Chiropractic for Ankle Sprains
By David Kiefer, MD
Clinical Assistant Professor, Department of Family Medicine, University of Wisconsin; Clinical Assistant Professor, Arizona Center for Integrative Medicine, University of Arizona, Tucson
Dr. Kiefer reports he is a consultant for WebMD.
SYNOPSIS: Ankle joint chiropractic manipulation as adjunctive therapy to typical rehabilitation improves symptoms of chronic ankle instability from repeated sprains.
SOURCE: Lubbe D, et al. Manipulative therapy and rehabilitation for recurrent ankle sprain with functional instability: A short-term, assessor-blind, parallel-group randomized trial. J Manipulative Physiol Ther 2015;38:22-34. doi: 10.1016/j.jmpt.2014.10.001.
SUMMARY POINTS
- This is a randomized, parallel group (no placebo), 5-week clinical trial in 33 patients with chronic ankle joint instability.
- Ankle manipulation administered by chiropractors relieved pain to a greater degree than rehabilitation alone.
- There was no statistically significant improvement in ankle function as per a standardized test.
Ankle sprains, usually related to an inversion mechanism, are a common injury. The authors of this study found that 40% of such injuries progress to chronic instability and/or pain, a major justification for the search for techniques to strengthen and improve functionality in the ankle in the long term.
Damage to the anterior talofibular ligament, if not all three of the lateral collateral ligaments, as well as loss of dorsiflexion, and, as the authors detailed, “loss of the posterior glide of the talus” and proprioception, all contribute to instability with activity that may or may not be detectable during a physical examination. Traditional treatments include proprioceptive exercises and muscle strength training, both of which have documentation in the medical literature for their utility. The authors wanted to expand on this research by studying joint manipulation as an adjunctive therapy to standard rehabilitation techniques.
The study included patients with “recurrent ankle sprain with functional instability,” a modification of the original inclusion criterion of “chronic ankle instability (CAI)”; the researchers found it difficult to meet the strict definition of CAI, so they broadened their search for participants. Participants had to have had a history of inversion ankle injuries (but none within the last 6 weeks) and mortise joint tenderness and/or pain. Thirty-nine patients met these eligibility criteria, and were then screened for inclusion in the study (see Table 1); five patients did not meet the criteria for inclusion and one declined to participate, leaving 33 patients for randomization. Randomization was to either standard care (18 people), or standard care plus manipulation (15 people) for 5 weeks. Standard care rehabilitation was done daily and included balance board and coordination training exercises, and strength training, the specifics of which were detailed in the article (in case the reader would like to duplicate in clinical practice).
TABLE 1: INCLUSION AND EXCLUSION CRITERIA |
|
|
Inclusion Criteria |
Exclusion Criteria |
|
|
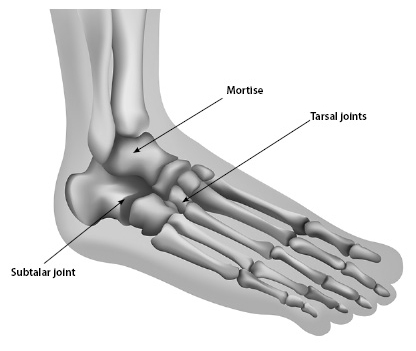
An instructor reviewed the protocol with the participant at the beginning of the study, and then the study participant completed daily exercise at home, with printed instructions to reference if necessary. The manipulation group completed the same rehabilitation protocol as described above while also receiving six manipulation treatments over the course of the 5 weeks from an “experienced chiropractic clinician.” The manipulation type was high-velocity-low-amplitude thrust-type and involved the mortise, subtalar, and/or tarsal joints. (See Figure 1.) There was some variability of the joint manipulated in each participant depending on the findings of the chiropractor with respect to joint restrictions. The researchers decided to have different practitioners examine the research participants for the presence of joint restrictions than the clinicians who administered the treatments. Separate providers, essentially a “blind assessor” and a treating clinician, were deemed necessary to avoid examination bias.
FIGURE 1: ANKLE JOINTS
|
The primary outcome was pain as determined by the Visual Analog Scale (VAS; 0-100 mm) and the Foot and Ankle Disability Index (FADI; 26 items, 4 for pain, and 22 for activity-related items; 104 total points, 0-4 points per item). A higher score on the FADI indicates better ankle function, whereas a higher VAS score indicates more pain. A secondary outcome was joint motion palpation as determined by the “experienced chiropractic clinician.” Data were analyzed using an intention-to-treat analysis.
For the 33 participants, the average age was 26, the average number of days with symptoms ranged from 136-484 (average 270), and participants had an average of five prior ankle sprains. During the study, participants completed an average of 30 rehabilitation sessions (out of 35 possible). The results of the VAS and FADI testing are shown in Table 2. Only the VAS showed statistically significant differences between the manipulation-rehabilitation and rehabilitation groups after the 5-week study period. Of note, the FADI and the VAS improved from baseline in both groups. No adverse events were reported, and there were no complications of the treatment, such as persistent severe pain, stiffness, or disability.
TABLE 2: VISUAL ANALOG SCALE (VAS) AND FOOT AND ANKLE DISABILITY INDEX (FADI) RESULTS |
||||
|
FADI Baseline |
FADI 5 weeks |
VAS Baseline |
VAS 5 weeks |
|
|
Rehabilitation only |
75.9 |
91.3 (P = 0.003 vs baseline) |
40.0 |
22.1 (P = 0.0016 vs baseline) |
|
Manipulation and rehabilitation |
80.4 |
98.9 (P = 0.001 vs baseline) |
47.3 |
6.2 (P < 0.0001 vs baseline) |
|
P = 0.26 between groups |
P = 0.0059 between groups |
|||
|
Note: An improvement in ankle symptoms and function occured with a lower VAS and/or a higher FADI. Also, there was no “manipulation only” group. |
||||
COMMENTARY
Perhaps, manipulation isn’t just for the back anymore. Practitioners of manipulation (physical therapists, osteopathic physicians, and chiropractors) have long known of the utility of the technique for a variety of locales beyond the spine. This study lends some credence to its usefulness for pathology in a distal joint, in this case, the ankle.
In this trial, the VAS for pain showed improvements in the manipulation group compared to the rehabilitation group, whereas the FADI, weaving in some functional assessments, did not differ significantly between the two groups. It is tempting to ascribe these findings simply to a “provider effect,” the well-known benefits that come with a hands-on aspect of a clinical encounter. This study could be explained completely in this way. Furthermore, the lack of a placebo group complicates our attempt to definitively comment on either of the therapies (rehabilitation or manipulation) studied here. Perhaps, soft tissue massage would have accomplished the same outcomes if touch were the important intervention. All told, what seems to be lacking in making an argument that there is more going on here than simply clinician touch is a convincing mechanism of action; although there are known restrictions in joint motion after an injury or other pathological disease states, why would removing those restrictions necessarily improve functionality? It makes one wonder how that might be studied and clarified.
Predictably, given the known benefits to a dedicated rehabilitation program, all groups showed improvements in both the FADI and VAS when the 5-week assessments were compared to baseline. This reaffirms that ankle rehabilitation works, and all patients with one-time or repeated injuries or lingering symptomatology should be encouraged to stick with a prescribed course of treatment.
Do these results translate easily into clinical practice? Chronic ankle instability is not uncommon, so presumably such patients will appear on our schedules at some point. “Real life” will have the diagnosing and treating clinician as the same person, so having different providers involved in this study seems to complicate the treatment, even possibly creating miscommunication and improper treatment, an issue the researchers acknowledged as well. However, these results might be enhanced, and the clinical utility bolstered, with the same clinician diagnosing and treating, as would happen in daily clinical practice — grounds for another study.
Is there any reason not to offer manipulation to a rehabilitation program? The researchers commented on the lack of adverse effects, although the methodology didn’t outline a specific approach to collecting that information. It might be safe. There is a cost issue such that the researchers offer a suggestion: Try 1 month of rehabilitation exercises and then add manipulation if the participant doesn't achieve satisfactory results, with an earlier start if pain is the primary symptom or to address “joint restriction,” especially in athletes. It is unclear why our athletic patients should have manipulative therapies sooner than others. Perhaps, once again, the way to weave in this treatment approach is a negotiation between patient and provider using the art of medicine to color the sparse facts that have arisen from this, and other, clinical trials.
Ankle joint chiropractic manipulation as adjunctive therapy to typical rehabilitation improves symptoms of chronic ankle instability from repeated sprains.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.