Tachycardia
November 1, 2017
Reprints
AUTHORS
Jason V. Brown, MD, Staff Physician, Emergency Services, 96th Medical Group, Eglin Air Force Base, Florida
Anne Walker, MD, Senior Resident, University of Maryland Medical Center, Baltimore
PEER REVIEWER
William J. Brady, MD, FACEP, FAAEM, Professor of Emergency Medicine, University of Virginia School of Medicine, Charlottesville
EXECUTIVE SUMMARY
- In unstable patients, tachycardias are best treated with synchronized electrical cardioversion to prevent deterioration into cardiac arrest.
- Multifocal atrial tachycardia is seen most often in chronic obstructive pulmonary disease exacerbations and is managed by treating the underlying condition.
- In stable patients, atrial fibrillation with rapid ventricular response is treated first with rate-control agents using calcium channel blockers or beta-blockers.
- In stable patients with ventricular tachycardia, procainamide is the most effective antiarrhythmic agent.
- Electrical defibrillation is used to treat cardiac arrest patients who are in ventricular tachycardia.
- Intravenous magnesium is used to treat and prevent episodes of torsades de pointes arrhythmias.
The recognition, diagnosis, and treatment of tachycardia is a cornerstone of emergency medicine practice. All patients presenting to the emergency department (ED) will have vital signs taken, and every chart showing an elevated heart rate requires an investigation into its cause. Tachycardia is defined as any heart rate greater than 100 beats per minute (bpm) in an adult. It can be a normal response to physiologic or external stressors (i.e., dehydration or pain) or a pathologic occurrence that requires emergent care. Because of the wide range of presentations and causes, a mastery of the diagnosis and treatment of tachycardia should be considered a core competency within the field of emergency medicine.
This article will cover the most commonly seen supraventricular and ventricular tachycardias encountered in the ED, with a focus on their electrocardiographic (ECG) diagnoses and treatment options. Supraventricular tachycardias (SVT) are broadly divided into six major categories: sinus tachycardia (ST), atrial fibrillation (AF), atrial flutter (AFL), multifocal atrial tachycardia (MAT), atrioventricular reentrant tachycardia (AVRT), and atrioventricular nodal reentrant tachycardia (AVNRT). Ventricular tachycardias primarily consist of ventricular tachycardia (VT), which can be classified further as either monomorphic or polymorphic.
Supraventricular Tachycardias
Tachyarrhythmias originating from the atria include ST, MAT, AF, AFL, and SVT. They can be classified further by whether they create a rhythm that is regular or irregular. (See Table 1.)
Table 1. Supraventricular Tachycardia Classification
Regular Rhythm |
Irregular Rhythm |
|
Additionally, any regular rhythm, when affected by a variable block, turns into an irregular rhythm. |
|
|
Sinus tachycardia |
Atrial fibrillation |
|
Atrial tachycardia |
Multifocal atrial tachycardia |
|
Atrial flutter |
Atrial flutter with variable conduction |
|
Atrioventricular reentrant tachycardia |
Sinus tachycardia with multiple premature atrial complexes |
|
Atrioventricular nodal reentrant tachycardia |
|
Sinus Tachycardia
ST generally is a result of an extrinsic cause, such as exercise, catecholamine surge, fever, stress, dehydration, or iatrogenic due to certain pharmacotherapies. Treatments are tailored to the underlying cause and can include oxygen, pain control, intravenous (IV) fluids, anxiolytics, and antipyretics. If a sinus tachycardia does not resolve with these measures, further investigation of an alternative cause should be pursued.
ST is recognized on ECG as a regular, rapid rhythm. As in normal sinus rhythm (NSR), there should be a P wave before every QRS complex, and a QRS complex should follow every P wave. P waves should be upright in leads I and II and inverted in lead aVR. Because emergency physicians are very familiar with sinus tachycardia, this topic will not be covered in greater detail in this article.
Multifocal Atrial Tachycardia
MAT, also referred to as ectopic atrial tachycardia,1 is caused by a variety of ectopic electrical outputs occurring within the atria. (See Figure 1.) The diagnosis is based on ECG identification of:
1) heart rate > 100 bpm;
2) irregularly irregular rhythm with varying PR and RR intervals; and
3) at least three different P wave morphologies in a single lead.
To diagnose MAT, examine a single lead in its entirety to evaluate for differing P wave morphologies. It is important to remember that it can be normal for P wave morphology to differ between leads.1
MAT is seen almost exclusively in patients with a diagnosis of chronic obstructive pulmonary disease (COPD). Often MAT can be triggered by an exacerbation of the disease.2 In hospitalized COPD patients, MAT is considered an ominous sign, particularly when the patient is on mechanical ventilation.2
MAT also can be found in the outpatient setting among patients who are asymptomatic. When not associated with an acute illness, MAT does not share the same bleak prognosis as it does in the patient one might see in respiratory distress in the ED.3
Figure 1. Multifocal Atrial Tachycardia
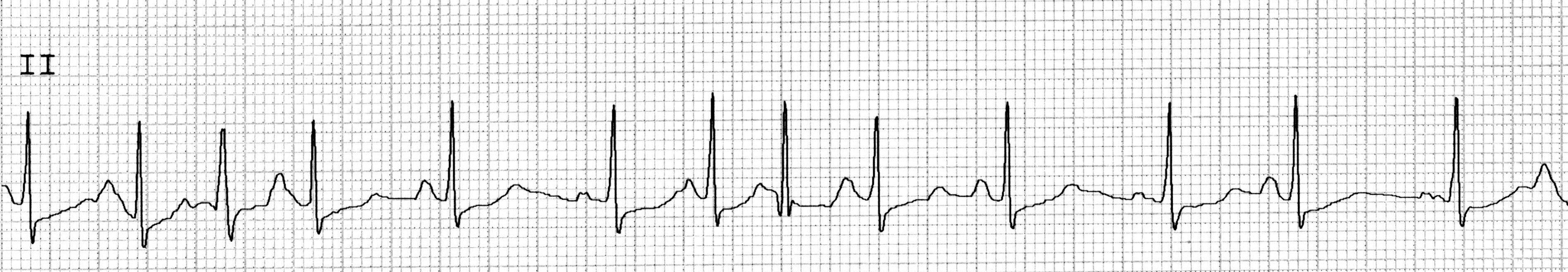
Lead II, P waves with at least three different morphologies
Image courtesy of J. Stephan Stapczynski, MD
MAT is seen most often in adults and occasionally in children.4,5 MAT is even less common in infants, comprising less than 1% of all SVT in this age group.5 In pediatric patients, consider drug toxicities as the most likely cause instead of chronic lung disease. There are case reports of MAT being caused by epinephrine4 and antipsychotics, such as risperidone.5,6 The long-term prognosis will vary based on the underlying cause, and MAT usually will terminate without intervention when due to medication overdose.4,5,6
MAT can be thought of as a sign of stress to the heart. Unlike other arrhythmias, it is not thought to originate from an intrinsic electrical problem; therefore, the treatment approach is to address the underlying cause rather than the tachyarrhythmia itself. If the tachycardia causes clinically significant symptoms or the rhythm is persistent, then β1-blockers or calcium channel blockers are considered a reasonable first-line treatment. Other options include magnesium and digoxin. AV junction-altering medications generally are used to control the ventricular rate and decrease symptoms in patients in whom treating the underlying cause is not feasible or effective.2
Atrial Fibrillation and Atrial Flutter
AF and AFL, although different in mechanism, overlap in management and will be discussed together.
AF is the most common sustained tachyarrhythmia seen in the ED. It is a supraventricular tachycardia with chaotic activation of the atria, resulting in contractional dyscoordination and ineffective contribution of the atria to cardiac output.7 During AF, cardiac output typically decreases by 20% to 30%.8
There is significant morbidity and mortality related to AF that, if undermanaged, can affect the patient’s quality of life. The most common presenting symptom is fatigue; however, patients also may complain of lightheadedness, palpitations, shortness of breath, or chest pain. AF is most often a disease seen in the elderly. Of those with atrial fibrillation, about 2% are 40 to 60 years of age, about 6% are between 60 and 65 years, about 70% are between 65 and 85 years of age, and about 22% are older than 85 years of age. AF often is associated with structural heart disease, including both ischemic and non-ischemic cardiomyopathy.7
An important clinical concern is the stroke risk associated with untreated or undertreated AF. A person with AF has five times the risk of stroke as a person without AF, with this risk compounding with age. A patient with a valvular AF has an even greater risk, estimated to be up to 20 times that of those without AF.7
There is a dearth of literature regarding the safe disposition of atrial fibrillation patients who present to the ED. A general rule is that patients with significant comorbidities should be admitted for both management of their AF and optimization of their underlying pathologies. Low-risk patients are those who do not have significant vital sign abnormalities or confounding comorbidities, and who have the capability to arrange follow-up in the next two to three days. These patients may be appropriate for discharge.11 Ideally, patients should receive a cardiology consultation prior to discharge. In situations in which this is not possible, following a pre-established protocol with a mechanism to ensure follow-up in two to three days is a reasonable alternative.
After an irregular rhythm is noted on exam, the diagnosis of AF ultimately is made with a 12-lead ECG.12 On ECG, look for the following: 1) the absence of discernable P waves; 2) an irregular RR interval when there is AV conduction; 3) absence of an isoelectric baseline; and 4) irregular atrial activation. (See Figures 2A and 2B.) These patients always have an irregularly irregular rhythm. Although MAT also may present with an irregularly irregular rhythm, the lack of P waves in AF is diagnostic.
Figure 2A. Atrial Fibrillation
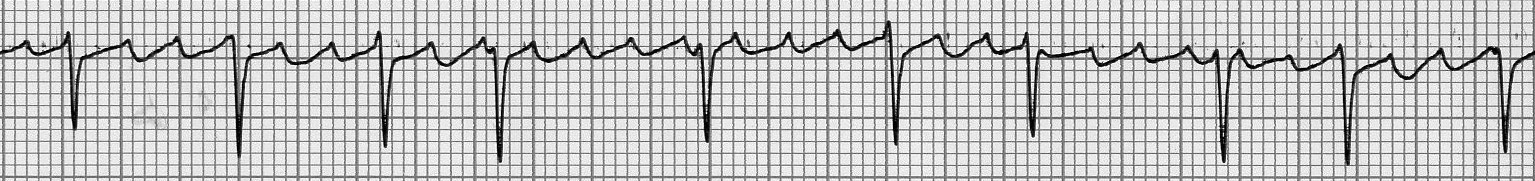
Lead V1, atrial fibrillatory waves at rate > 300 bpm
Image courtesy of J. Stephan Stapczynski, MD
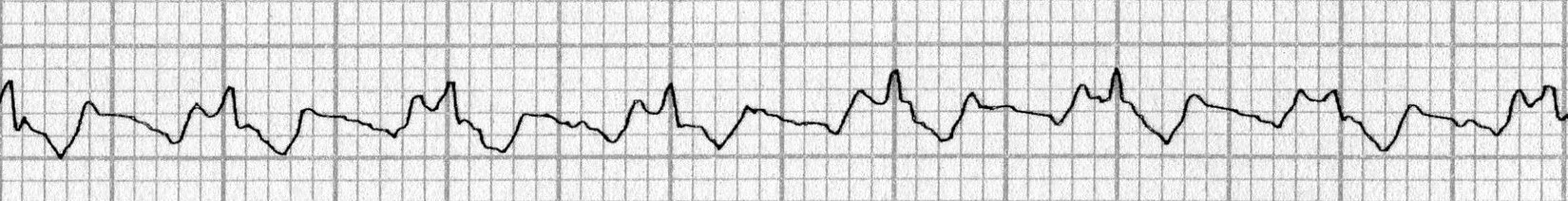
Figure 2B. Atrial Fibrillation
Lead II, no consistent P waves and irregular ventricular response
Image courtesy of J. Stephan Stapczynski, MD
As opposed to AF, AFL is an SVT with rapid regular atrial contraction. This increased rate of the atria compared to the ventricles decreases the cardiac output, as with AF. The prognosis of AFL is associated with how variable the conduction of the impulses is through the AV node and how quickly the ventricles are contracting.
The mechanism of AFL involves a reentrant circuit that encompasses the right atrium and is fairly predictable in terms of atrial rates, with a typical rate of 300 bpm but ranging from 200 to 400 bpm. The ventricular rate is determined by the degree of AV block. For example, a 4:1 block has a ventricular rate of 75 bpm; for 3:1, 100 bpm; and for 2:1, 150 bpm.
In AFL, the ECG shows a narrow complex tachycardia with loss of the isoelectric baseline; however, P waves should be evident and show regular atrial activity with a rate of approximately 300 bpm. (See Figure 3A.) Classically, flutter waves are seen and described as creating a “saw tooth” pattern. The best leads in which to visualize this pattern are II, III, and aVF. Flutter waves are oriented negatively in these inferior leads, so it can be helpful to flip the ECG paper upside down to better evaluate each lead for this pattern. AFL with a 1:1 block presents a more difficult challenge on ECG, as there may be no discernable flutter waves. In this case, transiently inducing AV block with vagal maneuvers or IV adenosine may unmask the arrhythmia. (See Figure 3B.)
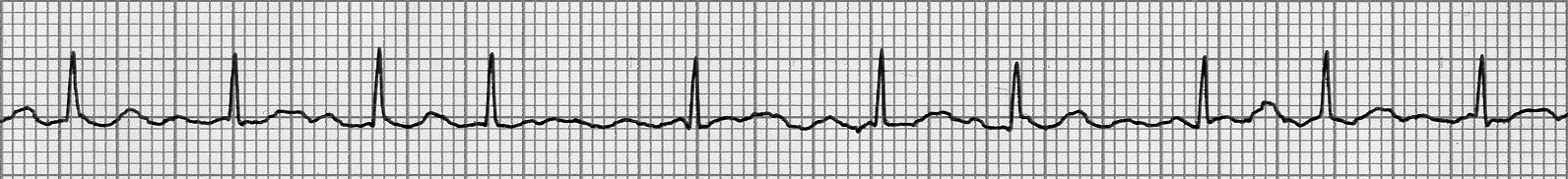
Figure 3A. Atrial Flutter
Lead II, inferiorly directed “saw-tooth” atrial flutter waves at rate about 300 bpm with 2:1 AV block and ventricular rate of 150 bpm
Image courtesy of J. Stephan Stapczynski, MD
Figure 3B. Atrial Flutter
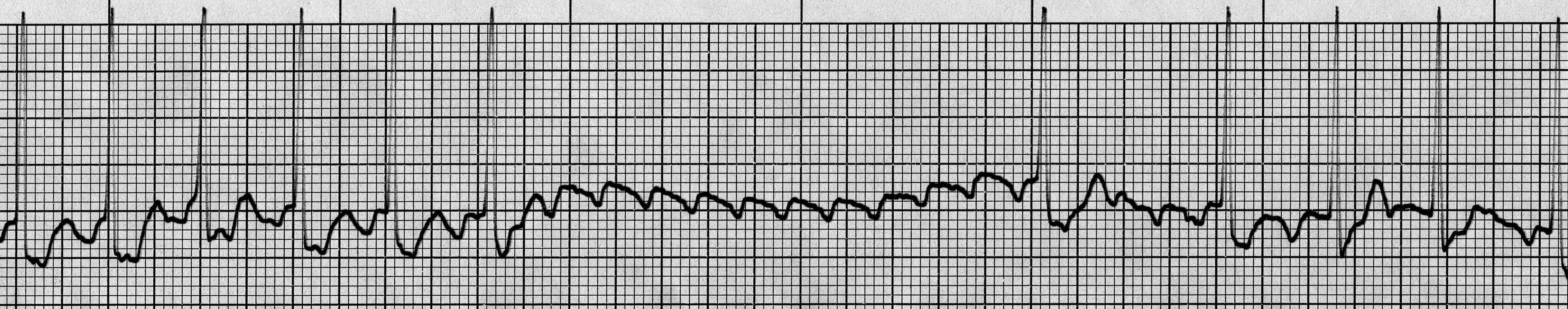
Lead II, transient AV block induced by carotid sinus massage allowing visualization of atrial flutter waves at rate of 300 bpm
Image courtesy of J. Stephan Stapczynski, MD
Management of AF/AFL can be considered in five different, distinct categories: 1) acute stabilization; 2) treatment of the underlying condition; 3) stroke prevention; 4) rate control; and 5) rhythm control.13 As with all patients, treatments for those with AF/AFL can be emergent, urgent, or routine.
Acutely, the first task is to assess the patient’s hemodynamic stability. The presence of hypotension, precipitously declining blood pressure, chest pain, shortness of breath, or altered mental status defines a patient as unstable.
Emergent
Consider a patient with lightheadedness and shortness of breath in AF/AFL at a heart rate in the 150s and a blood pressure of 60/40 mmHg. First, quickly consider if the unstable tachyarrhythmia is secondary to another treatable cause, such as sepsis or dehydration, if these are the most likely diagnoses, then treat the underlying cause.
If the etiology is not obvious or is considered cardiac in origin, then pharmacologic therapy should be skipped in preference for electrical cardioversion. Direct current (DC) cardioversion is performed by the delivery of an electric shock starting at 100 J with the defibrillator after placing it in “synchronized” mode and ensuring that the shock is synchronized with the peak of the QRS complex. Biphasic shocks are more effective than monophasic shocks, and the anteroposterior positioning of the pads is superior to the anterolateral positioning. If cardioversion is unsuccessful initially, it is reasonable to administer an antiarrhythmic medication and attempt cardioversion again, as the dual action of these therapies can increase the efficacy of the subsequent shock.7 The role of cardioversion in the ED is primarily for unstable patients to prevent total hemodynamic collapse.
Routine
Stable patients, regardless of heart rate, require a more nuanced approach to management. Cardioversion is not the first-line treatment, and pharmacologic agents are preferred. Pharmacologic strategies are divided into either rate or rhythm control depending on the length of time the patient has been in AF/AFL.
Urgent
The symptomatic patient in AF/AFL who has a stable blood pressure still requires urgent attention to prevent decompensation. As in emergent cases, first consider the etiology and treat the underlying condition appropriately. Treat any fever if present, give IV fluids for dehydration, administer blood products for significant anemia, and administer broad-spectrum antibiotics for sepsis. However, if the etiology is cardiogenic in nature, then pharmacologic rate control becomes the initial strategy of choice. Options for rate control include beta-blockers, non-dihydropyridine calcium channel blockers, digoxin, or, in resistant cases, amiodarone.
The therapeutic goals for ventricular rate control generally are < 80 bpm at rest and < 110 bpm with exertion, but there is a more lenient goal of < 110 bpm used in acute ED management.12 This is based on the findings that lower ventricular rates, particularly < 70 bpm, may be associated with worse outcomes in AF.7
The use of beta-blockers vs. calcium channel blockers for acute rate control of AF has been a matter of debate in recent years. Current literature suggests that diltiazem is the most effective, if only slightly. In a cohort study, Harvey et al retrospectively studied diltiazem vs. esmolol for rate control in the ED and found that 53% of patients achieved rate control to < 100 bpm in less than 30 minutes when treated with diltiazem, compared to only 43% of those treated with esmolol. After 60 minutes, 76% of those treated with diltiazem were rate controlled, compared to 50% with esmolol.14
Fromm et al conducted an additional prospective study evaluating diltiazem vs. metoprolol using a convenience sample and found that after 10 minutes and 30 minutes, 50% and 95% of those treated with diltiazem reached a goal heart rate of < 100 bpm, compared to only 11% and 46% of those treated with metoprolol. There was no difference in the number of adverse outcomes, including episodes of bradycardia and hypotension, between the two groups.15
However, the use of beta-blockers can be beneficial, especially if the patient has a history of heart failure with a reduced ejection fraction (HFrEF). In patients with HFrEF, beta-blockers are recommended for daily maintenance therapy. A large, randomized, controlled trial showed decreased mortality in patients with HFrEF treated with a beta-blocker; however, those findings cannot be extrapolated to patients being treated with AF in the ED.15
Digoxin, a cardiac glycoside AV nodal blocker, is considered the least effective rate-control agent overall, but can be a reasonable choice for the physically inactive patient > 80 years old who has failed other treatment options.16 Digoxin is administered as a 0.5 mg IV bolus, followed by 0.75-1.5 mg over 24 hours in divided doses. Rate control generally takes more than an hour, and the peak effect occurs in six hours. A major drawback is that digoxin is ineffective at maintaining heart rate < 110 bpm during exertion.
While acute stabilization is the primary focus in the ED, treatment and management of underlying conditions and/or sequelae should not be overlooked. If the etiology of the arrhythmia is primarily cardiac, this may involve optimizing diuretics, or obtaining an echocardiogram to evaluate for heart failure or valvular abnormalities in a new diagnosis of AF.17 Cardiac troponin (cTn) measurement is not necessary in the evaluation of every patient who comes to the ED with AF; however, if the patient has symptoms concerning for a recent myocardial ischemic event, then cTn may be warranted. Brain natriuretic peptide (BNP) also can be useful, although levels may be increased in patients with AF even without any heart failure present. When trended, these levels rapidly decrease after restoration of sinus rhythm. In a patient without signs of new heart failure, the expense of the BNP test may outweigh its clinical usefulness.
There also should be a focus on optimization of the patients’ comorbidities. In the LEGACY study, a five-year follow-up of patients with AF and body mass index (BMI) > 27 kg/m2, long-term weight loss was associated with higher maintenance of sinus rhythm. Researchers found that the more weight a patient lost, the more likely the patient was to remain in sinus rhythm.18 Other risk factors that should be addressed are control of hyperglycemia and hypertension by counseling on diet, exercise, and moderation of alcohol consumption.17
After the AF/AFL patient has been stabilized, determine the duration of the arrhythmia. Has it been definitively less than 48 hours? The answer to this question affects the patient’s need for anticoagulation therapy prior to cardioversion, whether it be pharmacologic or electrical. It also influences the need for anticoagulation prior to discharge from the ED. In general, a patient who requires anticoagulation due to prolonged AF greater than 48 hours should be treated for at least three weeks prior to initiation of rhythm control techniques. Exceptions to this rule are in emergent cardioversions for hemodynamic instability or if an atrial thrombus has been ruled out in the ED with transesophageal echocardiogram (TEE).
The reason for starting patients on anticoagulation is to mitigate future stroke risk by preventing thrombus formation in the left atrium. It is considered standard of care to use CHA2DS2-VASc and HAS-BLED as scoring tools to decide if anticoagulation therapy is appropriate. CHA2DS2-VASc estimates the stroke risk in a patient with AF, and HAS-BLED estimates the risk of bleeding on anticoagulation.19,20,21 (See Table 2.) It is important to note that CHA2DS2-VASc does not apply if the patient’s AF is due to a valvular etiology.
Table 2. CHA2DS2-VASc and HAS-BLED Scoring Systems
CHA 2 DS 2 -VASc |
HAS-BLED |
||
|
Congestive heart failure |
1 |
Hypertension |
1 |
|
Hypertension |
1 |
Abnormal renal function |
1 |
|
Age ≥ 75 years |
2 |
Abnormal liver function (cirrhosis or bilirubin > 2x normal with AST/ALT/AP |
1 |
|
Age 65-74 years |
1 |
Stroke |
1 |
|
Diabetes mellitus |
1 |
Bleeding tendency/predisposition |
1 |
|
Stroke/transient ischemic attack/thromboembolism |
2 |
Labile INRs (if on warfarin) — time in therapeutic range < 60% |
1 |
|
Vascular disease |
1 |
Elderly (age > 65 years) |
1 |
|
Sex (female) |
1 |
Drugs/alcohol |
1 each |
|
Total Possible |
9 |
Total Possible |
9 |
If the CHA2DS2-VASc score is 0, then the patient requires no anticoagulation upon discharge. If the score is 2 or greater, anticoagulation is indicated. With a score of 1, proper treatment is still debated. In Europe, a score of 1 would be treated with anticoagulation; however, in the United States, algorithms give the physician the option to decide to treat these patients with aspirin (ASA) only or not to treat at all.
The HAS-BLED score is used to determine the risk of bleeding prior to giving any anticoagulation treatment. These two scoring systems must be weighed against each other to determine whether to start anticoagulation. Interestingly, few studies have found any benefit in using ASA alone to prevent CVA in AF.7, 22
One study found a stroke event rate of 0.49 per 100 person-years for patients with AF and a CHA2DS2-VASc of 0 who were not anticoagulated, but this event rate increased to 1.55 if the score was 1. The study also found that warfarin treatment in patients with a score of 1 decreased morbidity and mortality compared to ASA alone or no treatment at all. The researchers also found that warfarin had no increased bleeding risk compared to using ASA alone.23 Additionally, it may be that ASA and clopidogrel increase the bleeding risk without any true benefit.24 While CHA2DS2-VASc gives us an algorithm for anticoagulation in nonvalvular AF, warfarin always is considered the first-line pharmacotherapy for anticoagulation in patients with mechanical heart valves.
Every year, about 2% of patients with AF treated with anticoagulation have a major bleeding event.25 The major cause of such bleeds is over-anticoagulation due to warfarin. Direct oral anticoagulants (DOAC) promise more predictable anticoagulation and reduced risk of bleeding. Warfarin or a DOAC is an appropriate first-line agent for stroke prevention in a patient with nonvalvular AF.20 Even in patients who have recently suffered from a transient ischemic attack, total bleeding risk from a DOAC started immediately is very low.26 In electrical cardioversions, when comparing DOAC to warfarin, the DOAC group was less likely to be subtherapeutic in anticoagulation goals and had decreased overall consumption of healthcare.27
Despite the increasing availability of DOACs, suboptimal use of anticoagulants for CVA prophylaxis in discharged AF patients remains a persistent challenge.28 If a patient is unable to maintain a therapeutic INR (between 2 and 3) on warfarin, then the 2014 American Heart Association (AHA) guidelines recommend switching the patient to a DOAC as a class 1C recommendation. The disadvantages of DOACs compared to warfarin are the twice-daily dosing of DOACs (except rivaroxaban) as well as their higher out-of-pocket cost for prescriptions. In a patient younger than 75 years of age with normal renal clearance, consider starting a DOAC instead of warfarin before discharge from the ED.29
For patients with AF who have had symptoms for less than 48 hours, rhythm control can be done using electrical or pharmacologic cardioversion.30 Pharmacologic options for rhythm conversion include dronedarone, amiodarone, flecainide, propafenone, and sotalol. In direct comparison studies, amiodarone is the most effective antiarrhythmic for maintaining a normal sinus rhythm7; however, it has multiple adverse outcomes, including bradycardia, QT prolongation, as well as effects on the thyroid, liver, lungs, blood vessels, and skin. Another option is flecainide, a class 1C antiarrhythmic and negative inotrope. It can increase mortality in patients with prior myocardial infarction with persistent left ventricular dysfunction.
Dronedarone, another class III antiarrhythmic like amiodarone, is less effective at rhythm control but without as many of the adverse effects of amiodarone. In 2014, a retrospective cohort study showed that, if taken daily for rhythm management in the outpatient setting, dronedarone decreased hospital admissions by 40% and ED visits by 30-45%.31 Similar to flecainide, propafenone’s negative inotropic properties require caution in post-myocardial infarction patients. Current data suggest that rhythm control does not affect survival overall in AF,7 whereas rate control does.
Electrical cardioversion also can be used for rhythm control in stable patients. There is an association between ED electrocardioversion and perceived ED effectiveness by patients receiving this modality; however, no association was found between this mode of treatment and a 30-day quality of life score.32
Pharmacologic rhythm control especially has adverse effects in acutely ill patients. Sheuermeyer et al found that in patients with a severe underlying medical condition (especially sepsis and HFrEF exacerbation) who presented with symptoms for less than 48 hours, 41% of patients with attempted rhythm control had an adverse effect such as hypotension or bradycardia requiring an intervention vs. 0.01% of those in that same group who were not given an antiarrhythmic.33
Cardiac ablation is becoming a tool that can be used earlier in a patient’s care for definitive treatment. The goal with ablation is to eliminate the arrhythmogenic foci. Ablation generally is indicated in patients who are anticoagulated and continue to have symptomatic occurrences despite appropriate pharmacotherapy. It can be considered first-line in patients who have symptomatic, paroxysmal AF.13 The argument for earlier consideration is that “AF begets AF,”7 meaning that atrial fibrillation often is progressive if untreated, and paroxysmal AF invariably will transition to permanent AF. This risk of progression is thought to be related to the time spent in AF. It seems that younger patients benefit more from ablation overall, but it can be effective in select older individuals.
Atrioventricular Nodal Reentrant Tachycardia and Atrioventricular Reentrant Tachycardia
SVT is a general term that describes any tachycardia originating from above the bundle of His. This would include atrial tachycardia, sinus tachycardia, AF, AFL, as well as AVNRT and AVRT. The term paroxysmal supraventricular tachycardia (PSVT) often is used interchangeably with AVNRT.
AVNRT and AVRT are both regular, narrow-complex rhythms and involve some reentrant pathway that is their foundation to produce tachycardia. (See Figure 4.) The anatomical difference is that with AVRT there is a myocardial strand that creates an electrical bridge between the atrium and the ventricle.34 Most commonly this structural difference is called the “bundle of Kent” as part of the Wolff-Parkinson-White (WPW) syndrome. On the other hand, AVNRT involves a reentrant circuit that is housed within the AV node. This circuit generally involves two pathways: a fast pathway (usually anterograde) and a slow pathway (usually retrograde). It is important to differentiate between the two terms because knowing if the AV node is the primary culprit will predict whether an AV-blocking agent is going to be effective.35
Figure 4. Supraventricular Tachycardia
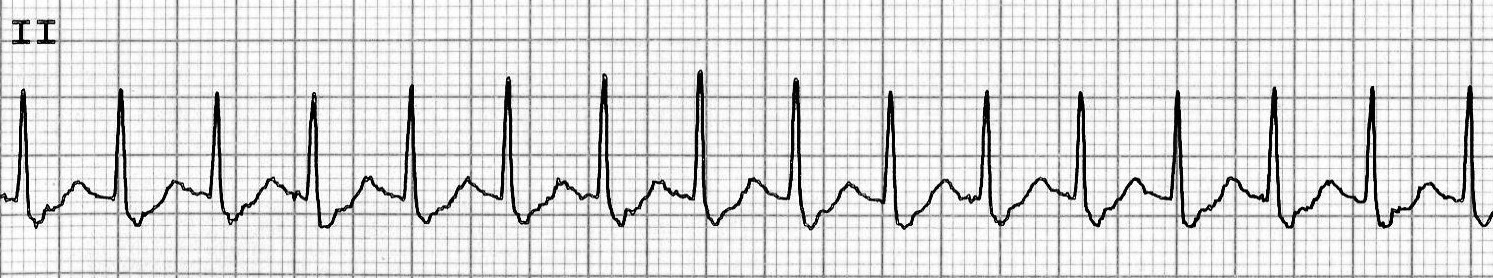
Lead II, narrow QRS complex tachycardia at rate of 184 without discernible P waves
Image courtesy of J. Stephan Stapczynski, MD
Palpitations are the most common symptom described by patients with AVNRT.35 Lightheadedness is a common symptom as well, but patients with AVNRT only very rarely present after a true syncope. Patients also may describe a sensation of “shirt flapping” or “neck pounding” when their symptoms begin.35 AVNRT is paroxysmal in nature, but also can be brought on by factors such as amphetamine use, alcohol or caffeine consumption, heavy exercise, or beta-blocker use. Women are affected more than men at a ratio of approximately 3:1. The age at onset is 32 ± 18 years.35
The hallmark for diagnosis of AVNRT on ECG is the recognition of a narrow-complex tachyarrhythmia. Commonly, P waves are not visible. If seen, they are conducted in a retrograde fashion and will be inverted in leads II, III, and aVF.
WPW syndrome refers to the ECG appearance during sinus rhythm, and provides the most common anatomical substrate for AVRT. The WPW pattern during sinus rhythm shows delta waves, slurring of the QRS upstroke indicative of ventricular pre-excitation, a shortened PR interval, and QRS prolongation.36 (See Figure 5.) During AVRT, there can be ST and T wave changes discordant with the QRS complex orientation.
Figure 5. Wolff-Parkinson-White Syndrome
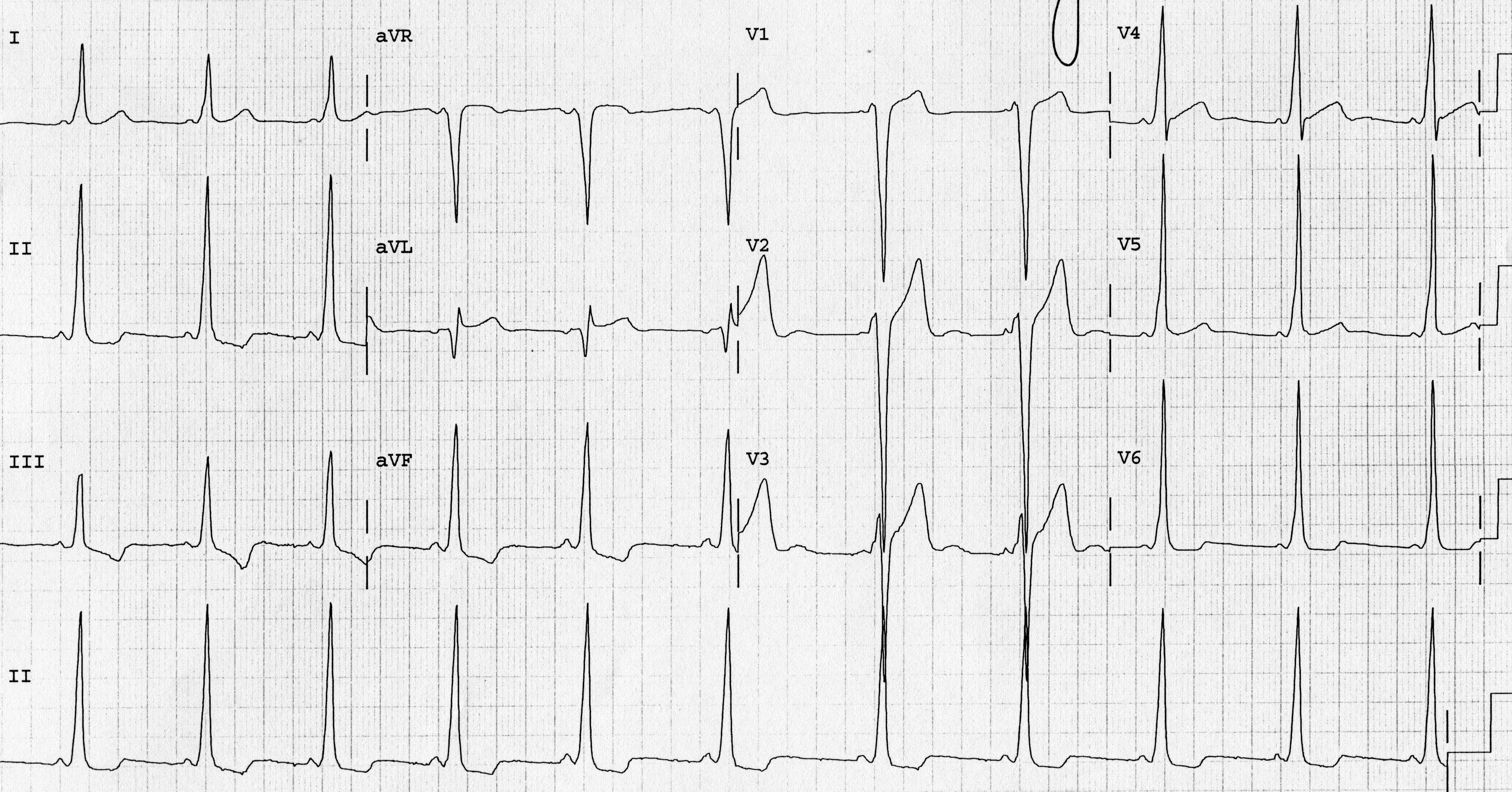
12-lead ECG showing delta wave and short PR interval
Image courtesy of J. Stephan Stapczynski, MD
AVRT can lead to wide QRS complexes if there is antidromic conduction (if the ventricles are depolarized by the accessory pathway), resulting in a wide-complex tachyarrhythmia that can be confused with VT. While these two entities can be difficult to differentiate on an ECG, the safest approach is to treat any unstable, wide-complex tachyarrhythmia as ventricular tachycardia.
Treatment of AVNRT and AVRT initially is the same. In the stable patient, use vagal maneuvers first. There are many techniques for this, such as asking the patient to bear down as if having a bowel movement or having the patient blow into a 5-cc syringe. These techniques work by increasing the intrathoracic pressure, causing stimulation of the baroreceptors in the carotid bodies and aortic arch, in turn causing vagal stimulation and activation of the parasympathetic (vagal) nervous system.37 Ocular pressure and carotid massage have fallen out of favor because of adverse effects.38 More recently, handstands have been described as a technique to achieve the same goal in pediatric patients.39
In 2015, the REVERT trial proposed a postural modification of the standard Valsalva to increase efficacy. In this study, the researchers compared the standard Valsalva to a modified Valsalva: starting patients in the semi-recumbent position, then having them bear down and then laying them flat and performing a passive leg raise. The authors found that the standard Valsalva technique converted 17% of patients with SVT to sinus rhythm, whereas the modified Valsalva converted 43%.40 It may be reasonable to start attempting this technique on patients who come into the ED with SVT if they are hemodynamically stable prior to trial of pharmacologic interventions.
If vagal maneuvers prove ineffective, second-line treatments include adenosine and diltiazem. Currently, adenosine is the preferred drug for SVTs that present to the ED and do not resolve with vagal maneuvers. The most common side effect of adenosine is described by patients as a feeling that they are “going to die.” Patients may have this feeling for up to one to two minutes after receiving the drug. Adenosine has a short half-life and rare adverse effects.41 It is both a therapeutic and diagnostic agent. By causing a temporary AV block and slowing the rhythm, the true dysrhythmia (such as AF or AVRT) can be seen more clearly and diagnosed more accurately. In ACLS, the standard algorithm is to first give a 6 mg dose, followed by a 12 mg push (if needed), which can be repeated one additional time. Adenosine is given as a fast IV push through a peripheral IV followed by a saline flush and raising the patient’s arm in the air.
Although the FDA-approved prescribing information for adenosine only includes three doses and up to 12 mg at a time, 18 mg boluses reportedly have been used safely, and higher initial doses often are needed in children (150 mcg/kg to 250 mcg/kg), with most requiring more than one dose for effective conversion.35,42 There are case reports of doses up to 36 mg being used for cardioversion, but these doses should not be attempted without cardiology consultation.43
In patients who fail vagal maneuvers and adenosine and remain hemodynamically stable, it is reasonable to try a calcium channel blocker or beta-blocker. Calcium channel blockers are considered more efficacious. Verapamil 1 mg/minute up to a maximum dose of 20 mg or diltiazem 2.5 mg/minute up to a maximum of 50 mg can be used with approximately 98% conversion rate. The potential side effects of calcium channel blockers include hypotension and bradycardia. Adenosine still is preferred since these drugs last much longer in the system than adenosine.44
In 2015, Dogan et al retrospectively investigated the effectiveness of adenosine vs. diltiazem. The results were surprising; 60% of patients converted back to normal sinus rhythm after the first 6 mg dose of adenosine, 65% after the second adenosine dose (12 mg), and 72% after the third adenosine dose (12 mg), compared to 95% of patients who received diltiazem (given 0.25 mg/kg IV over two minutes with a second dose at 0.35 mg/kg). Additionally, if diltiazem was given after a failed adenosine attempt, then the rate of success was 97%.34 These data suggest that there is benefit in including diltiazem in the initial treatment strategy, especially when the rhythm is refractory to conversion with adenosine.
In patients with paroxysmal symptoms, outpatient beta-blockers, diltiazem, or verapamil may be appropriate if there is no evidence of pre-excitation on ECG. According to the 2015 American College of Cardiology/AHA/Heart Rhythm Society guidelines for management of adults with SVT, vagal maneuvers, adenosine, and synchronized cardioversion have class I recommendations for treatment, while calcium channel blockers and beta-blockers have class IIa recommendations for acute management of SVT.35
If all of the pharmacologic methods have failed, synchronized cardioversion then can be performed even in the hemodynamically stable patient to prevent further strain on the heart. For AVRT-WPW, catheter ablation is considered the ultimate treatment of choice.45
Ventricular Tachycardias
By definition, VTs have a rate over 100 bpm and a QRS duration greater than 0.1-0.12 ms in adults.46 (See Figure 6.) VT can be classified as monomorphic or polymorphic. Monomorphic VT has long been thought to be more common; however, more recently, this was found to be true only in certain settings, such as in the CCU and the catheterization lab, and did not necessarily hold true in the ED.46 Monomorphic VT originates from one focus in a ventricle as opposed to several foci as with polymorphic VT. Monomorphic and polymorphic VT can be caused by myocardial ischemia as well as dilated cardiomyopathy or hypertrophy and their subsequent changes to the myocardial architecture.47 Monomorphic VT is more commonly from long-term structural abnormalities such as congestive heart failure and fibrous changes within the ventricles. These complexes are all uniform and are more likely to have signs of AV dissociation such as capture beats and fusion complexes.46
Figure 6. Ventricular Tachycardia
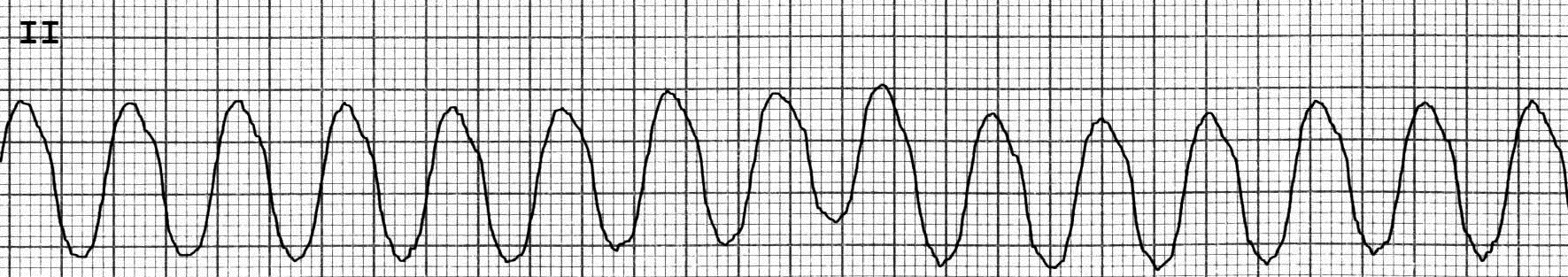
Lead II, monomorphic ventricular tachycardia at rate of 142
Image courtesy of J. Stephan Stapczynski, MD
Patients with new-onset, non-ischemic cardiomyopathy with LVEF < 35% have an especially high risk of VT and VF during the initiation and optimization of their medication therapy.47 There have been reports of exercise- (catecholamine) triggered ventricular arrhythmias in children, but these have an unclear etiology and significance. Patients may present with chest pain, palpitations, shortness of breath, syncope, seizures, or in cardiac arrest. Remember to obtain an ECG in the seizure patient, as seizure-like activity can be due to cerebral hypoxia from an arrhythmia and would not be cured by antiepileptic medications.48 In a 2017 demographic review by Gillis, the incidence of VT and sudden death were lower in women than in men. Women also were more likely to benefit from an ICD but, interestingly, were referred less frequently than men for ICD placement.49
Monomorphic VT usually is seen when a circuit around a region of scar tissue is present, except in one rare subtype found in structurally normal hearts. This rare subtype originates from the right ventricular outflow tract. It can be identified by a left bundle branch block pattern with tall R waves in the inferior leads on ECG. Generally, this type of VT does not result in hemodynamic decompensation as does traditional VT, thus its ECG characteristics can be reassuring. Nevertheless, if the identification is at all unclear or the patient’s condition is waning, choose traditional VT treatment.
Polymorphic VT encompasses torsades de pointes (TdP) and a bidirectional subtype. Polymorphic VTs are driven by ischemia and are associated with frequent ectopic ventricular beats and an R on T phenomenon. However, TdP can be thought of as a distinct entity that is highly affected by electrolyte concentrations. The best treatment for this arrhythmia is to re-perfuse the heart. In the case of TdP, electrolyte abnormalities also should be corrected immediately. Following successful percutaneous coronary intervention, the arrhythmia usually will resolve.50
Differentiating ECG diagnosis of wide-complex tachycardias from VT vs. an SVT with aberrancy has long been a challenge of the ED provider. A wide-complex tachycardia presents three potential diagnoses: 1) VT; 2) SVT with either a right or left bundle branch block; or 3) SVT (including AF) with ventricular activation uniformly via a bypass tract, as in WPW syndrome. The most critical step in diagnosis is determining whether the rhythm on the ECG is SVT or VT. This determination is essential for safe treatment, as an AV-nodal blocking agent will terminate many SVTs but has the potential to cause serious harm if given in the setting of VT. In stable patients, many algorithms have been employed to attempt differentiation of these entities. Examples include the Brugada51 and Vereckei52 algorithms. Although both of these show very good specificity for VT and thus may be helpful if they are able to confirm SVT with aberrancy, neither demonstrates good sensitivity. Several newer algorithms also have been proposed; however, in a study comparing many of these head to head, none were found to have significant sensitivity to be used confidently in clinical practice.53
Since it is not completely possible to rule out SVT with aberrancy in a wide-complex tachycardia, and assuming this incorrectly could result in serious consequences, when in doubt, all wide-complex tachycardias should be treated as VT.
In an unstable patient who still has a pulse, the treatment is very straightforward: Treat with DC cardioversion. The pulseless VT patient is treated according to ACLS guidelines with immediate defibrillation. Following successful cardioversion, an amiodarone drip should be considered to maintain sinus rhythm, and the patient should be admitted to the hospital.50
The treatment of stable monomorphic VT is controversial. The most effective treatment is certainly DC cardioversion; however, in stable patients, there are several antiarrhythmic medications that can be tried. These include procainamide, amiodarone, lidocaine, ajmaline, sotalol, propafenone, and flecainide. A randomized, open-label study comparing procainamide and amiodarone showed that procainamide terminated 57% of VT and amiodarone only 38%, with procainamide overall being associated with less adverse events.54 Another retrospective cohort study comparing amiodarone and procainamide showed 25% termination with amiodarone and 35% with procainamide; however, in this study, the difference between the two was not statistically significant.55
Lidocaine, once a mainstay antiarrhythmic, has fallen out of favor in the treatment of VT with preserved ejection fraction.56 Although it is superior at terminating ongoing VT in the setting of ongoing myocardial infarction, lidocaine has not shown any mortality benefit. In a 2015 systematic review of antiarrhythmic therapies, procainamide, ajmaline, and sotalol all were shown to be superior to lidocaine in terminating monomorphic VT. In the same study, amiodarone and procainamide were equally effective.57
Sotalol is another option for control of VT. It has been shown to convert patients out of 60% of all tachyarrhythmias, although effectiveness was higher in AVRT than in VT. An extra 15% were converted after propafenone was added to sotalol.58 Sotalol does cause modest QT interval prolongation, and efforts should be made to avoid concomitant use of other QT-prolonging medications.
Flecainide works by directly suppressing the calcium release from the sarcoplasmic reticulum in cardiac cells. Without the calcium efflux, catecholamine-triggered VT is blocked. Flecainide plus a beta-blocker for treatment can significantly decrease ventricular ectopy during exercise compared to just a beta-blocker in outpatient management.59 The decision about which agent to give can be made in conjunction with a cardiologist. When expert consultation is not available, and based on these studies, procainamide presents a better choice and has less risk of adverse effects, particularly if the wide complex tachycardia is due to WPW.
TdP is a form of polymorphic VT that requires pre-existing prolonged QT interval and sinusoidal variation in QRS complex direction and amplitude during the tachycardia. (See Figure 7.) Generally, it is initiated when a PVC occurs at the same time as the ventricles are repolarizing (on the T wave). This is the “R on T phenomenon.” TdP usually is short-lived and resolves on its own after several seconds; however, it does have a high risk to decompensate into VF. First-line treatment for TdP is a magnesium infusion. It also can be treated with isoproterenol or overdrive pacing.50 When VT is present, investigate for electrolyte abnormalities. Potassium, magnesium, and calcium often are culprits in the evolution and maintenance of arrhythmias.
Figure 7. Torsades de Pointes
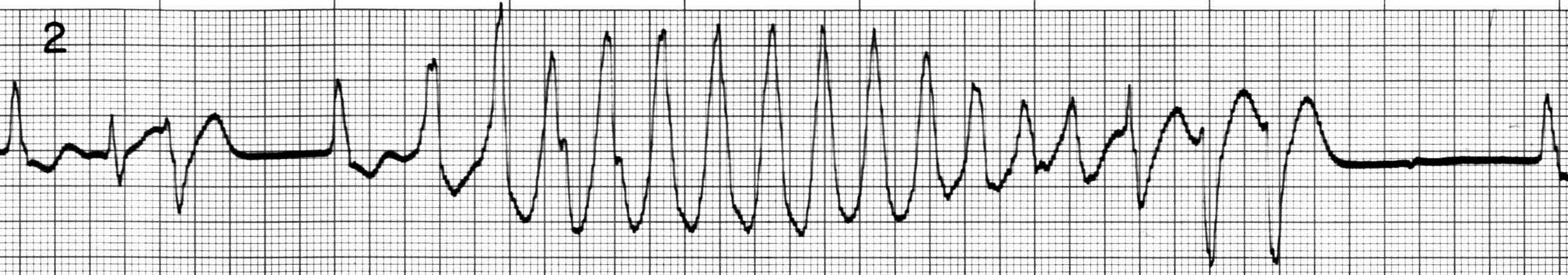
Lead II, 16-beat run of torsades with sinusoidal variation in QRS amplitude and direction triggered by PVC
Image courtesy of J. Stephan Stapczynski, MD
VT storm refers to a condition in which a patient has more than three episodes of sustained VT lasting longer than two to four hours each requiring an intervention to regain NSR. These patients need very close monitoring and often require more invasive therapies, such as an intra-aortic balloon pump or a left ventricular assist device. In these patients, maintain a low threshold to induce anesthesia to help decrease their sympathetic tone.50
Conclusion
Tachycardia is a common and potentially life-threatening finding in the ED. As such, having a systematic approach to the diagnosis and treatment of tachycardia is a mainstay of emergency medicine practice. Treatment of all unstable tachyarrhythmias requires prompt recognition and initiation of ACLS guidelines, whereas stable patients require a more nuanced approach to tailor therapies based on their ECG findings.
In addition to the acute management of these patients, it also is important to consider long-term management, as these arrhythmias often are diagnosed first in the ED. Decisions regarding rate vs. rhythm control, stroke risk mitigation, and lifestyle counseling all will have a significant impact on the health of these patients.
REFERENCES
- Hannibal GB. Wandering atrial pacemaker and multifocal ectopic atrial tachycardia. AACN Adv Crit Care 2015;26:73-76.
- Goudis CA, Konstantinidis AK, Ntalas IV, et al. Electrocardiographic abnormalities and cardiac arrhythmias in chronic obstructive pulmonary disease. Int J Cardiol 2015;199:264-273.
- Aburawi EH, Narchi H, Souid AK. Persistent wandering atrial pacemaker after epinephrine overdosing — a case report. BMC Pediatr 2013;13:1.
- Oner T, Akdeniz C, Adaletli H. Multifocal atrial tachycardia caused by risperidone. Int J Cardiol 2016;203:855-857.
- Meka SG, Shelden D, Mertens A, et al. A hol(e)y predicament. Respirol Case Reports 2017;5:e00237.
- Lazaros G, Chrysohoou C, Oikonomou E, et al. The natural history of multifocal atrial rhythms in elderly outpatients: Insights from the “Ikaria study.” Ann Noninvasive Electrocardiol 2014;19:483-489.
- Ponikowski P, Voors AA, Anker SD, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society for Cardiology (ESC) developed with the special contribution of the Heart Failure Association of the ESC. Eur Heart J 2016;37:2129-2200.
- Van Gelder IC, Rienstra M, Crijns HJ, Olshansky B. Rate control in atrial fibrillation. Lancet 2016;388:818-828.
- Redfearn DP, Furqan MA, Enriquez A, et al. Emergency department re-presentation for atrial fibrillation and atrial flutter. Can J Cardiol 2016;32:344-348.
- Lin MP, Ma J, Weissman JS, et al. Hospital-level variation and predictors of admission after ED visits for atrial fibrillation: 2006 to 2011. Am J Emerg Med 2016;34:2094-2100.
- von Besser K, Mills AM. Is discharge to home after emergency department cardioversion safe for the treatment of recent-onset atrial fibrillation? Ann Emerg Med 2011;58:517.
- Matusik P, Lelakowski J, Malecka B, et al. Management of patients with atrial fibrillation: Focus on treatment options. J Atr Fibrillation 2016;9:1450.
- Kirchhof P. The future of atrial fibrillation management: Integrated care and stratified therapy. Lancet 2017; doi: 10.1016/S0140-6736(17)31072-3. [Epub ahead of print.]
- Harvey S, Wilson K, Brad Hall A. Diltiazem versus esmolol for acute rate control in the emergency department. Am J Emerg Med April 2017; doi: 10.1016/j.ajem.2017.04.005. [Epub ahead of print.]
- Fromm C, Suau SJ, Cohen V, et al. Diltiazem vs. metoprolol in the management of atrial fibrillation or flutter with rapid ventricular rate in the emergency department. J Emerg Med 2015;49:175-182.
- Van Gelder IC, Healey JS, Crijns HJGM, et al. Duration of device-detected subclinical atrial fibrillation and occurrence of stroke in ASSERT. Eur Heart J 2017;38:1339-1344.
- Prystowsky EN, Benson DW Jr, Fuster V, et al. Management of patients with atrial fibrillation. A Statement for Healthcare Professionals. From the Subcommittee on Electrocardiography and Electrophysiology, American Heart Association. Circulation 1996;93:1262-1277.
- Pathak RK, Middeldorp ME, Meredith M, et al. Long-term effects of goal-directed weight management in an atrial fibrillation cohort: A long-term follow-up study (LEGACY). J Am Coll Cardiol 2015;65:2159-2169.
- Odum LE, Cochran KA, Aistrope DS, Snella KA. The CHADS2 versus the new CHA2DS2-VASc scoring systems for guiding antithrombotic treatment of patients with atrial fibrillation: Review of the literature and recommendations for use. Pharmacotherapy 2012;32:285-296.
- January CT, Wann LS, Alpert JS, et al. 2014 AHA/ACC/HRS guideline for the management of patients with atrial fibrillation: Executive summary: A Report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol 2014;64:2305-2307.
- Poli D, Antonucci E, Grifoni E, et al. Bleeding risk during oral anticoagulation in atrial fibrillation patients older than 80 years. J Am Coll Cardiol 2009;54:999-1002.
- Friberg L, Skeppholm M, Terént A. Benefit of anticoagulation unlikely in patients with atrial fibrillation and a CHA2DS2-VASc score of 1. J Am Coll Cardiol 2015;65:225-232.
- Lip GY, SkjØth F, Rasmussen LH, Larsen TB. Oral anticoagulation, aspirin, or no therapy in patients with nonvalvular AF with 0 or 1 stroke risk factor based on the CHA2DS2-VASc Score. J Am Coll Cardiol 2015;65:1385-1394.
- Golive A, May HT, Bair TL, et al. The population-based long-term impact of anticoagulant and antiplatelet therapies in low-risk patients with atrial fibrillation. Am J Cardiol 2017;120:75-82.
- Seiffge DJ, Traenka C, Polymeris A, et al. Early start of DOAC after ischemic stroke: Risk of intracranial hemorrhage and recurrent events. Neurology 2016;87:1856-1862.
- Alamneh EA, Chalmers L, Bereznicki LR. Suboptimal use of oral anticoagulants in atrial fibrillation: Has the introduction of direct oral anticoagulants improved prescribing practices? Am J Cardiovasc Drugs 2016;16:183-200.
- Sharif Z, Srinivas B, Tiedt I, et al. Evaluating cardioversion outcomes for atrial fibrillation on novel oral anticoagulants versus warfarin: Experience at a tertiary referral centre. Ir J Med Sci 2017; doi: 10.1007/s11845-017-1582-3. [Epub ahead of print.]
- Bajorek B. A review of the safety of anticoagulants in older people using the medicines management pathway: Weighing the benefits against the risks. Ther Adv Drug Saf 2011;2:45-48.
- Barnes G, Haymart B, Alexandris-Sorphis T. Anticoagulation toolkit: A consortium-developed quick reference for anticoagulation. Michigan Anticoagulation Quality Improvement Initiative (MAQI2). 2017; Version 1.7; 1-75.
- Hamilton A, Clark D, Gray A, et al. The epidemiology and management of recent-onset atrial fibrillation and flutter presenting to the emergency department. Eur J Emerg Med 2015;22:155-161.
- Kim MH, Lin J, Jhaveri M, Koren A. Impact of dronedarone treatment on healthcare resource utilization in patients with atrial fibrillation/flutter. Adv Ther 2014;31:318-332.
- Ballard DW, Reed ME, Singh N, et al. Emergency department management of atrial fibrillation and flutter and patient quality of life at one month postvisit. Ann Emerg Med 2015;66:646-654.e2.
- Scheuermeyer FX, Pourvali R, Rowe BH, et al. Emergency department patients with atrial fibrillation or flutter and an acute underlying medical illness may not benefit from attempts to control rate or rhythm. Ann Emerg Med 2015;65:511-522.e2.
- Dogan H, Ozucelik DN, Aciksari K, et al. To decide medical therapy according to ECG criteria in patients with supraventricular tachycardia in emergency department: Adenosine or diltiazem. Int J Clin Exp Med 2015;8:9692-9699.
- Page RL, Joglar JA, Caldwell MA, et al. 2015 ACC/AHA/HRS Guideline for the Management of Adult Patients With Supraventricular Tachycardia: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. J Am Coll Cardiol 2016;67:1575-1623.
- Benson DW, Cohen MI. Wolff-Parkinson-White syndrome: Lessons learnt and lessons remaining. Cardiol Young 2017;27:S62-S67.
- Smith GD, Fry MM, Taylor D, et al. The effectiveness of the Valsalva manoeuvre for reversion of supraventricular tachycardia. Cochrane Database Syst Rev 2015;(2):CD009502.
- van den Brink RB, de Lange FJ. [Carotid sinus massage is not a benign intervention]. Ned Tijdschr Geneeskd 2017;161:D1312.
- Hare M, Ramlakan S. Handstands: A treatment for supraventricular tachycardia? Arch Dis Child 2015;100:54-55.
- Appelboam A, Reuben A, Mann C, et al. Postural modification to the standard Valsalva manoeuvre for emergency treatment of supraventricular tachycardias (REVERT): A randomised controlled trial. Lancet 2015;386(10005):1747-1753.
- Rajkumar CA, Qureshi N, Ng FS, et al. Adenosine induced ventricular fibrillation in a structurally normal heart: A case report. J Med Case Rep 2017;11:21.
- Díaz-Parra S, Sánchez-Yañez P, Zabala-Argüelles I, et al. Use of adenosine in the treatment of supraventricular tachycardia in a pediatric emergency department. Pediatr Emerg Care 2014;30:388-393.
- Bailey AM, Baum RA, Rose J, Humphries RL. High-dose adenosine for treatment of refractory supraventricular tachycardia in an emergency department of an academic medical center: A case report and literature review. J Emerg Med 2016;50:477-481.
- Lim SH, Anatharaman V, Teo WS, Chan YH. Slow infusion of calcium channel blockers compared with intravenous adenosine in the emergency treatment of supraventricular tachycardia. Resuscitation 2009;80:523-528.
- Voss F, Eckardt L, Busch S, et al. [AV renentrant tachycardia and Wolff-Parkinson-White syndrome: Diagnosis and treatment]. Herzschrittmacherther Elektrophysiol 2016;27:381-389.
- Brady WJ, Mattu A, Tabas J, Ferguson JD. The differential diagnosis of wide QRS complex tachycardia. Am J Emerg Med 2017;35:1525-1529.
- Duncker D, KÖnig T, Hohmann S, et al. Ventricular arrhythmias in patients with newly diagnosed nonischemic cardiomyopathy: Insights from the PROLONG study. Clin Cardiol 2017;40:586-590.
- Wentlandt M, Morris SC, Mitchell SH. Ventricular tachycardia and prolonged QT interval presenting as seizure-like activity. Am J Emerg Med 2017;35:804.e5-804.e6.
- Gillis AM. Atrial fibrillation and ventricular arrhythmias: Sex differences in electrophysiology, epidemiology, clinical presentation, and clinical outcomes. Circulation 2017;135:593-608.
- Luther V, Nijjer SS, Lefroy DC. Management of ventricular tachycardia. Br J Hosp Med (Lond) 2017;78:C6-C9.
- Brugada P, Brugada J, Mont L, et al. A new approach to the differential diagnosis of a regular tachycardia with a wide QRS complex. Circulation 1991;83:1649-1659.
- Vereckei A, Duray G, Szenasi J, et al. New algorithm using only lead aVR for differential diagnosis of wide QRS complex tachycardia. Heart Rhythm 2008;5:89-98.
- Jastrzebski M, Kukla P, Czarnecka D, Kawecka-Jaszcz K. Comparison of five electrocardiographic metods for differentiation of wide QRS-complex tachycardias. Europace 2012;14:1165–1171.
- Ortiz M, Martin A, Arribas F, et al. Randomized comparison of intravenous procainamide vs. intravenous amiodarone for the acute treatment of tolerated wide QRS tachycardia: The PROCAMIO study. Eur Heart J 2017;38:1329-1335.
- Marill KA, de Souza IS, Nishijima DK, et al. Amiodarone or procainamide for the termination of sustained stable ventricular tachycardia: An historical multicenter comparison. Acad Emerg Med 2010;17:297-306.
- Long B, Koyfman A. Best clinical management: Emergency medicine management of stable monomorphic ventricular tachycardia. J Emerg Med 2017;52:484-492.
- deSouza IS, Martindale JL, Sinert R. Antidysrhythmic drug therapy for the termination of stable, monomorphic ventricular tachycardia: A systematic review. Emerg Med J 2015;32:161-167.
- Li X, Zhang Y, Liu H, et al. Efficacy of intravenous sotalol for treatment of incessant tachyarrhythmias in children. Am J Cardiol 2017;119:1366-1370.
- Kannankeril PJ, Moore JP, Cerrone M, et al. Efficacy of flecainide in the treatment of catecholaminergic polymorphic ventricular tachycardia: A randomized clinical trial. JAMA Cardiol 2017;2:759-766.
The recognition, diagnosis, and treatment of tachycardia is a cornerstone of emergency medicine practice. This article will cover the most commonly seen supraventricular and ventricular tachycardias encountered in the ED, with a focus on their electrocardiographic diagnoses and treatment options.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
