Gallstones and Associated Complications
AUTHORS
Jonathan Glauser, MD, Professor, Emergency Medicine, Case Western Reserve University, Faculty, Residency Program, Emergency Medicine, MetroHealth Medical Center, Cleveland, OH.
Burgundy Stanley, MD, Chief Resident, MetroHealth/Cleveland Clinic Residency Training Program in Emergency Medicine, Case Western Reserve University, Cleveland, OH.
PEER REVIEWER
Steven M. Winograd, MD, FACEP, St. Barnabas Hospital, Bronx, NY; Core Faculty, Department of Emergency Medicine, Assistant Clinical Professor, Emergency Medicine, NYiTCOM, Old Westbury, Long Island, NY.
EXECUTIVE SUMMARY
- Gallbladder disease is very common, affecting more than 10% of the U.S. population, with incidence increasing with age and approaching 30% by the ninth decade of life.
- Multiple imaging modalities can be used to visualize the biliary tract and to diagnose cholecystitis, but the most frequently employed modalities are ultrasonography and cholescintigraphy.
- Risk factors for development of gallstones include family history of cholecystectomy in a first-degree relative, body mass index > 30 kg/m2, rapid weight loss, and physical inactivity.
- Gallstones are the most common cause of acute pancreatitis. This may be a result of bile reflux or obstruction at the ampulla from stones or edema.
- Signs of bile duct obstruction include continuous epigastric pain, elevated serum bilirubin, and bile-free gastric aspirate.
- Common bile duct stones are suggested when the patient with gallstones has an elevated serum bilirubin and a dilated common bile duct on ultrasonography.
- Early endoscopic retrograde cholangiopancreatography may be beneficial for severe gallstone pancreatitis or when cholangitis, jaundice, or a dilated common bile duct is present.
- Cholangitis is an emergency condition characterized by bacterial infection and extrahepatic bile duct obstruction. Treatment entails antibiotic administration and biliary duct decompression via endoscopic retrograde cholangiopancreatography, surgery, or transhepatic decompression.
- Acute cholangitis is a clinical syndrome characterized by Charcot’s triad: fever, jaundice, and abdominal pain.
- Gallstone ileus is characterized by Rigler’s triad: pneumobilia, intestinal obstruction, and ectopic gallstone.
INTRODUCTION
There are many causes of right upper quadrant pain for which patients present to the emergency department (ED). It is the job of the emergency physician to distinguish between those that require emergent intervention and those that do not. Below is a review of biliary causes of right upper quadrant pain with the primary focus on gallstones and their associated complications.Role of the Gallbladder
The primary function of the gallbladder is to concentrate bile. Bile is composed mainly of water, but also contains bile acids, lecithin and other phospholipids, cholesterol, conjugated bilirubin, electrolytes, mucus, and various proteins. Bile is stored in the gallbladder during fasting and released into the duodenum in response to eating, which is neurally and hormonally mediated.1 When there is gallbladder dysmotility, bile becomes suspended with particulate material, forming biliary sludge. (See Figure 1.)
Figure 1. Biliary Sludge
Courtesy of Robert Jones, DO
Gallstones
Gallstones are composed of cholesterol, bilirubin, and calcium salts primarily, but also contain small amounts of proteins and other materials.2,3 The two major stone types are cholesterol stones, which make up 70-80%, and pigmented stones (either black or brown), which make up about 20%.4,5 The remaining stones are made up of a combination of cholesterol, bilirubin, and calcium salts.1,3 (See Table 1.) Most gallstones in the United States are cholesterol stones.2,3,6 The development of gallstones is multifactorial. Some of the recognized risk factors include age 40 years or older, female gender, pregnancy (incidence is up to 12%), family history of cholecystectomy, obesity, rapid weight loss, sedentary lifestyle, diabetes, inflammatory bowel disease, use of exogenous estrogen (in both women and men), dyslipidemia, hemolytic disorders, and cirrhosis.7-9 (See Table 2.) It has been demonstrated that statin use, coffee consumption, and increased physical activity lower risk of gallstone formation.6,8 Similar to biliary sludge, gallbladder dysmotility contributes to gallstone formation. However, cholesterol supersaturation in bile and defective conversion of cholesterol to bile acids also contribute to the formation of cholesterol stones.2,3 Black-pigmented stones are seen in individuals with hemolytic conditions and cirrhosis.2,3,9 Brown-pigmented stones generally form within bile ducts, not the gallbladder itself. These are associated with bacterial infections and are seen more commonly in Asian populations.2,3
Table 1. Gallstone Composition
|
Cholesterol |
Contain ≥ 90% cholesterol |
|
Pigmented (black and brown) |
Contain ≥ 90% bilirubin |
|
Mixed |
Varying proportions of cholesterol, bilirubin, and calcium salts |
Table 2. Risk Factors for the Development of Gallstones
- Increasing age
- Female gender
- Pregnancy
- Ethnicity (Native American or Scandinavian)
- Family history
- Obesity (body masss index > 30 kg/m2)
- Rapid weight loss
- Inflammatory bowel disease
- TPN use
- Exogenous estrogen use
- Diabetes mellitus
- Hypertriglyceridemia
- Sedentary lifestyle
Incidental Gallstones
Not all individuals with gallstones will be symptomatic. Some stones may be detected incidentally when diagnostic imaging is performed for another purpose. In fact, only 10-20% of the 20-25 million Americans with cholelithiasis will go on to develop gallstone disease.2-4,6,9-11 Therefore, incidental stones generally are managed expectantly. One of the reasons we care about gallstone disease, even in asymptomatic individuals, is that the chance of developing a complication, such as acute cholecystitis, choledocholithiasis, or gallstone pancreatitis, is 2-3% per year.10 Additionally, there is a documented association between gallstones and biliary tract cancers.12
Biliary Colic
The pain of biliary colic occurs when the gallbladder contracts, forcing a stone and/or sludge against the gallbladder neck or opening of the cystic duct. This results in increased intra-gallbladder pressure. Fatty meals are known to trigger gallbladder contraction and, therefore, many patients will report pain postprandially. There are also a measurable number of individuals who will have more significant nocturnal pain.10 The pain is classically described as being constant, located in the right upper quadrant or epigastric region, with possible radiation to the right scapula, typically lasting for 1-6 hours with a plateau in pain within an hour. The pain frequently is associated with nausea, vomiting, and/or diaphoresis. It remits spontaneously as the gallbladder relaxes and the intra-gallbladder pressure falls.1,3,6,10 Patients presenting with biliary colic are generally not ill appearing, are afebrile, and have benign abdominal exams. Laboratory studies should not reveal leukocytosis, elevated lipase, or derangement of liver function tests.10 (See Table 3.) The frequency of recurrent symptoms varies from patient to patient. However, most patients do not experience daily symptoms.10
Table 3. Characteristics of Biliary Colic
- Pain in right upper quadrant or epigastric region
- ± Radiation to right scapula
- Pain typically lasts 2-6 hours
- Constant in nature
- ± Nausea and/or vomiting
- ± Diaphoresis
- Spontaneously remits
- Patient is not ill-appearing
- Patient is afebrile
- Abdominal exam is benign
- Labs are without abnormality
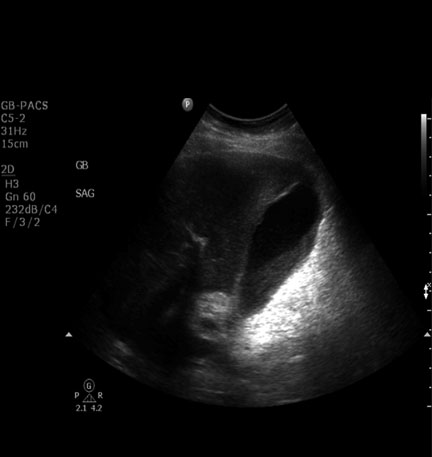
Gallstones are echogenic and cast an acoustic shadow on ultrasound. (See Figure 2.) This is contrasted with biliary sludge, which is visualized as low-level echoes within the gallbladder. Both stones and sludge are also gravity dependent.
The treatment for biliary colic is pain control and outpatient surgical follow-up for non-emergent cholecystectomy. While laparoscopic cholecystectomy is generally the preferred approach (as outlined below), it is estimated that 2-26% of patients undergoing elective laparoscopic cholecystectomy will require conversion to laparotomy.4,6
Figure 2. Multiple Gallstones Seen on Ultrasound
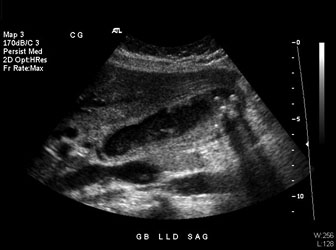
Courtesy of David Effron, MD
Acute Cholecystitis
Acute cholecystitis is the most common complication of gallstone disease and most frequently occurs when a stone becomes impacted in the cystic duct or gallbladder neck, leading to an outflow obstruction, luminal distention, and gallbladder inflammation.2,10,13 (See Figure 3.) Symptoms are often similar to those of biliary colic, although the pain may start more acutely and lasts longer (often 4-6 hours) than what typically is seen with biliary colic.13 Additionally, these patients may be febrile at presentation or develop fever during their ED course. Murphy’s sign is more commonly elicited in those with acute cholecystitis than in those with simple biliary colic. (See Table 4.) Laboratory studies in patients with acute cholecystitis will more commonly reveal a leukocytosis (51-53% of patients) as well as mildly elevated transaminases, bilirubin, and amylase.11
Figure 3. Gallstone Impacted in Gallbladder Neck
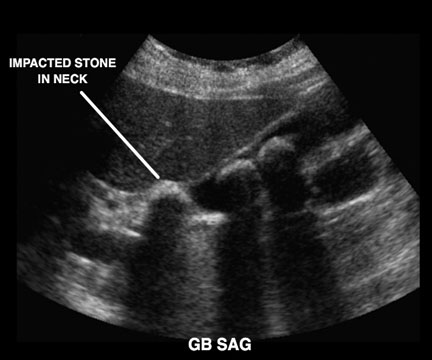
Courtesy of Robert Jones, DO
Table 4. Clinical Findings of Cholecystitis
|
|
|
|
|
|
Ultrasound will be notable for the presence of gallstones, gallbladder wall thickness of more than 3 mm, and pericholecystic fluid.10 (See Figure 4.) A sonographic Murphy’s sign also may be elicited; this, in combination with documented gallstones, has been shown to have a positive predictive value of 92% for cholecystitis.2 The sensitivity and specificity of ultrasound for the diagnosis of acute cholecystitis are 81-95% and 80-95%, respectively.2,13,14 In those patients who undergo CT imaging, findings usually include an overdistended gallbladder, mural thickening, mural enhancement, pericholecystic fat stranding, and pericholecystic fluid.13,15 Additionally, there is characteristic rim enhancement of the adjacent liver.
Figure 4. Acute Cholecystitis
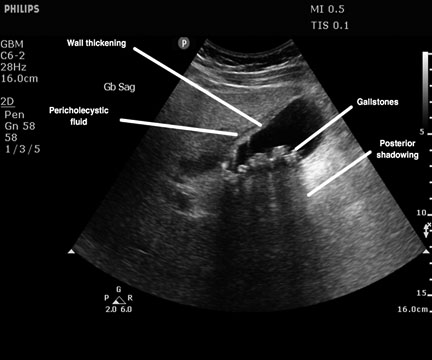
Courtesy of Robert Jones, DO
Treatment for acute cholecystitis is cholecystectomy. This is necessary, as untreated cholecystitis can progress to necrosis, gangrene, and even perforation of the gallbladder.2 The mortality rate of uncomplicated acute cholecystitis is 4%.2 The laparoscopic approach for cholecystectomy is considered the gold standard, given lower mortality, quicker recovery, shorter hospital stay, and its cost effectiveness compared to the open approach.6 However, as with all surgical procedures, there are known complications of laparoscopic cholecystectomy. Some of these include injury to the common bile duct, bile leak, and gallbladder perforation (discussed below).2,6,16
While acute cholecystitis is the most common complication of gallstone disease, it can itself result in many complications. These are discussed below.
Choledocholithiasis
Choledocholithiasis, the presence of one or more stones in the common bile duct, may present similarly to biliary colic. However, the pain is generally more protracted, and these patients will have elevated transaminases. If the stone remains impacted, then a cholestatic pattern will be seen on liver function tests, with bilirubin and alkaline phosphatase being elevated out of proportion to aspartate aminotransferase (AST) and alanine aminotransferase (ALT).4,10 It is estimated that 10-15% of patients with acute cholecystitis have choledocholithiasis and 5-20% of all patients undergoing cholecystectomy are found to have at least one stone in the common bile duct.2,17 These stones occur via two mechanisms and are referred to as primary and secondary stones. Primary stones are those that form within the biliary tract itself in the setting of bile stasis and colonization of the bile by enteric organisms, which is seen most commonly in East Asian populations.17 These stones are also commonly associated with parasitic infections. Secondary stones are those that migrate from the gallbladder through either the cystic duct or a cholecystocholedochal fistula. Secondary stones are the more common of the two.
Treatment for choledocholithiasis includes endoscopic retrograde cholangiopancreatography (ERCP) for removal of the stone(s), followed by cholecystectomy or cholecystectomy with intraoperative cholangiography (highly operator-dependent with a sensitivity and specificity of 59-100% and 93-100%, respectively).17 These procedures are necessary to avoid gallstone pancreatitis and acute cholangitis, which are the two main complications of choledocholithiasis.17
Gallstone Pancreatitis
Cholelithiasis is the most common cause of acute pancreatitis worldwide and accounts for 35-65% of cases.16 Gallstone pancreatitis occurs as a result of passage of stones from the gallbladder into the common bile duct, leading to transient obstruction of the main pancreatic duct as it passes near the common bile duct at the ampulla of Vater or from persistent common bile duct stone(s) that fail to traverse the ampulla.2,3,16 This disease entity is most common in women older than age 60 years and has a broad spectrum of severity ranging from mild pancreatic inflammation to fulminant pancreatic necrosis.18 Approximately 80% of patients fall into the mild category, which carries a 1-3% mortality rate.18 The mortality rate of those who progress to pancreatic necrosis is up to 30%.18 Patients present with symptoms typical of pancreatitis and/or those of biliary colic and have lipase levels up to three times greater than the upper limit of normal.11,17 However, providers should keep in mind that the degree of lipase elevation does not correlate with the severity of disease.11
The definitive treatment for gallstone pancreatitis is cholecystectomy and performance of this is recommended during the same hospitalization as the primary occurrence.6 Recurrent gallstone pancreatitis occurs in 61% of individuals who do not undergo cholecystectomy following the first occurrence.6 However, in patients with severe gallstone pancreatitis, it is contraindicated to perform early cholecystectomy due to the associated increased risk of infection and sepsis.6,18 One study reported an overall complication rate of 44% in those with severe pancreatitis who undergo early cholecystectomy.8 However, this subset of patients (especially those with coexisting cholangitis and/or elevated bilirubin levels indicating biliary obstruction) do benefit from early ERCP and possible endoscopic sphincterotomy or biliary stent placement.16-18
Acute Cholangitis
Bacterial superinfection can occur when stones are lodged in the common bile duct; this is known as acute cholangitis. The obstruction may be either partial or complete. This diagnosis should be considered in patients who present with Charcot’s triad (right upper quadrant pain, jaundice, and fever) and/or Reynolds’ pentad (right upper quadrant pain, jaundice, fever, hypotension, and altered mental status). (See Table 5.) Escherichia coli, Klebsiella pneumoniae, Enterococcus faecalis, and Streptococcus species are the most common bacteria associated with cholangitis.2 Pyogenic liver abscess and portal venous thrombosis can occur as complications of this disease entity. Ultrasonography in patients with cholangitis may reveal biliary dilatation and thickening of the common bile duct wall. CT will most commonly demonstrate biliary obstruction.2 Patients with cholangitis should be treated with antibiotics, and biliary drainage should be arranged either via ERCP or percutaneous means.2,16
Table 5. Clinical Features of Cholangitis
Charcot’s triad
- Right upper quadrant pain
- Jaundice
- Fever
Reynolds’ pentad
- Charcot’s triad plus
- Hypotension
- Altered mental status
Gallstone Ileus
Gallstone ileus is an overall rare complication of cholelithiasis, occurring in 0.4-3% of cases.19,20 It results from perforation of the gallbladder, from chronic gallstones and inflammation, with subsequent fistula formation between the gallbladder and an adjacent viscus. The duodenum (69-70%), colon (14%), and stomach (6%) are the most commonly affected.2,19,20 Mechanical obstruction of the bowel occurs when stones 2 cm or larger migrate from the gallbladder through the fistula tract and become lodged in the lumen of the small intestine.2,19,21 Gallstone ileus is the underlying etiology of approximately 1-5% of all cases of nonmalignant small bowel obstructions (SBO).2,15,21 The terminal ileum is the most common site of the obstruction, likely secondary to its being the narrowest portion of the intestine.2,15,21 Less than half of the patients who develop gallstone ileus have known biliary disease. Patients with gallstone ileus typically present with classic signs and symptoms of SBO. However, these symptoms initially may be intermittent, as the stone passes through more proximal portions of the bowel before finally becoming truly impacted.
CT is often the initial imaging study obtained, given the clinically similarity to SBO. The CT will reveal the small bowel obstruction, an obstructing ectopic gallstone at the transition point, and gas within the gallbladder and biliary tree.2 These three findings are referred to as Rigler’s triad. The fistula tract also may be visualized on CT. This disease entity carries a high morbidity and a mortality rate ranging from 4.5-25%.19,21 Additionally, there seems to be an association between cholecystoenteric fistulas and extrinsic compression of the common hepatic duct or common bile duct (known as Mirizzi syndrome, which is discussed below). In fact, 90% of patients with a cholecystoenteric fistula were found to have Mirizzi syndrome in one surgical series.22 Gallstone ileus is seen most frequently in women with an average age of 65 years.19 (See Table 6.)
Table 6. Characteristics of Gallstone Ileus
- Fistula tract formation between gallbladder and intestinal tract (most commonly the duodenum)
- Impaction of gallstone within the intestinal tract (most commonly the terminal ileum)
- CT will reveal Rigler’s triad
- Rigler’s triad: Small bowel obstruction, ectopic gallstone, pneumobilia
- Most frequently affects elderly women
- Most will not have a history of biliary disease
The treatment for gallstone ileus is enterolithotomy, at a minimum, which will relieve the obstruction. However, in patients only undergoing enterolithotomy, there is a documented recurrence rate of 5-8.2%, which can occur anytime within the first post-operative month to two years later.20 Fistula repair and/or cholecystectomy may be performed, in addition to enterolithotomy, depending on the acuity of the patient (more appropriate in lower acuity patients) and the surgeon’s discretion.21 The open or laparoscopic method may be performed. However, it is common to convert from the laparoscopic technique to laparotomy, as identification of gallstones can be technically difficult using a laparoscope.19
Mirizzi Syndrome
Extrinsic compression of the common hepatic duct or the common bile duct by a stone in the neck of the gallbladder or cystic duct is known as Mirizzi syndrome. This is a rare complication of gallstones. Recurrent episodes of jaundice and cholangitis are common presenting signs.2 Mirizzi syndrome is reported in up to 2% of individuals undergoing cholecystectomy for symptomatic cholelithiasis.2 Ultrasound, CT, or magnetic resonance cholangiopancreatography (MRCP) can be used to diagnose Mirizzi syndrome, with the hallmark being intrahepatic biliary dilation and dilation of the common hepatic duct to the level of the porta hepatis, with the distal common bile duct’s being normal in caliber.2,15 It is important to identify Mirizzi syndrome preoperatively, as the typical cholecystectomy technique is associated with increased risk of extrahepatic bile duct injury.2
Gangrenous Cholecystitis
Gangrenous cholecystitis is a severe form of acute cholecystitis in which there is vascular compromise leading to intramural hemorrhage, necrosis, and intramural abscess secondary to progressive distention of the gallbladder and ultimately ischemia of the gallbladder wall, due to stone impaction in the cystic duct. (See Figure 5.) The incidence is quoted as ranging from 2-39% of patients with acute cholecystitis, with elderly patients and diabetics being at higher risk.2,13,15 Patients with gangrenous cholecystitis present with a sepsis-like picture and also have signs/symptoms of cholecystitis.13 Forty-one percent of these patients will be febrile and 73% will have leukocytosis on laboratory evaluation.11
Figure 5. Abscess in Gallbladder Wall
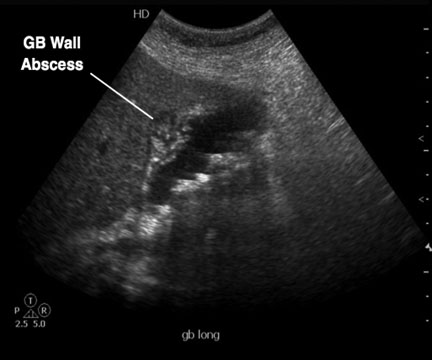
Courtesy of Robert Jones, DO
Ultrasonography in gangrenous cholecystitis reveals heterogeneous, striated thickening and irregularity of the gallbladder wall and intraluminal membranes, which are the result of desquamation of the gallbladder mucosa.2 The latter are considered a specific finding for this condition. The provider should bear in mind, though, that the ultrasound findings of gangrenous cholecystitis may be similar to those seen with carcinoma of the gallbladder. Findings of gangrenous cholecystitis on CT are similar to those seen on ultrasound. However, CT is better at distinguishing between gangrenous cholecystitis and cholangiocarcinoma.2 In the case of the latter, an enhancing gallbladder mass, direct invasion of the liver, and liver metastases may be present.
Treatment for gangrenous cholecystitis is the same as that for acute cholecystitis, which is emergent cholecystectomy. There is a higher likelihood that the patient with gangrenous cholecystitis will need an open cholecystectomy than a patient without gangrenous findings. If surgical intervention is not performed, the patient is at significant risk for life-threatening complications such as perforation.
Gallbladder Perforation
Perforation of the gallbladder occurs in individuals with emphysematous cholecystitis and in approximately 2-12% of severe acute cholecystitis. It carries a mortality rate of up to 24.1%.1,2,13 Obstruction of the cystic duct results in progressive gallbladder distension and inflammation with vascular compromise, gangrene, necrosis, and eventual perforation. Because of its poor blood supply, the fundus is the most common site of perforation.2
Imaging plays an important role in the diagnosis of gallbladder perforation, as the patient may present with nonspecific signs and symptoms. On ultrasound, the gallbladder wall will appear irregular or ill-defined, and a large amount of pericholecystic fluid may be seen. CT may more easily identify interruption of the gallbladder wall or a focal mural defect that is contiguous with pericholecystic fluid.2,15
Iatrogenic Perforation
Gallbladder perforation is reported to occur in 10-40% of laparoscopic cholecystectomies, and of these, 6-8% are associated with spillage of gallstones.2 Perforation may occur during resection from the hepatic bed or during removal of the gallbladder through the umbilical incision. The spilled gallstones most often remain adjacent to the liver and can lead to a subhepatic abscess or abscess in the retroperitoneum below the subhepatic space. However, some stones migrate to distant sites due to the pneumoperitoneum inherent to laparoscopic procedures. Abscess formation occurs with an overall incidence of less than 1%, and seems to occur most frequently with bilirubinate stones.2 This uncommon complication often is difficult to diagnose, as symptoms are vague (nausea, anorexia, and low-grade fever) and can occur anytime from one month to 10 years following the procedure.2 The abscess may be identified on ultrasound, CT, or MRCP and appears as a thick-walled fluid collection. Surgical or percutaneous removal is the treatment for spilled stones, as antibiotics have been found to be ineffective in the management of infected stones.
Hemorrhagic Cholecystitis
Hemorrhagic cholecystitis is an uncommon complication of acute cholecystitis and tends to occur most with gangrenous cholecystitis.2 Transmural inflammation results in mural necrosis and ulceration, with subsequent hemorrhage into the gallbladder lumen. As the blood clots, it may become lodged in the cystic or common bile duct leading to obstruction or it may pass into the duodenum. Some patients will present in the same manner as those with acute cholecystitis. However, others may present with signs or symptoms of simple biliary colic, have jaundice, or have hematemesis and/or melena. This entity is associated with high mortality; therefore, prompt diagnosis is needed.2 Blood in the gallbladder lumen is seen as hyperechoic material, having a higher signal than that from biliary sludge. Clotted blood may be seen as a clump or mass adherent to the gallbladder wall or as heterogeneous echogenic material.
Emphysematous Cholecystitis
Emphysematous cholecystitis is a life-threatening and rapidly progressive complication of acute cholecystitis, which carries a morality rate of 15%.1,2 It results from compromise of the cystic artery and resultant proliferation of gas-forming organisms. This gas penetrates into the gallbladder wall. Organisms frequently associated with this disease are Clostridium welchii and E. coli.2,13,15 Men and diabetic patients tend to have emphysematous cholecystitis with higher frequency than other populations.13 The clinical presentation of this disease entity can be identical to that of acute cholecystitis. Patients with diabetes may present with milder symptoms than non-diabetic patients.15 Interestingly, gallstones may be absent in 33-50% of patients.2,13 Emphysematous cholecystitis carries a perforation rate five times higher than in acute cholecystitis.
It is critical to rapidly identify emphysematous cholecystitis. Ultrasound findings will vary depending on the amount of gas present. Small amounts of gas will appear as echogenic foci with associated ring-down artifact. (See Figure 6.) Larger amounts of gas may appear as a curvilinear arc of increased echogenicity with associated dirty shadowing and may make ultrasound interpretation difficult.2,13 However, CT is more sensitive for the diagnosis, and findings may include gas within the gallbladder wall or dependent portion of the gallbladder lumen.2 (See Figure 7.)\
Figure 6. Emphysematous Cholecystitis Seen on Ultrasound
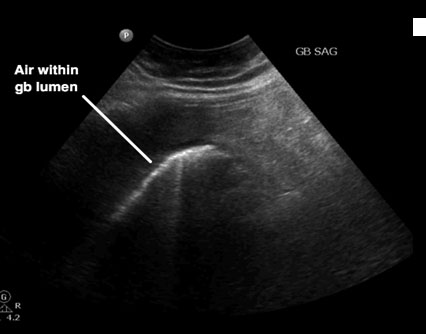
Courtesy of Robert Jones, DO
Figure 7. Emphysematous Cholecystitis Seen on CT
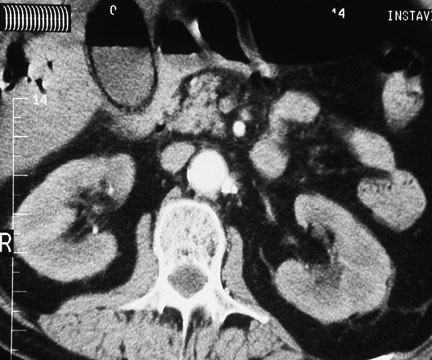
Courtesy of David Effron, MD
Chronic Cholecystitis
Chronic cholecystitis may result from a single episode or from recurrent episodes of acute cholecystitis. Intermittent obstruction of the cystic duct or gallbladder neck and gallbladder dysmotility are predisposing factors. Chronic inflammatory changes result in the gallbladder wall becoming thickened and fibrotic.
Diagnosis of chronic cholecystitis on imaging may be difficult. Typically, ultrasound will reveal gallstones, a thickened gallbladder wall, and contraction of the gallbladder even in the fasting state. Distinction between acute and chronic cholecystitis can be made using MRCP, on which the thickened gallbladder wall will give off a low signal intensity. However, gallbladder wall edema, seen in acute cholecystitis, is seen as a high-signal intensity.2
The treatment for chronic cholecystitis is generally elective cholecystectomy, as many patients do not have pain at the time the diagnosis is made but will give a classic history of recurrent episodes with symptoms similar to biliary colic.11
Role of Ultrasound
Ultrasonography is generally the initial imaging modality obtained to evaluate for biliary disease as the cause of right upper quadrant pain in the ED. It has a sensitivity of approximately 84-95% and a specificity of more than 98% for gallstones.3,4,6,10,13 Additionally, ultrasound is noninvasive, readily available in most EDs, and does not expose the patient to ionizing radiation. It is important to remember that ultrasounds obtained when patients are fasting may be easier to interpret, as stones are best seen when surrounded by bile in a non-contracted gallbladder.10 False-negative results may be obtained if the gallbladder is completely filled with stones or if it is contracted around many stones. (See Figure 8.) Stones also may be missed if they are less then 1 cm.2 False-positive results may be observed if polyps are present within the gallbladder. (See Figure 9.)
Figure 8. Multiple Stones Within a Contracted Gallbladder
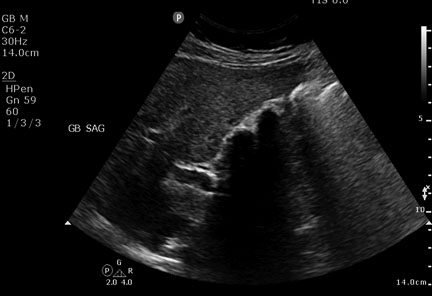
Courtesy of Robert Jones, DO
Figure 9. Polyp Within the Gallbladder
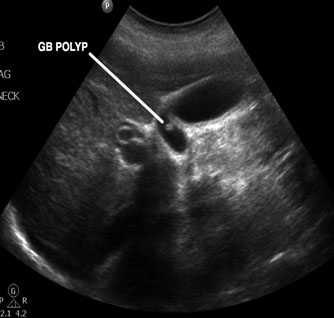
Courtesy of Robert Jones, DO
Additionally, the sensitivity for detecting stones in the common bile duct on ultrasound is 20-90%, and while a dilated common bile duct supports the diagnosis of choledocholithiasis, it is nonspecific.2,10,23 (See Figures 10-12.) This should be kept in mind when ultrasound is performed in patients with signs or symptoms suspicious for cholangitis. In these patients, MRCP, endoscopic ultrasound (EUS), or ERCP may be helpful in confirming the diagnosis.
Figures 10-12. Choledocholithiasis
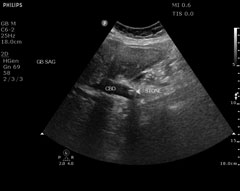
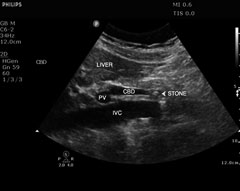
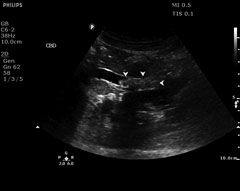
Courtesy of Robert Jones, DO
Other Imaging Modalities and Their Utility
While ultrasound remains the initial imaging modality of choice, it has limitations when evaluating for some of the complications of acute cholecystitis. As such, other imaging modalities may be needed.
Only 10-20% of stones contain enough calcium to make them sufficiently radiopaque to be seen on plain films.2,10 (See Figure 13.) Before the widespread and routine use of ultrasound and CT, abdominal plain films were used to make the diagnosis of emphysematous cholecystitis, as gas outlining the gallbladder wall can be visualized.2,15 (See Figure 14.) Additionally, this modality may be helpful in the diagnosis of gallstone ileus when CT is not available or if the patient is too unstable to be sent to CT. Findings of gallstone ileus on a plain film include signs of obstruction, pneumobilia, and possibly the obstructing stone (although the stone is seen in less than 15% of cases).19 (See Figure 15.)
Figure 13. Multiple Gallstones Seen on Plain Film
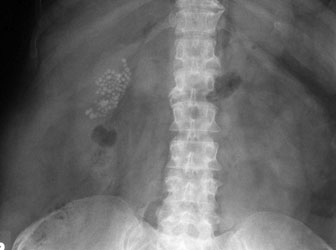
Courtesy of David Effron, MD
Figure 14. Emphysematous Cholecystitis on Plain Film
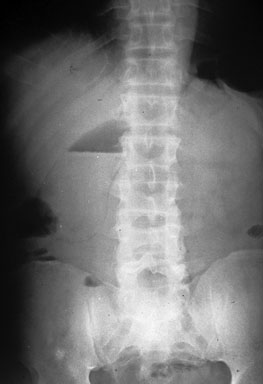
Courtesy of David Effron, MD
Figure 15. Gallstone Ileus on Plain Film
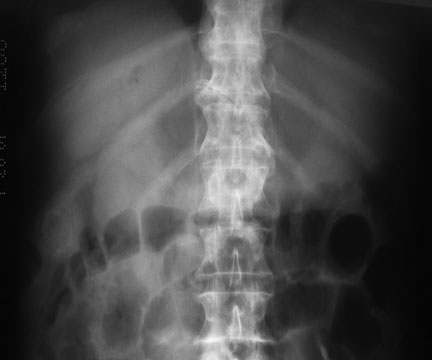
Courtesy of Robert Jones, DO
Hepatobiliary scintigraphy, while not commonly obtained from the ED, is a functional study and can be used to evaluate for acute cholecystitis.2,6 A radioactive tracer is injected intravenously and is normally excreted into the gallbladder within 30 minutes to one hour if the cystic duct is patent.13 If the gallbladder is not visualized within this timeframe and there is prompt biliary excretion of the tracer, then acute cholecystitis is likely the cause of the patient’s symptoms. It has been reported that cholecystoscintigraphy has a sensitivity of 90-97% and a specificity of 71-90% for the diagnosis of acute cholecystitis.4,6,13 However, false positives can occur in patients with abnormal bile flow.2 Additionally, delayed filling also may occur in patients with chronic cholecystitis.
CT is generally not obtained as the first imaging study in patients with expected gallstones and/or complications of these. However, this modality may be pursued when an alternative diagnosis is being considered or when ultrasound is not available or is equivocal. CT has a sensitivity of 55-80% and specificity of 100% for detecting gallstones.4 (See Figures 16-18.) The poor sensitivity of CT is attributed to the fact that many stones have the same density as bile and, therefore, are not easily distinguishable.2,10 However, the sensitivity and specificity of detecting acute cholecystitis on CT are significantly better and are noted to be 91.7% and 99.1%, respectively.2 The sensitivity of contrast-enhanced CT in the detection of choledocholithiasis is 85-97% and the specificity is 88-96%.18 Additionally, CT is 96% specific in the diagnosis of gangrenous cholecystitis but has a significantly lower sensitivity of 29.3%.2
Figures 16-18. Gallstones Seen on CT
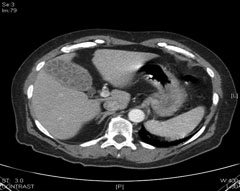
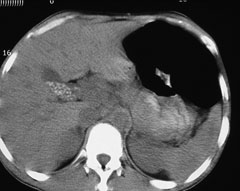
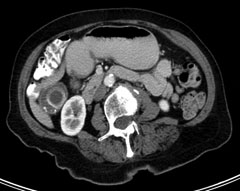
Courtesy of David Effron, MD
MRCP, like CT, is not considered a first-line imaging modality, but may be helpful in patients in whom acute cholecystitis is suspected but other imaging findings are equivocal.2 MRCP has a sensitivity of 89-100% and a specificity of 83-100% for the detection of gallstones and is more sensitive (85-93%) than ultrasound in the detection of choledocholithiasis.2,4,11,24 Additionally, this imaging study is better at detecting obstructing stones in the gallbladder neck and/or cystic duct.2,13 Many of the complications of acute cholecystitis are readily identifiable on MRCP, including mural necrosis, microabscesses, hemorrhage, perforation, and pericholecystic abscess. Additionally, there are no known harmful fetal effects associated with noncontrasted magnetic resonance studies.25
As mentioned above, ERCP is highly accurate for the detection of choledocholithiasis and also allows for therapeutic intervention (stone extraction, stent placement, and biopsy). ERCP employs a combination of upper gastrointestinal endoscopic techniques and fluoroscopic imaging. Its sensitivity and specificity for the detection of choledocholithiasis are 80-97% and 95-100%, respectively.4,7,18 The success rate for stone extraction is documented to be around 95%.18 Because ERCP is invasive, there are associated risks including the development of pancreatitis, cholangitis, sepsis, biliary tract perforation, and hemorrhage.4 Complications are reported at a rate of 3-10%.2,4 Additionally, there is a documented association between ERCP, preterm pregnancy, and low birth weight in the pregnant population. The rate of pancreatitis post-ERCP also seems to be higher than that of the general population in pregnancy.7 Therefore ERCP generally is reserved for those with choledocholithiasis demonstrated on imaging or for those considered to be at high risk for having choledocholithiasis.
EUS has a sensitivity of 93-98% and a specificity of 97-100% for the diagnosis of choledocholithiasis.16,18,26 Additionally, it is better than MRCP at detecting stones less than 6 mm in size.16,17 Because of this, EUS may assist in selecting which patients are most likely to benefit from therapeutic ERCP.
Medical Therapy vs. Surgical Intervention
Most patients with symptomatic cholelithiasis or those suffering from the complications of cholelithiasis will undergo cholecystectomy as definitive treatment. However, other therapies are available to patients who prefer nonsurgical management, in those for whom surgery is deemed too high risk, and also may be considered for patients undergoing rapid weight loss (such as those undergoing weight reduction procedures or those on very low calorie diets).8 These interventions are considered to be palliative at best and are used with much less frequency today than in the past.4,6 Ursodeoxycholic acid is a medication that works by reducing biliary cholesterol secretion, increasing biliary bile acid concentrations, and thereby reducing the cholesterol saturation index.5 This medication works best for cholesterol-rich gallstones. It has been documented that the average gallstone dissolution rate is 59% after 12 months of treatment.6 The major disadvantage of this intervention is the 25-50% gallstone recurrence rate within five years of treatment cessation.4-6 Percutaneous cholecystostomy and cystic duct stent placement, via ERCP, may be another option to consider in the critically ill population.4
Pregnancy and Postpartum Considerations
It is important to keep in mind that biliary sludge and gallstones are known to form during pregnancy.8 Equally as important is that cholelithiasis and its associated complications are a leading nonobstetrical cause for hospital admission in the first postpartum year.27 Women who were obese prior to pregnancy and those with pre-existing hypertension, preeclampsia, and/or pre-existing or gestational diabetes were found to be more likely to have gallstone-related admissions in a retrospective case-control study.27 Medical management, with intravenous fluids and analgesics, has been demonstrated to relieve biliary symptoms in 64% of these patients.6 Ultrasound, noncontrasted MRCP, and cholescintigraphy may be employed safely when imaging is needed to assist with the diagnosis. Surgical intervention in this patient population is reserved for those with recurrent symptoms, symptoms that do not respond to medical intervention, or for those with any of the above complications of cholelithiasis.4,6 The laparoscopic approach has been performed safely in all trimesters and is the preferred operative plan.4 However, this may be more technically difficult at or near term due to the size of the gravid uterus.28
What Else Is in the Differential of Right Upper Quadrant Pain?
In evaluating patients with right upper quadrant pain, it is important to consider causes other than those that are cholelithiasis related as well. It is imperative that emergency physicians also evaluate patients for other conditions, including acute coronary syndrome, gastroesophageal reflux/peptic ulcer disease, hepatitis, gallbladder torsion, sphincter of Oddi dysfunction, chronic pancreatitis, irritable bowel syndrome, ischemic bowel disease, pyelonephritis, ureteral calculi, Fitz-Hugh-Curtis syndrome, and right lower lobe pneumonia.13 (See Table 7.) The emergency physician should rely on the history and physical examination to help distinguish the likely etiology of the patient’s symptoms.
Table 7. Other Causes of Right Upper Quadrant Pain
- Acute coronary syndrome
- Gastroesophageal reflux disease/peptic ulcer disease
- Hepatitis
- Gallbladder torsion
- Sphincter of Oddi dysfunction
- Chronic pancreatitis
- Irritable bowel syndrome
- Ischemic bowel disease
- Pyelonephritis
- Ureteral calculi
- Fitz-Hugh-Curtis syndrome
- Right lower lobe pneumonia
The Patient Without Gallstones
Functional gallbladder disease, also called gallbladder dyskinesia, acalculous biliary disease, cystic duct syndrome, and gallbladder spasm, may cause biliary pain. This is generally thought to result from a primary gallbladder motility disturbance. Standard imaging tests employed in the ED do not reveal pathology, and this is generally diagnosed by cholecystokinin (CCK)-stimulated cholescintigraphy demonstrating a gallbladder ejection fraction of less than 40%. This may affect up to 7% of men and 21% of women experiencing biliary-type pain, with normal laboratory values and ultrasonography. Cholecystectomy is currently the primary treatment for functional gallbladder disease, and current data indicate that approximately 3.2-3.4% of all cholecystectomies in this country are performed for this reason.29 For the emergency physician, this is a diagnosis of exclusion.
CONCLUSION
There are many causes of right upper quadrant pain. It is important to consider the patient’s symptoms and exam in determining if gallstones and/or their complications are a likely cause. If this is the case, laboratory tests and an ultrasound should be obtained as part of the initial workup. For patients who are ultimately diagnosed with biliary colic, outpatient surgical follow-up should be arranged. For patients with any complication of cholelithiasis, surgical consultation should be obtained and admission arranged. In patients with equivocal ultrasounds, it is reasonable to pursue alternative imaging to ascertain the etiology of the patient’s symptoms.
REFERENCES
- Atilla R, Oktay C. Pancreatitis and cholecystitis. In: Tintinalli JE, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 7th ed. New York: McGraw Hill; 2011:558-566.
- Bennett GL. Evaluating patients with right upper quadrant pain. Radiologic Clin North Am 2015;53:1093-1130.
- Njeze GE. Gallstones. Nigerian J Surg 2013;19:49-55.
- Abraham S, Rivero HG, Erlikh IV, et al. Surgical and nonsurgical management of gallstones. Am Fam Physician 2014;89:796-802.
- Nunes D. Dissolution therapy for the treatment of gallstones. In: Post TW, ed. UpToDate. Waltham: UpToDate; 2013.
- Bellows CF, Berger DH, Crass RA. Management of gallstones. Am Fam Physician 2005;72:637-642.
- Almashhrawi AA, Ahmed KT, Rahman RN, et al. Liver diseases in pregnancy: Diseases not unique to pregnancy. World J Gastroenterol 2013;19:7630–7638.
- Afdhal NH. Epidemiology of and risk factors for gallstones. In: Post TW, ed. UpToDate. Waltham: UpToDate; 2015.
- Acalovschi M. Gallstones in patients with liver cirrhosis: Incidence, etiology, clinical and therapeutical aspects. World J Gastroenterol 2014;20:7277-7285.
- Zakko SF. Uncomplicated gallstone disease in adults. In: Post TW, ed. UpToDate. Waltham: UpToDate; 2015.
- Knab LM, Boller A, Mahvi DM. Cholecystitis. Surgical Clin North Am 2014;94:455-470.
- Nogueira L, Freedman ND, Engels EA, et al. Gallstones, cholecystectomy, and risk of digestive system cancers. Am J Epidemiol 2013;179:731-739.
- Zakko SF, Afdhal NH. Acute cholecystitis: Pathogenesis, clinical features, and diagnosis. In: Post TW, ed. UpToDate. Waltham: UpToDate; 2015.
- Gilo NB, Amini D, Landy HJ. Appendicitis and cholecystitis in pregnancy. Clin Obstet Gynecol 2009;52:586-596.
- Chawla A, Bosco JI, Lim TC, et al. Imaging of acute cholecystitis and cholecystitis-associated complications in the emergency setting. Singapore Med J 2015;56:438–444.
- de C Ferreira LE, Baron TH. Acute biliary conditions. Best Pract Res Clin Gastroenterol 2013;27:745-756.
- Arain MA, Freeman ML. Choledocholithiasis: Clinical manifestations, diagnosis, and management. In: Post TW, ed. UpToDate. Waltham: UpToDate; 2015.
- Cucher D, Kulvatunyou N, Green DJ, et al. Gallstone pancreatitis: A review. Surgical Clin North Am 2014;94:257-280.
- Keaveny AP, Afdhal NH, Bowers S. Gallstone ileus. In Post TW, ed. UpToDate. Waltham: UpToDate; 2015.
- Apollos JR, Guest RV. Recurrent gallstone ileus due to a residual gallstone: A case report and literature review. Int J Surg Case Rep 2015;13:12-14.
- Vasilescu A, Cotea E, Palaghia M, et al. Gallstone ileus: A rare cause of intestinal obstruction — Case report and literature review. Chirurgia 2013;108:741-744.
- Beltran MA, Csendes A, Cruces KS. The relationship of Mirizzi syndrome and cholecystoenteric fistula: Validation of a modified classification. World J Surg 2008;32:2237-2243.
- Maple JT, Ben-Menachem T, Anderson MA, et al. The role of endoscopy in the evaluation of suspected choledocholithiasis. Gastrointest Endosc 2010;71:1-9.
- Kaltenthaler E, Vergel YB, Chilcott J, et al. A systematic review and economic evaluation of magnetic resonance cholangiopancreatography compared with diagnostic endoscopic retrograde cholangiopancreatography. Health Technol Assess 2004;8:1-89.
- Brooks DC. Gallstones in pregnancy. In Post TW, ed. UpToDate. Waltham: UpToDate; 2014.
- Tse F, Liu L, Barkun A, et al. EUS: A meta-analysis of test performance in suspected choledocholithiasis. Gastrointest Endosc 2008;67:235-244.
- Ko CW. Risk Factors for gallstone-related hospitalization during pregnancy and the postpartum. Am J Gastroenterol 2006;101:2263-2268.
- Rollins MD, Chan KJ, Price RR. Laparoscopy for appendicitis and cholelithiasis during pregnancy: A new standard of care. Surgl Endosc 2004;18:237-241.
- Thiels CA, Hanson KT, Chawla KS, et al. Functional gallbladder disease: Operative trends and short-term outcomes. Surgery 2016; Apr. 26 [Epub ahead of print].
MONOGRAPH: Biliary causes of right upper quadrant pain with the primary focus on gallstones and their associated complications.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
