Atrial Flutter or Atrial Tachycardia?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer is the sole proprietor of KG-EKG Press, and publisher of an ECG pocket brain book.
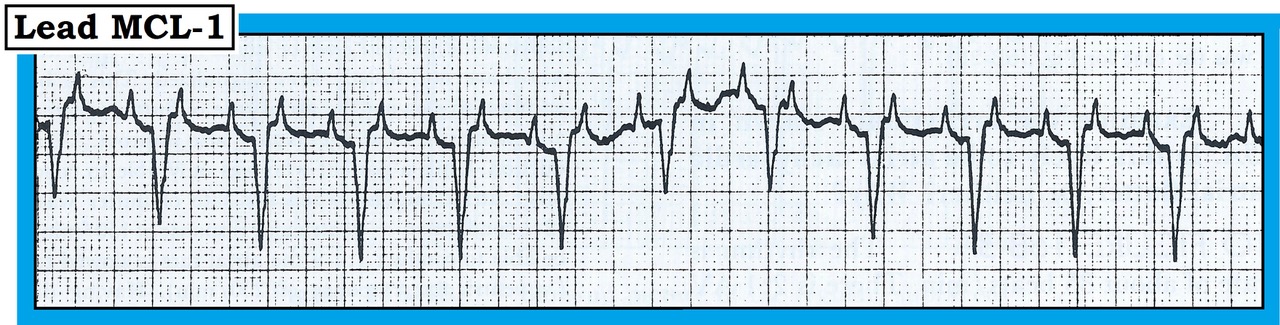
How would you interpret the rhythm in the figure below? What is your differential diagnosis? Can you be sure of your answer from looking at this lead MCL-1 rhythm strip? Why is it important to know if the patient is on digoxin?
The rhythm in the figure is regular, with a ventricular rate of ~115/minute. P waves outnumber QRS complexes by two to one, making the atrial rate ~230/minute. The QRS complex is narrow, implying a supraventricular mechanism, and each QRS complex is preceded by a P wave with a constant PR interval. Thus, P waves are related to the QRS complexes, albeit only one of every two P waves conducts to the ventricles. Therefore, this is a supraventricular tachycardia (SVT) rhythm with 2:1 AV conduction. The differential diagnosis is between atrial flutter and atrial tachycardia.
In favor of atrial flutter: Regular and rapid atrial activity with a peaked upward deflection in this right-sided MCL-1 monitoring lead. That said, the atrial rate of 230/minute is a bit below the usual atrial rate range for untreated atrial flutter (of 250-350/minute), and the expected “sawtooth” pattern of atrial flutter is missing in this lead.
In favor of atrial tachycardia: The atrial rate (below 250/minute) and the isoelectric baseline (rather than sawtooth) in this lead.
We do not know if this patient is taking an antiarrhythmic agent (such as flecainide, amiodarone, sotalol, etc.) that might slow the atrial rate of flutter. We do not know if this patient is taking digoxin. This is important because SVT with 2:1 conduction in a patient taking digoxin strongly suggests digitalis toxicity. Despite the greatly reduced use of this drug at the current time (atrial tachycardia with block because of digitalis toxicity is no longer seen commonly), it remains, nevertheless, important to inquire about this medication since it is still prescribed occasionally.
It is impossible to be certain of the rhythm diagnosis solely from the rhythm strip seen in the figure without the benefit of additional information (i.e., previous clinical history, knowing what medications the patient is taking). Seeing a full 12-lead ECG might help by revealing a typical sawtooth pattern in other leads. That said, the clinical reality is that neither rate nor baseline appearance (sawtooth vs. isoelectric baseline) have been shown to reliably distinguish between atrial tachycardia and atrial flutter. Fortunately, from a non-cardiologist’s perspective, both initial and long-term management of these two SVT rhythms is similar (once you have ruled out the possibility of digitalis toxicity). Initial efforts entail slowing the ventricular response, with consideration of electrophysiology referral if the arrhythmia is persistent or recurs.
For further discussion of this case, please visit: http://bit.ly/2tFJxnE.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
