What Can Be Said With LBBB?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The ECG in the figure below was obtained from a patient with new-onset chest pain. It was interpreted as showing complete left bundle branch block (LBBB). Thus, the provider reasoned that “it is impossible to tell if anything acute is going on because there is LBBB.” Do you agree with that assessment?
In the past, clinicians believed one could not diagnose an acute ST-elevation myocardial infarction (STEMI) in the presence of LBBB. This notion has been refuted completely. Although it often will be more difficult to diagnose acute ischemia/infarction in a patient with chest pain who presents in complete LBBB, in a surprising number of such patients, there will be at least a strong suggestion on the initial ECG of acute STEMI despite the presence of underlying LBBB.
The rhythm is sinus. The QRS complex is wide (≥ 0.12 second), and the QRS morphology is consistent with complete LBBB because there is a predominantly positive complex in lateral leads I and V6 and a predominantly negative QRS in lead V1. That said, several features are distinctly atypical for simple LBBB. These include the following:
Septal Q waves are present in lateral leads I and aVL. Because development of LBBB alters the direction of initial septal activation, which no longer can proceed from left to right, there never normally should be a septal Q wave in a lateral lead when there is uncomplicated LBBB. The prominent Q waves in leads I and aVL of this tracing leave little doubt that infarction has occurred at some point.
There is ST segment coving and primary ST elevation in lead aVL. This shouldn’t be seen with typical LBBB. The most reliable way to recognize acute STEMI that occurs in association with LBBB is by the presence of frank ST elevation in a lead that should not show ST elevation. While it is challenging to determine if the anterior ST elevation seen in the figure is a result of LBBB or acute anterior STEMI — because there often is some normal ST elevation in anterior leads with simple LBBB — there should not be ST elevation in lateral or inferior leads.
There are reciprocal ST-T wave changes in each of the inferior leads. We know the inferior ST-T wave changes that are seen here are likely to be both real and acute because these inferior ST-T wave changes are a “mirror image” reflection of the ST-T wave in lead aVL. This reciprocal change picture should not be seen with uncomplicated LBBB.
The final abnormality occurs in the chest leads and is subtle but it supports the above limb lead findings. That is, the ST segments in leads V5 and V6 are coved and manifest a disproportionate amount of J-point ST depression (considering the modest amplitude of the R wave in these leads). This abnormal shape of the ST-T wave extends to lead V4.
In a patient with new-onset chest pain, the combination of these findings should suggest an acute evolving STEMI until proven otherwise despite the presence of underlying LBBB. Clearly, it would help to examine a prior ECG on this patient to clarify whether the LBBB is new and whether the above noted changes are acute. But in the absence of a comparison tracing, the history of new chest pain in this patient whose ECG shows LBBB with inappropriate lateral Q waves and primary ST-T wave changes despite the LBBB should strongly suggest acute STEMI with need for immediate evaluation and reperfusion therapy until proven otherwise. For more information about and further discussion on this case, please visit: http://bit.ly/2DDk4Ei.
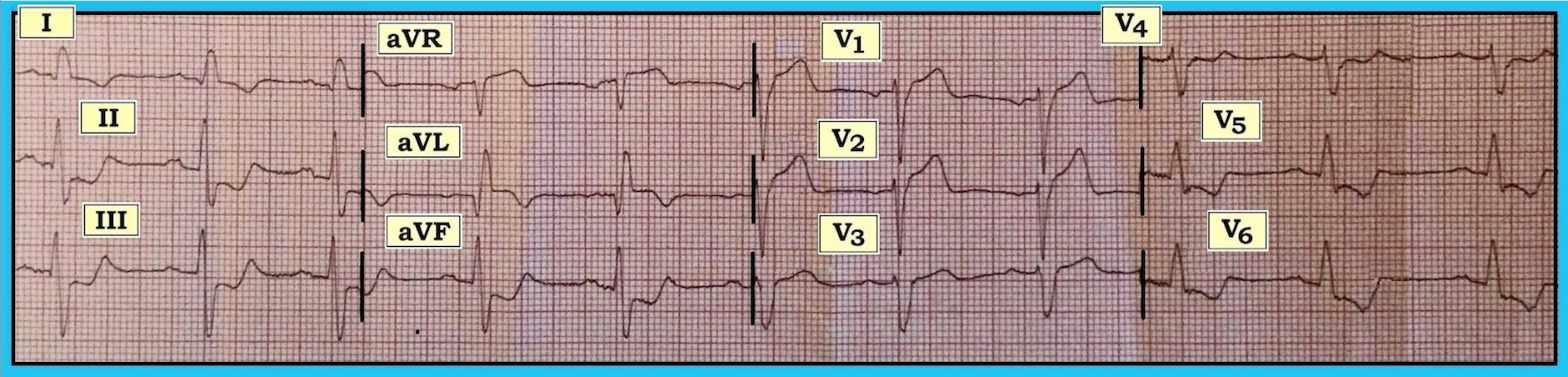
The ECG in the figure was obtained from a patient with new-onset chest pain. It was interpreted as showing complete left bundle branch block (LBBB). Thus, the provider reasoned that “it is impossible to tell if anything acute is going on because there is LBBB.” Do you agree with that assessment?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
