Dairy Intake and Risk of Parkinson’s Disease
June 1, 2018
Reprints
Naturopathic Doctor, Acupuncturist, Evansville, WI
Dr. Becker reports no financial relationships relevant to this field of study.
SUMMARY POINTS
- Consumption of more than three servings per day of low-fat dairy foods, including skim and low-fat milk, sherbet, and frozen yogurt, was associated with an increased risk of Parkinson’s disease.
- A significant linear trend for decreased risk was associated with a greater intake of high-fat dairy.
- Men and women have similar risks, increased or decreased, of Parkinson's disease, based on these variations in milk intake.
SYNOPSIS: Frequent consumption of dairy products is associated with a modest increased risk of Parkinson’s disease (PD) in women and men. In addition, intake of high-fat dairy is associated with decreased risk of PD.
SOURCE: Hughes KC, Gao X, Kim IY, et al. Intake of dairy foods and risk of Parkinson’s disease, Neurology 2017;89:46-52.
Parkinson’s disease (PD) is a long-term degenerative neurological condition that affects 6.2 million people worldwide.1,2 The aim of any therapy for the treatment of PD, albeit drug, diet, exercise, surgery, or acupuncture, is to slow the inevitable progression of the disease and minimize motor symptoms. As there is no cure for PD, identifying factors contributing to the development of PD and focusing on prevention is of utmost importance, particularly in those with a family history of the disease.
Dairy products are consumed widely and would be an important modifiable risk factor for this disease. Other researchers have found an association between dairy intake and the risk of PD. Hughes et al investigated two questions: whether certain dairy foods or nutrients present in dairy foods are driving this association and whether there are differences between men and women. PD affects men more than women in a 3:2 ratio.3 Hughes et al combined data from two large prospective chart studies: the Nurses’ Health Study (NHS; n = 80,736) and the Health Professionals Follow-up Study (HPFS; n = 48,610), with a total of 26 and 24 years of follow-up, respectively. Both studies collected dietary intake with a food frequency questionnaire completed every two years. Hughes et al presented data from both studies for an additional 12 years of follow-up, with a total of 1,036 incident cases of PD.
The NHS began in 1976 when female registered nurses aged 30 to 55 years responded to a questionnaire about their medical history and health-related behaviors. The HPFS also began in 1976 when male health professionals aged 40 to 75 responded to a similar questionnaire. Individuals in the current analysis were excluded if they had an excessive or insufficient caloric intake (< 660 or > 3,500 kcal/day for women and < 800 or > 4,200 kcal/day for men), had a previous diagnosis of PD, or had missing baseline dietary information. Multivariable models were adjusted for pack-years of smoking, coffee intake, body mass index, physical activity, alcohol intake, and total energy intake.
In the NHS study, diet was assessed at baseline in 1984, 1986, and every four years thereafter. In the HPFS study, diet was assessed initially in 1986 (baseline) and every four years thereafter. Participants were asked to report each portion of food from never to more than six times per day. Dairy intake was separated into the following categories: total dairy and individual dairy products including skim or low-fat milk, whole milk, cream, sour cream, cream cheese, cottage cheese, low-fat cheese, other cheese, ice cream, yogurt, sherbet, frozen yogurt, butter, and margarine.
Only patients with confirmed cases of PD were included in this analysis. These cases were confirmed if the physician considered the PD diagnosis definite or probable, the medical record included the final diagnosis of PD by a neurologist, or the medical record indicated the presence of at least two of the three cardinal signs of PD (resting tremor, rigidity, bradykinesia) in the absence of evidence for another diagnosis.
A lagged analysis was conducted that excluded the first four years of follow-up in each cohort. This was to address the possibility of participants who may have been experiencing PD symptoms at the time of the questionnaire changing their dietary habits. Often, people will improve their dietary habits when diagnosed with a chronic disease. This lagged analysis was intended to reduce this confounding variable. Overall, results of the lagged analysis were similar to those of the main analysis.
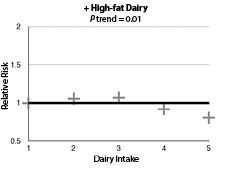
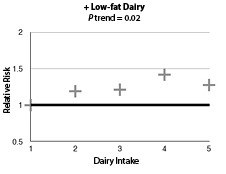
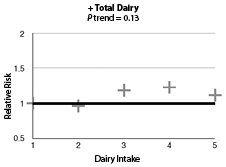
The authors included 554 PD cases in men and 482 PD cases in women. When comparing people who ate three or more dairy foods per day to those who ate less than one per day, the authors found no association with PD risk (hazard ratio [HR] 1.16; 95% confidence interval [CI], 0.92-1.48; P trend = 0.19). Interestingly, for low-fat dairy foods, there was an elevated risk for PD when the same high-intake vs. low-intake comparison was made (HR, 1.34; 95% CI, 1.01-1.79; P trend = 0.04). This association mostly seemed to be due to intake of skim or low-fat milk products, even more specifically sherbet/frozen yogurt. In contrast, high-fat dairy tended to be associated with a lower risk of PD development. (See Figure 1.) All of these results were similar in men and women.
Figure 1: Association of Dairy With Parkinson's Disease |
 |
 |
 |
The authors conducted further analysis for specific nutrients found in dairy products, including protein, calcium, vitamin D, and lactose. Neither total intake nor intake of these nutrients from dairy was significantly associated with PD risk. A sensitivity analysis was conducted by restricting the case definition to definite PD, by analyzing for nonsmokers, and by censoring participants at age 85 years because of the increased difficulty in diagnosing PD at older ages. The results were similar to the main analysis. These results for milk intake were pooled with three previously published studies with a total of 1,725 PD cases and total dairy results with one previously published study. The pooled relative risk for total milk intake was 1.56 and the pooled relative risk for total dairy intake was 1.27.
COMMENTARY
This analysis, the largest of its kind to date, yields useful guidance for clinicians. Most of the contributing factors to the development of PD are largely unknown. As with many other diseases, PD appears to be a combination of both inherited and environmental factors.3 The information in this analysis is particularly significant for individuals with a relative with a family history of PD. About 15% of people with PD have a first-degree relative with the disease.4 The genetic influence on the development of PD is likely due to susceptibility to negative environmental effects. However, clinicians should recognize those with a family history of PD and teach those patients about the association between frequent consumption of low-fat dairy and increased PD risk. Daily consumption of more than three servings of low-fat dairy products, especially skim and low-fat milk, frozen yogurt, and sherbet, significantly increased the risk of PD. This risk was reversed with the consumption of high-fat dairy. This effect was seen in men and women equally. The authors of previous studies on dairy and PD risk did not evaluate specific types of dairy. This current analysis yields unique information that can be used clinically to educate patients.
One mechanism proposed to explain the association between certain dairy products and the increased risk of PD is the “anti-uricemic effect” of dairy proteins, which refers to dairy effectively reducing serum urate levels.5,6 Reducing serum urate levels may be a problem for those PD patients. Studies show urate actually may be protective against PD.7,8 Specifically, consuming low-fat dairy, not high-fat dairy, reduces the risk of gout, demonstrating the particularly anti-uricemic effect of low-fat dairy.9 Full-fat dairy is high in saturated fat, which may counteract the anti-uricemic effect of the proteins in full-fat milk. This may explain why full-fat dairy decreases the risk of PD. Further research is needed to elucidate the mechanisms involved in this association.
Lastly, in particular, clinicians should pay attention to patients both with early signs of PD and with a genetic susceptibility for developing PD. Inquire into the patients’ dairy intake and educate patients about the increased risk of PD development with frequent low-fat dairy intake as well as a deceased risk with consumption of high-fat dairy.
REFERENCES
- GBD 2015 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national incidence, prevalence, and years lived with disability for 310 diseases and injuries, 1990–2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016; 388:1545-1602.
- GBD 2015 Disease and Injury Incidence and Prevalence Collaborators. Global, regional, and national life expectancy, all-cause mortality, and cause-specific mortality for 249 causes of death, 1980-2015: A systematic analysis for the Global Burden of Disease Study 2015. Lancet 2016;388:1459-1544.
- Kalia LV, Lang AE. Parkinson’s disease. Lancet 2015;386:896-912.
- Samii A, Nutt JG, Ransom BR. Parkinson’s disease. Lancet 2004;363:1783-1793.
- Garrel DR, Verdy M, PetitClerc C, et al. Milk and soy-protein ingestion: Acute effect on serum uric acid concentration. Am J Clin Nutr 1991;53:665-669.
- Dalbeth N, Wong S, Gamble GD, et al. Acute effect of milk on serum rate concentrations: A randomized controlled crossover trial. Ann Rheum Dis 2010;69:1677-1682.
- Gao X, O’Reilly EJ, Schwarzschild MA, Ascherio A. Prospective study of plasma urate and risk of Parkinson’s disease in men and women. Neurology 2016;86:520-526.
- Weisskopf MG, O’Reilly E, Chen H, et al. Plasma urate and risk of Parkinson’s disease. Am J Epidemiol 2007;166:561-567.
- Choi HK, Atkinson K, Karlson EW, et al. Purine-rich foods, dairy and protein intake, and the risk of gout in men. N Engl J Med 2004;350:1093-1103.
Frequent consumption of dairy products is associated with a modest increased risk of Parkinson’s disease (PD) in women and men. In addition, intake of high-fat dairy is associated with decreased risk of PD.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
