Melatonin and Chemotherapy: A Review
By Traci Pantuso, ND, MS
Adjunct Faculty, Bastyr University, Seattle; Owner Naturopathic Doctor Harbor Integrative Medicine, Bellingham, WA
Dr. Pantuso reports no financial relationships relevant to this field of study.
SUMMARY POINTS
- Melatonin is a popular supplement, with 3.1 million adults in the United States reporting use.
- Melatonin produces pleiotropic effects throughout the body that are not fully elucidated, and its role in cancer prevention or as an adjunctive treatment in oncology patients is not well defined.
- Melatonin used in research may be difficult to extrapolate to clinical use.
Recently, melatonin and its potential benefits in cancer and chemotherapy have been discussed in varying publications from the Lancet Oncology to the Huffington Post.1,2 Melatonin is best known for its role in the sleep-wake cycle and is a popular supplement used to promote sleep and decrease symptoms of jet lag.1-3 The National Health Interview Survey (NHIS) conducted in 2012 reported an estimated 1.3% of the U.S. adult population (3.1 million American adults) used melatonin in the last 30 days.3 The NHIS survey also concluded that the use of melatonin has more than doubled since 2007.3 Unfortunately, the reason for the use of natural supplements was beyond the scope of this survey.3 With the increased use of melatonin in the adult population, it is unclear how many individuals may be using it to promote sleep or for other health reasons such as an adjunctive therapy in cancer treatment.
Background
Melatonin (N-acetyl-5-methoxytryptamine) is an indolic compound that is synthesized from the amino acid tryptophan in the pineal gland; it was identified first in 1958 by Aaron Lerner’s group.4,5,6 (See Figure 1.) The pineal gland is the major producer of melatonin; however, other tissues, such as the gastrointestinal tract, retina, and bone marrow,5 have been shown to produce melatonin. The pineal gland secretes melatonin in response to the suprachiasmatic nucleus (SCN), which is synchronized to the light-dark cycle in the environment by detection of light by the retina. The SCN is described as acting as the master clock in the body that sets all of the peripheral tissue clocks. The pineal gland produces and secretes melatonin at night, which is reflected in the higher concentration of melatonin in the blood stream during the night and early morning hours and lower levels during the day.5 There is individual variation in the synthesis and secretion of melatonin, with low secretors having peak serum levels at night ranging from 18-40 pg/mL and high secretors from 54-75 pg/mL.5,6
The sleep-enhancing effects and circadian rhythm regulation are attributed to the signaling pathways that are activated with the binding of melatonin to the melatonin receptors. The melatonin receptors are the MT1 (Mel 1a) and MT2 (Mel 1b) receptors, which are expressed in the central nervous system and in the peripheral tissues.7 Melatonin also binds to nuclear and cytoplasmic receptors and intracellular proteins that are involved in cytoskeletal rearrangement and estrogen signaling pathways.7 In addition to the downstream effects from melatonin binding to the receptors, it is also a powerful antioxidant that scavenges both reactive oxygen and nitrogen species.8,9
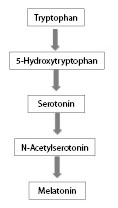
Figure 1: Biosynthesis of Melatonin |
 |
|
ADAPTED FROM: Vijayalaxmi, Thomas CR Jr, Reiter RJ, Herman TS. Melatonin: From basic research to cancer treatment clinics. J Clin Oncol 2002;20:2575-2601. |
Anticancer Effects
The anticancer effects of melatonin have yet to be fully elucidated in humans.5,6 In vitro studies have demonstrated that melatonin has many effects on the cell cycle, including inducing apoptosis and up-regulating p53 and p21 (tumor proteins) in cancer cell lines.8,9 Melatonin also has demonstrated inhibition of VEGF and HiF1α expression in cell lines supporting an antiangiogenic effect.5,6,8,9 In advanced cancer patients, melatonin supplementation decreased VEGF serum concentrations.9
Numerous immune-enhancing effects, including increased activity of natural killer cells, T cells, and B cells, and increased cytokine production, have been reported.5-9 In breast cancer cell lines, melatonin has demonstrated antiestrogenic effects, which occur through the MT1 receptor.7-9
Antioxidant Effects
As a free radical scavenger, melatonin may be able to decrease chemotherapy-induced toxicity. However, alkylating and platinum-based chemotherapeutic drugs exert anticancer effects through increasing free radicals in the body; antioxidants potentially could decrease the efficacy of these drugs.10,11 Yasueda et al conducted a recent systematic review (though no meta-analysis) investigating the efficacy and interactions of antioxidant supplements, including melatonin, as adjuvant therapy in cancer treatment.11 They concluded that more research is needed to further understand the effects of antioxidants in cancer patients and to determine the risks and benefits associated with use.11
Clinical Evidence
Two recent meta-analyses investigating the efficacy and safety of melatonin use in cancer patients undergoing chemotherapy demonstrated benefit.12,13 These two meta-analyses overlapped in the clinical trials they investigated. Seely et al included 21 clinical trials in 19 studies and Wang et al included eight of those same studies.12,13 The 11 studies (13 clinical trials) not included by Wang et al did not meet the selection criteria defined in the methods.12 The majority of the studies included in both meta-analyses were conducted by Lissoni et al. Wang et al included eight randomized, controlled trials, six of which were performed by Lissoni et al. In the Seely et al meta-analysis, 18 of the 21 studies were conducted by Lissoni et al. Both authors concluded that the general quality of the studies was poor overall, as many of the studies were not blinded, the randomization method was unclear, and there was often a lack of placebo arms.12,13
In the Wang et al meta-analysis, data from the eight randomized, controlled trials were pooled, comparing participants receiving 20 mg of melatonin with chemotherapy and/or radiotherapy to participants receiving conventional therapy alone.12 Complete and partial remission rates were 32.6% in the melatonin group compared to 16.5% in the conventional therapy alone group (P < 0.00001).12 Wang et al also reported a one-year survival rate of 52.2% in the melatonin group vs. 28.4% in the control group (P < 0.001).12 The relative risk (RR) reported was 1.90 (95% confidence interval [CI], 1.28-2.83; P = 0.001; I2 = 61.9%).12
Seely et al pooled data comparing conventional treatment with and without adjuvant melatonin and reported an RR for one-year mortality of 0.63 (95% CI, 0.53-0.74; P ≤ 0.001; I2 = 78%).13
In 2005, Mills et al published a systematic review and meta-analysis investigating the use of melatonin (ranging 20-40 mg) in participants with various solid tumor cancers from 10 research studies performed by Lissoni et al.14 The melatonin treatment group demonstrated reduced mortality risk at one year with a pooled RR of 0.66 (95% CI, 0.59-0.73; P ≤ 0.0001; I2 = 0%).14 There were no reports of serious adverse events mentioned in any of the studies.11-14
In summary, the majority of the studies used in the above meta-analyses were conducted by Lissoni et al and have not been replicated in double-blind, placebo-controlled, randomized, controlled trials performed by other research groups.1,11-14
Melatonin Purity, Sourcing, and Pharmacodynamics
Many of the studies included in the above meta-analysis were conducted in Europe, where melatonin is a prescribed medication rather than a supplement. It is unclear from the studies which melatonin product was used and whether it was analyzed for purity prior to its use in the studies. In the United States, melatonin is sold as an over-the-counter supplement and made synthetically.
Labdoor, a company that tests supplements for label accuracy, product purity, nutritional value, ingredient safety, and projected efficacy, tested 30 melatonin supplements.15 Labdoor found that nine out of the 30 melatonin products deviated off label claims by at least 20%.15 One product tested contained < 1% of the label claim for melatonin and another product tested contained 47.4% more than the product’s label claimed.15 Fifteen of the 30 melatonin products were within 10% of their label claims.15 Two of the products’ arsenic levels were higher than California Proposition 65 levels of 0.1 mcg/day of inorganic arsenic levels.15
Oral melatonin reaches its peak plasma levels in the human body in 60-150 minutes and has a serum half-life of approximately 20-30 minutes. The bioavailability of oral melatonin ranges from 10-56%. Serum melatonin undergoes extensive first-pass metabolism, with 90% being cleared by the liver through the cytochrome p450 enzymes. The metabolites of melatonin are excreted into the urine.5,6
A wide range of melatonin dosages are recommended for sleep. A research group at Massachusetts Institute for Technology found that 0.3 mg of melatonin was the optimal dose for sleep in adults.16 The researchers found that adults who took more melatonin reported feeling drowsy during the day, which they attributed to melatonin being present in the blood at higher levels than normal during the daylight hours.5,16 There is no recommended dose for melatonin in cancer patients; however, research studies have used a dosage of 20-40 mg of melatonin once daily in the evening.11-13
Side Effects/Interactions
No serious side effects were reported in the above meta-analysis studies. Melatonin is considered safe; however, there have been documented cases of small decreases in body temperature with oral administration.5 Drowsiness is a common side effect of melatonin that may occur the following day after administration and may be due to doses in the higher ranges.5,16-19
Interactions
Since melatonin is processed by the CYP450 pathway (isoenzymes CYP1A2, CYP1A1, and CYP1B1) in the liver, it is reasonable to assume that melatonin may interfere with the blood concentration of other drugs that use the same pathway. For example, caution is warranted with the coadministration of warfarin, which also uses the CYP1A2 isoenzyme.5,6,16
Conclusion
Melatonin is best known for its role in regulation of sleep and the circadian rhythm.1-6 Melatonin has demonstrated anticancer activities in basic science and animal studies that are promising for future studies.5-14 Although the RR improvements reported by the meta-analyses and the original research investigators are promising, other research groups have not verified them independently, and the study methodologies also are not of high quality. The mechanisms of action of melatonin also need to be fully elucidated so that research investigating safety, efficacy, and drug interactions can be further determined.
Individual cancer types that have demonstrated benefit with melatonin supplementation include breast cancer and non-small cell lung cancer.8,11-14 Malignant tumors of the same cancer type are heterogeneous in their protein expression and are under investigation.20 Melatonin produces pleiotropic effects that appear to be the result of numerous interactions with different receptors and proteins that need to be better defined to predict which cancer types and treatments would benefit. Further research with human participants that is both methodologically sound and conducted by more than one research group is required to be able to recommend high doses of melatonin to oncology patients. Another important issue to address to effectively use melatonin in clinical practice in the United States is to have available a standardized melatonin supplement that is free of heavy metals. Further understanding into the low and high melatonin secretors also is required, as there may be a wide range of dosage depending on individual variation, which could affect efficacy in oncology patients.
Although 20-40 mg doses of melatonin appear safe from the body of research investigating the effects of melatonin in oncology patients, it may not be efficacious. More research is needed to be able to determine whether adjunctive treatment with melatonin is beneficial to oncology patients in high doses.
REFERENCES
- Pinato DJ, Stebbing J. Melatonin: Resetting the clock of cancer progression? Lancet Oncol 2016;1:23-24.
- Chen J. Is melatonin more than just a sleep supplement. The Huffington Post Jan. 1, 2016.
- Clarke TC, Black LI, Stussman BJ, et al. Trends in the use of complementary health approaches among adults: United States, 2002–2012. National Health Statistics Reports; no 79. Hyattsville, MD: National Center for Health Statistics. 2015.
- Lerner AB, Case JD, Takahashi Y, et al. Isolation of melatonin, the pineal factor that lightens melanocytes. J Am Chem Soc 1958;80:2587.
- Srinivasan V, Spence DW, Pandi-Perumal SR, et al. Therapeutic actions of melatonin in cancer: Possible mechanisms. Integr Cancer Ther 2008;7:189-203.
- Vijayalaxmi, Thomas CR Jr, Reiter RJ, Herman TS. Melatonin: From basic research to cancer treatment clinics. J Clin Oncol 2002;20:2575-2601.
- Pandi-Perumal SR, Trakht I, Srinivasan V, et al. Physiological effects of melatonin: Role of melatonin receptors and signal transduction pathways. Prog Neurobiol 2008;85:335-353.
- Hill SM, Frasch T, Xiang S, et al. Molecular mechanisms of melatonin anticancer effects. Integr Cancer Ther 2009;8:337-346.
- Sanchez-Barcelo EJ, Mediavilla MD, Alonso-Gonzalez C, Reiter RJ. Melatonin uses in oncology: Breast cancer prevention and reduction of the side effects of chemotherapy and radiation. Expert Opin Investig Drugs 2012;21:819-831.
- Karbownik M, Lewinski A, Reiter RJ. Anticarcinogenic actions of melatonin which involve antioxidative processes: Comparison with other antioxidants. Int J Biochem Cell Biol 2001;33:735-753.
- Yasueda A, Urushima H, Ito T. Efficacy and interaction of antioxidant supplements as adjuvant therapy in cancer treatment: A systematic review. Integr Cancer Ther 2016;15:17-39.
- Wang YM, Jin BZ, Ai F, et al. The efficacy and safety of melatonin in concurrent chemotherapy or radiotherapy for solid tumors: A meta-analysis of randomized controlled trials. Cancer Chemother Pharmacol 2012;69:1213-1220.
- Seely D, Wu P, Fritz H, et al. Melatonin as adjuvant cancer care with and without chemotherapy: A systematic review and meta-analysis of randomized trials. Integr Cancer Ther 2012;11:293-303.
- Mills E, Wu P, Seely D, Guyatt G. Melatonin in the treatment of cancer: A systematic review of randomized controlled trials and meta-analysis. J Pineal Res 2005;39:360-366.
- Labddor. Top 10 Melatonin Supplements. Available at: https://labdoor.com/rankings/melatonin. Accessed Nov. 17, 2016.
- Zhdanova IV, Wurtman RJ, Morabito C, et al. Effects of low oral dose of melatonin, given 2-4 hours before habitual bedtime, on sleep in normal young humans. Sleep 1996;19:423-431.
- Auger RR, Burgess HJ, Emens JS, et al. Clinical Practice Guideline for the Treatment of Intrinsic Circadian Rhythm Sleep-Wake Disorders: Advanced Sleep-Wake Phase Disorder (ASWPD), Delayed Sleep-Wake Phase Disorder (DSWPD), Non-24-Hour Sleep-Wake Rhythm Disorder (N24SWD), and Irregular Sleep-Wake Rhythm Disorder (ISWRd). An Update for 2015. J Clin Sleep Med 2015;11:1199-1236.
- Dollins AB, Zhdanova IV, Wurtman RJ, et al. Effect of inducing nocturnal serum melatonin concentrations in daytime on sleep, mood, body temperature, and performance. Proc Natl Acad Sci U S A 1994;91:1824-1828.
- Dollins AB, Lynch HJ, Wurtman RJ, et al. Effect of pharmacological daytime doses of melatonin on human mood and performance. Psychopharmacology (Berl) 1993;112:490-496.
- Sun XX, Yu Q. Intra-tumor heterogeneity of cancer cells and its implications for cancer treatment. Acta Pharmacol Sin 2015;36:1219-1227.
Recently, melatonin and its potential benefits in cancer and chemotherapy have been discussed in varying publications. However, it is unclear how many individuals may be using it to promote sleep or for other health reasons such as an adjunctive therapy in cancer treatment.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
