Meropenem-vaborbactam
By Jamie Kuo, PharmD, BCCCP
Department of Pharmacy, Stanford Health Care
Dr. Kuo reports no financial relationships relevant to this field of study.
Meropenem-vaborbactam (Vabomere) is the latest β-lactam/β-lactamase inhibitor (BLI), approved by the FDA in August 2017 for treatment of complicated urinary tract infections (cUTI), including pyelonephritis, caused by susceptible Escherichia coli, Klebsiella pneumoniae, and Enterobacter cloacae species complex in adults older than 18 years of age. Meropenem is an existing carbapenem antibacterial that exhibits bactericidal activity by binding to intracellular penicillin-binding proteins (PBP) and inhibiting bacterial cell wall synthesis. Vaborbactam is a novel boronic acid, non-suicidal, reversible BLI without intrinsic antibacterial activity.
Vaborbactam prevents degradation of meropenem by serine β-lactamases to restore activity against Enterobacteriaceae including Klebsiella pneumoniae carbapenemase (KPC). Meropenem-vaborbactam has activity against most Ambler class A, C, and some class D β-lactamases (oxacillinases without carbapenemase activity). Notably, meropenem-vaborbactam is not active against metallo-β-lactamases (MBL). The addition of vaborbactam did not significantly improve activity of meropenem against Acinetobacter baumannii or Pseudomonas aeruginosa in vitro, nor did it affect activity against anaerobes when studied in combination with biapenem.
PHARMACOKINETICS/PHARMACODYNAMICS
(See Table 1.)
- Meropenem exposure is affected by renal impairment, resulting in increased AUC.
- Both meropenem and vaborbactam are removed by hemodialysis. Following administration of 2 g meropenem-vaborbactam, 38% of the meropenem and 53% of the vaborbactam dose was recovered in the dialysate.
- Pharmacokinetics of meropenem are not affected by hepatic impairment. Vaborbactam is not anticipated to be affected by hepatic function, either, given it does not undergo hepatic metabolism.
- Meropenem demonstrates time-dependent bacterial killing while the pharmacodynamics target of vaborbactam appears to be AUC:MIC based on in vitro and animal studies.
Table 1. Mean Population Pharmacokinetics of Meropenem-vaborbactam
|
Pharmacokinetic Parameter |
Meropenem |
Vaborbactam |
|
Protein binding |
2% |
33% |
|
Vd at steady-state |
20.2 L |
18.6 L |
|
Cl (L/h), multiple doses |
15.1 |
10.9 |
|
t½ (h) |
1.22 |
1.68 |
|
Metabolism |
Hydrolysis, 22% |
None |
|
Excretion |
Urine, 40-60% unchanged Feces, 2% |
Urine, 75-95% unchanged |
CLINICAL TRIALS3,4
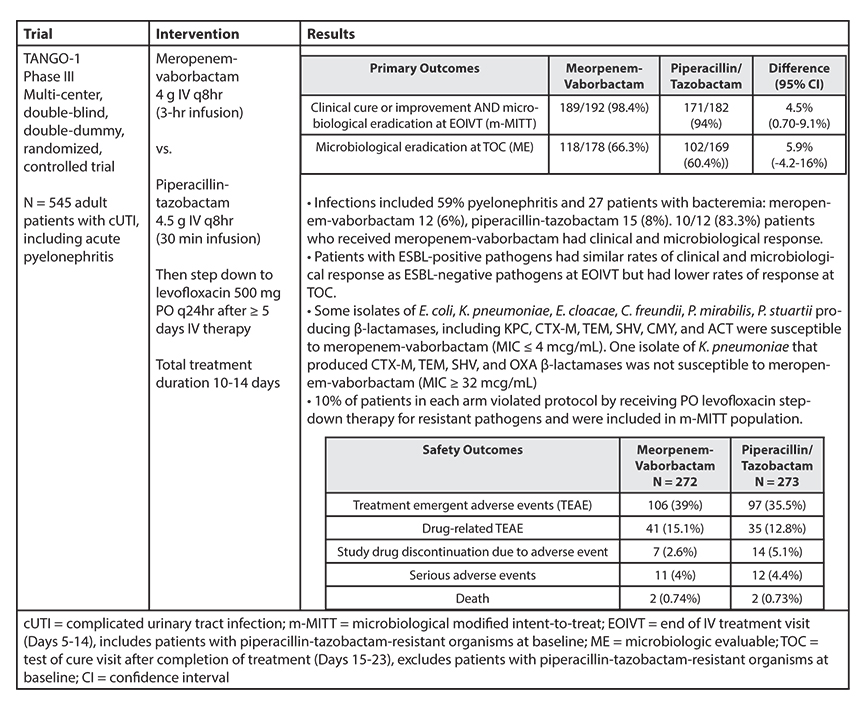
The efficacy and safety of meropenem-vaborbactam compared to piperacillin-tazobactam were examined in a Phase III multi-center, double-blind, double-dummy, randomized, controlled trial for the treatment of cUTI, including acute pyelonephritis, in adults. (See Table 2.) Meropenem-vaborbactam met statistical significance for superiority over piperacillin-tazobactam in the FDA primary endpoint of clinical cure or improvement and microbiological eradication at the end of IV treatment in the microbiological modified intent-to-treat population. For the primary endpoint of microbial eradication at test of cure visit, meropenem-vaborbactam was non-inferior to piperacillin-tazobactam in the microbiolic evaluable population.
Table 2. TANGO-1 Trial Summary
ADVERSE EFFECTS1,4
The most common adverse events reported in the Phase III clinical trial comparing meropenem-vaborbactam to piperacillin-tazobactam in adult patients with cUT/acute pyelonephritis were headache (8.8%), phlebitis/infusion site reactions (4.4%), and diarrhea (3.3%). Adverse events led to study drug discontinuation in 2.6% of patients receiving meropenem-vaborbactam compared to 5.1% of patients who received piperacillin-tazobactam. The most common reason for discontinuation due to adverse effect was hypersensitivity (1.1%), followed by infusion-related reactions (0.7%). Death occurred in two patients in each arm.
DOSAGE AND ADMINISTRATION1
- Meropenem-vaborbactam is administered as an intravenous infusion over three hours.
- Dosing is expressed as total grams of the meropenem-vaborbactam combination in a 1:1 ratio (i.e., 2 g is 1 g meropenem and 1 g vaborbactam).
- Duration of use is up to 14 days.
- Dosing is affected by renal function as calculated by the Modification of Diet in Renal Disease (MDRD) formula.
- Administer after hemodialysis on dialysis days.
- Dose adjustment for hepatic impairment is not necessary.
- Further dilution in 0.9% sodium chloride is required prior to administration.
Table 3. Meropenem-vaborbactam Dosing
|
eGFR (mL/min/1.73m2) |
Vabomere Dose |
Dosing Interval |
|
≥ 50 |
4 g (meropenem 2 g and |
Q 8 hours |
|
30-49 |
2 g (meropenem 1 g and |vaborbactam 1 g) |
Q 8 hours |
|
15-29 |
2 g (meropenem 1 g and |
Q 12 hours |
|
< 15 |
1 g (meropenem 0.5 g and vaborbactam 0.5 g) |
Q 12 hours |
CONTRAINDICATIONS1
- Hypersensitivity to meropenem or vaborbactam or other drugs in the same class
- History of anaphylactic reactions to other β-lactam antibacterials
WARNINGS/PRECAUTIONS1
- Hypersensitivity reactions were reported in clinical trials. Risk is increased in patients with a history of sensitivity to multiple allergens and/or other β-lactam antibacterials.
- Neurologic adverse events, including seizures, have been reported with meropenem. Incidence is higher in patients with underlying neurologic disorders, bacterial meningitis, and/or renal impairment.
- Super-infections, including Clostridium difficile-associated diarrhea (CDAD), have been reported with prolonged use.
- Drug-drug interaction with meropenem and valproic acid may result in increased risk of breakthrough seizures due to subtherapeutic valproic acid concentrations that may not be possible to overcome by increasing valproic acid dose. The combination should be avoided; otherwise, alternative anticonvulsant therapy should be considered.
- Use caution with meropenem in patients with renal impairment, which may increase risk of neurologic adverse events and thrombocytopenia.
SIGNIFICANT DRUG INTERACTIONS1
- Valproic acid and meropenem (see Warnings/Precautions)
- Meropenem is a substrate of OAT1 and OAT3 renal transporters. Probenecid may increase meropenem mean systemic exposure by 56% and mean elimination half-life by 38% by competing for active tubular secretion.
- Vaborbactam has low potential for clinically significant drug-drug interactions as it is not a substrate or inhibitor of cytochrome P450 enzymes or hepatic/renal transporters based on in vitro studies.
Table 4. Cost5
|
Medication |
How Supplied |
Average Wholesale Price |
Usual Dose |
Cost of Therapy per Day |
|
Meropenem- |
2 g vials |
$198 |
4 g q8hr |
$1,188 |
|
Ceftazidime- avibactam |
2.5 g vials |
$359.10 |
2.5 g q8hr |
$1,077.30 |
CONCLUSION
Vaborbactam is a novel BLI that, when given in combination with meropenem, restores activity against some carbapenemase-producing Enterobacteriaceae. Meropenem-vaborbactam is the second beta-lactam/BLI combination available in the United States to have activity against Klebsiella pneumoniae carbapenemases (KPCs). However, similar to ceftazidime-avibactam, meropenem-vaborbactam lacks activity against Ambler class B MBLs. In Phase III studies in cUTI, meropenem-vaborbactam demonstrated superiority to piperacillin-tazobactam in the FDA primary endpoint of clinical cure or improvement and microbiological eradication at the end of IV treatment and appears to be well tolerated with a similar safety profile.
Carbapenems are considered the first-line treatment for multi-drug-resistant (MDR) gram-negative infections, including extended-spectrum β-lactamases. In a climate of increasing carbapenem resistance, meropenem-vaborbactam represents an important treatment option in the management of carbapenem-resistant Enterobacteriaceae (CRE). Given limited treatment experience, the role of meropenem-vaborbactam compared to current best available therapy for CRE remains to be seen, including any potential differences on clinical outcomes. Judicious use and further study of relative resistance thresholds also will be necessary, as breakthrough avibactam resistance already has been reported in patients treated with ceftazidime-avibactam. TANGO-2, a Phase III multi-center, open-label study comparing meropenem-vaborbactam to best available treatment in adults with serious infections due to known or suspected KPC-producing CRE has been completed but the results have not yet been published. Of note, researchers ended randomization to the comparator arm early after an interim analysis reported favorable efficacy and safety results with meropenem-vaborbactam.6
REFERENCES
- Vabomere TM [Package Insert]. The Medicines Company, 2017.
- Wong D, van Duin D. Novel beta-lactamase inhibitors: Unlocking their potential in therapy. Drugs 2017;77:615-628.
- ClinicalTrials.gov. Efficacy, safety, tolerability of meropenem-
vaborbactam compared to piperacillin-tazobactam in complicated urinary tract infections (cUTIs), including acute pyelonephritis (AP), in adults. Available at: https://clinicaltrials.gov/ct2/show/NCT02166476. Accessed Nov. 11, 2017. - Meanwell C, Loutit J, Dudley M. TANGO 1 Phase 3 trial results; conference call, PDF; June 27, 2016.
- Lexi-Comp, Inc. (Lexi-DrugsTM). Lexi-Comp, Inc.
- BusinessWire. The Medicines Company to present new data from TANGO II study of Vabomere (meropenem and vaborbactam) at ID Week 2017. Oct. 5, 2017. Available at: http://www.businesswire.com/news/home/20171005005377/en/. Accessed Nov. 13, 2017.
Meropenem-vaborbactam (Vabomere) is the latest β-lactam/β-lactamase inhibitor (BLI), approved by the FDA in August 2017 for treatment of complicated urinary tract infections (cUTI), including pyelonephritis, caused by susceptible Escherichia coli, Klebsiella pneumoniae, and Enterobacter cloacae species complex in adults older than 18 years of age.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
