What Do You Know About Wound Care?
December 1, 2017
Reprints
AUTHORS
Richard Simman, MD, FACS, FACCWS, Plastic and Reconstructive Surgery, President and Chair of the American Board of Wound Medicine and Surgery, Co-Director Wound Care Program, ProMedica Health System, Jobst Vascular Institute/ProMedica Toledo Hospital, Toledo, OH; Clinical Professor, Department of Surgery at University of Toledo College of Medicine; Clinical Professor, Dermatology, Pharmacology, and Toxicology, Wright State University Boonshoft School of Medicine, Dayton
Anthony J. McNevin, Executive Director, American Board of Wound Medicine and Surgery
PEER REVIEWER
Dean L. Winslow, MD, Professor of Medicine, Division of General Medical Disciplines, Division of Infectious Diseases and Geographic Medicine, Stanford University School of Medicine, CA
Executive Summary
- The incidence of non-healing cutaneous wounds is 5 to 7 million per year in the United States, with a resulting $25 billion cost.
- Wound healing is a normal biological process that proceeds through four overlapping phases: hemostasis, inflammation, proliferation, and remodeling.
- The most frequently seen wounds are venous, diabetic, arterial, pressure, and surgical.
- Impairment of wound healing typically involves local factors, such as inadequate oxygenation, infection, and inadequate offloading. Age, stress, alcohol, nutrition, diabetes, obesity, smoking, and medications also play important roles.
- Treatment of complicated wounds is complex and embraces multiple new modalities. Referrals may be best guided to members of the American Board of Wound Medicine and Surgery.
- Currently, more than 10,000 physicians are believed to be practicing wound care, with family physicians and internists responsible for 35% of the providers.
Family physicians are called upon to respond to a wide array of patient problems from obesity to diabetes to breast cancer. The challenges are great and, in most cases, residency training equips physicians to address these problems. However, one area in which residency may not have done the job — or that’s what the evidence suggests — is wound care. An examination of the average four-year medical school curriculum found that only 9.2 hours of formal didactic training in wound care were offered, while specialties that claim the field of wound care give only scant attention to the field.1 Although a single article cannot provide the ever-expanding body of knowledge that is today’s wound care, this article will summarize its salient features, including demographics of a changing population, fundamental phases of wound healing, advances in therapeutic modalities, and steps family physicians can take to become recognized as certified wound care physicians.
The Demographics of Wound Care
Patient demographics are signals of change. The ways people live, move, and work are producing wounds that require specialized care by a physician able to provide the full scope of medical services.
The incidence of non-healing cutaneous wounds is 5 to 7 million per year in the United States. It is estimated that this clinical volume results in more than a $25 billion cost to the healthcare system. Wound healing has become a complex process that involves the coordinated integration of numerous clinical and biochemical pathways. The replacement of injured or damaged tissue can be compromised by multiple factors, including, but not limited to, obesity, diabetes, smoking, vascular disease, infection, renal failure, cancer, malnutrition, and offloading. A classic example of a non-healing wound is a diabetic foot ulceration. With peripheral neuropathy and frequently concomitant peripheral vascular disease, chronic ulcers can form easily in this ever-expanding population. With an estimated 36 million diabetic patients expected by 2030, primary care physicians can expect to see an increasing number of patients with chronic, non-healing wounds in the future. With an aging society, it is also expected that there will be an increase in the number of surgical wounds, pressure wounds, venous leg ulcerations, and traumatic wounds that will be at risk for non-healing. Complicating the situation is the lack of formal education on the science and treatment of non-healing wounds for physicians, nurses, therapists, and all ancillary healthcare providers.2
Advances in the Field of Wound Care
The age of modern wound care has ushered in new modalities of care in which physicians need to be educated and trained beyond the first professional degree.
Although wound care has been practiced for hundreds of years, it has been only during the past 45 years that the age of “modern wound care” has flourished. British researcher George D. Winter’s 1962 seminal paper in Nature on moist healing catalyzed a radical shift from the passive gauze therapy that was promoted at the time. However, the fear of promoting wound infections using occlusive dressings delayed the emergence of commercially available wound products (dressings) until the late 1970s. Hydrocolloid dressings were released in 1982, and nurses became early adopters of the treatment. Physical therapists provided a slightly different approach to wound healing, using energy-based modalities such as ultrasound, electrical stimulation, ultraviolet light, compression therapy, and manual lymphedema treatments.
The development of autologous platelet gel increased recognition of advanced wound care to clinicians. Virtually all modalities lacked substantive evidence of efficacy from well-designed, carefully conducted, prospective, randomized clinical trials, and many products were developed under 510K regulatory status that allowed marketing without rigorous evidence or clinical trials.
The first recombinant growth factor (Becaplermin) for chronic wounds along with bioengineered tissues (Apligraf, Dermagraft) brought biotechnology to the field of wound care. Increasingly, regenerative medicine will be applied to wound care, producing even more stunning results. Modern wound care centers, as well as a limited number of transitional care hospitals, were established to provide a central area of diagnosis and management of patients with complex wounds.3
The Science of Wound Healing
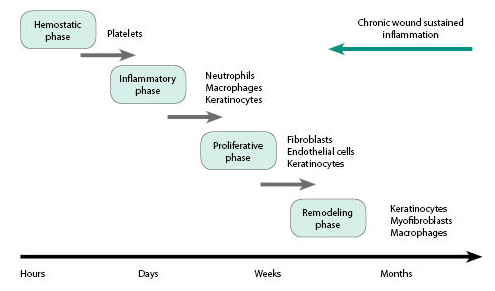
Wound healing is a normal biological process. This process proceeds through four precise, highly programmed, overlapping phases: hemostasis, inflammation, proliferation, and remodeling. Proper sequence, at a specific time and continuing for a specific duration at an optimal level of intensity, will ensure the healing process. The specific aspects of the wound healing process gleaned from recent research are listed below. (See Figure 1.)
Figure 1. Stages of Wound Healing |
 |
Phase I
The hemostasis phase begins immediately after wounding. The platelets clot along with vasoconstriction to stop the bleeding, and surrounding wound tissue releases pro-inflammatory cytokines and growth factors, such as transforming growth factor-β, platelet-derived growth factor, fibroblast growth factor, and epidermal growth factor.
Phase II
When bleeding is under control, inflammatory cells migrate into the wound and promote the inflammatory phase, which is characterized by the sequential infiltration of neutrophils, macrophages, and lymphocytes. Neutrophils clear the wound of invading microbes and cellular debris. Early on, macrophages release cytokines that promote the inflammatory response by recruiting and activating additional leukocytes, and also they are responsible for inducing and clearing apoptotic cells, thereby paving the way for the resolution of inflammation. As macrophages remove dying cells, they undergo a transition to a reparative state that stimulates keratinocytes, fibroblasts, and angiogenesis to promote tissue regeneration. Macrophages then promote the transition to the proliferative phase of healing.
Phase III
Following and overlapping the inflammatory phase, the proliferative phase is characterized by epithelial proliferation and migration over the provisional matrix within the wound. In the reparative dermis, fibroblasts and endothelial cells are the most prominent cell types present. They support capillary growth, collagen formation, and the formation of granulation tissue at the site of injury. Fibroblasts produce collagen in the wound bed as well as glycosaminoglycans and proteoglycans, which are major components of the extracellular matrix (ECM).
Phase IV
At this point, wound healing enters the final remodeling phase, which can last for years. Regression of many of the newly formed capillaries occurs during this phase, so that vascular density of the wound returns to normal. One critical feature of the remodeling phase is ECM remodeling to an architecture that approaches that of the normal tissue. The wound also will undergo contraction, which is believed to be mediated by contractile fibroblasts that appear in the wound.
The complexity and coordination of the healing process are major hurdles to therapeutic approaches, since any therapeutic intervention must be sequenced effectively to the appropriate healing phase.4
Impairment of Wound Healing
Although the wound will progress through its healing phases, certain factors will impede the progress. Each of the factors that impair the healing process will be discussed and annotated below. However, it may be helpful to note that the most frequently seen wounds are venous, diabetic, arterial, pressure, and surgical. (See Figures 2, 3, and 4.)
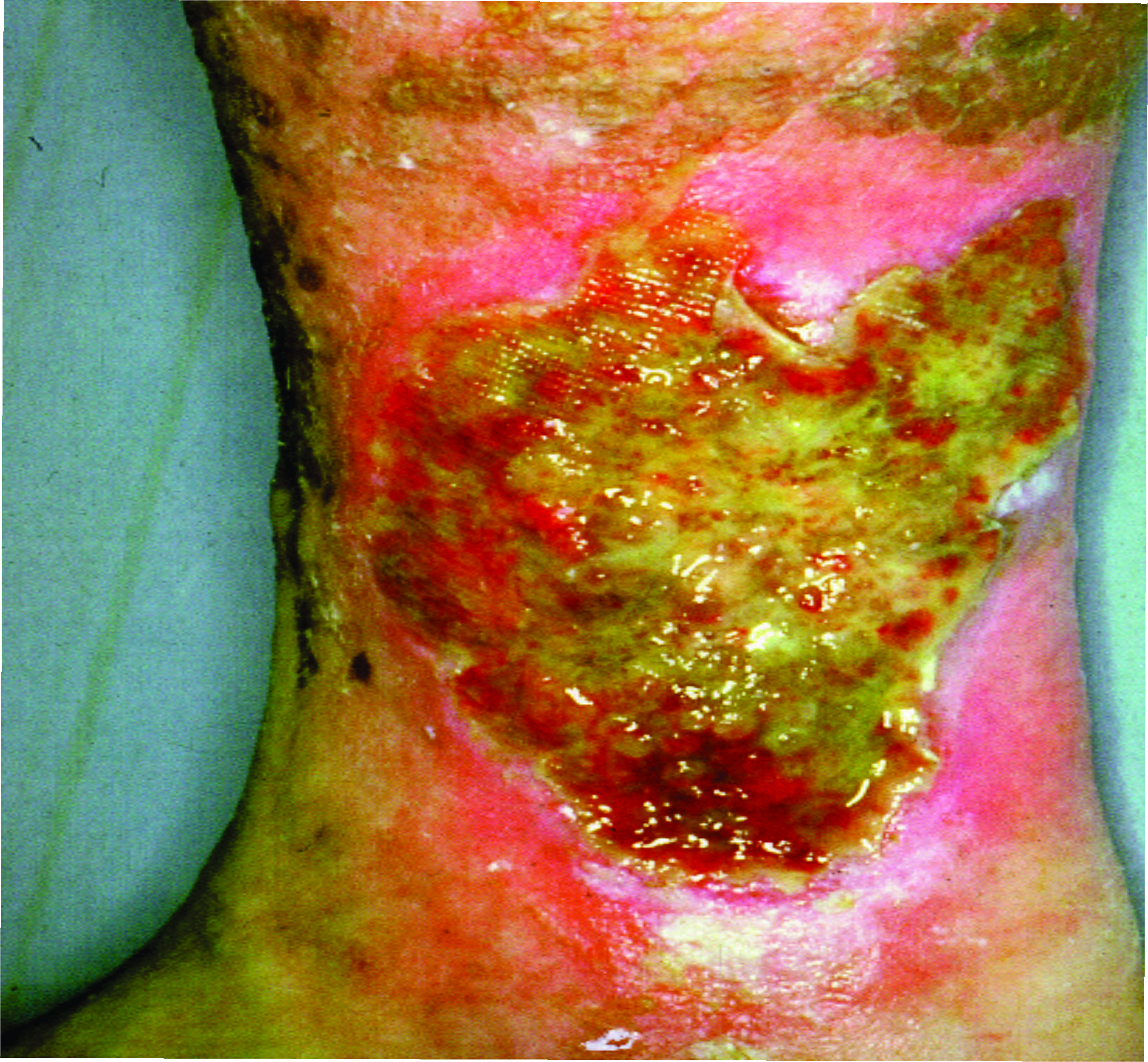
Figure 2. Venous Wound |
 |
|
Photo courtesy of Richard Simman, MD |
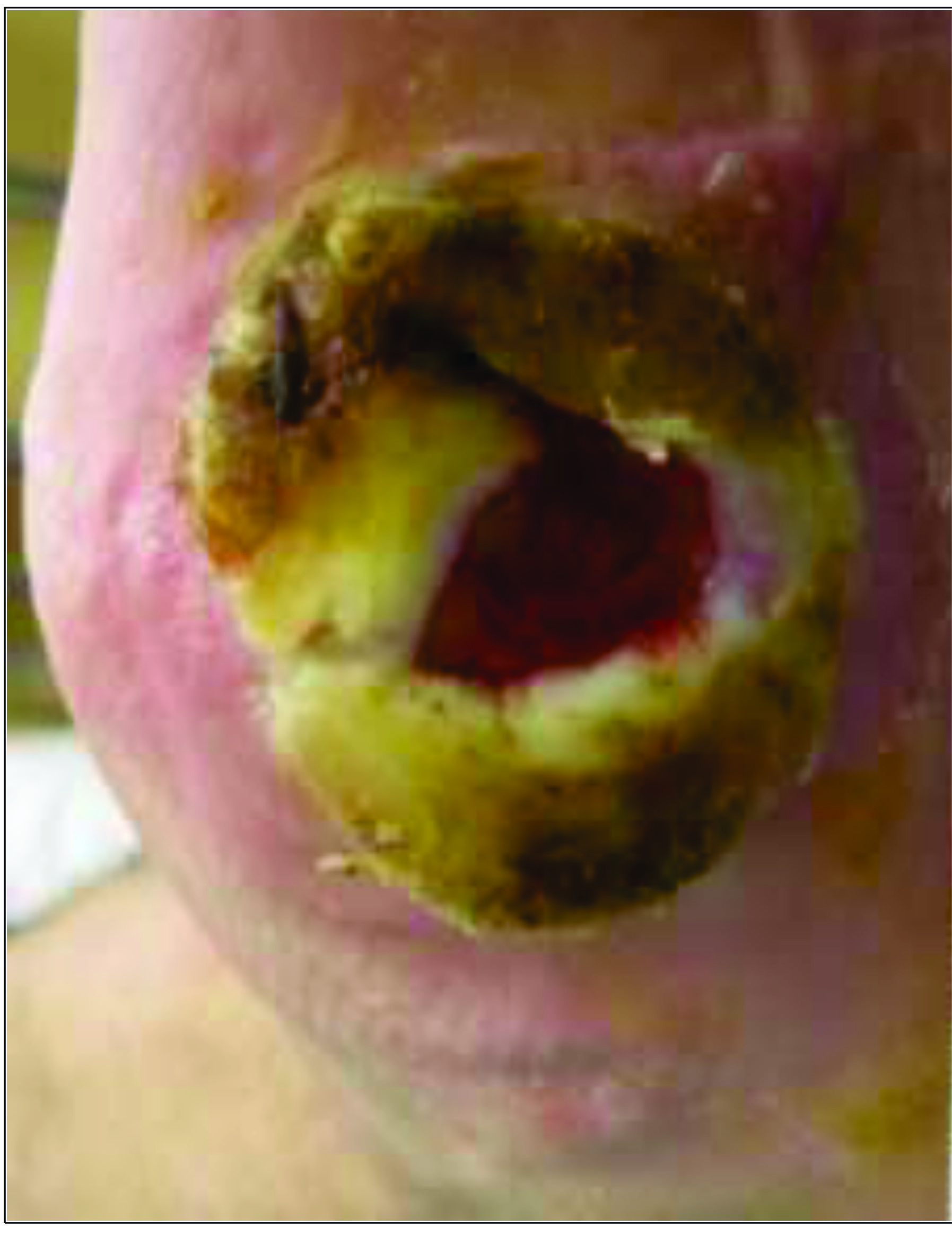
Figure 3. Diabetic Wound |
 |
|
Photo courtesy of Richard Simman, MD |
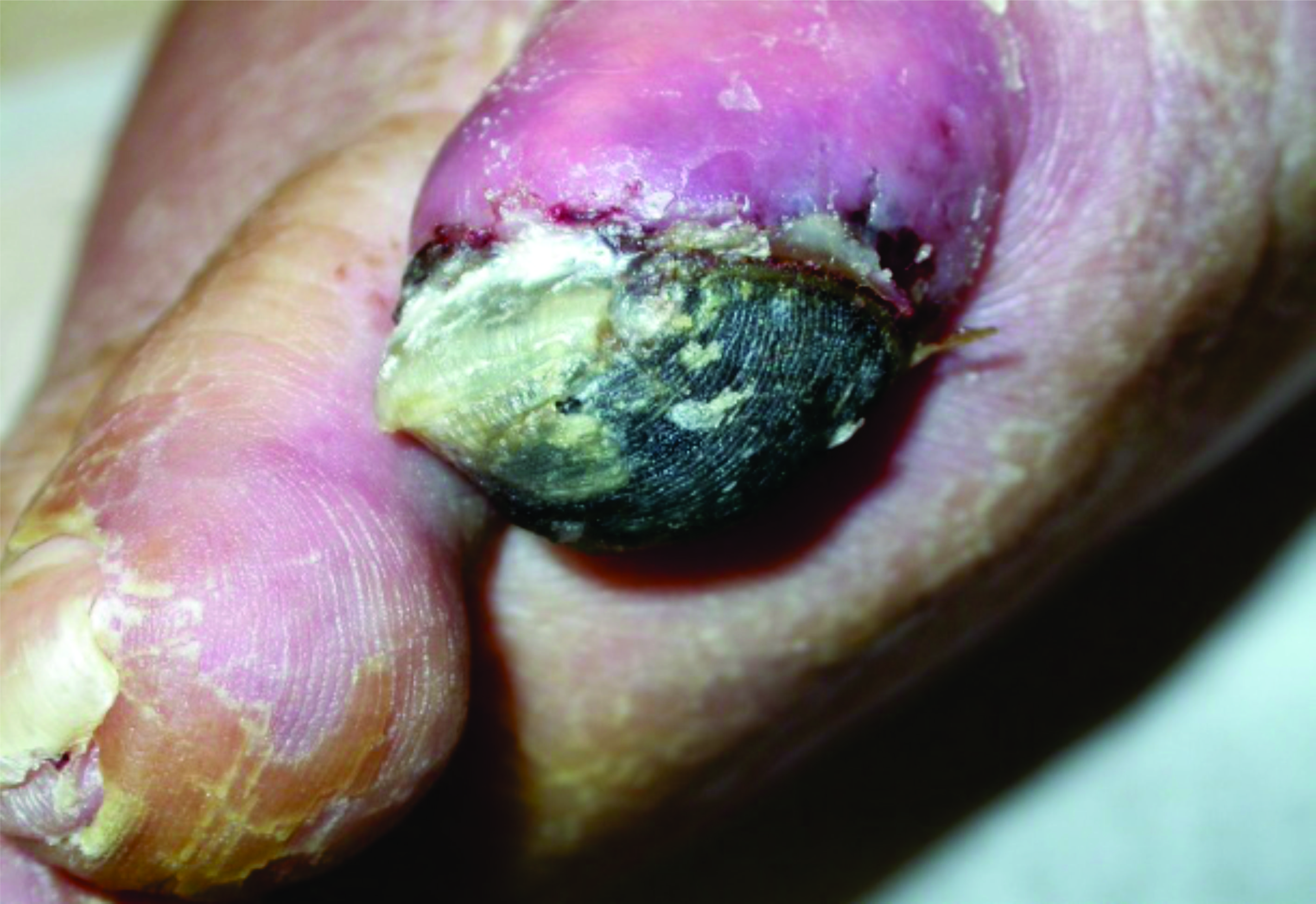
Figure 4. Arterial Wound |
 |
|
Photo courtesy of Richard Simman, MD |
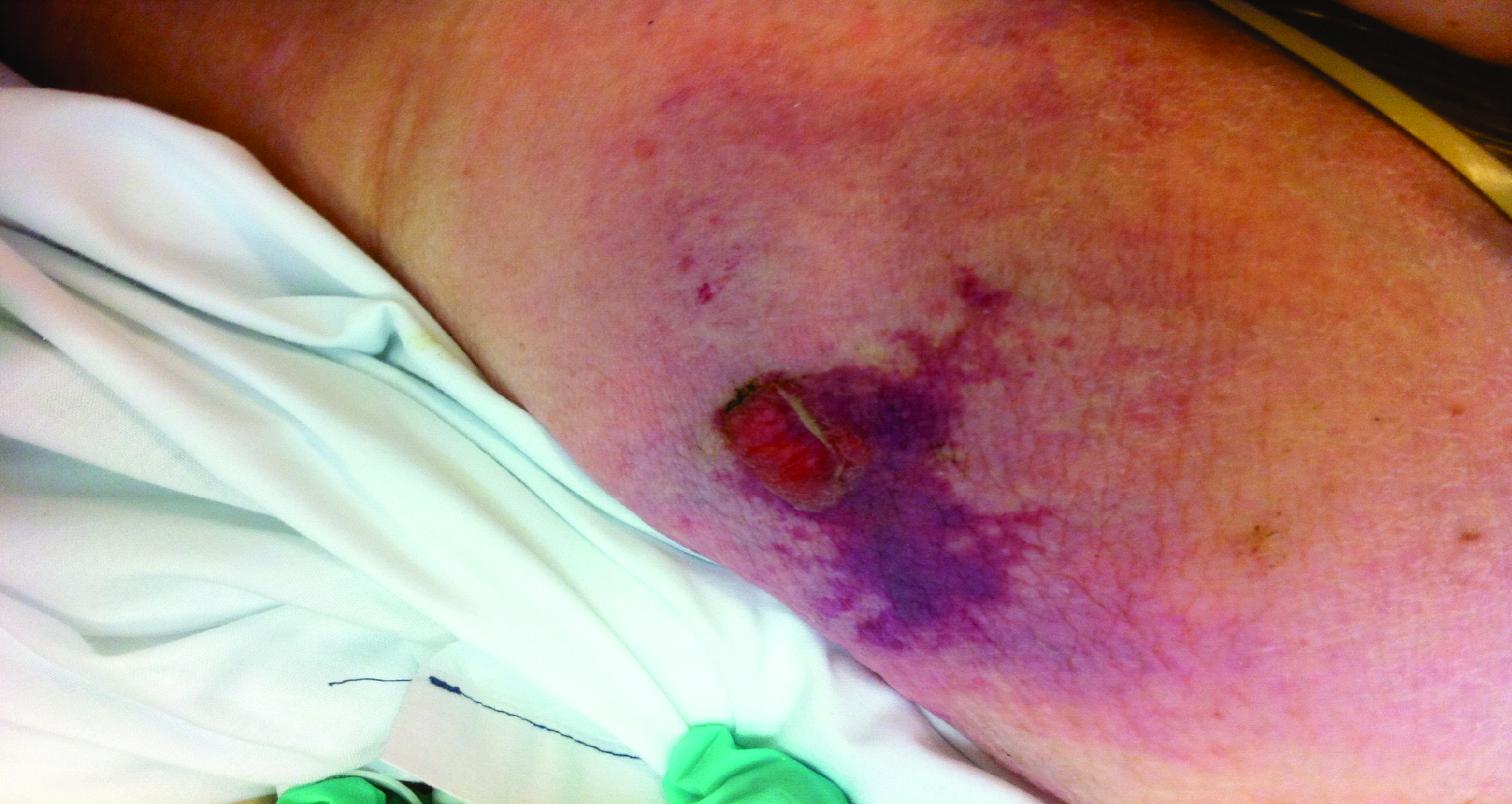
Less common and more difficult to diagnose are atypical or unusual wounds. (See Figures 5, 6, and 7.) Physicians should be familiar with these and be able to treat them once diagnosed. These types of wounds result from malignancies, infections, medications, vasculitis and rheumatologic syndromes, necrobiosis lipoidica diabeticorum, pyoderma gangrenosum and systemic inflammatory disease, thrombotic diseases (idiopathic thrombocytopenic purpura), blood disorders (e.g., sickle cell anemia), radiation tissue injury, calciphylaxis, insect bites, animal and human bites, trauma, burns, and factitious disorders.5
Figure 5. Calciphylaxis Atypical Wound, Early Stage |
 |
|
Photos courtesy of Richard Simman, MD |
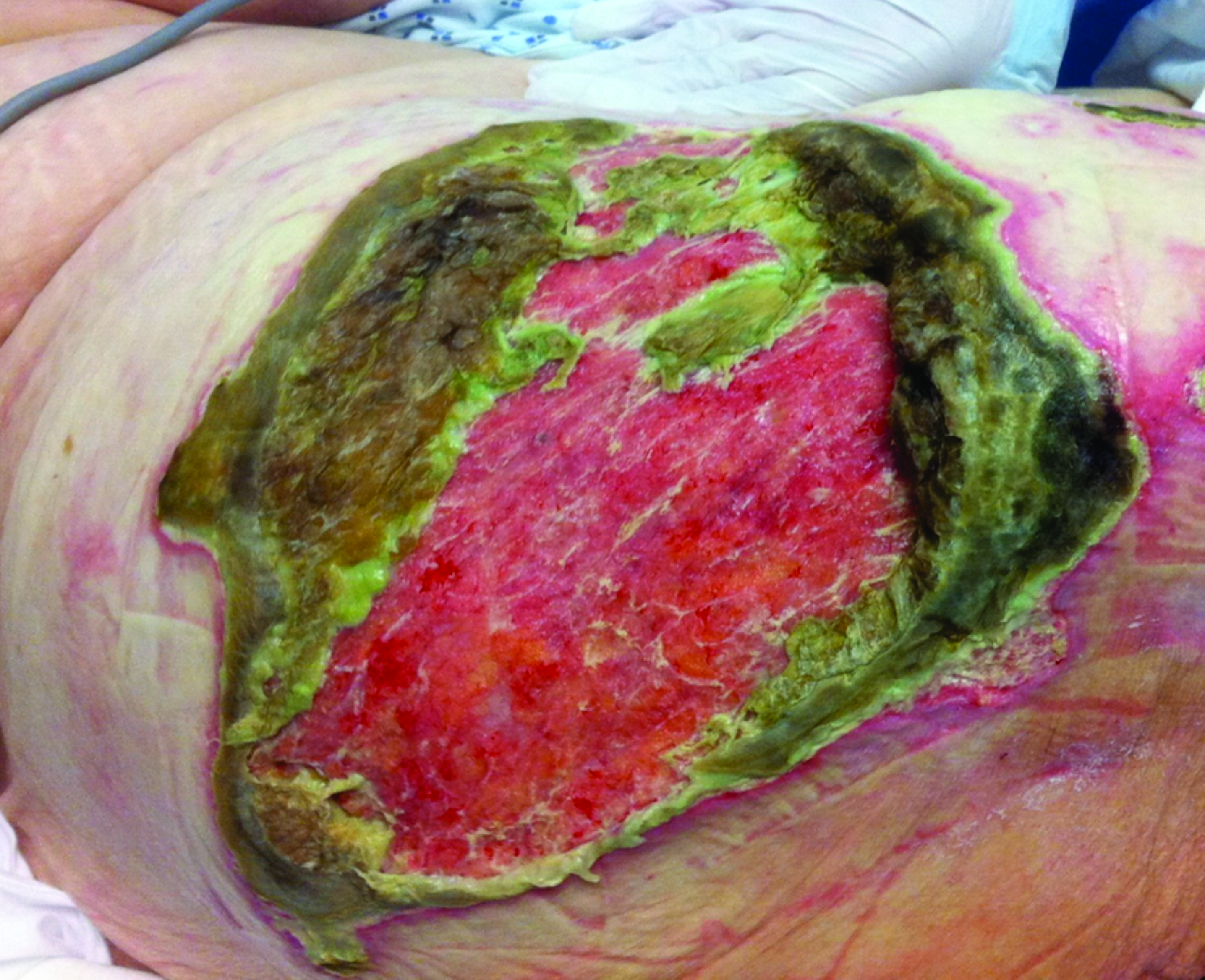
Figure 6. Calciphylaxis Atypical Wound, Later Stage After Debridement |
 |
|
Photos courtesy of Richard Simman, MD |
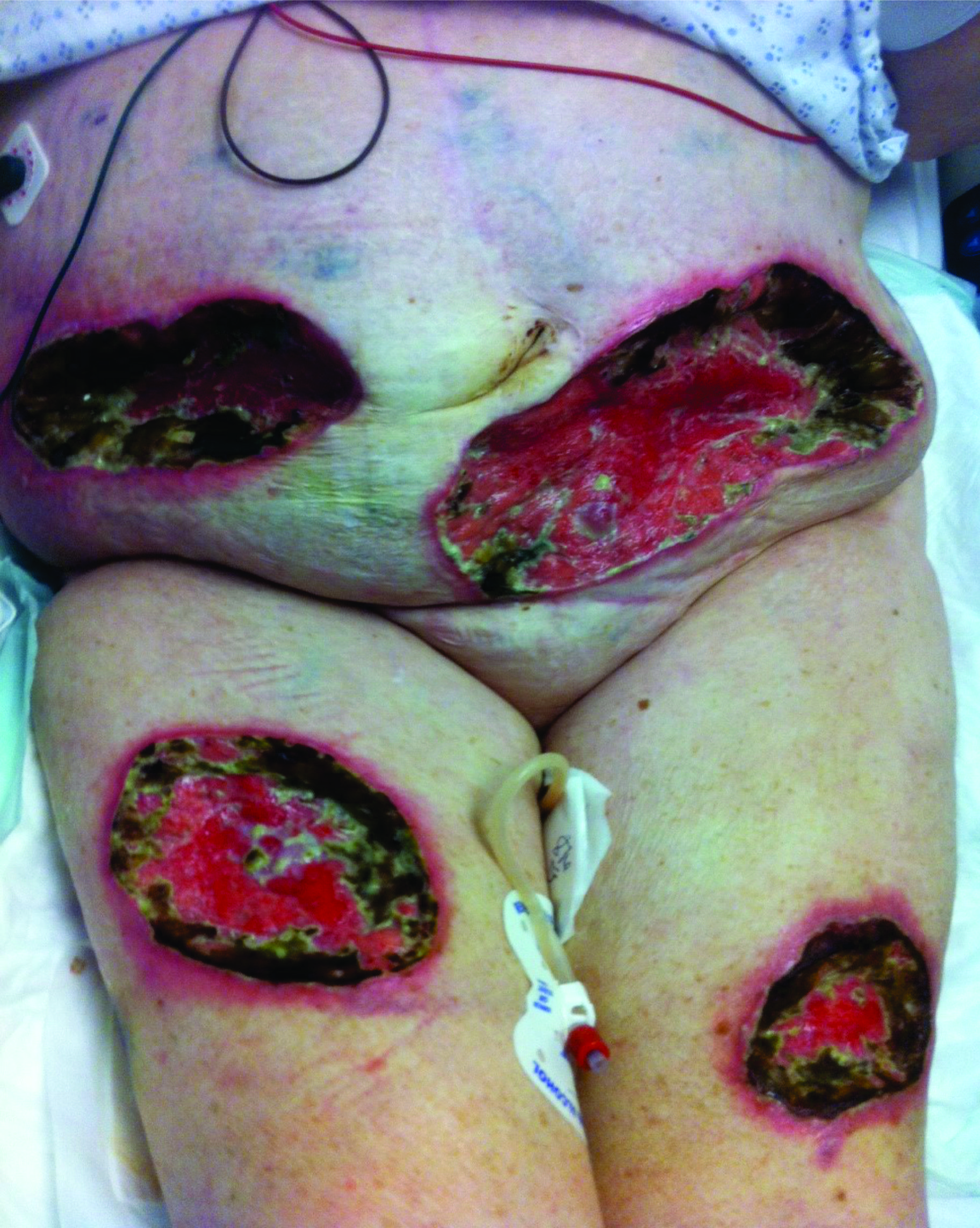
Figure 7. Calciphylaxis Atypical Wound, Later Stage After Debridement |
 |
|
Photos courtesy of Richard Simman, MD |
Local Factors
Oxygenation
Although oxygen is essential for wounds to heal, several factors can reduce oxygen to the wound locally. For example, vascular disruption or high oxygen consumption by other cells is a significant factor. All chronic wounds are hypoxic and healing is impaired. Hyperbaric oxygen therapy is an option frequently employed for patients with tissue hypoxia.
Infection
Inflammation is a normal part of the wound-healing process when skin is injured. Microorganisms are sequestered at the skin level and obtain access to the underlying tissues. While they are a cause for inflammation, they are important for the removal of contaminating microorganisms. However, in the absence of effective decontamination, inflammation may be prolonged, since microbial clearance is incomplete. Both bacteria and endotoxins can lead to the prolonged elevation of pro-inflammatory cytokines, such as interleukin, and elongate the inflammatory phase. Compared with aged females, aged males have been shown to have delayed healing of acute wounds. Estrogen affects wound healing by regulating a variety of genes associated with regeneration, matrix production, protease inhibition, epidermal function, and the genes primarily associated with inflammation. Sex hormones play an important role in age-related wound healing.6
Offloading
Any process in which pressure on the appendage is reduced is called offloading. It will prevent the development of chronic wounds and will accelerate the progression of the normal wound-healing process. Offloading is particularly helpful for patients with prolonged tissue ischemia and permanent occlusion of capillaries seen in bedridden patients, diabetic patients, and paraplegic and quadriplegic patients. Offloading is used most commonly in diabetic wounds and can be achieved through a variety of measures, from diabetic foot care options, such as shoes or socks that disperse normal pressure points in the foot, to the use of a wheelchair, scooter, or other device that minimizes the amount of weight that is put on the foot.7
Systemic Factors
Age
People older than 60 years of age represent the fastest growing segment of the U.S. population. Increased age is a major risk factor for impaired wound healing. It commonly is recognized that in healthy older adults, the effect of aging causes a temporal delay in wound healing, but not an actual impairment in terms of the quality of healing. Exercise is reported to improve cutaneous wound healing in older adults as well as aged mice, and the improvement is associated with decreased levels of pro-inflammatory cytokines in the wound tissue.
Stress
Psychological stress causes a substantial delay in wound healing, according to studies in both humans and animals. Stressors can lead to negative emotional states, such as anxiety and depression, which in turn may have an effect on physiologic processes and/or behavioral patterns that influence health outcomes. In addition to the direct influences of anxiety and depression on endocrine and immune function, stressed individuals are more likely to have unhealthy habits, which include poor sleep patterns, inadequate nutrition, less exercise, and a greater propensity for abuse of alcohol, cigarettes, and other drugs. These factors may come into play in negatively modulating the healing response. Numerous studies have confirmed that stress-induced disruption of neuroendocrine immune equilibrium is consequential to health. The pathophysiology of stress results in the deregulation of the immune system, mediated primarily through the hypothalamic-pituitary-adrenal and sympathetic-adrenal medullary axes or sympathetic nervous system.8
Diabetes
There is no question that diabetes significantly impairs the healing of acute wounds. Moreover, this population is prone to develop chronic non-healing diabetic foot ulcers, which are estimated to occur in 15% of all persons with diabetes. Diabetic foot ulcers are a serious complication of diabetes, and precede 84% of all diabetes-related lower leg amputations. The impaired healing of both diabetic foot ulcers and acute cutaneous wounds in persons with diabetes involves multiple complex pathophysiological mechanisms. Like venous stasis disease and pressure-related chronic non-healing wounds, diabetic foot ulcers are always accompanied by hypoxia. A situation of prolonged hypoxia, which may be derived from both insufficient perfusion and insufficient angiogenesis, is detrimental for wound healing. Hypoxia can amplify the early inflammatory response, thereby prolonging injury by increasing the levels of oxygen radicals.9
Medications
A significant number of medications have the capacity to affect wound healing. These medications are those that interfere with clot formation or platelet function, or inflammatory responses and cell proliferation. Glucocorticoid steroids, nonsteroidal anti-inflammatory drugs, and chemotherapeutic drugs commonly are used and have a significant adverse effect on the healing process.10
Lifestyle Factors
Obesity
More than 30% of adults and 15% of children and adolescents are classified as obese, according to a recent survey by the Centers for Disease Control and Prevention. Obesity is well-known to increase the risk of many diseases and health conditions, including coronary heart disease, type 2 diabetes, cancer, hypertension, dyslipidemia, stroke, sleep apnea, respiratory problems, and impaired wound healing. Obese individuals frequently face wound complications, including skin wound infection, dehiscence, hematoma and seroma formation, pressure ulcers, and venous ulcers.11
Alcohol
Clinical studies and animal studies have shown that exposure to alcohol impairs wound healing and increases the incidence of infection. Alcohol exposure diminishes host resistance, and ethanol intoxication at the time of injury is a risk factor for increased susceptibility to infection in the wound. Studies have demonstrated profound effects of alcohol on host-defense mechanisms, although the precise effects are dependent on the pattern of alcohol exposure. A recent review on alcohol-induced alterations on host defense after traumatic injury suggested that, in general, short-term acute alcohol exposure results in suppressed pro-inflammatory cytokine release in response to an inflammatory challenge. The higher rate of post-injury infection correlates with decreased neutrophil recruitment and phagocytic function in acute alcohol exposure.12
Smoking
Smoking increases the risk of heart and vascular disease, stroke, chronic lung disease, and many kinds of cancers. Similarly, the negative effects of smoking on wound-healing outcomes have been known for a long time. Postoperatively, patients who smoke show a delay in wound healing and an increase in a variety of complications, such as infection, wound rupture, anastomotic leakage, wound and flap necrosis, epidermolysis, and a decrease in the tensile strength of wounds. Cosmetic outcomes also appear to be worse in smokers, and plastic and reconstructive surgeons often are reluctant to perform cosmetic surgeries on individuals who refuse to quit smoking. Research has identified more than 4,000 substances in tobacco smoke that have a negative effect on healing.13
Nutrition
Nutrition has been recognized for more than 100 years as an important factor that affects wound healing. Most obvious is that malnutrition or specific nutrient deficiencies can have a profound effect on wound healing after trauma and surgery. Patients with chronic or non-healing wounds who are experiencing nutrition deficiency often require special nutrients. Deficits in energy, carbohydrates, protein, fat, vitamins, and mineral metabolism all can affect the healing process.14
Regenerative Medicine
Although exciting advances have been made in the field of regenerative medicine, many non-wound therapies are under development that hold a great deal of relevance to wound healing because of similarities in signaling and cell development pathways. Big data (for example, genomics, proteomics, and electronic medical record analyses) are informing basic research and population health management. These developments are likely to enhance our understanding of the pathophysiology of wounds and speed the dissemination of successful regenerative strategies throughout different areas of medicine.
As noted, chronic wounds (e.g., venous, diabetic, and pressure ulcers) are difficult to heal and cause much human suffering. Complications include infection, pain, amputation, and even death. Although many advanced therapies help a portion of patients, many remain unhealed after treatment. Regenerative medicine strategies may hold the potential to restore tissue, perhaps equaling or exceeding predamage levels, resulting in improved outcomes and quality of life.
The role of stem cells in cutaneous wound healing and tissue regeneration has received significant research attention, with a focus on the role of adult stem cells, such as epidermal stem cells and bone marrow-derived cells. Epidermal stem cells reside in the bulge area of hair follicles and the basal layer of the epidermis, and give rise to the keratinocytes that migrate to epithelialize wounds. Two stem cell populations are present in the bone marrow: hematopoietic and mesenchymal stem cells. Bone marrow-derived cells are able to differentiate into a variety of cell types, including adipocytes, osteoblasts, chondrocytes, fibroblasts, and keratinocytes. Endothelial progenitor cells derived from the hematopoietic stem cell lineage are key cells that contribute to neovascularization. Both types of stem cells are involved in the cutaneous wound healing process. Wound-induced hypoxia triggers the mobilization of bone marrow endothelial progenitor cells to the circulation, playing a significant role in the process of neovascularization.15
New and Advanced Therapeutic Modalities
Many different products have been developed to influence this wound environment to provide a pathogen-free, protected, and moist area for healing to occur. Newer products currently are being used to replace or augment various substrates in the wound healing cascade. The next section discusses the latest applications of silver in microbial prophylaxis and treatment, including issues involving resistance and side effects, the latest uses of negative pressure wound devices, advanced dressings and skin substitutes, biologic wound products including growth factor applications, and hyperbaric oxygen as an adjunct in wound healing. With the abundance of available products, the goal is to find the most appropriate modality or combination of modalities to optimize healing.
Silver
Developed and introduced in the late 1990s, nanocrystalline silver dressings are the latest forms of silver wound dressings. These products were designed to overcome some of the shortcomings of previous silver dressings. The typical products currently in use contain two layers of high-density polyethylene net sandwiching a layer of rayon/polyester gauze. The outer layer is coated with a nanocrystalline (< 20 nm), noncharged form of silver (Ag0), and the inner layer helps maintain a moist environment for wound healing. Aside from a more consistent therapeutic dose of silver, an additional benefit of nanocrystalline dressings is less frequent dressing changes, on the order of days as compared to standard, twice-daily dressing changes for silver sulfadiazine and up to 12 times per day for silver nitrate. This decreases patient discomfort as well as provides less disruption to the healing wound bed.16
Negative Pressure Wound Devices
Although negative pressure wound devices (NPWD) have undergone some minor advances in technology, the most significant changes have come from the indications for use. Advances in the actual devices include smaller size, allowing for portable units for home use, increased ability to remove large amounts of fluid, the ability to instill fluids in the wound for continuous irrigation, refinements in the foam with more consistent pore sizes, different sponge materials including silver, and increased safety and alarm systems. Acute wounds now are being treated more frequently with NPWD closure. In patients with significant comorbidities or other serious injuries, NPWDs can be used in large soft-tissue injuries, contaminated wounds, and wounds with compromised tissue. These also are being used immediately after split-thickness skin grafts to protect the grafts and prevent their displacement.17
Advanced Dressings
Although plain gauze is still the most commonly used dressing in hospitals today, new wound understanding and technologies have produced advanced products that help the body achieve the ideal moist, warm, protected wound healing environment. Plain gauze certainly has its place, as it is inexpensive, readily available, and appropriate for many wounds. Impregnated gauze improves on this by adding zinc, iodine, or petrolatum to help prevent desiccation and provide nonadherent coverage.
The process of autolysis (i.e., the breaking down of cells or tissues by their own enzymes) is important in wound care. If an occlusive dressing is provided as a barrier to the outside environment, the body’s own phagocytic processes will provide debridement of wounds. These products range from occlusive films such as Tegaderm, which are permeable to air and water vapor but impermeable to fluid and microorganisms, to hydrocolloids such as DuoDERM, which are also occlusive but provide absorption of exudates in addition to maintaining a moist environment for autolysis. For heavily exudative wounds, there are a range of absorptive products, including various hydrophilic foam dressings, hydrofibers, and alginates, which can absorb up to 20 times their weight. Although these products are more expensive than traditional gauze, recent studies seem to indicate an overall cost savings due to decreased labor costs: Advanced dressings typically are changed every one to three days, as opposed to gauze, which often is changed multiple times per day. Additionally, faster healing times from advanced dressings mean an overall decreased treatment period.18
Skin Substitutes
Bioengineered skin substitutes, both biosynthetic skin substitutes and cultured autologous engineered skin, are available to provide temporary or permanent coverage, with the advantages of availability in large quantities and negligible risk of infection or immunologic issues. The main limitation of these products is their expense. This section will discuss currently available products as well as some products that may confer an advantage over autologous tissue in terms of potential for wound healing in chronic wounds. Available products include the following:
- Biobrane is a temporary dressing composed of knitted nylon mesh bonded to a thin silicone membrane and coated with porcine polypeptides.
- TransCyte is a biosynthetic dressing of a semipermeable silicone membrane on a nylon mesh coated with porcine collagen and newborn human fibroblast cells.
- Dermagraft contains cryopreserved neonatal fibroblasts on a bioabsorbable polyglactin mesh. The fibroblasts produce dermal collagen, glycosaminoglycans, growth factors, and fibronectin to support wound healing.
- Apligraf is composed of an epidermal layer of allogeneic neonatal keratinocytes and fibroblasts from neonatal foreskin on bilayered type I bovine collagen that may be used as an adjunct covering to autograft, providing accelerated healing times.
- Integra is a semi-biologic bilayered dressing composed of a matrix of type I bovine collagen, chondroitin-6-sulfate, a glycosaminoglycan from shark cartilage, under a temporary silicone epidermal sheet.
- The human amniotic membrane allographs Grafix and EpiFix are recent products that can restart the healing process of a chronic or stalled wound to allow progression through the phases of normal would healing. Grafix® (Osiris Therapeutics, Inc., Columbia, MD), a human viable wound matrix, is designed to preserve the native components of the human placental membrane in a cryopreserved product that can be used on demand at point-of-care. Likewise, EpiFix (EpiFix®, MiMedx, Kennesaw, GA) is the dehydrated form.
Growth Factors and Biologic Wound Products
Biologic wound products have been an area of tremendous growth as our understanding of the details of the wound healing response has increased. In normal wound healing, as noted earlier, there is an orderly, predictable sequence passing through the inflammatory, proliferation, and remodeling phases. This process is driven by numerous cellular mediators. The field of biologic wound products aims to accelerate healing by augmenting or modulating these inflammatory mediators. While most investigations on these substances are small laboratory studies, there are some clear benefits seen in clinical investigations.
Growth factors stimulate mainly fibroblasts and keratinocytes via transmembrane glycoproteins. They have been studied more than any other biologic wound supplement. They are divided into five superfamilies, the most familiar being the platelet-derived growth factors. Regranex is the only current FDA-approved product in the growth factor family. Additional studies have confirmed increased odds of wound healing and decreased rates of amputation in diabetic foot ulcers, as well as accelerated wound healing in abdominal wound separation and irradiated wounds.19
The field of wound care is expanding with advances in technology. Although there is still no superior substitute for reconstruction using patients’ own tissues and carefully thought out reconstructive procedures, new products can help facilitate eventual healing by providing prophylaxis against barriers to healing, augmenting wound healing factors, assisting in temporizing and bridging time to definitive repair, and optimizing the ultimate results of wound reconstruction.
American Board of Wound Medicine and Surgery
In 2011, a group of wound care physicians established the American Board of Wound Medicine and Surgery (ABWMS). Its mission is to enhance the quality of available care by offering board certification in wound medicine and surgery to physicians in the United States and Canada. Certification is based on meeting required qualifications (i.e., certified by a recognized primary medical board like the American Board of Family Medicine or the American Board of Surgery), passing a written exam, and demonstrating a commitment to the care and management of patients with wounds.
Since the late 1990s, the American Board of Medical Specialties (ABMS) has been emphatic that it would not create any new medical or surgical specialties, thereby obligating organizations like the ABWMS to seek subspecialty recognition. To become a subspecialty recognized by the ABMS, a special area of clinical practice like wound care must be “adopted” by an established medical or surgical specialty board that is already recognized by the ABMS. In most cases, the adoption is based upon the “relatedness” of this special area of practice to the body of knowledge tested by the ABMS recognized board. As an ABMS recognized subspecialty, the field of wound care will become a valid and formally recognized field of medicine and consequently its legitimacy will be assured. In many ways, becoming a subspecialty is a meaningful advantage for patients.
Despite the reluctance of the ABMS to recognize new specialty areas, palliative medicine and hyperbaric medicine recently have been designated as subspecialties by a number of ABMS member boards. For example, palliative medicine initially was recognized by the American Board of Surgery and nine additional boards. Likewise, the Preventive Medicine and Emergency Medicine Boards designated hyperbaric medicine as a subspecialty. The organization currently representing hyperbaric oxygen therapy physicians is the Undersea and Hyperbaric Medicine Society.
Education and training are essential requirements for the physician practice of wound medicine and surgery. The ABWMS considers it essential that sometime in the near future all physicians who seek certification in wound care must complete a 12-month formal education and training regimen or fellowship. Toward that end, the board has prepared a model core curriculum. However, until more physicians are certified by examination, it will be difficult, if not impossible, to nurture the field by imposing a fellowship program on practicing physicians. For this reason, the board foresees that in the short term, perhaps five to seven years, physicians without fellowship training will need to become certified as a means to initially build up the discipline.
Finally, it is the plan of the board, that once the ABMS accredits wound medicine and surgery as a subspecialty, the ABWMS will seek the endorsements of other primary boards, such as family medicine, emergency medicine, physical medicine and rehabilitation, and infectious disease, as a means of encouraging these boards to incorporate formal training in wound care.20
What Is Being Done to Ensure Quality Wound Care?
As the field of wound care matures, there is a critical need for rigorous training, research, evidence development, and advocacy to improve outcomes of patients with non-healing wounds. As mentioned, presently physicians receive only limited formal education concerning the diagnosis and treatment of wounds in either their pre- or postgraduate medical education. Many physicians, depending on residency training, will not receive any further information about wound care throughout their career. When a wound care center opens in a hospital, members of the existing medical staff frequently are invited to participate and often receive less than one week of didactic training before working in the center. Although this training is a considerable improvement in the current conditions, it still is a far cry from formal residency and fellowship-based medical education.
General and plastic surgeons are trained to manage acute wounds, but not chronic wounds. No formal time is allocated in their residencies’ core curriculum to manage these complicated chronic wounds.
More than 10,000 physicians are believed to be practicing wound care. Many of these physicians are not educated or trained to perform the full range of wound care services available today for their patients. Consequently, the quality of care can suffer and costs are not contained.
Over the years, several organizations have sprung up to certify physicians in wound care. Some of these certifications can be obtained through an online course and test; others try to document knowledge yet do not measure up to standards to which physicians have become accustomed. Others offer certification after the completion of a rigorous examination, but because these organizations accept practitioners from multiple disciplines, they cannot secure the appropriate recognition physicians need, namely, certification by a board recognized by the ABMS, the gold-seal of medical boards, as in the case of American Board of Surgery, American Board of Family Medicine, and others.
Physicians spanning the spectrum from emergency medicine to infectious disease to physical medicine to family medicine are the primary providers of wound care. Yet, none of them receive the needed training in their formal educational programs, and the training they receive often is fragmented and limited in scope. Interestingly, data from Healogics Inc., the largest outpatient wound care management company in the world with more than 650 wound centers and staffed with 3,000 physicians, strongly indicate that the majority of wound care providers are not surgeons:
- Family medicine: 24%
- General surgery: 20%
- Podiatry: 15%
- Internal medicine: 11%
- Cardiovascular/thoracic: 8%
- Miscellaneous (vascular surgeons, plastic surgeons, emergency medicine): 22%.21
CONCLUSION
Wound care is a burgeoning field of study and practice and one into which increased numbers of physicians will enter. The field will be driven by new advances in knowledge and therapeutic modalities, calling on the medical community to ensure the field is recognized and accredited as a subspecialty with training requirements like any other subspecialty. In fact, physicians have come late to the field led historically by nurses. Because the field is dynamic and complex, physicians must play an ever-increasing role in its promotion and practice. Although this article has not exhausted the study, it has provided basic and current information about advances in the field, new ways to treat patients, and steps physicians can take to enhance their practices in the care of wounds.
REFERENCES
- Patel NP, Granick M, Kanakans N, et al. Comparison of wound education in medical schools in the United States, United Kingdom, and Germany. ePlasty 2008;8:8.
- Guo S, DiPietro LA. Factors affecting wound healing. J Dent Res 2010;89:219-229.
- Simman R, Fleck C. Modern collagen wound dressings: Function and purpose. J Am Col Certif Wound Spec 2011;2:50-54.
- Simman R. Wound closure and the reconstructive ladder in plastic surgery. J Am Col Certif Wound Spec 2009;1:6-11.
- Shukla D, Tripathi AK, Agrawal S, et al. Pain in acute and chronic wounds: A descriptive study. Ostomy Wound Manage 2005;51:47-51.
- Halim AS, Khoo TL, Saad AZ. Wound bed preparation from a clinical perspective. Indian J Plast Surg 2012;45:193-202.
- Sinacore DR, Mueller MJ. Off-loading for diabetic foot disease. In: Bowker JH, Pfeibert MA, eds. The Diabetic Foot. 7th ed. Philadelphia: Mosby/Elsevier; 2008: 287-304.
- Graham JE, Christian LM, Kiecolt-Glaser JK. Marriage, health, and immune function: A review of key findings and the role of depression. In: Beach S, Wambolt M, eds. Relational Processes and DSM-V: Neuroscience, Assessment, Prevention and the Treatment. Washington, DC: American Psychiatric Publishing; 2006: 61-76.
- American Diabetes Association. Statistics About Diabetes. Available at: http://www.diabetes.org/diabetes-basics/statistics/. Accessed June 12, 2017.
- Rosenberg L, De la Torre J. Wound healing, growth factors; phases of wound healing. Plast Surg 2006;457:3-6.
- Wagner IJ, Szpalski C, Allen RJ Jr, et al. Obesity impairs wound closure through a vasculogenic mechanism. Wound Repair Regen 2012;20:512-522.
- Ranzer MJ, Chen L, DiPiero LA. Fibroblast function and wound breaking strength is impaired by acute ethanol intoxication. Alcohol Clin Exp Res 2011;35:83-90.
- Sørensen LT, Toft B, Rygaard J. Smoking attenuates wound inflammation and proliferation while smoking cessation restores inflammation but not proliferation. Wound Repair Regen 2010;18:186-192.
- Van Anholt RD, Sobotka L, Meijer EP, et al. Specific nutritional support accelerates pressure ulcer healing and reduces wound care intensity in non-malnourished patients. Nutrition 2010;26:867-872.
- Gurtner GC, Chapman MA. Regenerative medicine: Charting a new course in wound healing. Adv Wound Care 2016;5:314-328.
- Lansdown AB. A review of the use of silver in wound care: Facts and fallacies. Br J Nurs 2004;13:6-19.
- KCI Licensing Inc. V.A.C UltaTm Negative Pressure Wound Therapy System Monograph. March 2013; 2nd ed. 202.
- Wu SC, Marston W, Armstrong DG. Wound care: The role of advanced wound healing technologies. J Vasc Surg 2010;52:59-66.
- Supp DM, Boyce ST. Engineered skin substitutes: Practices and potentials. Clin Dermatol 2005;23:403-412.
- Simman R, McNevin A. Pursuing the path to specialized wound care: The ABWMS Perspective. Today’s Wound Clin 2017;11:12-14.
- ABWMS Core Curriculum: Fellowship Training in Wound Medicine. Comprehensive curriculum for implementation in teaching settings for physicians pursuing certification in wound medicine; 2015.
This article will summarize the salient features of wound care, including demographics of a changing population, fundamental phases of wound healing, advances in therapeutic modalities, and steps family physicians can take to become recognized as certified wound care physicians.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
