Common Pediatric Upper Extremity Overuse Injuries
January 1, 2017
Reprints
AUTHORS
Daniel Migliaccio, MD, Resident Director of Undergraduate Medical Education, Stanford/Kaiser Emergency Medicine Residency Program, Stanford, CA
N. Ewen Wang, MD, Associate Professor, Emergency Medicine; Associate Director, Pediatric Emergency Medicine, Stanford School of Medicine, Stanford, CA
PEER REVIEWER
Jeffrey Bullard-Berent, MD, FAAP, FACEP, Medical Director, Child Ready Virtual Pediatric Emergency Department, Professor Emergency Medicine and Pediatrics, University of New Mexico School of Medicine, Albuquerque
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, we disclose that Dr. Dietrich (editor), Dr. Skrainka (CME question reviewer), Ms. Wurster (nurse planner), Dr. Migliaccio (author), Dr. Wang (author), Dr. Bullard-Berent (peer reviewer), Ms. Coplin (executive editor), and Ms. Mark (executive editor) report no relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- The physis contains germinal cells whose proliferation leads to longitudinal growth. This area is particularly susceptible to injury during growth spurts, and acute injury may alter the growth of the bone. If subject to chronic loading with intense activity, the physis can develop chronic disruptions of bone proliferation and blood supply, which even may lead to avascular necrosis.
- The apophysis is subject to repetitive tensile forces and is the most common location for overuse injury (apophysitis) and/or avulsion fractures. However, an injury to the apophyses does not disrupt skeletal growth (as opposed to physeal injuries), and has a favorable prognosis/recovery.
- Little league shoulder is largely a clinical diagnosis used to describe an overuse injury of the proximal humerus in overhead athletes with skeletally immature bone caused by repetitive forces and microtrauma from the overhead motion.
- Medial epicondylar apophysitis, or little league elbow, affects young throwing athletes and usually presents with progressive pain and focal tenderness over the medial epicondyle.
- A patient with bilateral or unilateral vague wrist pain with tenderness over the radial joint in the correct historical context (adolescent gymnast) may have distal radial epiphysitis or “gymnast wrist.”
Pediatric overuse injuries are becoming very common as the intensity of athletic competition extends to our younger population. Acute care providers must include these injuries in their differential as they listen to and examine young athletes. Identification and coordination of care with a sports medicine expert will optimize the long-term outcomes for these children.
— Ann M. Dietrich, MD, FAAP, FACEP, Editor
Musculoskeletal pain accounts for approximately 20% of the pediatric visits to emergency departments (EDs).1 Approximately half of these visits are related to overuse injuries from sports. 2 Although acute injuries are well-described in the emergency medicine literature, pediatric overuse injuries are less commonly addressed. This article reviews upper extremity overuse injuries, and will discuss diagnosis of overuse pediatric upper extremity injuries that present to the ED, appropriate ED management for these injuries, and appropriate follow-up and discharge instructions.
Etiology
It is estimated that more than 60 million children are involved in organized sports yearly,3 with an increasing expectation of extremely competitive performance. To keep up with these expectations, young athletes are undertaking intense training regimens with decreased rest periods between bouts of exercise or sport. In this setting, overuse injuries are increasing. It is believed that repetitive stress injuries account for approximately 2 million injuries annually.4,5 Since these numbers do not include those athletes who continue to play despite injury, this is most likely an underestimate.6
Sports with an emphasis on use of the upper extremities, such as baseball, tennis, swimming, and gymnastics, predispose youth athletes to upper extremity injuries. Historically, risk factors have been classified as “intrinsic” or “extrinsic.”7 Intrinsic risk factors include anatomic and growth characteristics, level of conditioning, and susceptibility of the growing cartilage to repetitive stress. In contrast, extrinsic factors include training, quantity/technique of an action, equipment, and environment. The most studied example of an extrinsic risk factor involves youth baseball pitchers and correlates the number of pitches being thrown to risk of injury.8
It is important to have knowledge of the skeletal system of the immature athlete to understand pediatric upper extremity pathophysiology. This skeletal immaturity makes young athletes susceptible to a unique set of overuse injuries not seen in the adult population. For example, overhand sports predispose the apophysis to repetitive microtrauma and can lead to an apophysitis, such as little league elbow. On the other hand, inflammation of tendons (or tendinitis) is less frequently encountered in the pediatric population. Both pathologies are managed similarly in the ED, with the exception that some cases of apophysitis may benefit from splinting. Also, sports medicine follow-up is indicated for the pediatric population to identify inciting causes and help prevent further morbidity. In contrast, tendinitis in adults initially can be managed by primary care.
Pediatric bone consists of the physis, or growth plate, which is situated between the metaphapysis and epiphysis. The physis contains germinal cells whose proliferation leads to longitudinal growth. This area is particularly susceptible to injury during growth spurts, and acute injury may alter the growth of the bone. If subject to chronic loading with intense activity, the physis can develop chronic disruptions of bone proliferation and blood supply, which even may lead to avascular necrosis.9 The apophysis or the site at which muscle tendons insert into skeletally immature bone is subject to repetitive tensile forces and is the most common location for overuse injury (apophysitis) and/or avulsion fractures.10 In general, an injury to the apophyses does not disrupt skeletal growth (as opposed to physeal injuries), and has a favorable prognosis and recovery.
General Approach
Patients with overuse injuries generally will come to the ED with a high degree of anxiety; for example, they may have pain that has been ongoing and has not improved or that has worsened just before an impending game or competition, or they may have an acute exacerbation of a chronic smoldering pain. For the diagnosis of an overuse injury in the ED, as with any other diagnosis, performing a thorough history and physical exam is crucial. Important historical features to gather from the patient, family, and coaches involve quality, location, radiation, onset, timing, association with activity/sport, mitigating and exacerbating factors, as well as any associated symptoms that may lead the provider to consider a more concerning diagnosis other than overuse injury. For example, weight loss and night sweats may point toward a malignancy, whereas fevers may indicate a septic joint or systemic disease.
The physical exam should focus on palpation, both active and passive range of motion, and/or lymph node exam of the affected area, as well as surrounding joints and structures. The area of pain and neighboring joints, muscles, and anatomic structures (such as the anatomic snuff box in wrist injuries) should be examined and evaluated for any pain, swelling, or change in range of motion. Specific exam maneuvers will be discussed with individual disease processes below. Ancillary tests will change depending on presenting symptoms and physician differential, but in the ED tests most likely will include plain radiographs to assess for fracture.11 In most circumstances, if further imaging is required (e.g., magnetic resonance imaging [MRI]), it can be done as an outpatient. In general, the management of overuse injuries includes avoidance of the inciting activity as well as movements/exercises that exacerbate the pain, strategic icing, and anti-inflammatory medications such as nonsteroidal anti-inflammatory drugs (NSAIDs). Tylenol also may help in the acute immediate setting for pain. Splinting, even in the setting of no occult fracture detected on imaging, is beneficial for pain control in a majority of the injuries discussed below.
The use of intra-articular injections of steroids for pediatric upper extremity overuse injuries has not been well studied and should not be performed routinely in the ED. These patients will need a personalized plan for re-introduction to their respective sport, which preferably would be dictated by a sports medicine physician, athletic trainer, or physical therapist. Given the increasing youth participation in organized sports, there will be a sense of anxiety among the young athletes, parents, and coaches to return to sport.
With all injuries discussed, it is necessary to have a rest period of a minimum of 2-3 weeks to sometimes months (depending on the extent of injury), during which the athlete does not participate in the inciting activity until assessed by a sports medicine specialist. It is important to stress that other physical activities that do not involve the upper extremities still may be done safely (i.e., lower extremity weight training and cardiovascular activities like jogging and biking) prior to seeing the sports medicine specialist or physical therapist. Although there are no definitive guidelines for return to sport for overuse injuries (as there are for concussions), the American Academy of Pediatrics strongly encourages prevention techniques, such as having 1-2 days off per week and 2-3 months per year from any one sport, and minimizing sport specialization (i.e., participating in solely one sport the entire year) until adolescence (mid-teen years when most of epiphyseal growth has occurred).12 A failure to undergo adequate recovery and rest in any of the following pathologies may lead to chronic musculoskeletal pain, decreased range of motion, and reduced functionality of the joint involved.3
Overuse Injuries by Presenting Symptoms
See Table 1 for a summary of characteristic patient presentations, pediatric overuse injury, and treatment.
Table 1. Common Associations Between Patient Characteristics and Pediatric Overuse Injuries |
|||
|
Patient Presentation |
Pediatric Overuse Injury |
Treatment |
Prognosis |
|
Teenage male baseball player or swimmer with gradual onset of pain over the lateral aspect of the proximal humerus that occurs with throwing and overhead activities |
Proximal humeral epiphysitis (little league shoulder) |
Conservative, rest, ice, elevation to decrease discomfort |
Good (Return to full play in weeks to months) |
|
Pre-teen male participating in overhead sports with poorly localized ache of the shoulder |
Rotator cuff tendonitis or multidirectional instability (also with associated subjective feeling of shoulder subluxation) |
Conservative |
Good |
|
Teenage overhead athlete with insidious onset pain/ swelling of the medial elbow and/or decreased range of motion in extension |
Medial epicondylar apophysitis (little league elbow), medial epicondylar avulsion, and/or a sprain or tear of the ulnar collateral ligament |
Conservative, immobilization, or operative (failed conservative or complete tears with functional loss) |
Good |
|
Pre-teen male with no history of sport participation with insidious onset lateral elbow pain |
Panner's disease, osteochondrosis of the capitellum |
Conservative, immobilization |
Good |
|
Teen overhead athlete with insidious onset lateral elbow pain |
Osteochondritis dissecans |
Conservative, immobilization, operative if loose bodies/fragments present |
Medium (many patients go on to have elbow pain indefinitely) |
|
Teen swimmer with sub-acute progressively worsening posterior elbow pain |
Olecranon apophysitis or olecranon stress fracture |
Conservative, immobilization |
Good |
|
Teen gymnast with bilateral or unilateral vague wrist pain with tenderness over the radial joint |
Distal radial epiphysitis (gymnast wrist) |
Conservative, immobilization |
Medium (pain may return commonly) |
|
Teen rock climber who presents with pain and swelling to a particular digit |
Salter-Harris type III fracture of base of the middle phalanx (climber’s finger) |
Conservative, immobilization |
Good |
|
Teen with atraumatic medial thumb pain with no evidence of infection or rash |
Flexor pollicis longus tendonitis (texter’s thumb) |
Conservative, immobilization |
Good |
|
Teen skier with thumb pain |
Ulnar collateral ligament rupture of the thumb metacarpophalangeal joint (gamekeeper’s thumb) |
Conservative, immobilization |
Good |
|
Source: Author created. |
|||
Shoulder
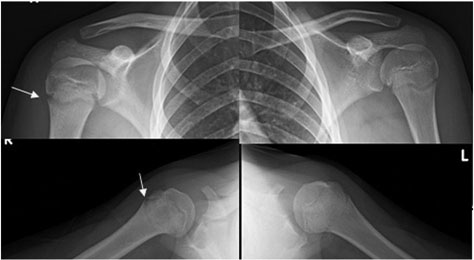
Approximately 15% of all pediatric musculoskeletal complaints presenting to the ED involve upper extremity, and nearly half of these injuries (45%) involve the upper extremity. A major risk factor for subacute, or acute on chronic, shoulder issues presenting to the ED is participation in overhand sports.13 One study looking at 476 baseball pitchers aged 9-14 years found that more than one-third (35%) noted shoulder pain in a single season.14 Similarly, the shoulder is the third most common location of injury among pediatric tennis athletes and the most common site of injury in wrestlers.15,16 Obtaining the underlying diagnosis may be difficult in the ED. The emergency physician should be attuned to certain clues from the history and physical exam that may assist with making a correct diagnosis. For example, a patient presenting with a gradual onset of pain over the lateral aspect of the proximal humerus that occurs with throwing and overhead activities is a classic presentation for proximal humeral epiphysitis or “little league shoulder.”17 Little league shoulder is largely a clinical diagnosis used to describe an overuse injury of the proximal humerus in overhead athletes with skeletally immature bone caused by repetitive forces and microtrauma from the overhead motion. It is seen most commonly in baseball players but can affect any athlete with increased overhead activity, including gymnasts, swimmers, and tennis players. It occurs predominately in males between ages 11-16 years, during the peak growth spurt of the proximal humeral physis.18 Extrinsic risk factors include improper biomechanics (throwing, for example) and frequent bouts of overhead activity without adequate rest.19 Physical examination may be normal (30%) or demonstrate tenderness over the proximal and lateral aspect of the humerus (70%).17 Radiographic findings may include widening, sclerosis, and irregularity of the humeral physis.13 (See Figure 1.) However, in many cases, radiographs may be normal and the diagnosis should be considered based on the classic history.20 Treatment of little league shoulder consists of avoiding the overhead motion until pain has resolved (approximately 2-3 months).21 A personalized strengthening and return to sport program is beneficial, as is adherence to sport specific guidelines, such as that of the USA Baseball Medical & Safety Advisory Committee and the American Academy of Pediatrics (AAP) to prevent recurrence.22
Figure 1. Little League Shoulder Radiographs |
|
AP and axillary radiographs demonstrate widening of right proximal humeral physis (arrows) in a 12-year-old athlete with right shoulder pain. Normal contralateral (left) shoulder presented for comparison.
|
|
Reprinted with permission: Paz DA, Chang GH, Yetto JM, Jr., et al. Upper extremity overuse injuries in pediatric athletes: Clinical presentation, imaging findings, and treatment. Clin Imaging 2015;39:954-964. |
Patients presenting with a dull, poorly localized ache in the proximity of the shoulder may have rotator cuff tendinitis. Although rare in the pediatric population, it may occur in the setting of multidirectional instability. Rotator cuff tendinitis develops from overuse and inflammation in one or more of the rotator cuff muscles (supraspinatus, infraspinatus, teres minor, subscapularis), and predisposes pediatric patients to complete rotator cuff tears. Provocative exams, which illicit pain and/or weakness include the empty can test and lift-off test. The empty can test, which tests the supraspinatus, is performed by having patients abduct the shoulders to 90 degrees in forward flexion with the thumbs pointing downward and having the patients attempt to elevate their arms against examiner resistance. Subscapularis function is assessed with the lift-off test, or having the patients place the dorsum of their hand on their lumbar back and having them attempt to move their hand off the back. Lastly, injury to the infraspinatus and/or teres minor, which contribute to the external rotation of the shoulder, is examined with patients flexing both elbows to 90 degrees and having the examiner provide resistance against external rotation. Although rotator cuff tendinitis is a clinical diagnosis, plain radiography in the ED is indicated to detect avulsion fractures of the lesser tuberosity of the humerus (the insertion point of most rotator cuff tendons). Outpatient MRI may be indicated if a complete tear is suspected, and may guide surgical intervention. In general, the treatment of rotator cuff tendinitis involves rest, ice, NSAIDs, and sports medicine and physical therapy follow-up for proper evaluation of biomechanics. Surgery may be indicated in complete and sometimes partial tears of the rotator cuff, and treatment modality depends largely on patient/provider preference.23 Tendinitis and partial tears of the rotator cuff may lead to decreased stability of the shoulder joint and predispose the patient to complete tears and shoulder dislocations if not properly rehabilitated with a strength and conditioning program.
Similarly, those patients presenting with dull shoulder pain also may describe recurrent shoulder subluxations with sports and activities of daily living. This may suggest to the emergency physician a diagnosis of atraumatic instability of the glenohumeral joint, or multidirectional instability. Multidirectional instability involves a laxity within the glenohumeral joint and leads to hypermobility and decreased stability of the shoulder joint.24 When it becomes symptomatic, multidirectional instability causes a generalized shoulder pain in pediatric patients who participate in overhead activities. Symptomatic multidirectional instability can be evaluated by the apprehension test. If affected, while having their arm in the abducted and externally rotated position, passive stressing of the shoulder into further external rotation will cause a subjective feeling of subluxation and create “apprehension” in the patient.25 Plain films usually are normal, and outpatient MRI is useful only to evaluate for rotator cuff or labral tears. Multidirectional instability can predispose pediatric patients to rotator cuff tendinitis and tears.
Initially, therapy for multidirectional instability is conservative with NSAIDs, rest, and ice. If strengthening-based physical therapy programs fail, surgical correction of the instability may be pursued.26
Shoulder pain is prevalent among pediatric swimmers (25%) and is commonly referred to as “swimmer’s shoulder.” Swimmer’s shoulder has significant overlap with little league shoulder, multidirectional instability, and rotator cuff tendinitis, and is diagnosed and treated as discussed for these conditions.27
With an acute presentation for any of these shoulder injuries described, intermittent icing (10 minutes on/10 minutes off strategy to help prevent ice burns and skin irritation) is recommended for the first 24-48 hours, after which heat may be applied to increase blood flow to the area of injury. A sling may be provided for initial comfort; however, early mobility with simple range-of-motion exercises is key to prevent functional range of motion loss within the limitations of the patient's pain. Prognosis is favorable in each of these shoulder pathologies if patients get adequate rest and follow a proper rehabilitation program.18
Elbow
Children presenting with elbow pain comprise roughly 10% of all ED visits for pediatric musculoskeletal complaints.1 Similar to shoulder complaints, throwing sports are associated with the highest incidence of elbow pain.28 Approximately 70% of Little League and adolescent baseball players (ages 7-19 years) report elbow pain at some point in their lifetime.29 A similar percentage is seen in tennis players (50%).16 Anatomic stability of the elbow is provided by flexor/pronator muscles and in a large part by the ulnar collateral ligament (UCL), all of which insert on the medial epicondyle.30 Repetitive valgus stress on the immature elbow predisposes the pediatric population to injuries of/near these structures.31 Patients who present to the ED with pain and swelling of the medial elbow and/or decreased range of motion in extension may have medial epicondylar apophysitis (little league elbow), medial epicondylar avulsion, and/or a sprain or tear of the ulnar collateral ligament.
Medial epicondylar apophysitis, or little league elbow, affects young throwing athletes and usually presents with progressive pain and focal tenderness over the medial epicondyle. Little league elbow is a clinical diagnosis with characteristic exam and historical features, as radiographs are normal more than 90% of the time.32 Plain radiographs are useful for detecting avulsion fractures of the medial epicondyle. In the absence of a fracture, little league elbow is treated with immobilization with an elbow brace or long arm splint (see Figure 2), and NSAIDs. Orthopedic/sports medicine follow-up and activity cessation are important considerations, as well as a guided return to sport program (approximately 4-12 weeks). Epicondylar avulsion fractures with 5-15 mm of displacement are treated nonoperatively, with a long arm splint for immobilization in the acute setting and orthopedic follow-up.33 In the evaluation of a suspected avulsion fracture, the ED physician must examine the ulnar nerve for signs and symptoms of entrapment, as fractures affecting the nerve usually are treated surgically.34
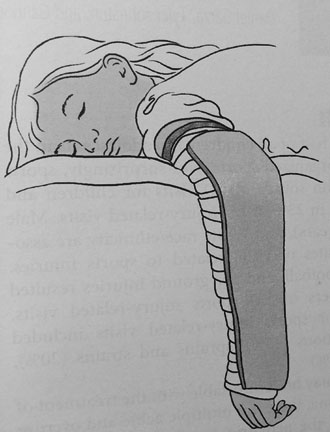
Figure 2. Long Arm Splint |
 |
|
Reprinted with permission: N. Ewen Wang, MD. |
Tears of the ulnar collateral ligament present similarly with pain over the medial elbow, but also may have associated valgus instability in flexion and extension compared to the contralateral side. Plain films of the elbow usually are normal. Although there is no indication for emergent MRI in the ED, dynamic bedside ultrasound may be used as an adjunct to detect a complete ulnar collateral ligament tear.35 In patients with a suspected tear, splinting in a long arm splint and orthopedic follow up is necessary. Ultimately, nonoperative vs. operative treatment for complete and partial tears depends on the patient, surgeon, and level of competition. 36 Tommy John surgery, or ulnar collateral ligament reconstruction, remains a highly controversial topic in the baseball world as it is highly sought out. Outcomes of surgery are variable, with most patients recovering completely and returning to pre-injury strength. Recovery time for ulnar collateral ligament injuries is roughly 3-4 months.
Patients presenting to the ED with subacute progressively worsening posterior elbow pain in the setting of repetitive elbow extension (as in swimming/throwing) may have olecranon apophysitis or stress fracture. Physical exam usually reveals local tenderness and swelling over the olecranon. A thorough physical exam of the elbow always should include palpation of the olecranon. Provocative physical exam maneuvers include the snapping extension test. After ruling out an occult fracture with plain radiographs, the snap extension test involves a forceful extension of a flexed forearm. Reproduction of pain in the posterior elbow is a positive finding.37 Plain radiography may reveal widening of the physis compared with the contralateral elbow and/or bony fragments/sclerosis of the olecranon.38 (See Figure 3.) Initial treatment in the ED involves long arm splinting (see Figure 2) to decrease tensile extension forces on the olecranon, rest, ice, NSAIDs, and orthopedic follow-up. Some patients with olecranon stress fractures refractory to conservative treatment eventually may undergo operative repair. Although some orthopedic specialists recommend vitamin D to patients with stress fractures secondary to the association of low serum vitamin D levels with stress fractures, there is no evidence of causation, and prophylactic supra-therapeutic vitamin D supplementation should be avoided.39
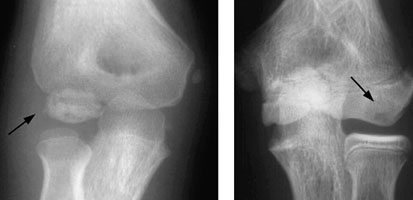
Figure 3. Olecranon Apophysitis |
|
AP radiographs with the elbow in 45° of flexion demonstrating fragments (A) and sclerosis of the olecranon (B) (arrows)
|
|
Reprinted with permission: Matsuura T, Kashiwaguchi S, Iwase T, et al. The value of using radiographic criteria for the treatment of persistent symptomatic olecranon physis in adolescent throwing athletes. Am J Sports Med 2010;38:141-145. |
Insidious onset of lateral elbow pain presenting in the dominant arm of children/adolescents may represent osteochondrosis of the humeral capitellum (Panner’s disease) or osteochondritis dissecans of the capitellum. Panner’s disease (osteochondrosis) describes an abnormal ossification and necrosis of the capitellum, a condition only found in the pediatric population.40 Panner’s disease is a self-limiting disease with resolution of symptoms in most patients. Patients with Panner’s disease are usually boys younger than 10 years of age who have had several weeks of pain and stiffness in the lateral elbow, without a history of trauma or overuse.41 Although some argue that Panner’s disease and osteochondritis are on the same continuum, there is no evidence that having one condition is a predisposition to the other.42 Radiographs of patients with Panner’s disease typically demonstrate fissuring and/or fragmentation of the entire capitellum.43 (See Figure 4.) Initial management is conservative, with many studies citing benefit in temporary immobilization with a long arm splint for pain control.41
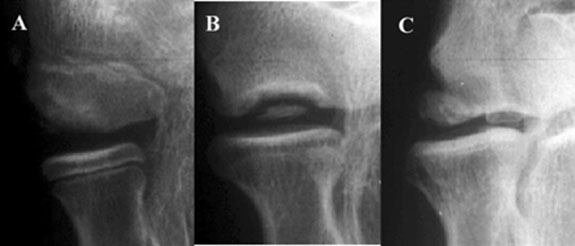
Figure 4. Radiographic Findings in Panner’s Disease |
|
Translucency in humeral capitellum (A), nondisplaced fragments (B), loose bodies and sclerotic change (C).
|
|
Reprinted with permission: Matsuura T, Kashiwaguchi S, Iwase T, et al. Conservative treatment for osteochondrosis of the humeral capitellum. Am J Sports Med 2008;36:868-872. |
On the other hand, osteochondritis dissecans is an inflammation of the osteochondral articular surface and usually affects the dominant arm in adolescent athletes. In osteochondritis dissecans, patients also complain of lateral elbow pain but, in addition, may report a sensation of locking and catching. In both conditions, physical examination usually reveals tenderness to the lateral elbow over the capitellum and loss of extension. Plain radiographs of the affected elbow as well as of the contralateral elbow for comparison should be obtained if one is concerned for Panner’s disease or osteochondritis dissecans. In osteochondritis dissecans, radiographs can demonstrate rarefaction (or radiolucency) of the lateral capitellum, with loose bodies being seen in advanced stages.44 (See Figure 5.) Initial treatment of osteochondritis dissecans involves immobilization in a long arm splint or elbow brace, rest, NSAIDs, and orthopedic referral.45 Operative and non-surgical management largely depends on the stability of the fragmented lesion as well as the presence of loose bodies.46,47 Prognosis and functional outcomes for patients with osteochondritis dissecans are largely dependent on the severity of the lesion, but many patients will go on to have lateral elbow pain indefinitely. 45
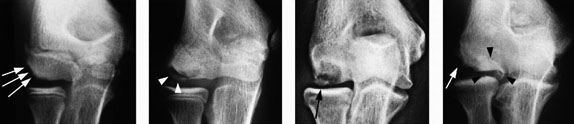
Figure 5. Osteochondritis Dissecans |
|
AP radiographs obtained with the elbow in 45° of flexion demonstrating localized subchondral bone flattening without fragments (arrows) (A) and nondisplaced bone fragments (arrowheads) (B). C, AP radiograph demonstrating a displaced fragment (arrow). D, AP radiograph demonstrating a loose fragment (arrowheads) and a bone defect (arrow).
|
|
Reprinted, with permission, from Radiology 2000;216:207-212. © RSNA. |
Wrist
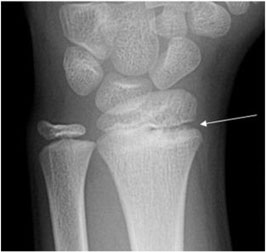
Although acute wrist injuries commonly are encountered in the ED, chronic/subacute wrist pain visits are rising. Up to 80% of youth athletes participating in sports will have wrist pain.50 Gymnasts, in particular, who undergo chronic repetitive extension and axial compression of the wrist, are prone to wrist pain and injury.31 Differential diagnosis of wrist pain in children should always include acute/subacute fractures (i.e., of the scaphoid, hook of hamate), stress fractures, and septic arthritis in the correct clinical context.51 However, a patient with bilateral or unilateral vague wrist pain with tenderness over the radial joint in the correct historical context (adolescent gymnast) may have distal radial epiphysitis or “gymnast wrist.” Typically, the patient with distal radial epiphysitis endorses dorsal wrist pain with extension and axial loading (as on the balance beams).52 Physical exam demonstrates tenderness over the dorsal radius to palpation and pain reproduced by wrist extension and axial loading (table push-off).53 Radiographs demonstrate widening of the distal radius physis (compared to unaffected wrist) in 75% of patients with distal radial epiphysitis.54,55 (See Figure 6.) Treatment is supportive, with rest, ice, NSAIDs, and cessation of activity until symptoms are resolved. Immbolization with a volar splint helps to prevent excessive extension of the wrist, which improves pain.51,56
Figure 6. Gymnast Wrist |
|
Frontal radiograph demonstrates mild physeal widening (arrow) of the distal radius with metaphyseal irregularity in a 12-year-old female gymnast
|
|
Reprinted, with permission, from RadioGraphics 2016;36:1672-1687. © RSNA. |
Fingers
Injuries to the phalanges are common in the ED. Although most visits involve acute fractures/lacerations of the phalanges, there is an increasing prevalence of stress fractures and tendinitis. A rock climber who presents with pain and swelling to a particular digit may have “climber’s finger.”57 The repetitive phalangeal flexion and extension in climbing can lead to climber’s finger or subacute Salter-Harris type III stress fractures at the base of the middle phalanx.58,59 (See Figure 7.) Radiographs are used to confirm the diagnosis, and initial treatment is with splinting with either a radial or ulnar gutter splint, depending on which digit is affected (gutter splints provide more stability than aluminum finger splints), and urgent (within 5-7 days) orthopedic follow-up.60
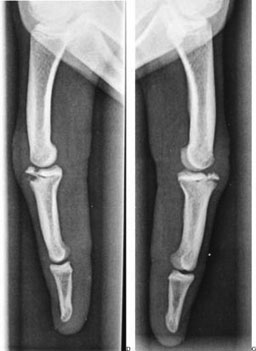
Figure 7. Dorsal Bilateral Fracture |
|
Displaced dorsal bilateral fracture of the base of the middle phalanx and the middle fingers
|
|
Reprinted with permission: Chell J, Stevens K, Preston B, Davis TR. Bilateral fractures of the middle phalanx of the middle finger in an adolescent climber. Am J Sports Med 1999;27:817-819. |
Atraumatic thumb pain in a healthy, well-appearing adolescent may be suggestive of flexor pollicis longus tendinitis or “texter’s thumb.” Physical exam will reveal tenderness along the medial aspect at the base of the first phalanx, long extensor, and abductor pollicis tendons. Treatment is supportive, and patients may benefit from a thumb spica splint for comfort and to prevent them from further irritating the tendon.
Avid pediatric skiers presenting with thumb pain after chronic or acute valgus directed force to the thumb (holding skiing poles while skiing) may have ulnar collateral ligament of the thumb metacarpophalangeal (MCP) joint partial or complete rupture, or “gamekeeper’s thumb.” Physical exam may demonstrate valgus laxity of the thumb MCP joint as compared to the unaffected hand. Plain imaging is useful for detecting avulsions at the base of the thumb MCP joint.61 Emergency management with or without fracture is the same and includes conservative treatment with NSAIDs, icing, splinting in a thumb spica splint for MCP immobilization, and orthopedic follow-up. Surgery may be indicated for severe laxity. Prognosis is favorable for both surgical and conservative management.61
CONCLUSION
Emergency physicians frequently are challenged to determine the etiology of a variety of musculoskeletal processes in children, including overuse injuries. The intensity of sports competitions and the need to return the child to play as quickly as possible both contribute to the need for acute care providers to be proficient in the recognition and management of children with overuse injuries. The emergency physician frequently encounters less emergent and chronic health issues. In this same light, appropriate follow-up with a sports specialist or physical therapist may be delayed, and it is crucial to be a patient advocate and help coordinate a feasible follow-up plan. Although the differential diagnosis for emergent pediatric musculoskeletal complaints is broad, red flags must be identified and overuse injuries must be considered. The emergency physician should focus on important historical and clinical clues to help prevent further morbidity and long-lasting musculoskeletal issues in this young vulnerable population. Challenges to proper diagnosis include a lack of insight into the activities that led to injury, difficulty in obtaining a “textbook” history in children/their families, lack of familiarity with specific examination techniques, and difficulty in interpreting sometimes-subtle radiological findings.63 Most overuse injuries will require conservative treatment and generally will improve with cessation of the inciting activity. However, without recognition and identification of the stressor, continued use can lead to further injury and even growth disruptions.64 The article presented describes common upper extremity overuse injuries in the pediatric population.
REFERENCES
- de Inocencio J, Carro MA, Flores M, et al. Epidemiology of musculoskeletal pain in a pediatric emergency department. Rheumatol Int 2016;36:83-89.
- Clarsen B, Myklebust G, Bahr R. Development and validation of a new method for the registration of overuse injuries in sports injury epidemiology: The Oslo Sports Trauma Research Centre (OSTRC) overuse injury questionnaire. Br J Sports Med 2013;47:495-502.
- Fabricant PD, Lakomkin N, Sugimoto D, et al. Youth sports specialization and musculoskeletal injury: A systematic review of the literature. Phys Sportsmed 2016;44:257-262.
- Stracciolini A, Casciano R, Friedman HL, et al. A closer look at overuse injuries in the pediatric athlete. Clin J Sport Med 2015;25:30-35.
- Luke A, Lazaro RM, Bergeron MF, et al. Sports-related injuries in youth athletes: Is overscheduling a risk factor? Clin J Sport Med 2011;21:307-314.
- Yang J, Tibbetts AS, Covassin T, et al. Epidemiology of overuse and acute injuries among competitive collegiate athletes. J Athl Train 2012;47:198-204.
- DiFiori JP, Benjamin HJ, Brenner JS, et al. Overuse injuries and burnout in youth sports: A position statement from the American Medical Society for Sports Medicine. Br J Sports Med 2014;48:287-288.
- Olsen SJ, Fleisig GS, Dun S, et al. Risk factors for shoulder and elbow injuries in adolescent baseball pitchers. Am J Sport Med 2006;34:905-912.
- Bedoya MA, Jaramillo D, Chauvin NA. Overuse injuries in children. Top Magn Reson Imaging 2015;24:67-81.
- Amieva-Wang NE. A Practical Guide to Pediatric Emergency Medicine: Caring for Children in the Emergency Department. Cambridge; New York: Cambridge University Press; 2011.
- Lomasney LM, Lim-Dunham JE, Cappello T, Annes J. Imaging of the pediatric athlete: Use and overuse. Radiol Clin North Am 2013;51215-226.
- Brenner JS, Council On Sports Medicine and Fitness. Sports specialization and intensive training in young athletes. Pediatrics 2016;138(3): pii: e20162148. doi: 10.1542/peds.2016-2148.
- Paz DA, Chang GH, Yetto JM, Jr., et al. Upper extremity overuse injuries in pediatric athletes: Clinical presentation, imaging findings, and treatment. Clin Imaging 2015;39:954-964.
- Lyman S, Fleisig GS, Waterbor JW, et al. Longitudinal study of elbow and shoulder pain in youth baseball pitchers. Med Sci Sport Exer 2001;33:1803-1810.
- Yard EE, Collins CL, Dick RW, Comstock RD. An epidemiologic comparison of high school and college wrestling injuries. Am J Sports Med 2008;36:57-64.
- Hjelm N, Werner S, Renstrom P. Injury profile in junior tennis players: A prospective two-year study. Knee Surg Sport Traumatol Arthrosc 2010;18:845-850.
- Osbahr DC, Kim HJ, Dugas JR. Little league shoulder. Curr Opin Pediatr 2010;22:35-40.
- Lazaro LE, Cordasco FA. Physical exam of the adolescent shoulder: Tips for evaluating and diagnosing common shoulder disorders in the adolescent athlete. Curr Opin Pediatr 2016 [Epub ahead of print].
- Chen FS, Diaz VA, Loebenberg M, Rosen JE. Shoulder and elbow injuries in the skeletally immature athlete. J Am Acad Orthop Surg 2005;13:172-185.
- May MM, Bishop JY. Shoulder injuries in young athletes. Pediatr Radiol 2013;43(Suppl 1):S135-140.
- Heyworth BE, Kramer DE, Martin DJ, et al. Trends in the presentation, management, and outcomes of little league shoulder. Am J Sports Med 2016;44:1431-1438.
- Rice SG, Congeni JA, Council on Sports Medicine and Fitness. Baseball and softball. Pediatrics 2012;129:e842-856.
- Weiss JM, Arkader A, Wells LM, Ganley TJ. Rotator cuff injuries in adolescent athletes. J Pediatr Orthop B 2013;22:133-137.
- Johansson K. Multidirectional instability of the glenohumeral joint: An unstable classification resulting in uncertain evidence-based practice. Br J Sports Med 2016;50:1105-1106.
- Longo UG, Rizzello G, Loppini M, et al. Multidirectional instability of the shoulder: A systematic review. Arthroscopy 2015;31:2431-2443.
- Warby SA, Pizzari T, Ford JJ, et al. Exercise-based management versus surgery for multidirectional instability of the glenohumeral joint: A systematic review. Br J Sports Med 2016;50:1115-1123.
- Matzkin E, Suslavich K, Wes D. Swimmer’s shoulder: Painful shoulder in the competitive swimmer. J Am Acad Orthop Surg 2016;24:527-536.
- Makhni EC, Jegede KA, Ahmad CS. Pediatric elbow injuries in athletes. Sports Med Arthrosc 2014;22:e16-24.
- Magra M, Caine D, Maffulli N. A review of epidemiology of paediatric elbow injuries in sports. Sports Med 2007;37:717-735.
- Bryce CD, Armstrong AD. Anatomy and biomechanics of the elbow. Orthop Clin North Am 2008;39:141-154, v.
- Ellington MD, Edmonds EW. Pediatric elbow and wrist pathology related to sports participation. Orthop Clin North Am 2016;47:743-748.
- Braithwaite KA, Marshall KW. The skeletally immature and newly mature throwing athlete. Radiol Clin North Am 2016;54:841-855.
- Osbahr DC, Chalmers PN, Frank JS, et al. Acute, avulsion fractures of the medial epicondyle while throwing in youth baseball players: A variant of Little League elbow. J Shoulder Elbow Surg 2010;19:951-957.
- Louahem DM, Bourelle S, Buscayret F, et al. Displaced medial epicondyle fractures of the humerus: Surgical treatment and results. A report of 139 cases. Arch Orthop Trauma Surg 2010;130:649-655.
- Wood N, Konin JG, Nofsinger C. Diagnosis of an ulnar collateral ligament tear using musculoskeletal ultrasound in a collegiate baseball pitcher: A case report. N Am J Sports Phys Ther 2010;5:227-233.
- Ford GM, Genuario J, Kinkartz J, et al. Return-to-play outcomes in professional baseball players after medial ulnar collateral ligament injuries: Comparison of operative versus nonoperative treatment based on magnetic resonance imaging findings. Am J Sports Med 2016;44:723-728.
- Greiwe RM, Saifi C, Ahmad CS. Pediatric sports elbow injuries. Clin Sports Med 2010;29:677-703.
- Matsuura T, Kashiwaguchi S, Iwase T, et al. The value of using radiographic criteria for the treatment of persistent symptomatic olecranon physis in adolescent throwing athletes. Am J Sports Med 2010;38:141-145.
- Miller JR, Dunn KW, Ciliberti LJ, Jr., et al. Association of vitamin D with stress fractures: A retrospective cohort study. J Foot Ankle Surg 2016;55:117-120.
- Atanda A, Jr., Shah SA, O’Brien K. Osteochondrosis: Common causes of pain in growing bones. Am Fam Physician 2011;83:285-291.
- Claessen FM, Louwerens JK, Doornberg JN, et al. Panner’s disease: Literature review and treatment recommendations. J Child Orthop 2015;9:9-17.
- Akkaya N, Dogu B, Unlu Z, et al. Ultrasonographic evaluation of the flexor pollicis longus tendon in frequent mobile phone texters. Am J Phys Med Rehabil 2015;94:444-448.
- Bancroft LW, Pettis C, Wasyliw C, Varich L. Osteochondral lesions of the elbow. Semin Musculoskelet Radiol 2013;17:446-454.
- Smucny M, Kolmodin J, Saluan P. Shoulder and elbow injuries in the adolescent athlete. Sports Med Arthrosc 2016;24:188-194.
- Churchill RW, Munoz J, Ahmad CS. Osteochondritis dissecans of the elbow. Curr Rev Musculoskelet Med 2016;9:232-239.
- Takahara M, Mura N, Sasaki J, et al. Classification, treatment, and outcome of osteochondritis dissecans of the humeral capitellum. J Bone Joint Surg Am 2007;89:1205-1214.
- Mihara K, Tsutsui H, Nishinaka N, Yamaguchi K. Nonoperative treatment for osteochondritis dissecans of the capitellum. Am J Sports Med 2009;37298-304.
- Matsuura T, Kashiwaguchi S, Iwase T, et al. Conservative treatment for osteochondrosis of the humeral capitellum. Am J Sports Med 2008;36:868-872.
- Takahara M, Ogino T, Takagi M, et al. Natural progression of osteochondritis dissecans of the humeral capitellum: Initial observations. Radiology 2000;216:207-212.
- Jonasson P, Halldin K, Karlsson J, et al. Prevalence of joint-related pain in the extremities and spine in five groups of top athletes. Knee Surg Sports Traumatol Arthrosc 2011;19:1540-1546.
- Chawla A, Wiesler ER. Nonspecific wrist pain in gymnasts and cheerleaders. Clin Sports Med 2015;34:143-149.
- Poletto ED, Pollock AN. Radial epiphysitis (aka gymnast wrist). Pediatr Emerg Care 2012;28:484-485.
- Webb BG, Rettig LA. Gymnastic wrist injuries. Curr Sports Med Rep 2008;7:289-295.
- Delgado J, Jaramillo D, Chauvin NA. Imaging the injured pediatric athlete: Upper extremity. Radiographics 2016;36:1672-1687.
- Swischuk LE. Musculoskeletal: What’s different in children? Follow-up for sinusitis visit: And oh, could you check her left wrist—it hurts. Emerg Radiol 2015;22(Suppl 1):7-8.
- Frush TJ, Lindenfeld TN. Peri-epiphyseal and overuse injuries in adolescent athletes. Sports Health 2009;1:201-211.
- Yamaguchi T, Ikuta Y. Climber’s finger. Hand Surg 2007;12:59-65.
- Chell J, Stevens K, Preston B, Davis TR. Bilateral fractures of the middle phalanx of the middle finger in an adolescent climber. Am J Sports Med 1999;27:817-819.
- Hochholzer T, Schoffl VR. Epiphyseal fractures of the finger middle joints in young sport climbers. Wilderness Environ Med 2005;16:139-142.
- Desaldeleer AS, Le Nen D. Bilateral fracture of the base of the middle phalanx in a climber: Literature review and a case report. Orthop Traumatol Surg Res 2016;102:409-411.
- Ritting AW, Baldwin PC, Rodner CM. Ulnar collateral ligament injury of the thumb metacarpophalangeal joint. Clin J Sport Med 2010;20:106-112.
- Farion KJ, Wright M, Zemek R, et al. Understanding low-acuity visits to the pediatric emergency department. PLoS One 2015;10:e0128927.
- Jaimes C, Jimenez M, Shabshin N, et al. Taking the stress out of evaluating stress injuries in children. Radiographics 2012;3:537-555.
- Tisano BK, Estes AR. Overuse injuries of the pediatric and adolescent throwing athlete. Med Sci Sports Exerc 2016;48:1898-1905.
Pediatric overuse injuries are becoming very common as the intensity of athletic competition extends to our younger population. Acute care providers must include these injuries in their differential as they listen to and examine young athletes. Identification and coordination of care with a sports medicine expert will optimize the long-term outcomes for these children.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.