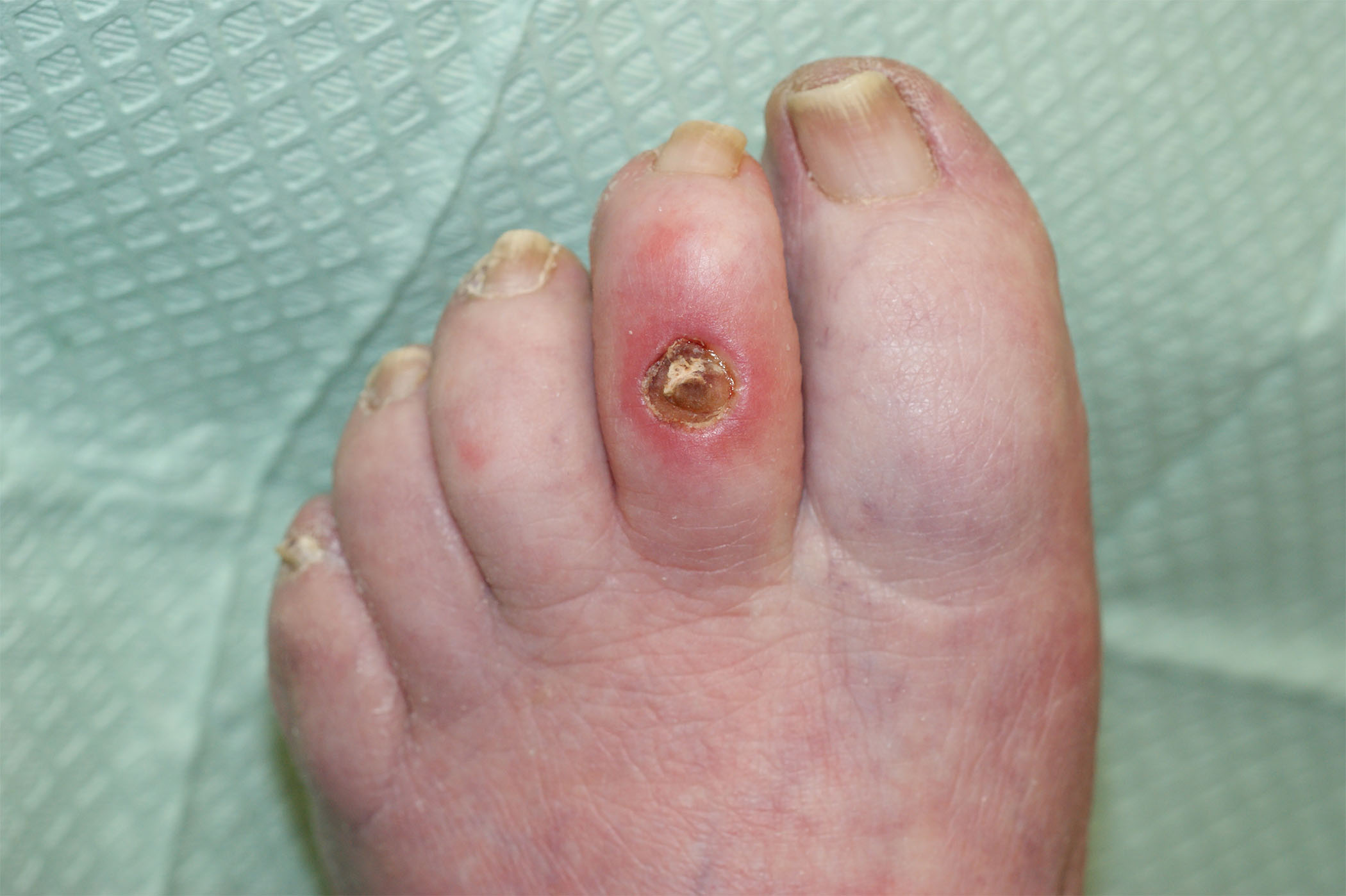
Peripheral Neuropathy and the Diabetic Foot
March 1, 2017
Reprints
AUTHORS
Kevin F. Sunshein, DPM, Fellow, American College of Foot and Ankle Surgeons, Chief, Podiatry Section, Kettering Medical Center and Sycamore Medical Center, Dayton, OH
Anastasia Samouilov, DPM, PGY-3, Chief Resident, Dayton VAMC Podiatry Residency Program, Dayton, OH
PEER REVIEWER
Jay H. Shubrook, DO, FACOFP, FAAFP, Professor, Primary Care Department, Director of Clinical Research and Diabetes Services, Touro University California College of Osteopathic Medicine, Vallejo, CA
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, Dr. Farel (CME question reviewer) owns stock in Johnson & Jonhson. Dr. Shubrook (peer reviewer) receives grant/research support from Sanofi, Astra Zeneca, Lilly, and Takeda; and is a consultant for Lilly and Novonordisk. Dr. Sunshein (author), Dr. Samouilov (author), Dr. Schneider (editor), Dr. Stapczynski (editor), Ms. Fessler (nurse planner), Ms. Coplin (executive editor), Ms. Mark (executive editor), and Ms. Hatcher (AHC Media Editorial Group Manager) report no financial relationships with companies related to the field of study covered by this CME activity.
EXECUTIVE SUMMARY
- Sensory polyneuropathy is common in diabetics.
- Symptoms of sensory polyneuropathy can be both positive (paresthesias, dysesthesias, or hyperalgesia) and negative (numbness, loss of balance, and heaviness).
- Wasting of the lumbricals in the feet is a sign of neuropathy.
- No one drug is consistently effective in the treatment of diabetic neuropathy; there is considerable variance between patients in their response.
- Pharmacologic treatments reduce the painful effects of diabetic peripheral neuropathy, but it is the loss of sensation and proprioception that place diabetic patients at extreme risk for limb loss.
- Weight offloading with splints is an important principle in the treatment of diabetic foot ulcers.
- Oral antibiotics can be used to treat mild diabetic foot infections.
A high percentage of patients in my emergency department (ED) at the “county hospital” have diabetes. Control is often suboptimal, so complications are common — from atherosclerotic disease and renal failure to diabetic foot infections. So many of these patients receive only episodic care from the ED with little ongoing comprehensive primary care. By default, the ED often is called upon to evaluate, initiate treatment, and make referrals for diabetic neuropathy and foot ulcers. This issue discusses the principles of assessing and treating these patients so that problems can be identified and appropriately managed to prevent limb loss.
— J. Stephan Stapczynski, MD, Editor
Introduction
Peripheral neuropathy is a common diabetic complication that may precipitate patients coming to the ED, either for the discomfort or for foot problems related to the neuropathy. Peripheral neuropathy affects the nerves, which impairs sensation, movement, and gland or organ function. Among the many types of peripheral neuropathy, diabetic peripheral neuropathy is the most common in the U.S. population.1 Nearly one-half of patients with diabetes will develop peripheral neuropathy.1,2 Tight glycemic control is the best method for diabetics to reduce the occurrence of neuropathy and to control symptoms once it develops.1
Peripheral neuropathy is subdivided into three types: mononeuropathy, mononeuropathy multiplex, and polyneuropathy. Mononeuropathies are caused by an injury to a single nerve, such as a common peroneal nerve injury in the leg. These are usually acute findings following trauma. Mononeuropathies also can occur from a vasculitis or focal ischemia, but they usually manifest as mononeuropathy multiplex, in which two or more mononeuropathies arise simultaneously.3 This type of neuropathy often is secondary to a connective tissue disorder, underlying vasculitis, infections, or metabolic conditions.
Diabetic peripheral neuropathy is the leading cause of polyneuropathy, and its progression leads to loss of protective sensation, skin ulcerations, and chronic wounds, which in turn cause soft tissue and bone infections often requiring amputation.
Manifestations of neuropathy result from disrupting normal functions of the peripheral nerves. There are three main types of nerves: 1) motor nerves, which control muscles and voluntary movement; 2) sensory nerves, which transmit signals from specialized receptors in the skin, joints, and internal organs; and 3) autonomic nerves, which control involuntary functions, such as blood pressure, heart rate, sweating, and the bowel and bladder.
Anatomy of Peripheral Nerves
Peripheral nerve fibers are classified based on the diameter, signal conduction velocity, and myelination state of the axons. These classifications apply to both sensory and motor fibers. Fibers of the A group have a large diameter, high conduction velocity, and are myelinated. (See Tables 1, 2, and 3.) The A group is further subdivided into four types (A-alpha, A-beta, A-delta, and A-gamma fibers) based on the information carried by the fibers and the tissues they innervate.
- A-alpha fibers are motor and are the primary receptors of the muscle spindle.
- A-beta fibers are sensory and act as secondary receptors of the muscle spindle and contribute to cutaneous mechanoreceptors.
- A-delta fibers are free nerve endings that conduct painful stimuli related to pressure and temperature.
- A-gamma fibers are typically motor neurons that control the intrinsic activation of the muscle spindle.
Fibers of the B group are myelinated with a small diameter and have a low conduction velocity. The primary role of B fibers is to transmit autonomic information.
Fibers of the C group are unmyelinated, have a small diameter, and low conduction velocity. C fibers are considered polymodal because they often can respond to combinations of thermal, mechanical, and chemical stimuli, and therefore are considered multi-use. A-delta and C fibers both contribute to the detection of diverse painful stimuli. Because of their higher conduction velocity, A-delta fibers are responsible for the sensation of a sharp, initial pain and respond to a weaker intensity of stimulus. These nerve fibers are associated with acute pain and, therefore, constitute the afferent portion of the reflex arc that results in pulling away from noxious stimuli. An example is the retraction or your hand from a hot stove. Slowly conducting, unmyelinated C fibers, by contrast, carry slow, longer-lasting pain sensations.3
Large fibers (A and B group) are insulated with a myelin sheath that allows for more rapid conduction of the electrical impulse. The small nerve fibers (C group) are non-myelinated and are slower in conducting and transmitting signals from pain receptors in the skin. They also form the autonomic fibers that send signals to and from the internal organs. Neuropathies also can be characterized as demyelinating or axonal, small or large fiber, motor or sensory, or mixed.
Table 1. Overview of Peripheral Nerve Function |
|
|
Peripheral Nerve Type |
Function |
|
Motor |
Muscles, voluntary movement |
|
Sensory |
Transmit signals from skin, joints, and organs, sensations including pain and pressure |
|
Autonomic |
Involuntary functions, blood pressure, heart rate, bowel movements, bladder emptying, digestion |
Table 2. Group A Nerve Anatomy |
||
|
A Group |
Primary Receptor |
Secondary Receptor |
|
A-Alpha |
Motor |
Muscle spindles |
|
A-Beta |
Sensory |
Secondary muscle spindles |
|
A-Delta |
Free nerve endings |
Painful stimuli |
|
A-Gamma |
Motor |
Intrinsic muscle spindle |
|
Primary receptor implies information nerves carry; secondary receptor is the tissues they innervate. |
||
Table 3. Fiber Composition of Peripheral Nerves |
||||
|
Diameter |
Signal Conduction Velocity |
Myelination |
Function |
|
|
A Group |
Large |
High |
Yes |
Sharp initial pain, others |
|
B Group |
Small |
Low |
Yes |
Autonomic transmission |
|
C Group |
Small |
Low |
No |
Long-lasting pain |
Signs and Symptoms of Peripheral Neuropathy
The symptoms of neuropathy depend on the type and distribution of the nerves that are affected. Initially, symptoms can be subtle and hard for patients to describe. The three different types of symptoms are presented below in typical order of presentation and disease progression.
Sensory Symptoms. Sensory symptoms are extremely variable and can be divided into positive and negative symptoms.5 Examples of positive symptoms include different types of pain, such as burning, tingling, sharp, dull, and searing. There may be spontaneous sensations (paresthesias), unpleasant sensations (dysesthesias), or hypersensitivity (hyperalgesia) to pressure or touch. They are inherently classified as new, abnormal, and sometimes painful sensations.
Negative sensations may occur as numbness, loss of balance, heaviness in the legs, stiffness, or feelings of something bunched up on the ball or sulcus of the foot. These are only a few examples of patient chief complaints. Further examination may reveal a wider stance or base of gait, an unsteady gait, or loss of balance, especially with the eyes closed. These findings are the result of a loss of normal sensations.5,6,7
Motor Symptoms. Motor neuropathy is manifested by weakness in the arms or legs; however, in the early stages, the weakness may be too mild to recognize. Some of the subtle symptoms include heaviness in the legs, difficulty standing from a seated position, having to pull on the rail while climbing stairs, or tripping over uneven flooring. Weakness gradually will become more obvious as the disease progresses. In severe cases, muscle wasting can be seen in the feet due to loss of the intrinsic muscles, which can lead to muscle imbalance in the toes causing gradual clawing of the toes and other deformities.6 Muscle wasting occurs because of impaired signals to distal musculature in the body, usually affecting the intrinsic foot muscles. Once the signals are impaired or lost, the muscles do not function and atrophy from disuse. As these intrinsic foot muscles lose function, the larger extrinsic leg muscles gain advantage and deform the foot in a variety of contracted positions. This muscle imbalance is the cause of the features found in an intrinsic minus foot with many prominences that can lead to ulcerative lesions.8 (See Figure 1.)
Figure 1. Intrinsic Minus Foot |
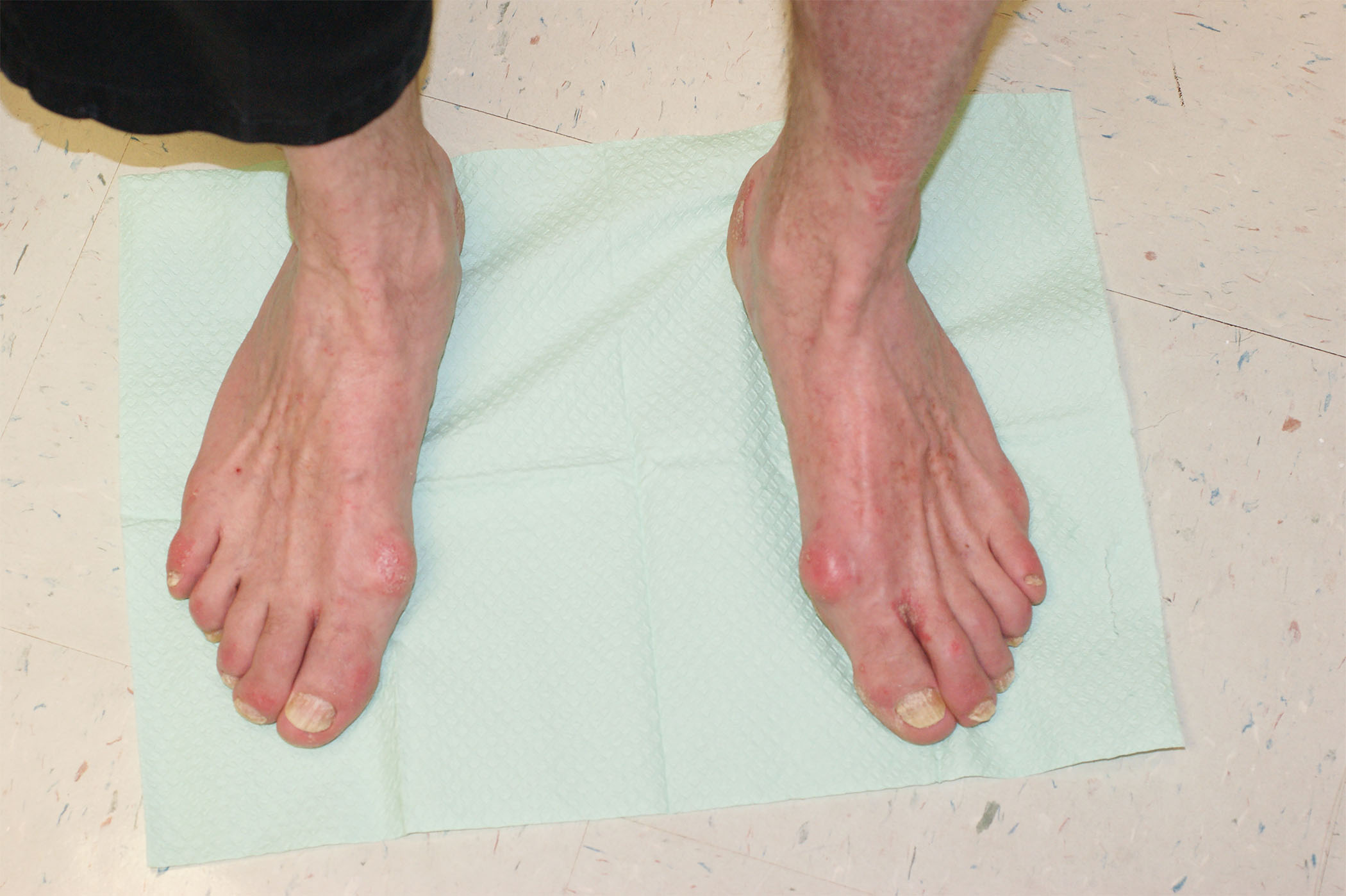 |
|
Note deep channels between the metatarsals indicative of lumbrical muscle wasting from denervation. Image courtesy of Kevin F. Sunshein, DPM. |
Autonomic Symptoms. Autonomic symptoms can affect the legs and feet in several ways. Autonomic nerves regulate skin temperature and sweating. Patients with neuropathy, especially diabetic neuropathy, have challenges with atrophy, dry or overly moist skin, and hair loss on the legs. Autonomic neuropathy contributes to delayed skin healing and can affect the nails, which usually present as ridged, brittle, and/or dystrophic.2,6,9 The autonomic nervous system affects temperature regulation. When temperature is no longer regulated appropriately, patients can have abnormal signal proliferation, which manifests as sweating to the distal extremities. As the neuropathy progresses, temperature regulation limits itself and the skin becomes dry.
Evaluation and Diagnosis of Diabetic Peripheral Neuropathy
Evaluating peripheral neuropathy in patients with diabetes is many times secondary to the patient’s presenting chief complaint of ingrown or deformed toenails, calluses, or wounds of the foot.10,11 Sometimes, patients have difficulty articulating exact symptoms of neuropathy since the progression of the disease can be insidious. Obvious symptoms may include numbness or painful tingling sensations in their feet, although early nerve damage to the feet may be indicated by changes not noticeable as concrete symptoms to the patient. Patients may make statements such as “my socks seem to be bunched up but when I take my shoes off to look, there is nothing wrong.”5 Many patients realize tingling and burning symptoms to their feet during the evening, although symptoms can be present all day long.2,7,12
The most important aspect of the diagnostic evaluation is an appropriate history and physical examination. This should include whether the patient has type 1 or 2 diabetes mellitus, as well as the duration of the disease, management of the blood sugar, and any other systemic complications of diabetes, such as retinopathy or nephropathy.
The Diabetic Foot Exam
A typical foot exam encompasses four aspects: dermatologic, vascular, neurologic, and musculoskeletal. Physical findings in the feet resulting from diabetic neuropathy are termed the “intrinsic minus foot.” (See Figure 1 and Table 4.) The longest motor nerves in the body are those that innervate the lumbricals found in the feet. Since diabetic neuropathies commonly start distally and progress proximally, the lumbricals are the first muscles to be affected.
Table 4. Features of the Intrinsic Minus Foot
Feature |
Comment |
|
Xerotic (dry) skin |
Due to sympathetic neuropathy |
|
Visible channels between the metatarsals |
Due to wasting of the lumbrical and interossei from denervation |
|
Hammer toes |
Denervation of the lumbricals allows opposing muscles to flex the interphalangeal and extend the metatarsal-phalangeal joints with the resultant hammer toes |
|
Prominent plantar metatarsal heads |
Due to extension at the metatarsal-phalangeal joints Initially most visible at the first and fifth toe; with disease progression, affects all toes with calluses overlying each metatarsal head |
|
Upward rotation of the forefoot |
Continued extension at the metatarsal-phalangeal joints eventually leads to upward movement of the entire forefoot |
|
Weak hallus longus extension |
Flexion and extension strength of the great toe is normally equal; with loss of lumbrical function, upward drift at the metatarsal-phalangeal joint reduces the strength of extension |
|
Cock-up deformity of great toe |
Extension at the metatarsal-phalangeal joint with prominent extensor hallucis tendon |
|
High arch |
Due mostly from tightening of the plantar fascia |
Dermatologic Exam
Inspection of the skin will provide clues as to the health of the patient’s feet. Toenails that are abnormally thickened, opaque, crumbling, yellow in color, and malodorous are likely to be fungal, showing symptoms of sensory neuropathy, autonomic neuropathy, or both. Dryness of the skin is very common, but any signs of inflammation, especially along the plantar aspect of the feet or the medial and lateral borders, may indicate a chronic asymptomatic tinea pedis infection. The incidence of dermal fungal infections is much higher in the diabetic population because of a compromised immune system and is a clue to the patient’s overall health.2,7
The dermatologic exam of the foot and legs includes observation of any thickening or discoloration of the toenails and hyperkeratoses on the toes or balls of the feet. One telltale sign of neuropathy is subdermal hemorrhages within calluses.2 Most likely, patients with full sensation to their feet would not be able to tolerate the pain that is associated with having enough pressure on the foot to produce subdermal hemorrhages within calluses. Peripheral neuropathy dulls sensation and allows patients to tolerate more prolonged pressure without pain on a small area of skin. Shear forces will cause the skin to react to abnormal stimuli and increase keratinization.
Peripheral neuropathy may contribute to a patient wearing a smaller shoe than normal due to loss of sensation and the inability to feel rubbing and discomfort. Any burns should be noted to the feet as well, as patients have temperature sensation loss and may unknowingly scald or burn themselves; this is more common in the winter.2
Autonomic neuropathy impedes regular skin moisture balance and regulation. Either the skin becomes too dry and scaly or it is too moist, which fosters dermatophyte infections and skin maceration within the webspaces. Often, dermatophyte infections may give the appearance of “dry skin,” further confusing a clinician. Differentiation includes inspection of the skin to evaluate for a chronic inflamed appearance, especially along the plantar and borders of the feet. This is referred to moccasin dermatophytosis or dry tinea pedis.11,14
Vascular Exam
The vascular examination should include palpation of the dorsalis pedis and posterior tibial. In about 12% of the population, the dorsalis pedis artery is absent or markedly reduced in size, so a palpable pulse may not be felt. Capillary refill time to each digit also is important in determining blood flow to the toes and tests the microvasculature. The capillary refill time test is performed with the feet slightly above the level of the heart. Normal values are less than five seconds. Presence of peripheral edema may indicate autonomic neuropathy. Venous insufficiency manifests as pitting edema to the lower extremities, and sometimes brawny, brown discoloration to the lower legs up to the level of the mid-tibia.
Neurologic Exam
The neurologic exam includes evaluating the patellar and Achilles deep tendon reflexes. Loss of the Achilles reflex is indicative of advanced peripheral neuropathy. Sensation is tested for vibratory loss with a 128 Hz tuning fork. Decreased proprioception and loss of light touch indicate neuropathy.
Gait analysis will demonstrate balance deficiencies. Walking heel to toe may be quite difficult with peripheral neuropathy. A patient’s wider base of gait may indicate loss of proprioception, and balance may be significantly decreased with the eyes closed. The Romberg test (loss of balance with feet together and eyes closed) also is useful when evaluating for neuropathy.10
Musculoskeletal Exam
The musculoskeletal exam includes observation for any typical foot deformities, such as bunion (hallux valgus) deformities, contracted toes, and Tailor’s bunions (lateral exostosis fifth metatarsal head). Clinicians should look for any obvious asymmetric changes in arch height with the patient standing. Charcot deformities are quite obvious, but even subtle changes in the arch height may be a sign of more serious foot problems, which will be discussed later. The common complaints of a patient’s foot “looking funny” or changing in appearance and becoming red, hot, and swollen without any history of trauma to the area should at least warrant a radiograph and referral to a podiatrist for an evaluation. Active Charcot changes in the feet are identified by unexplained swelling, particularly if only one foot is involved. Differentials to a Charcot deformity include a diabetic foot infection, osteomyelitis and cellulitis, acute inflammatory arthropathy, gout, acute thrombosis, and trauma.15
Treatment of Painful Diabetic Peripheral Neuropathy
Treatment of the painful symptoms from diabetic peripheral neuropathy requires a multifaceted approach in most patients. There is no one specific therapy that will prove beneficial to all patients. Many times, the side effects from the medications used in the treatment of diabetic peripheral neuropathy will limit the patient’s ability to take them. Although the pharmacologic and alternative treatments are designed to reduce the painful effects of diabetic peripheral neuropathy, it is the loss of sensation and proprioception that place diabetic patients at extreme risk for loss of limb and or life.
Pharmacologic Treatment of Diabetic Peripheral Neuropathy
Treatment of symptomatic diabetic neuropathy addresses the painful component of this disease. Drugs are the mainstay of treatment for painful symptoms. No one drug is consistently effective, and there is considerable variance between patients in their response. Patients often require trials of different medications, both topical and oral, to adequately control symptoms. In addition, side effects from taking these medications may negate the potential benefits from them.18
There are several categories of pharmacologic agents used for all types of painful sensory peripheral neuropathy, regardless of the cause. They include antidepressants, anticonvulsants, opioids, and topical agents. The anti-pain effects of the anticonvulsants or antidepressants can occur over a wider range of doses than when used for their other indications. The lowest therapeutic dose in any particular drug used to relieve the pain may be quite high and may cause side effects. Careful titration of the dose is needed to monitor the side effects of these drugs.
Neuropathy Pain Management with Anticonvulsant Drugs
Pregabalin (LyricaTM) is FDA-approved for painful diabetic peripheral neuropathy. The initial starting dose is 150 mg per day, taken in the evening so the drowsiness side effects do not interfere with the patient’s daytime activities. The dose can be increased up to a maximum of 300 mg per day. Potential side effects may include sleepiness, dizziness, difficulty concentrating, peripheral edema, and blurred vision.
Gabapentin (NeurontinTM) is started at 300 mg once per day, and then increased in increments of 300 per day taken twice or three times per day every 5-7 days until symptoms are under control. Relief of diabetic neuropathic pain may require total daily doses up to 3,600 mg per day (1,200 mg taken three times per day). Common side effects include dizziness, fatigue, drowsiness, ataxia, and peripheral edema. Although gabapentin has the most evidence for treatment of painful neuropathy, it is not FDA-approved specifically for diabetic peripheral neuropathy.19
Neuropathy Pain Management with Antidepressant Drugs
Duloxetine (CymbaltaTM) is FDA-approved for diabetic neuropathic pain. Duloxetine is a selective neurotransmitter reuptake inhibitor for serotonin, norepinephrine, and, to a lesser degree, dopamine. Usual dosage is 30 mg/day and is increased by 30 mg every four days up to 60 mg twice daily. Side effects include nausea, dizziness, fatigue, dry mouth, constipation, loss of appetite, excessive perspiration, insomnia, and sexual dysfunction.
Amitriptyline (ElavilTM) is a tricyclic antidepressant that inhibits the reuptake of norepinephrine and serotonin. The usual dose is 25 mg at bedtime with a maximum dosage of 150 mg daily in three divided doses. Side effects include drowsiness, dry mouth, urinary retention, and arrhythmia.20
Narcotic Management of Chronic Neuropathic Pain
Opioid analgesics and tramadol (UltramTM) generally are used as second-line treatment of severe pain from diabetic neuropathy. Treatment with narcotics should be used judiciously and should be individualized for the patient, considering side effects vs. potential benefits, and whether prompt onset of pain relief is necessary. Longer-acting opioids, such as oxycodone, are recommended for better efficacy. Shorter-duration narcotics or tramadol is more appropriate if the pain is occasional or of limited duration during the day or sporadic as opposed to chronic. Side effects include constipation, dizziness and drowsiness, nausea, vomiting, pruritus, memory loss, anorexia, sexual dysfunction, and urinary retention.
Topical Medications for Treatment of Painful Diabetic Peripheral Neuropathy
Common topical treatments for diabetic peripheral neuropathy include capsaicin (ZostrixTM) and lidocaine 5% patches (LidodermTM). Capsaicin stimulates the C fibers to release and deplete substance P. Lidocaine 5% dermal patches block neuronal sodium channels. These prescriptions do not carry direct FDA approval for diabetic peripheral neuropathy and can be used in conjunction with oral medications or if patients cannot tolerate them.
Compounded prescription topical formulations have evolved in the treatment of painful diabetic peripheral neuropathy. In a study by Somberg et al, a combination cream consisting of ketamine (10%), baclofen (2%), gabapentin, (6%), amitriptyline (4%), bupivacaine (2%), and clonidine (0.2%) produced good or excellent effects in 82% of patients.21,22
Nutritional and Vitamin Therapy for Diabetic Peripheral Neuropathy
Chronic metformin use results in vitamin B12 deficiency in 30% of patients; this can by itself produce peripheral neuropathy. Vitamin B12 supplementation decreases symptoms in some patients with diabetic peripheral neuropathy.23
Alpha lipoic acid (ALA) also is known to have beneficial effects on diabetic polyneuropathy, although the exact mechanism by which ALA exerts its effect is unknown.24 ALA might exert its beneficial effects at least partially by improving microcirculation to the nerves.
Foot Complications Due to Neuropathy
Loss of protective sensation can lead to severe consequences for the patient with diabetes, especially in the feet and legs. The cumulative effect of unrecognized recurrent minor trauma, delayed care of injury, and poor wound healing leads to chronic soft tissue wounds that threaten the viability of the foot and even the leg. Expenses related to the care of diabetes and its complications have a significant impact on the U.S. economy.4 The Centers for Disease Control and Prevention estimated in 2007 that 27 million people in the United States have diabetes and another 86 million have prediabetes.4 The cost of caring for patients with diabetes, including medications, wound care, hospitalizations, and surgery, is estimated to exceed $174 billion per year.1 Much of this cost is associated with complications like diabetic foot ulcers and the required medical and surgical care.
Diabetic Foot Ulcers
Diabetic foot ulcers begin with the inability to feel normal sensations, such as pressure and pain. Loss of protective sensation leads to increased damage to the skin due to prolonged pressure that does not result in the normal response to a painful stimulus. When there are areas of callused skin due to either foot deformities or excessive shear pressure (i.e., blister formation), ischemic changes from initial skin damage lead to further insult, resulting in erosion of the epidermis and dermis. Continued unabated, abnormal pressure may lead to fat necrosis and exposure of bone. The subsequent damage is noticed by patients not from pain but from either bloody discharge that they notice on their socks or from malodor that represents an infection.
Diabetic foot ulcers precede more than 80% of non-traumatic lower limb amputations.26 The most common sites for foot ulcers are toes, followed by the plantar metatarsal heads and the heel. Foot risk factors include peripheral neuropathy, peripheral arterial disease, and foot deformities.
A detailed assessment and adequate documentation of diabetic foot ulcers is important to appropriately assess the degree of disease and guide treatment. When possible, photographs of the wound with an adjacent ruler in the image are useful to document size and appearance for subsequent reassessment. On initial presentation, note the appearance of the ulcer and surrounding area. Are the margins erythematous? Is there edema or erythema spreading away from the ulcer? Is there maceration, callused skin, malodor, tunneling, and drainage, and if so, is it mild, moderate, or severe? Measure the ulcer in length, width, and depth. Is there a granular base to the ulcer or is there fibrosis and necrosis of the wound? Note the depth of the wound. Is it partial or full thickness? Is it through the dermis into the fat or subcutaneous layer? Is tendon or bone exposed?
Exposure down to bone, either visible or by palpation, suggests the possibility of osteomyelitis. Obtain a radiograph looking for changes of osteomyelitis, such as lytic bone lesions. Obtain a CBC, erythrocyte sedimentation rate (ESR), C-reactive protein (CRP), and complete chemistry panel. The MRI is the best imaging modality to diagnose osteomyelitis, especially if tendon or bone is exposed. If unavailable, a CT scan with IV contrast is an acceptable alternative.
There is a difference between an infected ulcer and a contaminated ulcer. Initial cultures and sensitivities may show colonization of multiple bacteria but not all of the identified bacteria are causing infection. Gram-positive cocci are most common, although a wide variety of pathogens have been known to infect diabetic foot ulcers. The typical presentation of an infected ulcer includes erythema, edema, malodor, rubor, calor, and purulent drainage. Colonizers do not exhibit symptoms of infection. In the absence of infection, thorough debridement of the ulcer with removal of the perimeter callus and removal of any “high point” along the periphery of the ulcer will prevent undue pressure over the ulcer.
Offloading of the ulcer is mandatory, and the patient must be taken out of normal foot gear for the side affected.2,29 Appropriate offloading devices may include a stiff surgical shoe, although this is only slightly better than conventional shoes.29 The extremity must be offloaded of all abnormal forces acting along the plantar aspect of the foot. This is the most difficult aspect to control. A diabetic foot ulcer on the plantar aspect of the foot must be relieved of the body weight to allow granulation of the wound to begin. Excessive shear pressures on the foot continue the destructive forces and will lead to further damage and increase the depth of the wound. It is imperative to stop the insult so the wound does not extend to bone.19,27,28 The gold standard for offloading diabetic foot ulcers is a total contact cast, although many patients cannot tolerate them.
Various devices to offload the foot include diabetic walking boots that are designed to keep the foot from bending, thereby reducing shear forces on the plantar aspect of the foot. In addition, a soft multi-density insole fitted into the boot can assist in offloading the foot.
The gold standard for offloading the foot in the management of diabetic foot ulcers is a total contact cast.29 Total contact casting has been used extensively to heal these difficult wounds. The practicality of using this type of cast has improved significantly in recent years with the development of several brands of fiberglass casting systems with improved ease of use. However, this type of casting technique requires expertise and diligence or it may cause further wound complications.28,30 The success of the total contact cast will depend on the expertise of the practitioner applying it and the patient’s cooperation. The cast needs to be changed at least weekly or sooner depending on the clinical necessity. The wound will need to be debrided as appropriate and measurements taken to document progress. There are many factors that influence the rate of healing of diabetic foot ulcers after therapy is initiated. No consistent expectations can be applied to individual patients; however, 50% improvement in one month is considered optimal.30
Once the wound is healed, measures must be taken to modify the patient’s foot gear to continue to address plantar shear forces acting on the foot. There are many types of shoes and shoe modifications that are available to achieve this. Adding custom molded foot orthoses to the shoes will help alleviate pressure from the plantar foot surfaces. It is much easier to prevent formation of plantar foot ulcers than to heal them. Many diabetic foot ulcerations are preventable, but it takes an extreme amount of diligence to educate and counsel patients on the significance that foot gear has on their feet. Custom foot orthotics are indicated and can be ordered by referring a patient to a podiatrist or directly through an orthotist. The authors recommend patients be established with a podiatrist, so all biomechanical and foot deformity accommodations can be prescribed.
Classification Systems of Diabetic Foot Ulcers
There are many wound classification systems used to describe diabetic foot ulcers. Two of the most well established systems used today are the Wagner and the University of Texas San Antonio Diabetic Wound Classification System. (See Tables 5 and 6 and Figure 2.)
The Wagner system is based mainly on wound depth and consists of six wound grades. These include grade 0 (intact skin), grade 1 (superficial ulcer), grade 2 (deep ulcer to tendon, bone, or joint), grade 3 (deep ulcer with abscess or osteomyelitis), grade 4 (forefoot gangrene), and grade 5 (whole foot gangrene). Infection is only included in one of the ulcer grades. It does not adequately address vascular components in most of the grades. Also, this system does not allow for classification of superficial wounds that are infected or dysvascular.5
First described in 1996, the University of Texas San Antonio Diabetic Wound Classification System addresses not only the depth of the wound but also the presence of infection or ischemia. This system is comprised of four grades based on depth with four subsections for each grade that address the vascular component and the presence or absence of infection.2
Table 5. Wagner Classification |
|
|
Grade |
Lesion |
|
0 |
No open lesions; may have deformity or cellulitis |
|
1 |
Superficial diabetic ulcer (partial or full thickness) |
|
2 |
Ulcer extension to ligament, tendon, joint capsule, or deep fascia without abscess or osteomyelitis |
|
3 |
Deep ulcer with abscess, osteomyelitis, or joint sepsis |
|
4 |
Gangrene of toes or forefoot |
|
5 |
Extensive gangrene of foot |
Table 6. University of Texas Diabetic Wound Classification |
||||
|
Grade 0 |
Grade 1 |
Grade 2 |
Grade 3 |
|
|
Stage A |
Pre-ulcer, no skin break |
Superficial wound, no penetration |
Wound penetrating tendon or capsule |
Wound penetration bone or joint |
|
Stage B |
With infection |
With infection |
With infection |
With infection |
|
Stage C |
With ischemia |
With ischemia |
With ischemia |
With ischemia |
|
Stage D |
With infection and ischemia |
With infection and ischemia |
With infection and ischemia |
With infection and ischemia |
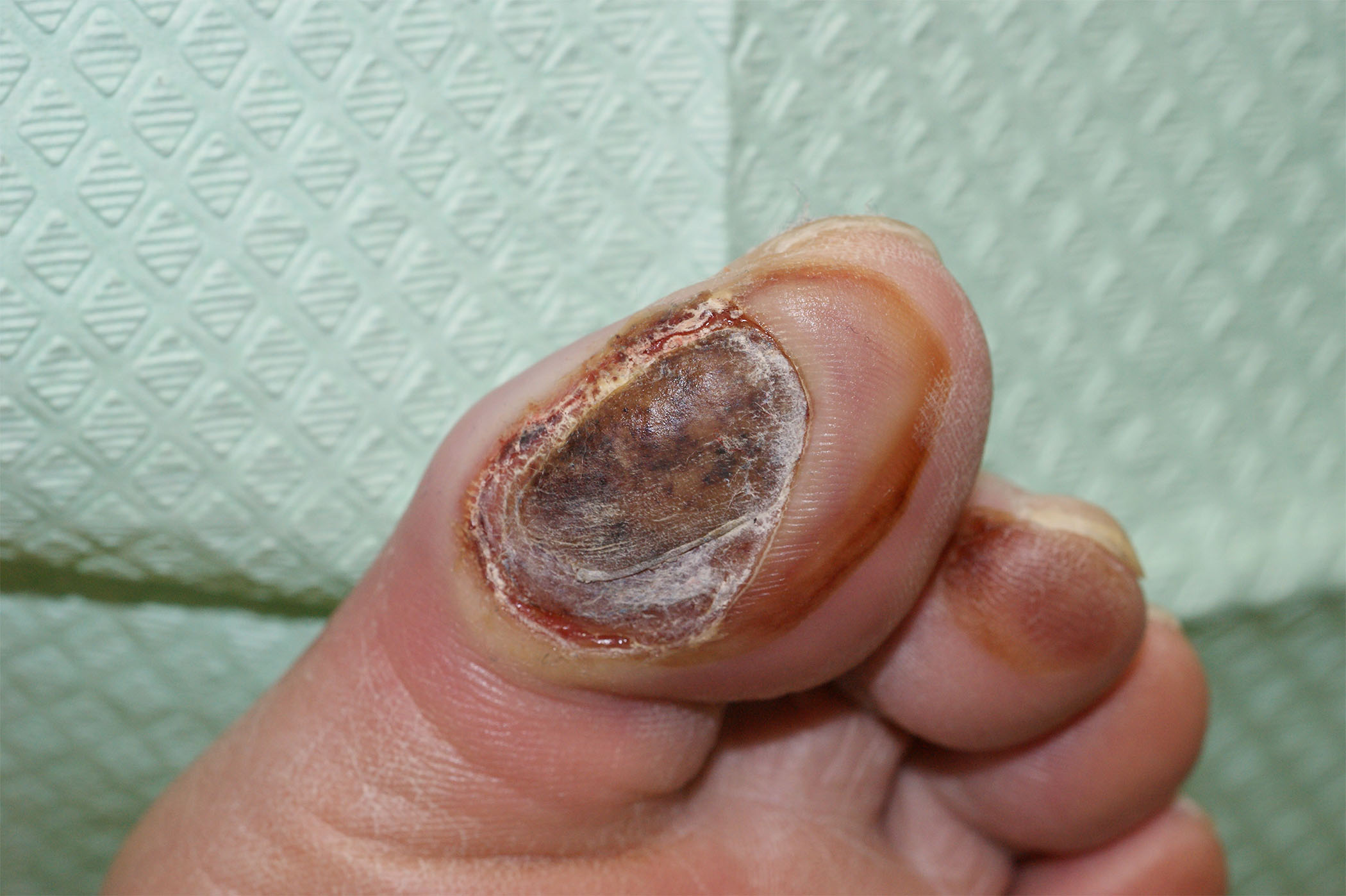
Figure 2. Wagner Classification |
|
|
Grade 0 |
Grade 1 |
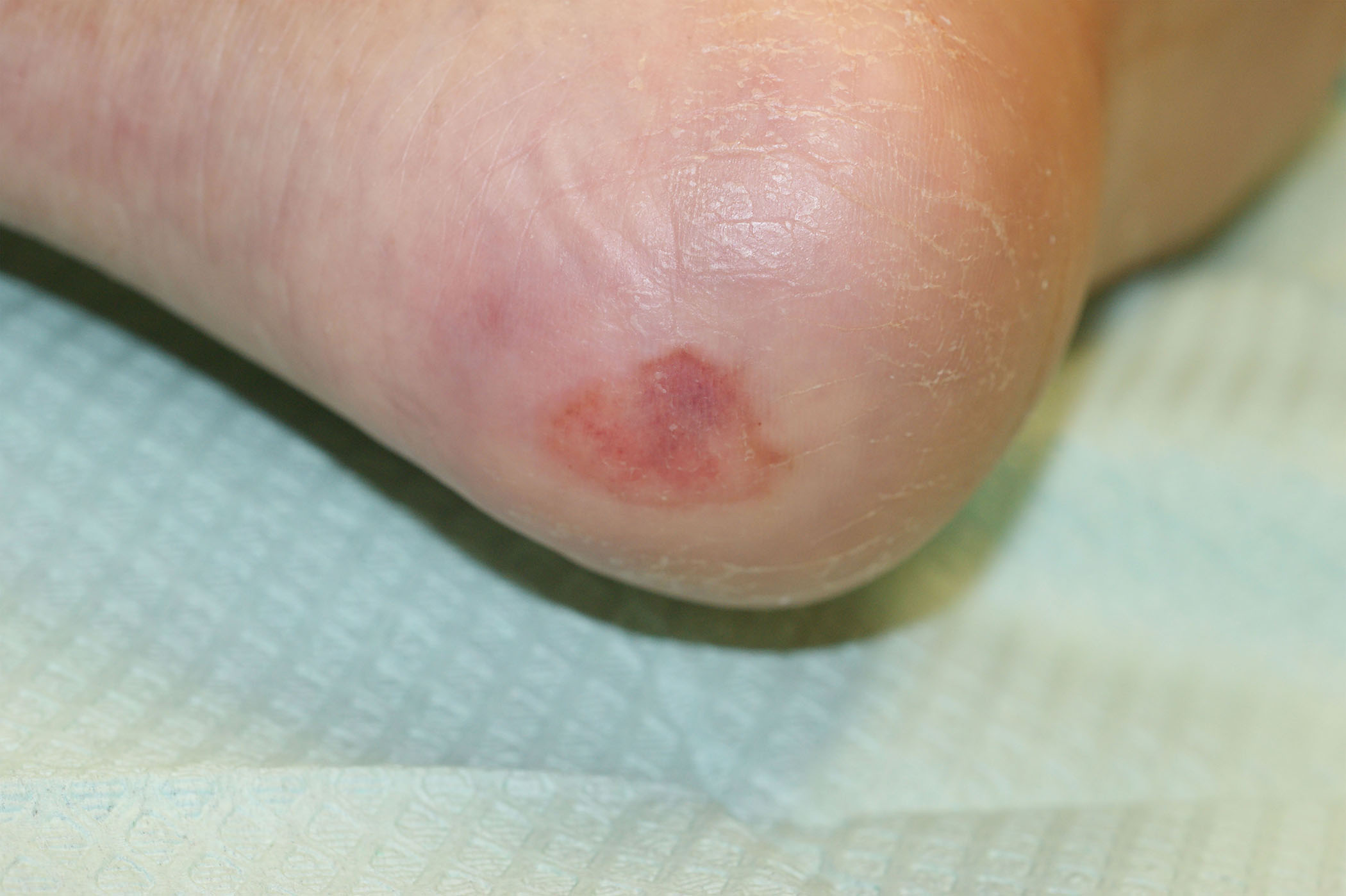 |
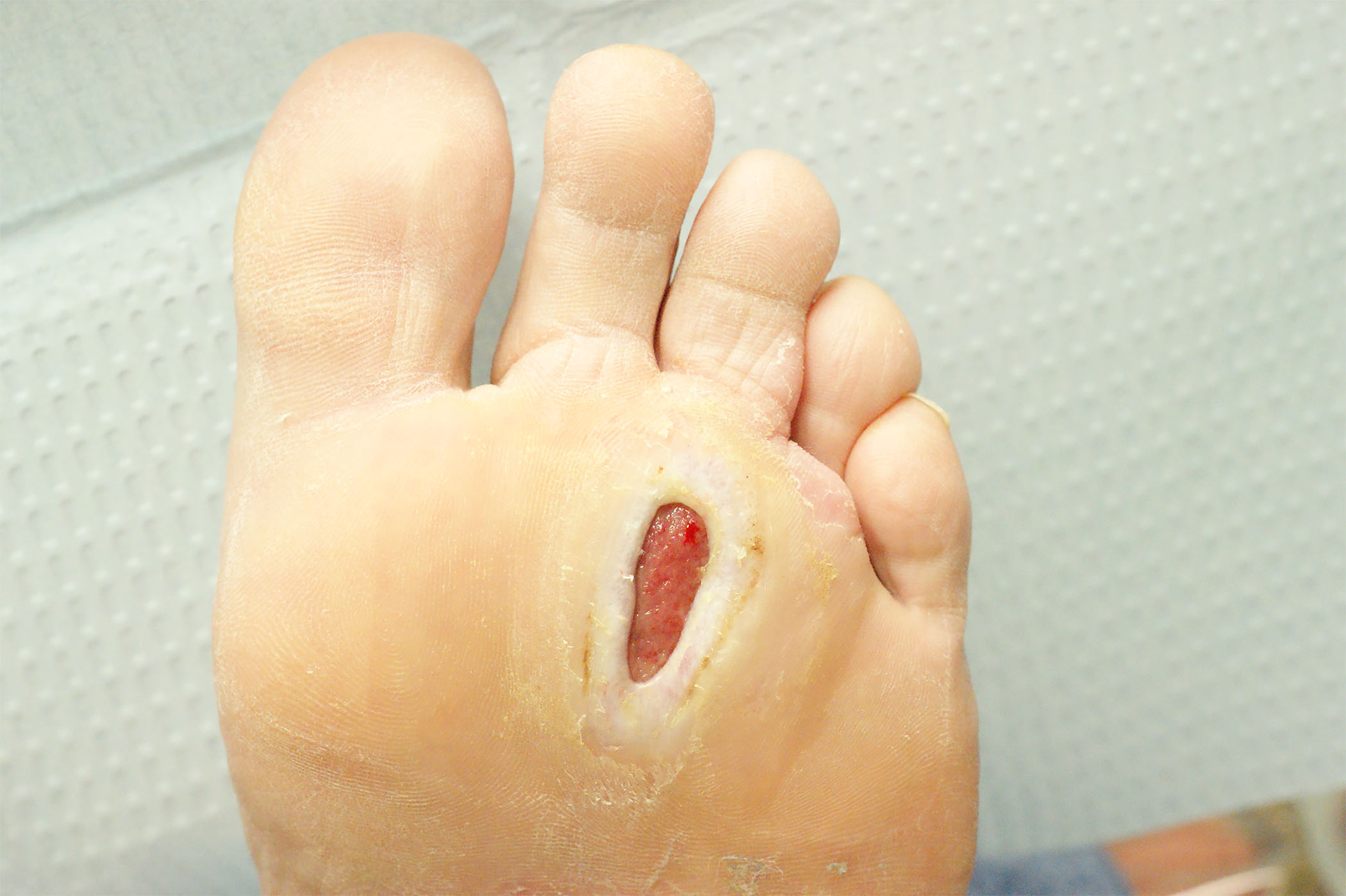 |
|
Grade 2 (Visible tendon)
|
Grade 3 (Destruction on X-ray consistent with OM)
|
|
Images courtesy of Kevin F. Sunshein, DPM. |
|
Infection
Infection of the diabetic foot ranges from superficial skin infections, localized cellulitis, infected ulcers, abscesses, osteomyelitis, septic arthritis, and necrotizing fasciitis. The sensory, motor, and autonomic neuropathy, in conjunction with factors such as deformities of the feet, compromised soft tissues, and foot type, makes the contiguous spread of infection more likely than hematogenous etiologies.2 Many times, the presenting problem, such as an infected ingrown toenail or a small blister, may seem very minor. Sensory neuropathy leads to delay in treatment because of lack of feeling. Prolonged pressure on areas of the foot susceptible to trauma will lead to more dermal damage, and a bloody sock or foul odor may be the first indications to the patient that there is a problem.
Initial presentation of a hot swollen foot must be differentiated between an infection and neuroarthropathy. Obvious sources of infection, such as a blister, ingrown toenail, or foot ulcer, suggest infection over neuroarthropathy. A keen index of suspicion and a thorough history and physical examination are critical in the initial evaluation. Routine laboratory exams such as CBC with differential, ESR, CRP, basic electrolytes, renal function, and blood glucose should be ordered. Inflammatory markers may not be useful in deciding if there is an infection because patients with diabetes may not be able to mount a normal inflammatory response.15 However, an ESR of > 70 does suggest infection.27,31
Treatment of diabetic foot infections is guided by the severity of the infection. Non-limb-threatening infections involve superficial ulcerations without significant ischemia, and they do not involve bone or joint. Many diabetic foot infections may be treated on an outpatient basis with oral antibiotics in the absence of systemic manifestation, such as fever, chills, and malaise. Such mild or moderate infections are monomicrobial, with Staphylococcus aureus, Staphylococcus epidermidis, and streptococci the most common pathogens.32 Reliable specimens for cultures may be obtained through curettage of the infected ulcer. In addition to the standard treatment for ulcerations (i.e., offloading and dressing changes), oral antibiotic therapy usually is sufficient as initial therapy. (See Table 7.) Antimicrobial treatment should be started with an agent providing adequate Gram-positive coverage, recognizing that Gram-negative organisms also might be involved.
Table 7. Initial Empiric Antibiotic Treatment for Diabetic Foot Infections
Severity |
Features |
Antibiotic |
Comment |
|
Mild |
Local infection of skin and subcutaneous tissue only No involvement of deeper tissues Erythema < 2 cm No systemic signs |
Cephalexin Amoxicillin-clavulanate Dicloxacillin Clindamycin Doxycycline Trimethoprim-sulfamethoxazole |
Oral therapy Effective against MSSA and Streptococcus spp If history of prior infection with MRSA, consider doxycycline or trimethoprim-sulfamethoxazole |
|
Moderate |
Local infection with erythema > 2 cm or involving deeper structures (bone, joints, abscess) No systemic signs |
Levofloxacin Ciprofloxacin plus clindamycin Moxifloxacin Ampicillin-sulbactam Cefoxitin Ertapenem |
May be treated with oral or initial parenteral therapy |
|
Severe |
Systemic signs |
Vancomycin and piperacillin-tazobactam Ertapenem |
Combination parenteral therapy |
|
MSSA = methicillin-sensitive S. aureus; MRSA = methicillin-resistant S. aureus |
|||
Hospitalization with intravenous antibiotic therapy is necessary for any severe foot infection. Localized pedal edema with erythema and ascending cellulitis and lymphangitis with or without ulceration require hospitalization whether there are systemic symptoms of infection. This type of infection requires a multidisciplinary approach to treatment, including consultations with internal medicine, infectious diseases, podiatry or orthopedics, vascular surgery, wound care, nutrition services, and social work.
Abscesses need to be drained in the operating room and may require further surgery. Partial toe or foot (transmetatarsal) amputations may be necessary. If the foot cannot be salvaged, a higher amputation such as a Syme’s (at the ankle joint) or below-the-knee amputation may be required to stop the infection.13
Imaging
Plain radiography is imperative for assessment of the diabetic foot. It is inexpensive and readily available. Weight-bearing views should be taken if possible. Radiographs can detect osteomyelitis, osteolysis, fractures, dislocations seen in neuropathic arthropathy, medial arterial calcification, soft tissue gas, and foreign bodies, as well as structural foot deformities and the presence of arthritis.
The first sign of osteomyelitis is focal demineralization and may reveal soft tissue swelling.15 Periosteal reaction and osteolysis may be present but may not be definitive in reaching a diagnosis of osteomyelitis. The sensitivity of plain radiography for identifying osteomyelitis is relatively poor, with a range of between 40-75%.15 Specificity is better, ranging from 60-90%. These numbers represent the delay of 10-20 days before signs of osteomyelitis are visible. The initial presentation of focal demineralization also is seen in neuroarthropathy and, therefore, may be indicative of either infection or neuroarthropathy.
Bone scans are an important tool in the management of diabetic foot infections, especially if the X-rays show non- specific bony changes. It is very difficult many times to differentiate between the two without more advanced imaging techniques.
Technetium-99 methylene diphosphonate (Tc-99 MDP) bone scans often are used in diabetic foot infection to determine the presence of osteomyelitis. Although highly sensitive, this modality lacks specificity in the neuropathic foot.33 Osteomyelitis, fractures, arthritis, and neuropathic arthropathy all will demonstrate increased radiotracer uptake. However, a negative bone scan is strong evidence against the presence of infection. To improve the specificity of nuclear imaging, white blood cells can be labeled with Tc-99 hexamethyl propylene amine oxime (Tc-99 HMPAO), indium-111 oxime, or gallium-67 citrate. Indium-111 selectively labels polymorphonuclear leukocytes and is more specific for acute infections than Tc-99 MDP scanning. Chronic infections and inflammation are not well-imaged with indium-111 because chronic inflammatory cells (i.e., lymphocytes) predominate and are not well labeled with indium. Combining Tc-99 MDP and indium-111 increases the specificity of diagnosing osteomyelitis.33
CT scans may be indicated in the assessment of suspected bone and joint pathology not evident on plain radiographs. CT offers high anatomic detail and resolution of bone with osseous fragmentation and joint subluxation. Subluxation of the transverse tarsal or tarsometatarsal joints can be seen prior to being visualized on radiographs.2,27,29
MRI usually is preferred over CT for the investigation of osteomyelitis, because of its enhanced resolution and ability to visualize the extent of any infectious process.27,29 MRI often is used in evaluating both soft tissue and bone pathology. This scan may be indicated to aid in the diagnosis of osteomyelitis, deep abscess, septic joint, and tendon rupture. MRI has a very high sensitivity for bone infection and also can be used for surgical planning.33
Vascular Evaluation in Diabetic Feet
The lower extremity should be assessed for vascular and neuropathic risk factors. Although positive findings in the neurologic examination rarely require further evaluation, positive findings of vascular insufficiency may require further consultation, as wounds may not heal without appropriate blood flow. Patients who have absent pulses, ulcers that do not exhibit healing through wound measurements, history of smoking, or kidney issues are at risk for vascular problems, along with patients who exhibit cramping in legs while walking certain distances or experience rest pain.
Noninvasive arterial studies should be performed to determine lower extremity perfusion. Such studies may include Doppler segmental arterial pressures and waveform analysis, ankle-brachial indices (ABI), toe blood pressures, and TcPO2. Ankle-brachial indices may be misleading, because ankle pressures can be falsely elevated because of medial arterial calcinosis and noncompressibility of affected arteries.2,13
The indications for a vascular surgery consultation include an ankle brachial index of < 0.7, toe blood pressures
< 40 mmHg, or transcutaneous oxygen tension (TcPO2) levels < 30 mmHg, since these measures of arterial perfusion are associated with impaired wound healing.34
Charcot Neuroarthropathy
Charcot neuroarthropathy is a serious complication of diabetes characterized by joint dislocation, pathologic fractures, and severe destruction of the osseous architecture of the foot and ankle. This condition can result in debilitating deformity or even amputation. The etiology of Charcot neuroarthropathy most likely is a combination of the effects involved in the neurovascular and neurotraumatic theories.2 Trauma superimposed on a severely neuropathic extremity is the most widely accepted theory regarding the development of an acute Charcot foot. As a result of associated autonomic neuropathy, blood flow to the foot increases, resulting in osteopenia and attendant weakness of the bone.2 Because of the loss of protective sensation that accompanies peripheral sensory neuropathy, the patient is unaware of the initiating trauma and the profound osseous destruction that often occurs during ambulation. A vicious cycle ensues in which the patient continues to walk on the injured foot, allowing further damage to occur.
The destruction commonly occurs in the midtarsal region of the foot, causing a collapse of the medial longitudinal arch with abduction of the forefoot. The resultant deformity causes a rocker bottom appearance of the foot. Abnormal pressures along the plantar medial aspect of the foot more than likely will result in ulcerations and may progress to developing osteomyelitis due to deepening of the ulceration down to bone or joint structures.35
Early recognition and treatment is imperative to prevent collapse of the medial arch. In the initial stages of Charcot neuroarthropathy, the foot must be immobilized to reduce further trauma to the foot. Offloading (sometimes in the form of external fixation) the foot in the acute active stage of the Charcot foot is the most important management strategy that can arrest the progression to deformity.2 Initial imaging options are plain radiographs, MRI evaluation, and conventional three-phase bone scan (technetium-99m MDP). If plain radiographs are negative, either the MRI or bone scan can confirm changes in the bony architecture or increased blood flow to the affected area.
Duration and aggressiveness of immobilization and offloading are guided by clinical assessment of healing of Charcot neuroarthropathy based on edema, erythema, and skin temperature changes.35 Serial X-rays and MRI are needed to help in the clinical decision to transition the patient into foot gear. Specialized custom braces, such as a Charcot restraint orthotic walker, may be needed long term to prevent foot deformity.
Guidelines for Proper Foot Health in Diabetic Patients
A healthy, intact diabetic foot is best maintained by a consistent and recurrent preventive treatment strategy as it is for diabetes in general. This is best accomplished through a multidisciplinary approach involving a team of specialists and personnel who provide a coordinated process of care. Team members may include a podiatrist, internist, ophthalmologist, endocrinologist, infectious disease specialist, cardiologist, nephrologist, vascular surgeon, orthopedic surgeon, nurse (educator, wound care, and home care), and pedorthist/orthotist. Patient and family education assumes a primary role in prevention. Such education encompasses instruction in glucose assessment, insulin and other diabetes medication administration, diet, daily foot inspection and care, proper footwear, and the necessity for prompt treatment of new lesions. Regularly scheduled podiatric visits, including debridement of calluses and toenails, are opportunities for frequent foot examination and patient education. Such visits can provide early warning of impending problems and subsequent modification of activity and care; they also can alleviate the catastrophic complications frequently associated with diabetic peripheral neuropathy.
Any patient who begins to exhibit foot deformity or symptoms of neuropathy should be referred to a podiatrist to establish baseline foot care and evaluation. These visits can prevent problems down the line and educate the patient about necessary foot care. The sooner the patient is evaluated, the more likely that severe foot complications will be avoided. However, prevention is the best treatment. Typically, a patient with neuropathy should be seen by a podiatrist every six months, and sometimes sooner if they exhibit progression of their disease or have any severe foot deformity.
REFERENCES
- American Diabetes Association. Statistics about diabetes. Available at: http://www.diabetes.org/diabetes-basics/statistics/. Accessed Jan. 29, 2017.
- Boulton AJM. The Diabetic Foot. Philadelphia: Elsevier; 2016. In: De Groot LJ, Chrousos G, Dungan K, et al, eds. SourceEndotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-2016; Oct 26.
- Boundless. Classification of Nerves. Boundless Anatomy and Physiology. Boundless, 12 Oct. 2016. Available at: https://www.boundless.com/physiology/textbooks/boundless-anatomy-and-physiology-textbook/peripheral-nervous-system-13/nerves-130/ classification-of-nerves-696-9338. Accessed: Jan. 3, 2017.
- Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. Atlanta, GA: US Department of Health and Human Services; 2014.
- Frykberg RG.Diabetic foot ulcers: Pathogenesis and management. Am Fam Physician 2002;66:1655-1663.
- Brown SJ, Handsaker JC, Bowling FL, et al. Diabetic peripheral neuropathy compromises balance during daily activities. Diabetes Care 2015;38:1116-1122.
- Bowling FL, Rashid ST, Boulton AJM. Preventing and treating foot complications associated with diabetes mellitus. Nat Rev Endocrinol 2015;11: 606-616.
- Andersen H, Gjerstad MD, Jakobsen J. Atrophy of foot muscles: A measure of diabetic neuropathy. Diabetes Care 2004;27:2382-2385.
- Jeffcoate WJ, Bus SA, Game FL, et al. Reporting standards of studies and papers on the prevention and management of foot ulcers in diabetes: Required details and markers of good quality. Lancet Diabetes Endocrinol 2016;4:781-788.
- Handsaker JC, Brown SJ, Bowling FL, et al. People with diabetic peripheral neuropathy display a decreased stepping accuracy during walking: Potential implications for risk of tripping. Diabet Med 2016;33:644-649.
- Boulton AJ. Diabetic neuropathy and foot complications. Handb Clin Neurol 2014;126:97-107.
- Markakis K, Bowling FL, Boulton AJM. The diabetic foot in 2015: An overview. Diabetes Metab Res Rev 2016;32(suppl 1):169-178.
- Forsythe RO, Hinchliffe RJ. Assessment of foot perfusion in patients with a diabetic foot ulcer. Diabetes Metab Res Rev 2016;32(Suppl 1):232-238.
- Bowling FL, Rashid ST, Boulton AJ. Preventing and treating foot complications associated with diabetes mellitus. Nat Rev Endocrinol 2015;11:606-616.
- Peterson N, Widnall J, Evans P, et al. Diagnostic imaging of diabetic foot disorders. Foot Ankle Int 2017;38:86-95.
- Myerson MS. Foot and Ankle Disorders. Philadelphia: Saunders;2000.
- Preston DC, Shapiro BE. Electromyography and Neuromuscular Disorders. Butterworth-Heinemann: Boston;1998:103-142.
- Scheinberg N, Salbu RL, Goswami G, Cohen K. Treatment of diabetic autonomic neuropathy in older adults with diabetes mellitus. Consult Pharm 2016;31.11:633-645.
- Dworkin RH, Simpson DM, McArthur JC. Neuropathic Pain: Mechanisms, Diagnosis, and Treatment. New York: Oxford University Press; 2012.
- Santillan RM. Management of diabetic peripheral neuropathic pain. US Endocrinology 2005;1:55-57.
- Somberg JC, Molnar J. Retrospective evaluation on the analgesic activities of 2 compounded topical creams and voltaren gel in chronic noncancer pain. Am J Ther 2015;22:342-349.
- Sawynok J, Zinger C. Topical amitriptyline and ketamine for post-herpetic neuralgia and other forms of neuropathic pain. Expert Opin Pharmacother 2016;17:601-609.
- Bell DS. Metformin-induced vitamin B12 deficiency presenting as a peripheral neuropathy. South Med J 2010;103:265-267.
- Haak E, Usadel KH, Kusterer K, et al. Effects of alpha-lipoic acid on microcirculation in patients with peripheral diabetic neuropathy. Exp Clin Endocrinol Diabetes 2000;108:168-174.
- Bosi E, Conti M, Vermigli C, et al. Effectiveness of frequency-modulated electromagnetic neural stimulation in the treatment of painful diabetic neuropathy. Diabetologia 2005;48:817-823.
- Jain A. A simple new classification for diabetic foot ulcers. Med-Sci 2015;4:2109.
- Game FL, Apelqvist J, Attinger C, et al. Effectiveness of interventions to enhance healing of chronic ulcers of the foot in diabetes: A systematic review. Diabetes Metab Res Rev 2016;32(Suppl 1):154-168.
- Burns J, Begg L. Optimizing the offloading properties of the total contact cast for plantar foot ulceration. Diabet Med 2011;28:179-185.
- Lipsky BA. Diabetic foot infections: Current treatment and delaying the “post-antibiotic era.” Diabetes Metab Res Rev 2016;32(Suppl 1):246-253.
- Kikuchi M, Yasuhiro I, Masato Y, Tetsuji U. Total contact cast for diabetic foot lesions. J Japanese Soc Limb Salvage Podiatric Med 2014;6:100-105.
- Oyibo SO, Jude EB, Tarawneh I, et al. A comparison of two diabetic foot ulcer classification systems: The Wagner and the University of Texas wound classification systems. Diabetes Care 2001;24:84-88.
- Infectious Diseases Society of America. Correct treatment of common diabetic foot infections can reduce amputations. May 22, 2012. Available at: http://www.idsociety.org/2012_Diabetic_Foot_Infection_Guideline/. Accessed: Jan. 29, 2017.
- Ergen FB, Sanverdi SE, Oznur A. Charcot foot in diabetes and an update on imaging. Diabet Foot Ankle 2013;4:10.3402/dfa.V4i0.21884.
- Agency for Healthcare Research & Quality. Chartbook on Effective Treatment. Diabetes. U.S. Department of Health and Human Services: Agency for Healthcare Research and Quality. Sept. 3, 2015. Available at: https://www.ahrq.gov/research/findings/nhqrdr/2014chartbooks/effectivetx/eff-intro.html. Accessed Jan. 30, 2017.
- Jeffcoate WJ. Charcot foot syndrome. Diabet Med 2015;32:760-770.
This issue discusses the principles of assessing and treating patients with diabetic neuropathy so that problems can be identified and appropriately managed to prevent limb loss.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.