Penetrating Neck Trauma
July 1, 2017
Reprints
AUTHORS
Dennis P. Hanlon, MD, FAAEM, Quality Director, Department of Emergency Medicine, Allegheny General Hospital, Pittsburgh, PA.
Daniel A. Adams, MD, Department of Emergency Medicine, Allegheny General Hospital, Pittsburgh, PA.
PEER REVIEWER
Jay Menaker, MD, Associate Professor of Surgery and Emergency Medicine, R Adams Cowley Shock Trauma Center, University of Maryland, Baltimore.
Statement of Financial Disclosure
To reveal any potential bias in this publication, and in accordance with Accreditation Council for Continuing Medical Education guidelines, Dr. Dietrich (editor in chief), Dr. Hanlon (author), Dr. Adams (author), Dr. Menaker (peer reviewer), Ms. Behrens (nurse planner), Ms. Mark (executive editor), Ms. Coplin (executive editor), and Ms. Hatcher (AHC Media editorial group manager) report no relationships with companies related to this field of study.
EXECUTIVE SUMMARY
- More recently, Zone I has been proposed to extend from below the cricoid cartilage to the sternal angle to more precisely define a thoracocervicoaxillary region, which includes the vascular structures running from the aortic arch into both the base of the neck as well as those coursing behind the clavicles into the axilla.
- In recent studies, Zone II is the most common site of injury (38-67%), followed by Zone III (16-19%), and Zone I (13-18%).
- Overt or “hard” signs that suggest major vascular or aerodigestive tract injury include airway compromise, air bubbling in the wound and/or subcutaneous emphysema, an expanding or pulsatile hematoma, active bleeding, shock, hematemesis, and neurologic deficit.
- The Prehospital Trauma Life Support Program of the American College of Surgeons no longer recommends spinal immobilization in penetrating neck trauma because of a lack of data to support its use and potential complications associated with its use (interfered with other life-saving interventions like airway management, caused delay in transport, or was responsible for delayed recognition of clinically important injuries).
- Given the current state of the evidence, the approach of avoiding cervical spine immobilization in the majority of patients with isolated PNT unless there is a neurologic deficit present is recommended.
- Indications for emergent airway management with RSI include inability to protect the airway because of altered mental status, airway compromise and aspiration risk because of blood and/or secretions in the airway, expanding neck hematoma, and inability to oxygenate or ventilate adequately.
- Video laryngoscopy with devices such as the GlideScope offer improved visualization of the glottis and may decrease the number of failed intubations in patients with a difficult airway.
- Selective operative management in penetrating neck trauma is supported by a significant body of literature. This approach has been demonstrated to decrease unnecessary operative neck exploration by approximately 50-60% without an increase in mortality or complication rates.
Penetrating neck trauma presents a clinical challenge to the emergency physician. Patients may present in extremis requiring emergent airway and hemorrhage control, whereas others can have subtle signs of injury that require careful investigation so that an injury is not missed. Clinicians must have a planned approach to these patients to optimize outcomes.
— Ann M. Dietrich, MD, Editor
Introduction
Penetrating injuries to the neck historically have been a unique challenge to emergency physicians, both because of the range in severity of these injuries, and because the extent of injury may not be apparent immediately on initial evaluation. While some patients will present in extremis, requiring immediate airway control, resuscitative intervention, and emergent operative exploration, others may present without obvious physiologic derangements, yet have serious occult aerodigestive, vascular, and/or neurologic injuries. These injuries may reside within the anatomic borders of the neck or extend into critical nearby structures.
Optimal management of these injuries requires an understanding of the anatomic structures that can be injured within the neck via direct penetration or blast injury of other vital structures. Recently, a shift has occurred in how these injuries are evaluated and managed at trauma centers. After initial resuscitative interventions, a thorough diagnostic evaluation and a high index of suspicion for occult injury in the emergency department (ED) is necessary to avoid missed injuries. A more selective approach to surgery has been advocated over mandatory exploration. The roles of computed tomographic angiography (CTA), traditional angiography, bronchoscopy, and esophagoscopy are still debated.
This review will present an approach to the ED evaluation and management of patients with penetrating neck trauma (PNT).
Anatomy
The neck is perhaps the most complex region in human anatomy because of the proximity of many structures. The neck is a complex network of airway, vascular, digestive, endocrine, lymphatic, musculoskeletal, and neurologic structures. The most important superficial structure in the initial evaluation and management of PNT is the platysma muscle. The platysma arises from the superior borders of the pectoralis major and deltoid muscles and extends to the inferior aspect of the mandible. By definition, a penetrating injury that violates the platysma is PNT and requires further evaluation.1
Traditionally, the neck has been divided into three zones for the management of PNT.2 Zone I was defined originally as being below the level of the clavicles, with Zone II extending from the clavicles to the angle of the mandible, and Zone III extending from the angle of the mandible to the base of the skull. (See Table 1.) Many emergency physicians will be more familiar with a modification to this anatomic classification, which defines the superior border of Zone I as the inferior cricoid cartilage.3
Studies and guidelines for the management of PNT have used both the original and modified anatomic classifications for Zone I. In the United States, for example, the Western Trauma Association’s (WTA) algorithm for PNT (2013) uses the original zones of the neck,1 while the Eastern Association for the Surgery of Trauma’s (EAST) practice guideline (2008) uses the modified classification.4 (See Figure 1.)
Table 1. Anatomic Contents of the Zones of the Neck
Zone |
Location |
Anatomic Contents |
|
I |
Sternal notch of clavicle to cricoid cartilage |
Major vasculature of superior mediastinum, subclavian artery and vein, common carotid artery, vertebral artery, internal jugular vein, trachea, lung apex, esophagus, thyroid, vagus nerve, recurrent laryngeal nerve, phrenic nerve, spine |
|
II |
Cricoid cartilage to angle of mandible |
Common carotid artery, internal and external carotid arteries, vertebral artery, jugular veins, trachea, larynx, pharynx, esophagus, phrenic nerve, vagus nerve, recurrent laryngeal nerve, spine |
|
III |
Angle of mandible to skull base |
Internal and external carotid arteries, vertebral artery, jugular veins, oropharynx, salivary glands, parotid glands, cranial nerves IX-XII |
Figure 1. Zones of the Neck
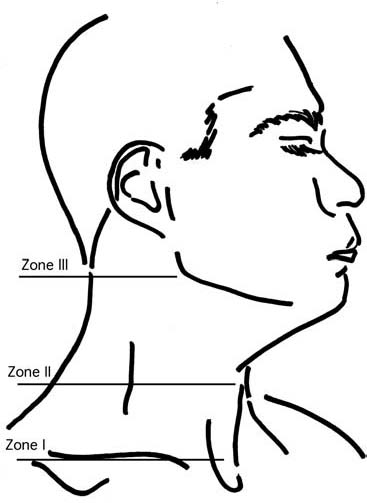
Illustration by Marcus Eubanks, MD.
More recently, Zone I has been proposed to extend from below the cricoid cartilage to the sternal angle to more precisely define a thoracocervicoaxillary region, which includes the vascular structures running from the aortic arch into both the base of the neck as well as those coursing behind the clavicles into the axilla.5 However, the zone in which an external wound to the neck is located does not necessarily correlate with the location of injured internal structures, as the vector of the penetrating object or missile is unpredictable.6
The neck also can be demarcated anteroposteriorly by the posterior border of the sternocleidomastoid muscle.1 The well-known anterior and posterior triangles of the neck may be of relevance, as the majority of critical structures are located in the anterior triangle. The anterior triangle lies between the anterior midline of the neck, the mandible, the anterior border of the sternocleidomastoid, and the clavicle, whereas the posterior triangle is defined by the posterior border of the sternocleidomastoid, the clavicle, and the trapezius. The most recent WTA and EAST guidelines do not include the triangles of the neck in their algorithm for PNT.1,4
Types of Injury and Pathophysiology
The etiology of PNT can be divided into wounds inflicted by low- and high-velocity weapons. The definition of low and high velocity in regard to ballistics is controversial, with low-velocity weapons being described in the range between 335 to 914 m/sec by various researchers.7 Low-velocity PNT includes stab wounds from knives and other miscellaneous objects, as well as projectiles from handguns and long-range wounds inflicted by birdshot and buckshot. High-velocity PNT includes wounds inflicted by rifles, as well as those from explosive devices, including bombs and improvised explosive devices. Low-velocity PNT causes direct injury to structures along the vector of the penetrating object and a permanent cavity created by the wound. Because of tissue displacement by temporary cavitation created by high-velocity weapons, the pattern in these injuries often is more severe and unpredictable.7 The type of projectile used also can affect the injury pattern, as in the case of expanding soft-point and hollow-point bullets, which may cause extensive tissue disruption.7
Vascular injury in PNT can be secondary to direct injury by the penetrating object itself, and from indirect injury from temporary cavitation and shear forces. Vascular injuries seen in PNT include vessel transection, laceration, and puncture, intimal flaps, and pseudoaneurysms. Thrombosis, arteriovenous fistulae, and pseudoaneurysms also may present in a delayed fashion after initial trauma.
Epidemiology
Data published in the past 10 years have identified PNT as a relatively uncommon reason for admission to civilian trauma centers in the United States, with a recent large series from both the Los Angeles County/University of Southern California Medical Center and the R Adams Cowley Shock Trauma Center in Baltimore reporting PNT accounting for approximately 1.7% of their trauma center admissions.8 In the United States, penetrating neck trauma most commonly is secondary to stabbings and gunshot wounds (GSW), with stab wounds recently reported as the etiology of 40-75% of cases, GSW in 24-48% of these injuries, and other miscellaneous causes being less common.8-11 The range in etiology published likely is due to differences in prevalence of firearm-related injuries in various regions of the United States.
Males are approximately four times more likely to be affected by PNT, and the mean age of patients with PNT in the United States is approximately 30 years. In recent studies, Zone II is the most common site of injury (38-67%), followed by Zone III (16-19%), and Zone I (13-18%).8-11 Approximately 50% of patients with GSW and 10-20% of patients with stab wounds will have significant injuries, and the mortality for major vascular injuries approaches 50%.4 Overall mortality from PNT has been reported as 1.3-3% in the United States in the past 10 years, but these data do not include patients who did not survive to presentation to the hospital.8-11
Clinical Features of Penetrating Neck Trauma
The presentation of PNT may range from patients who are hemodynamically stable and relatively asymptomatic to patients presenting in shock with active exsanguination and/or airway compromise. Unstable patients require immediate intervention and operative exploration. In stable, asymptomatic or mildly symptomatic patients, a thorough and systematic evaluation must be employed to avoid missing subtle findings of occult injury. Overt or “hard” signs that suggest major vascular or aerodigestive tract injury include airway compromise, air bubbling in the wound and/or subcutaneous emphysema, an expanding or pulsatile hematoma, active bleeding, shock, hematemesis, and neurologic deficit.1 (See Table 2.) The presence of hard signs of injury indicates the need for immediate operative exploration. This occurs in less than 10% of patients presenting with PNT; however, it is highly specific for serious vascular and/or aerodigestive tract injury. A recent prospective study identified hard signs as having an 89.7% positive predictive value for vascular and/or aerodigestive injury identified at immediate operative neck exploration.8 A small, retrospective study proposed a more selective approach to stable patients with Zone II injuries and hard signs. This study concluded that incorporating CTA into the evaluation would decrease negative explorations significantly without increasing missed injuries.12 Most authorities disagree with this conclusion.1,8
Table 2. Hard Signs of Major Vascular or Aerodigestive Tract Injury in Penetrating Neck Trauma
- Airway compromise
- Massive subcutaneous emphysema/air bubbling through wound
- Expanding or pulsatile hematoma
- Active bleeding
- Shock
- Hematemesis
- Neurologic deficit
Stable patients without hard signs on physical examination still may have significant injuries. Modest or moderate (“soft”) signs of vascular injury include prehospital reports of bleeding from the wound; the proximity of the wound to the expected course of carotid artery or jugular vein; and/or the presence of a non-expanding hematoma, subtle neurologic deficits, the presence of a palpable thrill or audible bruit, and/or brachial or radial artery pulse deficits.13,14 (See Table 3.) Many authorities consider palpable thrills or bruits to be hard signs.
Table 3. Soft Signs and Symptoms of Vascular Injury in Penetrating Neck Trauma
- Prehospital bleeding from the wound
- Proximity of the wound to the carotid artery or jugular vein
- Presence of a non-expanding hematoma
- Subtle neurologic deficits or signs of cerebral ischemia
- Palpable thrill or bruit audible in neck*
- Pulse deficit in the upper extremity
* Some classify as a hard sign.
Soft signs and symptoms of laryngotracheal injury include change in voice, hoarseness, palpable crepitus, hemoptysis, air leaking through the wound, and cervical or mediastinal air seen on neck or chest radiographs.13 (See Table 4.) Patients with suspicion of laryngotracheal injury may benefit particularly from endoscopic evaluation of the airway with a fiberoptic bronchoscope, both for diagnostic and therapeutic purposes. This technique may allow insertion of the endotracheal tube and inflation of its cuff distal to the injury, preventing massive air leak.15
Isolated injuries to the esophagus are uncommon because of the relatively protected anatomic location of the esophagus in the neck, and patients with esophageal injuries often have other severe injuries.14 Overall mortality of patients with esophageal injury in PNT has been reported at 19-44%, with many of these deaths occurring within the first 24 hours after injury.17,18 Soft signs of esophageal injury include deep neck pain, hematemesis, odynophagia and dysphagia, and air visualized in the neck or mediastinum on neck or chest radiographs.13 (See Table 5.) Although esophageal injury is uncommon in PNT, with an incidence reported at less than 5%, early recognition of esophageal injury is paramount, as delay in operative intervention has been associated with significantly increased mortality.17 Patients with missed esophageal injury can succumb to mediastinitis and septic shock later in their hospital course. Delayed diagnosis of esophageal injury also may be associated with a higher likelihood of failing primary esophageal repair and requiring more aggressive surgical intervention with esophagectomy.19
Table 4. Soft Signs and Symptoms of Airway Injury in Penetrating Neck Trauma
- Change in voice and/or hoarseness
- Palpable crepitus
- Hemoptysis
- Air leak through wound
- Cervical and/or mediastinal air visualized on X-ray
Table 5. Soft Signs of Esophageal Injury in Penetrating Neck Trauma
- Deep neck pain
- Hematemesis
- Odynophagia
- Dysphagia
- Cervical or mediastinal air visualized on X-ray
Injuries to the nervous system in PNT occur in approximately 7% of cases20 and can include direct cervical spinal injury (with or without cord injury) and injuries to both peripheral and cranial nerves coursing through the neck. Ischemic stroke also may occur in the setting of vascular injury, particularly in the setting of carotid injury, although neurologic deficits in these patients can be due to alcohol or drugs, as well as hypotension.13
Cervical spine injury is very uncommon in patients with stab wounds to the neck, with rates reported from 0-1.5%.20,21 However, these injuries are significantly more common in GSW to the neck, with reported rates of associated cervical spine injuries of 12-18%.20-22 Unstable cervical spine injuries in PNT are very rare (< 0.5% of GSW to the neck) and are associated with severe focal neurologic deficit or altered mental status.21
Prehospital Care of Penetrating Neck Trauma
In PNT, time to definitive treatment is critical. The initial prehospital management of PNT should include a focused primary survey, performance of emergent life-sustaining maneuvers (if indicated), and rapid transport to a trauma center.23 A secondary survey can be completed en route.
Airway compromise after PNT can occur early after injury. Signs of respiratory distress, airway obstruction, laryngotracheal injury, altered mental status, and expanding neck hematoma are clinical signs that airway control may be required prehospital. If the patient is in respiratory distress at the scene or there is concern for progression to airway compromise en route, rapid sequence induction (RSI) with orotracheal intubation should be considered prior to transport. There is a risk of dislodging a contained neck hematoma with direct laryngoscopy and orotracheal intubation, and surgical airway may be the only possibility of securing the airway if orotracheal intubation fails. If possible, prehospital RSI and orotracheal intubation should be avoided in many urban settings where transport time to the trauma center is short. In patients with concern for airway obstruction from bleeding, laying the patient back may precipitate loss of airway patency. These awake patients can be transported in an upright position while using continuous suction with a Yankauer catheter to maintain airway patency, allowing for rapid hospital transport.
In patients who require prehospital airway control, orotracheal intubation is the intervention of choice. If orotracheal intubation fails, a supraglottic airway may be a potential temporizing measure, although surgical cricothyroidotomy may be the only viable option (depending on the skills/credentialing of the prehospital provider). Although prehospital cricothyroidotomy is controversial, there are some data that it can be performed with a high rate of success by trained personnel. In a military database of life-saving procedural interventions performed by combat medics on 1,927 patients, 34 had prehospital cricothyroidotomy performed, primarily in the setting of severe head, face, and neck trauma. Eighty-six percent of these procedures were successful.24 In some patients with open tracheal injury, the injury itself may create a visible site for direct intubation of the trachea.
In cases of respiratory failure or hemodynamic instability, prehospital providers may consider needle thoracostomy.23 The apices of the lungs are at risk in PNT and may extend anatomically into Zone I. Although prehospital needle thoracostomy is controversial, it has been shown to have very few instances of actual complications in several recent series; it is likely to be most beneficial in patients who still have vital signs.25-27 The most common adverse event of prehospital needle thoracostomy is unsuccessful placement, and longer angiocatheters have been associated with a significantly higher degree of success without an increase in complications.28 A lateral approach to needle thoracostomy also may increase success rates, as the chest wall is thinner in the mid-axillary line.29
Prehospital circulatory resuscitative care focuses on hemorrhage control while en route to the hospital. Sources of hemorrhage should be controlled with direct pressure. In most cases of PNT in urban settings, prehospital intravenous access should not be obtained routinely, as it likely prolongs on-scene times.30 Although more studies are needed, prolonged on-scene time has been associated with increased mortality in trauma patients in several recent retrospective analyses.31,32 Further, advanced life support interventions have been linked to increased mortality in penetrating trauma patients in the urban environment,33,34 and a case has been made for a “scoop and run” approach to prehospital care in urban penetrating trauma, including some advocating for rapid police transport of patients directly to a trauma center without EMS intervention.35,36 Moribund patients with PNT require rapid transport to a trauma center for immediate operative intervention.
Whether cervical spine immobilization is beneficial in PNT is somewhat controversial, as many of these injuries are not unstable nor would they benefit from immobilization. A recent retrospective review associated cervical spine immobilization with an increased risk of death in PNT, with the authors postulating that cervical spine immobilization may have interfered with other life-saving interventions like airway management, caused delay in transport, or was responsible for delayed recognition of clinically important injuries.37 The Prehospital Trauma Life Support Program of the American College of Surgeons38 no longer recommends spinal immobilization in penetrating neck trauma because of a lack of data to support its use. Further, spinal immobilization has been associated with a transport time delay of 2-5.5 minutes.39,40 This time delay potentially can harm patients as noted above, and cervical spine immobilization also can increase the difficulty of airway management and not allow for continuous visual assessment of the anterior neck, potentially delaying recognition of life-threatening conditions like an expanding neck hematoma.41
A recent cost-utility analysis of prehospital spine immobilization in penetrating trauma labeled the cost-benefit of spine immobilization as “equivocal” (in cases of PNT specifically), stating that more studies are needed.42 Given the current state of the evidence, we favor the approach of avoiding cervical spine immobilization in the majority of patients with isolated PNT unless there is a neurologic deficit present. With altered mental status or neurologic deficit, cervical spine immobilization may be attempted, particularly because concomitant blunt cervical injury cannot be ruled out in patients who are altered, and there is a small subset of patients with neurologic deficit and GSW to the neck who have unstable cervical spine injury. However, patients with PNT who are in respiratory distress, hemodynamically unstable, and/or moribund should be transported rapidly to a trauma center without delay for placement of a cervical immobilizer.
ED Management of Penetrating Neck Trauma
The initial evaluation and management of patients who present to the ED with PNT is similar to any potential major trauma patient and should follow standard Advanced Trauma Life Support protocols.43 This approach ensures systematic attention to immediate life-threatening injuries and reduces the potential for missed injuries. When resources are available, different aspects of the resuscitation should be performed concurrently by multiple providers in a team-based approach to expedite stabilization. The emergency provider must determine if the wound violates the platysma, which defines PNT. In the absence of clinical suspicion for other traumatic injuries, wounds that do not violate the platysma may be managed with appropriate wound care, and the patient may be discharged home. The probing or exploration of wounds that violate the platysma should be avoided outside of the operating room because of the potential for clot dislodgement and risk of subsequent hemorrhage.
Of primary concern in patients with PNT are airway compromise and potential for exsanguinating vascular injury. A primary survey should be performed rapidly, with concurrent evaluation and management as indicated by the clinical situation. Supplemental oxygen is provided for preoxygenation in anticipation of the need for endotracheal intubation, vital signs are monitored, and vascular access is obtained with at least two large-bore (18-gauge or larger) intravenous or intraosseous catheters. Venous access is established preferentially opposite the site of injury. The entire skin surface must be exposed and inspected to avoid delayed recognition of other traumatic injuries.
Airway
Airway management in patients with PNT can be challenging for even the most experienced provider. The airway in PNT can be complicated by direct airway trauma, including tracheal laceration and transection, excess blood and secretions in the airway, and anatomic distortion by tissue disruption and hematoma formation. These patients may be exsanguinating concurrently from vascular injury, creating highly stressful and time-sensitive intubating conditions. In a retrospective analysis of 748 patients with PNT, 11% of patients presented with active airway compromise requiring immediate airway control.44 Early airway control is mandatory in patients with respiratory distress or anticipated loss of airway patency. Regardless of the method of initial attempts at airway control, providers should be prepared to secure the airway surgically should these fail.
Assessment of the airway in patients with PNT includes assessment of the patients’ ability to phonate, how well they are tolerating secretions, examination of the exterior neck for evidence of laryngotracheal or significant vascular injury, and gross assessment of the patients’ mental status and ability to protect their airway. A focused physical exam should assess for tracheal deviation, soft tissue crepitance, air bubbling, and expanding hematomas, which could compress the airway or distort its anatomy. The oropharynx also should be inspected rapidly to assess for blood and other signs of trauma, such as tongue swelling, pharyngeal swelling or asymmetry, and/or a deviated uvula. A laryngoscope can be used to obtain a view of the oropharynx in the awake patient by using its blade as a tongue depressor.
Lateral soft tissue neck X-rays may be useful to assess for signs of soft tissue air, which may increase suspicion for laryngotracheal injury14 and potentially change the approach to initial airway management (in patients who are otherwise stable).
Orotracheal Intubation
As in all trauma patients, orotracheal intubation with RSI and direct laryngoscopy (DL) is the method of choice for patients who require emergent intubation in PNT, as DL is the method most familiar to emergency medicine providers and has a very low failure rate.45 Indications for emergent airway management with RSI include inability to protect the airway because of altered mental status, airway compromise and aspiration risk because of blood and/or secretions in the airway, expanding neck hematoma, and inability to oxygenate or ventilate adequately. Patients with laryngotracheal injury also will require intubation, but the clinical situation will dictate how emergently and by which method this is performed. In patients with laryngotracheal injury, the optimal method for securing the airway may be awake fiberoptic intubation, with a second provider at the neck prepared to perform cricothyroidotomy or tracheostomy if fiberoptic intubation fails.15
In a retrospective analysis of a population of 748 patients presenting to an urban academic ED with PNT, 44 patients had initial airway management attempted with orotracheal intubation by emergency physicians with a 100% success rate.44 In this study, two patients had initial airway management with emergent tracheostomy, and 12 patients had initial attempts at intubation by fiberoptic laryngoscopy by otolaryngology resident physicians, in whom three were unsuccessful. All three of these patients who failed fiberoptic intubation then were intubated successfully orotracheally with rescue RSI by the emergency physician.44
The potential complications of orotracheal intubation include worsening of laryngotracheal injury, disruption of a neck hematoma with resultant hemorrhage, and failed intubation with requirement of an emergent surgical airway. Limitations of this technique include the inability to diagnostically assess the distal parts of the airway internally.
Gum Elastic Bougie
The gum elastic bougie is a useful adjunct to airway management in the trauma patient,45 particularly in cases where a limited view of the glottis can be obtained, or when there is difficulty in passing the endotracheal tube through the cords.46 The shape of the bougie tip facilitates its placement through the vocal cords. The laryngoscope should be left in place once the bougie is visualized to pass through the cords, and the endotracheal tube optimally should be rotated 90 degrees posteriorly when passed over the bougie, as this may assist with passing the tube through laryngeal soft tissues and into the trachea.47
Video Laryngoscopy
Video laryngoscopy (VL) is relatively new to the armamentarium of many emergency physicians. These devices allow for indirect view of the cords by placing a video camera on the end of the laryngoscope blade. EAST’s guidelines on emergency tracheal intubation immediately following traumatic injury, as well as the Difficult Airway Society Guidelines, both offer VL as a potentially viable option in patients with difficult airways. VL with devices such as the GlideScope offer improved visualization of the glottis and may decrease the number of failed intubations in patients with a difficult airway.48 A recent prospective analysis of 709 trauma patients intubated at a Level I trauma center demonstrated a significantly higher rate of success with VL over DL, which was particularly apparent in patients who were being maintained in cervical spine immobilization.49 However, a recent randomized, controlled trial of VL vs. DL in a general trauma patient population failed to demonstrate a benefit to VL and actually found that VL had a longer intubation time than DL, although almost 30% of patients in this study were not enrolled because of attending anesthesiologist preference. A potential difficulty with the use of VL in PNT is that blood can obscure the laryngoscope lens, severely affecting visualization. Further study of VL in the trauma population, including those with PNT, is needed.
Fiberoptic Intubation
Fiberoptic endotracheal intubation is a viable option for securing the airway in patients with PNT and has the advantage of allowing for diagnostic assessment of the distal airway prior to endotracheal tube placement. As in VL, the lens can be obscured easily by blood and may require active suction and use of saline flushes to maintain visualization. It is time-consuming to set up and perform fiberoptic intubation, and many EDs will not have rapid access to flexible fiberoptic laryngoscopes or bronchoscopes. It is not recommended for patients who require emergent airway control.
Fiberoptic intubation can be an excellent option for awake intubation in patients who are cooperative and have suspicion for airway injury. Desjardins et al described their technique for awake fiberoptic intubation in PNT.15 They recommend topical anesthesia of the oral cavity and tongue with viscous lidocaine or lidocaine spray prior to the procedure. This is followed by local anesthesia with aerosolized 4% lidocaine via the bronchoscope port (with a mix of 2 mL 4% lidocaine and 8 mL air), which is injected under direct visualization as the bronchoscope is advanced slowly. They advocate for injection of aerosolized anesthetic at the base of the tongue, before the epiglottis, after the epiglottis, at the larynx, and inside the trachea. The advantage of this technique is that it allows the patient to maintain the intrinsic respiratory drive and airway reflexes until intubation and sedation are achieved and also allows for direct assessment for airway injury. After the airway is inspected, the endotracheal tube is passed over the fiberoptic scope under direct visualization. If an airway injury is present, the endotracheal tube is inserted and cuff inflated distal to the point of injury.15 Depending on training and experience, the emergency medicine provider may defer this procedure to an anesthesiologist, if available.
Awake Intubation
Awake intubation is an optimal choice for securing the airway in patients who have an anticipated difficult airway but do not require emergent intubation. These patients are following commands and currently protecting their airway, but require semi-urgent airway control because of anticipated clinical course and/or concern for gradual loss of airway patency. George Kovacs provides an excellent description of his technique of urgent awake intubation in the ED, including his experience in a case of PNT with associated tracheal injury.50 The mouth is suctioned and then dried with gauze pads, as this may facilitate effective topicalized anesthesia. Then, the entire oropharynx is generously anesthetized with 8-10 mL of atomized 4% lidocaine. This is followed by grasping the tongue with a gauze pad and applying approximately 1.5 cm of 5% lidocaine ointment to the posterior tongue with a tongue depressor to anesthetize areas of the posterior oropharynx. Then, three separate sprays of 4% atomized lidocaine are administered sequentially intranasally, timed with inhalation. If the patient is uncooperative, sequential 0.3 mg/kg doses of ketamine can be used to provide dissociative analgesia and sedation to facilitate the procedure.
DL, VL, fiberoptic, and flexible video laryngoscope intubation techniques can be used successfully in awake patients. If DL or VL is used, Kovacs recommends the patient be seated at 45 degrees with the bed as low as possible. The intubating provider stands behind and to the left of the patient. After appropriate anesthesia and sedation, the laryngoscope blade is inserted gently with the operator’s left hand, while his or her right hand is used to guide the blade into the mouth without applying pressure to the tongue. Once the epiglottis is visualized, gentle pressure is applied to the vallecula to obtain a view of the larynx. At this point, the endotracheal tube can be gently passed directly into the trachea while the patient is awake, or a bougie can be placed through the cords while the patient is awake, followed by RSI and intubation over the bougie under direct laryngoscopic visualization.
Adequate analgosedation must be provided immediately once the endotracheal tube is in place. Further, the operator must be prepared to convert immediately to traditional RSI and orotracheal intubation should awake intubation fail.
Nasotracheal Intubation
Blind nasotracheal intubation (NTI) should be avoided in PNT because of the risk of dislodging a hematoma and causing complete airway obstruction, blindly entering a false passage in the neck, or worsening a laryngotracheal injury such as a tracheal disruption.15 There are limited data on NTI in PNT. Failure rates of 10-25% have been reported, although sample sizes were small.51,52 Other airway management techniques available in the ED should be used preferentially in PNT.
Surgical Airway Control
In patients with an anticipated difficult airway, some have advocated for a dual setup for orotracheal intubation and surgical airway prior to RSI.53 We would advocate this in all patients with penetrating neck trauma when resources and clinical situations allow. If multiple providers are available, a member of the airway team can be ready to convert immediately to a surgical airway if endotracheal intubation is unsuccessful.
Point-of-care ultrasound can be a valuable adjunct to assess and map tracheal anatomy.54 This can be useful prior to attempts at endotracheal intubation to define tracheal anatomy and the location of the cricothyroid membrane in preparation for conversion to a surgical airway.46 During ultrasonographic assessment, a surgical marker can be used to mark the anatomy externally, which can be helpful should a surgical airway be required.55 Lidocaine 1% with epinephrine can be infiltrated generously above the cricothyroid membrane under direct ultrasound guidance pre-emptively during this exam, as this may reduce bleeding and improve surgical visualization during cricothyroidotomy if endotracheal intubation is not successful.
To visualize the trachea with point-of-care ultrasound, place the high-frequency linear probe on the anterior neck at the suprasternal notch in the transverse plane. Moving the probe cephalad and caudad, the tracheal course can be mapped and marked. With the probe centered over the trachea, rotate the probe cephalad into the longitudinal plane, and scan in that plane to locate and mark the location of the cricothyroid membrane.56,57
The R Adams Cowley Shock Trauma Center published its experience with its emergency airway algorithm in 2009.58 This algorithm allowed three attempts at orotracheal intubation via laryngoscopy and the use of adjuncts like the gum elastic bougie. If these attempts failed, the providers proceeded to LMA placement. If the LMA placement was successful, the attending anesthesiologist’s discretion was used to determine the next course of action, whether to intubate through the LMA, pursue further attempts at laryngoscopy, or proceed with placement of a surgical airway under more controlled conditions. If the LMA was unsuccessful, a surgical airway was performed immediately. In a series of 6,088 emergent intubations in a general population of trauma patients presenting to the center, only 21 (0.3%) required a surgical airway. Of the patients who received a surgical airway, 27/31 (87%) patients survived to hospital discharge, with none of the deaths being attributed to failed airway management.
We would urge providers to consider and prepare for surgical airway early in PNT. While the surgical airway is generally a rescue therapy, early preparation for this procedure may increase its likelihood of success. The aggressive use of surgical airway management is preferred to failed airway management, hypoxia, hypercarbia, and death.
Cricothyroidotomy
Cricothyroidotomy is a rescue method for surgical airway control in PNT, but it also can be performed semi-electively as described above if its need is anticipated early and resources are available. It can be challenging technically, particularly if neck anatomy is distorted because of trauma, and tracheostomy is preferred if there is airway trauma below the level of the cricothyroid membrane. If the patient cannot be oxygenated and/or ventilated using the above methods, an emergent surgical airway should be performed without delay. The patient should receive complete neuromuscular blockade prior to performance of a surgical airway if possible. A supraglottic airway can be inserted in an attempt to maximize oxygenation/ventilation during the procedure, although this may not be helpful depending on the cause of the inability to intubate orotracheally and ventilate the patient.
There are many variations on how to perform a cricothyroidotomy, and one is not necessarily superior to another. Some have advocated for a scalpel-bougie-tube method. The neck is extended and the cricothyroid membrane palpated and stabilized with the non-dominant hand. A #10 blade is used to make a horizontal stab incision into the cricothyroid membrane. The scalpel is rotated vertically, and a bougie is inserted into the trachea adjacent the blade, and the scalpel is removed. A 6.0 mm cuffed endotracheal tube is passed over the bougie, the cuff is inflated and tube secured, and placement is verified by end-tidal capnography.46
A scalpel-finger-tube method also has been described, which allows the operator to palpate the inside of the trachea, potentially reduce the risk of creating a false passage, and ensure that the incision is large enough to accommodate an endotracheal tube. This method was described by Paix and Griggs in a case series of 24 patients, with a reported 100% success rate.59 In this method, the cricothyroid membrane is incised and extended laterally, the scalpel is removed, a finger is inserted into the incision to confirm proper positioning and that the incision is large enough to accommodate the tube, the finger is removed, and an endotracheal tube simply is inserted into the trachea.
Tracheostomy
Tracheostomy is an alternative method for surgical airway control and is preferred in cases of airway injury below the level of the larynx. This method generally is performed by surgical colleagues, and should be performed at least one tracheal ring below the level of tracheal injury.15
Direct Tracheal Intubation Via an Open Neck Wound
Direct tracheal intubation through the open anterior neck may be possible in patients with open tracheal injury in PNT. In cases of tracheal transection, the distal tracheal segment is located by following the air leak.13 The trachea is grasped with hemostats, tracheal hook, or towel clips, and the endotracheal tube is placed directly into the trachea. A gum elastic bougie also may be used if there is difficulty in passing the endotracheal tube.60 The bougie also can be used to facilitate intubation through tracheal lacerations or punctures.61
The method of securing the airway will depend on the skills of the operator, the condition of the patient, and the resources available.
Breathing
The evaluation and management of breathing in PNT is similar to that for any other major trauma patient. The lungs are auscultated, and sources of respiratory failure are investigated and simultaneously addressed. Point-of-care thoracic ultrasound can be used to evaluate for pneumothorax. A portable chest X-ray is obtained because, as mentioned previously, the apices of the lungs are in Zone I of the neck, and hemothorax and pneumothorax can be important causes of respiratory failure in PNT.13 Rigid, large-bore chest tubes are placed as indicated, as in any trauma patient.
Circulation
The primary goal in the initial circulatory resuscitation of patients with PNT is hemorrhage control. As sites of hemorrhage are identified, they are simultaneously managed. Vigorous direct pressure is placed immediately on sites of active external bleeding.1 As in any trauma patient, two large-bore intravenous or intraosseous catheters are placed, and balanced resuscitation with blood products or whole blood should be undertaken. If bleeding is unable to be controlled with direct pressure, balloon tamponade with a Foley catheter may be attempted. An 18 French Foley catheter is advanced through the wound tract and periodically inflated until the appropriate location for tamponade of bleeding is found. The catheter then is sutured to the skin with the balloon inflated.13 This method of hemorrhage control has been reported successful in 50-94% of patients.62-64
Given that the superior mediastinum also is at risk in PNT, point-of-care ultrasound may be of value in assessing for pericardial effusion and/or tamponade in the resuscitation bay. Chest X-ray can help define the vector and course of a penetrating missile and define sites of intrathoracic hematoma formation. If hemodynamically stable, patients with hematoma seen on chest X-ray should undergo CT of the chest to screen for intrathoracic aerodigestive injury, as well as CT angiography to evaluate for intrathoracic vascular trauma.13
Any patient with hard signs of major vascular or aerodigestive injury or hemodynamic instability should be transferred promptly to the operating room for surgical hemorrhage control. This should be delayed only by attempts to secure an unstable airway.1
Diagnostic Strategies
As mentioned previously, patients with PNT who have hard signs of major vascular or aerodigestive injury or hemodynamic instability proceed immediately to the operating room or are transferred to a tertiary care center after the airway is stabilized. While the management of unstable patients generally has not changed, the approach to the evaluation and management of patients who have wounds that violate the platysma and are hemodynamically stable has evolved in recent years. In the past, any patient with a Zone II wound that violated the platysma underwent mandatory operative neck exploration, but approximately 45% of these explorations were negative or “non-therapeutic.”13 This approach is no longer practiced widely.14 Historically, patients with Zone I injuries would have a diagnostic evaluation prior to surgery, as the surgical approach may be cervical or thoracic depending on underlying injuries. Because of difficulties in surgical exploration, Zone III injuries also would undergo a diagnostic evaluation prior to surgery.
Currently, leading authorities in the United States and abroad advocate the practice of selective operative management to reduce unnecessary operations for PNT, in which patients with soft signs of injury undergo further evaluation with imaging (CT angiography of the neck ± other studies) and asymptomatic patients are observed.1,4,14 Selective operative management in penetrating neck trauma is supported by a significant body of literature. This approach has been demonstrated to decrease unnecessary operative neck exploration by approximately 50-60% without an increase in mortality or complication rates.11,65-67 The overall sensitivity and specificity of multi-detector CTA for detection of clinically significant vascular or aerodigestive injury in the neck in PNT has been described as high as 100% and 97.5%, respectively, on prospective evaluation.8
In hemodynamically stable patients with PNT who have soft signs or symptoms of potential vascular or aerodigestive injury, the current standard of care is to obtain a CTA of the neck as the initial diagnostic study. The WTA algorithm for the management of penetrating neck trauma currently recommends CTA of the neck in patients with any clinical suspicion of injury, regardless of the anatomic zone of the external wound. In patients without signs of serious injury, but who have platysma violation, Sperry et al recommend observation with serial exams.1 These exams can occur every 6-8 hours for 24-36 hours until the patient is discharged.13
Patients with aerodigestive injuries detected on CTA generally require operative intervention, particularly because delayed treatment of esophageal injury can lead to increased mortality and morbidity, as described previously. In patients in whom there is still a suspicion for aerodigestive injury due to symptoms or wound trajectory despite negative CTA, water-soluble esophagography or fiberoptic esophagoscopy should be performed. When clinical suspicion is present, assessment for airway injury should be undertaken with fiberoptic laryngoscopy and/or bronchoscopy.
Arterial injuries from PNT detected on CTA, particularly those in Zones I and III, potentially can be managed endovascularly, although there is institutional variation in this practice.1,13 Venous injuries often can be managed safely nonoperatively.1
While the WTA algorithm still divides its approach by anatomic neck “zones,” it is thought by some to be obsolete, in part because of the presence of increasingly advanced imaging technologies. A “no zone” approach for penetrating neck trauma increasingly is being practiced. Selective nonoperative management (with observation and serial exams for asymptomatic patients, and imaging reserved for those with soft signs or symptoms of serious injury) has been shown to be safe and effective in PNT. However, some propose using CTA of the neck in all patients with platysma violation to expedite triage and reduce the labor and resource utilization required by serial exams in the modern trauma center.68
Other imaging technologies, including duplex and color Doppler flow ultrasound and magnetic resonance angiography (MRA), have been proposed for the evaluation of PNT. While ultrasound is operator-dependent and potentially time-consuming, it can be highly accurate in diagnosing vascular injuries in the neck.13,69 Duplex and Doppler ultrasound clearly cannot provide as thorough an evaluation of the neck in patients with PNT as that provided by CTA. However, ultrasound may have utility in certain clinical situations, such as in patients with soft signs of vascular injury who cannot receive IV contrast because of institutional protocols for patients with prior contrast reactions and/or elevated serum creatinine. MRA is very sensitive, but likely impractical in the evaluation of most cases of PNT because of its incompatibility with various medical equipment and concern about metallic fragments retained in the neck after PNT.68
In summary, hemodynamically unstable patients and/or those patients with hard signs of vascular and/or aerodigestive injury with PNT should be transferred urgently to the operating room after attempts at rapid hemorrhage control and airway management in the ED, when clinically indicated. Those patients with soft signs of injury should undergo CTA of the neck. If the CTA is negative, and suspicion still is present for aerodigestive injury, particularly for esophageal injury, further studies should be obtained. The management of asymptomatic patients with platysma violation in PNT is somewhat controversial in the United States. A viable and evidence-based option is to observe these patients with serial exams for 24-36 hours and proceed with further imaging if indicated, but others advocate for CTA of the neck in all patients to expedite triage and optimize resource utilization. In all cases, patients with platysma violation should undergo evaluation by a trauma surgeon in a center with the resources to care for these potentially complex injuries.
Disposition
All patients with penetrating neck trauma ideally should be admitted to a tertiary trauma center. Mortality benefits have been associated with transfer of major trauma patients from non-tertiary centers to Level I and Level II trauma centers.70 Given the potential complexity of penetrating neck injuries, and the significant morbidity and mortality associated with these injuries, patients with PNT should be cared for by trauma surgeons in a center with all the resources available to provide optimal care. Non-tertiary trauma receiving facilities should have transfer guidelines in place to facilitate transfer to a trauma center. Emergency physicians should be familiar with their facility’s resources and should transfer patients, following stabilization, as appropriate. Prior to transfer, the transferring physician must use his or her judgement in terms of whether the patient’s airway should be controlled in the ED.
Summary
Penetrating neck trauma presents a clinical challenge to the emergency physician in both evaluation and management. Patients can present in extremis requiring emergent airway and hemorrhage control, but others can have subtle signs of injury that require careful investigation. Optimal care of PNT requires knowledge of the complex anatomy at risk, expertise at control of the difficult airway, and a thorough and structured approach to the management of the complex injuries that can occur. Collaboration with trauma surgical colleagues at tertiary trauma centers is essential in providing the best outcomes for these patients.
REFERENCES
- Sperry JL, Moore EE, Coimbra R, et al. Western Trauma Association critical decisions in trauma: Penetrating neck trauma. J Trauma Acute Care Surg 2013;75:936-940.
- Monson DO, Saletta JD, Freeark RJ. Carotid vertebral trauma. J Trauma 1969;9:987-999.
- Roon AJ, Christensen N. Evaluation and treatment of penetrating cervical injuries. J Trauma 1979;19:391-397.
- Tisherman SA, Bokhari F, Collier B, et al. Clinical practice guideline: Penetrating zone II neck trauma. J Trauma 2008;64:1392-1405.
- Rodríguez-Luna MR, Guarneros-Zárate JE, Hernández-Méndez JR, et al. Defining Zone I of penetrating neck trauma: A surgical controversy in the light of clinical anatomy. J Trauma Acute Care Surg 2016;80:670-673.
- Low GM, Inaba K, Chouliaras K, et al. The use of the anatomic “zones” of the neck in the assessment of penetrating neck injury. Am Surg 2014;80:970-974.
- Fackler ML. Gunshot wound review. Ann Emerg Med 1996;28:194-203.
- Inaba K, Branco BC, Menaker J, et al. Evaluation of multidetector computed tomography for penetrating neck injury: A prospective multicenter study. J Trauma Acute Care Surg 2012;72:576-583.
- Biffl WL, Moore EE, Rehse DH, et al. Selective management of penetrating neck trauma based on cervical level of injury. Am J Surg 1997;174:678-682.
- Demetriades D, Theodorou D, Cornwell E, et al. Evaluation of penetrating injuries of the neck: Prospective study of 223 patients. World J Surg 1997;21:41-47.
- Osborn TM, Bell RB, Qaisi W, Long WB. Computed tomographic angiography as an aid to clinical decision making in the selective management of penetrating injuries to the neck: A reduction in the need for operative exploration. J Trauma 2008;64:1466-1471.
- Schroll R, Fontenot T, Lipcsey M, et al. Role of computed tomography angiography in the management of Zone II penetrating neck trauma in patients with clinical hard signs. J Trauma Acute Care Surg 2015;79:943-950; discussion 950.
- Feliciano DV. Penetrating cervical trauma: “Current concepts in penetrating trauma,” IATSIC Symposium, International Surgical Society, Helsinki, Finland, August 25-29, 2013. World J Surg 2015;39:1363-1372.
- Burgess CA, Dale OT, Almeyda R, Corbridge RJ. An evidence based review of the assessment and management of penetrating neck trauma. Clin Otolaryngol 2012;37:44-52.
- Desjardins G, Varon AJ. Airway management for penetrating neck injuries: The Miami experience. Resuscitation 2001;48:71-75.
- Lyons JD, Feliciano DV, Wyrzykowski AD, Rozycki GS. Modern management of penetrating tracheal injuries. Am Surg 2013;79:188-193.
- Asensio JA, Chahwan S, Forno W, et al. Penetrating esophageal injuries: Multicenter study of the American Association for the Surgery of Trauma. J Trauma 2001;50:289-296.
- Patel MS, Malinoski DJ, Zhou L, et al. Penetrating oesophageal injury: A contemporary analysis of the National Trauma Data Bank. Injury 2013;44:48-55.
- Fonseca AZ, Ribeiro MA Jr, Frazão M, et al. Esophagectomy for a traumatic esophageal perforation with delayed diagnosis. World J Gastrointest Surg 2009;1:65-67.
- Vanderlan WB, Tew BE, Seguin CY, et al. Neurologic sequelae of penetrating cervical trauma. Spine (Phila Pa 1976). 2009;34:2646-2653.
- Lustenberger T, Talving P, Lam L, et al. Unstable cervical spine fracture after penetrating neck injury: A rare entity in an analysis of 1,069 patients. J Trauma 2011;70:870-872.
- Klein Y, Cohn SM, Soffer D, et al. Spine injuries are common among asymptomatic patients after gunshot wounds. J Trauma 2005;58:833-836.
- Ernest E, Burnett A, Frascone RJ. High index of suspicion. Recognizing & managing traumatic neck injuries. JEMS 2014;39:50-54.
- Barnard EB, Ervin AT, Mabry RL, Bebarta VS. Prehospital and en route cricothyrotomy performed in the combat setting: A prospective, multicenter, observational study. J Spec Oper Med 2014;14:35-39.
- Weichenthal L, Crane D, Rond L. Needle thoracostomy in the prehospital setting: A retrospective observational study. Prehosp Emerg Care 2016;20:399-403.
- Warner KJ, Copass MK, Bulger EM. Paramedic use of needle thoracostomy in the prehospital environment. Prehosp Emerg Care 2008;12:162-168.
- Davis DP, Pettit K, Rom CD, et al. The safety and efficacy of prehospital needle and tube thoracostomy by aeromedical personnel. Prehosp Emerg Care 2005;9:191-197.
- Aho JM, Thiels CA, El Khatib MM, et al. Needle thoracostomy: Clinical effectiveness is improved using a longer angiocatheter. J Trauma Acute Care Surg 2016;80:272-277.
- Inaba K, Branco BC, Eckstein M, et al. Optimal positioning for emergent needle thoracostomy: A cadaver-based study.
J Trauma 2011;71:1099-1103; discussion 1103. - Engels PT, Passos E, Beckett AN, et al. IV access in bleeding trauma patients: A performance review. Injury 2014;45:77-82.
- Brown JB, Rosengart MR, Forsythe RM, et al. Not all prehospital time is equal: Influence of scene time on mortality.
J Trauma Acute Care Surg 2016;81:93-100. - McCoy CE, Menchine M, Sampson S, et al. Emergency medical services out-of-hospital scene and transport times and their association with mortality in trauma patients presenting to an urban Level I trauma center. Ann Emerg Med 2013;61:167-174.
- Rappold JF, Hollenbach KA, Santora TA, et al. The evil of good is better: Making the case for basic life support transport for penetrating trauma victims in an urban environment. J Trauma Acute Care Surg 2015;79:343-348.
- Seamon MJ, Doane SM, Gaughan JP, et al. Prehospital interventions for penetrating trauma victims: A prospective comparison between Advanced Life Support and Basic Life Support. Injury 2013;44:634-638.
- Band RA, Salhi RA, Holena DN, et al. Severity-adjusted mortality in trauma patients transported by police. Ann Emerg Med 2014;63:608-614.e3.
- Wandling MW, Nathens AB, Shapiro MB, Haut ER. Police transport versus ground EMS: A trauma system-level evaluation of prehospital care policies and their effect on clinical outcomes. J Trauma Acute Care Surg 2016;81:931-935. .
- Vanderlan WB, Tew BE, McSwain NE Jr. Increased risk of death with cervical spine immobilisation in penetrating cervical trauma. Injury 2009;40:880-883.
- McSwain NE and Pons PT, eds. PHTLS: Prehospital Trauma Life Support. Burlington, MA: Jones & Bartlett Learning, 2016.
- Haut ER, Kalish BT, Efron DT, et al. Spine immobilization in penetrating trauma: More harm than good? J Trauma 2010;68:115-120.
- Brown JB, Bankey PE, Sangosanya AT, et al. Prehospital spinal immobilization does not appear to be beneficial and may complicate care following gunshot injury to the torso. J Trauma 2009;67:774-778.
- Stuke LE, Pons PT, Guy JS, et al. Prehospital spine immobilization for penetrating trauma — review and recommendations from the Prehospital Trauma Life Support Executive Committee. J Trauma 2011;71:763-769.
- Garcia A, Liu TH, Victorino GP. Cost-utility analysis of prehospital spine immobilization recommendations for penetrating trauma. J Trauma Acute Care Surg 2014;76:534-541.
- ATLS Subcommittee; American College of Surgeons’ Committee on Trauma; International ATLS working group. Advanced trauma life support (ATLS®): The ninth edition. J Trauma Acute Care Surg 2013;74:1363-1366.
- Mandavia DP, Qualls S, Rokos I. Emergency airway management in penetrating neck injury. Ann Emerg Med 2000;35:221-225.
- Mayglothling J, Duane TM, Gibbs M, et al. Emergency tracheal intubation immediately following traumatic injury: An Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg 2012;73(5 Suppl 4):S333-S340.
- Frerk C, Mitchell VS, McNarry AF, et al. Difficult Airway Society 2015 guidelines for management of unanticipated difficult intubation in adults. Br J Anaesth 2015;115:827-848.
- Dogra S, Falconer R, Latto IP. Successful difficult intubation. Tracheal tube placement over a gum-elastic bougie. Anaesthesia 1990;45:774-776.
- Lewis SR, Butler AR, Parker J, et al. Videolaryngoscopy versus direct laryngoscopy for adult patients requiring tracheal intubation. Cochrane Database Syst Rev 2016;11:CD011136.
- Michailidou M, O’Keeffe T, Mosier JM, et al. A comparison of video laryngoscopy to direct laryngoscopy for the emergency intubation of trauma patients. World J Surg 2015;39:782-788.
- Kovacs G, Weingart S. Podcast 194: Definitive emergent awake intubation with George Kovacs. EMCrit Blog, March 6, 2017. Available at: https://emcrit.org/podcasts/definitive-emergent-awake-intubation/. Accessed March 18, 2017.
- Weitzel N, Kendall J, Pons P. Blind nasotracheal intubation for patients with penetrating neck trauma. J Trauma 2004;56:1097-1101.
- Shearer VE, Giesecke AH. Airway management for patients with penetrating neck trauma: A retrospective study. Anesth Analg 1993;77:1135-1138.
- Leeuwenburg T. Airway management of the critically ill patient: Modifications of traditional rapid sequence induction and intubation. Crit Care Horizons 2015;1:1-10.
- Osman A, Sum KM. Role of upper airway ultrasound in airway management. J Intensive Care 2016;4:52.
- Mallin M, Curtis K, Dawson M, et al. Accuracy of ultrasound-guided marking of the cricothyroid membrane before simulated failed intubation. Am J Emerg Med 2014;32:61-63.
- Siddiqui N, Arzola C, Friedman Z, et al. Ultrasound improves cricothyrotomy success in cadavers with poorly defined neck anatomy: A randomized control trial. Anesthesiology 2015;123:1033-1041.
- Curtis K, Ahern M, Dawson M, Mallin M. Ultrasound-guided, Bougie-assisted cricothyroidotomy: A description of a novel technique in cadaveric models. Acad Emerg Med 2012;19:876-879.
- Stephens CT, Kahntroff S, Dutton RP. The success of emergency endotracheal intubation in trauma patients: A 10-year experience at a major adult trauma referral center. Anesth Analg 2009;109:866-872.
- Paix BR, Griggs WM. Emergency surgical cricothyroidotomy: 24 successful cases leading to a simple “scalpel-finger-tube” method. Emerg Med Australas 2012;24:23-30.
- Steinfeldt J, Bey TA, Rich JM. Use of a gum elastic bougie (GEB) in a zone II penetrating neck trauma: A case report.
J Emerg Med 2003;24:267-270. - Bhattacharya P, Mandal MC, Das S, et al. Airway management of two patients with penetrating neck trauma. Indian J Anaesth 2009;53:348-351.
- Navsaria P, Thoma M, Nicol A. Foley catheter balloon tamponade for life-threatening hemorrhage in penetrating neck trauma. World J Surg 2006;30:1265-1268.
- Ball CG, Wyrzykowski AD, Nicholas JM, et al. A decade’s experience with balloon catheter tamponade for the emergency control of hemorrhage. J Trauma 2011;70:330-333.
- Gilroy D, Lakhoo M, Charalambides D, Demetriades D. Control of life-threatening haemorrhage from the neck: A new indication for balloon tamponade. Injury 1992;23:557-559.
- Teixeira F, Menegozzo CA, Netto SD, et al. Safety in selective surgical exploration in penetrating neck trauma. World J Emerg Surg 2016;11:32.
- Prichayudh S, Choadrachata-anun J, Sriussadaporn S, et al. Selective management of penetrating neck injuries using “no zone” approach. Injury 2015;46:1720-1725.
- Madsen AS, Laing GL, Bruce JL, et al. An audit of penetrating neck injuries in a South African trauma service. Injury 2016;47:64-69.
- Shiroff AM, Gale SC, Martin ND, et al. Penetrating neck trauma: A review of management strategies and discussion of the “no zone” approach. Am Surg 2013;79:23-29.
- Montorfano MA, Pla F, Vera L, et al. Point-of-care ultrasound and Doppler ultrasound evaluation of vascular injuries in penetrating and blunt trauma. Crit Ultrasound J 2017;9:5.
- Garwe T, Cowan LD, Neas B, et al. Survival benefit of transfer to tertiary trauma centers for major trauma patients initially presenting to nontertiary trauma centers. Acad Emerg Med 2010;17:1223-1232.
Penetrating neck trauma presents a clinical challenge to the emergency physician. Clinicians must have a planned approach to these patients to optimize outcomes.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
