Should This Patient Be Cardioverted?
The lead II rhythm strip shown in the figure below was obtained from an older adult patient on telemetry. Should the patient be immediately cardioverted?
Although at first glance, this tracing prompted much concern on the telemetry unit, prompt cardioversion is not the optimal initial intervention. Instead, there is much baseline aberration with spurious-looking complexes that occur at a rate of more than 300/minute in parts of the tracing. No real tachyarrhythmia exhibits a ventricular rate this fast in adults.
The first thing to do when confronted with a potentially worrisome tracing such as this is to check the patient. Doing so revealed that the patient was coughing vigorously at the time this tracing was recorded. The artifact totally disappeared as soon as the patient stopped coughing.
Artifact is common in clinical practice. At times, it may be extremely difficult to distinguish artifact from a real tracing. The consequences of mistaking artifact for ventricular tachycardia (as was almost done for the tracing in the figure) are not trivial. Patients have been shocked, and investigative procedures (such as cardiac catheterization) have been ordered. Remember the following:
Check on the patient first. If the patient is alert and hemodynamically stable, then the rhythm is far less likely to be ventricular tachycardia.
The most likely causes of artifact simulating ventricular tachycardia are inconsistent skin-electrode contact and body movement (scratching, tremor, shivering, coughing, hiccups, brushing teeth, writhing in bed, interference from a mechanical device, etc.).
ECG features that suggest artifact as the cause include geometric appearance (unphysiologic vertical deflections) that are unpredictably irregular, often at exceedingly rapid rates. On a 12-lead tracing, one often inexplicably sees highly unusual deflections in some leads, but not in others. Identifying an underlying regular rhythm that is undisturbed by artifactual deflections provides proof that the phenomenon is not real.
For further discussion about this case, please visit: http://bit.ly/2jT37f4.
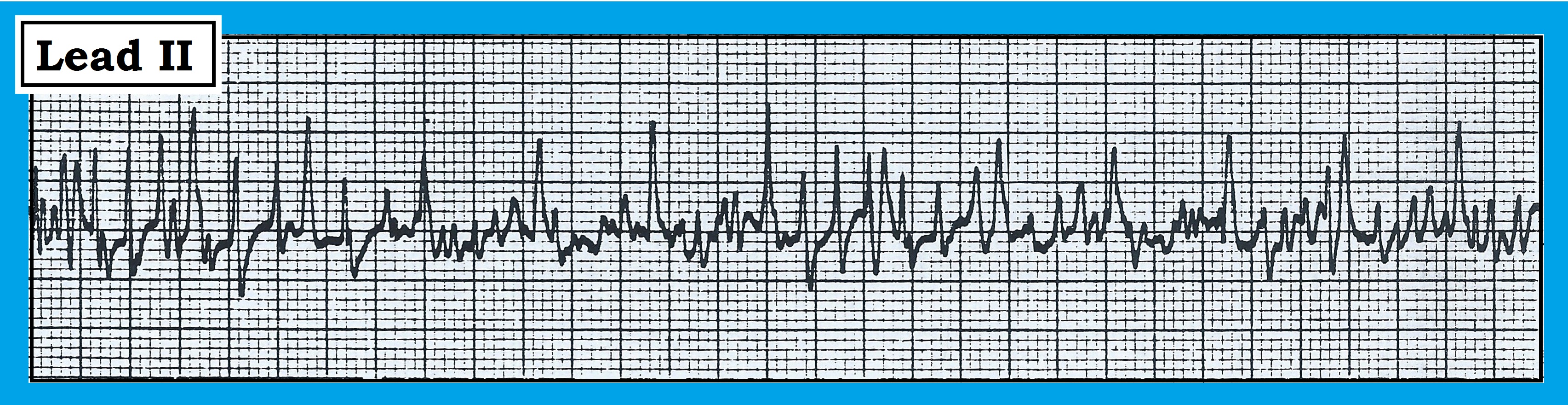
The lead II rhythm strip shown in the figure in this article was obtained from an older adult patient on telemetry. Should the patient be immediately cardioverted?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
