Tuberculosis in the United States in 2017
By Stan Deresinski, MD, FACP, FIDSA
Clinical Professor of Medicine, Stanford University
Dr. Deresinski reports no financial relationships relevant to this field of study.
SYNOPSIS: While the incidence of tuberculosis in the United States in 2017 was the lowest ever recorded, the current rate of decline would be required to almost double to reach the goal of elimination of the disease in this country by the year 2100.
SOURCE: Stewart RJ, Tsang CA, Pratt RH, et al. Tuberculosis — United States, 2017. MMWR Morb Mortal Wkly Rep 2018;67:317-323.
The incidence of tuberculosis in the United States in 2017 was 2.8 cases per 100,000 persons, the lowest rate on record. However, the rate of reduction in incidence has slowed and is insufficient to reach the goal of elimination by the year 2100.
Based on provisional data, the CDC reports that 9,093 new cases of tuberculosis were reported in the United States, for an incidence of 2.8 cases per 100,000 population, a 2.5% decrease from the previous year — and the lowest incidence ever recorded. Among U.S.-born persons with new onset of tuberculosis in 2017, African Americans and whites accounted for 37.1% and 29.5% of cases, respectively, with a 55% decrease in case counts for each group over the past 10 years. The incidence ranged from 0.3 cases per 100,000 in Montana to 8.1 in Hawaii; it was 4.1 in New York state and 5.2 in California. The highest incidences among the U.S.-born were recorded for Native Hawaiians and other Pacific Islanders (6.5 per 100,000) and American Indians and Alaska Natives (3.7), followed by African Americans (2.8), Asians (2.0), Hispanics (1.5), and whites (0.4).
The decrease in the absolute number of new cases of tuberculosis in U.S.-born individuals was accompanied by an increasing proportion of cases attributed in non-U.S.-born individuals, who accounted for 69.8% of the total and whose incidence of tuberculosis was now 15 times greater than in U.S.-born persons. (See Figure.) The highest rate among these was in Asians (27.0 per 100,000), followed by non-Hispanic blacks (22.0). The countries of origin of these cases in absolute numbers was highest for Mexico, followed by the Philippines, India, Vietnam, and China. The rate in non-U.S.-born decreased by only 0.9% from 2016 to 2017 (compared to a decline of 7.0% in U.S.-born individuals). Although not probative, but consistent with evidence that the majority of cases of tuberculosis in the United States result from activation of latent infection (LTBI), 45.0% of all cases in non-U.S. individuals occurred among those who had been in the United States for ≥ 10 years.
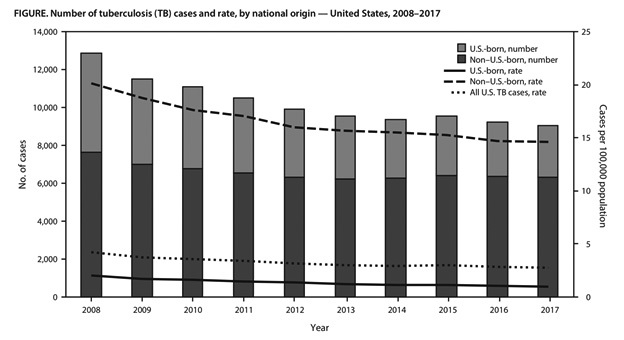
Figure: Number of Tuberculosis (TB) Cases and Rate, by National Origin — United States, 2008-2017 |
 |
|
Source: Centers for Disease Control and Prevention |
Overall, 4.6% of cases occurred in individuals who had experienced homelessness in the previous year, while 1.6% were in residents of long-term care facilities and 3.0% were confined to a correctional facility.
Only 1.0% of infections were caused by multidrug-resistant (MDR) Mycobacterium tuberculosis and there was only a single isolate of extensively drug-resistant (XDR) M. tuberculosis.
COMMENTARY
Although the United States experienced the lowest recorded incidence of tuberculosis in 2017, the rate of decrease has slowed from 5.3% in 2010-2013 to 2.0% in 2014-2017. (See Figure.) As pointed out by the authors, the 2017 rate is 28 times higher than the threshold of tuberculosis elimination in the United States, which is < 1 per 1 million persons. Achieving elimination of tuberculosis by 2100 would require a sustained annual decrease of 3.9% — almost twice the current rate of decrease.
As Stewart et al indicated, any hope of approaching such a rate of improvement requires maintaining efforts to reduce transmission of tuberculosis and enhanced efforts to detect and treat patients with LTBI. Testing for detection of LTBI should be focused on high-risk individuals, including individuals born in countries with a high prevalence of tuberculosis (no matter how long they have resided in the United States) and in persons in high-risk congregate situations, such as correctional facilities and homeless shelters.
While the incidence of tuberculosis in the United States in 2017 was the lowest ever recorded, the current rate of decline would be required to almost double to reach the goal of elimination of the disease in this country by the year 2100.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
