Stridor in the Infant and Young Child
April 15, 2017
Reprints
AUTHORS
Jason Toews, MD, Resident Physician, Pediatrics (PGY2), St. Christopher’s Hospital for Children, Philadelphia, PA.
Evan J. Weiner, MD, FAAP, FACEP, FAAEM, Director, Department of Emergency Medicine, Program Director, PEM Fellowship, St. Christopher’s Hospital for Children, Philadelphia, PA.
PEER REVIEWER
Alfred Sacchetti, MD, FACEP, Chief of Emergency Services, Our Lady of Lourdes Medical Center, Camden, NJ; Clinical Assistant Professor, Emergency Medicine, Thomas Jefferson University, Philadelphia, PA.
EXECUTIVE SUMMARY
- Evaluate patients with stridor expediently, as it has the potential to be life-threatening. Ensuring adequate airway patency, breathing, and circulation (ABCs) is the first priority in managing stridor.
- Viral croup is the most common etiology of stridor in children, and typically presents along with symptoms of an upper respiratory infection. Patients presenting to the emergency department with croup should receive 0.6 mg/kg of dexamethasone. Those who are actively stridorous also should receive nebulized L-epinephrine.
- Suspect possible foreign body aspiration until it can be disproven.
- In chronic or subacute presentations of croup, the possible etiologies are myriad, and likely will require laryngoscopy. A viral upper respiratory infection is often the first presentation of underlying airway abnormalities.
Introduction
Stridor is a high-pitched, monophonic sound caused by turbulent air flow through a narrowed airway, and is a common symptom among young children presenting to the emergency department (ED). The term originates from the Latin stridere, which means “creaking” or “grating noise.” It may occur during inspiration or expiration, but often is limited to inspiration. It may be caused by any obstruction that narrows the airway, including edema or inflammation, masses, aspirated foreign objects, or decreased tone of the airway walls, among other causes. It is distinct from stertor, a lower pitched snoring and snorting sound originating in the nasopharynx.
Epidemiology
The most common cause of stridor in young children between the ages of 3 months and 5 years is viral croup. The peak incidence of croup is during the second year of life. Most croup occurs in mid-autumn, with fewer cases in the summer. Croup has been found to be more common in males than females, and about 15% of patients have a strong family history of croup, perhaps due to smaller airway diameters. Peritonsillar and retropharyngeal abscesses also are common, although they occur more frequently in older children, and only a relatively small proportion result in stridor. Interestingly, the prevalence of these infections appears to be increasing.1,2 Epiglottitis was once one of the most common infectious causes of upper airway obstruction, but now occurs much less frequently. It affects approximately 1.3 out of every 100,000 children per year in the United States,3 with a peak incidence at 3 years of age. Bacterial tracheitis, another potentially life-threatening infection that can cause stridor, typically presents in older children between the ages of 5 and 7 years, but can occur at any age.
Foreign body aspiration is the most common noninfectious cause of upper airway obstruction, which may or may not result in stridor, and causes the deaths of more than 150 children per year and leads to more than 17,000 ED visits per year in the United States.4 The vast majority of childhood aspirations occur in children younger than 3 years of age.5
Neoplasms also may cause airway obstruction and stridor, and typically are associated with a gradual onset. The most common laryngeal neoplasm in children is laryngeal papillomatosis, also known as benign laryngeal warts, which has an incidence of 4.3 per 100,000 children. Tumors of the neck are uncommon in infants and children, although they may occur. The two most common benign tracheal tumors are inflammatory pseudotumor, which is a local inflammatory section to a previous tracheal injury or insult, and hamartomas, which are composed of normal tissue elements arranged abnormally.
Anaphylaxis and acute allergic reactions may also lead to stridor through upper airway edema. The incidence of severe allergies in pediatrics is increasing, and the most common antigens are foods.6 Although some parents may be concerned about anaphylaxis to vaccines, this is exceedingly rare, occurring at a rate of one per 1,000,000 vaccine doses.7 Although anaphylaxis is much less common in infants than in older children, it can occur and is increasing in prevalence in this age group.6
Laryngomalacia and tracheomalacia are the most prevalent causes of congenital stridor, accounting for 60% of cases. Congenital vocal cord paralysis is the next most common cause. Subglottic hemangioma is a rare cause of stridor that typically begins to cause airway obstruction within the first two months of life, but may first present any time within the first six months of life. Hemangiomas are most prevalent in Caucasians and females.8 The vast majority of hemangiomas are cutaneous, and 1% of children with cutaneous hemangiomas have a subglottic hemangioma. However, approximately 50% of patients with subglottic hemangioma also have a facial cutaneous hemangioma, typically within a beard distribution pattern.
Vascular anomalies of the aortic arch complex may compromise the airway. These are relatively common, estimated to be present in up to 1% of infants, although the majority are asymptomatic.9 The most common malformation to cause stridor is a double aortic arch encircling both the trachea and the esophagus.9
Patients with cranial facial abnormalities, such as micrognathia, are at increased risk of developing stridor from any cause. A retrospective study also revealed an increase in the prevalence of stridor from multiple causes in patients with trisomy 21.10
Pathophysiology
Stridor may result from any obstruction that impedes the flow of air through the airway. Infants and young children are particularly susceptible, as their airways have a smaller diameter than airways of older children and adults. This causes increased resistance to air flow as represented by Poiseuille’s law, which states that the resistance of the airway is inversely proportional to the fourth power of the radius. Thus, even a very small obstruction in the pediatric airway has an outsized effect on resistance. The source of the noise of stridor is usually the oscillation of the walls of the airway secondary to turbulent air flow. According to Bernoulli’s principle, the wall of the airway moves toward areas of low pressure.
In croup, inflammation causes edema of the mucosal lining of the airway, reducing its diameter. Laryngotracheobronchitis is the term used to describe this viral inflammation of the glottic and subglottic regions of the trachea. The most implicated pathogen in croup is parainfluenza, which accounts for approximately 75% of cases, although influenza A and B, adenovirus, rhinovirus, enterovirus, bocavirus, and respiratory syncytial virus also are implicated.11 Influenza A has been noted to cause particularly severe croup.
Haemophilus influenzae type B historically was the dominant etiology of epiglottitis, which now has become very rare in children in the developed world because of widespread vaccination. Now, the most commonly implicated pathogens in epiglottitis are Streptococcus pyogenes, Streptococcus pneumoniae, nontypeable H. influenzae, and Staphlycoccus aureus, including methicillin-resistant S. aureus. The most commonly implicated pathogen in bacterial tracheitis, also referred to as bacterial croup, is S. aureus, although it also may be caused by other pathogens, including Moraxella catarrhalis, S. pneumoniae, S. pyogenes, nontypeable H. influenzae, and anaerobes. The role of the latter is questionable.2
Foreign bodies in the airway are another source of stridor. One study found seeds to be the most commonly aspirated objects.12 Another study reported the most common objects were hard candy.5 Other commonly aspirated objects include nuts, grapes, apples, carrots, and popcorn. Inorganic objects rarely are aspirated. Multiple studies have shown that foreign body aspiration is significantly more prevalent in male children than in females.12,13 The most common site for an object to lodge is in the right main stem bronchus (about 58% of cases); approximately 10% lodge in the trachea or larynx. About 60% of aspirated foreign objects that lodge in the trachea cause stridor. Ingestion of foreign bodies may cause stridor if they lodge in the esophagus and cause impingement of the trachea.
Laryngeal papillomas may cause stridor when they become large enough. These growths result from vertical transmission of human papillomavirus (HPV) during birth, corroborated by the fact that 67% of children with respiratory papillomatosis were born to a mother who had condylomata acuminata, the vaginal form of the infection. The rate of vertical transmission from mothers with condylomata acuminata is approximately one in 500. HPV types 6 and 11 are the serotypes most responsible for laryngeal growths.
Laryngomalacia and tracheomalacia are caused by decreased laryngeal and tracheal tone, respectively, which leads to supraglottic collapse during inspiration. In laryngomalacia, subglottic stenosis causes narrowing of the subglottic larynx, typically about 2-3 mm below the glottis, and may be acquired or congenital. Ninety percent of acquired stenosis is secondary to trauma following intubation, especially over a prolonged period of time, and particularly if an oversized endotracheal tube was used. Pressure of the endotracheal tube on the inside of the trachea causes ischemia and ulceration of the mucosa, which heals in most patients following extubation, but develops into obstructive fibrosis and/or chronic edema in a small percentage of cases. This also may be exacerbated by gastroesophageal reflux. Congenital narrowing of the trachea may be caused by fibrosis secondary to injury, a tracheal ring trapped beneath the cricoid cartilage, submucosal gland hypertrophy in the area, a cyst, or abnormally shaped cricoid cartilage. In these cases, symptoms often first are noticed with the onset of a viral upper respiratory infection, which causes edema in the already compromised airway, precipitating biphasic or inspiratory stridor.
Cysts in the airway may cause stridor. Most often, supraglottic cysts are congenital.14 Vallecular cysts are one of the more prevalent examples.15 Subglottic cysts typically develop secondary to trauma to the trachea, such as from endotracheal intubation. Vascular rings also may impinge on the airway, leading to stridor. Any congenital cardiac lesion that causes pulmonary hypertension also may lead to stridor if the pulmonary arteries become enlarged enough to compress the left main bronchus.
There are many additional, rare causes of stridor. Multiple case reports reported hypocalcemia from various causes, leading to laryngospasm and stridor as the presenting symptoms.16,17,18 Gastroesophageal reflux may present initially as stridor in infants. One case report detailed a lesion in the erythroids of a child secondary to Crohn’s disease that presented with stridor.19 Multiple patients have developed contracted vocal folds resulting in stridor secondary to electrical impulses from implanted vagal nerve stimulators for the treatment of epilepsy.20
Thus, it is imperative to consider a wide range of etiologies when the diagnosis is unclear and when there is something unique about the child.
Table 1. Differential Diagnosis of Stridor
|
Acute Infectious Viral croup Peritonsillar and retropharyngeal abscess Epiglottitis Bacterial tracheitis Severe lymphadenopathy |
Acute Noninfectious Foreign body aspiration Foreign body ingestion causing airway obstruction Allergic airway edema Airway edema Neck trauma and caustic ingestions Laryngeal spasm Tumors |
|
Chronic Infectious Laryngeal papillomatosis |
Chronic Noninfectious Laryngomalacia Subglottic stenosis Laryngeal webs Vocal cord paralysis Subglottic hemangioma Laryngeal cysts Vascular rings Gastroesophageal reflux |
Table 2. Infectious Causes of Stridor
Viral Croup |
Epiglottitis |
Bacterial Tracheitis |
Retropharyngeal Abscess |
|
|
Author adapted from: Long S, Pickering LK, et al. Principles and Practice of Pediatric Infectious Diseases, 4th ed. Elsevier; Philadelphia, PA; 2012:162–171. |
||||
|
Peak age |
1-2 years |
3-6 years, any |
2-4 years, any |
6 months-3 years |
|
Cause |
Parainfluenza virus, other viruses |
Streptococcus pyogenes, Streptococcus pneumoniae, Haemophilus influenzae type B |
Staphylococcus aureus, |
S. pyogenes, |
|
Percent receiving artificial airway |
< 20 |
> 90 |
> 75 |
75 |
Clinical Presentation and Assessment
Rapidly assess patients presenting to the ED with stridor, as those in significant distress must be managed emergently. Initial observation should focus on assessing airway patency, respiratory effort, and any signs of acute hypoxia, such as cyanosis or poor perfusion. Examine the nares and oropharynx closely, noting any signs of upper respiratory infection or visible obstructions, swelling, or drooling. Take particular note during the respiratory exam for signs of respiratory distress such as suprasternal or subcostal retractions and nasal flaring. Assess aeration of the lung fields, as asymmetry may indicate an obstruction in one of the bronchi. Closely examine the neck for overt masses and to ensure full range of motion. Look for cervical lymphadenopathy that may suggest an infectious etiology, or bruising or lacerations suggesting recent trauma to the neck.
The quality of the cry in infants and phonation in older children are important to document. The patient’s desired positioning also should be assessed; a sniffing position (leaning forward with the head extended) indicates an obstruction at the level of the larynx. A thorough cardiac and abdominal exam should be performed.
The location of obstruction in the airway often influences the quality of stridor, which is useful in assessment of these patients. Obstruction may occur in the oropharynx above the glottis, at the level of the glottis, in the extrathoracic portion of the trachea, or in the intrathoracic trachea and bronchi. There is some inherent flexibility in the structures of the pharynx, meaning stridor originating in this area may vary with changes in position. All extra-thoracic causes of stridor will have an inspiratory phase predominance, as this is when the pressure inside the airway is at its lowest, drawing in the walls of the airway. In contrast, intrathoracic obstructions are fixed due to the rigidity of the thorax and would be expected to cause biphasic or expiratory stridor only. Laryngeal and subglottic obstructions are associated with higher pitched stridor, as these are the narrowest areas of the airway. Finally, obstruction at the level of the larynx would be expected to result in a prolonged inspiratory phase, while bronchial obstructions cause a prolonged expiratory phase. Both phases are prolonged with tracheal obstructions.
Identify if the stridor is acute or chronic in nature. Most presentations to the ED will be for acute or subacute stridor, and salient history to elicit includes the time of onset, character of onset (immediate vs. gradual), whether it is persistent or intermittent, aggravating and relieving factors (such as lying supine or sleeping), and whether there has been any associated cyanosis or apnea. Also establish whether there are any concomitant or preceding symptoms, especially fever, which correlates strongly with infectious etiologies, as well as cough, rhinorrhea, dysphagia, feeding history, and hydration status. Always ascertain the child’s immunization status, as children who are not immunized are at increased risk of epiglottitis and other infections. Foreign body aspiration should be high on the differential diagnosis for any case of stridor with acute onset, particularly if onset was associated with gagging or choking or if the child was unsupervised or not being directly observed at the time the stridor began.
Stridor in very young infants is most often due to congenital abnormalities. Birth history and past medical history are important, especially diagnoses or surgeries related to the airway or neck and any recent history of intubation, which may have caused injury to the airway.
Confirm medications the patient has taken, with particular regard to any recent changes or those that may decrease muscle tone.
Even in cases in which chronic stridor exists at baseline, often it will have worsened to cause presentation to the ED. Also, viral upper respiratory infection causing acute edema frequently is the first presentation of another underlying etiology. Thus, conduct a thorough history and remember that more than one etiology may be present in any given patient.
Croup. Croup often is preceded by typical symptoms of a viral upper respiratory infection such as fever, cough, or pharyngitis for one to three days before the onset of stridor. Along with stridor, patients often develop a characteristically “barky” cough and hoarseness. Respiratory symptoms typically are worse at night and are aggravated by irritation and crying. Croup should be diagnosed clinically; confirmatory viral testing is not necessary. It is important to visualize the posterior pharynx and, if concern exists for possible epiglottitis, the epiglottis. Assessment of croup has been quantified using tools such as the Westley Croup Score, which classifies the severity of croup using stridor, as well as retractions, air entry, cyanosis, and level of consciousness.21 Because alveolar gas exchange is normal, parameters such as hemoglobin oxygen saturation typically are normal until respiratory collapse is imminent.
Some patients may present with spasmodic croup, a variant that lacks the viral prodrome and is more transient and recurrent in nature. The pathogenesis of this is unknown, but has been postulated to be an allergic response to viral antigens.
Epiglottitis. Epiglottitis, or inflammation of the glottis, may lead to stridor. Stridor is a late finding and typically is preceded by high fever, pharyngitis, and rapidly progressing dyspnea. Patients may display characteristic signs of drooling22 and tripoding, which is characterized by leaning forward with one’s neck extended and mouth open. If concern for epiglottitis exists, the epiglottis must be visualized using a tongue blade, laryngoscope, or video laryngoscope. If epiglottitis is present, the epiglottis will appear enlarged and either cherry-red or pale.
Bacterial Tracheitis. Bacterial tracheitis often develops as a superinfection following a course of viral croup, likely secondary to edema and trauma to the tracheal mucosa caused by coughing. Concern for tracheitis should be high when stridor persists despite standard treatment for croup. Tracheitis also may occur in children who were extubated recently or who otherwise have sustained tracheal trauma, which predisposes to infection. In contrast to patients with epiglottitis, patients with bacterial tracheitis will be able to lie flat and will not tripod. They may or may not have dysphagia and drooling. These children often present with a toxic appearance and respiratory distress.
Peritonsillar Abscess. Peritonsillar abscess often is accompanied by fever and reticence to swallow, and should be suspected if there is uvular deviation or retropharyngeal fullness upon visual examination of the pharynx.2 Meningismus and torticollis from muscular irritation, secondary to the abscess, may be present.
Foreign Body Aspiration. Foreign body aspiration must be ruled out in any stridulous infant or child, particularly in cases in which a choking or gagging episode was witnessed prior to the initiation of the stridor, or when the onset of stridor was very sudden and was not preceded by other symptoms. The incidence of foreign body aspiration is highest in children older than 6 months of age who are self-mobile, but should be not be ruled out in younger children, especially in cases in which other children were nearby, as they may have placed objects or food in the affected child’s mouth. Only slightly more than half of foreign body aspirations involve a specific history of aspiration. Aspiration commonly occurs while swallowing; young children are at increased risk, as their swallowing coordination remains underdeveloped and they have reduced ability to masticate. Perform a focused respiratory exam, and examine the oropharynx for foreign objects or food. Asymmetric aeration of the lungs may indicate an object in a bronchus, which should prompt X-ray evaluation.
Laryngeal Papillomatosis. Laryngeal papillomatosis typically presents first with stridor in children between age 2 and 4 years. Most lesions occur in the larynx, especially on the vocal cords, but they also may develop anywhere in the respiratory tract, including the pharynx, trachea, and bronchi. Hoarseness may develop prior to respiratory distress, and stridor may occur as the lesions increase in size.
Tumor. Tumor should be higher on the differential diagnosis in cases in which both inspiratory and expiratory stridor are present, which suggests a fixed obstruction, especially if other more common etiologies do not fit the presentation. Constitutional symptoms associated with malignancy, such as weight loss, anorexia, fevers, and night sweats, may be present. Malignant tumors of the upper respiratory tract include rhabdomyosarcomas, bronchial adenomas, bronchogenic carcinomas, bronchial carcinoid tumors, and others. Any mediastinal tumor also may compress the trachea and lead to stridor. These include mediastinal teratomas, which have an increased incidence of diagnosis soon after birth.23 Further, T-cell acute lymphoblastic leukemia (ALL) can present with a mediastinal space-occupying mass, which may compress the trachea and cause stridor. Thyroid tumors and hypertrophy may do the same. Patients with neurofibromatosis may develop fibromas in the larynx, which also may result in stridor.
Edema. Iatrogenic airway edema should be considered in patients who have been extubated recently and present with stridor. Trauma to the airway can cause injury to the mucosa, leading to edema. Post-extubation stridor is relatively common, with one study showing an incidence of 8%.24
Angioneurotic edema is a rare entity seen in children as young as 2 years of age, and causes swelling of the airway without any urticaria, pain, or discoloration. This may be precipitated by trauma or stress.
Anaphylaxis typically presents with the involvement of multiple systems. Approximately 56% of allergic reactions in children younger than 2 years of age involve the respiratory system, while 98% also involve the skin, with generalized urticaria being the most common complaint in children old enough to express themselves.25 In the pediatric age group, most reactions occur between one and three hours after exposure.25
Other Causes. Laryngeal webs causing stenosis may present suddenly in infants with stridor and respiratory distress through their first year of life. The onset of stridor typically is precipitated by a viral upper respiratory infection, which causes edema and narrows an already compromised airway.
Vocal cord paralysis may be bilateral, which often is caused by a central nervous system lesion such as a Chiari malformation or hydrocephalus, or unilateral, which may have an iatrogenic cause sustained during surgery. Bilateral vocal cord paralysis results in high-pitched inspiratory stridor, while the unilateral variant may produce weak stridor as well, along with choking, coughing, and aspiration due to the vocal cord remaining open and allowing secretions into the trachea, and a weak cry.
Hemangiomas in the airway are fixed obstructions, so they typically cause biphasic stridor. Patients may present with cough and hoarseness, and stridor often is first apparent with the onset of a viral upper respiratory infection, which further compromises the airway.26,27 If the hemangioma itself is compromised, it also may produce hemoptysis.
Vascular malformations may cause stridor, and almost always will present by 3 months of age. These should be considered in an infant who presents with worsening stridor and respiratory distress, but without another more likely etiology. The respiratory distress often is associated with feeding.
Laryngomalacia and tracheomalacia may be exacerbated by feeding, supine positioning, and agitation, and may worsen acutely with viral upper respiratory infections. It may begin immediately after birth or any time within the first two weeks of life and may worsen over the first six months of life, making it an important consideration in the differential diagnosis of an infant with new-onset stridor. Patients with neurological disease or gastroesophageal reflux may be affected more negatively.
Laryngospasm may result in stridor, and may be the result of a myriad of etiologies. Hypocalcemia can present with laryngospasm, as well as other symptoms such as irritability, tremors, twitching, and carpopedal spasm. If a syndrome that may result in hypocalcemia is suggested by a patient’s history, a basic metabolic panel should be collected to assess the serum electrolyte level.
Iatrogenic administration of ketamine is a rare but important cause of laryngospasm, and most frequently occurs in infants. It typically is self-limited and usually lasts less than one minute. Laryngospasm due to ketamine is treated with supplemental oxygen and positive pressure ventilation with bag and mask. In cases of nonresolution, endotracheal intubation may be necessary.
Diagnostic Studies
X-rays of the chest and neck should be ordered only on a case-specific basis; they are not indicated in all cases of stridor. If a diagnosis of croup is clear, for example, an X-ray is not needed. If an X-ray of the neck is obtained in a case of croup, it may show characteristic subglottic narrowing, or a “steeple sign,” although this is not sensitive or specific to croup, and does not correlate well with disease severity. (See Figure 1.) Lateral X-ray of the neck often is useful in confirming suspected epiglottitis. Proper positioning for this is crucial; the patient’s neck should be in full hyperextension to best visualize the inflamed epiglottis on the X-ray film. Ensure that the X-ray is not taken from an oblique angle or the epiglottis may appear round on the film. The X-ray may reveal a diagnostic enlarged epiglottis, termed a “thumb sign.” (See Figure 2.) An evaluation of five case series has shown that non-concerning X-rays do not exclude epiglottitis with adequate specificity and sensitivity.11 Thus, the epiglottis must be visualized to rule out epiglottitis in suspected cases, even in the event of non-enlargement of the epiglottis on X-ray.
Figure 1. Steeple Sign, Croup
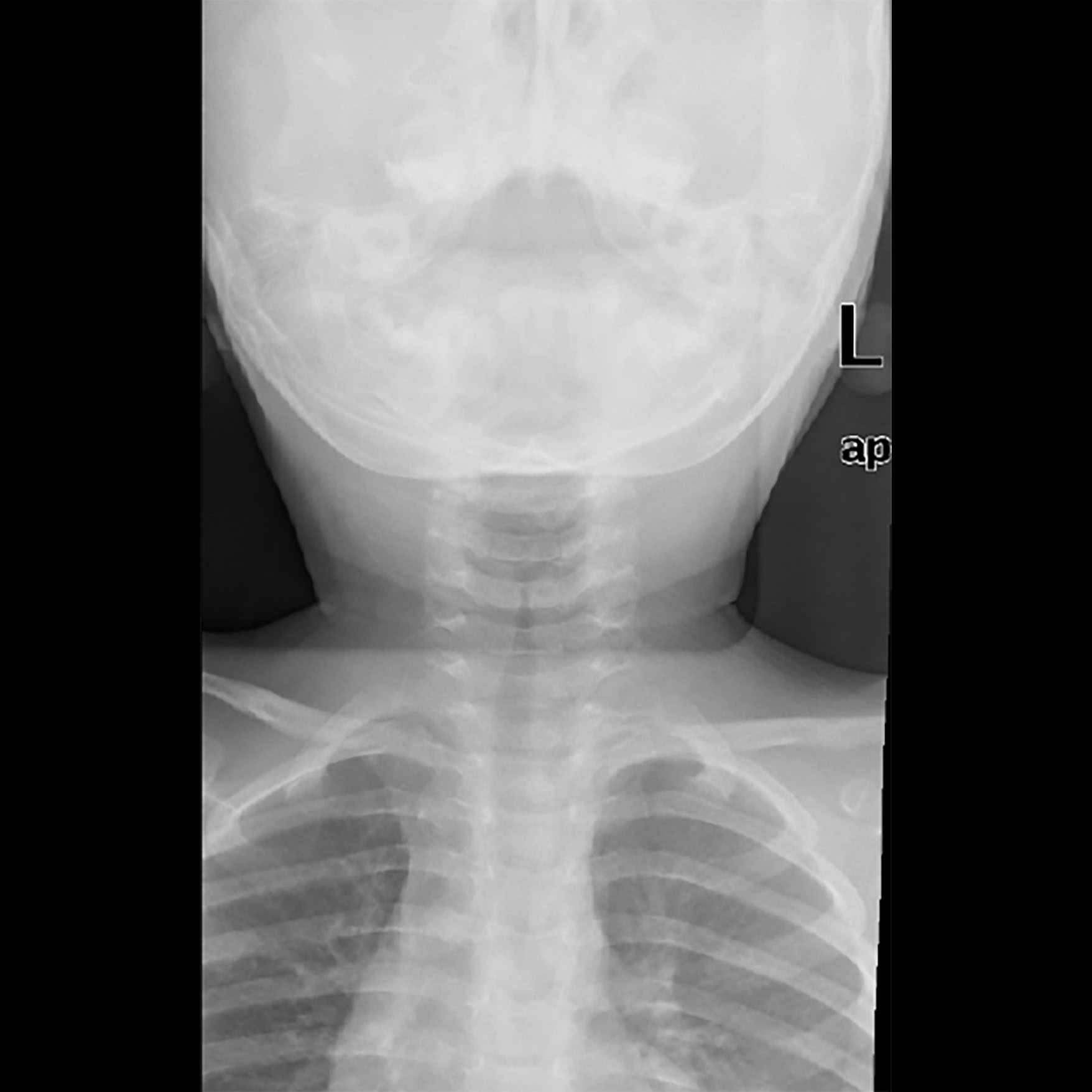
Figure 2. Epiglottitis, Thumb Sign
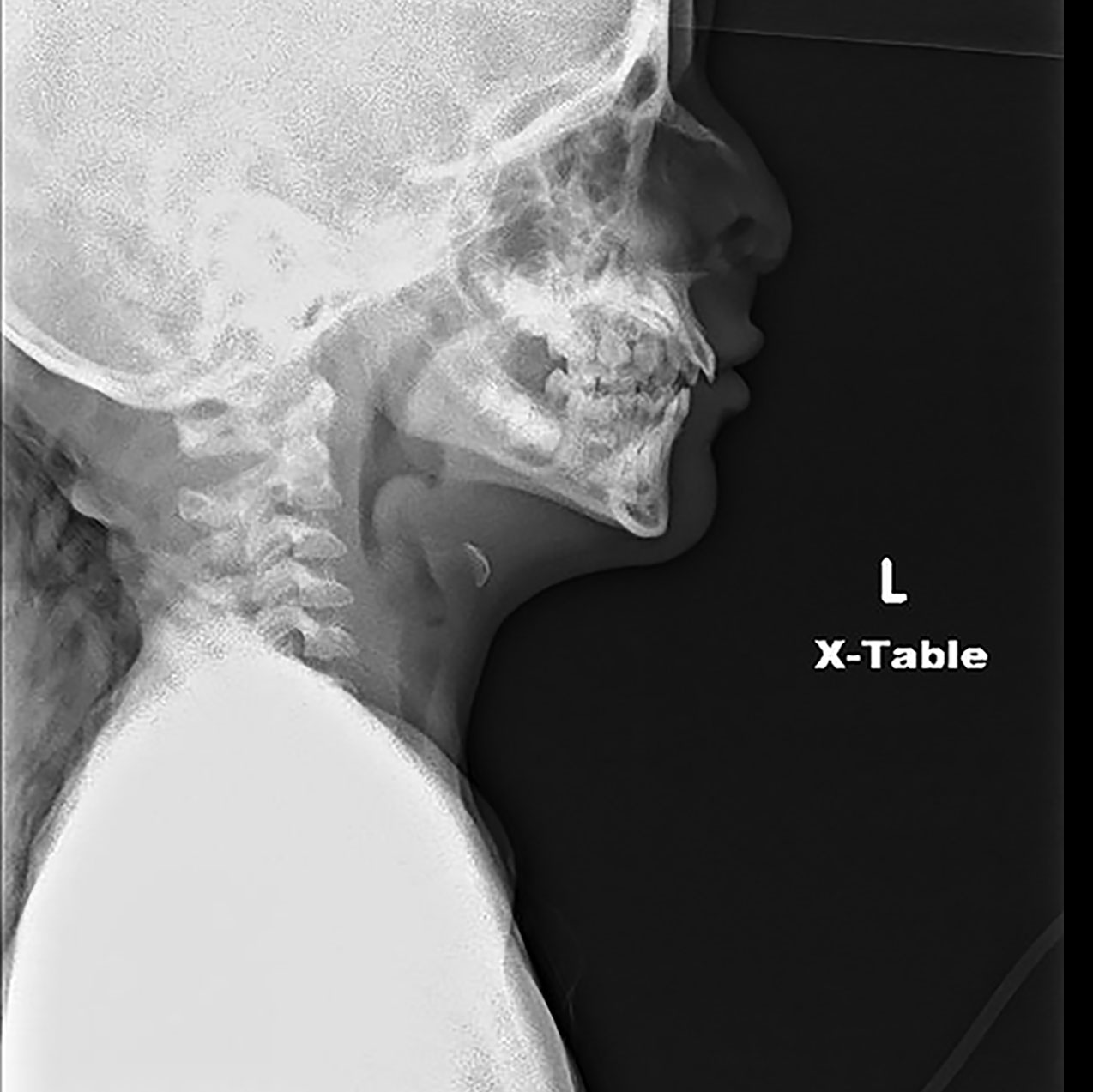
Advanced imaging such as computerized tomography (CT) or magnetic resonance imaging (MRI) should be done when a space-occupying lesion, such as a retropharyngeal or peritonsillar abscess, is suspected.28 A neck X-ray is not required for diagnosis of bacterial tracheitis, but if obtained it may reveal a ragged appearance of the tracheal wall, secondary to sloughing of the mucosa, and/or subglottic narrowing of the trachea.
Any patient suspected to have aspirated a foreign body should undergo a lateral and antero-posterior X-ray of the neck and chest. Historically, a good expiratory chest X-ray has been considered to be invaluable, since during expiration the object would obstruct the bronchus most completely, causing air trapping and expansion of the lung on the affected side and deviating the trachea from midline. However, a recent large study challenged this, demonstrating that the addition of an expiratory film to standard chest X-rays did not significantly change specificity or sensitivity of diagnosing foreign body aspirations.29 The same study also concluded that the addition of a decubitus view X-ray is not warranted, as it does not significantly increase accuracy.29 It is important to note that only radiopaque objects will be visible on X-ray. Neck X-rays (posteroanterior and lateral) are abnormal in 92% of lodged foreign body aspirations; only 58% of chest X-rays are abnormal. CT or MRI may be considered if suspicion remains following negative X-rays. If suspicion for a foreign body aspiration is very high, however, proceed directly to bronchoscopy.
When a tumor is suspected, obtain an MRI or CT scan, as well as a laboratory workup to screen for an oncologic process, including complete blood count (CBC), blood smear, LDH, and inflammatory markers. If a subglottic hemangioma is suspected, a CT or MRI should be performed and may reveal asymmetric narrowing of the trachea.26
Concern for a vascular abnormality impinging on the airway should be confirmed with a barium swallow study, which would reveal an indentation in the esophagus at the level of the malformation. Some children may require CT angiogram or MRI angiogram to confirm the diagnosis,30 and one of these studies ultimately will be needed to assess the specifics of the malformation to prepare for eventual surgery.
Figure 3. Foreign Body in Esophagus, Obstructing Airway
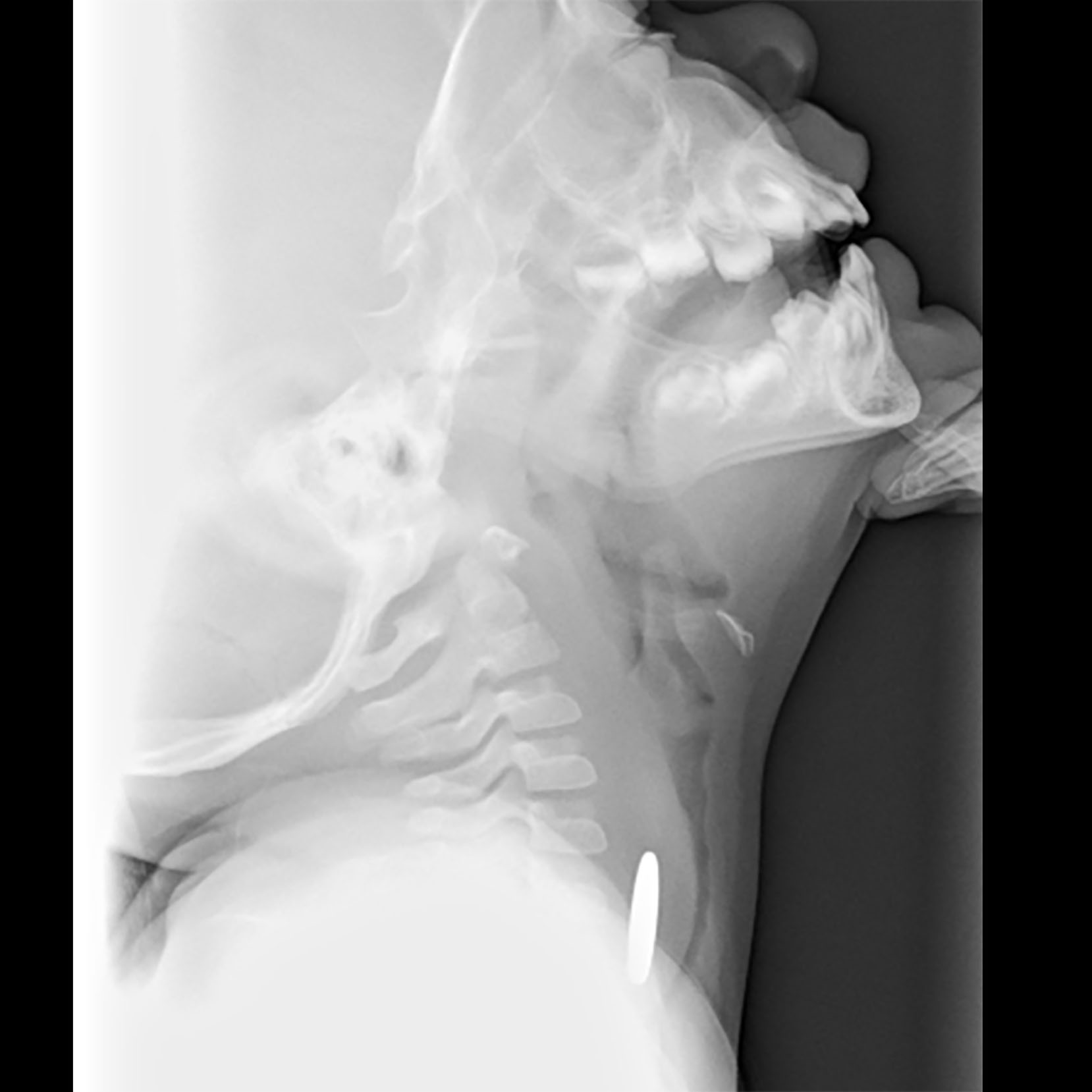
Figure 4. Retropharyngeal Abscess
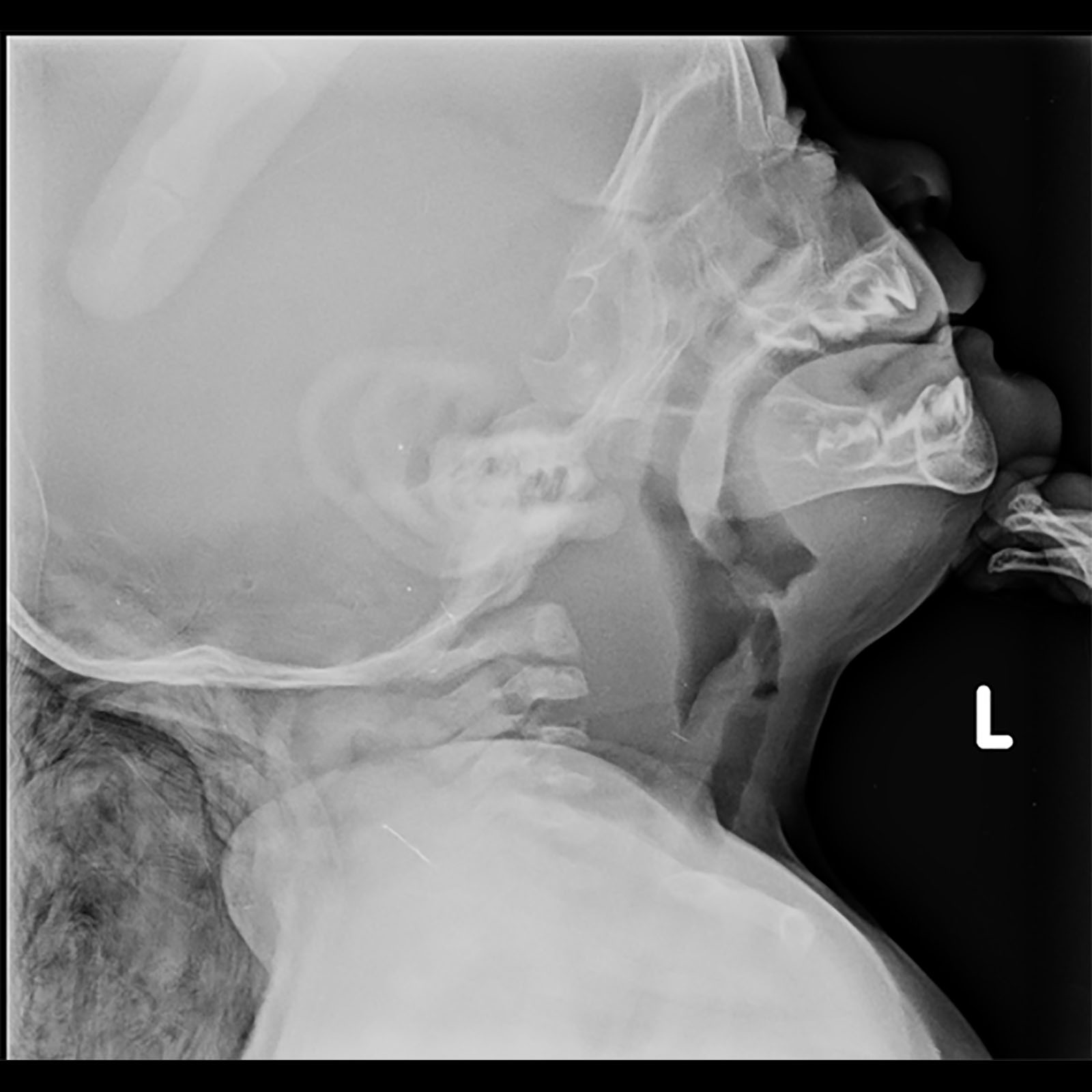
Management
Airway Management. As with any emergency situation, the top priorities are the patient’s airway, breathing, and circulation (ABCs). If the patient is in significant respiratory distress but continuing to breathe spontaneously, first consider high-flow nasal cannula, bilevel positive airway pressure, or continuous positive airway pressure. Urgent endotracheal intubation using rapid sequence intubation (RSI) may be required in a child who is hypoventilating, agonal, or apneic. As the cause of stridor is partial airway obstruction, endotracheal intubation may be challenging or unsuccessful depending on the etiology of the stridor, for example if there is a foreign body in the airway. If the etiology of the stridor is edema of the airway, intubation may exacerbate this, both acutely and following extubation. Thus, proceed with endotracheal intubation only when necessary.
If RSI is necessary, local protocols and drug availability will determine the drugs used. A typical agent used for sedation will be etomidate (0.3 mg/kg intravenous [IV]) or ketamine (1 to 2 mg/kg IV), with the latter preferred if there is concern for septic shock. The typical paralytic agent is succinylcholine (2 mg/kg IV in younger children, and 1 to 1.5 mg/kg IV in older children), unless there is a contraindicating crush injury, in which case rocuronium (1 mg/kg IV) is used. When intubating, use a smaller sized endotracheal tube than recommended for the child’s age to account for expected reduced airway diameter. External laryngeal manipulation may help improve visualization of the glottis in difficult airways. In rare cases when obstruction above the glottis makes endotracheal intubation impossible and the patient is unable to be ventilated, cricothyroidotomy may be necessary. In this case, a conduit for ventilation is passed through the cricothyroid membrane, which is located superior to the laryngeal prominence. In children younger than 10 years of age, the use of a 16- or 18-gauge needle passed through the central, lower portion of the cricothyroid membrane is preferred to the surgical cricothryoidotomy, which is used in older children and adults. This is because anatomical restriction of the area of the cricothyroid membrane exists in younger children. If the cricothyroid membrane is not appreciable in a young child, passing a needle through the tracheal rings inferiorly is also an acceptable option to provide ventilation. In such patients, transtracheal jet ventilation may be used, which provides high frequency and low tidal volume ventilation.
Croup. The first line of treatment for croup is glucocorticoids, which reduce inflammation and edema in the airway. Children presenting to the ED with croup should receive oral dexamethasone (0.6 mg/kg to a maximum of 20 mg); some studies indicate a lower dose may be effective as well. Meta-analyses have shown that glucocorticoids decrease return to the ED.31 The onset of action of glucocorticoids may be evident within about 30 minutes.11 Children presenting with croup also should receive nebulized dexamethasone concurrently, which acts as a vasoconstrictor and reduces airway edema. When stridor is actively present and the child is experiencing respiratory distress, nebulized L-epinephrine (3 mL, 1:1,000), which acts on alpha-adrenergic receptors to constrict pre-capillary arterioles in the airway to further reduce edema, should be administered. Nebulized treatments of epinephrine typically take about 20 minutes and are effective when compared to placebo.32 Patients should continue to receive nebulized L-epinephrine as frequently as necessary while stridor and respiratory distress persist. Providing cold air for inhalation has been suggested as a treatment for croup, as decreased temperature causes increased density of the air and, thus, less turbulence. The efficacy of this treatment, however, has not been established in the medical literature. Likewise, heliox has been noted anecdotally to improve stridor and respiratory distress, but a meta-analysis of relevant studies revealed no significant difference in outcomes.33
Laboratory testing typically is not indicated in children with croup unless there are concerns for concomitant dehydration, in which case serum electrolytes may be assessed. Routine confirmatory viral testing is not indicated.
Admit the patient if his or her stridor is progressive despite therapy, if it persists after two courses of L-epinephrine, or if he or she presented with hypoxia, cyanosis, altered mental status, or has had inadequate oral intake and requires IV fluids. Patients younger than 6 months of age or those returning to the ED also should be strongly considered for admission. Multiple studies have shown that approximately 8% of patients who present with croup require admission, while about 1% require ICU admission.11
Without treatment, the typical course of croup is self-limited, and studies have indicated that about 75% of stridor from croup will self-resolve within three days.11 Almost all resolve within one week of onset.
Spread of infection occurs in approximately 15% of patients, most commonly to the terminal bronchioles, pulmonary parenchyma, or the middle ear. Bacterial tracheitis also may develop after croup, secondary to the trauma caused to the tracheal wall by coughing.
Epiglottitis. If epiglottitis is suspected, attempt to visualize the epiglottis using a tongue depressor or with a laryngoscope if necessary. Historically, concern had been raised that manipulation of the oropharynx may trigger airway compromise, but this was premised on only two case reports,11 and thus should not dissuade the clinician from performing this important visualization. Confirmed epiglottitis warrants placement of an artificial airway as soon as context permits. Case series have shown that 6% of patients with epiglottitis who do not receive an artificial airway die, while less than 1% of those with an artificial airway die. The endotracheal tube used should be 0.5-1 mm smaller than what otherwise would be used for the patient to account for increased edema of the airway. Until an artificial airway can be placed, the patient is given nebulized L-epinephrine, which may reduce the size of the epiglottis, and the patient should receive oxygen via high-flow nasal cannula. To guide antibiotic management, CBC, blood culture, and respiratory culture from the epiglottis should be obtained after an artificial airway is established, and if concern for possible meningitis exists, cerebrospinal fluid analysis should be performed as well. The patient should be started on parenteral cefotaxime, ceftriaxone, or meropenem pending cultures, as up to 40% of H. influenzae type B are resistant to ampicillin. If MRSA is suspected based on trends in the community, or if the patient or family has a history of MRSA, add vancomycin.3 Intubated patients generally require admission to the ICU, and typically are ready to be extubated in two to three days, after antibiotics take effect. Antibiotic treatment should be continued for 10 days. Prophylaxis for all family members of a patient who tests positive for H. influenzae is indicated if there is any child younger than 4 years of age in the home who is inadequately or incompletely vaccinated for any reason. Prophylaxis is with rifampin (20 mg/kg PO once daily for four days).
Bacterial Tracheitis. Patients may require endotracheal intubation depending on their level of respiratory distress secondary to airway edema. The edema is most critical at the level of the cricoid cartilage, as this is the narrowest section of the airway and may be complicated by purulent secretions. Fifty to sixty percent of patients are intubated during their hospital course,2 with younger patients requiring intubation more frequently because of their smaller airway diameters. It is not uncommon for the endotracheal tube to become obstructed with thick secretions and result in a ball-valve effect which can lead to hyperdistention of the lungs and pneumothorax. If ventilation becomes difficult, the tube should be removed and a new tube inserted. Treatment with parenteral antibiotics should be initiated promptly. Empiric treatment should be started with clindamycin or vancomycin to cover gram-positive organisms, as well as a third-generation cephalosporin. Supplemental oxygen often is necessary as well. Toxic shock syndrome has been associated with Staphylococcal and group A streptococcus tracheitis,34 so monitor vital signs very closely. Patients with tracheitis should be admitted for continued antibiotic treatment and close observation. Tracheal edema typically begins to resolve within two to three days of appropriate antibiotics.
Peritonsillar and Retropharyngeal Abscess. Many abscesses will need drainage. Peritonsillar abscesses are often drained by emergency physicians, although very young children may require consultation. Regardless of whether an abscess is drained, administer clindamycin, amoxicillin-clavulanate, or ceftriaxone28 to treat for gram-positive organisms, which are almost always implicated.2 Obtain a CBC and blood culture. If incision and drainage is performed, ensure that a wound culture is collected so that bacterial speciation and susceptibilities can be identified to allow for the most efficacious use of antibiotics. If incision and drainage is successful and stridor resolves, the patient may be able to be discharged; if this is not the case, then he or she will require admission. Abscesses causing stridor often require admission to the ICU.
Foreign Body Aspiration. If an object is visible in the posterior oropharynx and the child is able to breathe, use your judgment as to whether it can be removed expediently in a safe manner. If not, removal should be performed in a controlled environment with a specialist present, as manipulation of the object may compromise the airway acutely. However, the risk of airway compromise exists if the object is not removed immediately. If the history suggests a foreign body aspiration and the child stops breathing, the Heimlich maneuver should be performed.
If no foreign body is visible in the oropharynx, an anteroposterior and lateral chest X-ray should be obtained. If X-rays are negative, CT or MRI is useful in identifying an aspirated foreign object, but is unnecessary if the history clearly suggests an aspiration, as bronchoscopy is indicated in all such cases.
If an object is identified, otolaryngology, pulmonary, general surgery, or anesthesia should be consulted to determine a plan for removal, in many instances by rigid bronchoscopy. Bronchoscopy has been found to be 97% effective in removing known objects.12 It is imperative that foreign bodies be identified and removed expediently; one study found a two-fold increase in complications in children who had a bronchoscopy more than 24 hours after presentation to the ED compared to those who had bronchoscopy within the first 24 hours.35 Another study showed that 19% of patients undergoing bronchoscopy had tracheal foreign bodies that had been aspirated more than 60 days prior.13 Late presenting signs of foreign body aspiration may include hemoptysis, fever, cough, and pneumonia. Gastroenterology should be consulted for removal of ingested foreign bodies that are lodged in the esophagus.
Tumors. All tumors causing stridor warrant admission and very close monitoring until the airway is no longer compromised. Be especially wary of the child who refuses to lay supine, as a mediastinal mass may be compressing the airway. Such a child requires immediate imaging to identify whether a mass exists. If a mass is deemed malignant, emergent radiation is required to shrink the size of the tumor. Steroids are contraindicated in any child for whom malignancy remains on the differential diagnosis.
Anaphylaxis. Allergic reactions with acute airway compromise should be treated emergently with intramuscular epinephrine in the outer thigh at a dose of 0.01 mg/kg.6 Monitor hemoglobin oxygen saturation and, if necessary, supplement with 8 to 10 L of O2 by face mask.6 Peripheral IV access should be obtained promptly, and the child should be given a bolus of 10 to 20 mL/kg of normal saline.6 Albuterol also may be considered as an adjuvant, although this will cause bronchodilation only through beta-adrenergic receptors in the lungs, and will have no effect on the alpha-adrenergic receptors in the mucosa of the airway, which are targeted by epinephrine. In the event of stridor and worsening respiratory distress refractory to epinephrine administration, endotracheal intubation may be necessary. Corticosteroids also should be given to reduce inflammation, although their effects will not be appreciated immediately. The length of observation prior to discharge or indications for admission vary according to the severity of the reaction and the institution.
At discharge, all patients should be prescribed a self-administering epinephrine device to be available at all times in case of recurrence. Recipients should be trained in proper use, and patients should be referred for IgE testing to confirm the responsible antigen and possible desensitization.6
Trauma and Caustic Ingestions. Trauma to the neck or chest may cause stridor, and likely will be a clear etiology based on patient history and physical exam. In these cases, stabilization of the neck using a collar is important, and emergent airway management may be necessary. If a foreign object was involved, ensure that no aspect of the object remains lodged in the neck; if it does, it must be removed surgically. If vascular compromise is suspected, obtain an urgent CT or MRI angiogram to assess the vascular structures. Monitor the child closely, as a hematoma may develop and compromise the airway. When assessing imaging, attempt to ascertain whether a hematoma, tracheal disruption, or simple edema is causing the stridor, as this will affect management. Crepitus on physical exam indicates compromise of the airway wall or the lungs.
Caustic trauma secondary to ingestion also may cause stridor — these patients should be admitted and otolaryngology should be consulted. Epiglottitis and other airway burns may result from aspiration of hot liquids, even hours after the incident.36 If experiencing acute respiratory distress, these patients may need to undergo tracheostomy to establish an artificial airway.
Other Etiologies of Stridor. Definitive diagnosis of stridor may require direct laryngoscopy if the diagnosis is not obvious. These include subglottic hemangiomas, laryngeal papillomatosis, vocal cord paralysis, subglottic stenosis, and laryngeal webs. Treatment for subglottic hemangiomas should be initiated after consultation. Propranolol recently has emerged as an effective first-line treatment option for involuting any hemagioma, particularly those that are compromising the airway.37 Its mechanism of action remains incompletely understood. Propranolol may cause hypotension, bradycardia, hypoglycemia, and bronchospasm, among other symptoms, so any patient who receives it should be monitored very closely and may require ICU admission.
If laryngeal papillomatosis is producing stridor, the lesions should be excised endoscopically. For vocal cord paralysis, depending on the etiology, the paralysis often resolves within six to 12 months of onset, although if it persists for more than three years it is unlikely to resolve. The likelihood of spontaneous resolution is greater than 50% whatever the cause;38 reinnervation also may be a possible option for some patients. Children with vocal cord paralysis should avoid foods that can be aspirated, such as nuts and seeds.
Subglottic stenosis typically needs to be 50% or more of the diameter of the airway to become symptomatic.39 If a patient requires intubation, it is crucial to use a small enough endotracheal tube, depending on the size of the child and the degree of stenosis. Emergent airway compromise, as in other cases, may require cricoidectomy or tracheostomy, although clearly this should be a last resort.
Patients with laryngeal webs should undergo CT of the neck, as about one-third of these patients also have a pulmonary artery sling. Treatment will depend on the extent and nature of the obstruction. In the case of enlarged pulmonary arteries secondary to pulmonary hypertension, the root cause of the pulmonary hypertension must be treated. Any vascular lesion causing stridor warrants an immediate consultation and admission. Any laryngeal cyst causing stridor should be resected.14
The diagnosis of laryngomalacia is clinical, but should be confirmed with laryngoscopy as an outpatient.40 In cases in which the patient is stable, the condition should be managed conservatively, as it often spontaneously resolves at 12-24 months of age, although this cannot be predicted accurately.41 Patients with apnea, hypoxia, or failure to thrive are candidates for surgical correction.42 Continuous positive airway pressure may help in keeping the airway open in the short term, as may a forward jaw thrust.
Summary
Obstructions of the airway that cause stridor can take many forms. Initial assessment of a patient with stridor should be expedient, particularly if respiratory failure has occurred or is imminent, and emergent airway management may be necessary. The causes of stridor are stratified into acute and chronic, and further into infectious and noninfectious. Fever and other symptoms consistent with infection suggest an infectious etiology, of which croup is most common. Suspicion of foreign body aspiration should be high until it can be ruled out. Eliciting a thorough history should help narrow the differential diagnosis, and X-rays and other imaging often can help confirm it. Many noninfectious sources of stridor will require laryngoscopy for definitive diagnosis. It is important to remember that congenital sources of stridor may present well after birth, often in the context of a viral upper respiratory infection.
REFERENCES
- Lee SS, Schwartz RH, Bahadori RS. Retropharyngeal abscess: Epiglottitis of the new millennium. J Pediatr 2001;138:435-437.
- Long S. Respiratory tract symptom complexes. In: Long S, Pickering LK, Prober CG. Principles and Practice of Pediatric Infectious Diseases, 4th ed. Elsevier;2012:162-171.
- Richards AM. Pediatric respiratory emergencies. Emerg Med Clin North Am 2016;34:77-96.
- Centers for Disease Control and Prevention. Nonfatal choking-related episodes among children — United States, 2001. MMWR Morb Mortal Wkly Rep 2002;51:945-948.
- Chapin MM, Rochette LM, Annest JL, et al. Nonfatal choking on food among children 14 years or younger in the United States, 2001–2009. Pediatrics 2013;132:275-281.
- Simons FE, Sampson HA. Anaphylaxis: Unique aspects of clinical diagnosis and management in infants (birth to age 2 years). J Allergy Clin Immunol 2015;135:1125-1131.
- Kelso JM, Greenhawt MJ, Li JT, et al. Adverse reactions to vaccines practice parameter 2012 update. J Allergy Clin Immunol 2012;130:25-43.
- Hemangioma Investigator Group, Haggstrom AN, Drolet BA, Baselga E, et al. Prospective study of infantile hemangiomas: Demographic, prenatal, and perinatal characteristics. J Pediatr 2007;150:291-294.
- Licari A, Manca E, Rispoli GA, et al. Congenital vascular rings: A clinical challenge for the pediatrician. Pediatr Pulmonol 2015;50:511-524.
- Hamilton J, Yaneza MM, Clement WA, Kubba H. The prevalence of airway problems in children with Down’s syndrome. Int J Pediatr Otorhinolaryngol 2016;81:1-4.
- Petrocheilou A, Tanou K, Kalampouka E, et al. Viral croup: Diagnosis and a treatment algorithm. Pediatr Pulmonol 2014;49:421-429.
- Cevik M, Gokdemir MT, Boleken ME, et al. The characteristics and outcomes of foreign body ingestion and aspiration in children due to lodged foreign body in the aerodigestive tract. Pediatr Emerg Care 2013;29:53-57.
- Safari M, Manesh, M. Demographic and clinical findings in children undergoing bronchoscopy for foreign body aspiration. Ochsner J 2016;16:120-124.
- Pfleger A, Eber E. Assessment and causes of stridor. Paediatr Respir Rev 2016;18:64-72.
- Breysem L, Goosens V, Vander Poorten V, et al. Vallecular cyst as a cause of congenital stridor: Report of five patients. Pediatr Radiol 2009;39:828-831.
- Chou CT, Siegel B, Mehta D. Stridor and apnea as the initial presentation of primary hypoparathyroidism. Int J Pediatr Otorhinolaryngol 2016;80:30-32.
- Venkatesh C, Chhavi N, Gunasekaran D, Soundararajan P. Acute stridor and wheeze as an initial manifestation of hypocalcemia in an infant. Indian J Endocrinol Metab 2012;16:320-321.
- Train JJ, Yates RW, Sury MR. Hypocalcaemic stridor and infantile nutritional rickets. BMJ 1995;310:48.
- Stein R, Fish S, Godwin B, et al. Respiratory system manifestations of pediatric Crohn disease: A report of three cases. Inflammatory Bowel Diseases 2014;20(Suppl 1):S77.
- Kelts G, O’Connor PD, Hussey RW, Maturo S. An electrical cause of stridor: Pediatric vagal nerve stimulators. Int J Pediatr Otorhinolaryngol 2015;79:251-253.
- Westley CR, Cotton EK, Brooks JG. Nebulized racemic epinephrine by IPPB for the treatment of croup: A double-blind study. Am J Dis Child 1978;132:484-487.
- Tibballs J, Watson T. Symptoms and signs differentiating croup and epiglottitis.J Paediatr Child Health 2011;47:77-82.
- De Pasquale MD, Crocoli A, Conte M, et al. Mediastinal germ cell tumors in pediatric patients: A report from the Italian Association of Pediatric Hematology and Oncology. Pediatr Blood Cancer 2016;63:808-812.
- Sathyamoorthy M, Lerman J, Asariparampil R, et al. Stridor in neonates after using the Microcuff and uncuffed tracheal tubes: A retrospective review. Anesth Analg 2015;121:1321-1324.
- Rudders SA, Banerji A, Clark S, Camargo CA Jr. Age-related differences in the clinical presentation of food-induced anaphylaxis. J Pediatr 2011;158:326-328.
- King-Shultz LW, Orvidas LJ, Mannenbach MS. Stridor is not always croup. Pediatr Emerg Care 2015;31:140-143.
- Ting M, Roseby R, McAdam C. Subglottic infantile haemangioma: A rare but important consideration in young infants presenting with stridor. J Paediatr Child Health 2016;52:1111-1113.
- Grisaru-Soen G, Komisar O, Aizenstein O, et al. Retropharyngeal and parapharyngeal abscess in children — Epidemiology, clinical features and treatment. Int J Pediatr Otorhinolaryngol 2010;74:
1016-1020. - Brown JC, Chapman T, Klein EJ, et al. The utility of adding expiratory or decubitus chest radiographs to the radiographic evaluation of suspected pediatric airway foreign bodies. Ann Emerg Med 2013;61:19-26.
- Rogers DJ, Cunnane MB, Hartnick CJ. Vascular compression of the airway: Establishing a functional diagnostic algorithm. JAMA Otolaryngol Head Neck Surg 2013;139:586-591.
- Russell KF, Liang Y, O’Gorman K, et al. Glucocorticoids for croup. Cochrane Database Syst Rev 2011;(1):CD001955.
- Eghbali A, Sabbagh A, Bagheri B, et al. Efficacy of nebulized L-epinephrine for treatment of croup: A randomized, double-blind study. Fundam Clin Pharmacol 2016;30:70-75.
- Moraa I, Sturman N, McGuire T, van Driel ML. Heliox for croup in children. Cochrane Database Syst Rev 2013;12:CD006822.
- Tak R, Semmekrot B, Warris A, et al. Bacterial tracheitis and septic shock. Pediatr Infect Dis J 2016;35:226-227.
- Shlizerman L, Mazzawi S, Rakover Y, Ashkenazi D. Foreign body aspiration in children: The effects of delayed diagnosis. Am J Otolaryngol 2010;31:320-324.
- Kudchadkar SR, Hamrick JT, Mai CL, et al. The heat is on … thermal epiglottitis as a late presentation of airway steam injury.
J Emerg Med 2014;46:e43-e46. - Drolet BA, Frommelt PC, Chaplin SL, et al. Initiation and use of propranolol for infantile hemangioma: Report of a consensus conference. Pediatrics 2013;131:128-140.
- de Gaudemar I, Roudaire M, Francois M, Narcy P. Outcome of laryngeal paralysis in neonates: A long term retrospective study of 113 cases. Int J Pediatr Otorhinolaryngol 1996;35:101-110.
- Zdanski C, Davis S, Hong Y, et al. Quantitative assessment of the upper airway in infants and children with subglottic stenosis. Laryngoscope 126:1225-1231.
- Cooper T, Benoit M, Erickson B, El-Hakim H. Primary presentations of laryngomalacia. JAMA Otolaryngol Head Neck Surg 2014;140:521-526.
- Isaac A, Zhang H, Soon SR, et al. A systematic review of the evidence on spontaneous resolution of laryngomalacia and its symptoms. Int J Pediatr Otorhinolaryngol 2016;83:78-83.
- Cheng J, Smith L. Endoscopic surgical management of inspiratory stridor in newborns and infants. Am J Otolaryngol 2015;36:697-700.
- King C, Rappaport LD. Emergent endotracheal intubation. In: King C, Henretig FM, et al. Textbook of Pediatric Emergency Procedures, 2nd ed. Lippincott Williams and Wilkins;2008:152.
Stridor is a high-pitched, monophonic sound caused by turbulent air flow through a narrowed airway, and is a common symptom among young children presenting to the emergency department.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
