Emergency Management of Rabies Exposure
September 1, 2017
Reprints
AUTHORS
Timothy J. Honeycutt, MD, PGY-3, Department of Pediatrics, University of Texas Health Sciences Center, San Antonio
Daniel J. Dire, MD, FACEP, FAAEM, FAAP, Clinical Professor, Departments of Emergency Medicine and Pediatrics, Director, Pediatric Emergency Medicine, University of Texas Health Sciences Center, San Antonio
PEER REVIEWER
James Wilde, MD, Professor of Emergency Medicine, Associate Professor of Pediatrics, Augusta University, Augusta, GA
EXECUTIVE SUMMARY
- Nonbite methods of infection include inhalation of droplets (bat caves), organ transplant, or contamination of an open wound, scratch, abrasion, or mucous membrane by infected saliva or neural tissue.
- Bat bites are more likely to go unrecognized. The Centers for Disease Control and Prevention recommends post-exposure prophylaxis (PEP) be considered for persons who were in the same room as a bat and who might be unaware that a bite or direct contact had occurred (e.g., a sleeping person awakens to find a bat in the room or an adult witnesses a bat in the room with a previously unattended child, mentally disabled person, or intoxicated person) and rabies cannot be ruled out by testing the bat.
- Of the 32 deaths associated with animal transmission, 22 were transmitted by bats in which exposure occurred in the United States, compared to nine deaths in which exposures all took place with rabid dog or mongoose bites received outside the continental United States.
- The incubation period varies in length from two weeks to six months or more (average one to two months); the incubation period is shorter for bites to the head and face and longer for bites to the upper or lower extremities.
- Immediate and thorough washing of all bite wounds and scratches with soap and water is perhaps the most effective measure for preventing rabies. Preferably, the bite wound should be irrigated thoroughly and copiously with a virucidal agent (e.g., 1% benzalkonium chloride or povidone-iodine solution), which has been shown experimentally to kill the rabies virus, followed by normal saline irrigation.
- The decision to begin PEP depends on the type of animal involved, whether it is available for postmortem testing (wild animals) or observation (dogs, cats, or ferrets), and the circumstances surrounding the bite. PEP consists of a combination of a passive immunoprophylactic agent and an active immunoprophylactic agent.
Rabies is an uncommon disease with a very high fatality rate. Recognition of a potential exposure and effective prophylaxis are critical in prevention of this devastating disease. The authors review recognition of suspicious bites/exposures, clinical presentation of rabies, and utilization of effective prevention strategies.
— Ann M. Dietrich, MD, FAAP, FACEP
Rabies is a viral disease that is carried by animals and can be spread to humans, usually through a bite. It is caused by an RNA virus in the genus Lyssavirus, and all mammals are susceptible to rabies.1 Over the last several decades, the predominant source of human rabies infections in the United States has shifted from terrestrial animals to insectivorous bats. Rabies has the highest case fatality rate of any infectious disease, and once clinical signs of rabies develop, there is no proven cure;2 only a few well-documented cases of human survival exist. Therefore, all efforts must be performed to prevent rabies following a potential exposure to the virus.
Worldwide, an average of 60,000 people die from rabies annually and more than 15 million people receive rabies post-exposure prophylaxis (PEP).3 In the United States, animal bite incidents are estimated to range from 1 million to 4.5 million a year, with approximately 334,000 emergency department (ED) visits from dog and cat bites alone.4 Each encounter requires an assessment of the need for PEP. The bites of dogs and cats are the main reason PEP is administered in the United States.5 The estimated annual spending on rabies (including diagnostic tests, PEP, and animal control) is $245-500 million in the United States alone.6 Although that is nowhere near the more than $100 billion spent yearly on obesity, it is no small number either, especially for a disease that has accounted for only 15 deaths in the United States since 2010. Therefore, its high cost per patient contrasted with the low frequency with which exposures are seen in the ED makes understanding rabies and who should receive PEP critical to any emergency physician.
A Brief History
Rabies is not a new disease; it has been known to man as far back as history is recorded.7 Rabies in wild animals has been recognized in the Middle East since biblical times, and many ancient Greek and Roman scholars wrote of rabies in dogs and other domestic animals.2 In the first century AD, the Roman encyclopedist Aulus Cornelius Celsus wrote about the disease saying, “especially if the dog was mad, the poison must be drawn out by a cup.” In 200 AD, the Greek physician Galen wrote even more specifically on the disease, concluding it to be a poison transmitted by a “Mad Dog … if contacting its saliva.” In the 1500s, rabies was present in Europe, as Spain was ravaged by wild dogs infected with the disease. In the 1700s, the first case was reported in North America,2 and in the 1880s, Louis Pasteur turned his work toward rabies.8 After some successful work with vaccines in chicken cholera and anthrax, Pasteur produced the first rabies vaccine by growing the virus in rabbits. In 1885, Pasteur successfully completed the world’s first PEP on a 9-year-old boy who had been mauled by a rabid dog. The boy received 13 injections over the course of two weeks and survived.9
The Virus
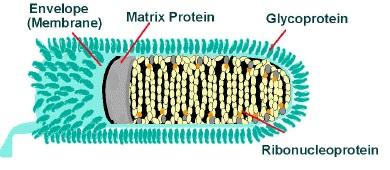
Rabies virus, from the family Rhabdovirus and the genus Lyssavirus, is actually a group of enveloped, bullet-shaped RNA viruses, which are atypical in shape compared to normal polyhedral-shaped human pathogens.2 (See Figure 1.) They are transmitted from an animal reservoir through their virus-containing, infected saliva into the bite victim’s exposed tissue. The virus begins replicating in the tissue until it is able to bind to nicotinic acetylcholine receptors at the neuromuscular junction.10 Here the virus takes advantage of the axons’ innate, retrograde fast axonal transport to travel (50-100 mm/d) to the dorsal root ganglion in the central nervous system. This retrograde transport is what produces the classic delay in symptoms seen in rabies and similar pathogens (herpes simplex virus, tetanus, and polio). Once the virus reaches the spinal cord, the virus is able to divide rapidly and spread to the brain, where it presents clinically with its classic symptoms.
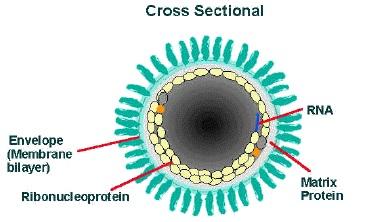
Figure 1. Rabies Virions |
|
A: Rabies virions are bullet-shaped with 10-nm spike-like glycoprotein peplomers covering the surface. The ribonucleoprotein is composed of RNA encased in nucleoprotein -(), phosphorylated or phosphoprotein. |
 |
|
B: The cross-sectional diagram demonstrates the concentric layers: envelope membrane bilayer, M protein, and tightly coiled encased genomic RNA. |
 |
|
SOURCE: Centers for Disease Control and Prevention. Rabies. The Rabies Virus. Available at: |
Exposure
The first and sometimes difficult task in treating rabies is identifying an exposure. Table 1 compares the difference in cost-effectiveness of rabies treatment among different exposure types.11 The large number of non-cost-effective exposures shows why it is important to define true exposure. A bite from a rabid animal is the most effective manner to transmit rabies. Nonbite methods include inhalation of droplets (bat caves), organ transplant, or contamination of an open wound, scratch, abrasion, or mucous membrane by infected saliva or neural tissue.2,11,12 Contact with a rabid animal, such as petting, or contact with blood, urine, or feces of a rabid animal does not constitute an exposure. Bat bites are more likely to go unrecognized. The Centers for Disease Control and Prevention (CDC) recommends PEP be considered for persons who were in the same room as a bat and who might be unaware that a bite or direct contact had occurred (e.g., a sleeping person awakens to find a bat in the room or an adult witnesses a bat in the room with a previously unattended child, mentally disabled person, or intoxicated person) and rabies cannot be ruled out by testing the bat.13
Table 1. Cost-effectiveness Ratio (Cost/Life Saved) for Rabies Post-exposure Prophylaxis, by Different Scenarios of Potential Exposure * — United States |
||
|
Contact Scenario |
Probability of Rabies† Median (Minimum – Maximum) |
Baseline Cost Scenario§ Average Cost Effectiveness (Most |
|
Animal tests positive for rabies |
(0.01-0.7) |
Cost saving |
|
Skunk bite¶ |
0.05 |
Cost saving |
|
Possible bat bite¶** |
0.001 |
$2.9 million |
|
Dog bite¶ |
0.00001 |
$403 million |
|
Dog lick¶ |
0.000001 |
$4 billion |
|
Cat bite¶ |
0.001 |
$2.9 million |
|
Cat lick¶ |
0.000001 |
$4 billion |
|
Contact with rabid human in clinical setting** |
0.000001 |
$4 billion |
|
* Contact with a potentially rabid animal does not necessarily constitute an exposure. A bite exposure is defined as “any penetration of the skin by teeth.” A nonbite exposure is defined as ”contamination of open wounds, abrasions (including scratches), or mucous membranes with saliva or other potentially infectious material (e.g., neural tissue).“ † Probabilities of rabies transmission to a human were obtained from a panel of experts, except for ”animal tests positive for rabies“ when probabilities obtained from a previous study. § Estimates of the direct medical costs of rabies post-exposure prophylaxis (PEP) were converted into 2004 dollars using the medical care price index. The cost-effectiveness of PEP under each contact scenario is calculated using the median probability of becoming clinically ill with rabies and the average cost of PEP. The most cost-effective ratio is calculated using the minimum cost of PEP and the maximum probability of becoming clinically ill with rabies. The least cost-effective ratio is calculated using the maximum cost of PEP and the minimum probability of becoming clinically ill with rabies. ¶ Animals not available for testing. The skunk bite data are considered applicable to bites from other rabies reservoir species (e.g., bats, raccoons, and foxes in the United States and dog bites occurring in countries with dog variant rabies). ** No recognized bite or saliva exposure. Source: Manning SE, Rupprecht CE, Fishbein D, et al. Human rabies prevention — United States, 2008: Recommendations of the Advisory Committee on Immunization Practices. MMWR Recomm Rep 2008;57(RR-3):1-28. |
||
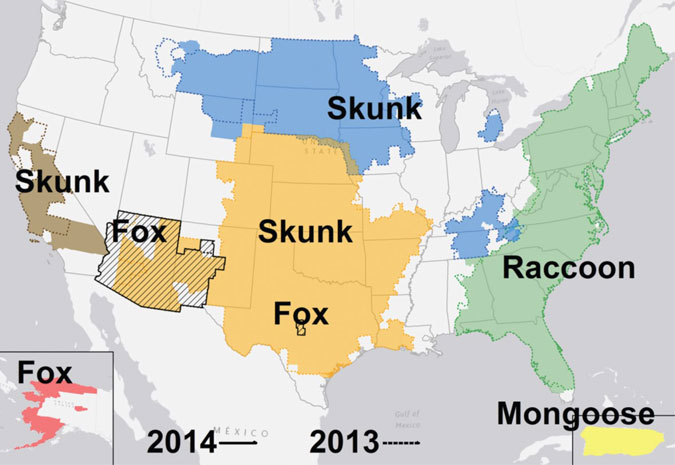
All mammals have the ability to act as reservoirs for the rabies virus; however, animal reservoir populations vary by continent, country, and even smaller sub-regions. (See Figure 2.) Worldwide, dogs account for 98% of human rabies deaths.1 India, which has a large stray dog population, accounts for more than 35% of the yearly worldwide deaths.14 Significant human mortality from rabies also still is seen in South America, Africa, and Southeast Asia.14,15 Canine-associated rabies is very rare in countries that have made large attempts to vaccinate domestic animals; the last isolation of the canine strain of rabies in the United States was in 2004. Non-domesticated animals in these countries are the most common rabies reservoir. The most common animals with the disease in the United States are bats, raccoons, skunks, and foxes. (See Figure 3.) In 2015, for the first time since the CDC began rabies surveillance, bats surpassed raccoons as the wild animal found infected most frequently.1 This is likely a result of the increased sampling of bats for rabies and regional wildlife oral vaccination programs. Between 2003 and 2016, there were only 38 human deaths in the United States caused by rabies; six of the deaths were the result of contracting rabies through organ transplants.1 (See Table 2.) Of the 32 deaths associated with animal transmission, 22 were transmitted by bats in which exposure occurred in the United States, compared to nine deaths in which exposures all took place with rabid dog or mongoose bites received outside the continental United States. Rabid dogs and cats in the United States usually are infected with the raccoon virus variant, and less commonly with skunk variants or, rarely, bat rabies variants.1
Figure 2. Distribution of Major Rabies Virus Variants Among Mesocarnivores in the United States and Puerto Rico for 2008 Through 2014 |
|
Black diagonal lines represent fox rabies variants (Arizona gray fox and Texas gray fox). Solid borders represent 5-year rabies virus variant aggregates for 2010 through 2015; dashed borders represent the previous 5-year aggregates for 2009 through 2014. |
|
Source: Centers for Disease Control and Prevention. Rabies. Available at: https://www.cdc.gov/rabies/resources/publications/2014-surveillance/2014-us-map.html. Accessed June 1, 2017. |
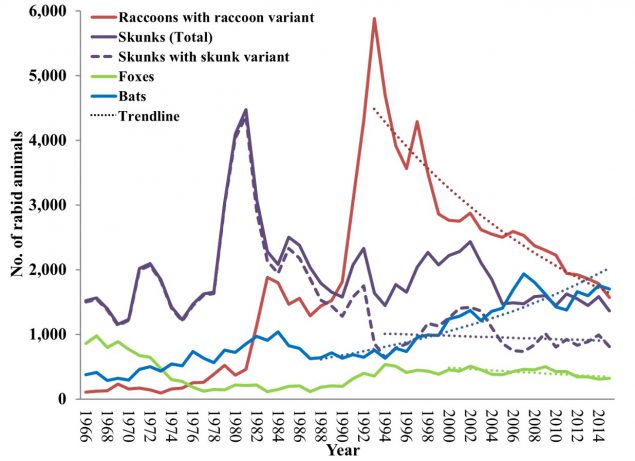
Figure 3. Cases of Rabies Among Wildlife in the United States, by Year and Species, for 1966 Through 2015 |
|
Since 1998, more than 50% of skunks were infected with a presumed raccoon rabies virus variant. |
|
SOURCE: Centers for Disease Control and Prevention. Rabies. Available at: https://www.cdc.gov/rabies/resources/publications/2015-surveillance/2015-wildlife.html. Accessed June 1, 2017. |
Bats are concerning not just for their high prevalence of rabies. When compared to other animals, transmission of rabies among bats to humans is also unique. Bats are small creatures, with more than 20 species testing positive for rabies virus in 2015 in the United States.1 Their bites alone, which measure less than 0.5 cm, are unlikely to send anyone to the ED. No rabid bats were reported in Alaska, Hawaii, or Puerto Rico in 2015.1
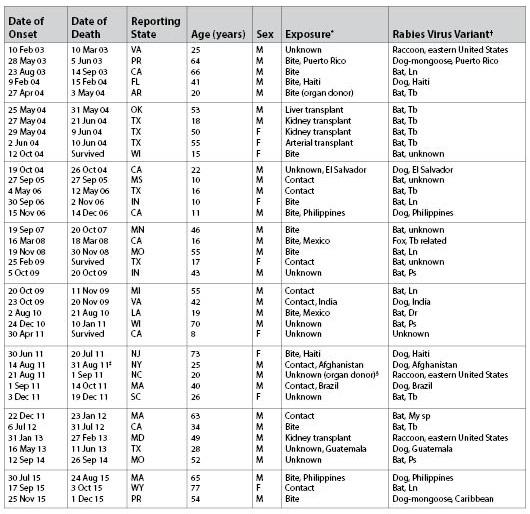
Table 2. Cases of Rabies in Humans in the United States and Puerto Rico, January 2003 Through September 2016, by Circumstances of Exposure and Rabies Virus Variant
|
||||||
|
* Data for exposure history are reported when plausible information was reported directly by the patient (if lucid or credible) or when a reliable account of an incident consistent with rabies virus exposure (e.g., dog bite) was reported by an independent witness (usually a family member). Exposure histories are categorized as bite, contact (e.g., waking to find bat on exposed skin) but no known bite was acknowledged, or unknown (i.e., no information about known contact with an animal was elicited during case investigation). † Rabies virus variants associated with terrestrial animals in the United States and Puerto Rico are identified with the names of the reservoir animal (e.g., dog or raccoon), followed by the name of the most definitive geographic entity (usually the country) from which the variant has been identified. Rabies virus variants associated with bats are identified with the names of the species of bats in which they have been found to be circulating. Because information regarding the location of the exposure and the identity of the exposing animal is almost always retrospective and much information is frequently unavailable, the location of the exposure and the identity of the animal responsible for the infection often are limited to deduction. ‡ The date of death was erroneously reported as August 21, 2011, in previous surveillance reports. § Infection was not identified until 2013, when an organ recipient developed rabies. Dr = Desmodus rotundus. Ln = Lasionycteris noctivagans. My sp = Myotis species. Ps = Perimyotis subflavus. Tb = Tadarida brasiliensis. Source: Centers for Disease Control and Prevention. Human Rabies. Available at: https://www.cdc.gov/rabies/location/usa/surveillance/human_rabies.html. Accessed June 1, 2017. |
Signs and Symptoms
Human rabies can be divided into five stages: incubation period, prodrome period, acute neurologic phase, coma, and death.7,16 The incubation period varies in length from two weeks to six months or more (average one to two months); the incubation period is shorter for bites to the head and face and longer for bites to the upper or lower extremities.15,17 During the incubation period, the patient may notice some tingling at the bite site; the patient carries the virus but is unable to transmit the virus to others. Unless they are presenting to the ED for bite wound management, patients usually will not present for medical care until the prodromal period. The prodrome period is characterized by two to 10 days of mild-moderate nonspecific flu-like symptoms, including malaise, fever, headache, sore throat, nausea, vomiting, diarrhea, and general musculoskeletal pain.7 By this time, the virus already is disseminated widely throughout the central nervous system.12 Without a known rabies exposure, it is unlikely a physician will include rabies in any differential at this point.
The acute neurologic phase presents as a serious deterioration and can be broken up into two subcategories of symptoms: furious rabies and paralytic (or dumb type) rabies. Furious rabies is the more common type, accounting for about two-thirds of cases, and presents with hyperactive symptoms, including hyperactivity, agitation, hypersalivation, hydrophobia, fluctuating consciousness and changed mental status, autonomic stimulation signs, and seizures.12 Paralytic rabies resembles Guillain-Barré syndrome, although progression to coma, myoedema, and bladder incontinence clearly differentiates these two disorders. Rabies after bat exposure has atypical features, such as focal brainstem signs, myoclonus, hemichorea, and Horner’s syndrome.12 The pathognomonic presentation of hydrophobia universally known in rabies (50-80% of patients) is actually a combination of hypersalivation (likely from viral reproduction in salivary glands) and pharyngeal muscle spasms. These spasms can be triggered by even a glimpse of water, thus resulting in the classic aversion to liquids. Eventually both types lead to coma (the paralytic type can take up to 30 days), followed by death. Rabies has nearly a 100% mortality rate, and occurs an average of five to 11 days after symptoms are present.12
Diagnosis
Human rabies can be a diagnostic challenge because of its rare occurrence in the United States and its varied clinical presentations, with symptoms that can be difficult to distinguish from Guillain-Barré syndrome.16 MRI findings during the prodromal and acute neurologic phases include enhancing hypersignal T2 changes along the brachial plexus and associated spinal nerve roots at levels corresponding with the bitten extremity and non-enhancing, ill-defined, mild hypersignal T2 changes of the spinal cord, temporal lobe cortices, hippocampal gyri, and cerebral white matter.12
Several tests are used to diagnose rabies antemortem in humans; however, no single test is sufficient.18 Tests should be performed on samples of saliva, serum, spinal fluid, and skin biopsies of hair follicles at the nape of the neck. Saliva is tested by virus isolation or reverse transcription followed by polymerase chain reaction (RT-PCR). Serum and spinal fluid are tested for antibodies to the rabies virus in patients who have never received rabies vaccinations. Skin biopsy specimens are examined for rabies antigen in the cutaneous nerves at the base of hair follicles. (See Figure 4.) Polymerase chain reaction (PCR) process with specific primers gives the ability to differentiate the rabies virus variants. The PCR produces an amplified “picture” of the genetic makeup of the virus. A restriction enzyme analysis step cuts the “amplicon” into unique DNA fragment patterns (sometimes referred to as DNA fingerprints), allowing the specific variant identification.19
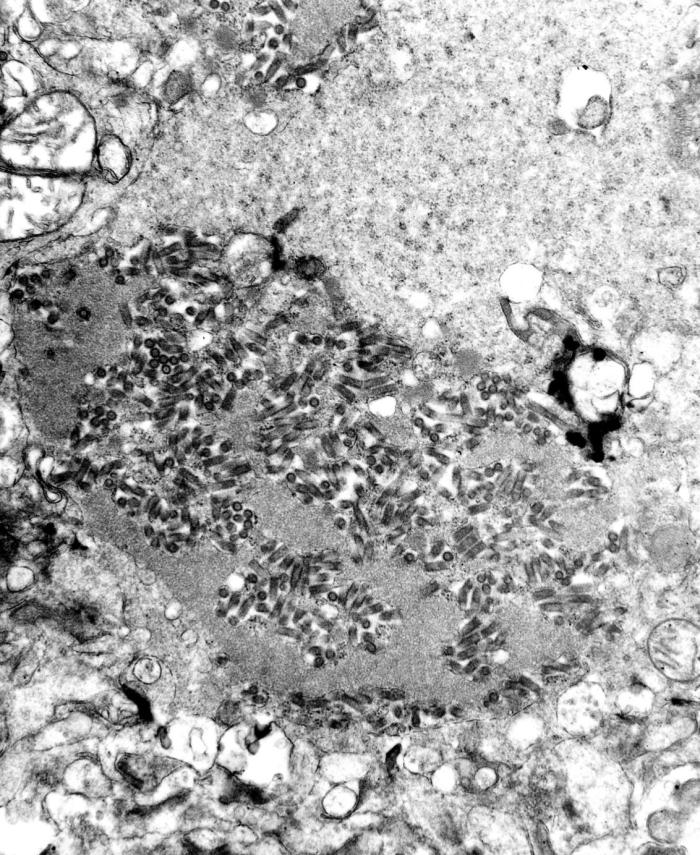
Figure 4. Rabies-infected Neuronal Cell |
|
This transmission electron microscopic (TEM) image reveals the presence of numerous dark, bullet-shaped rabies virions within an infected tissue sample. |
 |
|
SOURCE: Centers for Disease Control and Prevention. CDC/ F. A. Murphy. |
Treatment and PEP
Immediate and thorough washing of all bite wounds and scratches with soap and water is perhaps the most effective measure for preventing rabies. Preferably, the bite wound should be irrigated thoroughly and copiously with a virucidal agent (e.g., 1% benzalkonium chloride or povidone-iodine solution), which has been shown experimentally to kill the rabies virus, followed by normal saline irrigation.5,20
The rationale for PEP is based on the hypothesis that optimum efficacy requires both early and long-lasting neutralizing antibodies against the rabies virus. These are started as soon as possible after exposure, but there is no time limit prohibiting treatment initiation.5 The decision to begin PEP depends on the type of animal involved, whether it is available for postmortem testing (wild animals) or observation (dogs, cats, or ferrets), and the circumstances surrounding the bite. (See Figure 5.) PEP consists of a combination of a passive immunoprophylactic agent and an active immunoprophylactic agent. PEP is effective universally in preventing human rabies when administered promptly and appropriately. 20
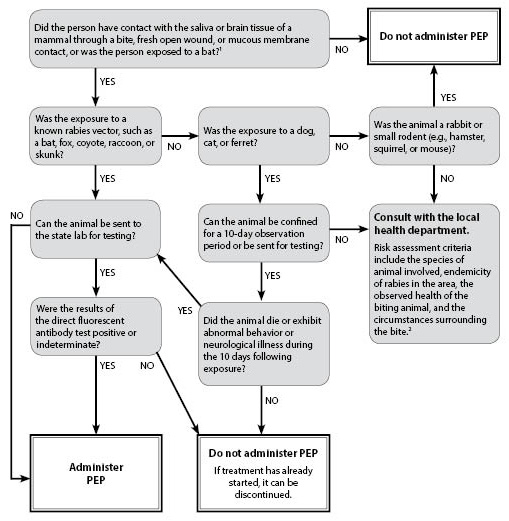
Figure 5. Human Rabies Post-exposure Prophylaxis (PEP) Algorithm |
 |
|
1. In addition to obvious bites or mucous membrane exposures, the CDC suggests that PEP be considered in cases where there is a reasonable probability that contact with a bat may have occurred (e.g., a deeply sleeping person awakens to find a bat in the same room; an adult witnesses a bat in the room with a previously unattended child; the exposed person is mentally disabled or was intoxicated when the exposure occurred), and rabies cannot be ruled out by testing the bat. PEP would not be warranted for other household members who do not meet these exposure criteria. Consult your local health department for questions regarding uncommon incidents. 2. Unprovoked exposures are rare and typically are characterized by an animal crossing neutral space to attack. Provoked exposures may include the following: attempting to feed an animal, having contact with an injured animal, entering an animal's territory, picking up, petting, or playing with an animal, attempting to break up a fight between animals, walking, running, or riding a bicycle past an animal. |
|
Adapted from materials developed by the Centers for Disease Control and Prevention and the Michigan Department of Community Health. |
Two brands of rabies vaccines currently are on the market: Imovax® Rabies (human diploid cell vaccine [HDCV]) and RabAvert® (purified chick embryo vaccine [PCEC]). Both are considered equivalent; however, because multiple doses are given in succession, it is recommended to administer the same brand for all doses if possible. The dose is 1 mL given intramuscularly in the deltoid only for adults/older children, and the outer thigh in young children (never gluteal). The dosing schedule for the rabies vaccine is four doses to be given on days 0, 3, 7, and 14 (day 0 being the first day of exposure or presentation for care). (See Table 3.) Previously, a fifth dose was given on day 28; however, the Advisory Committee on Immunization Practices no longer endorses the fifth dose and the CDC’s treatment recommendations no longer include the fifth dose.20 All rabies vaccines are inactivated cell cultured viruses and, thus, still are recommended for all immunosuppressed patients; however, the older five-dose vaccine series still is recommended in this population. (See Table 4.) The antibody response to these two active rabies vaccinations requires seven to 10 days to develop and usually persists for more than two years.
Table 3. Rabies Post-exposure Prophylaxis for Healthy, Immunocompetent Persons, Including Pregnant Women |
|||
Vaccination Status |
Treatment |
Dosage/Administration Guidelines for All Ages |
Day of Regimen |
|
Not previously vaccinated |
|
|
Day 0 (HRIG can be given up to day 7) |
|
|
Days 0, 3, 7, 14 |
|
|
Previously vaccinated† |
|
|
Days 0, 3 |
|
* Indicated if last tetanus vaccine was more than 5 years prior to exposure † Completed pre- or post-exposure regimen of human diploid cell vaccine (HDCV) or purified chick embryo cell vaccine (PCEC) within the past 20 years, or received another vaccine with documented serum titer corresponding to complete neutralization at ≥ 1.5 serum dilution (or its equivalent, approximately 0.1-0.2 IU/mL) by the rapid fluorescent focus inhibition test (RFFIT). SOURCE: Minnesota Department of Health |
|||
Table 4. Rabies Post-exposure Prophylaxis for Immunocompromised Persons |
|||
Vaccination Status |
Treatment |
Dosage/Administration Guidelines for All Ages |
Day of Regimen |
|
Immunocompromised, unvaccinated persons |
|
|
Day 0 (can be given up to day 7) |
|
|
Days 0, 3, 7, 14, 28 |
|
|
|
7-14 days following PEP completion |
|
|
Immunocompromised, previously vaccinated persons† |
|
|
Days 0, 3 |
|
|
7-14 days following PEP completion |
|
|
* Indicated if last tetanus vaccine was more than 5 years prior to exposure † Completed pre- or post-exposure regimen of human diploid cell vaccine (HDCV) or purified chick embryo cell vaccine (PCEC) within the past 20 years, or received another vaccine with documented serum titer corresponding to complete neutralization at ≥ 1.5 serum dilution (or its equivalent, approximately 0.1-0.2 IU/mL) by the rapid fluorescent focus inhibition test (RFFIT). SOURCE: Minnesota Department of Health |
|||
The passive immunoprophylactic agent is the human rabies immune globulin (HRIG). Two forms currently are available in the United States: Imogam® Rabies-HT and HyperRAB™ S/D. For treatment purposes, the two can be considered equivalent, as both come in 2 mL (300 IU) and 10 mL (1,500 IU) vials with concentrations of 150 IU per 1 mL. The weight-based dosing regimens, 20 IU/kg (0.133 mL/kg), also are equal for both drugs as in all age groups. This dosing is based on actual body weight. Ideal administration of HRIG is the full dose infiltrated around the bite or wound. Any remaining dose should be given intramuscularly at a site distant from the HDCV or PCEC vaccine administration site. The HRIG should be administered as early as possible, with the goal being on the day of presentation; however, it still can be given up to day 7 of the rabies vaccine protocol. The goal of this passive immunoprophylactic agent is to provide immediate protection from viral replication and transport to allow time for the active immunoprophylactic agent (rabies vaccine) to work.
Rabies PEP is expensive. Retail prices are approximately $350 per dose for Imovax® Rabies and RabAvert® and are $5,000 for 1,500 IU for Imogam® Rabies-HT and HyperRAB™ S/D.21,22 Not all hospitals or EDs carry these vaccinations, so clinicians can prescribe the vaccine for patients to fill at a pharmacy, including instructions as to the site at which the vaccine can be administered if they do not have a primary care provider who is willing to provide this service. ED providers also can use local county and state health departments to assist if needed. In addition, manufacturers have patient assistance programs and can be contacted for details. (See Table 5.)
Table 5. Human Rabies Products |
Human rabies immune globulin (HRIG) products |
|
Imogam® Rabies-HT Sanofi Pasteur 1-800-822-2463 |
|
HyperRab™ S/D Grifols Therapeutics Bayer Biological Products 1-800-243-4153 |
Human rabies vaccines |
|
Human Diploid Cell Vaccine (HDCV) Imovax IM® (pre- and post-exposure) Sanofi Pasteur 1-800-822-2463 |
|
Purified Chick Embryo Cell Vaccine (PCEC) RabAvert® (pre- and post-exposure) GlaxoSmithKline 888-825-5249 |
Once symptoms are present, rabies almost always is fatal, and treatment is supportive. There are four documented rabies survivors in the United States.23-26 All four patients had a vigorous and early immune response, with auto-sterilization (i.e., no detected virus or RNA in tissue or biological fluids) and rabies antibodies detected in serum and cerebrospinal fluid. Two received coma induction therapy, one had standard intensive care support, and another had presumptive abortive infection and did not receive any intensive support. Two patients, one of whom did not receive coma induction therapy, had non-neutralizing antibodies, suggesting that other mechanisms played a part in eradication of the virus. Survivors of rabies may have significant neurologic impairment.2,27
Family members and healthcare providers of patients who develop rabies should be evaluated for potential exposure of non-intact skin or mucous membranes to the patient’s saliva, tears, respiratory tract secretions, spinal fluid, or nuchal biopsy specimens. PEP should be offered to those with potential exposure after consultation with public health authorities (e.g., county or state health departments) and infectious disease experts.
SUMMARY
Rabies is an uncommon disease that rarely is encountered in U.S. EDs. Rabies is considered a uniformly fatal disease, but with proper awareness and early PEP, it can be prevented. All patients presenting to the ED with animal bites or bat exposures should be evaluated for criteria for rabies PEP. Rabies should be on the differential diagnosis of any patient who presents with acute encephalitis and a history of animal bites or bat exposures.
REFERENCES
- Birhane MG, Cleaton JM, Monroe BP, et al. Rabies surveillance in the United States during 2015. J Am Vet Med Assoc 2017;15:1117-1130.
- Christian KA, Rupprecht CE. Chapter 28: Rhabdovirus: Rabies. In: Kaslow RA, Stanberry LR, Le Duc JW, eds. Viral Infections of Humans: Epidemiology and Control. 5th ed. New York: Springer Science+Business Media; 2014.
- World Health Organization. Rabies. Human Rabies. Available at: http://www.who.int/rabies/human/en/. Accessed May 25, 2017.
- Gale Encyclopedia of Children’s Health: Infancy Through Adolescence. Animal Bite Infections. Available at: http://www.encyclopedia.com/medicine/diseases-and-conditions/pathology/animal-bite-infections. Accessed May 26, 2017.
- Dire DJ. Emergency management of dog and cat bite wounds. Emerg Med Clin North Am 1992;10:719-736.
- Centers for Disease Control and Prevention. Human Rabies. Available at: http://www.cdc.gov/rabies/location/usa/surveillance/human_rabies.html. Updated Sept. 21, 2015. Accessed May 23, 2017.
- Fishbein DB. Rabies in humans. In: Baer GM, ed. The Natural History of Rabies. 2nd ed. Boca Raton: CRC Press; 1991: 519-520.
- Schwartz M. The life and works of Louis Pasteur. J App Microbiol 2001;91:597-601.
- Hoenig LJ. Triumph and controversy: Pasteur’s preventive treatment of rabies reported in JAMA. Arch Neurol 1986;43:397-399.
- Lentz TL, Burrage TG, Smith AL, et al. Is the acetylcholine receptor a rabies virus receptor? Science 1982;215:182-184.
- Manning SE, Rupprecht CE, Fishbein D, et al. Human rabies prevention — United States, 2008: Recommendations of the Advisory Committee on Immunization Practices. MMWR Recomm Rep 2008;57(RR-3):1-28.
- Hemachudha T, Ugolini G, Wacharapluesadee S, et al. Human rabies: Neuropathogenesis, diagnosis, and management. Lancet Neurol 2013;12:498-513.
- Centers for Disease Control and Prevention. Rabies. Bats. Available at: https://www.cdc.gov/rabies/exposure/animals/bats.html. Updated April 29, 2016. Accessed May 25, 2017.
- Chatterjee P. India’s ongoing war against rabies. Bull World Health Organ 2009;87:890-891.
- Sudarshan MK, Madhusudana SN, Mahendra BJ, et al. Assessing the burden of human rabies in India: Results of a national multi-center epidemiological survey. Int J Infect Dis 2007;11:29-35.
- Hemachudha T, Laothamatas J, Rupprecht CE. Human rabies: A disease of complex neuropathogenetic mechanisms and diagnostic challenges. Lancet Neurol 2002;1:101-109.
- Smith JS, Fishbein DB, Rupprecht CE, Clark K. Unexplained rabies in three immigrants in the United States: A virologic investigation. N Engl J Med 1991;324:205-211.
- Centers for Disease Control and Prevention. Rabies. Diagnosis in animals and humans. Available at: https://www.cdc.gov/rabies/diagnosis/animals-humans.html. Updated Sept. 20, 2011. Accessed May 23, 2017.
- Texas Health and Human Services. Texas Department of State Health Services. Rabies. Available at: https://www.dshs.texas.gov/idcu/disease/rabies/testing/lab/typing. Updated July 13, 2012. Accessed May 23, 2017.
- Rupprecht CE, Briggs D, Brown CM, et al. Use of a reduced (4-dose) vaccine schedule for postexposure prophylaxis to prevent human rabies: Recommendations of the Advisory Committee on Immunization Practices. MMWR Recomm Rep 2010;59(RR02);1-9.
- GoodRx. Available at: https://www.goodrx.com. Accessed May 24, 2017.
- WellRx. Available at: https://www.wellrx.com. Accessed May 24, 2017.
- Hattwick MA, Weis TT, Stechschulte CJ, et al. Recovery from rabies. A case report. Ann Intern Med 1972;76:931-942.
- Willoughby RE Jr, Tieves KS, Hoffman GM, et al. Survival after treatment of rabies with induction of coma. N Engl J Med 2005;352:2508-2514.
- Centers for Disease Control and Prevention (CDC). Presumptive abortive human rabies—Texas, 2009. MMWR Morb Mortal Wkly Rep 2010;59:185-190.
- Centers for Disease Control and Prevention (CDC). Recovery of a patient from clinical rabies—California, 2011. MMWR Morb Mortal Wkly Rep 2012;61:61-65.
- Subramaniam Mani R. Correction: Human rabies survivors in India: An emerging paradox? PLOS Negl Trop Dis 2016;10:e0004975.
Rabies is an uncommon disease with a very high fatality rate. Recognition of a potential exposure and effective prophylaxis are critical in prevention of this devastating disease. The authors review recognition of suspicious bites/exposures, clinical presentation of rabies, and utilization of effective prevention strategies.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.