Hypersensitivity Reactions in the Pediatric ED: The Tip of the Iceberg
November 1, 2017
Reprints
AUTHOR
John Cheng, MD, Pediatric Emergency Medicine Physician, Pediatric Emergency Medicine Associates, LLC, Children’s Healthcare of Atlanta, Wellstar Health System, Atlanta, GA
PEER REVIEWER
Aaron Leetch, MD, FACEP, Assistant Professor of Emergency Medicine and Pediatrics, Residency Director, Combined Emergency Medicine and Pediatrics Residency, University of Arizona, Tucson
Executive Summary
- Food allergies typically are divided into IgE-mediated and non-IgE-mediated diseases. IgE-mediated allergies are rapid in onset, starting within minutes and up to two hours after ingestion. Usually, the children present with cutaneous, respiratory, gastrointestinal (GI), or cardiovascular (CV) symptoms via inflammatory mediator release from tissue mast cells and circulating basophils. Anaphylaxis to food presents most often with respiratory symptoms (70%), followed by GI (45%) and CV (45%) symptoms.
- Chicken egg allergy is the most common IgE-mediated food allergy in children, affecting 1-2% of children. The usual culprit is the proteins in egg whites. Unlike with milk allergy, even those children who react to eggs in baked products still have an excellent chance of outgrowing their allergy. In addition to food products, egg protein is used in immunizations, such as the influenza; measles, mumps, and rubella (MMR); measles, mumps, rubella, and varicella (MMRV); yellow fever; and rabies vaccines. Egg-allergic children still should receive the MMR and MMRV vaccines, but they should be observed for a longer period after administration.
- Exercise-induced anaphylaxis is characterized by extreme fatigue, warmth, flushing, pruritus, and urticaria, occasionally progressing to angioedema, wheezing, upper airway obstruction, and syncope.
- Oral allergy syndrome, or pollen-food allergy syndrome, is a type of contact allergy in people with allergic rhinitis due to pollen with symptoms that usually are confined to the oropharynx with immediate pruritus, irritation, and mild swelling of the lips/tongue/ palate/throat.
- More than 85% of food anaphylaxis is caused by peanuts or tree nuts. Some commonalities in fatalities are reactions to peanuts or tree nuts, adolescent or young adult age, lack of knowledge that allergies can be fatal, lack of enquiry as to what ingredients are in a dish or how it is cooked, and lack of an epinephrine auto-injector.
- Acute food protein-induced enterocolitis syndrome (FPIES) presents with profuse vomiting and diarrhea, severe dehydration, lethargy, and pallor. The emesis is usually severe, repetitive, and projectile, and occurs one to three hours after ingestion of the allergen. Diarrhea occurs later, about two to 10 hours after ingestion. Acute FPIES occurs if the allergen is ingested sporadically or if it was removed from the diet and then reintroduced.
Hypersensitivity reactions are very common. Understanding the different types, including serum sickness-like reactions, Stevens-Johnson syndrome, toxic epidermolytic necrolysis, and drug reaction with eosinophilia and systemic symptoms, is valuable both for an accurate and timely diagnosis as well as appropriate management.
— Ann M. Dietrich, MD, FAAP, FACEP
Visits to the emergency department (ED) for “allergic reactions” are common occurrences and encompass a wide variety of symptoms and presentations. The basic principles for treatment of these reactions are largely the same, regardless of the underlying etiology. The goal of this article is to discuss some of the common causes and presentations of these hypersensitivity reactions, as well as to provide information that can be useful in the care of these children, not only in the ED, but also after disposition from the ED. Some rare hypersensitivity reactions, such as serum sickness-like reactions (SSLR), Stevens-Johnson syndrome (SJS), toxic epidermolytic necrolysis (TEN), and drug reaction with eosinophilia and systemic symptoms (DRESS), also will be discussed. Although this article will cover a broad range of hypersensitivity reactions, this is just the proverbial tip of the iceberg.
Cases
- A 6-year-old girl presents with erythematous plaques, lip swelling, sore throat, coughing, and nausea. She is being treated for a urinary tract infection with cefprozil. She has had two doses so far. Her symptoms started after the first dose, but were very mild initially. They got much worse after her second dose. She has a history of anaphylaxis to amoxicillin. Her vital signs are as follows: temperature 37.6° C, heart rate 116, respiratory rate 32, blood pressure 109/63 mmHg. On exam, she has diffuse urticaria, edema, and erythema to her posterior oropharynx, and diffuse wheezes. She complains of abdominal pain, but is soft on exam.
- A 2-week-old boy presents with worsening vomiting and lethargy. He had an unremarkable birth history. His mother had negative serologies and was negative for group B streptococcal infection and herpes simplex virus (HSV). His mother reports profuse and repetitive emesis after every feed. Now, he is listless and does not seem to be interested in feeding at all. She was told that this was just typical reflux, but she thinks it is getting worse. On exam, you note a pale, lethargic newborn with the following vital signs: temperature 36.4°C, heart rate 190, respiratory rate 52, O2 saturations 93% on room air, blood pressure 72/38 mmHg. He has cool, loose skin with a capillary refill time of four to five seconds.
- A 16-year-old girl with a history of seizures presents with malaise, fatigue, and fever for the past two days. Yesterday, she started with a rash to her face that has generalized. Today, she developed facial edema. She does not report any new exposures in the past week; however, she was switched to lamotrigine four weeks ago since her previous regimen did not seem to be working. On exam, she has diffuse confluent, dark red plaques, erythema of her oral mucosa, ulcerations on her lips, and bilateral conjunctival injection.
Definition
Hypersensitivity reactions can be induced by any number of things that may or may not be obvious on initial presentation to the ED. The basic management of these reactions includes removal of the offending agent, if known, and supportive care. Although several medications are used in the care of these patients, there are few, if any, randomized case-control trials to evaluate their effectiveness. Many allergens can be organized into three large groups: food, insect venom, and medications/drugs. This article is organized by these three common allergen groups. See Table 1 for triggers of allergic reactions.
Table 1. Triggers for Allergic Reactions |
|
Insect Stings (Hymenoptera)
Medications
|
Exercise
Cholinergic
Environmental
Pressure
Other
|
Food: IgE-mediated Hypersensitivity Reactions
One-fifth of the U.S. population avoids particular foods at some point in their lives for fear of having an allergic reaction.1 Twenty percent of healthcare costs associated with food allergies are from ED visits, to the tune of $45 million per year. Some children who present with “food allergies” actually have food intolerance (an adverse physiologic response) or food aversion.2 Food intolerances often are mistaken for allergic reactions, but actually are irritant, non-immunologic reactions to food or to factors inherent to the food. Some such factors can be contaminants (e.g., fish parasites, mites in flour, scombroid), pharmacologic properties of the food (e.g., tyramine), and host characteristics that cause problems with digestion of the food.3-6 One example is the perioral rash that sometimes develops after eating tomatoes or berries. These symptoms do not last long and tend to resolve without intervention within six months.7 Non-immunologic reactions to food are more common than true food allergies. Food aversions can look like food intolerance but cannot be reproduced when the patient ingests the food in question in a blinded fashion.5
In contrast, food allergies are adverse health effects that arise from immune responses to an ingested food and are reproducible on exposure to the given food.5 To be classified as having a food allergy, a patient must have sensitization and develop specific signs and symptoms after exposure to the food.6 However, sensitization to a food does not necessarily equate to an allergy. This means that despite having circulating antibodies to the allergen, the child will not develop signs of an allergic reaction (e.g., hives, swelling, difficulty breathing, etc.) after ingestion of the allergen. For example, 8.6% of children have a positive peanut allergy test, but only 0.4% have a true allergy.8
Food allergies usually present in the first two years of life, with peak prevalence at 1 year of age. They affect 6-8% of children younger than 5 years of age and up to 4% of the general U.S. population.1,2,5,7,9 The highest rate of food anaphylaxis and hospitalization occurs in school-age children, but the highest rate of fatal anaphylaxis occurs in adolescents.10 The rate and the severity of allergic reactions to food has been increasing over time.2,5 See Table 2 for historical information needed to identify allergic reactions to food.
Table 2. Historical Information Needed to Identify Allergic Reaction to Food |
|
|
The Allergen |
|
|
The Reaction |
|
|
Prior History |
|
Food allergies typically are divided into IgE-mediated and non-IgE-mediated diseases.2,5,11 IgE-mediated allergies are rapid in onset, starting within minutes and up to two hours after ingestion. Usually, the children present with cutaneous, respiratory, gastrointestinal (GI), or cardiovascular (CV) symptoms via inflammatory mediator release from tissue mast cells and circulating basophils. Anaphylaxis to food presents most often with respiratory symptoms (70%), followed by GI (45%) and CV (45%) symptoms.12 See Table 3 for common symptoms of anaphylaxis.13 In addition, several factors have been found to make allergic reactions to foods both easier and more severe: ingestion of ethanol, nonsteroidal anti-inflammatory drugs (NSAIDs), gastric acid-reducing drugs, exercise, fever, intercurrent illness, and menstruation.5
Table 3. Common Symptoms of Anaphylaxis |
|
|
Skin
Respiratory
|
Gastrointestinal
Cardiovascular
Neurologic
|
|
Adapted from: Simons FE. Anaphylaxis. J Allergy Clin Immunol 2008;121(2 Suppl 2): S402-S407. |
|
The most common forms of food-induced anaphylaxis are IgE-mediated. They usually require ingestion of the allergen. There is no strong evidence that physical or casual contact with an allergen via skin, close proximity, or inhalation of aerosolized food proteins can cause anaphylaxis. Rarely does steam or vapor from cooking food (usually fish and shellfish) cause anaphylaxis.2,9,14 The most common allergens vary by age and geographic region. Overall, the most common allergens are peanuts, tree nuts, shellfish, and fish. Allergies to cow’s milk and chicken eggs, as well as soy and wheat, also are seen; however, these are often outgrown by childhood or adolescence.2,5,7
Cow’s Milk Allergy
Cow’s milk allergy affects 2.5% of children within in the first two years of life, usually presenting with GI or skin symptoms about a week after starting formula. Sixty percent of these are IgE-mediated. About 50% of milk-allergic children will outgrow their allergy by 1 year of age; 60-75%, by 2 years of age; and 90%, by 3 years of age. About half will develop sensitivities to other foods. Most of the children with non-IgE-mediated reactions will outgrow their sensitivity by 3 years of age. Those children with other allergic diseases will be less likely to grow out of their allergy. About 75% of children with milk allergy will be able to tolerate extensively heated milk in baked products. If they cannot tolerate milk in baked products, they most likely have a severe allergy and are less likely to outgrow it. Of note, about 13% of fatal anaphylaxis cases are due to milk. There is a high degree of cross-reactivity between milk proteins from cows, goats, and sheep.1,5,7
Chicken Egg Allergy
Chicken egg allergy is the most common IgE-mediated food allergy in children, affecting 1-2% of children. The usual culprit is the proteins in egg whites. About 70% of egg-allergic children may be able to eat egg proteins in baked products. However, unlike with milk allergy, even those children who react to eggs in baked products still have an excellent chance of outgrowing their allergy. Most will outgrow their allergy in childhood or adolescence. In addition to food products, egg protein is used in immunizations, such as the influenza; measles, mumps, and rubella (MMR); measles, mumps, rubella, and varicella (MMRV); yellow fever; and rabies vaccines. Egg-allergic children still should receive the MMR and MMRV vaccines, but they should be observed for a longer period after administration. As for influenza, rabies, and yellow fever vaccines, most organizations recommend against giving these to anyone with a history of hives, angioedema, allergic asthma, or anaphylaxis to egg proteins.1,5-7,15
Nut Allergy
Peanuts are the most common food allergen in people older than 4 years of age, affecting an estimated 0.6-1% of the population in developed countries. Many peanut products retain their allergenicity even after processing. One exception is highly refined peanut oil, since the refining process often removes most of the allergenic proteins. In contrast, cold-pressed (or extruded) oils still will be allergenic because of the presence of the peanut proteins. Peanut allergy usually presents between 14 and 24 months of age. Skin or air contact with the allergen usually does not cause a reaction. Twenty percent of peanut-allergic children will become tolerant with age; however, the allergy can recur in about 10% of cases if they do not eat peanuts on a regular basis. There is a low (5%) cross-reactivity with other legumes (soy, lupini beans, and peas). Between 25-50% of people with a peanut allergy also will have an allergy to tree nuts. Tree nut allergy affects about 0.6% of the U.S. population and includes walnuts, cashews, almonds, pecans, pistachios, and others (hazelnuts, Brazil nuts, pine nuts, and macadamia nuts). There is extensive cross-reactivity between the tree nuts. Tree nut allergy usually presents by 36 months of age. Nine percent of these children will become tolerant with age. Unfortunately, 74% of peanut allergies and 68% of tree nut allergies will present without a known prior exposure, usually as anaphylaxis.5,16-18
Shellfish and Fish Allergy
Shellfish and fish are other common allergens. True fish allergy must be distinguished from food-borne syndromes such as scombroid (where an oily fish such as tuna, mahi mahi, or mackerel is improperly stored and develops high levels of histamine) or an allergy to Anisakis simplex, a fish parasite. More people are allergic to white fish, salmon, and tuna, in order of decreasing prevalence. Those allergic to fresh or cooked salmon or tuna often can tolerate canned salmon or tuna. Shellfish allergy is the major cause of allergic reactions in adults, affecting about 2.3% of the U.S. population, compared to only 0.6% of children. There is a lot of cross-reactivity between crustaceans. Most do not outgrow this allergy.1,5
Other Food Allergies
Other food allergens include wheat and cereal grains and galactose-α-1,3-galactose. Wheat and cereal grains share a lot of homology with grass pollen and frequently are implicated in food allergies in children with eczema. Many children will develop a tolerance for wheat and soy over time, usually by adolescence. Galactose-α-1,3-galactose is a carbohydrate found in mammalian meats such as beef, pork, and lamb. Unlike reactions to other foods, this allergy presents several hours (usually three to four hours) after ingestion. Interestingly in some cases, there is a history of a bite by the Lone Star tick (Amblyomma americanum) prior to development of this allergy.3,5,6,15
Two subtypes of food allergies worth mentioning are food-dependent exercise-induced anaphylaxis and oral allergy syndrome.
Food-dependent Exercise-induced Anaphylaxis
Exercise-induced anaphylaxis is characterized by extreme fatigue, warmth, flushing, pruritus, and urticaria, occasionally progressing to angioedema, wheezing, upper airway obstruction, and syncope. It often has a co-trigger, typically food; other co-triggers include NSAIDs, ethanol, premenstrual state, high humidity, extreme heat or cold, and high pollen counts. Treatment plans include avoidance of the co-trigger for four to six hours prior to exercising, never exercising alone, discontinuation of exertion immediately once symptoms start, and always carrying a phone and an epinephrine auto-injector (EAI). Premedication and warm-ups do not affect incidence; however, some cases will benefit from daily medications such as an H1-antihistamine or cromolyn. Most patients experience fewer episodes over time.19-22
For food-dependent exercise-induced anaphylaxis, certain foods are co-triggers, commonly wheat, celery, other grains, nuts, and shellfish. Symptoms typically occur when the co-trigger is ingested within three to four hours of exercising. If the patient does not eat the co-trigger, then exercise occurs without a problem; conversely, the patient can eat the co-trigger without a problem as long as he or she does not exercise afterward. For treatment, patients should be counseled not to exercise less than four hours after eating; if there are no problems, this time interval can be shortened gradually.5,22
Oral Allergy Syndrome
Oral allergy syndrome, or pollen-food allergy syndrome, is a type of contact allergy in people with allergic rhinitis due to pollen. Some foods have proteins that are similar enough to certain pollen proteins that they cross-react with existing anti-pollen IgE. When these foods are ingested, the patients develop symptoms usually confined to oropharynx with immediate pruritus, irritation, and mild swelling of the lips/tongue/palate/throat. The culprit foods are fresh or uncooked fruits and vegetables; if the food is cooked and the proteins are denatured, there are no symptoms. Some examples are apples, pears, cherries, carrots, celery, soy, apricots, parsley, hazelnuts, and potatoes causing problems for birch-allergic patients and celery and mustard for mugwort-allergic patients.5,23
Anaphylaxis to Foods
Anaphylaxis due to food accounts for about half of anaphylaxis cases presenting to the ED and kills about 25 people in the United States per year, about 30% of anaphylaxis fatalities.24 More than 85% of food anaphylaxis is caused by peanuts or tree nuts. Some commonalities in fatalities are reactions to peanuts or tree nuts, adolescent or young adult age, lack of knowledge that allergies can be fatal, lack of enquiry as to what ingredients are in a dish or how it is cooked, and lack of an EAI. Typically, in fatal reactions, symptoms develop more rapidly, with a median onset of 25 to 35 minutes and death in less than an hour. Skin symptoms are less common in fatal reactions. Death usually is caused by respiratory collapse, not distributive shock. Of those reactions that are not fatal, one-third cause a biphasic reaction and one-fourth cause prolonged symptoms.1,3,5,9,15,19,20,24-26
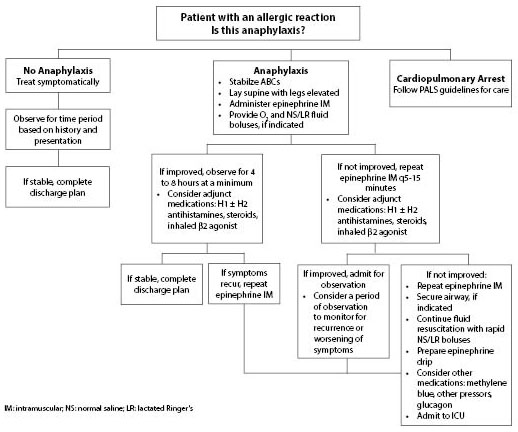
Testing can be done to look for sensitization to an allergen, but these tests do not prove that a person has a clinically significant allergy to a food and have limited, if any, utility in the ED setting. Treatment for food anaphylaxis is the same as for any anaphylaxis. See Figure 1 for a summary of anaphylaxis treatment.6,8,15,17,21,23,27
Food: Non-IgE-mediated Hypersensitivity Reactions
Non-IgE-mediated diseases present with subacute or chronic symptoms, taking more than two to three hours to present, and usually are isolated to the GI tract or the skin.2,5,8,11 A couple of common diagnoses that often present to the ED are food protein-induced proctitis and food protein-induced proctocolitis. These otherwise healthy infants present with mucous, blood-tinged stools and look well clinically. The stools typically are not diarrheal. Lab work usually is unremarkable. The symptoms commonly are triggered by cow’s milk proteins or soy, either in the formula or in the mother’s breast milk (up to 60% of cases). Symptoms start between 2 to 8 weeks of age and resolve by 2 years of age. The treatment consists of the elimination of the trigger; symptoms resolve in 48 to 96 hours. If the child is formula-fed, this most likely will mean switching to a hydrolyzed formula. Should the symptoms persist, the child should be placed on an elemental formula.2,28-31
Food Protein-induced Enterocolitis Syndrome
Rarer, but much more severe, non-IgE-mediated reactions are food protein-induced enterocolitis syndrome (FPIES) and food protein-induced enteropathy (FPIE). FPIES is thought to be a T-cell-mediated process involving the entire GI tract. It has a prevalence of 0.34%, with an onset at less than 2 months of age; however, diagnosis often is delayed for several months since these children are toxic-looking on presentation and are evaluated for other diagnoses before the diagnosis of FPIES is entertained. The differential diagnosis includes sepsis, metabolic/endocrine disorders, coagulation disorders, GI disorders (e.g., gastroesophageal reflux disease [GERD] or GI hemorrhage), and surgical problems (e.g., necrotizing enterocolitis, intussusception, and Hirschsprung’s disease). About one-third of these children also suffer from other atopic diseases or have a family history of atopy.
Acute FPIES presents with profuse vomiting and diarrhea, severe dehydration, lethargy, and pallor. The emesis is usually severe, repetitive, and projectile, and occurs one to three hours after ingestion of the allergen. Diarrhea occurs later, about two to 10 hours after ingestion. Acute FPIES occurs if the allergen is ingested sporadically or if it was removed from the diet and then re-introduced. In contrast, chronic FPIES occurs if the allergen is ingested daily. It presents with intermittent emesis, bloody diarrhea, lethargy, dehydration, abdominal distention, weight loss/failure to thrive, and metabolic acidosis. Solid food FPIES is different from acute and chronic FPIES in that it is associated with food-specific IgE and tends to have a more protracted course. It presents at a later age since solid foods are introduced later; however, onset after 1 year of age is rare.
The most common triggers are cow’s milk and soy. Acute and chronic FPIES usually start one to four weeks after the introduction of formula. Sixty percent of cases will occur after the first exposure, but many will occur after a period of tolerance. Fifty percent of children who react to cow’s milk also will react to soy. Breastfeeding may be protective; there have been only a couple of reported cases in breastfed babies.32 About one-third of these children will develop solid food FPIES. Solid foods that have been implicated include oats, rice, eggs, chicken, and turkey.
As stated above, these children will present very ill-appearing. They may present hypothermic, as well as with clinical signs of shock. Blood work can show metabolic acidosis, hyponatremia, hypoalbuminemia, methemoglobinemia, leukocytosis with bandemia, anemia, and thrombocytosis. Stool studies may have blood, reducing substances, and fecal leukocytes or eosinophils. An abdominal X-ray can show intramural gas, particularly in chronic FPIES. ED treatment consists of intravenous (IV) hydration, antibiotics (to cover for possible sepsis) and pressor support, if needed. Ondansetron has been reported to help with vomiting. A single dose of steroids (e.g., methylprednisolone 1 mg/kg, maximum dose of 60-80 mg) can be considered if there is a history of serious reactions or severe repetitive emesis, profuse diarrhea, lethargy, hypotension, or hypothermia to help suppress the presumed T-cell-mediated immune response.32
The key to the resolution of symptoms is elimination of the trigger. These children should be switched to extensively hydrolyzed formulas. If they do not improve, an amino acid-derived formula, such as EleCare or Neocate, is indicated. If they still do not improve, their symptoms are less likely to be due to a food allergy. If cow’s milk or soy is the trigger, the majority of patients become tolerant by 3 years of age at the latest. Chronic FPIES usually takes longer to resolve, by 5 years of age. Solid food FPIES has an even more protracted course. Ultimately, FPIES is a clinical diagnosis. If there is any doubt, an oral food challenge can be done. Families should be educated about monitoring their child going forward because of the possibility of cross-
contamination and of developing multiple triggers.2,28-40
FPIE is similar to FPIES in presentation, but only affects the small bowel. It usually presents in the first few months of life with diarrhea/steatorrhea, emesis, abdominal distention, poor weight gain/failure to thrive, early satiety, and malabsorption. Again, cow’s milk is the most frequent cause; other offenders include soy, eggs, wheat, rice, chicken, and fish. Celiac disease is the most severe form.2,31
Food: Mixed-IgE-mediated Hypersensitivity Reactions
Some reactions have a mixed picture in terms of whether IgE is implicated in the pathogenesis of the symptoms. Typically, these disorders present with GI and skin symptoms. Some examples are atopic dermatitis, eosinophilic esophagitis (EOE), and eosinophilic gastroenteritis. Atopic dermatitis can flare with the ingestion of a particular food allergen, either rapidly if IgE-mediated or much later if non-IgE-mediated. Chronic ingestion of the allergen can result in persistent skin lesions. EOE is a disorder in which eosinophils infiltrate the esophagus, resulting in abdominal pain, vomiting, and dysphagia. Presenting symptoms vary with age. Infants and toddlers present with gagging, choking, feeding refusal, and poor growth; school-age children present with pain or vomiting; and adolescents present with dysphagia and food impaction. There is a 1.25/100,000 incidence and a 4.3/100,000 prevalence in children younger than 19 years of age; more than 70% have a history of allergic diseases such as asthma, eczema, food allergies or sensitization, environmental allergies, or chronic rhinitis. Symptoms are intermittent and rarely occur in association with a particular food trigger; the severity of the symptoms does not necessarily predict the severity of the inflammation. These children typically are treated for GERD without success and ultimately are diagnosed via tissue biopsies taken during upper endoscopy. On the off-chance that there is a food trigger, some sources recommend a trial with an elimination diet, either focused or broad (e.g., empirically eliminating the six most common allergens: cow’s milk, hen’s egg, soy, wheat, fish and shellfish, and peanuts and tree nuts). Other treatment consists of swallowed steroids such as fluticasone or budesonide. Eosinophilic gastroenteritis is even more rare than EOE. In this case, eosinophils infiltrate the stomach, small intestine, and, rarely, the colon. It presents with abdominal pain, nausea, vomiting, diarrhea, malabsorption, and weight loss. Food allergy testing typically is not helpful. Elimination diets have variable success. Long-term management often requires immunomodulation with steroids, 6-mercaptopurine, or azathioprine. Acute management for food impaction typically involves IV hydration and endoscopic removal of the impaction and possible dilation of the narrowed area.28,29,31
Insect Stings
Reactions to insect stings are a frequent ED complaint. Fortunately, anaphylaxis is less common; only 0.5-5% of anaphylactic reactions are due to insect stings. About 3% of adults and < 1% of children have anaphylaxis to insect stings. Stings can be fatal on the first reaction; about half of the cases have no prior history of hypersensitivity reactions to stings. At least 40 to 50 deaths in the United States are caused by venomous insect stings annually. About half are caused by stings from insects in the Hymenoptera order, which includes the family Apidae (honey bees), Vespidae (yellow jackets, yellow hornets, white faced hornets, and paper wasps), and Formicidae (ants). All of these, except for the Apidae, can sting multiple times per insect. Less commonly, the saliva from biting insects, such as flies, mosquitoes, ticks, kissing bugs, and caterpillars, can cause reactions.3,19,41-44
The venom in these stings induces an IgE response, but also has its own vasoactive amines (histamine, dopamine, norepinephrine), acetylcholine, kinins, phospholipidase, and hyaluronidase. There is extensive cross-reactivity between venoms from the different members of the Vespidae family, and less so between members of the Apidae and Formicidae families. There is almost no cross-reactivity between the different families’ venoms. Although there can be a family history of sting allergies, it does not necessarily mean there is a higher risk of an allergy in a given child.41,42,45-48
When stung by a hymenopteran, children usually get cutaneous symptoms. The appearance of symptoms can be delayed up to 24 hours or more. Many sources group reactions into five types: local, large local, generalized, systemic, and delayed or unusual. In local reactions, there is limited swelling with pain and redness (1-5 cm) lasting < 24 hours. People who have this type of reaction tend to continue with the same type of reaction with future stings. In large local reactions, a large area of swelling (>10 cm) will develop contiguous to the sting over the course of hours to days and will persist for several days (five to 10 days). This reaction typically does not cause a problem unless there is anatomic compression based on where the sting is located (e.g., stings on the head, neck, throat, or tongue). About 11.5-19% of children have this type of reaction. About 5-10% of people with this reaction will have worse reactions with future stings.
In generalized reactions, symptoms, especially urticaria, angioedema, and pruritus, will develop beyond the sting site within minutes. Interestingly, the absence of urticaria or angioedema is associated with more severe reactions. In systemic reactions, anaphylactic symptoms develop within an hour of the sting. This reaction is less common in children (0.15-0.8%) than in adults (0.5-3%). If there is a large number of stings, a similar clinical picture can be seen but also may involve fever, malaise, nausea, and vomiting. Delayed or unusual reactions present later and include serum sickness, nephrotic syndrome, nephritis, acute renal failure, encephalopathy, myasthenia gravis, peripheral neuritis, Guillain-Barré syndrome, optic neuropathy, vasculitis, rhabdomyolysis, myocardial infarction, thrombocytopenic purpura, and diffuse alveolar hemorrhage.19,41,42,45,46,48-53
The likelihood of a systemic reaction increases with stings in the following order: yellow jackets < hornets < honeybees. Other risk factors for anaphylaxis from an insect sting include increasing age, male gender, history of a recent sting, previous severe systemic reaction, a sting on the head/neck/throat, the number of stings during a given event (e.g., getting stung by a swarm), and concurrent medical problems and therapies such as CV disease and medications (e.g., angiotensin-converting enzyme inhibitors, beta-blockers), mastocytosis, or increased baseline tryptase or platelet-activating factor levels. Thankfully, < 1% of cases have worsening reactions with future stings; most of the time, future stings cause about the same reaction as the index case.19,20,41-44,50,51
When treating these children, an attempt to remove the venom sac if the culprit was a bee is warranted; other hymenopterans typically do not leave a stinger/venom sac. Removal should be performed by scraping or dragging the stinger out of the skin. Methods that apply pressure to the stinger (e.g., pinching or grabbing it with tweezers) can release more venom from the venom sac. The venom usually is released within seconds, so if a patient presents much later after the sting, removal of the venom sac will not be as helpful. If the insect is still present, prompt removal is necessary, as some of the hymenopterans can sting more than once. In cases of multiple stings, one should consider checking a complete blood count, serum chemistries, and a myoglobin to screen for the unusual reactions listed above. Treatment is the same as with any other allergic reaction or anaphylaxis.
For local reactions, cold compresses and analgesics usually are sufficient. For large local reactions, a steroid burst also should be given. Treatment for more severe reactions is the same as for any severe allergic reactions and anaphylaxis. (See Figure 1.) The slower the onset of the reaction, the less likely it is to be life-threatening. In one study, 16% of sting anaphylaxis cases were biphasic. Experts recommend varying observation periods, ranging anywhere from three to eight hours at a minimum. Of note, local and large local reactions often can look like cellulitis, but rarely are infected; many of the venoms have inherent antimicrobial properties. The exceptions are stings by yellow jackets and fire ants, as they tend to scavenge rotting food. Interestingly, some people develop chronic or cold urticaria after a sting.41-43,45,46,48-50
Figure 1. Summary of Recommendations for Anaphylaxis Treatment |
 |
Sensitization to insect venom can be diagnosed by skin testing or venom-specific IgE titers. However, just as with food allergies, sensitization does not predict anaphylaxis. Discharge instructions, as with other types of anaphylaxis, should include education, prescription for EAI, and referral to an allergist. As part of the education, emphasis should be placed on avoidance or removal of insects and wearing of protective clothing. The patient should be reminded that hymenopterans usually sting in self-defense or to protect their nests from a perceived threat and that insect repellents are useful to minimize insect bites, not stings. There is some debate as to whether people with sensitivity to or allergy to insect stings should always carry an EAI, with the naysayers arguing that there is a low likelihood of getting stung (assuming that the patient does not do activities or have a job with unavoidable or increased exposure) and that it is more psychologically damaging to live in constant fear of getting stung. Referral to an allergist is important in these cases, not just for further screening for other medical conditions (such as mast cell disorders that are present in 1-2% of cases), but also to determine whether venom immunotherapy is warranted; courses last three to five years, but decrease the risk for severe anaphylaxis to insect stings by 98% and have an effect that lasts for decades.3,20,43,45,46,49,54
Drugs
Drug reactions span all the types of hypersensitivity reactions: penicillin reactions are IgE-mediated; vancomycin, radiocontrast media (or contrast), and opioid reactions are non-IgE-mediated. In addition to these, there are the immune complex-mediated reactions (e.g., serum sickness) and the delayed hypersensitivity reactions (e.g., SJS, TEN, and DRESS). About 6.7% of these reactions occur in hospitalized patients and 0.32% are fatal.55-57 Cutaneous symptoms are the most common reactions, usually a maculopapular rash within a few hours of taking a medication, urticaria within the first couple of weeks of starting a medication, or a fixed drug eruption. A fixed drug eruption is characterized by erythematous plaques that recur in almost the exact same spots with re-exposure to the offending drug, commonly caused by trimethoprim-sulfamethoxazole, NSAIDs, and acetaminophen. Immune complex-mediated and delayed hypersensitivity reactions rarely are seen.57-59
The most common medications that cause reactions are penicillins and trimethoprim-sulfamethoxazole, followed by NSAIDs. Other medications that frequently cause reactions are chemotherapeutic agents, monoclonal antibodies, immunotherapy allergens, anti-epileptics, antifungals, perianesthetics (e.g., most commonly muscle relaxants/neuromuscular blocking agents), contrast, and opioids. Again, these reactions can be IgE-mediated or non-IgE-mediated (i.e., by direct stimulation of mast cells). Risk factors for having a reaction include prior exposure to the medication, route of administration, dose, dosing schedule, properties of the causative agent, patient age, hypergammaglobulinemia and cryoglobulinemia, and genetic predispositions. As an example of genetic predisposition, antibiotic sensitivity in a parent confers a 15-fold increased risk for the same sensitivity in the child and a 10-fold increased risk for sensitivity to a different, unrelated antibiotic.19,21,56,57
Penicillin is the most common cause of drug-induced anaphylaxis. It has multiple antigenic determinants to which antibodies can be made. Although there is very low cross-reactivity (< 2%) between penicillins and cephalosporins, it is most commonly seen with first-generation cephalosporins. Similarly, there is low cross-reactivity between penicillins and carbapenems. Allergic reactions to cephalosporins are rare, usually caused by a reaction to the cephalosporin side chain.59 If there is a question as to whether a child who is penicillin-allergic can receive cephalosporins, a penicillin skin test can be done. If the skin test is negative, it is unlikely that there will be any reactions to cephalosporins.
As for other major classes of antibiotics, anaphylaxis to sulfonamides, trimethoprim, macrolides, and fluoroquinolones is rare. Reactions to aspirin/NSAIDs, vancomycin, and opioids usually are non-IgE-mediated, resulting from direct stimulation of mast cells. Anaphylaxis to NSAIDs typically is drug-specific rather than class-specific, except for aspirin-related reactions; aspirin-exacerbated respiratory disease shows cross-reactivity across the different NSAIDs. Reactions to vancomycin and opioids can be minimized by infusing the medications over a longer period of time and the concomitant use of antihistamines.3,19,57,60
Although neuromuscular blocking agents and chlorhexidine are among the more common perianesthetics to cause anaphylaxis, other anesthetics are known offenders. Barbiturates, such as phenobarbital and methohexital, are one such class of drug; there is cross-reactivity between the different barbiturates. Most non-barbiturates (e.g., propofol, ketamine, etomidate, and benzodiazepines) usually do not cause problems. Propofol allergy is rare, despite the fact that it contains egg phosphatide and a soybean emulsion. The reported cases of propofol allergy have not been clearly caused by propofol.3,61
Vaccinations seldom trigger anaphylaxis. More often, if a reaction occurs, it is the result of something with which the vaccine is made rather than the biologically active agent. The most commonly implicated vaccines for reactions are the vaccines for measles, diphtheria-tetanus-pertussis, and the hepatitis B virus. The incidence of reactions is 1.6 to 1.8 per million doses. The incidence of anaphylaxis to vaccines is even more rare: 0.26 per million doses, using the established definition of anaphylaxis. Typically, if there is going to be an allergic reaction to a vaccine, it will occur in less than 60 minutes.14,62-64
Latex allergy is a result of IgE-mediated reactivity to antigens from the plant Hevea brasiliensis. The risk of this allergy is higher in healthcare workers, people with certain medical conditions (e.g., spina bifida, urologic abnormalities), and workers with occupational exposure. The reaction can present with urticaria, angioedema, allergic rhinitis, asthma exacerbation, or anaphylaxis. The treatment for reactions is the usual treatment for any anaphylactic reaction; limitation of exposure is key. Of note, there are several foods that cross-react with latex of which patients should be aware: kiwi, potato, tomato, papaya, avocado, chestnut, and green pepper.14,19-21
Reactions to contrast, including gadolinium (although very rare), are not IgE-mediated, but have the same clinical appearance as IgE-mediated anaphylaxis. Symptoms for this reaction typically include CV and cutaneous symptoms (urticaria, angioedema), as well as vomiting. The reaction is thought to be related to the hypertonicity of the contrast that augments basophil and mast cell histamine release. It is independent of contrast dose or concentration. With the advent of lower osmolality contrast, the risk of reactions decreased to one-fifth of what it was previously. There is a 5-8% frequency for adverse reactions, about 1% for moderate reactions, and < 0.1% for life-threatening anaphylaxis with high osmolality contrast. Patients at higher risk of a reaction are those who have had prior reactions to contrast, as well as patients with atopy, asthma, or CV disease, particularly needing beta-blockers. There is no evidence that patients with allergies to the inorganic iodine present in seafood or in topically applied iodine-containing solutions will have adverse contrast reactions. There have been some reports of success in decreasing adverse contrast reactions with premedication regimens consisting of steroids, H1 and H2 blockers, and, on occasion, other medications such as ephedrine. These regimens typically start hours before the actual administration of contrast.3,19,57
With all of these reactions, the acute management is the same as for any type of anaphylaxis. (See Figure 1.) Long-term management consists of avoiding the offending medication and use of non-cross-reacting medication. In some cases, however, avoiding the medication is impossible. In these cases, desensitization protocols can be used to induce tolerance for the duration of an uninterrupted treatment course. These protocols work, but only temporarily; should the drug need to be used again, another desensitization protocol must be completed. Follow-up with an allergist is necessary to confirm allergy to a medication.
Serum Sickness/Serum Sickness-like Reactions
In 1905, Pirquet and Schick coined the term “serum sickness” to describe the course of a patient who had received horse serum as an antitoxin for diphtheria and scarlet fever. It is a type III hypersensitivity reaction where an antigen and antibody are both present, forming an antigen-antibody (immune) complex. Usually, these complexes are cleared by the mononuclear phagocytic system. However, if there is any excess, these complexes get deposited on blood vessel walls or within tissues, activating complement and granulocytes, resulting in a cascade of inflammatory mediators. Typically, the reaction starts seven to 12 days after the injection of foreign material, but can appear as late as three weeks. If there was a previous exposure, the reaction can appear even sooner on re-exposure. SSLRs have a similar clinical appearance and course, but are caused by different, as of yet unelucidated, mechanisms. They usually are less severe. Common causes for serum sickness and SSLR are medications (e.g., penicillins, tetracyclines, cefprozil, cefaclor, sulfonamides, macrolides, griseofulvin, and itraconazole), antitoxins (e.g., anti-rabies, anti-diphtheria, anti-botulinum toxin), antivenoms (i.e., snake and spider), immune modulators (e.g., monoclonal antibodies), immunizations (e.g., rabies, possibly pneumococcal and Haemophilus influenza B), illnesses (e.g., hepatitis B, streptococcal infections, other viral infections), bovine serum albumin, streptokinase, and insect stings.58,63-67
These children present with a triad of rash, arthralgia, and fever. Often, there is a history of edema and erythema at the injection site (if there was an injection), followed by the appearance of other symptoms including intermittent fever, malaise, rashes that are fixed and do not fade within 24 to 36 hours (e.g., urticaria, morbilliform), pruritus, edema, myalgias, lymphadenopathy, arthralgias (especially metacarpal phalangeal joints, knees, wrists, ankles, and shoulders), arthritis (less commonly), nausea/vomiting/diarrhea, abdominal pain, and melena. The urticarial rash usually starts in flexural creases and then generalizes. There is no involvement of mucosal membranes, unlike in SJS or TEN. The edema and erythema of the hands and feet, along with the joint pain, usually are severe enough that these patients are fussy and often refuse to walk.58,66
The differential diagnosis is broad, including any diagnoses with fever, arthralgias, and a rash such as DRESS, viral illnesses with exanthema, hypersensitivity vasculitis, acute rheumatic fever, acute meningococcal or gonococcal infection, systemic juvenile idiopathic arthritis, Kawasaki’s disease, acute annular urticaria, and other types of drug reactions. The diagnosis is made mainly by history and presentation. Lab studies can be done to support the diagnosis of serum sickness, showing decreased C3/C4/CH50, increased A3a anaphylatoxin, increased erythrocyte sedimentation rate and C-reactive protein, decreased platelets, renal dysfunction, hypoalbuminemia, and mild protein/hemoglobin/red blood cells in the urine. However, in the case of SSLR, lab tests frequently are unremarkable and are not needed.58,66,68
Usually, these reactions are self-limited, resolving within one to two weeks, although they can last up to six weeks. They usually can be managed on an outpatient basis. Key to the resolution of symptoms is the removal of the offending agent. Supportive care with antihistamines and analgesics (e.g., NSAIDs) is helpful. Severe cases may require a steroid burst with a rapid taper (< 1 week). For worst-case scenarios of serum sickness in which symptoms are not resolving or organ system dysfunction is noted, the antibodies may need to be removed by various methods such as intravenous immunoglobulin (IVIG), anti-B cell antibodies (i.e., rituximab), cytotoxic agents, or plasmapheresis. Rare complications of serum sickness include Guillain-Barré syndrome, peripheral neuritis, carditis, and glomerulonephritis.58,65-67
Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis
SJS and TEN (Lyell’s syndrome) are rare type IV hypersensitivity reactions and often, but not always, are caused by a drug reaction. Originally thought to be a form of erythema multiforme, SJS and TEN now are thought be along the same spectrum, but distinct from erythema multiforme, which typically is caused by a reactivation of HSV, rather than a drug reaction.69-71 They are characterized by severe mucocutaneous reactions with varying amounts of skin detachment with blisters and erosions. They are classified based on body surface area (BSA) affected. SJS affects < 10% BSA and TEN affects > 30% BSA. A third group is an overlap between SJS and TEN that affects 10-30% BSA. BSA is measured as it would be with a burn, with a Lund and Browder chart or by the palmar method.58,70,72-77
There are an estimated two to seven cases per million of SJS and TEN per year, with SJS being about three times more common than TEN. They can occur at any age; about 10-20% of cases have been reported in children. Risk factors include genetic factors (e.g., human leukocyte antigen [HLA] types with specific drugs), malignancy, high doses and rapid introduction of medications, autoimmune diseases (e.g., systemic lupus erythematosus), immunosuppression with long-term glucocorticoid therapy or HIV infection, and physical stimuli (e.g., ultraviolet light or radiation therapy). Overall, mortality is 1-5% for SJS and 25-30% for TEN, continuing even one year after onset of disease. Fortunately, in children, the mortality is lower, ranging from 0-9.5%. The highest morbidity and mortality occurs in cases of TEN with visceral lesions, with sepsis and multi-organ failure as the most common causes of death.55,58,72,73,75,76,78-82
SJS and TEN commonly are triggered by medications, usually within the first eight weeks of treatment, with an average time of six to 14 days. However, symptoms can occur within hours if the child has been re-exposed to the drug. Commonly implicated drugs are allopurinol, aromatic anticonvulsants (phenytoin, carbamazepine, lamotrigine, phenobarbital), antibacterial sulfonamides, nevirapine, oxicam NSAIDs (e.g., meloxicam and piroxicam), and penicillins. There have been reported cases with cephalosporins, quinolones, and acetaminophen also. However, 20-25% of cases cannot be clearly linked to a drug. Another common trigger in children is Mycoplasma pneumoniae infection. In addition, some infections may be cofactors with a given drug such as viruses (e.g., cytomegalovirus [CMV], coxsackie, influenza, Epstein-Barr virus [EBV], human herpesvirus [HHV] 6 and 7, parvovirus), bacteria (e.g., group A streptococcus), and rickettsia. Usually, the infections start about a week before the symptoms appear.72,74-76,78,82-84
The pathogenesis of these diseases is poorly understood. Studies are looking at interactions involving cell surface proteins (e.g., the major histocompatibility complex) and drugs leading to keratinocyte apoptosis via cell-mediated cytotoxic reactions involving various mediators. The hallmark of SJS and TEN, seen on skin biopsy, is keratinocyte necrosis with separation at the dermoepidermal junction, resulting in partial to full thickness necrosis of the epidermis and the appearance of frank subepidermal bullae.72,73,75,76,78,82,84,85
These patients usually report a prodrome of fever and influenza-like symptoms with malaise, myalgia, and arthralgia. Occasionally, they can also have cough, rhinitis, nausea, diarrhea, and headache. Other symptoms quickly develop and include photosensitivity, conjunctival itching or burning, and odynophagia. Within 24 to 48 hours, a tender rash develops, initially ill-defined, then coalescing into erythematous macules with purpuric centers or sometimes diffuse erythema. The rash usually starts on the face and trunk and then spreads symmetrically, rarely involving the palms and soles and sparing the scalp. The lesions progress to vesicles and bullae; both Nikolsky’s sign (production of new bullae with gentle friction on intact skin) and Asboe-Hansen sign (lateral spread of bullae with pressure) are observed. Mucosal lesions can precede or follow the appearance of the rash and occur in about 90% of cases, resulting in painful crusting and erosions on any surface. Painful hemorrhagic erosions with grayish-white membranes appear on the oral mucosa and vermillion border, often resulting in poor oral intake and dehydration. Pharyngeal mucosa usually is similarly affected. Severe conjunctivitis with purulent discharge occurs in about 80% of cases and can result in corneal ulceration, anterior uveitis, and panophthalmitis. Urethritis occurs in two-thirds of cases, as well as genital erosions, leading to urinary retention. Although respiratory, esophageal, and intestinal involvement are rare, there is a higher risk of airway obstruction in children because of their smaller airways. The acute phase of the illness usually lasts eight to 12 days; the average time from onset of symptoms to maximum detachment of skin is eight days. SJS often takes four to six weeks to recover. TEN often takes two to four weeks to heal. Usually, the skin that was attached (including nails) will be shed as part of the healing process.55,58,59,72,73,75-77,79,81,84-88
The differential diagnosis for SJS/TEN includes erythema multiforme, erythroderma and other erythematous drug eruptions, acute generalized exanthematous pustulosis, generalized bullous fixed drug eruption, phototoxic eruptions, staphylococcal scalded skin syndrome, paraneoplastic pemphigus, and linear IgA bullous dermatosis. Although many of these can be distinguished from each other based on history and physical exam, a skin biopsy can be done to make a definitive diagnosis. Other labs can be supportive, but most testing done in cases of SJS and TEN are more to evaluate severity of disease and efficacy of resuscitation rather than to establish diagnosis. A complete blood count typically will show anemia and lymphopenia. Neutropenia can be seen in one-third of cases, but may be masked by demargination due to stress or to administration of steroids. Metabolic panels often show increased blood urea nitrogen (BUN) and glucose, hypoalbuminemia, and mild increases in AST and ALT (but not overt hepatitis). Cultures, often obtained because of concerns for infection, usually are negative. Testing for Mycoplasma pneumoniae can be useful should it be the underlying etiology of the symptoms.68,70,72,73,79
The treatment consists of removal of the offending agent and supportive care. These patients usually need to be cared for in a burn unit, ICU, or a specialized dermatology unit. As with burns, supportive care consists of wound care, careful fluid and electrolyte management, temperature management, nutritional support, pain control, and monitoring/treating for superinfections. Non-adherent dressings should be used to dress wounds, with or without debridement. Although these patients do need fluid resuscitation, they have been found not to need as much as a burn patient (about one-third). Several sources report using a modified Parkland formula of [(2 mL/kg) × (kg) × (% BSA affected)] to guide fluid resuscitation and then titrating fluids to a goal of > 1 mL/kg/hour of urine output. Particular attention should be paid to temperature and analgesia to minimize catabolism and further stresses on the system. Although monitoring for infections is important, prophylactic antibiotics are not recommended. Inpatient management includes early ophthalmologic consult and treatment to minimize eye injury.58,59,70-73,75,77-79,82,84,88-91
Beyond supportive care, many adjunct medications have been tried over the years. Unfortunately, given the rarity of the SJS/TEN, only small studies have been published. Because of this, no official recommendations have been made about the use of systemic corticosteroids, IVIG, or other medications such as cyclosporine, TNF inhibitors, plasmapheresis, and cyclophosphamide. However, given existing data, many sources now believe that steroids are contraindicated.70-75,77-79,84,88,90,92-94,99-101
Acute complications of SJS/TEN mirror what is seen with burn patients: shock and electrolyte imbalance due to massive fluid loss, bacterial superinfection (especially bacteremia), pulmonary problems (e.g., pneumonia, pneumonitis, acute respiratory distress syndrome), GI complications due to epithelial necrosis along the GI tract, insulin resistance, hypercatabolic state, and multi-organ dysfunction. Long-term complications result from the healing process and post-inflammatory changes in any affected organ systems.79,80,84 The prognosis for children with SJS/TEN is better than for adults; they have decreased mortality and faster re-epithelialization.71 Unfortunately, recurrence is possible. In one study, one-fifth of children had a recurrence of SJS within seven years. In some cases, there was a recurrent infection with Mycoplasma pneumoniae or HSV; in others, an exposure to another medication.99 With recurrence in mind, parents should be warned about cross-reactivity between medications.79
Drug Reaction with Eosinophilia and Systemic Symptoms
DRESS is a rare, but life-threatening, type IV hypersensitivity reaction to a drug. Over the years, it has had several names, such as drug hypersensitivity syndrome, anticonvulsant hypersensitivity syndrome, drug-induced pseudolymphoma, dapsone syndrome, and phenytoin syndrome. Its true incidence is unknown. In retrospective studies, it has been shown to have a 5-10% mortality rate, mainly due to acute liver failure, multi-organ failure, fulminant myocarditis, or hemophagocytosis. The most commonly reported offending drugs are carbamazepine, lamotrigine, phenytoin, phenobarbital, valproic acid, zonisamide, and allopurinol. Other reported offenders include olanzapine, sulfonamides, dapsone, minocycline, and vancomycin. As with SJS/TEN, there is some thought in some cases that there is an association with certain HLA haplotypes.55,58,73,102-104
DRESS is defined by a rash, blood abnormalities, lymphadenopathy, and internal organ involvement. The reaction typically has a long latency period, starting two to eight weeks (up to three months) after drug exposure, even if the drug has been stopped. Onset of symptoms can happen faster if there is re-exposure to the drug. It is thought to be the result of a delayed cell-mediated response with expansion of activated T cells leading to an infiltration of eosinophils into tissues resulting in edema and inflammation. Interestingly, an association with the reactivation of a human herpesvirus (e.g., HHV6, HHV7, EBV, CMV) has been noted.55,58,73,81,84,102,104,105
Patients with DRESS present similarly to those with SJS/TEN: fever, malaise, fatigue, skin pain and pruritus, and odynophagia. Lymphadenopathy also is a prominent symptom in many cases. Soon, a rash develops, starting as a morbilliform eruption on the face that then spreads diffusely. The rash becomes confluent, resulting in an infiltrated erythema with follicular accentuation; the color becomes increasingly blue or violaceous. Often, more than 50% BSA is affected, and victims have two or more of the following: facial edema (periorbital and midface), infiltrated lesions, scaling, or purpura. Blood work shows leukopenia initially, then leukocytosis (usually eosinophilia), anemia, and thrombocytopenia. In addition, there is other organ involvement, usually liver, kidneys, and lungs. The liver is the most frequently affected internal organ, presenting with hepatomegaly and jaundice. However, there may not be any clinical signs, only lab abnormalities (elevated ALT and alkaline phosphatase). Severe liver impairment (i.e., hepatic necrosis) is a poor prognostic indicator. The kidneys usually present with interstitial nephritis, showing increases in creatinine with a high BUN/creatinine and decreased creatinine clearance, proteinuria, and abnormal urinary sediment. The lung usually has nonspecific symptoms such as cough, tachypnea, or dyspnea. Other organ systems also can be affected: CV (myocarditis), GI (gastroenteritis, ulcers, dehydration), endocrinologic (pancreatitis, type I diabetes mellitus) and thyroid dysfunction (thyroiditis, sick euthyroid), neurologic (rarely meningitis or encephalitis, headache, seizures, palsies, coma), muscular, and ophthalmologic. Although not all symptoms need to be present to make the diagnosis of DRESS, there must be at least a rash, suspicion that symptoms are drug-related, need for hospitalization, and three out of four of the following features: fever > 38°C, lymphadenopathy at two sites, any internal involvement, and hematologic abnormalities.58,59,73,81,84,102-105
Again, management consists of withdrawal of the offending drug and supportive care. As with SJS/TEN, subspecialty care most likely will be needed. The average recovery time is six to nine weeks. In up to 20% of cases, the disease can persist for months with remission and relapses; however, most patients recover completely. Beyond supportive care, people have turned to immunomodulators, such as steroids, cyclosporine, and IVIG, to try and treat DRESS faster and/or manage complications during their inpatient stay. As with SJS/TEN, parents should be educated on avoidance of the offending drug in the future, as well as the possibility of genetic predisposition for reaction to other drugs and for reactions to related drugs due to cross-reactivity.59,73,81,84,102,105,106
Summary
This article briefly covered hypersensitivity reactions from the more common allergic reactions and anaphylaxis to the rarer serum sickness/SSLR, SJS/TEN, and DRESS. The article also reviewed common groupings of allergens: food, insect stings, and drugs. Each of these can have different mechanisms and presentations. Some are IgE-mediated and others are non-IgE-mediated. Regardless of the reaction, basic management in the ED is the same: remove the allergen and provide supportive care. Each reaction has other medications that can help with treatment (e.g., epinephrine, steroids, antihistamines for anaphylaxis; IVIG and steroids for SJS/TEN and DRESS), but there have been no large, randomized case-control studies to establish effectiveness of any of these treatments. For the majority of cases of allergic reactions/anaphylaxis, diagnostic testing in the ED is not helpful. However, in the rarer diagnoses, such as serum sickness (not SSLR), SJS/TEN, and DRESS, diagnostic testing to evaluate for organ system involvement, other than skin, should be done, along with admission for observation and supportive care. Should the patient become stable for discharge, careful counseling about allergen avoidance and the cross-reactivity of various allergens to prevent future reactions is mandatory. In addition, a prescription for an EAI and a referral to an allergist is indicated in most cases.
Case Conclusions
- This young girl with the amoxicillin allergy who was being treated for a urinary tract infection with cefprozil was in anaphylaxis. She was given epinephrine IM, as well as diphenhydramine, methylprednisolone, ranitidine, and IV fluids. Her exam and vital signs normalized completely after the epinephrine. After about 1.5 hours, her hives returned, and she started wheezing again. A second dose of epinephrine IM was given, again with complete resolution of symptoms. She was admitted overnight for observation and discharged home the next day with prescriptions for prednisolone, diphenhydramine, ranitidine, and EAI and with instructions to follow up with her pediatrician in 24 hours and ultimately with an allergist.
- This newborn was evaluated for sepsis and an inborn error of metabolism. His workup was negative and he improved with IV fluids. On hospital day #2, he was allowed to take Pedialyte. Since he did well with that, he was later switched back to Gerber Good Start. Within an hour of taking the formula, he began having profuse non-bilious, non-bloody vomiting. A couple of hours later, he had a watery, non-bloody stool. Repeat labs showed acidosis again, but were otherwise reassuring. Abdominal X-ray and pyloric ultrasound were normal. He was switched to an amino acid formula after 24 hours of improvement and did well. He was diagnosed with FPIES and discharged home after 24 hours of tolerating the new formula.
- This young woman ultimately was diagnosed with TEN. Her rash continued to worsen, forming bullae in > 30% of her BSA. She had both Nikolsky and Asboe-Hansen signs on exam. Her labs showed mild lymphopenia and anemia, a high BUN/creatinine ratio, and a low CO2, but otherwise was unremarkable. After a normal saline bolus and a dose of morphine for her pain, she was transferred to a burn center. There, she was treated with meticulous wound care, continued IV hydration and analgesia, as well as a course of IVIG. She improved quickly and was discharged home within a week, with instructions to avoid lamotrigine in the future and to follow up with an allergist and her neurologist to discuss future choices for anti-epileptics, with an eye toward avoiding cross-reactive medications.
REFERENCES
- Keet CA, Wood RA. Food allergy and anaphylaxis. Immunol Allergy Clin North Am 2007;27:193-212.
- Sampson HA, Leung DYM. Chapter 150: Adverse Reactions to Foods. In: Kleigman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. 18th ed. Phildelphia: Saunders Elsevier; 2007: 986-990.
- Lieberman P, Nicklas RA, Randolph C, et al. Anaphylaxis — a practice parameter update 2015. Ann Allergy Asthma Immunol 2015;115:341-384.
- Simons FE, Ardusso LR, Dimov V, et al. World Allergy Organizations Anaphylaxis Guidelines: 2013 update of the evidence base. Int Arch Allergy Immunol 2013;162:193-204.
- Nowak-Wegrzyn A, Burks AW, Sampson HA. Chapter 81: Reactions to Foods. In: Adkinson NF Jr, Bochner BS, Burks AW, et al, eds. Middleton’s Allergy: Principles and Practice. 8th ed. Volume 2. Philadelphia: Elsevier Saunders; 2014: 1310-1339.
- Boyce JA, Assa’ad A, Burks AW, et al. Guidelines for the diagnosis and management of food allergy in the United States: Summary of the NIAID-sponsored Expert Panel Report. J Allergy Clin Immunol 2010;126:1105-1118.
- Wood RA. Food allergy in children: Prevalence, natural history, and monitoring for resolution. Sicherer SH, TePas E, eds. UpToDate Available at: www.uptodate.com. Accessed Sept. 20, 2016.
- Kim JS. Food allergy: Diagnosis, treatment, prognosis, and prevention. Pediatr Ann 2008;37:546-551.
- Sampson HA. Food-induced anaphylaxis. Sicherer SH, Kelso JM, Feldweg AM, eds. UpToDate Available at: www.uptodate.com. Accessed Sept. 29, 2016.
- Umasunthar T, Leonardi-Bee J, Turner PJ, et al. Incidence of fatal food anaphylaxis in people with food allergy: A systematic review and meta-analysis. Clin Exp Allergy 2015;45:1621-1636.
- Burks W. Clinical manifestations of food allergy: An overview. Sicherer SH, TePas E, eds. UpToDate Available at: www.uptodate.com. Accessed Sept. 20, 2016.
- Sharma HP, Bansil S, Uygungil B. Signs and symptoms of food allergy and food-induced anaphylaxis. Pediatr Clin North Am 2015;62:1377-1392.
- Simons FE. Anaphylaxis. J Allergy Clin Immunol 2008;121(2 Suppl 2):S402-S407.
- Sampson HA, Aceves S, Bock SA, et al. Food allergy: A practice parameter update-2014. J Allergy Clin Immunol 2014;134:1016-1025.e43.
- Fishbein AB, Makhija MM, Pongracic JA. Anaphylaxis to food. Immunol Allergy Clin North Am 2015;35:231-245.
- Burks AW. Peanut allergy. Lancet 2008;371:1538-1546.
- Al-Muhsen S, Clarke AE, Kagan RS. Peanut allergy: An overview. CMAJ 2003;168:1279-1285.
- Pansare M, Kamat D. Peanut allergies in children — a review. Clin Pediatr 2009;48:709-714.
- Lieberman P, Nicklas RA, Oppenheimer J, et al. The diagnosis and management of anaphylaxis practice parameter – 2010 update. J Allergy Clin Immunol 2010;126:477-480.e42.
- Simons FE. Anaphylaxis. J Allergy Clin Immunol 2010;125(2 Suppl):S161-S181.
- Simons FE, Ardusso LR, Bilo MB, et al. World Allergy Organization anaphylaxis guidelines: Summary. J Allergy Clin Immunol 2011;127:587-593.
- Feldweg AM. Exercise-induced anaphylaxis. Immunol Allergy Clin North Am 2015;35:261-275.
- Kurowski K, Boxer RW. Food allergies: Detection and management. Am Fam Physician 2008;77:1678-1686.
- Sharma HP, Mansoor DK, Mikhail IJ, et al. Recognition and management of pediatric food allergy in the emergency department. Pediatr Emerg Care 2013;29:527-536.
- Bock SA, Muñoz-Furlong A, Sampson HA. Fatalities due to anaphylactic reactions to foods. J Allergy Clin Immunol 2007;119:1016-1019.
- Shah E, Pongracic J. Food-induced anaphylaxis: Who, what, why, and where? Pediatr Ann 2008;37:536-541.
- Cheng J. Anaphylaxis: The underrecognized killer. Pediatr Emerg Med Reports 2017;22:93-108.
- Wolfe JL, Aceves SS. Gastrointestinal manifestations of food allergies. Pediatr Clin North Am 2011;58:389-405.
- Maloney J, Nowak-Wegrzyn A. Educational clinical case series for pediatric allergy and immunology: Allergic proctocolitis, food protein-induced enterocolitis syndrome and allergic eosinophilic gastroenteritis with protein-losing gastroenteropathy as manifestations of non-IgE-mediated cow’s milk allergy. Pediatr Allergy Immunol 2007;18:360-367.
- Bone J, Claver A, Guallar I, Plaza AM. Allergic proctocolitis, food-induced enterocolitis: Immune mechanisms, diagnosis, and treatment. Allergol Immunopathol (Madr) 2009;37:36-42.
- Mansoor DK, Sharma HP. Clinical presentations of food allergy. Pediatr Clin North Am 2011;58:315-326.
- Järvinen KM, Nowak-Wegrzyn A. Food protein-induced enterocolitis syndrome (FPIES): Current management strategies and review of the literature. J Allergy Clin Immunol Pract 2013;1:317-322.
- Mehr S, Firth K, Campbell DE. Epidemiology of food protein-induced enterocolitis syndrome. Curr Opin Allergy Clin Immunol 2014;14:208-216.
- Feuille E, Nowak-Wegrzyn A. Definition, etiology, and diagnosis of food protein-induced enterocolitis syndrome. Curr Opin Allergy Clin Immunol 2014;14:222-228.
- Guibas GV, Tsabouri S, Makris M, Priftis KN. Food protein-induced enterocolitis syndrome: Pitfalls in the diagnosis. Pediatr Allergy Immunol 2014;25:622-629.
- Leonard SA, Nowak-Wegrzyn A. Clinical diagnosis and management of food protein-induced enterocolitis syndrome. Curr Opin Pediatr 2012;24:739-745.
- Leonard SA, Nowak-Wegrzyn A. Manifestations, diagnosis, and management of food protein-induced enterocolitis syndrome. Pediatr Ann 2013;42:135-140.
- Miceli Sopo S, Dello Iacono I, Greco M, Monti G. Clinical management of food protein-induced enterocolitis syndrome. Curr Opin Allergy Clin Immunol 2014;14:240-245.
- Nowak-Wegrzyn A, Katz Y, Mehr SS, Koletzko S. Non-IgE-mediated gastrointestinal food allergy. J Allergy Clin Immunol 2015;135:1114-1124.
- Golden DBK. Chapter 78: Insect Allergy. In: Adkinson NF Jr, Bochner BS, Burks AW, et al, eds. Middleton’s Allergy: Principles and Practice. 8th ed. Volume 2. Philadelphia: Elsevier Saunders; 2014: 1260-1273.
- Golden DB. Insect sting anaphylaxis. Immunol Allergy Clin North Am 2007;27:261-272.
- Golden DB. Anaphylaxis to insect stings. Immunol Allergy Clin North Am 2015;35:287-302.
- Shaker MS, Hsu D, Gurenberg DA. An update on venom allergy. Curr Opin Pediatr 2013;25:629-634.
- Sampson HA, Leung DYM. Chapter 148: Anaphylaxis. In: Kliegman RM, RE Behrman, HB Jenson, BF Stanton, eds. Nelson Textbook of Pediatrics. 18th ed. Philadelphia: Saunders Elesevier; 2007: 983-985.
- Hodge III D. Chapter 83: Bites and Stings. In: Fleisher GR, Ludwig S, eds. Textbook of Pediatric Emergency Medicine. 6th ed. Philadelphia: Lippincott Williams & Wilkins; 2010: 671-689.
- Golden DB. Stinging insect allergy. Am Fam Physician 2003;67:2541-2546.
- Betten DP, Richardson WH, Tong TC, Clark RF. Massive honey bee envenomation-induced rhabdomyolysis in an adolescent. Pediatrics 2006;117:231-235.
- Freeman T. Bee, yellow jacket, wasp, and other Hymenoptera stings: Reaction types and acute management. Golden DB, Feldweg AM, eds. UpToDate Available at: www.uptodate.com. Accessed Oct. 21, 2016.
- Bilo MB, Bonifazi F. The natural history and epidemiology of insect venom allergy: Clinical implications. Clin Exp Allergy 2009;39:1467-1476.
- Tan JW, Campbell DE. Insect allergy in children. J Paediatr Child Health 2013;49:E381-E387.
- Reisman RE. Unusual reactions to insect stings. Curr Opin Allergy Clin Immunol 2005;5:355-358.
- Reisman RE. Natural history of insect sting allergy: Relationship of severity of symptoms of initial sting anaphylaxis to re-sting reactions. J Allergy Clin Immunol 1992;90:335-339.
- Severino M, Bonadonna P, Passalacqua G. Large local reactions from stinging insects: From epidemiology to management. Curr Opin Allergy Clin Immunol 2009;9:334-337.
- Abonia JP, Castells M. Drug allergy in pediatric patients. Pediatr Ann 2011;40:200-204.
- Boguniewicz, Leung DYM. Chapter 151: Adverse Reactions to Drugs. In: Kliegman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. 18th ed. Philadelphia: Elesevier Saunders; 2007:990-993.
- Celik GE, Pichler WJ, Adkinson NF. Chapter 79: Drug Allergy. In: Adkinson NF Jr, Bochner BS, Burks AW, et al, eds. Middleton’s Allergy: Principles and Practice. 8th ed. Volume 2. Philadelphia: Elsevier Saunders; 2014: 1274-1295.
- Noguera-Morel L, Hernandez-Martin A, Torrelo A. Cutaneous drug reactions in the pediatric population. Pediatr Clin North Am 2014;61:403-426.
- Segal AR, Doherty KM, Leggott J, Zlotoff B. Cutaneous reactions to drugs in children. Pediatrics 2007;120:e1082-e1096.
- Pichichero ME. A review of evidence supporting the American Academy of Pediatrics recommendation for prescribing cephalosporin antibiotics for penicillin-allergic patients. Pediatrics 2005;115:1048-1057.
- Kelso JM. Potential food allergens in medications. J Allergy Clin Immunol 2014;133:1509-1518.
- Babl FE, Lewena S, Brown L. Vaccination-related adverse events. Pediatr Emerg Care 2006;22:514-519.
- Bohlke K, Davis RL, Marcy SM, et al. Risk of anaphylaxis after vaccination of children and adolescents. Pediatrics 2003;112:815-820.
- Stone KD. Advances in pediatric allergy. Curr Opin Pediatr 2004;16:571-578.
- Sicherer SH, Leung DYM. Chapter 149: Serum Sickness. In: Kliegman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. 18th ed. Philadelphia: Saunders Elsevier; 2007: 985-986.
- Wener MH. Serum sickness and serum sickness-like reactions. Adkinson NF, Feldweg AM, eds. UpToDate Available at: www.uptodate.com. Accessed Oct. 18, 2016.
- Frank MM, Hester CG. Chapter 38: Immune Complex-Mediated Diseases. In: Adkinson NF Jr, Bochner BS, Burks AW, et al, eds. Middleton’s Allergy: Principles and Practice. 8th ed. Volume 1. Philadelphia: Elsevier Saunders; 2014: 602-617.
- Mathur AN, Mathes EF. Urticaria mimickers in children. Dermatol Ther 2013;26:467-475.
- Roujeau JC. Stevens-Johnson syndrome and toxic epidermal necrolysis are severity variants of the same disease which differs from erythema multiforme. J Dermatol 1997;24:726-729.
- Creamer D, Walsh SA, Dziewulski P, et al. U.K. guidelines for the management of Stevens-Johnson syndrome/toxic epidermal necrolysis in adults 2016. Br J Dermatol 2016;174:1194-1227.
- Del Pozzo-Magana BR, Lazo-Langner A, Carleton B, et al. A systematic review of treatment of drug-induced Stevens-Johnson Syndrome and toxic epidermal necrolysis in children. J Popul Ther Clin Pharmacol 2011;18:e121-e133.
- Nirken MH, High WA, Roujeau JC. Stevens-Johnson syndrome and toxic epidermal necrolysis: Pathogenesis, clinical manifestations, and diagnosis. Adkinson NF Jr, Levy ML, Corona R, eds. UpToDate. Available at: www.uptodate.com. Accessed March 17, 2017.
- Belver MT, Michavila A, Bobolea I, et al. Severe delayed skin reactions related to drugs in the paediatrics age group: A review of the subject by way of three cases (Stevens-Johnson syndrome, toxic epidermal necrolysis and DRESS). Allergol Immunopathol (Madr) 2016;44:83-95.
- Ferrandiz-Pulido C, Garcia-Patos V. A review of causes of Stevens-Johnson syndrome and toxic epidermal necrolysis in children. Arch Dis Child 2013;98:998-1003.
- Goyal S, Gupta P, Ryan CM, et al. Toxic epidermal necrolysis in children: Medical, surgical, and ophthalmologic considerations. J Burn Care Res 2009;30:437-449.
- Schwartz RA, McDonough PH, Lee BW. Toxic epidermal necrolysis: Part I. Introduction, history, classification, clinical features, systemic manifestations, etiology, and immunopathogenesis. J Am Acad Dermatol 2013;69:173.e1-13.
- Cohen BA, Davis HW, Gehris RP. Chapter 8: Dermatology. In: Zitelli BJ, Davis HW, eds. Atlas of Pediatric Physical Diagnosis. 5th ed. Philadelphia: Mosby Elsevier; 2007: 275-346.
- High WA, Nirken MH, Roujeau JC. Stevens-Johnson syndrome and toxic epidermal necrolysis: Management, prognosis, and long-term sequelae. Adkinson NF Jr, Levy ML, Mockenhaupt M, Corona R, eds. UpToDate. Available at: www.uptodate.com. Accessed March 17, 2017.
- Schwartz RA, McDonough PH, Lee BW. Toxic epidermal necrolysis: Part II. Prognosis, sequelae, diagnosis, differential diagnosis, prevention, and treatment. J Am Acad Dermatol 2013;69:187.e1-e16.
- Sheridan RL, Schulz JT, Ryan CM, et al. Long-term consequences of toxic epidermal necrolysis in children. Pediatrics 2002;109:74-78.
- Hausmann O. Chapter 9: Drug Allergy. In O’Hehir RE, Sheikh A, Holgate ST, eds. Middleton’s Allergy Essentials. China: Elsevier; 2017: 225-247.
- Koh MJ, Tay YK. An update on Stevens-Johnson Syndrome and toxic epidermal necrolysis in children. Curr Opin Pediatr 2009;21:505-510.
- Levi N, Basuji-Garin S, Mockenhaupt M, et al. Medications as risk factors of Stevens-Johnson syndrome and toxic epidermal necrolysis in children: A pooled analysis. Pediatrics 2009;123:e297-e304.
- Morelli JG. Chapter 653: Vesiculobullous Disorders. In: Kleigman RM, Behrman RE, Jenson HB, Stanton BF, eds. Nelson Textbook of Pediatrics. 18th ed. Philadelphia: Saunders Elsevier; 2007: 2685-2693.
- Heng YK, Lee HY, Roujeau JC. Epidermal necrolysis: 60 years of errors and advances. Br J Dermatol 2015;173;1250-1254.
- Fritsch PO, Sidoroff A. Drug-induced Stevens-Johnson syndrome/toxic epidermal necrolysis. Am J Clin Dermatol 2000;1:349-360.
- Quirke KP, Beck A, Gamelli RL, Mosier MJ. A 15-year review of pediatric toxic epidermal necrolysis. J Burn Care Res 2015;36:130-136.
- Rizzo JA, Johnson R, Cartie RJ. Pediatric toxic epidermal necrolysis: Experience of a tertiary burn center. Pediatr Dermatol 2015;32:704-709.
- Mayes T, Gottschlich M, Khoury J, et al. Energy requirements of pediatric patients with Stevens-Johnson syndrome and toxic epidermal necrolysis. Nutr Clin Pract 2008;23:547-550.
- McCullough M, Burg M, Lin E, et al. Steven Johnson syndrome and toxic epidermal necrolysis in a burn unit: A 15-year experience. Burns 2017;43:200-205.
- Shiga S, Cartotto R. What are the fluid requirements in toxic epidermal necrolysis? J Burn Care Res 2010;31:100-104.
- Corrick F, Anand G. Question2: Would systemic steroids be useful in the management of Stevens-Johnson syndrome? Arch Dis Child 2013;98:828-830.
- Liu W, Nie X, Zhang L. A retrospective analysis of Stevens-Johnson syndrome/toxic epidermal necrolysis treated with corticosteroids. Int J Dermatol 2016;55:1408-1413.
- Techasatian L, Panombualert S, Uppala R, Jetsrisuparb C. Drug-induced Stevens-Johnson syndrome and toxic epidermal necrolysis in children: 20 year study in a tertiary care hospital. World J Pediatr 2017;13:255-260.
- Barron SJ, Del Vecchio MT, Aronoff SC. Intravenous immunoglobulin in the treatment of Stevens-Johnson syndrome and toxic epidermal necrolysis: A meta-analysis with meta-regression of observational studies. Int J Dermatol 2015;54:108-115.
- Huang YC, Li YC, Chen TJ. The efficacy of intravenous immunoglobulin for the treatment of toxic epidermal necrolysis: A systematic review and meta-analysis. Br J Dermatol 2012;167:424-432.
- Romero-Tapia SJ, Camara-Combaluzier HH, Baez-Bacab MA, et al. Use of intravenous immunoglobulin for Stevens-Johnson syndrome and toxic epidermal necrolysis in children: Reported of two cases secondary to anticonvulsants. Allergol Immunopathol (Madr) 2015;43:227-229.
- Tristani-Firouzi P, Petersen MJ, Saffle JR, et al. Treatment of toxic epidermal necrolysis with intravenous immunoglobulin in children. J Am Acad Dermatol 2002;47:548-552.
- Finkelstein Y, Soon GS, Acuna P, et al. Recurrence and outcomes of Stevens-Johnson syndrome and toxic epidermal necrolysis in children. Pediatrics 2011;128:723-728.
- Kirchhof MG, Miliszewsin MA, Sikora S, et al. Retrospective review of Stevens-Johnson syndrome/toxic epidermal necrolysis treatment comparing intravenous immunoglobulin with cyclosporine.J Am Acad Dermatol 2014;71:941-947.
- Lee HY, Fook-Chong S, Koh HY, et al. Cyclosporine treatment for Stevens-Johnson syndrome/toxic epidermal necrolysis: Retrospective analysis of a cohort treated in a specialized referral center. J Am Acad Dermatol 2017;76:106-113.
- Roujeau JC. Drug reaction with eosinophilia and systemic symptoms. In: Mockenhaupt M,Corona R, eds. UpToDate. Available at: www.uptodate.com. Accessed March 14, 2017.
- Kardaun SH, Sekula P, Valeyrie-Allanore L, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): An original multisystem adverse drug reaction. Results from the prospective RegiSCAR study. Br J Dermatol 2013;169:1071-1080.
- Husain Z, Reddy BY, Schwartz RA. DRESS syndrome: Part I. Clinical perspectives. J Am Acad Dermatol 2013;68:693.e1-14.
- Newell BD, Horii KA. Cutaneous drug reactions in children. Pediatr Ann 2010;39:618-625.
- Husain Z, Reddy BY, Schwartz RA. DRESS syndrome: Part II. Management and therapeutics. J Am Acad Dermatol 2013;68:709.e1-9.
Hypersensitivity reactions are very common. Understanding the different types, including serum sickness-like reactions, Stevens-Johnson syndrome, toxic epidermolytic necrolysis, and drug reaction with eosinophilia and systemic symptoms, is valuable both for an accurate and timely diagnosis as well as appropriate management.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
