frontal scalp hematoma, abnormal activity according to the parents, or a severe mechanism of injury (see definition above). CT imaging should be more strongly considered in infants younger than 3 months of age, as the absence of clinical signs of brain injury is not as reliable. A summary of decision rules for avoiding CT in children with head trauma is presented in Table 5.
Table 5. Decision Rules for Avoiding CT in Children with Head Trauma |
|
|
< 2 years of age |
> 2 years of age |
|
Normal mental status |
Normal mental status |
|
No scalp hematoma except frontal |
No loss of consciousness |
|
Loss of consciousness < 5 seconds |
No vomiting |
|
Non-severe injury mechanism* |
Non-severe injury mechanism* |
|
No palpable skull fracture |
No signs of basilar skull fracture |
|
Normal behavior |
No severe headache |
|
*Severe mechanism defined as motor vehicle collision with patient ejection, death of a passenger, rollover; pedestrian or cyclist without helmet struck by motorized vehicle; fall > 1.5 m for children (> 2 years), struck by motorized vehicle; fall > 1.5 m for children (> 2 years), fall > 0.9 m for < 2 years; or head struck by high-impact object |
|
Two other studies have developed clinical guidelines regarding when to image children with head trauma. The children’s head injury algorithm for the prediction of important clinical events (CHALICE) study identified 14 high-risk criteria for clinically important traumatic brain injury that indicate the need for further imaging. Criteria included witnessed loss of consciousness > 5 minutes, > 5 minutes of amnesia, abnormal drowsiness, more than three episodes of emesis, suspicion of non-accidental injury, seizure, GCS < 14, signs of basilar or depressed skull fracture, focal neurologic exam, or high-risk mechanism. Using these criteria, the group achieved a sensitivity of 98.6% and a specificity of 86.9%.10 Similarly, the Canadian Assessment of Tomography for Childhood (CATCH) study identified four high-risk factors and three medium-risk factors for clinically significant head injury in children. (See Table 6.) The high-risk features include a GCS < 15 at 2 hours after injury, suspected open or depressed skull fracture, worsening headache, or irritability. The medium-risk factors include signs of basal skull fracture, large boggy scalp hematoma, and mechanism of injury (motor vehicle collision, fall from elevation ≥ 3 ft or five stairs, fall from bicycle with no helmet). The high-risk features were 100% sensitive and 70.2% specific in detecting clinically important traumatic brain injury, while the medium-risk features were 98.1% sensitive and 50.1% specific.11 However it is important to note that these rules have not been as well validated as the PECARN rule.12
Table 6. Canadian Assessment of Tomography for Childhood Head Injury: The CATCH Rule |
|
CT of the head is required for children with a minor head injury* plus any one of the following findings: |
|
High risk (need for neurological intervention)
|
|
Medium risk (brain injury on CT scan)
|
|
*Minor head injury is defined as an injury sustained within the past 24 hours associated with witnessed loss of consciousness, definite amnesia, witnessed disorientation, persistent vomiting (more than one episode), or persistent irritability (in a child younger than 2 years of age) in a patient with a Glasgow Coma Scale score of 13 to 15. CT = computed tomography |
Diagnosis of Concussion
Once the diagnosis of structural brain injury has been excluded (with or without imaging), concussion can still be difficult to identify, as there is currently no objective measure with which to make the diagnosis. Given that the majority of concussions do not result in dramatic symptoms such as loss of consciousness, a concussion can go unrecognized by both the patient and medical providers. Thus, a number of cognitive diagnostic tools have been developed to aid in the identification of a concussion. The Standardized Assessment of Concussion (SAC) and the Sport Concussion Assessment Tool 3 (SCAT3) are the most commonly used cognitive screens. The SAC, which was part of the predecessor for the SCAT3, was developed for the sideline evaluation of athletes who sustained head trauma, and includes measures of orientation, immediate memory, delayed recall, concentration, neurologic testing, and exertional maneuvers, with lower scores associated with concussion. It is important to note that while the scores were found to be slightly lower in children with concussion, it only reached statistical significance in the age group of 12-14 years. Furthermore, it should not be used in isolation to determine return to play.13
Endorsed by the Consensus Statement on Concussion in Sport in 2014, SCAT3 increasingly has been used. It assesses subjective symptoms, includes the SAC cognitive assessment, and evaluates coordination and balance. It differs from SCAT2 in that it includes a neck exam. For children younger than age 12 years, a Child SCAT3 has been developed.2 Checklists for the SCAT3, Child SCAT3, and SAC assessments can be found online: (SAC/SCAT3: http://bjsm.bmj.com/content/47/5/259.full.pdf, accessed Sept. 2015; Child SCAT3: http://bjsm.bmj.com/content/47/5/263.full.pdf, accessed Sept. 2015).
SCAT3 can be time-consuming and ideally it is used as a tool for repeat assessment; therefore, it is not an ideal test to perform in the ED. However, there is general consensus that balance testing is the most specific finding for concussion.
Disposition
Patients can be discharged safely from the ED if the following criteria are met: a return to baseline level of function with a GCS of 15, tolerance of oral intake without significant nausea or vomiting, no other injuries warranting admission, and reliable caretakers. Discharge instructions should outline strict return precautions, including inability to awaken the child, seizure, vomiting that begins 4-6 hours after the injury or continued vomiting, a change in mental status, or new unsteady gait or clumsiness/incoordination. Although there is still debate about periodically waking up the child from sleep during the night, providers now feel that there may be more benefit from uninterrupted sleep, and frequent awakenings may exacerbate symptoms.14 Follow-up with a physician or an athletic trainer should be arranged within 48 hours for symptom re-evaluation and initiation of progression to return to activity if appropriate.15
Typically, if a child has not been imaged and continues to be symptomatic or returns with increased symptoms, he or she should be imaged. If the child has been imaged, it is important to note that delayed clinically important traumatic brain injury after a normal CT scan is extremely rare. A retrospective cohort study of more than 17,000 children in Canada with a normal CT or asymptomatic 6-hour observation period identified delayed clinically important traumatic brain injury in 0.03% of patients.16 Magnetic resonance imaging (MRI) can detect cerebral contusion, petechial hemorrhage, and white matter injury at a superior level to CT; however, its use in a child with a negative CT and without severe or focal symptoms is not recommended in the ED setting, as the management of the patient likely would not change based on the results. Rather, further imaging is best coordinated, if indicated, through the care of an outpatient physician evaluating the child.14 Care and reimaging should be managed in conjunction with parents and considering the entire clinical picture. It is not unreasonable to admit a patient with a negative head CT for observation, hydration, and management of symptoms.
Headache is a frequent complaint after blunt head trauma, and is of particular concern to parents, patients, and practitioners when it is persistent or worsening over time. However, if mild-to-moderate headache is the only symptom, even if the patient was not imaged initially (in accordance with PECARN guidelines), imaging studies are not generally indicated, as the risk of a clinically important traumatic brain injury is low. A recent prospective multicenter cohort of approximately 28,000 verbal children with minor head trauma found that there was no associated clinically important traumatic brain injury when headache was an isolated symptom.17
Generally, acetaminophen is the recommended medication for treatment of post-concussion headache. Nonsteroidal anti-inflammatory drugs (NSAIDs) should be avoided for at least the first 48-72 hours after a head injury. It is generally recommended to also avoid narcotics to prevent changes in mental status or neurologic exam. A retrospective study in adolescent patients with concussion demonstrated that overuse of analgesics may exacerbate concussion-related headaches or prolong their duration.18 Nausea is also a common problem associated with concussion, so using non-sedating antiemetics, such as ondansetron, can be helpful in both the immediate and outpatient setting. Vertiginous symptoms post trauma can be treated with meclizine. Patients with ongoing and/or severe symptoms may require vestibular rehabilitation for their vertigo, although this determination will need to be done as an outpatient by a primary care physician or a provider specializing in concussion.19
Some patients may be asymptomatic initially and develop symptoms hours after the head trauma. A 2014 study by Eisenberg et al showed that fatigue, sleep disturbance, forgetfulness, and frustration often developed within 1 week of the initial head trauma.20 Thus, in the ED, it is important to set expectations for possible occurrence and follow-up of the above-mentioned delayed symptoms. For the majority of patients, symptoms resolve within 2 weeks of injury. However, during this recovery period, symptoms can be debilitating, with more than two-thirds of patients reporting continued headaches 1 week after the injury, and the majority complaining of dizziness, fatigue, and slower thinking.20
During counseling, it is important to discuss potential complications and provide thorough instructions regarding physical and cognitive rest. Pediatric patients have a higher risk of prolonged post-concussive symptoms and recurrent concussion when there is premature return to cognitive and physical activity. Furthermore, there is evidence that pediatric patients take longer to recover from mild traumatic brain injury compared to adults.21,22
Patients diagnosed with concussion should be told to avoid any resistance and aerobic activities, including returning to sports, for a minimum of 48 hours or until evaluated by a medical provider, particularly when concussion symptoms are ongoing. Recent evidence has suggested that light cardiovascular activity, initiated 48 hours after head injury, may shorten duration of symptoms.23 Although children should be told to see their primary physician prior to return to play, emergency practitioners should be aware of the general recommendations of Return to Play protocols (see Table 7). Once athletes are asymptomatic and their SCAT3 scores are at baseline (if one is available), they may begin the Return to Play protocol and should spend a minimum of 24 hours at each step of the pathway. If symptoms recur at any step, the patient should return to the previous asymptomatic step and should only attempt to progress after remaining asymptomatic for 24 hours. The Return to Play protocol was developed for high school and college-aged athletes; in younger children, a more prolonged progression through the protocol should be considered.24
Table 7. Graduated Return to Play Protocol |
||
|
Rehabilitation Stage (usually a minimum of 24 hours per stage) |
Functional Exercise at Stage |
Objective of Stage |
|
No activity |
Symptom limited physical and cognitive rest |
Recovery |
|
Light aerobic exercise |
Walking, swimming, stationary bike, keeping intensity < 70% maximum permitted heart rate |
Increase heart rate |
|
Sport-specific exercise |
No head impact activities |
Add movement |
|
Noncontact training drills |
|
Exercise, coordination, and cognitive load |
|
Full contact practice |
Participation in normal training activities |
Assess functional skills by coaching staff |
|
Return to play |
Normal game play |
|
|
Adapted from: McCrory P, Meeuwisse W, Aubry M, et al. Consensus statement on concussion in sport: The 4th International Conference on Concussion in Sport, held in Zurich, November 2012. Clin J Sport Med 2013;23:89-117. |
||
Cognitive rest is a more controversial topic. Strict cognitive rest, including the absence from school and avoidance of screen time, social activities, video games, loud music, and reading, has been part of the primary treatment for pediatric concussion. However, a recent study demonstrated that strict cognitive rest was associated with more daily reported post-concussive symptoms during the 10 days of follow-up, with no differences in neurocognitive function.23 Therefore, a more individualized approach to cognitive rest — in which patients are instructed to avoid mental activities that worsen symptoms, with close follow-up by their outpatient provider — may be prudent. Patients who continue to have symptoms beyond 2 weeks may warrant neuropsychological testing, further follow-up with a concussion specialist, and potentially further imaging (e.g., MRI) at the discretion of that provider.
Complications
The long-term effects of concussions in the pediatric population are not well understood given the lack of long-term prospective studies. Studies have shown that 3 months after concussion, 35% of children between the ages of 8 and 16 years complained of difficulty with concentration and memory.25 Another study indicated that > 60% of pediatric patients reported a decline in grades for that term.26
Post-concussion Syndrome. While there is no universally accepted definition for post-concussion syndrome, the DSM-IV defines it as 3 months duration of three or more of the following symptoms: fatigue, dizziness/vertigo, headache, personality or behavioral changes, anxiety or depression, or apathy. There is often a decline in school performance and difficulty in memory or attention.27 (See Tables 8 and 9.) Post-concussion syndrome is a common sequelae of mild traumatic brain injury, with studies citing anywhere from 29-43% of patients experiencing symptoms including headaches, dizziness, neuropsychiatric symptoms, and cognitive impairment.25,28 Risk factors for developing persistent post-concussive symptoms include older age, headache as the initial symptom, high initial level of symptomology, post-traumatic amnesia, loss of consciousness, and premorbid conditions including previous concussions, learning difficulties, and underlying psychiatric difficulties.29,30 Children with presumptive post-concussion syndrome should be referred to a concussion specialist for further management, which may include neuropsychiatric testing.
Table 8. Diagnostic Criteria for Post-concussive Disorder |
|
A history of head trauma that has caused considerable cerebral concussion |
|
Evidence from neuropsychological testing or quantified cognitive assessment of difficulty in attention (concentrating, shifting focus of attention, performing simultaneous cognitive tasks) or memory (learning or recall of information) |
|
Three (or more) of the following occurring shortly after the trauma and lasting at least 3 months:
|
|
The symptoms in bullets 2 and 3 have their onset following head trauma or represent a substantial worsening of pre-existing symptoms. |
|
The disturbance causes considerable impairment in social or occupational functioning and represents a considerable decline from a previous level of functioning. In school-age children, the impairment might manifest as a substantial worsening in school or academic performance dating from the trauma. |
|
The symptoms do not meet criteria for dementia due to head trauma and are not better accounted for by another mental disorder (e.g., amnesic disorder due to head trauma, personality change due to head trauma). |
|
No single test score can be the basis of a concussion diagnosis. Moderate evidence that standardized symptom checklists (Post-Concussion Symptom Scale/Graded Symptom Checklist [GSC]) and the Standardized Assessment of Concussion (SAC) when administered early after a suspected concussion have moderate to high sensitivity and specificity in identifying sports concussions relative to those of the reference standard of a clinician-diagnosed concussion. Low-moderate evidence that the Balance Error Scoring System (BESS) has low to moderate sensitivity and moderate to high specificity in identifying sports concussions. Those affected may have exacerbation of symptoms with mental or physical exertion. Adapted from: Diagnostic and Statistical Manual of Mental Disorders, 4th edition. |
Table 9. Diagnostic Criteria for Post-Concussion Syndrome (ICD-10) |
|
A. History of head trauma with loss of consciousness preceding symptom onset by a maximum of 4 weeks. B. Symptoms in 3 or more of the following symptom categories:
|
|
World Health Organization. ICD-10 Version:2016. F07.2 Postconcussional syndrome Available at: http://apps.who.int/classifications/icd10/browse/2016/en#/F07.2. Accessed Jan. 7, 2016. |
Second Impact Syndrome. Second-impact syndrome is a rare condition in which the brain undergoes rapid and severe swelling. It occurs when a second head injury occurs before the symptoms associated with the initial injury have resolved. The pathophysiology is poorly understood, but it is thought to result from a loss of autoregulation, causing cerebral vascular congestion that can progress to severe cerebral edema.31 Interestingly, all reported cases have been in athletes younger than 20 years of age, leading to the conclusion that pediatric and adolescent athletes are at higher risk for this complication.
Summary
Concussion is a common presentation in the pediatric population. Patients and parents should be made aware that symptoms can persist for some time and that recovery time can vary. After ruling out clinically important traumatic brain injury, the emergency physician should treat symptoms, counsel patients about the need for close follow-up, and provide discharge instructions to not resume exacerbating cognitive or physical activities until evaluated by their outpatient provider.
REFERENCES
- Schutzman S. Minor head trauma in infants and children: Management. In: Post TW, ed. UpToDate. Waltham, MA. Available at: http://www.uptodate.com/contents/minor-head-trauma-in-infants-and-children-evaluation. Accessed Aug. 8, 2015.
- McCrory P, Meeuwisse W, Aubry M, et al. Consensus statement on concussion in sport: The 4th International Conference on Concussion in Sport Held in Zurich, November 2012. Clin J Sport Med 2013;23:89-117.
- Caskey RC, Nance ML. Management of pediatric mild traumatic brain injury. Adv Pediatr 2014;61:271-286.
- Stewart TC, Gilliland J, Fraser DD. An epidemiologic profile of pediatric concussions. J Trauma Acute Care Surg 2014;76:736-742.
- Friedman JM. Post-traumatic vertigo. Med Health R I 2004;87:296-300.
- Graham R, Rivara FP, Ford M, Spicer CM. Treatment and Management of Prolonged Symptoms and Post-Concussion Syndrome. In: Sports-Related Concussions in Youth: Improving the Science, Changing the Culture. Washington, DC: The National Academies Press; 2014.
- Brody AS, Frush DP, Huda W, Brent RL; American Academy of Pediatrics Section on Radiology. Radiation risk to children from computed tomography. Pediatrics 2007;120:677-682.
- Kuppermann N, Holmes JF, Dayan PS, et al. Identification of children at very low risk of clinically-important brain injuries after head trauma: A prospective cohort study. Lancet 2009;374:1160-1170.
- Lee LK, Monroe D, Bachman MC, et al. Isolated loss of consciousness in children with minor blunt head trauma. JAMA Pediatr 2014;168:837-843.
- Dunning J, Daly JP, Lomas JP, et al. Derivation of the children’s head injury algorithm for the prediction of important clinical events decision rule for head injury in children. Arch Dis Child 2006;91:885-891.
- Osmond MH, Klassen TP, Wells GA, et al. CATCH: A clinical decision rule for the use of computed tomography in children with minor head injury. CMAJ 2010;182:341-348.
- Lyttle MD, Crowe L, Oakley E, et al. Comparing CATCH, CHALICE and PECARN clinical decision rules for paediatric head injuries. Emerg Med J 2012;29:785-794.
- Grubenhoff JA, Kirkwood M, Gao D, et al. Evaluation of the standardized assessment of concussion in a pediatric emergency department. Pediatrics 2010;126:688-695.
- Halstead M, Walter KD; Council on Sports Medicine and Fitness. American Academy of Pediatrics. Clinical Report: Sport-related concussion in children and adolescents. Pediatrics 2010;126:597-615.
- Ropper AH, Gorson KC. Clinical practice. Concussion. N Engl J Med 2007;356:166-172.
- Hamilton M, Mrazik M, Johnson DW. Incidence of delayed intracranial hemorrhage in children after uncomplicated minor head injuries. Pediatrics 2010;126;e33-e39.
- Dayan PS, Holmes JF, Hoyle J Jr, et al. Headache in traumatic brain injuries from blunt head trauma. Pediatrics 2015;135:504-512.
- Bernhardt DT. Concussion Medication. Medscape. Available at: http://emedicine.medscape.com/article/92095-medication. Accessed July 22, 2015.
- Hoffer ME, Gottshall KR, Moore R, et al. Characterizing and treating dizziness after mild head trauma. Otol Neurotol 2004;25:135-138.
- Eisenberg MA, Meehan WP 3rd, Mannix R. Duration and course of post-concussive symptoms. Pediatrics 2014;133:999-1006.
- Grady MF. Concussion in the adolescent athlete. Curr Probl Pediatr Adolesc Health Care 2010;40:154-169.
- Atabaki SM. Updates in the general approach to pediatric head trauma and concussion. Pediatr Clin North Am 2013;60:1107-1122.
- Thomas DG, Apps JN, Hoffmann RG, et al. Benefits of strict rest after acute concussion: A randomized controlled trial. Pediatrics 2015;135:213-223.
- May KH, Marshall DL, Burns TG, et al. Pediatric sports specific return to play guidelines following concussion. Int J Sports Phys Ther 2014;9:242-255.
- Blinman TA, Houseknecht E, Snyder C, et al. Postconcussive symptoms in hospitalized pediatric patients after mild traumatic brain injury. J Pediatr Surg 2009;44:1223-1228.
- Corwin DJ, Zonfrillo MR, Master CL, et al. Characteristics of prolonged concussion recovery in a pediatric subspecialty referral population. J Pediatr 2014;165:1207-1215.
- Alla S, Sullivan SJ, Hale L, McCrory P. Self-report scales/checklists for the measurement of concussion symptoms: A systematic review. Br J Sports Med 2009;43(Suppl 1):i3-12.
- Babcock L, Byczkowski T, Wade SL, et al. Predicting postconcussion syndrome after mild traumatic brain injury in children and adolescents who present to the emergency department. JAMA Pediatr 2013;167:156-161.
- Zemek RL, Farion KJ, Sampson M, McGahern C. Prognosticators of persistent symptoms following pediatric concussion: A systematic review. JAMA Pediatr 2013;167:259-265.
- McCrea M, Guskiewicz K, Randolph C, et al. Incidence, clinical course, and predictors of prolonged recovery time following sport-related concussion in high school and college athletes. J Int Neuropsychol Soc 2013;19:22-33.
- McClain R. Concussion and trauma in young athletes: Prevention, treatment, and return-to-play. Prim Care 2015;42:77-83.
MONOGRAPH: Here are crucial steps to treat this common presentation in children.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
