Acute Pericarditis or Something Else?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
A 28-year-old man was found nearly comatose in front of his house. There was a history of alcohol consumption. The patient was not lucid enough to answer questions. His initial ECG is shown in the figure below. Does this ECG suggest either acute pericarditis or acute infarction? What key piece of information is missing from the history? How would you interpret this tracing?
There is much baseline wandering and significant artifact. Approaching the tracing systematically, we note there appears to be a sinus rhythm at ~55/minute. However, P waves are of such low amplitude in lead II that we cannot rule out the possibility of an ectopic atrial rhythm. The PR interval is normal, and the QRS complex is narrow. However, the QTc interval is prolonged. The axis is normal, and there is no chamber enlargement. There is only one tiny Q wave (in lead II), and transition occurs early (i.e., the R wave already has become taller than the S wave is deep by lead V2).
The J-point elevation, with marked J-point notching at the junction between the end of the QRS complex and the beginning of the ST segment, and the presence of upward-sloping ST segment elevation in multiple leads are remarkable findings on this tracing. J-point elevation with prominent notching at the onset of the ST segment (as is seen in the figure) is designated as an Osborn wave. First described in 1953 by John J. Osborn, the presence of Osborn waves in multiple leads is associated with significant hypothermia (usually indicating a temperature below 32° C = below 89.6° F).
Other commonly associated ECG features with hypothermia include: bradycardia (which may be marked), atrial fibrillation or other arrhythmias, and artifact (from baseline undulations resulting from associated shivering).
The key information missing from the history in this case was the patient’s core temperature. Cold exposure plus excess alcohol consumption combined to predispose this patient to developing profound hypothermia, with a nearly comatose state by the time he was finally found. Neither acute pericarditis nor acute infarction were present, and ST segment elevation quickly resolved after the patient’s core temperature was corrected.
For more information about and additional discussion on this case, please visit: https://bit.ly/2wORr4M.
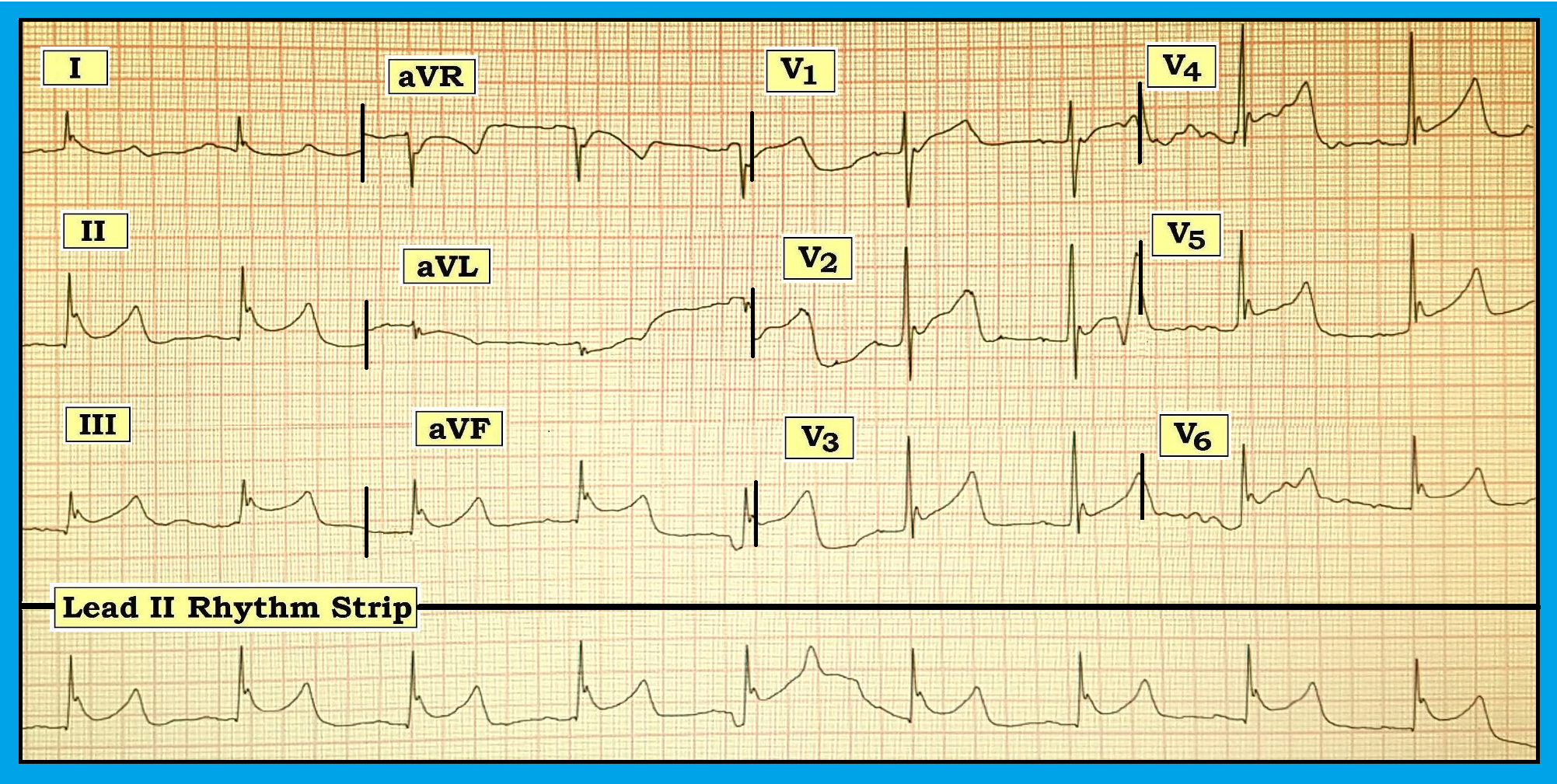
Does the ECG included with this article suggest either acute pericarditis or acute infarction? What key piece of information is missing from the history? How would you interpret the tracing?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
