Commonly Missed Radiographic Findings
February 15, 2016
Reprints
Authors
Caroline M. Molins, MD, FACEP, FAAEM, Curriculum Director, Florida Hospital Emergency Medicine Residency, Orlando, FL; Assistant Professor, University of Central Florida College of Medicine, Orlando; Clinical Assistant Professor, Florida State University, College of Medicine, Orlando.
Carmen J. Martinez Martinez, MD, FACEP, FAAEM, Core Faculty, Florida Hospital Emergency Medicine Residency, Orlando, FL; Clinical Faculty, Florida Hospital Pediatric Residency, Orlando; Assistant Professor, University of Central Florida College of Medicine, Orlando; Clinical Assistant Professor, Florida State University, College of Medicine, Orlando.
Peer Reviewer
Charles L. Emerman, MD, Professor and Chairman of Emergency Medicine, Case Western Reserve University, Cleveland, OH.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Farel (CME question reviewer) owns stock in Johnson & Johnson. Dr. Stapczynski (editor) owns stock in Pfizer, Johnson & Johnson, Walgreens Boots Alliance Inc., GlaxoSmithKline, Bristol Myers Squibb, and AxoGen. Dr. Schneider (editor), Ms. Fessler (nurse planner), Dr. Molins (author), Dr. Martinez (author), Dr. Emerman (peer reviewer), Ms. Mark (executive editor), Leslie Coplin (executive editor), and Mr. Landenberger (editorial and continuing education director) report no financial relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- Missed fractures are often subtle, small, and occur in areas where overlapping bones obscure their detection.
- Carefully inspect hand, wrist, and foot images.
- Ask the radiology technician and radiologist (if available) for advice on alternative imaging views to visualize specific areas.
- If initial radiographs are “normal” but continued pain and tenderness suggest occult fracture, consider referral for advanced imaging with computed tomography or magnetic resonance imaging.
- When in doubt, immobilize the injured limb and refer to appropriate specialist.
“Errors in judgment must occur in the practice of an art which consists largely in balancing probabilities.”
— Sir William Osler (1849-1919), Aequanimitas, with Other Addresses, Teacher and Student
“As the gods are my witness, I have seen things on subsequent viewing that I initially did not.”
— Sign in a radiologist’s cubicle, c. 1978
The practice of medicine involves judgment, the weighing of possibilities and probabilities. Even more so when interpreting radiographs. Even though the image exists in black and white, with shades of gray, the important point is, do we recognize what it means? I hope you find this issue of Emergency Medicine Reports, which discusses some radiographic findings that have the potential to be missed or underappreciated, useful in your practice.
— J. Stephan Stapczynski, MD, Editor
INTRODUCTION
Plain radiographs are commonly ordered for patients who arrive in the emergency department (ED), and interpretation of those radiographs is critical. Misinterpretation of these studies is of great importance and a great source of medical error.1,2 Analysis of medical legal cases has repeatedly shown that fractures are among the top six high-risk diagnoses and alleged missed fractures are the second highest payouts in malpractice litigation, comprising 20% of malpractice claims between 1980 and 1987, decreasing to 10% between 1988 and 1990.3-5 While there is no direct evidence that shows which specific missed radiographic findings are the most common, a common feature is that a significant number of misinterpretations are made by non-radiologists.6-9 Studies have been conducted to evaluate the reasons for these misinterpretations.
Some studies have found that a significant number of misinterpretations occur during “off” hours, such as between 12 a.m. and 7 a.m. on weekdays and 6 p.m. to 7 a.m. on weekends. In many hospitals, the emergency physician (EP) is responsible for interpreting plain radiographs during these hours. It is easy to envision that a busy clinician, viewing these radiographic images on standard computer monitors in a noisy environment, may miss findings that a radiologist with less distraction and better equipment may find. However, it must also be acknowledged that radiologists have more knowledge and experience than other clinicians at interpreting radiographs. Thus the reported 2% to 11% discrepancy rate between EP and radiologist interpretations is real.10-13 To reduce misinterpretations, an increasing number of hospitals are going “digital,” replacing physical film sheets with digitized picture archiving and communication systems (PACS) that allow for off-site interpretation (tele-radiology)14-17 and more robust quality improvement programs.18
Despite the above interventions, errors in radiograph interpretation still occur on the EP’s part. This article will discuss some steps to take to avoid such mistakes. The EP should perform a careful physical exam, formulate a differential diagnosis, order tests based on the presumptive diagnosis, know and search for the radiographic findings associated with that diagnosis, examine the radiographs thoroughly, and apply the image findings to patient care.19 Even though we may apply the above reasoning, we should acknowledge that a breakdown in the diagnostic process can still occur. A study of closed ED malpractice claims shows that these breakdowns are due to failures in: ordering the appropriate diagnostic test (58%), performing an adequate history and physical exam (42%), incorrectly interpreting a diagnostic test, and ordering an appropriate consultation (33%).20
A retrospective study of diagnostic errors in the ED found that approximately 80% of missed diagnoses were fractures, with 80% of these being due to missed radiographic findings and 4% were non-traumatic injuries.21 Tables 1 and 2 show the specific areas of missed fractures or missed radiographic interpretations.22-23 One of the more recent studies shows that among the most commonly missed findings are also foreign body, airspace disease, pulmonary nodules, and pneumothorax.24 It would also be prudent to note that the pediatric population is a high-risk population for missed radiographic interpretation.19
TABLE 1. MISSED EMERGENCY RADIOLOGY EXTREMITY FRACTURES BY REGION22
|
Location |
Percentage Missed (%) |
Missed/All Fractures |
|
Foot |
7.6 |
18/238 |
|
Knee |
6.3 |
14/224 |
|
Elbow |
6.0 |
14/234 |
|
Hand |
5.4 |
10/185 |
|
Wrist |
4.1 |
25/606 |
|
Hip |
3.9 |
20/512 |
|
Ankle |
2.8 |
8/282 |
|
Shoulder |
1.9 |
5/266 |
|
Tibia/Fibula |
0.4 |
1/266 |
|
Total |
3.7 |
115/3081 |
TABLE 2. MISSED EMERGENCY RADIOLOGY EXTREMITY FRACTURES by SPECIFIC LOCATION22
|
Percentage Missed (%) |
Missed/All Fractures |
|
|
Tibial Plateau |
16 |
3/19 |
|
Radial head |
14 |
12/84 |
|
Elbow-child |
14 |
5/35 |
|
Scaphoid |
13 |
7/53 |
|
Calcaneus |
10 |
5/50 |
|
Patella |
6 |
3/53 |
|
Ribs |
4 |
23/548 |
GENERAL APPROACH TO RADIOGRAPHS
Interpretation of radiographs is not an easy task, and almost every physician has a different and unique approach, although many are similar. Two commonly utilized approaches to radiographic interpretation are the systematic and targeted approach. The systematic approach looks at all the different types of tissue seen on the film. Common mnemonics for this technique include “A,B,Cs” (Airway, Bones, Circulation, and Soft Tissue for chest radiographs and Alignment, Bones, Cartilage, and Soft Tissue for skeletal images), “In to Out,” and “Out to In.” Using the targeted approach means that the radiograph is examined with the pathological patterns in mind (i.e., pattern recognition for common abnormalities, looking for commonly missed findings, diagnosis based on the clinical presentation and examination).25 Once a physician has developed his or her own approach to radiographic interpretation, it is important to continue to practice that method and use it as frequently as possible. As we discuss different radiographs, we will be focusing the discussion on the commonly missed diagnosis and the signs to look for when considering them.
CHEST RADIOGRAPHS
Chest radiographs are very commonly ordered in the ED for a variety of reasons. It is inevitable that with the frequency that EPs order this study, there inherently will also be some diagnostic error associated with them. As previously mentioned, the most commonly missed findings of chest plain films include airspace disease, pulmonary nodules, and pneumothorax.26 All of these diagnoses have one thing in common: They are commonly found in the most difficult place to evaluate on chest X-ray (CXR) — the lung apices and inferior bases. The lung apices and inferior bases pose challenges in their evaluation due to the presence of overlying structures, such as ribs, clavicle, diaphragm, and solid organs.26
Airspace disease is a broad category that includes pneumonia, pulmonary edema, and pulmonary embolism, among others. Some small or hazy focal pulmonary infiltrates can be difficult to visualize. Some find it helpful to consider silhouette signs to help identify them. These silhouette signs are: obliteration of normal air/soft-tissue interface, accentuation of the interlobar fissures, air bronchograms, and obliteration of normal pulmonary vascular markings.19 Despite looking for these clues, pneumonia can still be present despite a negative CXR.27
Pneumothorax is a critical diagnosis that all EPs should be comfortable with diagnosing through CXR. As previously mentioned, although CXR poses some challenges to making this diagnosis, it is prudent to look very closely. On an upright radiograph, an EP should look for the fine white line of the visceral pleural surface, “pleural cap,” of the collapsed lung, with or without the presence of subcutaneous emphysema. A supine film can also show the presence of a “deep sulcus” sign, which is defined as an exceptionally deep radiolucent costophrenic sulcus.19,20 (See Figure 1.)
FIGURE 1. PNEUMOTHORAX
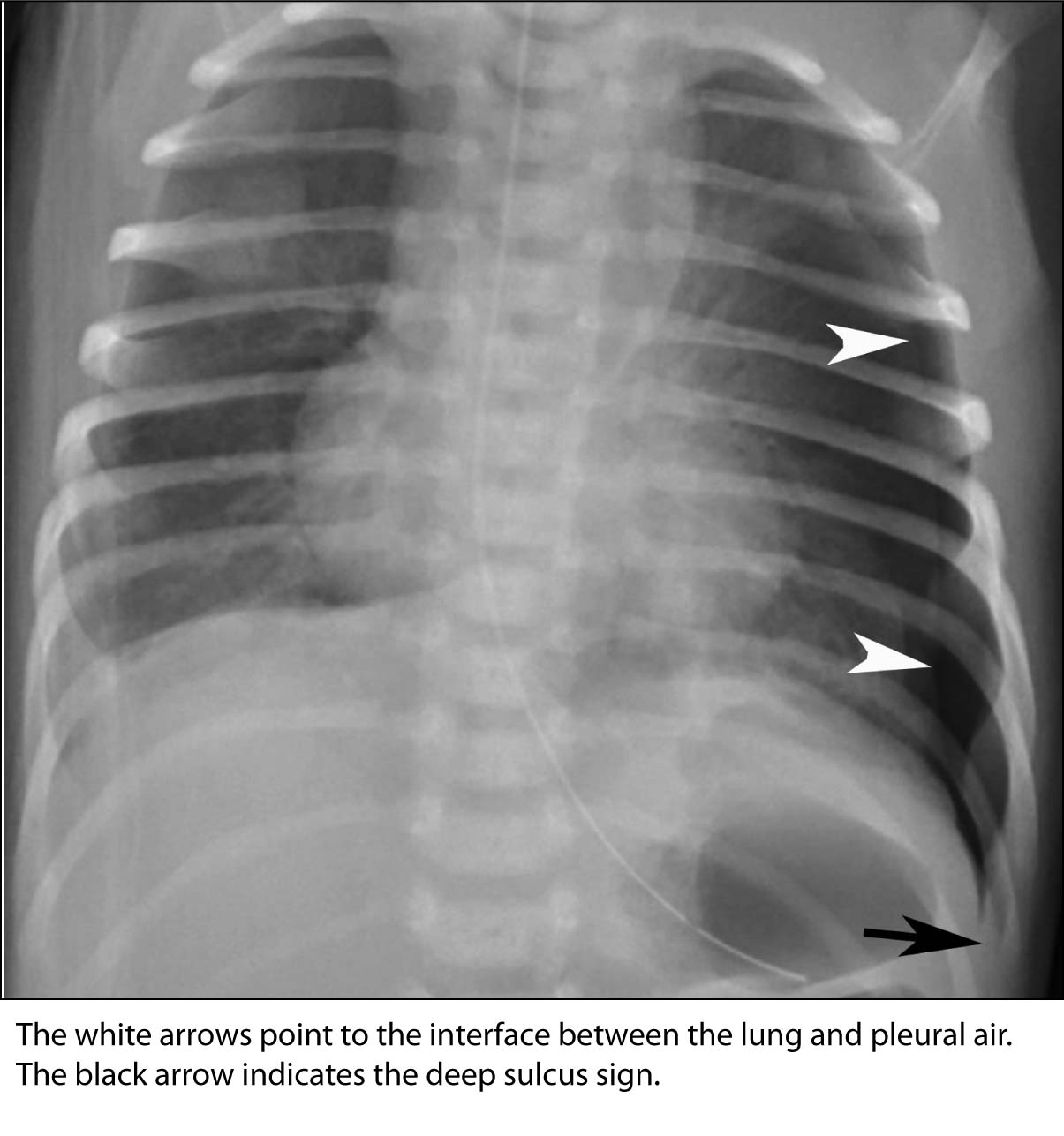
The white arrows point to the interface between the lung and pleural air. The black arrow indicates the deep sulcus sign.
FOREIGN BODY
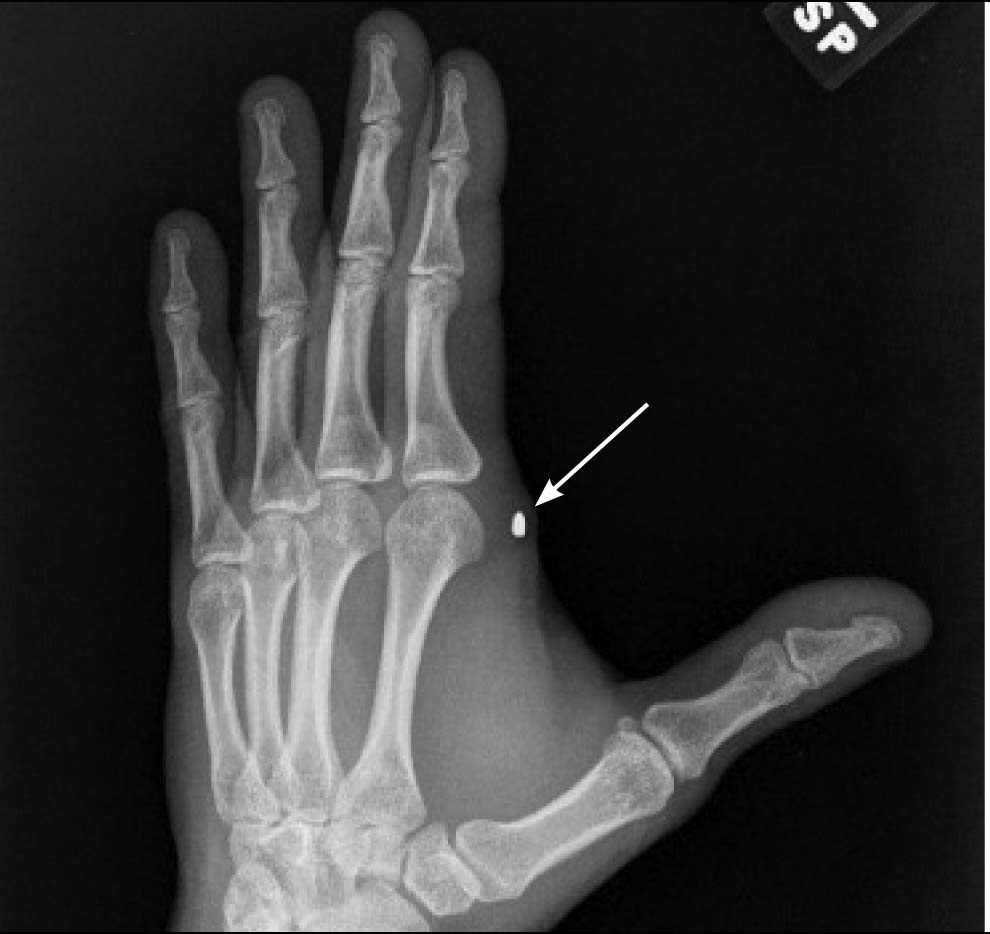
Missed foreign bodies are a frequent source of malpractice litigation, although the monetary settlements and judgments tend to be for small amounts. For the majority of these, an adequate history and physical exam can help eliminate the possibility of a foreign body, but if the possibility remains high, an imaging study is usually performed. Several studies have examined the imaging modality that is best used for foreign bodies. Plain radiographs remain the initial imaging modality for almost all types of foreign bodies, although the yield of this test is variable. There is a higher probability to visualize glass, gravel, and plastic on plain radiographs than organic materials such as wood.28 (See Figure 2.) Ultrasound is the imaging modality recommended for organic and non-radiopaque soft-tissue foreign bodies.
FIGURE 2. METALLIC FOREIGN BODY LATERAL TO DISTAL METACARPAL BONE
SKELETAL RADIOLOGY
In the practice of emergency medicine, it is important to learn how to read skeletal radiographs, as previously mentioned. It is especially important for EPs to develop and consistently use a personal approach to their interpretation to minimize errors. It is also important to know the standard and supplemental views for each series, properly determine if they have been done correctly, and acknowledge the role of each radiographic view. With this basic understanding, it will become easier to distinguish between normal and abnormal findings.29 Specifically, when looking at skeletal radiology, being able to identify a fracture is critical. Three radiographic signs of a fracture are the identification of the fracture line in two distinct and perpendicular views, changes in skeletal contour or alignment, and alterations in adjacent soft tissues.25,29 It is also important to know when it is necessary to order supplementary views. These types of views are usually oblique views and should be ordered if the EP suspects an injury that is not seen on the standard views, to better visualize a questionable abnormality, or to better delineate an injury that has already been identified.19
The next section will discuss the most commonly missed fractures and dislocations in the upper extremity, starting with the most distal aspect and moving proximally.
UPPER EXTREMITY
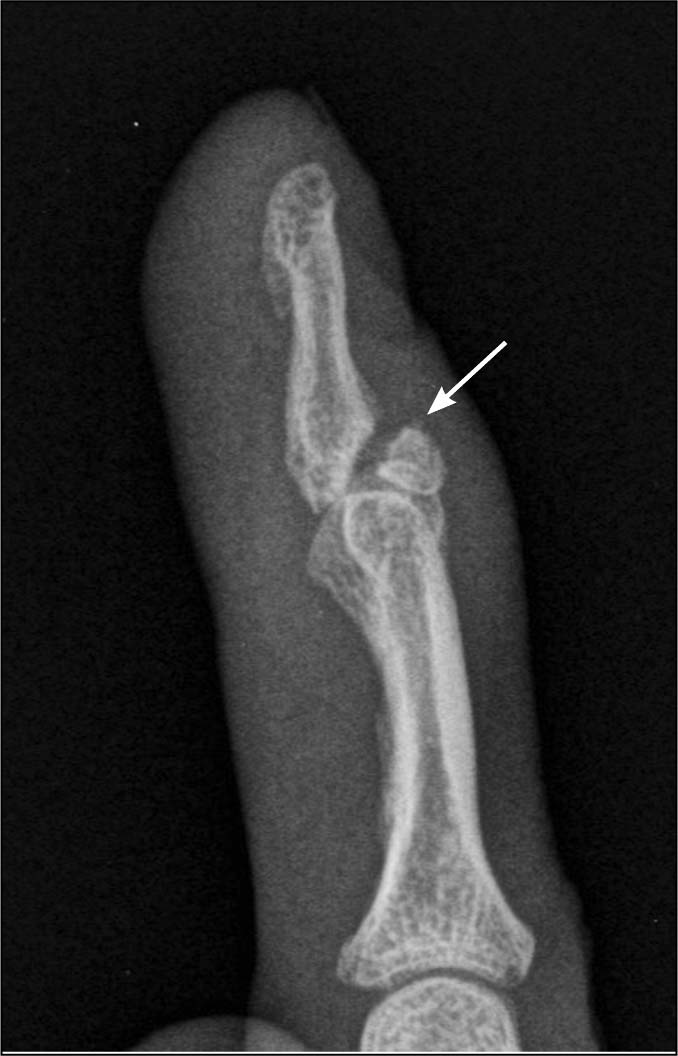
Hand. Tendon and ligament injuries are the most common in the hand, and include mallet finger, boutonniere deformity, and gamekeeper’s thumb. These can present as avulsion fractures in which a fraction of the distal phalanx is pulled away with the tendon. On radiographs, one can see that the bony fragment can be either nondisplaced or minimally displaced, making the fracture line difficult to visualize. It is important when suspecting these injuries to evaluate the cortex of each individual phalanx looking for irregularities and loss of alignment. (See Figures 3 and 4.)
FIGURE 3. GAMEKEEPER'S THUMB WITH ROTATED FRAGMENT
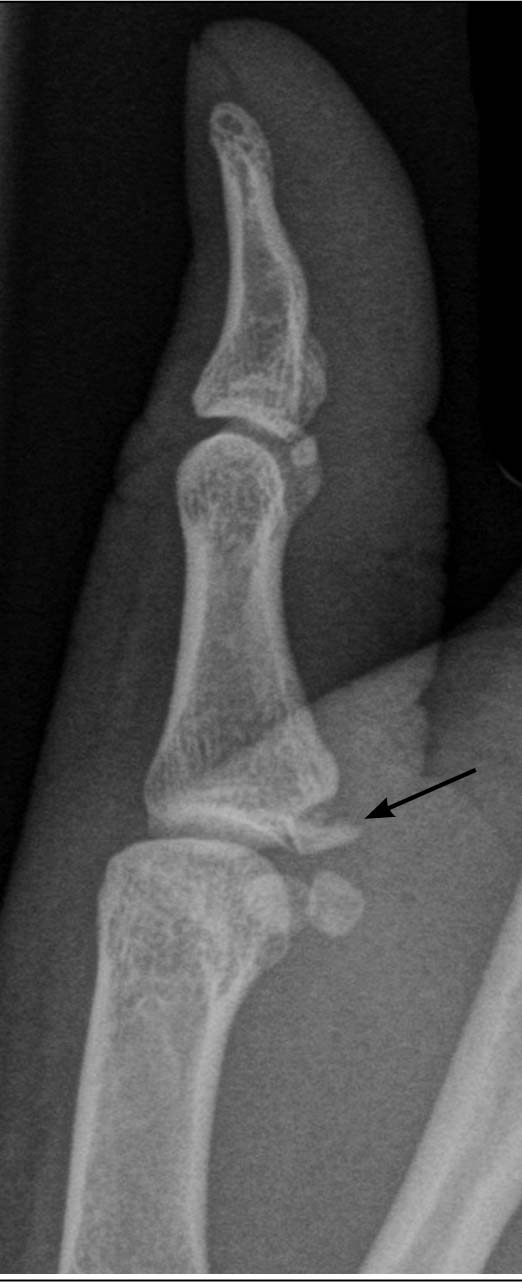
FIGURE 4. MALLET FINGER
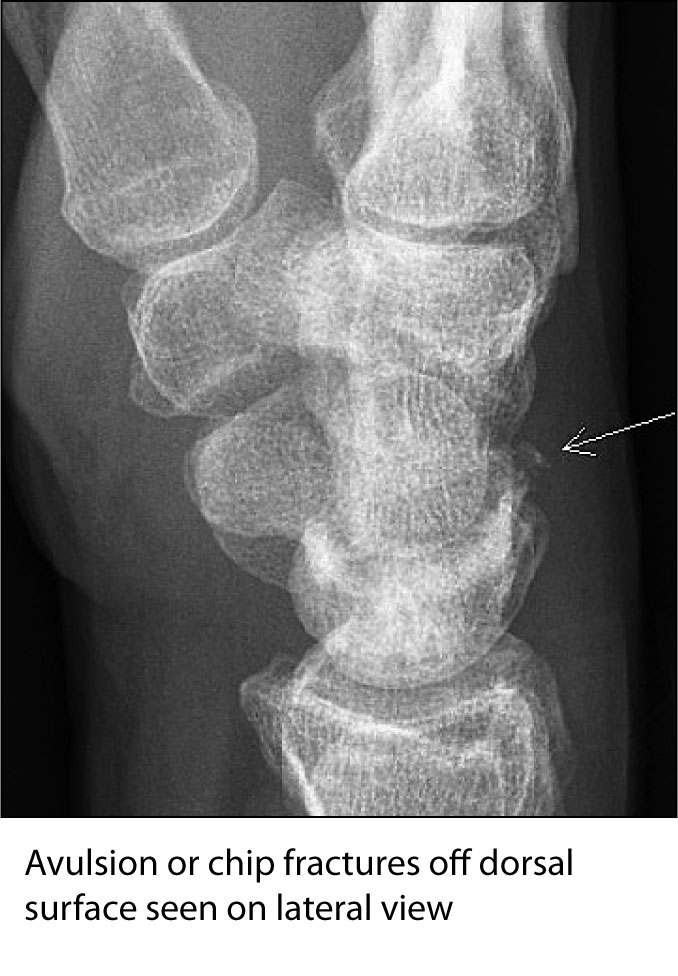
Wrist. Proceeding proximally, the wrist is a highly complex region with many bones and ligaments. As a result, it can be difficult at times to evaluate the wrist by radiograph, thus making it difficult to diagnose fractures and dislocations. The scaphoid and triquetrum are the most commonly injured carpal bones.30 Detection of carpal bone fractures is challenging, and scaphoid fractures are notorious for being radiographically occult (up to 18% of the time).31 (See Figure 5.) A specific scaphoid view can be helpful if the physical exam exhibits “snuffbox” tenderness. Despite negative X-ray findings and with the presence of “snuffbox” tenderness on physical exam, these particular patients should be properly immobilized and sent to an orthopedic or hand specialist for evaluation and re-imaging. Triquetral fractures, like phalanx injuries, can be categorized as an avulsion or “chip” fracture that involves the dorsal aspect of the triquetrum. They can be seen best on lateral views, although supplemental views can be helpful as well.30 (See Figure 6.)
FIGURE 5. SCAPHOID FRACTURE
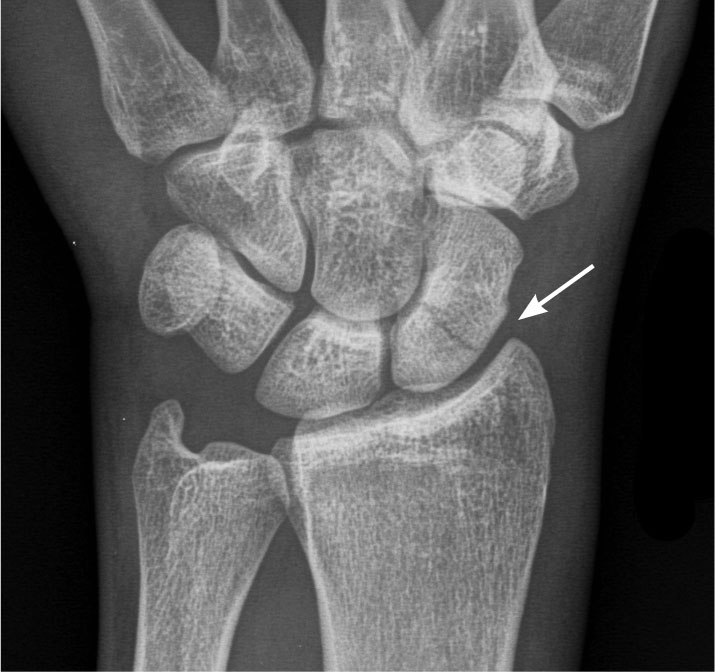
FIGURE 6. TRIQUETRAL FRACTURE
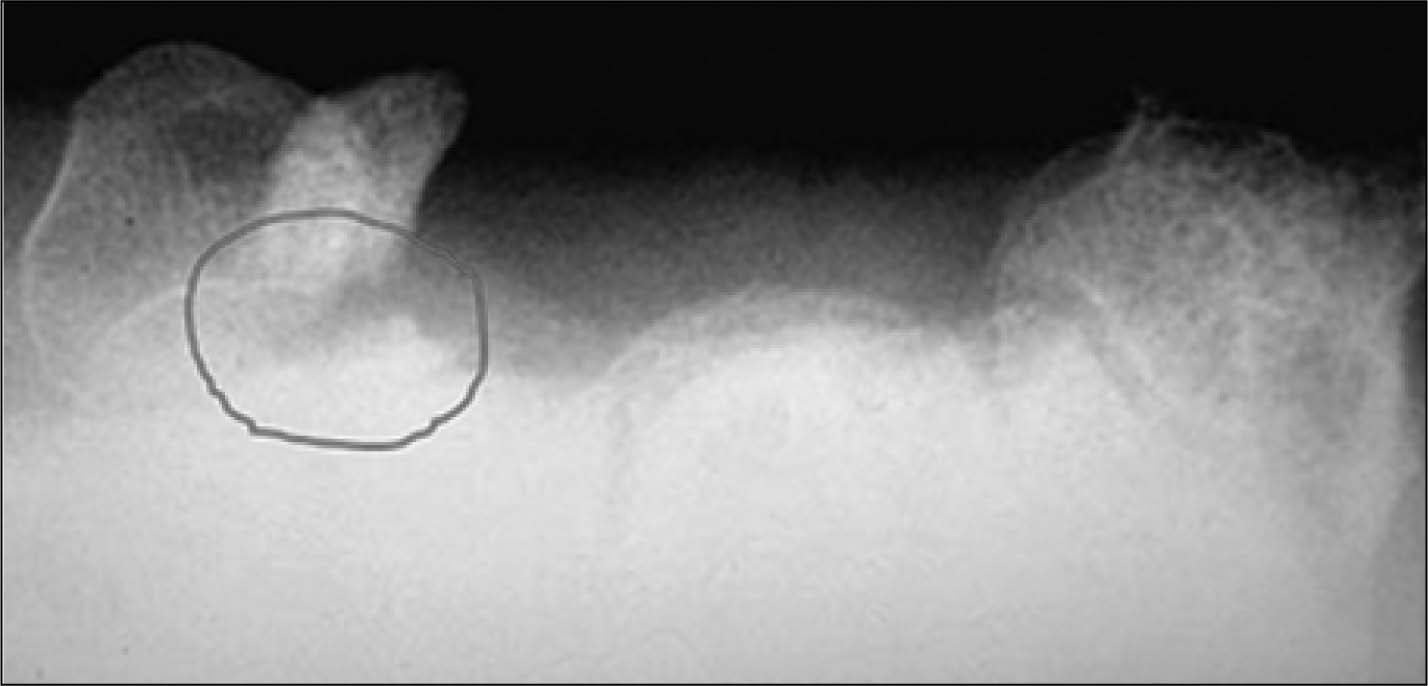
An uncommon but often initially missed injury in the wrist region is a fracture of the hook of the hamate. The typical mechanism of injury occurs when an individual swings a bat, club, or racket and strikes an unmoving object. The end of the bat, club, or racket handle is then forced into the hypothenar region and fractures the underlying hook of the hamate. Patients present with localized tenderness to the proximal hypothenar area and often have paresthesias in the ulnar nerve distribution. The ulnar nerve courses lateral to the hook of the hamate, and injury to that region will contuse the nerve. Standard hand and wrist radiographs will usually miss this injury. A carpal tunnel radiographic view is usually necessary to see this fracture. (See Figure 7.)
FIGURE 7. CARPAL TUNNEL RADIOGRAPH DEMONSTRATING A FRACTURE OF THE HOOK OF THE HAMATE (CIRCLE)
Hook of the hamate fractures should be immobilized immediately in an ulnar gutter splint that also immobilizes the little finger. This is because the flexor digiti minimi originates on the hook of the hamate and inserts on the proximal phalanx of the little finger. Even with prompt immobilization, nonunion rates of 50% are reported.
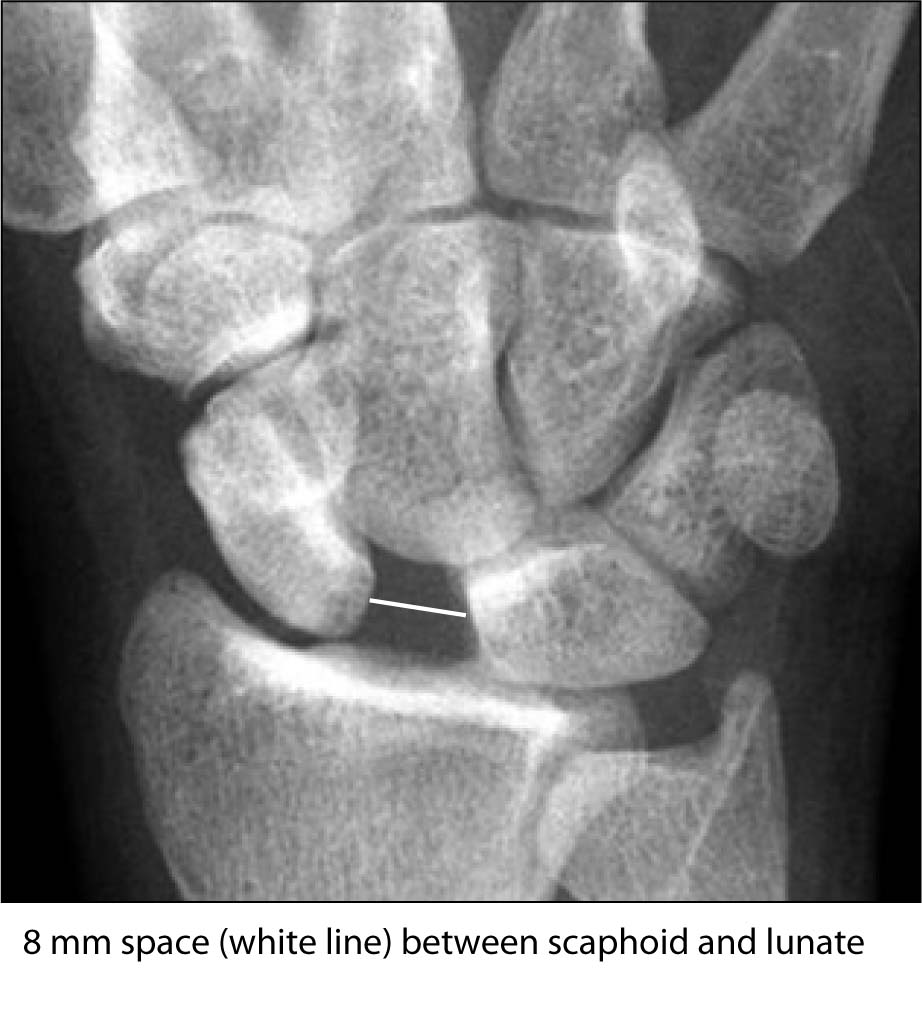
Another wrist injury that may be missed initially is a scapholunate dislocation, especially if the separation of the involved carpal bones is subtle. The scapholunate ligament connects the scaphoid and lunate bone. Complete disruption, such as what may occur from a fall on an outstretched arm and extended wrist, produces dorsal wrist pain and instability with movement. In the standard anterior-posterior (AP) wrist radiograph, the gap between the scaphoid and lunate should be measured at the midpoint of the adjacent parallel articular contours of the two bones. In adults, this interval is < 2 mm, and a gap of > 3 mm is indicative of scapholunate disruption. (See Figure 8.) Patients should be placed in a thumb spica splint and referred to a hand specialist. For a large gap and/or instability, surgical repair is necessary to prevent long-term complications.
FIGURE 8. SCAPHOLUNATE DISLOCATION
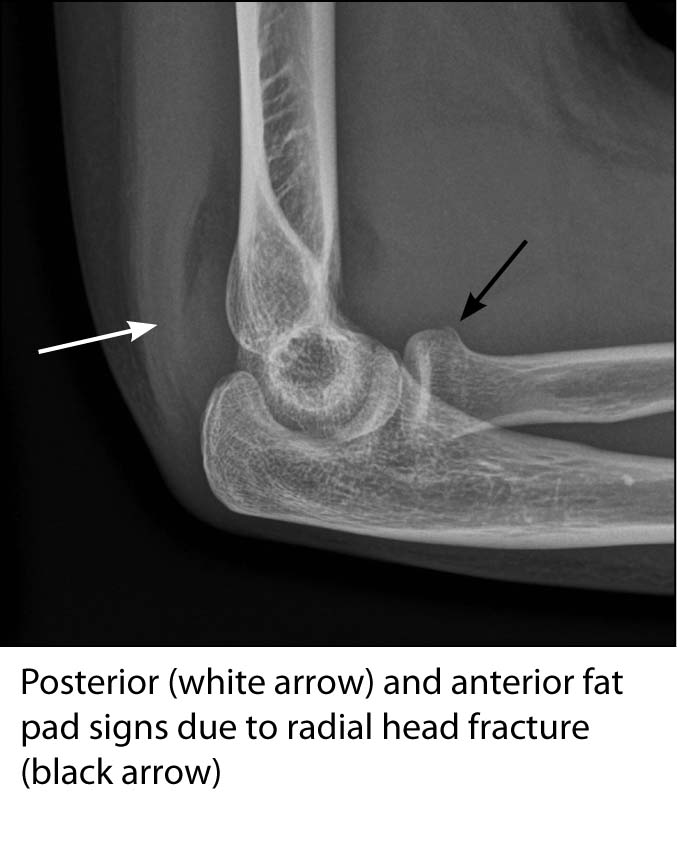
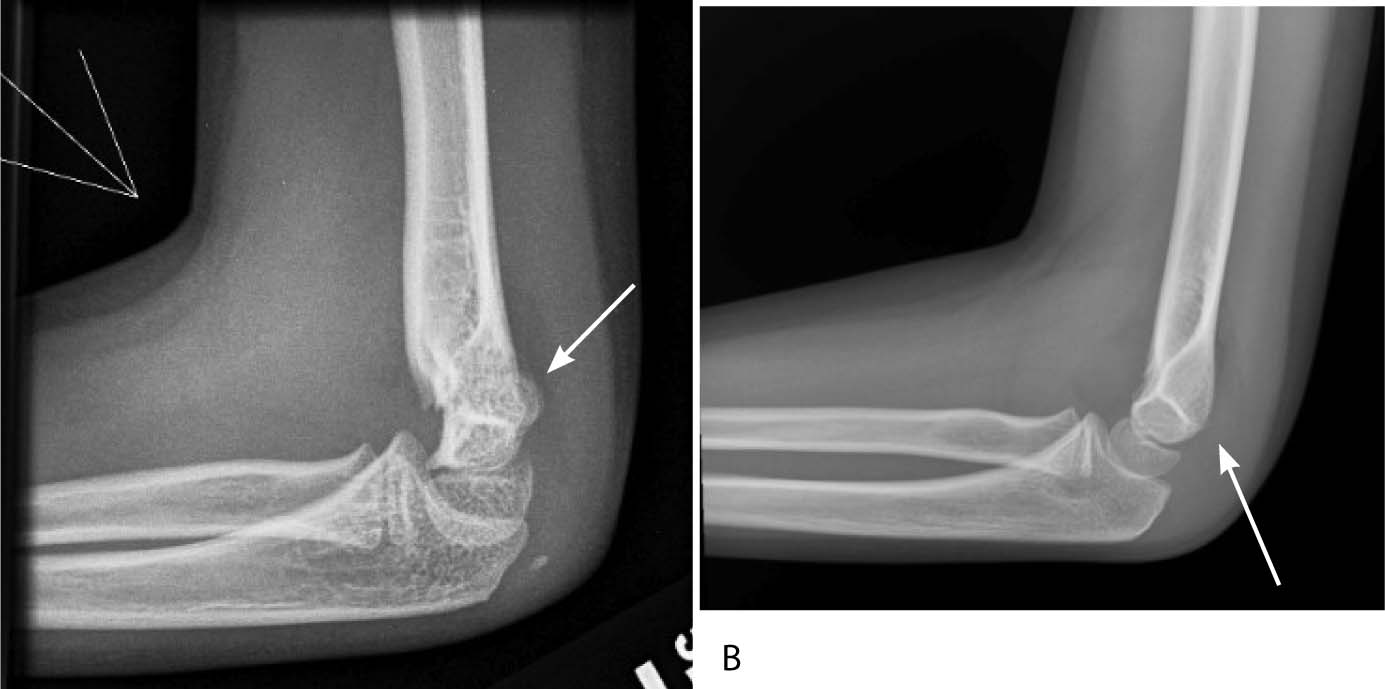
Elbow. In the elbow, one of the most commonly missed diagnoses in adults is a nondisplaced radial head fracture. Signs on physical exam are subtle, and patients mostly complain about mild pain with pronation and supination. Characteristically, elbow films need to be examined with close attention to the anterior and posterior fat pads. A posterior fat pad is said to be enhanced in a pathological state, and highly suspicious for an occult fracture, whereas the anterior fat pad sign can be normal.32 If an elbow X-ray displays a posterior fat pad sign, it is important to properly immobilize these particular patients and send them to orthopedics for evaluation. (See Figure 9.)
FIGURE 9. RADIAL HEAD FRACTURE
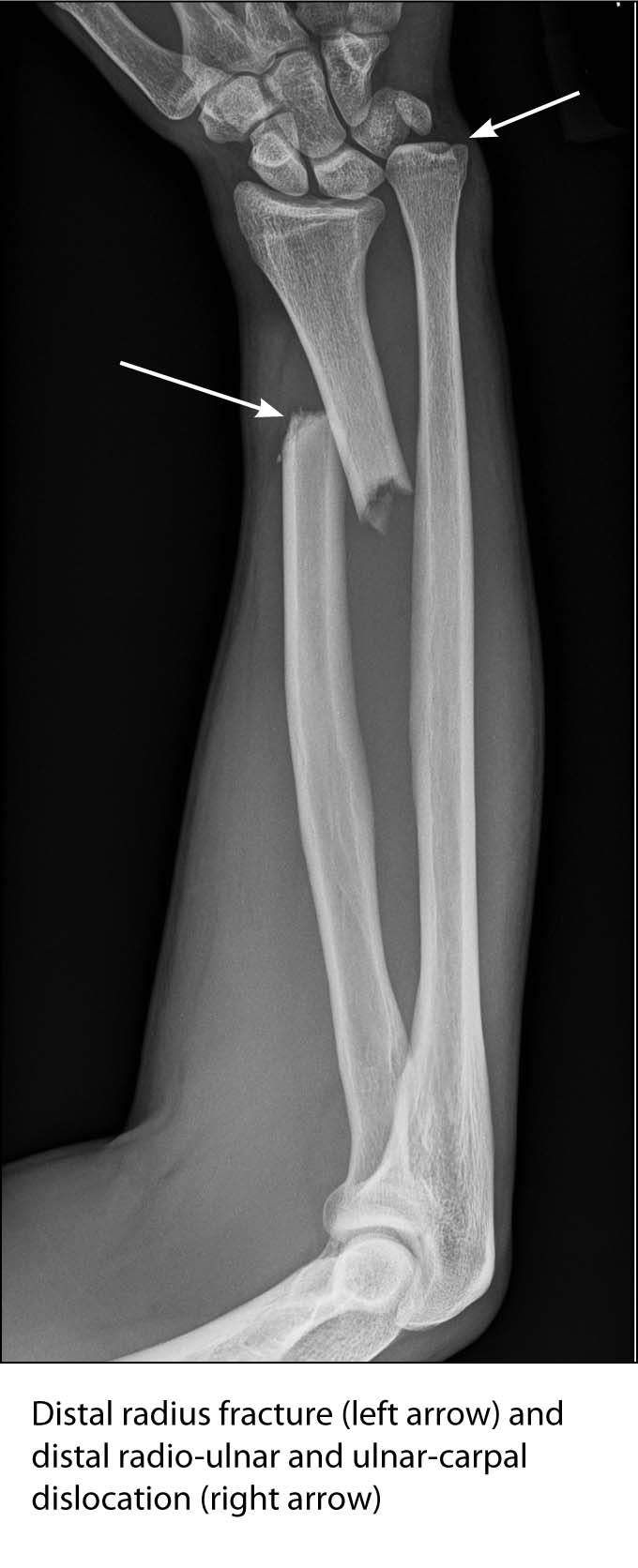
In addition, two fracture dislocations are more commonly seen than previously thought: the Monteggia and Galeazzi.33 The Monteggia fracture dislocation is characteristically defined as a fracture of the proximal third of the ulna with a concomitant dislocation of the radial head. In comparison, the Galeazzi fracture dislocation is known as the combination of a radius fracture, the middle and distal third of the bone, with a dislocation of the distal ulna at the distal radio-ulnar and ulnar-carpal joints. It is also known as the “reverse Monteggia” or the “fracture of necessity.” Both of these are known to occur from a fall onto an outstretched hand with the hand held in pronation or hyper-pronation.33 In both of these fracture dislocations, the fractures themselves are easily evident and the difficulty is observing for the dislocation. In the Monteggia, it is important to look at the radiocapitellar line (drawing a line down the shaft of the radius toward the elbow joint where it should intersect the capitellum). Alteration of this line will point toward a radial head dislocation or a capitellum displacement. In the Galeazzi, it is important to note the relationship of the ulna with the distal aspect of the radius. A normal distal radio-ulnar joint is usually about 1-2 mm; therefore, any distance greater than that can be classified as a subluxation.25,29 (See Figures 10 and 11.)
FIGURE 10. MONTEGGIA FRACTURE DISLOCATION
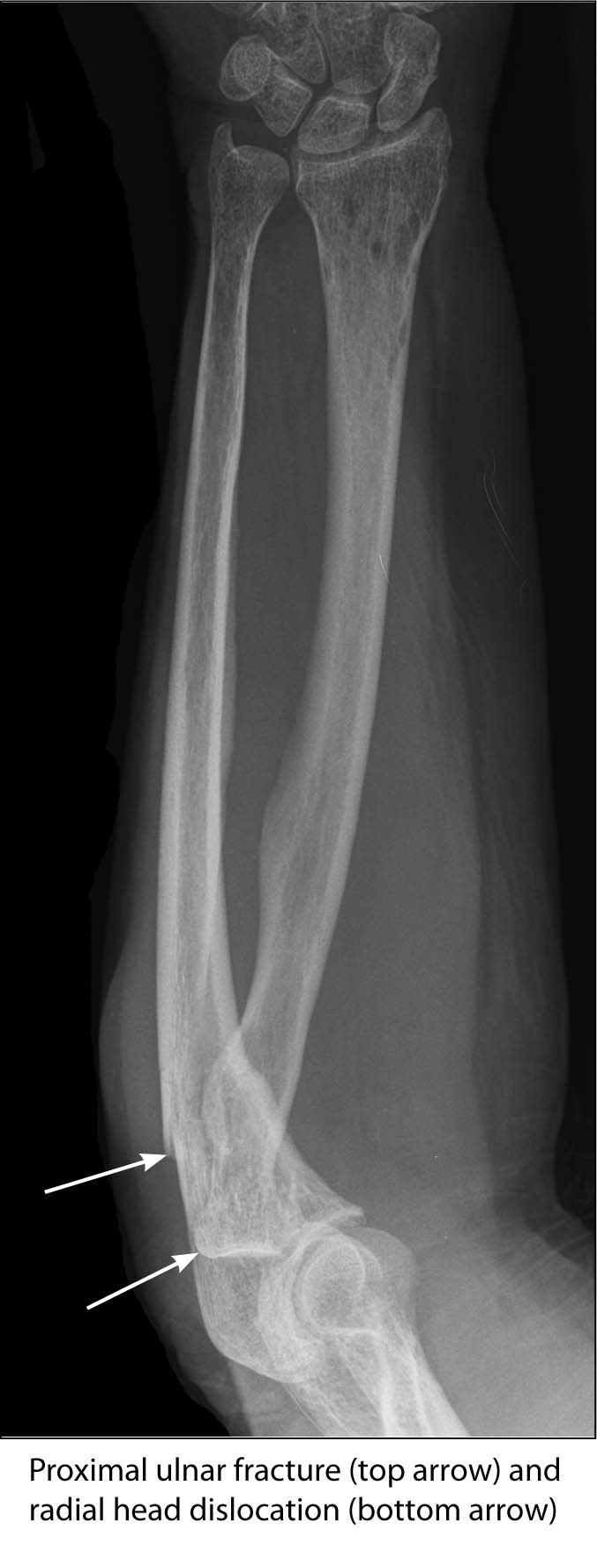
FIGURE 11. GALEAZZI FRACTURE DISLOCATION
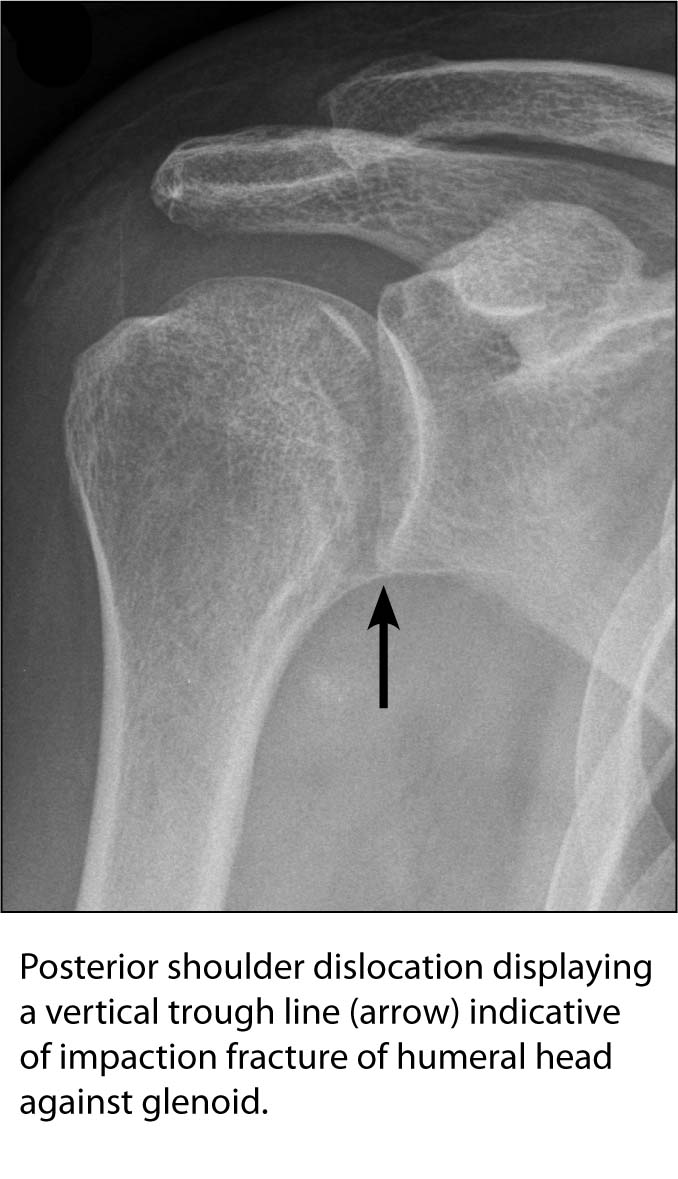
Shoulder. If the EP suspects a posterior shoulder dislocation in a patient due to the mechanism of injury, he or she should know that it would be difficult to visualize on plain films. On the AP view, look for the “light bulb on a stick” sign; the humeral head is fixed in internal rotation with the tuberosity rotated forward, resulting in a more rounded appearance to the humeral head. About two-thirds of posterior shoulder dislocations will have a rim sign, in which the distance between the medial border of the humeral head and anterior glenoid rim is > 6 mm. A minority of patients will display a “trough line,” which is a vertical line made by the impaction fracture of the humeral head against the glenoid. An axillary view is often necessary for diagnosis, while the scapular Y view is less accurate. Beware of proximal humeral neck fractures with a posterior dislocation as well.19,25,29 (See Figure 12.)
FIGURE 12. POSTERIOR SHOULDER DISLOCATION
LOWER EXTREMITY
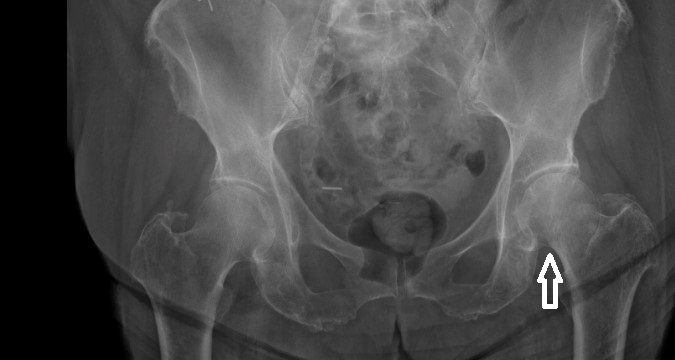
Hip. Approximately 15-20% of femoral neck fractures are nondisplaced and are notorious for having subtle radiographic signs.32 Some signs that may be helpful in the evaluation of hip radiographs for these types of fractures include: discontinuity of the normal smooth contour of the cortical bone; disruption of the normal trabecular architecture; transverse band of increased bone density where the fracture fragments are impacted; shortening of the femoral neck; and abnormal angle between the femoral neck and head.19,25,29 In a patient with a suspected hip fracture and negative radiographs, it is important to consider further imaging with either multislice computed tomography (CT) or magnetic resonance imaging (MRI). (See Figure 13.)
FIGURE 13. LEFT FEMORAL NECK FRACTURE
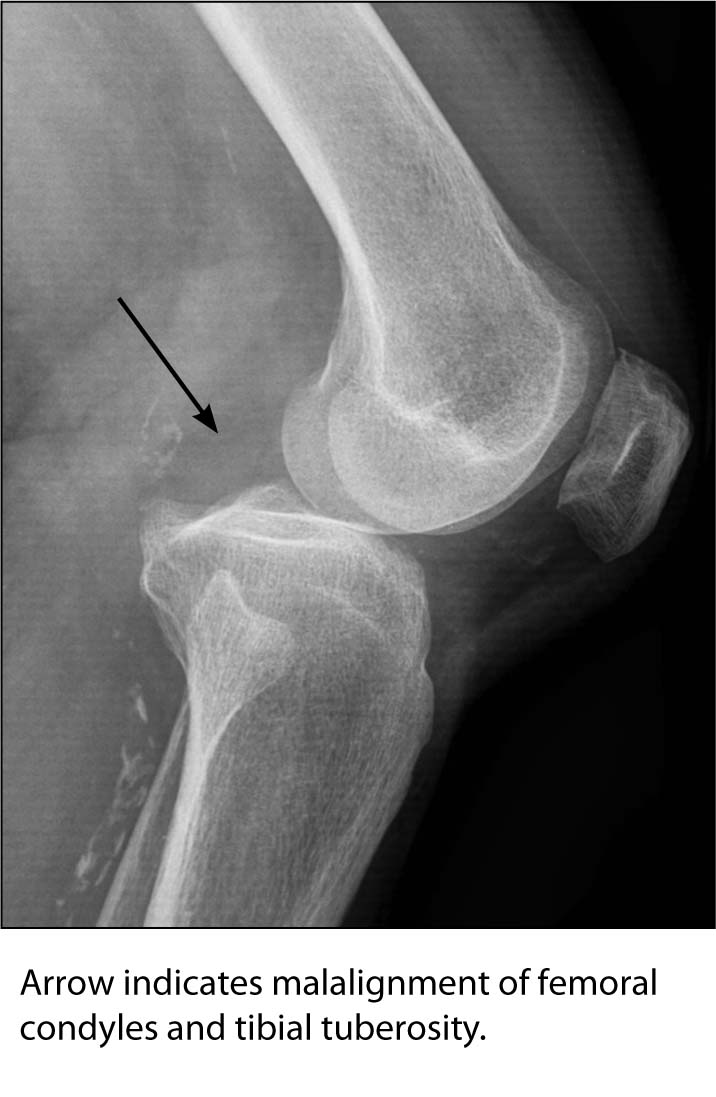
Knee. Knee dislocations most often occur when the foot is planted on the ground and a force is applied to the upper part of the body (i.e., motor vehicle collisions – dashboard injury, sports injury). Many knee dislocations reduce spontaneously or are reduced in the field prior to arrival in the ED. Therefore, it is important for emergency medicine providers to focus on the neurovascular aspect of this injury, since a well-known complication of a knee dislocation is a popliteal artery injury. Patients with these types of injuries usually arrive with a severe amount of swelling at the joint accompanied by pain, which can make completing the physical exam difficult, especially if the patient is not able to describe the event. Consequently, it is important to identify key findings in plain radiographs that can point the clinician toward evidence that a knee dislocation has occurred followed by spontaneous reduction, therefore prompting the provider to look for its complication. These key finding are asymmetric or irregular joint spaces, avulsion fractures of the lateral tibial condyle (Segond sign), avulsion fracture of the fibular head (arcuate sign), misalignment of the femoral condyles in respect to the tibial tuberosities, and osteochondral defects.34-36 (See Figure 14.)
FIGURE 14. POSTERIOR KNEE DISLOCATION
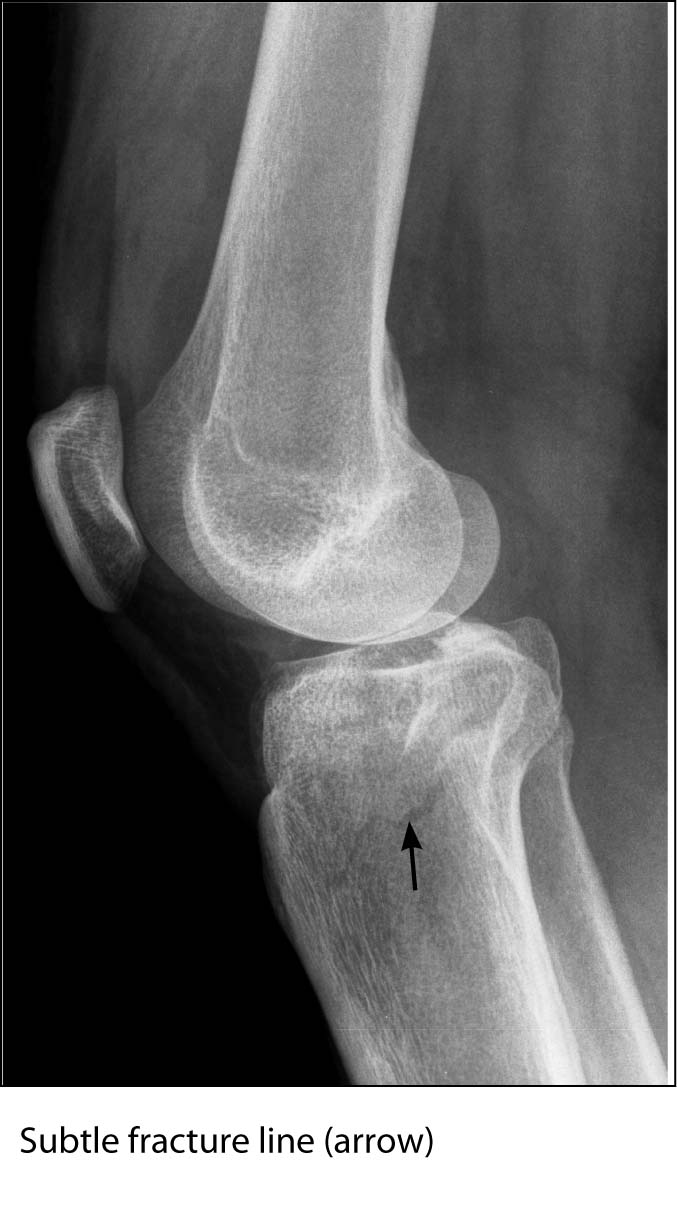
Another commonly missed fracture within the knee joint is the tibial plateau fracture. Characteristic features of these types of fractures include high-impact injuries, intra-articular involvement of the fracture, and lipoarthrosis. Patients with this type of fracture can present with knee effusion, decreased flexion and extension of the knee, and bony tenderness. About 85% of these fractures involve the lateral aspect of the tibia. Two main reasons these fractures are difficult to visualize can be due to the fracture lying in the oblique plane and the tibial plateau surface slopes inferiorly from anterior to posterior. Both of these finding are difficult to see because the fracture does not lie parallel to the X-ray beam. Cortical irregularity and trabecular impaction of the tibia are signs to look for, and it may be necessary to obtain oblique views to corroborate tibial plateau fractures. It is also important to be familiar with the normal anatomical radiographic findings in order to detect abnormal findings.19,25,29 (See Figures 15A and B.)
FIGURE 15A. LATERAL TIBIAL PLATEAU FRACTURE (AP VIEW PARTIALLY ROTATED)
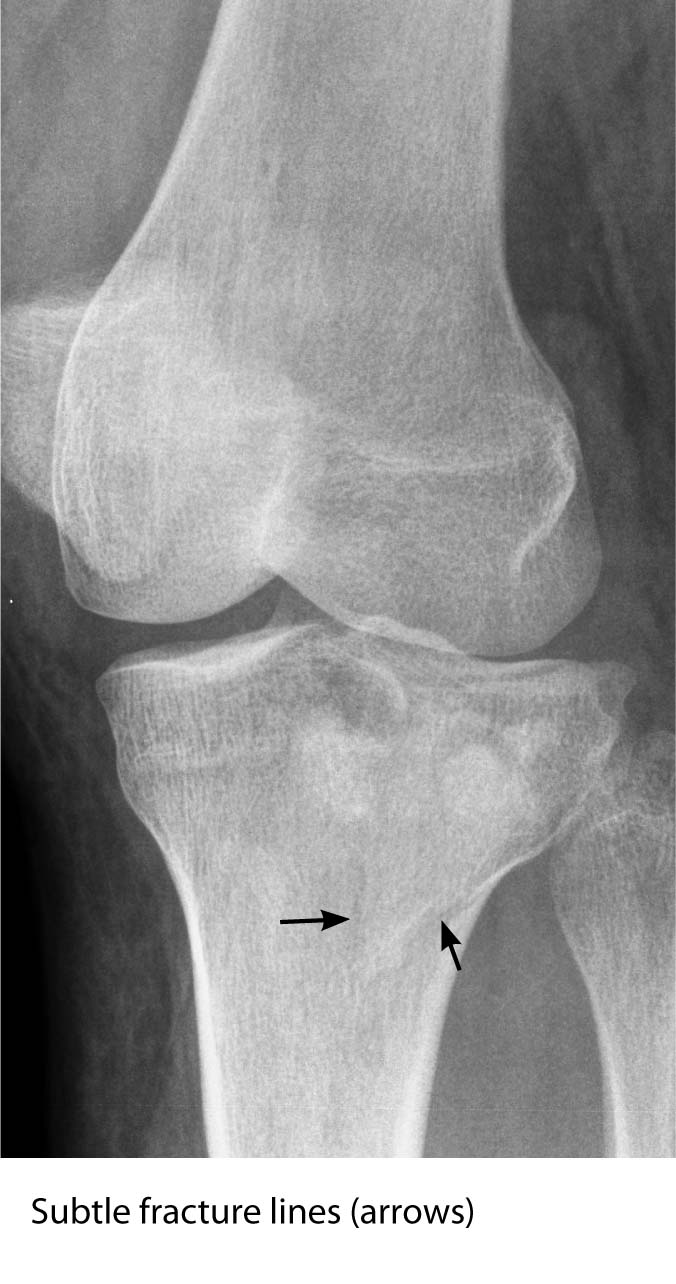
FIGURE 15B. LATERAL TIBIAL PLATEAU FRACTURE(LATERAL VIEW)
Ankle and Foot. One study found that 51.4% of missed fractures involved the ankle and foot.37 At the ankle, EPs need to be vigilant for proximal fibular fractures in patients who may exhibit medial malleolus tenderness. Patients with a Maisonneuve fracture usually present after a pronation with external rotation injury and have radiographic findings of a distal tibiofibular syndesmotic disruption with a proximal fibular fracture.38 Lisfranc injuries are characterized as a tarso-metatarsal fracture-dislocation and can be subtle or occult, especially on non-weight bearing radiographs. It is important to look for misalignment of the metatarsal bases and the cuneiform with or without a concomitant fracture of the base of the second metatarsal, or “fleck” sign. If this type of injury is suspected, it might be prudent to order weight-bearing films to visualize the instability.19,25,29,39,40 (See Figures 16 and 17.)
FIGURE 16. MAISONNEUVE FRACTURE
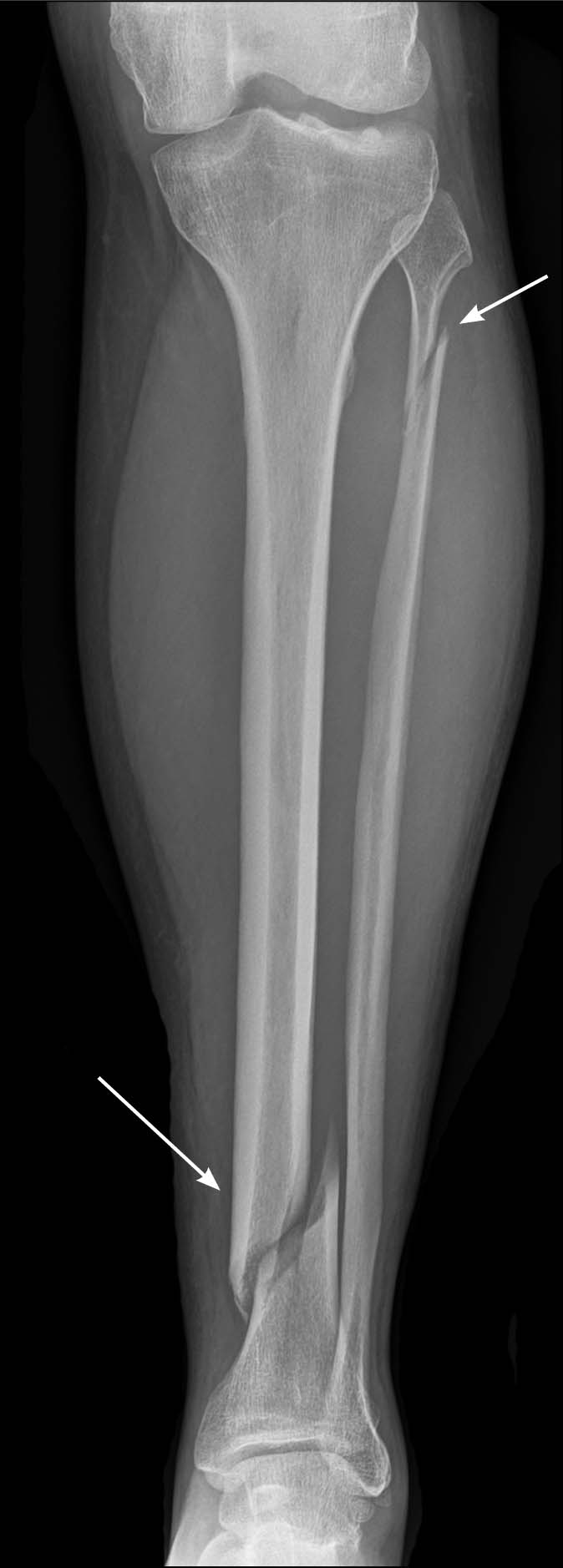
FIGURE 17. LISFRANC FRACTURE DISLOCATION
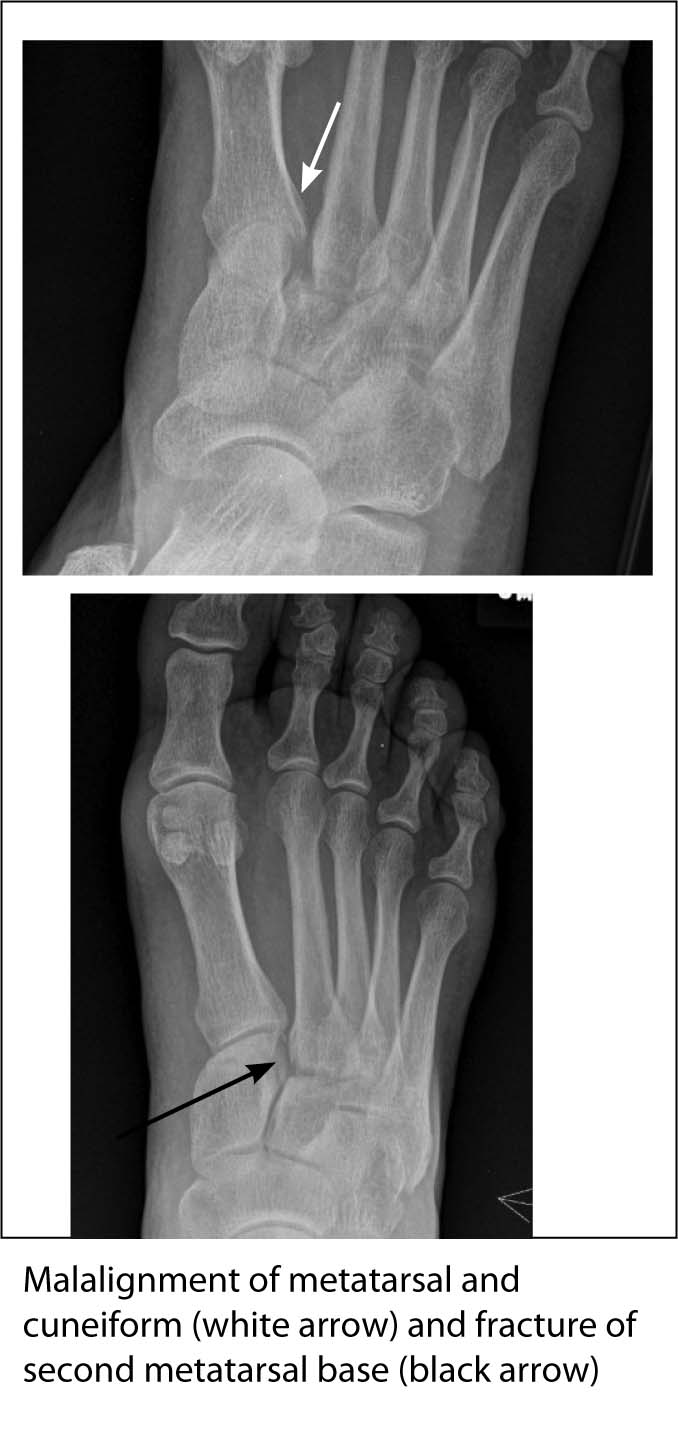
There are specific injuries that are only seen in the pediatric population. A study on the diagnostic errors made by radiology trainees interpreting radiographs in a pediatric ED found that 69% involved the diagnosis of fractures and/or dislocations. The majority of these were buckle (torus) fractures (47% of the radius) and Salter Harris II fractures. Both of these can be difficult to distinguish because X-rays can show signs of it being a normal variant.41 A buckle fracture occurs with axial loading injuries. An outward buckling of the cortex can be seen, and it is important to look at the contour of the bone, especially at the metaphysis, to find these fractures. The proximal radius is a common site for missed buckle fractures.42 (See Figure 18.) Salter Harris II fractures are the most common type of physeal injuries (75%). The line of fracture runs through the physis and then out through a segment of metaphyseal bone. This segment of bone is commonly referred to as the Thurston-Holland sign.43 (See Figure 19.)
FIGURE 18. TORUS OR BUCKLE FRACTURE OF DISTAL RADIUS
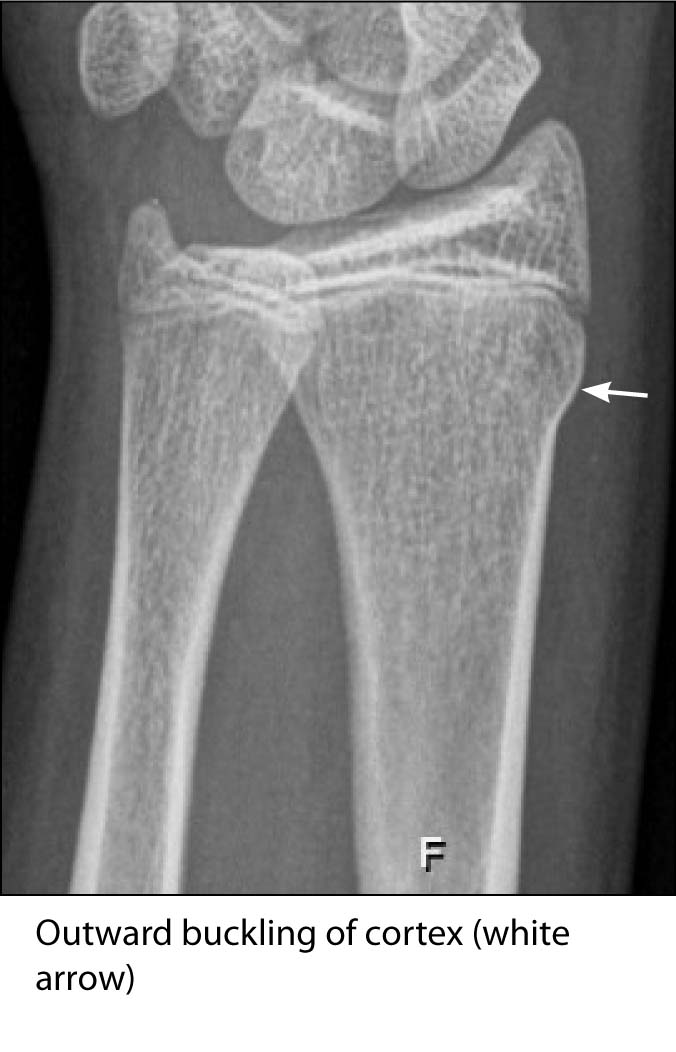
FIGURE 19. SALTER HARRIS II FRACTURE OF THE DISTAL FEMUR
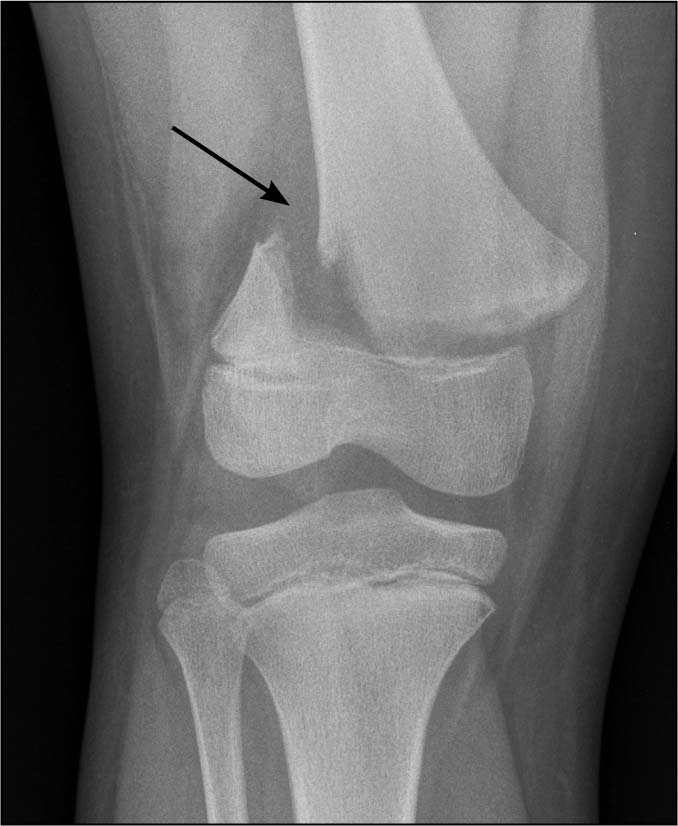
Regarding pediatric fractures, it is worth mentioning the supracondylar humerus fracture. These fractures are the most common upper extremity fractures seen around the elbow. They usually occur after falls on an outstretched hand and range from mild swelling (mild nondisplaced fracture) to severe deformity with neurovascular complications. On radiographic exam of these pediatric elbows, it is important to look for a posterior fat pad sign, and examine the radiocapitellar line (both discussed earlier), as well as the anterior humeral line. The anterior humeral line is drawn down the anterior aspect of the humeral cortex toward the elbow until it intersects the capitellum. This line should intersect the middle third of the capitellum for it to be normal, whereas if an injury has occurred it is usually displaced so that the anterior humeral line lies behind the capitellum.44 (See Figure 20.)
FIGURE 20. SUPRACONDYLAR FRACTURE: A. DISPLACED. B. NONDISPLACED
CONCLUSION
This discussion of some of the most commonly missed findings on radiographs reiterates the importance of keeping a close eye when interpreting films. Knowing the most commonly missed findings and strategies to eliminate these types of errors can make you a better emergency physician. (See Table 3.) You may now see radiographs in a different light.
TABLE 3. TIPS FOR INTERPRETING X-RAYS19,25,29
- Verify name, correct side (right/left), and site (ankle, wrist etc.).
- Develop your personal logical method for reviewing radiographs (i.e., systematic vs. targeted) and consistently use it.
- Perform a careful history and physical exam and generate a differential diagnosis.
- Look at the entire image (“A,B,Cs” ); don’t focus on just where the pain is!
- Make sure to obtain all the radiographic views needed for the patient’s complaint. Order supplemental views if necessary.
- Intelligently apply the radiographic information to patient care.
- If still in doubt, consult another physician or radiologist.
Or
- Treat conservatively by splinting the extremity and referring to an orthopedic, sports medicine, or hand specialist for follow-up X-rays.
Acknowledgements: Images courtesy of Laura Bancroft, MD, Florida Hospital Radiology Program Director, Orlando, and J.S. Stapczynski, MD.
REFERENCES
- Paakkala T. Training of general practitioners in interpreting chest radiographs. Med Educ 1988;22:449-453.
- Bergus GR, Franken EA, Koch TJ, et al. Radiologic interpretation by family physicians in an office practice setting. J Fam Pract 1995;41:352-356.
- Fastow JS. Medico‐legal risks: Identification and reduction. In: American College of Emergency Physicians: Comprehensive Guide to Effective Practice Management. Dallas: ACEP, 1986.
- Karcz A, Korn R, Burke MC, et al. Malpractice claims against emergency physicians in Massachusetts: 1975‐1993. Am J Emerg Med 1996;14:341‐345.
- Karcz A, Holbrook J, Burke MC, et al. Massachusetts Emergency Medicine Closed Malpractice Claims: 1988-1990. Ann Emerg Med 1993;22:553-559.
- Guly HR. Missed diagnoses in an accident & emergency department. Injury 1984;15:403-406.
- Tulloh BR. Diagnostic accuracy in head-injured patients: An emergency department audit. Injury 1994;25:231-234.
- Robinson PJ. Radiology’s Achilles’ heel: Error and variation in the interpretation of the Röntgen image. Br J Radiol 1997;70:1085-1098.
- Schenkel S. Promoting patient safety and preventing medical error in emergency departments. Acad Emerg Med 2000;7:1204-1222.
- Lufkin KC, Smith SW, Matticks CA, et al. Radiologists’ review of radiographs interpreted confidently by emergency physicians infrequently leads to changes in patient management. Ann Emerg Med 1998;31:202-207.
- Robinson PJ, Wilson D, Coral A, et al. Variation between experienced observers in the interpretation of accident and emergency radiographs. Br J Radiol 1999;72:323-330.
- Scott WW Jr, Bluemke DA, Mysko WK, et al. Interpretation of emergency department radiographs by radiologists and emergency medicine physicians: Teleradiology workstation versus radiograph teadings. Radiology 1995;195:223-229.
- Hallas P, Ellingsen T. Errors in fracture diagnoses in the emergency department-characteristics of patients and diurnal variation. BMC Emergency Medicine 2006,6:4.
- Franken EA, Berbaum KS, Smith WL, et al. Teleradiology for rural hospitals: Analysis of a field study. J Telemed Telecare 1995;1:202-208.
- Franken EA, Berbaum KS, Brandser EA, et al. Pediatric radiology at a rural hospital: Value of teleradiology and subspecialty consultation. AJR Am J Roentgenol 1997;168:1349-1352.
- Franken EA, Harkens KL, Berbaum KS. Teleradiology consultation for a rural hospital: Patterns of use. Acad Radiol 1997;4:492-496.
- Lambrecht CJ. Emergency physicians’ roles in a clinical telemedicine network. Ann Emerg Med 1997;30:670-674.
- Preston CA, Marr JJ 3rd, Amaraneni KK, et al. Reduction of “callbacks” to the ED due to discrepancies in plain radiograph interpretation. Am J Emerg Med 1998;6:160-162.
- Schwartz D T. Ten most commonly missed radiographic findings in the ED, in ACEP Scientific Assembly, Boston Convention and Exhibition Center, 2009.
- Kachalia A, Gandhi TK, Puopolo AL, et al. Missed and delayed diagnoses in the emergency department: A study of closed malpractice claims from 4 liability carriers. Ann Emerg Med 2007;49:196‐205.
- Guly HR. Diagnostic errors in an accident and emergency department. Emerg Med J 2001;18:263‐269.
- Wei CJ, Tsai WC, Tiu CM, et al. Systematic analysis of missed extremity fractures in emergency radiology. Acta Radiol 2006;47:710‐717.
- Freed HA, Shields NN. Most frequently overlooked radiographically apparent fractures in a teaching hospital emergency department. Ann Emerg Med 1984;13:900-904.
- Petinaux B, Bhat R, Boniface K, et al. Accuracy of radiographic reading in the emergency department. Am J Emerg Med 2011;29:18-25.
- Schwartz DT. Emergency Radiology: Case Studies. McGraw‐Hill, 2008.
- Ropp A, Waite S, Reede D, et al. Did I miss that: Subtle and commonly missed finding on chest radiographs. Curr Probl Diag Rad 2015;44:277-289.
- Maughan B, Asselin N, Carey JL, et al. False–negative chest radiographs in the emergency department diagnosis of pneumonia. R I Med J 2014;8:20-23.
- Russel RC, Williamson DA, Sullivan JW, et al. Detection of foreign bodies in the hand. J Hand Surg Am 1991;16:2.
- Schwartz DT, Reisdorff EJ. Emergency Radiology. McGraw‐Hill, 2000.
- Goldfarb CA, Yin Y, Gilula LA, et al. Wrist fractures: What the clinician wants to know. Radiology 2001;219:11-28.
- Welling JA, Jacobson JA, Jamadar DA, et al. MDCT and radiography of wrist fractures: Radiographic sensitivity and fracture patterns. AJR Am J Roentgenol 2008;190:10-16.
- Marx JA, Hockberger RS, Walls RM, et al., eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. Philadelphia, PA: Mosby/Elsevier; 2014.
- Perron AD, Brady WJ, Miller MD. Orthopedic pitfalls in the ED: Galeazzi and Monteggia fracture dislocation. Am J Emerg Med 2001;19:225-228.
- Henrichs AA. Review of knee dislocations. J Athletic Training 2004;39:365-369.
- Roberts DM, Stallard TC. Emergency department evaluation and treatment of knee and leg injuries. Emerg Med Clin 2000;18:67-84.
- Crimmins JT, Wissman RD. The arcuate sign: A marker of potential knee dislocation? A report of two cases. Radiology Case Reports 2008;3(2).
- Er E, Kara PH, Oyar O, et al. Overlooked extremity fractures in the emergency department. Ulus Travma Acil Cerrahi Derg 2013;19:25-28.
- Levy BA, Vogt KJ, Herrera DA, et al. Maisonneuve fracture equivalent with proximal tibiofibular dislocation: A case report and literature review. J Bone Joint Surg Am 2006;88:1111-1116.
- van Rijn J, Dorleijn DM, Boetes B, et al. Missing the Lisfranc fracture: A case report and review of the literature. J Foot Ankle Surg 2012;51:270-274.
- Sherief TI, Mucci B, Greiss M. Lisfranc injury: How frequently does it get missed? And how can we improve? Injury 2007;38:856-860.
- Halsted MJ, Kumar H, Paquin JJ, et al. Diagnostic error by radiology residents in an emergency setting. Pediatr Radiol 2004;34:331-336.
- Jadhav SP, Swischuk LE. Commonly missed subtle skeletal injuries in children. Emerg Radiol 2008;15:391‐398.
- Perron AD, Miller MD, Brady WJ. Orthopedic pitfalls in the ED: Pediatric growth plate injuries. Am J Emerg Med 2002;20;50‐54.
- Wu MJ, Perron AD, Miller MD, et al. Orthopedic pitfalls in the emergency department: Pediatric supracondylar humerus fractures. Am J Emerg Med 2002;20:544-550.
The practice of medicine involves judgment, the weighing of possibilities and probabilities. Even more so when interpreting radiographs.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
