Cervical Spinal Injury
Although spinal injuries are uncommon, they should be considered when children have sustained head or neck trauma or multiple severe injuries. The cervical spine is the area most commonly affected. The upper cervical vertebrae (C1-C4) is injured more commonly in children younger than 8 years of age, whereas adolescents and adults are more likely to suffer injury to the lower cervical vertebrae (C5-T1). Children with severe or multisystem trauma are more likely to suffer a spinal injury. Thus, emergency department (ED) providers should have a lower threshold to immobilize and image such patients to prevent morbidity and mortality. These authors review the most common pediatric spinal fractures and injuries and optimal management practices.
— Ann M. Dietrich, MD, FAAP, FACEP
Etiology
Despite trauma being the leading cause of morbidity and mortality in children, cervical spinal injury (CSI) is relatively uncommon.1 When present, it can carry tremendous clinical sequelae if not recognized early and managed appropriately. Spinal injuries should be considered in all children presenting to the ED who have sustained head or neck trauma or multiple severe injuries. The risk of CSI increases with age, with a 10-fold increase after age 11.2 Nearly three-fourths of spinal injuries in young children occur in the cervical spine. Upper cervical vertebral injuries (C1-C4) are more common in children younger than 8 years of age, whereas adolescents and adults are more likely to suffer lower cervical vertebral (C5-T1) trauma.3 Spinal injuries are more common in males than females.4 Motor vehicle accidents in which the victim was unrestrained or improperly restrained are the most common mechanism of CSI in children.5 Falls are the second most common mechanism in patients younger than 8 years of age, and sports injuries are the second most common mechanism in older children.
Mortality rates for CSI range from 4% to 41%.6 Higher cervical vertebral injuries, including atlanto-occipital dislocation, are associated with the highest mortality rate. (See Figure 1.) Children with severe or multi-system trauma are more likely to suffer a spinal injury. Therefore, providers should have a lower threshold to immobilize and image such patients to prevent morbidity and mortality. Even after proper care, nearly one-third of children with CSI will require surgical intervention.7
Figure 1. Atlanto-occipital, C1-C2 Injury |
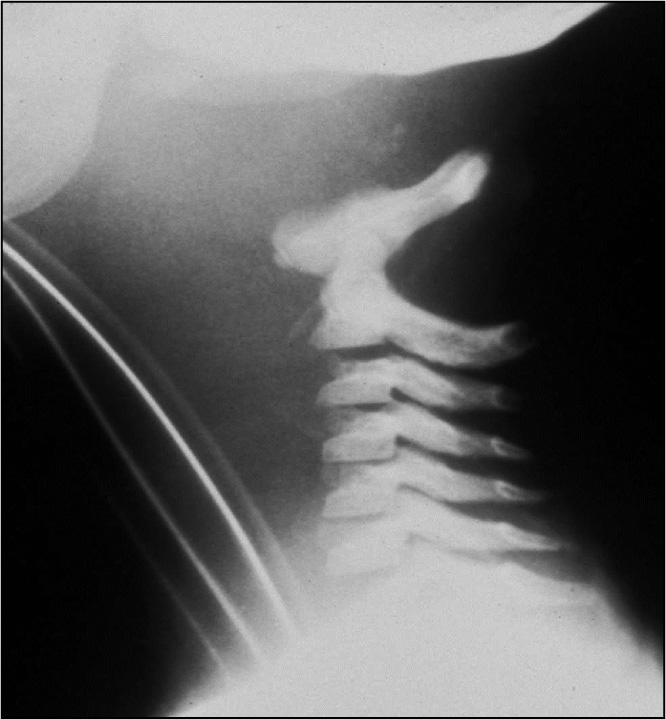 |
|
Reprinted with permission: Matthew C. DeLaney, MD. |
Children with underlying structural abnormalities or genetic predisposition to ligamentous laxity are more vulnerable to injury. Such patients include those with Down syndrome (atlanto-occipital instability), a history of previous CSI or cervical spine arthritis, Klippel-Feil syndrome (congenital fusion of cervical spine), Morquio syndrome (hypoplasia of odontoid), Larsen syndrome (cervical vertebrae hypoplasia, multiple joint dislocations), and any other syndromes associated with spinal abnormalities.8,9 In addition, chin trauma, fractures of the posterior teeth, and mandibular condyles may be associated with CSI.
Nonaccidental trauma (NAT) contributes to about 1% of spinal injuries in children.10 In those with intracranial injury from NAT, the incidence rises to more than 15%. These generally occur in patients younger than 2 years of age, generally are in the cervical spine, and nearly always are part of a multisystem trauma. Most often, these children will have focal neurologic findings, although occasionally they will present with a normal exam initially.11 Cervical spinal imaging should be considered in patients with NAT to evaluate for occult injuries in this vulnerable population.
Pediatric Cervical Spinal Injury Patterns
The cervical spine can be thought of as having three columns: an anterior, a posterior, and a middle column. Together, all three columns provide stability to the spine; if one column is injured, the other two can continue to compensate for a short time. Two- and three-column injuries generally are considered unstable. These injuries can be grouped by mechanism and are described in Table 1. There are several important structural differences between the pediatric and the adult spine:
- The cervical spine fulcrum is more cephalad (C2-C3) in children younger than 8 years of age. As children age, it progresses more caudally to the C5-C6 region.
- Children younger than 8 years of age have increased laxity of the cervical spine ligaments and musculature, allowing greater mobility in flexion/extension.
- Children younger than 8 years of age have increased elasticity of interspinous ligaments, posterior joint capsule, and cartilaginous end plates.
- Wedge-shaped and horizontally oriented vertebral bodies predispose younger patients to injury.
- Intervertebral disc and annulus have high water content and can have longitudinal expansion without rupture during spinal column distraction.
- Children younger than 8 years of age have relatively larger and heavier heads.
Table 1. Unstable Cervical Spine Injuries by Mechanism |
|
Mechanism |
Characteristics |
|
Hyperflexion |
|
|
Hyperflexion with rotation |
|
|
Hyperextension |
|
|
Axial loading |
|
Younger children are susceptible to growth plate and ligamentous injuries. Children have immature growth centers that are susceptible to shear forces during rapid deceleration or hyperflexion/extension, particularly at the synchondrosis between the odontoid and vertebral body of C2. In young children, a more elastic spinal column can tolerate more distraction before rupture, thus leading to spinal cord injury without obvious bony spinal column injury or ligamentous disruption. Injuries to the spinal cord itself are listed in Table 2.
Table 2. Spinal Cord Injuries by Mechanism |
||
Spinal Cord Syndrome |
Mechanism |
Neurologic Deficit |
|
Anterior Cord Syndrome |
Hyperflexion injury and anterior cord compression |
|
|
Central Cord Syndrome |
Hyperextension injuries |
|
|
Brown-Sequard Syndrome |
Hemisection of the cord |
|
|
Horner’s Syndrome |
Injury to cervical paravertebral sympathetic chain and inferior cervical ganglion |
|
|
Cervical Cord Neuropraxia |
Axial loading of neck in flexion or extension (common in football players and increased risk in cervical stenosis) |
|
|
Transection of Spinal Cord |
Severe spinal column disturbance |
|
Four injury patterns are common in children 8 years of age and younger:6
- Fracture with subluxation;
- Fracture without subluxation;
- Subluxation without fracture; and
- Spinal cord injury without radiographic abnormality (SCIWORA).
Between the ages of 8-10 years is a transition point in anatomic development.2,12,13 Epidemiologic studies show that children older than 8 years of age more commonly have injuries in a pattern similar to adults (i.e., C7-T1 region in contrast to the upper vertebral injuries sustained in younger children).13 These studies show an independent correlation not only to age but also to mechanism. This makes sense given that children’s activities change as they mature and develop.
Common Types of Fractures
Jefferson Fracture
Jefferson fractures refer to burst fractures of C1 and may involve both the anterior and posterior arches. (See Figure 2.) The mechanism usually is from an axial load (i.e., diving). The fracture is seen on an odontoid view, but this view is difficult to obtain in children younger than 3 years of age. (See Figure 3.) Typically, there will be a lateral offset of the lateral mass of C1 of > 1 mm from the vertebral body of C2. A pseudo-Jefferson fracture can be seen between 2-6 years of age secondary to the increased growth of the atlas compared to the axis.
Figure 2. Patient With a Jefferson (C1 Burst) Fracture |
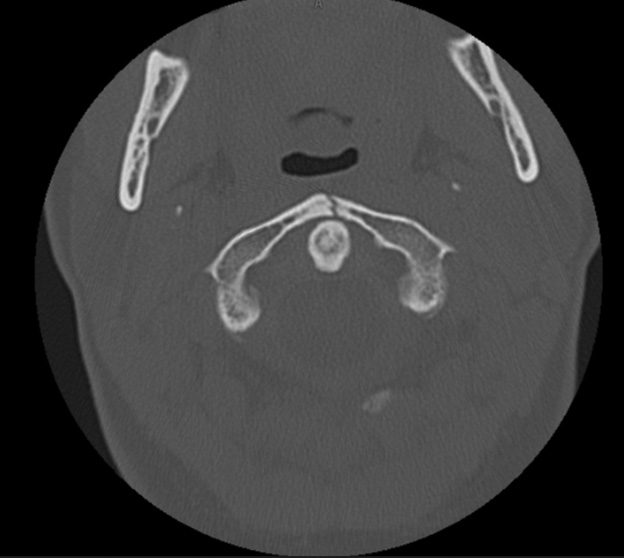 |
Figure 3. Normal Open Mouth View |
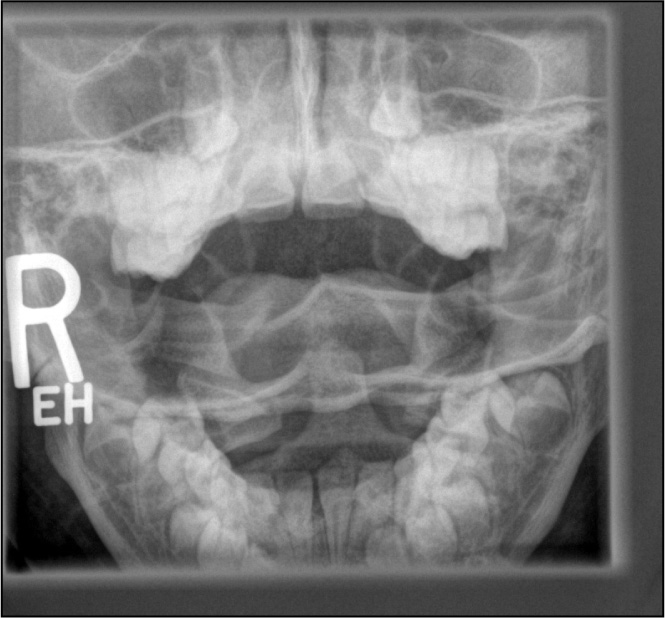 |
|
Reprinted with permission: Matthew C. DeLaney, MD. |
Hangman Fracture
Hangman fracture is a traumatic spondylolisthesis of C2, fracture of the pars interarticularis of the axis, horizontal tearing of the C2-C3 disk, and anterior subluxation of C2 on C3. Hangman fractures often result from hyperextension forces. If hyperflexion occurs after hyperextension, C2 may sublux onto C3 and cause spinal cord damage. The subluxation can be mistaken for pseudosubluxation.
Pseudosubluxation
Pseudosubluxation is seen in the C2-C3 or C3-C4 region in 25% of children younger than 8 years of age but can persist to age 16 years. On radiographs, evaluate the spinolaminar line or Swischuk line, which is drawn from the posterior arches of C1-C4. (See Figure 4.) This should pass within 1-2 mm of the anterior cortex of the posterior arch of C2 in children with pseudosubluxation. Distances greater than 1-2 mm usually are abnormal.
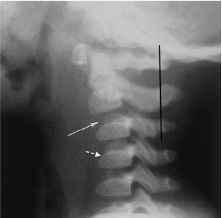
Figure 4. Pseudosubluxation of C2 on C3 and Anterior Wedging |
 |
|
The white arrow depicts the “pseudosubluxation” of C2 on C3. The line of Swischuk (black line) was developed to help differentiate between pseudosubluxation and real pathology. A line from the cortex of the posterior arch of C1 to the cortex of the posterior arch of C3 should pass, intersect, or be < 1 mm away from the posterior arch of C2. Also demonstrated in this image is normal anterior wedging (dashed white arrow). SOURCE: Figure reprinted, with permission, from RadioGraphics 2003;23:539-560. © RSNA |
Atlanto-axial Subluxation
Atlanto-axial subluxation occurs as a result of movement between C1 and C2 secondary to transverse ligament rupture or a fractured dens.14 On lateral spine radiographs, there will be a widened predental soft tissue space (normal < 5 mm). Patients often present after falls with symptoms such as neck pain and torticollis, although sometimes only torticollis is present.15 Presentation can be delayed in more minor trauma. Rotary subluxation involves facet fracture or dislocation. These injuries present with muscle spasm on the sternocleidomastoid on the same side to which the chin points. These injuries usually are associated with a ligamentous injury. Management is variable, although the decision between conservative treatment with a soft collar or surgical fixation with halo placement generally is based on the presence or absence of neurologic symptoms.
Odontoid Fracture
Odontoid fractures are the most common cervical spine injuries in children. These fractures may be confused with normal anatomic variations due to synchondrosis between the body and the axis. Type 1 odontoid fractures involve the apex of the dens. Type 2 fractures are through the waist of the dens, and Type 3 extend into the body of C2. Type 2 and 3 are considered unstable and require emergent consultation.
Distraction injuries occur with a longitudinal stress on the cervical column. The most serious type is the atlanto-occipital dislocation. On radiographs, there is an increased distance between the occiput and C1 or widening of intervertebral disk space without adjacent compression. (See Figure 1.) These injuries are associated with high cervical spinal cord injuries and commonly are incompatible with long-term survival. This injury often is fatal on impact, causing an internal decapitation.
SCIWORA
Spinal cord injury without radiographic abnormality (SCIWORA) is a clinical-radiological condition that mostly affects children.16-19 Patients present with neurologic symptoms and deficits consistent with cord injury but without radiographic abnormalities on plain radiography and computed tomography (CT). These injuries can occur through many mechanisms, including hyperextension, hyperflexion, and distraction. In hyperextension injuries, the posterior interlaminar ligaments impinge the spinal cord, whereas, in hyperflexion injuries, the anterior interlaminar ligaments impinge on the cord. Distraction injuries occur when the longitudinal distraction stretches the spinal column beyond the tolerance of the spinal cord. This is seen with rapid acceleration/deceleration forces. Hematomyelia may occur with these injuries, causing hemorrhage into the spinal cord and severe neurologic injury.
SCIWORA lesions are found mainly in the cervical spine but also can be seen, although much less frequently, in the thoracic or lumbar spine. The level of spinal cord injury corresponds to the location of these changes. Thoracic SCIWORA has been described, but is less common because of the splinting protection of the rib cage.
The prognosis for children with SCIWORA alone is better than for children with vertebral fractures and neurologic symptoms. Some will have only transient neurologic symptoms and completely recover after 24 hours. Some may not have any neurologic symptoms immediately after the injury, but may develop them up to four days post-injury.
Magnetic resonance imaging (MRI) is the diagnostic study of choice. A recent systematic review emphasizes the prognostic value of spinal MRI for children with SCIWORA and highlights the role of the MRI classification system in improving the comparability and interpretability. With recent advances in neuroimaging techniques and increasing availability of MRI, the overall detection rate of SCIWORA has improved significantly and the term has become more ambiguous.20 Children with true SCIWORA should have a neurologic deficit with normal imaging, including MRI. Consequently, these children have substantially more favorable clinical outcomes than those with cervical cord abnormalities on MRI. In the ED setting, providers should remember the previous application of SCIWORA to those children with normal radiography and CT and be vigilant to re-examine patients for signs of neurologic stigmata.
Diagnosis/Evaluation
Children with suspected CSI must be evaluated efficiently and their injury recognized promptly. Initial assessment includes the primary and secondary survey with attention to the airway, breathing, and circulation according to Advanced Trauma Life Support Guidelines.21 Hypotension, bradycardia, and temperature instability may be signs of spinal shock, which results from disruption of the sympathetic chain and unopposed parasympathetic innervation. Apnea/hypoventilation may be a result of diaphragmatic paralysis (C3-C5).
A thorough neurologic examination should be performed. (See Table 3.) Children with fractures typically have pain, muscle spasm, and decreased range of motion. They may complain of transient or persistent paresthesia, paralysis, or weakness. The distribution may vary based on the injury. Some children are unable to express their symptoms, and others may have distracting injuries. Transient burning of the upper extremities may be indicative of a hyperextension injury with central cord contusion. For unconscious children, maintain spinal immobilization, log roll the patient, and quickly feel down the back for step-off deformities.
Table 3. Neurologic Signs and Symptoms |
|
Abnormal motor exam
|
|
Abnormal sensory exam
|
|
Altered mental status |
|
Neck pain |
|
Torticollis |
|
Limitation of motion |
|
Neck muscle spasm |
|
Neck ecchymosis or swelling |
|
Abnormal or absent reflexes |
|
Transient depression of reflexes below injury |
|
Clonus without rigidity |
|
Diaphragmatic breathing without retractions |
|
Neurogenic shock |
|
Absence of rectal tone
|
|
Priapism |
|
Absence of bulbocavernosus reflex
|
|
Decreased bladder function |
|
Fecal retention |
|
Unexplained ileus |
|
Autonomic hyperreflexia |
|
Blood pressure variability with flushing and sweating |
|
Poikilothermia |
|
Hypothermia or hyperthermia |
Spinal immobilization should be maintained and rapid radiologic evaluation should be performed.21 The cervical spine should be maintained in midline position with the airway open. Children are very good at protecting their injuries and are unlikely to move an injured neck spontaneously. Most children only require pain control, distraction, or parental presence to maintain spinal immobilization.22 The use of cervical collars has become synonymous with spinal immobilization; however, the evidence to support this recommendation is sparse.23 Although cervical collars are known to cause complications with prolonged use, they still are the mainstay of trauma management in the ED setting.24
Clinical Clearance of the Cervical Spine
Given the overall low prevalence of CSI in children, clinical clearance is most likely to be employed in awake patients.25 The majority of children with CSI will have some conspicuous findings, and providers with an attentive eye are unlikely to miss them.26 Still, decision algorithms for cervical spine imaging have been extrapolated from the adult literature to aid providers.27 (See Figure 5.) The Canadian C-Spine Decision Rule excluded patients younger than 16 years of age and, therefore, cannot be used readily for cervical spine clearance in children.28 However, the NEXUS study included children and has been validated for use in pediatric patients.29 (See Table 4.) However, only 2.5% of patients younger than 8 years of age and no children younger than 2 years of age were included.30 The authors stress caution in applying these rules to younger children, especially infants and toddlers. A multicenter study determined four high-risk factors for CSI in patients younger than 3 years of age:31
- Age ≥ 2 years;
- Motor vehicle collision;
- Glasgow coma score < 14; and
- Patient does not open eyes to painful stimulus.
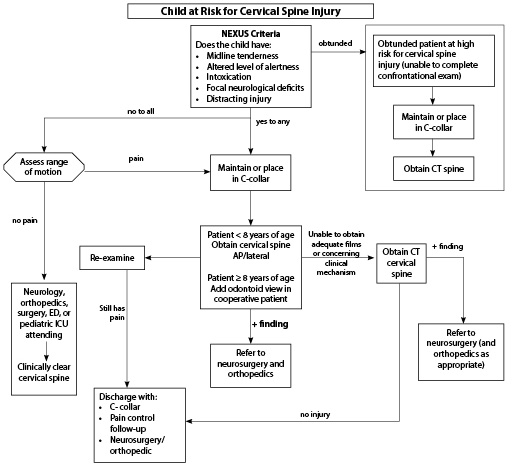
Figure 5. Approach to Evaluating a Pediatric Patient at Risk for Cervical Spine Injury |
|
At-risk patients have the following characteristics: altered loss of consciousness/amnesic to event; neurologic deficits; high-energy mechanisms, traumatic injury above clavicles; fall from more than 10 feet or two to three times the patient's height, fracture of other levels of the spine. |
|
|
|
Adapted from: Pediatric Trauma Society. Initial Evaluation of a Patient at Risk for Cervical Spine Injury. Available at: http://pediatrictraumasociety.org/multimedia/files/clinical-resources/C-Spine-5.pdf. Accessed May 8, 2018. |
Table 4. Low-risk Features of Children With Suspected Cervical Spine Injury |
NEXUS Criteria for Low Probability of Injury |
|
|
Adapted from: Hoffman JR, Wolfson AB, Todd K, Mower WR. Selective cervical spine radiography in blunt trauma: Methodology of the National Emergency X-Radiography Utilization Study (NEXUS). Ann Emerg Med 1998;32:461-469. |
When applied to a cohort of infant and toddler trauma patients from a trauma registry, no CSIs were missed and authors suggest that these criteria can be used to screen effectively for CSI.
Unconscious, obtunded, or intubated children presenting after trauma should be presumed to have a CSI until effectively evaluated by imaging. In obtunded adults, there is literature suggesting that collars can be removed after a normal CT.32,33 However, the relatively higher rate of SCIWORA precludes the use of this literature in children. Currently, there is no methodology for clearing these patients after normal imaging, although collars generally can be cleared after a normal MRI.34
Imaging of the Pediatric Cervical Spine
In patients with high-risk features for cervical spinal injury, imaging is recommended. (See Table 5.) Available modalities include plain radiography, CT, and MRI, each of which carries its own risks and benefits. Plain radiographs are readily available and quickly obtainable in all EDs with a minimal amount of ionizing radiation. Although CT long has been recognized as the gold standard for adults,36 plain radiographs still are the first-line recommendation for suspected cervical spinal injury in children because of the risk of ionizing radiation delivered to the thyroid by CT.37-39 Plain radiograph cervical spine series should include at least three views of the cervical spine (lateral, anterior-posterior, and, if possible, open-mouth odontoid). Cross-table lateral views identify most fractures, dislocations, and subluxations but are not sufficient to exclude injury without anterior-posterior views. Odontoid views increase the sensitivity of identifying injuries although they can be omitted in an uncooperative or preverbal child. This series has been shown to be > 90% sensitive in identifying CSI in pediatric patients.40,41
Table 5. High-risk Features of Children With Suspected Cervical Spine Injury |
|
|
Adapted from: Leonard JC, Kuppermann N, Olsen C, et al. Factors associated with cervical spine injury in children after blunt trauma. Ann Emerg Med 2011;58:145-155. |
Still, the interpretation of cervical spinal radiographs in children is difficult and requires an experienced radiologist or provider to interpret the anatomic variations. (See Table 6.)
Table 6. Anatomic Variations |
|
Cervical lordosis |
|
Incomplete ossification of the posterior elements |
|
Ligamentous laxity |
|
Pseudosubluxation of C2 on C3 or C3 on C4 |
|
Anterior wedging |
|
Disruption of alignment of the four cervical spine contour lines (anterior vertebral body line, posterior vertebral body line, spinolaminar line, and tips of the spinous processes)
|
|
Predental space: between posterior surface of the anterior arch of C1 and anterior surface of odontoid
|
|
Prevertebral space at C2-C4
|
CT is recommended for any patient with inconclusive initial films or continued high clinical suspicion for CSI. CT is an excellent modality for identifying bony abnormalities, although it still will miss ligamentous injury unless there is a bony malalignment. Some patients with high-risk features as described earlier may benefit from immediate CT, such as those who are unconscious, intubated, or show focal neurologic deficit.
MRI is preferred for visualizing soft tissues, ligamentous injuries, spinal cord edema, hemorrhage, compression, and transection. However, MRI is not readily available in all ED settings, and younger children may not tolerate the duration of scanning while awake. MRI should be obtained in all children with focal neurologic findings with or without injury identified on plain radiograph or CT. In areas where this is unavailable, transfer should be initiated.
Management/Treatment
Children with clinical findings suggestive of spinal cord injury should be treated conservatively with immobilization, even in the absence of radiographic abnormalities. Immediate consultation or referral to a regional trauma center for pediatric neurosurgical and pediatric orthopedic evaluation is crucial for definitive management. All patients with CSI and neurologic deficit should be admitted to the pediatric intensive care unit.
Steroid therapy is debated, and randomized, controlled trials are needed in the pediatric population to assess the advantages of steroid use after SCI in children.42-44 The use of steroids in patients is associated with increased infectious risks and no neurological improvements, with some literature suggesting an increased incidence of complications in children.13 Current expert opinion-based guidelines recommend against steroids for pediatric spinal cord injury.
Some patients may meet criteria for discharge from the ED with a padded hard cervical collar despite persistent neck pain.45 Consider discharge if any of the following are present:
- Transient symptoms have resolved;
- Normal neurologic examination;
- Normal imaging;
- No other serious injuries;
- Parent or caregiver and patient aware of restriction of any activity that may lead to re-injury;
- Neurosurgical follow-up in one to two weeks.
Conclusion
Pediatric CSI can be a complicated issue in the ED. It is not diagnosed often but is considered quite often. Higher frequency of adult CSI leads to more uncertainty in children. Because of these concerns, adult clinical decision rules can be inappropriately used in children. A good understanding of both low-and high-risk factors for pediatric CSI, coupled with a thorough and repeated physical exam, generally can alleviate these concerns while still maintaining a high sensitivity for injury. The use of plain radiography as a first-line imaging modality can help further with diagnostic uncertainty without the considerable ionizing radiation of CT. The relative increased incidence of SCIWORA in children highlights the importance of serial exams over reliance on imaging. A structured, evidence-based approach to pediatric CSI evaluation is an invaluable tool for the ED provider to ensure quality patient care and minimize radiation exposure.
REFERENCES
- Avraham JB, Bhandari M, Frangos SG, et al. Epidemiology of paediatric trauma presenting to US emergency departments: 2006-2012. Inj Prev 2017 Oct. 22; pii: injuryprev-2017-042435. doi: 10.1136/injuryprev-2017-042435. [Epub ahead of print].
- McGrory BJ, Klassen RA, Chao EY, et al. Acute fractures and dislocations of the cervical spine in children and adolescents. J Bone Joint Surg Am 1993;75:988-995.
- Platzer P, Jaindl M, Thalhammer G, et al. Cervical spine injuries in pediatric patients. J Trauma 2007;62:389-396.
- Chaudhry AS, Prince J, Sorrentino C, et al. Identification of risk factors for cervical spine injury from pediatric trauma registry. Pediatr Neurosurg 2016;51:167-174.
- Brown RL, Brunn MA, Garcia VF. Cervical spine injuries in children: A review of 103 patients treated consecutively at a level 1 pediatric trauma center. J Pediatr Surg 2001;36:1107-1114.
- Easter JS, Barkin R, Rosen CL, Ban K. Cervical spine injuries in children, part I: Mechanism of injury, clinical presentation, and imaging. J Emerg Med 2011;41:142-150.
- Puisto V, Kaariainen S, Impinen A, et al. Incidence of spinal and spinal cord injuries and their surgical treatment in children and adolescents: A population-based study. Spine 2010;35:104-107.
- Kenefake ME, Swarm M, Walthall J. Nuances in pediatric trauma. Emerg Med Clin North Am 2013;31:627-652.
- Copley LA, Dormans JP. Cervical spine disorders in infants and children. J Am Acad Orthop Surg 1998;6:204-214.
- Knox J, Schneider J, Wimberly RL, Riccio AI. Characteristics of spinal injuries secondary to nonaccidental trauma. J Pediatr Orthop 2014;34:376-381.
- Baerg J, Thirumoorthi A, Vannix R, et al. Cervical spine imaging for young children with inflicted trauma: Expanding the injury pattern. J Pediatr Surg 2017;52:816-821.
- Jones TM, Anderson PA, NoonanKJ. Pediatric cervical spine trauma. J Am Acad Orthop Surg 2011;19:600-611.
- Leonard JR, Jaffe DM, Kuppermann N, et al. Cervical spine injury patterns in children. Pediatrics 2014;133:e1179-1188.
- Beier AD, Vachhrajani S, Bayerl SH, et al. Rotatory subluxation: Experience from the Hospital for Sick Children. J Neurosurg Pediatr 2012;9:144-148.
- Neal KM, Mohamed AS. Atlantoaxial rotatory subluxation in children. J Am Acad Orthop Surg 2015;23:382-392.
- Pang D, Pollack IF. Spinal cord injury without radiographic abnormality in children — the SCIWORA syndrome. J Trauma 1989;29:654-664.
- Pang D. Spinal cord injury without radiographic abnormality in children, 2 decades later. Neurosurgery 2004;55:1325-1343.
- Farrell CA, Hannon M, Lee LK. Pediatric spinal cord injury without radiographic abnormality in the era of advanced imaging. Curr Opin Pediatr 2017;29:286-290.
- Launay F, Leet AI, Sponseller PD. Pediatric spinal cord injury without radiographic abnormality: A meta-analysis. Clin Orthop Relat Res 2005;433:166-170.
- Yucesoy K, Yuksel KZ. SCIWORA in MRI era. Clin Neurol Neurosurg 2008;110:429-433.
- ATLS Subcommittee, American College of Surgeons’ Committee on Trauma, International ATLS Working Group. Advanced trauma life support (ATLS®): The ninth edition. J Trauma Acute Care Surg 2013;74:1363.
- Mikrogianakis A, Grant V. The kids are alright: Pediatric trauma pearls. Emerg Med Clin North Am 2018;36:237-257.
- Kwan I, Bunn F, Roberts IG. Spinal immobilisation for trauma patients. Cochrane Database Syst Rev 2001;CD002803.
- Chan M, Al-Buali W, Charyk Stewart T, et al. Cervical spine injuries and collar complications in severely injured paediatric trauma patients. Spinal Cord 2013;51:360-364.
- Hutchings L, Willett K. Cervical spine clearance in pediatric trauma: A review of current literature. J Trauma 2009;67:687-691.
- Hale DF, Fitzpatrick CM, Doski JJ, et al. Absence of clinical findings reliably excludes unstable cervical spine injuries in children 5 years or younger. J Trauma Acute Care Surg 2015;78:943-948.
- Slaar A, Fockens MM, Wang J, et al. Triage tools for detecting cervical spine injury in pediatric trauma patients. Cochrane Database Syst Rev 2017;CD011686.
- Stiell IG, Wells GA, Vandernheen KL, et al. The Canadian C-spine rule for radiography in alert and stable trauma patients. JAMA 2001;286:1841-1848.
- Hoffman JR, Wolfson AB, Todd K, Mower WR. Selective cervical spine radiography in blunt trauma: Methodology of the National Emergency X-Radiography Utilization Study (NEXUS). Ann Emerg Med 1998;32:461-469.
- Viccellio P, Simon H, Pressman BD, et al. A prospective multicenter study of cervical spine injury in children. Pediatrics 2001;108:e20.
- Pieretti-Vanmarcke R, Velmahos GC, Nance ML, et al. Clinical clearance of the cervical spine in blunt trauma patients younger than 3 years: A multi-center study of the American Association for the Surgery of Trauma. J Trauma 2009;67:543-549.
- Bush L, Brookshire R, Roche B, et al. Evaluation of cervical spine clearance by computed tomographic scan alone in intoxicated patients with blunt trauma. JAMA Surg 2016;151:807-813.
- Raza M, Elkhodair S, Zaheer A, Yousaf S. Safe cervical spine clearance in adult obtunded blunt trauma patients on the basis of a normal multidetector CT scan — a meta-analysis and cohort study. Injury 2013;44:1589-1595.
- Hutchings L, Atijosan O, Burgess C, Willett K. Developing a spinal clearance protocol for unconscious pediatric trauma patients. J Trauma 2009;67:681-686.
- Leonard JC, Kuppermann N, Olsen C, et al. Factors associated with cervical spine injury in children after blunt trauma. Ann Emerg Med 2011;58:145-155.
- Sheikh K, Belfi LM, Sharma R, et al. Evaluation of acute cervical spine imaging based on ACR Appropriateness Criteria®. Emerg Radiol 2012;19:11-17.
- National Institute for Health and Care Excellence. Head injury: Assessment and early management (CG176). 2014. Available at: https://www.nice.org.uk/guidance/cg176. Accessed May 7, 2018.
- Jimenez RR, Deguzman MA, Shiran S, et al. CT versus plain radiographs for evaluation of c-spine injury in young children: Do benefits outweigh risks? Pediat Radiol 2008;38:635-644.
- Arbuthnot M, Mooney DP. The sensitivity and negative predictive value of a pediatric cervical spine clearance algorithm that minimizes computerized tomography. J Pediatr Surg 2017;52:130-135.
- Nigrovic LE, Rogers AJ, Adelgais KM, et al. Utility of plain radiographs in detecting traumatic injuries of the cervical spine in children. Pediatr Emerg Care 2012;28:426-432.
- Cui LW, Probst MA, Hoffman JR< Mower WR. Sensitivity of plain radiography for pediatric cervical spine injury. Emerg Radiol 2016;23:443-448.
- Rozzelle CJ, Aarabi B, Dhall SS, et al. Management of pediatric cervical spine and spinal cord injuries. Neurosurgery 2013;72(Suppl 3):205-226.
- Breslin K, Agrawal D. The use of methylprednisolone in acute spinal cord injury: A review of the evidence, controversies, and recommendations. Pediatr Emerg Care 2012;28:1238-1245.
- Stahel PF, VanderHeiden T, Finn MA. Management strategies for acute spinal cord injury: Current options and future perspectives. Curr Opin Crit Care 2012;18:651-660.
- Dorney K, Kimia A, Hannon M, et al. Outcomes of pediatric patients with persistent midline cervical spine tenderness and negative imaging result after trauma. J Trauma Acute Care Surg 2015;79:822-827.
Although spinal injuries are uncommon, they should be considered when children have sustained head or neck trauma or multiple severe injuries. Children with severe or multisystem trauma are more likely to suffer a spinal injury. Thus, emergency department providers should have a lower threshold to immobilize and image such patients to prevent morbidity and mortality. This article reviews the most common pediatric spinal fractures and injuries and optimal management practices.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.