The Initial Evaluation and Clearance of Spinal Injuries in Emergency Medical Practice
July 1, 2016
Reprints
AUTHORS
Benjamin J. Lawner, DO, MS, EMT-P, FACEP, Assistant Professor, Department of Emergency Medicine, University of Maryland School of Medicine; Deputy EMS Medical Director, Baltimore City Fire Department.
Brandon M. Parker, DO, Emergency Medicine Residency, University of Maryland Medical System, Baltimore.
PEER REVIEWER
Dennis Hanlon, MD, FAAEM, Associate Professor of Emergency Medicine, Quality Site Director, Allegheny General Hospital, Pittsburgh, PA.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, Dr. Dietrich (editor in chief), Dr. Lawner (author), Dr. Parker (author), Dr. Hanlon (peer reviewer), Ms. Behrens (nurse reviewer), Ms. Mark (executive editor), Ms. Coplin (executive editor), and Mr. Landenberger (continuing education and editorial director) report no relationships with companies related to this field of study.
EXECUTIVE SUMMARY
- Current research shows that cervical immobilization collars cause increased intracranial pressure, which has the potential to worsen traumatic brain injury.
- Chest straps used in immobilization have a marked pulmonary restrictive effect, even in healthy nonsmokers with presumed normal baseline lung function.
- A statement from the American College of Surgeons advises against immobilization for victims of penetrating trauma.
- Spinal immobilization is advocated in cases of spinal tenderness, multisystem trauma, severe head or facial trauma, numbness or weakness in an extremity after trauma, loss of consciousness, altered mental status, and distracting injury.
The initial evaluation and management of patients with potential spinal injuries in emergency medicine practice is in evolution. The authors thoughtfully explore the evidence available and its limitations.
—The Editor
Introduction and Epidemiology
Spinal injuries present a multitude of challenges to the treating emergency physician or trauma professional. Suspected cervical spine injuries place a significant burden of injury upon emergency medical services (EMS) as well as emergency departments (EDs). In North America, it is estimated that EMS annually transports more than 1 million patients suspected of having a cervical spine injury, according to a 2005 survey.1 An estimated 14,000 spinal cord injuries are encountered annually, and the majority occur in the cervical spine with concomitant cervical spine fractures or dislocations. Indeed, thousands more cervical spine injuries happen without concomitant spinal cord injury.2 Cervical spine injury is relatively rare, given that only 2% of patients transported with a suspected injury are ultimately found to have a spine fracture, and less than 1% of those patients ultimately develop a neurologic deficit. A recent study featured in the European Spine Journal confirms widely understood epidemiological data. Of 250,584 multiple trauma patients aged 16 years and older, 8,871 (3.5%) sustained some type injury to the cervical spine. Less than 1% of the total population experienced an injury to the actual spinal cord.3 Nevertheless, spine trauma is accompanied by significant morbidity and mortality.4,5
Clinicians grapple with the challenges of time and diagnostic accuracy in their quest to identify life-threatening injuries. Patients may not always present with consistent physical examination findings, and the altered level of consciousness that frequently accompanies major trauma further confounds the initial assessment. Because of the potential for paralysis or other major injury, recognition of cervical spine injury is of prime importance. Prehospital spinal immobilization has long been considered as the standard of care for patients with suspected cervical spine injury.6,7 Recent literature has called into question some of these long-standing immobilization strategies. Fortunately, decision rules and commonly available radiologic modalities reliably identify the presence of clinically significant spine injury, so the emergency physician must understand the limitations and indications for each tool. Fortunately, certain factors are reliably associated with the presence of some type of cervical trauma: advanced age, Le Fort facial fractures, and an impaired level of consciousness.3 Lower systolic blood pressures also were linked to spine trauma, and that finding echoes the need for vigilance in the presence of systemic hypotension.3
Spinal immobilization must be implemented and discontinued, as with all interventions, with an analysis of risks vs. benefits. The collar is designed to protect patients from secondary spinal cord trauma by restricting movement in an unstable spine. Some studies have quoted ranges from 3-25% of spinal cord injuries being caused by a secondary injury during transport or early hospital care. However, it is very difficult to credit spinal immobilization with protection against secondary injury.4 Current research shows that cervical immobilization collars cause increased intracranial pressure, which has the potential to worsen traumatic brain injury.8–10 Chest straps used in immobilization have a marked pulmonary restrictive effect, even in healthy nonsmokers with presumed normal baseline lung function.11,12 Furthermore the process of immobilization on a long spine board leads to progressively worsening pain in the head, neck, and back area, often resulting in the necessity to radiograph the spine in the ED.11
Further complicating the evaluation of spinal injuries is the recent research that has shed light on the deleterious effects of spinal immobilization. Historically, nonselective spinal immobilization represented the standard of care in many EMS systems. It was not uncommon for EMS providers to secure ambulatory patients to rigid backboards and apply a cervical collar to anyone who endured a significant mechanism of injury.13 A thorough discussion of the evidentiary basis for routine spinal immobilization is beyond this article’s scope. However, it is clear that spinal immobilization is not without untoward side effects. Recent position statements from the National Association of EMS Physicians (NAEMSP) have endorsed the use of more selective spinal immobilization protocols, and EMS systems across the United States are moving away from routine use of the spine board.14,15 Another statement from the American College of Surgeons advises against immobilization for victims of penetrating trauma.
The paradigm shift toward a more thoughtful use of cervical immobilization devices does not relieve the emergency provider from the burden of ruling out significant injury. Indeed, prehospital and emergency clinicians must remain vigilant and understand the limitations associated with current clinical decision rules and the current standard of more “selective spinal care.” It has been shown that clinical examination can reliably exclude clinically significant cervical spine injuries. A prospective evaluation of 2,176 consecutive patients with trauma revealed 33 (1.6%) with a cervical spine injury. Of the 33 cervical spine injuries, only three had negative clinical examinations. These three patients were found to have a C2 spinous process fracture (no specific treatment needed) and C6-C7 body fractures (considered “stable” fractures but treated with a halo), and a C1 lamina fracture along with C6-C7 body fractures (considered “stable,” but treated with a cervical-thoracic orthosis).16 These three cases demonstrate limitations of clinical examination for 100% sensitivity; however, the missed cases were of questionable clinical significance. When clinical exam is used in conjunction with radiographic evaluation, fewer injuries are missed.
This article will review the evidence behind current prehospital spinal immobilization strategies. Furthermore, the authors will discuss clinically available decision rules for clearance of the cervical spine and highlight recent advances in imaging modalities designed to “clear” the spine of injury. It is hoped that a more nuanced understanding of the literature will contribute to a comprehensive approach to the identification and “clearance” of cervical spine trauma.
Prehospital Clearance of the Cervical Spine and Evidence-based Prehospital Protocols
In an effort to avoid unnecessary immobilization and facilitate timely transport of trauma victims, some prehospital systems have adopted algorithms for spinal clearance. These strategies have the benefit of increasing patient comfort and are predicated upon existing tools that are more commonly employed in the ED. Data exist to support the use of “clearance” protocols. In early 2001, Stroh and Braude advocated for a more “selective strategy” for spinal immobilization.17 The authors described the use of a detailed protocol to guide paramedics in the application of restrictive devices. Their proposed protocol advocated spinal immobilization in cases of spinal tenderness, multisystem trauma, severe head or facial trauma, numbness or weakness in an extremity after trauma, loss of consciousness, and altered mental status. The protocol was later modified to include distracting injury.17 The authors recognized the potential ill effects of indiscriminate backboard use, and reported that their multi-jurisdictional protocol did not miss any significant injuries. The study used a retrospective review to examine spine-injured patients transported to five receiving hospitals. Of the 504 patients who arrived via EMS, 495 were transported with spinal precautions. Five out of 504 patients were found to have cervical spine injuries, and two of the injuries were deemed “unstable.” Not surprisingly, all patients with missed injuries were at the extremes of age: older than 65 years or younger than 1 year. The authors reported that their protocol excluded spinal injuries with a 99% sensitivity and advocated for a more judicious use of collars and rigid boards.
In 2009, Vailaincourt et al attempted to validate the Canadian C-Spine rule in the out-of-hospital environment.12 The study was carried out in multiple EMS regions and enrolled 1,949 patients. The Canadian systems participating in this study included “basic” and “advanced care paramedics.” Paramedics completed online training on the Canadian C-Spine rule and documented findings in their patient care report. Important outcome measures included any fracture, dislocation, or unstable cervical spine injury discovered during the patient’s hospital course. The study reported that the rule was applied with 100% sensitivity, despite the fact that paramedics “misinterpreted” the rule in 320 patients. The authors estimated that application of the rule would have averted more than 700 instances of spinal immobilization. Obvious limitations of this study included a relatively small number of clinically important spine injuries (n = 12) and the utilization of an all-paramedic level EMS system.
Reduction of unnecessary immobilization is important. Patients will be more comfortable and avoid potentially adverse physiologic effects, including pain and impaired chest excursion.18,19 Current EMS protocols, such as the one recently approved by the Maryland Institute for Emergency Medical Services Systems (see Table 1), incorporate these considerations into treatment algorithms.15 As opposed to tasking EMS providers with “clearance,” clear-cut protocols theoretically offer less ambiguous treatment choices while minimizing missed injuries. A recent article published in the Western Journal of Emergency Medicine compared three contemporary spinal motion restriction protocols.20 In this cross-sectional study, patients were evaluated by trained assistants following arrival via EMS. Four hundred ninety-eight patients had spinal immobilization in place, and 82 patients had a cervical collar applied in the ED. Two “missed” injuries were found in the group that was not immobilized. Upon further investigation, the authors contend that all spinal injuries would have been immobilized appropriately in the prehospital setting if the protocol was followed with “100% compliance.” Interestingly enough, causality between protocol noncompliance and worsening of spinal injury has not been borne out in the literature. Achieving a balance between identification of all potential cervical spine injuries and the avoidance of important untoward effects is an exceedingly difficult proposition. The evidence base supporting spinal immobilization has come under increased scrutiny, and the consequences of transporting an injured patient without a cervical collar in place have yet to be elucidated in the literature. Fortunately, EMS protocols are moving away from reliance on mechanistic criteria for immobilization and are embracing a more scientific approach to assessment. Indeed, the two protocols cited in the study, with the highest level of paramedic compliance, are similar to existing, validated clinical decision rules. The ideal prehospital protocol has yet to be crafted, although its goals are shared: 1) the identification of patients at high risk for injury, and 2) minimization of unnecessary immobilization.
Table 1. Spinal Protection
Indication for initiating spinal protection:
“Spinal protection” refers to the act of protecting the spinal cord from further injury.
“Spinal immobilization” is the act of placing a patient on a backboard with a cervical collar for the purpose of trying to prevent excessive movement of the spinal column.
Patients who have a blunt trauma with a high-energy mechanism of injury that has potential to cause spinal cord injury or vertebral instability and one or more of the following should receive spinal protection:
- Midline spinal pain, tenderness, or deformity
- Signs and symptoms of new paraplegia or quadriplegia
- Focal neurological deficit
- Altered mental status or disorientation
- Distracting injury: Any injury (e.g., fracture, chest, or abdominal trauma) associated with significant discomfort that could potentially distract from a patient’s ability to accurately discern or define spinal column pain or tenderness.
Adapted from the 2015 edition of the Maryland Medical Protocols for Emergency Medical Services Providers https://www.miemss.org/home/Portals/0/Docs/Guidelines_Protocols/Protocols_2015_FULL_Web.pdf.
The current position statement from the American Academy of Neurological Surgeons (AANS) recognizes that there is a lack of data for cervical spine immobilization in both hospital and prehospital settings.21 For this reason, immobilization strategies vary from one institution to another. The AANS policy statement advocates for the following conservative approach: “All trauma patients with a cervical spinal column injury or with a mechanism of injury having the potential to cause cervical spinal injury should be immobilized at the scene and during transport using a combination of a rigid cervical collar and supportive blocks on a backboard with straps.” This recommendation should be interpreted in the context of all available data and applied on a patient-to-patient basis with consideration of benefits and risks of full spine immobilization. It is also worth mentioning that recommendations contained within the AANS document conflict with more recent statements from the National Association of EMS Physicians and many state-endorsed prehospital treatment algorithms. Indeed, the current state of prehospital practice has embraced an approach that favors spinal “protection” over more conservative methods of immobilization.
Clinical Decision Rules for Spinal Clearance
ED providers primarily use one of two algorithms for clinical clearance of the cervical spine. The National Emergency X-Radiography Utilization (NEXUS) rule (see Table 2) and the Canadian C-spine rule form the basis for medical decision-making about when imaging is required. Both rules have been studied extensively in the literature, and a recent meta-analysis published in the Canadian Medical Association Journal more critically examined their diagnostic accuracy.22 These rules have excellent sensitivity and reliably predict which patients will not benefit from routine imaging. Importantly, both rules must be applied to patients with a normal level of alertness following a traumatic injury. Clinicians must be familiar with pearls and pitfalls of each tool so that diagnostic yield and patient safety are not compromised.
Table 2. NEXUS Criteria for Clearance of the Cervical Spine
Consider clinical clearance of the cervical spine if NONE of the following are present:
- Focal neurologic deficit
- Midline spinal tenderness
- Altered level of consciousness
- Intoxication
- Distracting injury
*Caution is advised in patients at the extremes of age
NEXUS remains a “go-to” tool because of its simplicity. It consists of five basic criteria and does not include a provision for the patient’s mechanism of injury. The rule highlights five “low-risk” criteria. If all criteria are met, then the patient is unlikely to have sustained a clinically significant injury. NEXUS has been prospectively validated and boasts a sensitivity of 99% when applied correctly. Furthermore, NEXUS criteria have been extrapolated — and examined — for use in the pediatric population.22,23
It is important to recognize the nuances of the NEXUS rule when applying to a practice managing patients with suspected C-spine injury. The impressive negative predictive value of the NEXUS low-risk rule was applied in its original study with specific definitions for each of the five criteria. The presence of a distracting injury remains a difficult criterion to objectify, and physician interpretation is required. When assessing for evidence of intoxication, it is important to recognize that the original authors defined this broadly to include a recent history of intoxicating ingestion, physical findings of clinical intoxication, or positive testing of bodily secretions for alcohol or other drugs affecting levels of alertness. In the original article, an altered level of consciousness was defined as any of the following: “GCS [Glasgow Coma Scale] of 14 or less; disorientation to person, place, time, or events; an inability to remember three objects at five minutes; a delayed or inappropriate response to external stimuli; or other findings.”24
The Canadian C-Spine rule applies three high-risk criteria, five low-risk criteria, and the ability of patients to rotate their necks. (See Figure 1.) The high-risk criteria include age older than 64 years, numbness or tingling in the extremities, or a dangerous mechanism. The dangerous mechanism is further described as including a fall from greater than three feet or down five stairs, an axial load to the head, a motor vehicle collision (MVC) at a high speed or with ejection, or a motorized recreational vehicle or bicycle collision. Low-risk criteria are defined as a simple rear-end MVC, ambulatory status at any time on scene, no neck pain immediately at scene, and absence of midline C-spine tenderness.5,12,22 This rule offers a more objective decision tree and can be applied to patients with tenderness in their cervical spine. Multiple studies have found the Canadian C-Spine rule to be superior to the NEXUS rule. In a systematic review, Michaleff et al found the Canadian C-Spine rule to have better diagnostic accuracy than the NEXUS rule. This study included 15 studies and found the Canadian C-Spine rule to have a sensitivity ranging from 0.90 to 1.00, while NEXUS had a sensitivity ranging from 0.83 to 1.00. Specificity was poor, as expected, ranging from 0.01 to 0.77 and 0.02 to 0.46 in the Canadian C-Spine rule and NEXUS, respectively.22 In a prospective cohort study of more than 8,000 patients, Stiell et al found superior sensitivity and specificity when comparing the Canadian C-Spine rule to NEXUS as well as reduced rates of radiography when using the Canadian C-Spine rule.5
Figure 1. Canadian C-Spine Rule
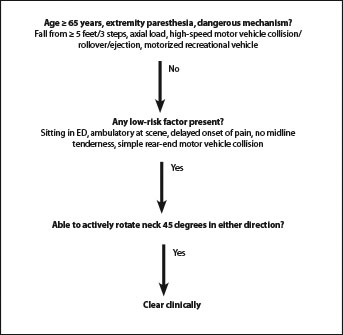
Radiographic Strategies for Spinal Clearance
Radiographic evaluation is often useful in the assessment of a patient with suspected spinal cord injury when clinical decision rules for clearing the spine are not applicable. Physicians in the ED can evaluate the cervical spine with plain films, CT scanning, or magnetic resonance imaging (MRI). Plain film evaluation has been shown to miss more than 50% of clinically significant cervical spine injuries and has a sensitivity of as low as 45%.25 The Eastern Association for the Surgery of Trauma (EAST) guidelines offer a level 2 recommendation that “Plain radiographs contribute no additional information and should not be obtained.”26 Although CT scanning represents a superior imaging modality, it may not be widely available across all urgent care settings. Furthermore, it is more challenging to justify the attendant risks of increased radiation exposure in the setting of a low-risk injury mechanism. This same paper states that MRI is indicated only in patients who have neurologic deficit attributable to a cervical spine injury, a population not included in eligibility for cervical spine clearance. There is new evidence available offering support for clearance of the cervical spine after CT alone, even in obtunded patients. A paper supported by EAST reports that “In obtunded adult blunt trauma patients, we conditionally recommend cervical collar removal after a negative high-quality C-spine CT scan result alone.”27 Although this method may prove more beneficial in the inpatient setting, it supports the ED physician tasked with the challenge of diagnosing injury in an unconscious patient. Indeed, the presence of a cervical collar has the potential to interfere with airway management and hinder vascular access techniques. However, it is important to recognize the limitations of the CT-only recommendation. The article requires a pristine CT with an axial thickness less than 3 mm and assumes over-reading by a trauma-trained radiologist.27
Management: Prehospital Cervical Spine Immobilization and Future Directions
“To date, the emergency care of trauma patients with suspected spinal injuries has been highly ritualized.”28 The biomechanical underpinnings of cervical spine immobilization have been called into question from data featured in two recent studies.28,29 Furthermore, a review article featured in the 2014 Journal of Neurotrauma acknowledges the relative paucity of data in support of the cervical collar.4 A summary of recent literature is essential to understanding evidence-based recommendations for prehospital immobilization.
The Engsberg study attempted to quantify the amount of head motion relative to torso motion during a simulated extrication. The authors used veteran prehospital providers and a realistic model of a crashed vehicle. Motion capture technology was applied to a human volunteer who acted as a patient. The mock-up vehicle was based on a 2001 Toyota Corolla that was totaled in a high-speed, head-on collision. The reconstructed “vehicle” attempted to replicate the actual barriers encountered during an extrication; restrictions imposed by a damaged dashboard and steering wheel had to be negotiated by the treatment team while minimizing spinal motion. Several different extrication scenarios were replicated. The “unassisted unprotected” scenario simply encouraged the patient to exit the vehicle without any assistance from treating providers. Yet another scenario instructed the patient to exit the vehicle following application of a cervical collar, and the final case used a Kendrick Extrication Device (KED) prior to securing the patient onto a standard, long spine board. Spinal motion was examined in three planes: flexion extension, lateral flexion, and rotation. A significantly higher degree of motion was observed in all planes of motion when the simulated driver exited the vehicle with the traditional, full-spinal immobilization strategy that incorporated the KED and a long spine board. The least amount of motion was observed when providers applied a cervical collar and permitted an unassisted exit from the car. At the very least, this article lends additional support for the need to review currently existing extrication strategies. The practice of permissive self-extrication is not routinely incorporated into EMS protocols and may deserve further consideration.
A similar study featured in a 2015 issue of the Emergency Medicine Journal shed additional light on cervical spine motion during the extrication process.28 Dixon’s study used a prehospital extrication crew of six to remove a human volunteer from a test vehicle. Unlike the reconstructed model featured in the Engsberg study, this simulation used a modified Ford Taurus automobile. A variety of extrication scenarios were tested, including the “unprotected” strategy of self-extrication. Although no immobilization devices or assistance was provided to the patient during the self-extrication scenario, the patient received specific instructions on how to minimize unnecessary movement. Not surprisingly, the authors found that the degree of spinal motion increased with the use of EMS extrication equipment. The control group, consisting of volunteers without a collar who were instructed to exit the vehicle, experienced the least amount of cervical motion. Also, the degree of motion varied in accordance with the volunteer patient’s height and mass. The Dixon article is consistent with the recent paradigm shift in prehospital spinal injury care. Routine backboard use is not likely to result in patient benefit, and EMS providers should implement protocols that restrict unnecessary movement. These treatment strategies might involve minimal assistance for cooperative patients and permit self-extrication except in circumstances of demonstrated neurologic deficit or altered consciousness.
In 2014, Sundstrom et al offered some controversial management recommendations in a comprehensive review article.4 This is an important piece of literature, as it is featured in a prominent neurosurgical journal and contradicts existing policy recommendations of surgical trauma societies. The authors compiled more than 50 journal entries relevant to the practice of prehospital spinal immobilization and the utilization of cervical collars. Similar to the re-evaluation of the backboard’s utility, Sundtrom’s article begins with a recitation of adverse effects linked to the application of the cervical collar. Pressure sores, patient discomfort, and airway management difficulty are magnified following collar application. Furthermore, collars can obviate identification of underlying injury such as an expanding vascular hematoma.
The paper also questions the consequences associated with injuries that are “missed,” or not immobilized, in the prehospital setting. Missed cervical spine injuries that present with neurologic disability are rare, even in the setting of trauma, and it is unclear whether the lack of cervical spine precautions worsens existing injury. Conscious patients have a tendency to maintain their neck in a position that will prevent worsening of muscle spasm, and “low-energy movements are … unlikely to cause secondary spinal cord injury.”4 Like other interventions in the emergency setting, a careful risk-benefit analysis is recommended to properly evaluate the effects of treatment. Sundstrom and colleagues cited data from non-immobilized trauma patients and proposed alternative mechanisms for the emergency treatment of secondary spinal cord injury. Indeed, neurologic sequelae are more likely to result from edema, inflammation, and injury biomechanics as opposed to the absence of a rigid collar. Although the authors acknowledge that “temporary use of a rigid collar is an option” during extrication, the article proposed that unconscious trauma patients might benefit from transport in a modified recovery position. Indeed, the reasons for routine use of the collar are rooted mostly in tradition and practice as opposed to data.
The high morbidity associated with injuries to the cervical spine often is used to justify the relatively low threshold for immobilization. As previously discussed, spinal protection interventions are not without harm and must be balanced against the potential for further injury. Medical directors and prehospital providers must acknowledge that the evidentiary basis for immobilization is relatively low. That said, it is entirely possible to articulate prehospital protocols that account for these pitfalls. Select EMS systems have demonstrated a relatively high compliance rate with protocols for cervical spine clearance. However, EMS systems vary widely according to region, and it is not always possible to guarantee a consistent level of education and training. Urban EMS systems are faced with the challenges of high call volume and comparatively less rigorous physician oversight. Rural EMS systems are forced to contend with lower volumes of traumatic injury and, thus, are tasked with maintaining skills. Selective spinal protection protocols represent one strategy for bridging any gaps that exist with respect to provider training. These protocols do not rely on specific neurologic findings and instead encourage application of immobilization to patients actually at risk for injury.
Despite decades of tradition and practice in emergency medical technician classrooms, the long spine board has not been shown to reduce morbidity or protect the cervical spine from further injury. The long spine board must be understood to be an extrication device and reserved for patients who require active assistance with movement or transportation. Patients should then be log-rolled or otherwise transitioned onto a soft mattress as soon as possible. The use of slide boards or other friction-reducing devices can facilitate transport from an EMS gurney to a hospital stretcher without the need for additional movement.
The recent collaborative position statement promulgated by the NAEMSP represents a synthesis of the best available evidence and offers some advice for management.30 It briefly reviews current literature and affirms that backboards should be used primarily as a device for patient extrication as opposed to transport. The more focused used of backboards represents a major change in both the culture and practice of prehospital medicine. For many years, spinal immobilization directly implied utilization of the long spine board. In the absence of an altered level of awareness, neurologic complaint, cardiac arrest, or demonstrated deficit, there is little imperative for their use. The NAEMSP position statement describes the stretcher as a “padded backboard” and therefore provides some of the theoretical protection without any of the attendant risks of pressure sores, pain, and restriction of respiratory motion. Ambulatory patients at risk for injury can be secured to the ambulance stretcher in a position of comfort and fitted with a cervical collar.13
Patients who present to EMS personnel and who exhibit an intact level of awareness and do not report neck pain may not benefit from inclusion into spinal protection protocols. As opposed to offering specific protocols that may vary by provider region, a “selective” approach to spinal immobilization identifies patients at risk for poor outcomes and encourages appropriate intervention. Further investigation is needed to determine if the practice of self-extrication can be applied to a broader population of injured patients.
Management: Cervical Spine Clearance in the ED
The abundance of recent evidence against immobilization equipment implies that fewer patients may be arriving via EMS secured to long spine boards and cervical immobilization devices. The absence of spinal protection devices does not imply freedom from injury, and emergency providers must exercise vigilance in the evaluation of the traumatically injured patient. For patients entering the ED who are secured to a long spine board, it is imperative to encourage removal from the board as soon as possible. Injuries linked to the rigid spine board are time-sensitive, and adverse effects have been documented in less than 30 minutes post application.31 Although the study by Berg et al was conducted on healthy patients, it confirmed the presence of compromised tissue oxygenation following spinal immobilization. When transport time is included in the calculation of a patient’s total immobilization time, it is possible for patients to remain strapped to a backboard in excess of 60 minutes.32 The 2000 study, featured in the American Journal of Emergency Medicine, noted that patients who required radiographic clearance of the spine remained on the backboard for an average of 181 minutes.33
Devices such as slide boards serve to minimize friction and to facilitate patient movement. It seems reasonable to encourage the process of “log rolling” for patients who are obtunded, who present with an impaired level of consciousness, or who have an abnormal neurologic examination. The accurate application of clinical decision rules represents a necessary first step in the assessment of such patients. Patients who do not fit into NEXUS or Canadian C-spine rule algorithms should undergo radiographic evaluation.
Emergency physicians have multiple tools at their disposal in the evaluation of suspected cervical spine injury, and the specific imaging strategy depends on the immediate availability of resources. Given the limitations inherent in plain film radiography, that modality should be reserved for patients who are deemed at low risk for injury. CT scan has emerged as the standard of care for the initial evaluation of the acutely traumatized patient. Furthermore, high-level trauma facilities that use multi-detector CT technology and incorporate trauma-trained radiologists have the potential to “clear” the spine of significant injury even in the absence of magnetic resonance technology. (See Figure 2.) However, this strategy remains controversial, and more robust data and unambiguous support from national organizations are lacking.
Figure 2. Suggested Algorithm for Cervical Spine Imaging
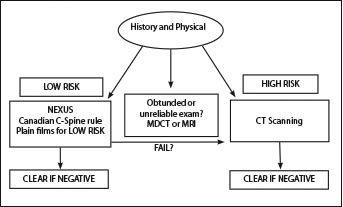
Pearls/Pitfalls
Providers should have comprehensive understanding of the potential benefits and risks in cervical spine immobilization when evaluating a patient with suspected cervical spine injury for potential clearance of the collar. The above clinical decision rules and radiographic imaging are all adjuncts to clinical exam, history, and physical and will aid in the ultimate clinical decision. A pitfall in the application of these clinical decision rules is to use two-tailed reasoning from a one-tailed test. Rules such as NEXUS and the Canadian C-spine rule can support a decision to remove a collar but do not provide useful information in ruling in a cervical spine injury. In cases in which the risk of maintaining cervical spine immobilization outweighs the potential benefit, a clinical decision is indicated. This is to say that if a lifesaving intervention is being delayed by a cervical collar’s placement and NEXUS and Canadian C-spine rule have not ruled out an injury, it is important to recognize that it has not confirmed an injury either. However, if the patient’s condition tolerates the placement of a cervical collar, a methodical and evidence-based approach should be taken in the clearance of the cervical collar. Clinical exam and gestalt alone cannot adequately evaluate for cervical spine injury, as up to 80% of confirmed cervical spine injuries can have a normal neurologic exam at the time of diagnosis.4
With the application of modern radiographic modalities and clinical decision rules, the rate of missed cervical spine injuries in the United States is extremely low (0.01%). Of the approximately 2% of injured persons found to have a cervical spine injury, only 1.3% are missed on initial screening and found in a delayed manner.34 This supports the notion that our current practices are effective in preventing secondary neurologic injury that is feared in blunt trauma patients. Emergency medicine physicians and other providers of trauma care should feel comfortable with the tools at their disposal to adequately address potential cervical spine injuries in the traumatically injured patient.
Pediatrics
There are several innate difficulties when evaluating a traumatically injured pediatric patient, including scarce data to support your decisions, difficulty in performing comprehensive physical exams with patient cooperation, difficulty and risks in obtaining radiographic studies, and the natural high stress involved with pediatric injuries. The pediatric patient requires a unique approach to the evaluation of a potentially injured cervical spine. First, the pathology of pediatric cervical spine injuries differs. In children younger than 12 years of age, the majority of cervical spine injuries occur at the C1-C2 level; however, complete cord injuries are more common in the lower cervical spine.35 There is also subset of cervical spine injury that occurs in both adults and children, but is more common in pediatric patients: spinal cord injury without radiographic abnormality (SCIWORA).23,35 SCIWORA is more common in younger patients, as subluxation joints are more lax and with more horizontal facet joints allowing for subluxation of the spine, causing injury to the spinal cord with return to normal anatomy of the vertebrae by the time of radiographic evaluation.23 In radiographic evaluation of the pediatric patient, there is concern for increased radiation burden, as well as the possible need for sedation to obtain desired studies. With both anatomic differences in pediatrics and the varying pathology of the injury, a tailored approach should be implemented in the clearance of the pediatric cervical spine.
Viccellio performed a prospective study to evaluate the effectiveness of applying NEXUS criteria to trauma patients younger than 18 years of age. This study found that NEXUS can be effective in the pediatric population and its use could reduce pediatric cervical spine imaging by nearly 20%;23 however, the data were primarily in patients older than 8 years of age, who are arguably similar to adults both anatomically and in terms of ability to obtain an adequate physical exam. Of the few patients younger than 8 years of age in the study, even fewer had cervical spine injuries, and none of the patients younger than 2 years of age had a cervical spine injury. This lack of pathology in the pediatric patients limits the usefulness of the conclusions in clinical practice when applied to patients younger than 8 years old.
There are promising data from a 2009 study in the Journal of Trauma that focuses on pediatric patients younger than 3 years of age.36 This study retrospectively evaluated 12,537 blunt trauma patients younger than 3 years of age and found cervical spine injuries in 83 patients (0.66%). Their goal was to apply a clinical rule to identify these injuries using four independent predictors: GCS < 14, GCS eye score of 1, motor vehicle collision, and patient 2 years of age or older. Each item was given 1 point if present and a score of less than 2 had a negative predictor value of 99.93% in ruling out cervical spine injury.36 These are promising results in a cohort of patients in which all patients were imaged; however, this was a retrospective review and has not been prospectively validated.
Most recently, Hale et al looked at this younger cohort in a study to assess the reliability of clinical findings in children younger than 5 years of age in excluding unstable cervical spine injuries.37 This study retrospectively looked at almost 3,000 patients admitted to a Level I trauma center with blunt injury, of which 22 (0.74%) had confirmed cervical spine injuries. The authors concluded that cervical spine CT can be reserved for symptomatic patients to reduce radiation exposure to the thyroid. This conclusion was supported by the fact that all patients with cervical spine injury had clinical findings suggestive of or diagnostic for cervical spine injury: abnormal neurologic examination, torticollis, and neck pain.37
CONCLUSION
Cervical spine clearance and management remain contentious topics, especially in the realm of prehospital medical care. The significant morbidity of secondary neurologic injuries must be considered against the real risks of full spine immobilization. Although there is no clear evidence supporting effectiveness of full spine immobilization, it remains a mainstay in current EMS systems. The risks and benefits of spinal immobilization should be applied on an individual basis, as there is no support for a “one size fits all approach” to spinal protection. EMS systems must work toward re-imagination of the long spine board as a device that can facilitate extrication. Although the backboard may have utility as a patient movement device, the associated risks and lack of benefit encourage its removal from routine spinal protection protocols. Accordingly, the cervical collar is viewed as a low-risk intervention, but that, too, is not without inherent problems. Increased difficulty with intubation and delayed identification of traumatic neck injuries warrant careful consideration of the cervical collar’s use.
ED management of cervical spine injuries must incorporate principles of early liberation from spinal immobilization devices and a nuanced understanding of clinical decision rules. Patients arriving to the ED secured to a spine board are more likely to undergo unnecessary radiologic testing and are at risk for harm from pressure sores and respiratory motion restriction. Rules for spine clearance have demonstrated benefit and identify patients who will need further investigation. Finally, technological advances in the area of radiologic evaluation have the potential to reduce delays in injury identification. High-definition multi-detector CT scanning, coupled with specialty radiologic expertise, can identify subtle injuries and obviate the need for potentially more expensive and time-consuming tools such as magnetic resonance imaging.
REFERENCES
- Nawar EW, Niska RW, Xu J. National Hospital Ambulatory Medical Care Survey: 2005 emergency department summary. Adv Data 2007;(386):1-32.
- Hadley MN, Walters BC, Grabb P, et al. Guidelines for the management of acute cervical spine and spinal cord injuries. Clin Neurosurg 2002;49:407-498.
- Hasler RM, Exadaktylos AK, Bouamra O, et al. Epidemiology and predictors of spinal injury in adult major trauma patients: European cohort study. Eur Spine J 2011;20:2174-2180.
- Sundstrøm T, Asbjørnsen H, Habiba S, et al. Prehospital use of cervical collars in trauma patients: A critical review. J Neurotrauma 2014;31:531-540.
- Stiell IG, Clement CM, McKnight RD, et al. The Canadian C-spine rule versus the NEXUS low-risk criteria in patients with trauma. N Engl J Med 2003;349:2510-2518.
- Bulger EM, Maier R V. Prehospital care of the injured: What’s new. Surg Clin North Am 2007;87:37-53.
- Del Rossi G, Heffernan TP, Horodyski M, et al. The effectiveness of extrication collars tested during the execution of spine-board transfer techniques. Spine J 2004;4:619-623.
- Kolb JC, Summers RL, Galli RL. Cervical collar-induced changes in intracranial pressure. Am J Emerg Med 1999;17:135-137.
- Mobbs RJ, Stoodley MA, Fuller J. Effect of cervical hard collar on intracranial pressure after head injury. ANZ J Surg 2002;72:389-391.
- Paterek E, Isenberg DL, Salinski E, et al. Characteristics of trauma patients overimmobilized by prehospital providers. Am J Emerg Med 2015;33:121-122.
- Chan D, Goldberg R, Tascone A, et al. The effect of spinal immobilization on healthy volunteers. Ann Emerg Med 1994;23:48-51.
- Vaillancourt C, Stiell IG, Beaudoin T, et al. The out-of-hospital validation of the Canadian C-Spine Rule by paramedics. Ann Emerg Med 2009;54:663-671.
- White CC, Domeier RM, Millin MG. EMS spinal precautions and the use of the long backboard — resource document to the position statement of the National Association of EMS Physicians and the American College of Surgeons Committee on Trauma. Prehosp Emerg Care 2014;18:306-314.
- National Association of EMS Physicians. EMS Spinal Precautions and the Use of the Long Backboard. Prehospital Emerg Care 2013;17:392-392.
- Maryland Institute for Emergency Medical Services Systems. 2015 Protocols — Complete Manual. Maryl Med Protoc Emerg Med Serv Provid 2015:334.
- Gonzalez RP, Fried PO, Bukhalo M, et al. Role of clinical examination in screening for blunt cervical spine injury. J Am Coll Surg 1999;189:152-157.
- Stroh G, Braude D. Can an out-of-hospital cervical spine clearance protocol identify all patients with injuries? An argument for selective immobilization. Ann Emerg Med 2001;37:609-615.
- Totten VY, Sugarman DB. Respiratory effects of spinal immobilization. Prehospital Emerg Care 1999;3:347-352.
- Cordell WH, Hollingsworth JC, Olinger ML, et al. Pain and tissue-interface pressures during spine-board immobilization. Ann Emerg Med 1995;26:31-36.
- Hong R, Meenan M, Prince E, et al. Comparison of three prehospital cervical spine protocols for missed injuries. West J Emerg Med 2014;15:471-479.
- Theodore N, Hadley MN, Aarabi B, et al. Prehospital cervical spinal immobilization after trauma. Neurosurgery 2013;72:22-34.
- Michaleff ZA, Maher CG, Verhagen AP, et al. Accuracy of the Canadian C-spine rule and NEXUS to screen for clinically important cervical spine injury in patients following blunt trauma: A systematic review. Can Med Assoc J 2012;184:867-876.
- Viccellio P, Simon H, Pressman BD, et al. A prospective multicenter study of cervical spine injury in children. Pediatrics 2001;108:E20.
- Hoffman JR, Wolfson AB, Todd K, et al. Selective cervical spine radiography in blunt trauma: Methodology of the National Emergency X-Radiography Utilization Study (NEXUS). Ann Emerg Med 1998;32:461-469.
- Mathen R, Inaba K, Munera F, et al. Prospective evaluation of multislice computed tomography versus plain radiographic cervical spine clearance in trauma patients. J Trauma Inj Infect Crit Care 2007;62:1427-1431.
- Como JJ, Diaz JJ, Dunham CM, et al. Practice management guidelines for identification of cervical spine injuries following trauma: Update from the Eastern Association for the Surgery of Trauma Practice Management Guidelines Committee. J Trauma 2009;67:651-659.
- Raza M, Elkhodair S, Zaheer A, et al. Safe cervical spine clearance in adult obtunded blunt trauma patients on the basis of a normal multidetector CT scan — a meta-analysis and cohort study. Injury 2013;44:1589-1595.
- Dixon M, O’Halloran J, Cummins N. Biomechanical analysis of spinal immobilisation during prehospital extrication: A proof of concept study. Emerg Med J 2014;31:745-749.
- Engsberg JR, Standeven JW, Shurtleff TL, et al. Cervical spine motion during extrication. J Emerg Med 2013;44:122-127.
- White CC 4th, Domeier RM, Millin MG; Standards and Clinical Practice Committee, National Association of EMS Physicians. EMS spinal precautions and the use of the long backboard — resource document to the position statement of the National Association of EMS Physicians and the American College of Surgeons Committee on Trauma. Prehosp Emerg Care 2014;18:306-314.
- Berg G, Nyberg S, Harrison P, et al. Near-infrared spectroscopy measurement of sacral tissue oxygen saturation in healthy volunteers immobilized on rigid spine boards. Prehosp Emerg Care 2010;14:419-424.
- Lerner EB, Moscati R. Duration of patient immobilization in the ED. Am J Emerg Med 2000;18:28-30.
- Lerner EB, Moscati R. Duration of patient immobilization in the ED. Am J Emerg Med 2000;18:28-30.
- Grossman MD, Reilly PM, Gillett T, et al. National survey of the incidence of cervical spine injury and approach to cervical spine clearance in U.S. trauma centers. J Trauma 1999;47:684-690.
- Brown RL, Brunn MA, Garcia VF. Cervical spine injuries in children: A review of 103 patients treated consecutively at a level 1 pediatric trauma center. J Pediatr Surg 2001;36:1107-1114.
- Pieretti-Vanmarcke R, Velmahos GC, Nance ML, et al. Clinical clearance of the cervical spine in blunt trauma patients younger than 3 years: A multi-center study of the American Association for the Surgery of Trauma. J Trauma 2009;67:543-550.
- Hale DF, Fitzpatrick CM, Doski JJ, et al. Absence of clinical findings reliably excludes unstable cervical spine injuries in children 5 years or younger. J Trauma Acute Care Surg 2015;78:943-948.
The initial evaluation and management of patients with potential spinal injuries in emergency medicine practice is in evolution. The authors thoughtfully explore the evidence available and its limitations.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
