Therapeutic Strategies for Hypertension
September 1, 2018
Reprints
AUTHORS
Hunter Mwansa, MD, St. Vincent Charity Medical Center, Case Western Reserve University, Cleveland, OH
Sula Mazimba, MD, MPH, Division of Cardiovascular Medicine, University of Virginia Health System, Charlottesville
PEER REVIEWER
Glen D. Solomon, MD, FACP, Professor and Chair, Department of Internal Medicine, Wright State University, Boonshoft School of Medicine, Dayton, OH
EXECUTIVE SUMMARY
Recent guidelines released by the American College of Cardiology/American Heart Association emphasize cardiovascular disease risk reduction and recommend determination of the estimated 10-year risk of cardiovascular disease to individualize care.
- Evidence consistently shows that effective treatment of hypertension reduces cardiovascular disease risk, complications, and overall mortality.
- Proven nonpharmacological interventions include weight loss, dietary modification, reduced sodium intake, potassium supplementation, and increased physical activity.
- Although monotherapy can be considered in stage 1 hypertension, those with stage 2 hypertension should be initiated on two first-line agents of different classes, as more than 60% of hypertensive patients require two or more agents to reach target blood pressure.
- Poor compliance can be attributed to physician inertia, patients’ low therapeutic adherence, and healthcare system deficiencies.
Last month, we focused on the definition of high blood pressure and current guidelines, risk factors, relationship to cardiovascular disease, blood pressure measurement, patient evaluation, and secondary causes. This issue will cover treatments (pharmacological and nonpharmacological), initial therapy, relationship to various disease conditions (diabetes, ischemic heart disease, heart failure, chronic kidney disease, cerebrovascular disease, ischemic stroke, stroke prevention, atrial fibrillation, valvular heart disease, aortic regurgitation, sexual dysfunction), resistant hypertension, hypertensive crises and emergencies, preoperative management, and adherence strategies.
— Gregory R. Wise, MD, FACP, Editor
Treatment of Hypertension
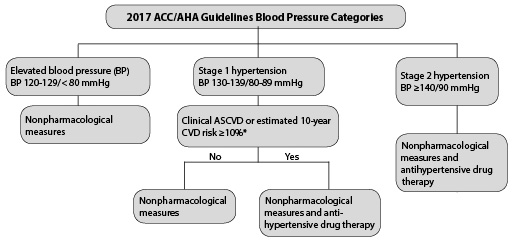
Blood pressure (BP) treatment may involve lifestyle interventions (nonpharmacological approach) alone or a combination of both nonpharmacological and pharmacological interventions, depending on BP categories.1 (See Figure 1.)
Figure 1. Management of Hypertension |
 |
|
ACC, American College of Cardiology; AHA, American Heart Association; ASCVD, atherosclerotic cardiovascular disease |
The 2017 American College of Cardiology/American Heart Association (ACC/AHA) guidelines on hypertension (HTN) place emphasis on cardiovascular disease (CVD) risk reduction, and recommend determination of the estimated 10-year risk of cardiovascular disease to individualize care. As noted in Figure 1, nonpharmacological interventions are recommended for patients with elevated BP (BP 120-129/< 80 mmHg) and those with stage 1 HTN (BP 130-139/80-89 mmHg) with an estimated 10-year CVD risk ≤ 10%. However, patients with stage 1 HTN and an estimated 10-year CVD risk ≥ 10% should receive pharmacological intervention as well as nonpharmacological measures. The 2017 ACC/AHA guidelines further emphasize follow-up of patients diagnosed with HTN. They recommend three to six months of follow-up for patients with elevated BP and stage 1 HTN with < 10% 10-year CVD risk, and one month of follow-up for those with stage 1 HTN and > 10% 10-year CVD risk.2 Clinical CVD includes coronary heart disease (CHD), congestive heart failure (CHF), and cerebrovascular accident. Evidence consistently has shown that treatment of HTN reduces CVD risk, complications, and overall mortality.3,4
Nonpharmacological Intervention. These measures, constituting mainly lifestyle modification, should be used to prevent HTN in patients with elevated BP and hypertensive patients with BP levels below the threshold for pharmacological intervention. These measures can help prevent HTN in those without the disease and help offset potential CVD complications and death.5 These measures can be complementary to pharmacological therapy and have proven to be helpful in reducing overall CVD risk.6 Nonpharmacological interventions proven to reduce BP include weight loss, dietary modification, reduced sodium intake, potassium supplementation, and increased physical activity. Weight loss through increased physical activity and reduced calorie intake has been proven to reduce BP.7 In general, about 1 mmHg reduction in BP is expected for every 1 kg decrease in body weight. Weight loss can lead to as much as 5 mmHg drop in BP in those who are hypertensive.7 This effect of weight loss on BP also has been observed in normotensive individuals, albeit to a lesser degree.
Adopting a healthy diet can help BP control. The Dietary Approaches to Stop Hypertension (DASH) diet has demonstrated systolic blood pressure (SBP) reductions of about 11 mmHg and 3 mmHg in hypertensive and normotensive individuals, respectively.8 The DASH diet is rich in vegetables, fruits, whole grains, and low-fat dairy products, and has reduced saturated and total fat. This diet was most effective in blacks.9 Other diets, including the Mediterranean, vegetarian, high-protein, and low-calorie diets, also have shown a benefit for reducing BP.10,11,12
Reduced dietary sodium intake can help prevent and lower BP in adults with established HTN.13 The reduction in SBP has been estimated to be 2-3 mmHg in normotensive individuals, and more pronounced decreases in BP can be expected in patients with higher BPs, the elderly, and blacks, who appear more susceptible to effects of sodium on BP.14 Used with other approaches, such as the DASH diet, weight reduction, and pharmacotherapy, dietary sodium reduction can achieve significant decreases in SBP.6,15 These BP effects of sodium may explain why reduced dietary intake may prevent CVD.16 Clinicians should counsel patients on how to reduce salt intake, including choosing fresh foods, selecting appropriate foods with low salt when eating out, using table salt judiciously, reducing food portion sizes, and using food labels to ensure selection of foods that have “low” or “no added” salt.
Dietary potassium has an inverse relationship with BP.17,18 For example, administration of 60 mmoL of potassium chloride can lead to a 2 mmHg to 4-5 mmHg reduction in BP in normotensive and hypertensive individuals, respectively.19,20 The BP response to potassium intake is twice as much in those with high sodium intake21 and blacks. Data suggest that the sodium/potassium index may be more important than either electrolyte alone. A higher sodium/potassium index is associated with higher CVD risk.16 Therefore, clinicians should encourage patients to consume potassium-rich diets, such as the DASH diet, nuts and soy products, low-dairy products, and selected meats. Daily dietary potassium intake between 3,510 mg22 and 4,700 mg23 has been recommended.
Physical activity consistently has been shown to improve BP. Dynamic aerobic exercise, dynamic resistance training, and static isometric exercise have been estimated to produce BP reductions of 5-8 mmHg, 4 mmHg, and 5 mmHg, respectively.24,25 These BP reduction effects have been reported even with low-intensity and interval exercise.26,24 The ACC/AHA recommends 90-150 minutes of exercise per week.2
Alcohol intake is associated with increased BP.27 Studies consistently have demonstrated increased SBP and diastolic blood pressure (DBP) in those consuming an equivalent of three or more standard drinks per day (about 36, 15, and 4.5 ounces of regular beer, wine, or distilled spirits, respectively).28,29 Cutting down on alcohol consumption can lead to reduction in SBP of ≥ 4 mmHg and ≥ 3 mmHg in hypertensive and normotensive individuals, respectively.28 Restriction of alcohol intake to two or less drinks per day in men and one or less drinks per day in women who consume alcohol has been recommended because of the beneficial effects of moderate alcohol consumption on overall CVD risk.30
Pharmacological Therapy
General Considerations. BP reduction with antihypertensive agents leads to a decrease in CVD risk, stroke, and death.31 The primary classes of antihypertensive agents include angiotensin-converting enzyme inhibitors (ACEIs), angiotensin receptor blockers (ARBs), thiazide diuretics, and calcium channel blockers (CCBs). Other less commonly used classes of antihypertensive agents include vasodilators, beta-blockers, aldosterone antagonists, centrally acting agents, alpha-1 receptor blockers, and direct renin inhibitors. Primary agents should be used to control BP because of their proven efficacy and benefit of CVD risk reduction.32 See Table 1 for a summary of common antihypertensive agents.
Table 1. Antihypertensive Agents |
||
Drug |
Dose Range/Frequency |
Comments |
Thiazide or thiazide-type diuretic |
||
|
Chlorthalidone* |
12.5 mg to 25 mg qd |
|
|
Hydrochlorothiazide |
25 mg to 50 mg qd |
|
|
Indapamide |
1.25 mg to 5 mg qd |
|
|
Metolazone |
2.5 mg to 5 mg qd |
|
Angiotensin-converting enzyme inhibitors (ACEIs) |
||
|
Benazepril |
20 mg to 40 mg qd or divided q12 |
|
|
Captopril |
12.5 mg to 50 mg bid to tid |
|
|
Enalapril |
5 mg to 40 mg or divided q12 qd |
|
|
Fosinopril |
10 mg to 40 mg qd or divided q12 |
|
|
Lisinopril |
10 mg to 40 mg qd |
|
|
Moexipril |
7.5 mg to 30 mg qd or divided q12 |
|
|
Perindopril |
4 mg to 16 mg qd or divided q12 |
|
|
Quinapril |
10 mg to 80 mg qd or divided q12 |
|
|
Ramipril |
2.5 mg to 10 mg qd to q12 |
|
|
Trandolapril |
1 mg to 4 mg qd |
|
Angiotensin receptor blockers (ARBs) |
||
|
Azilsartan |
40 mg to 80 mg qd |
|
|
Candesartan |
8 mg to 32 mg qd or divided q12 |
|
|
Eprosartan |
400 mg to 800 mg qd or divided q12 |
|
|
Irbesartan |
150 mg to 300 mg qd |
|
|
Losartan |
50 mg to 100 mg qd or divided q12 |
|
|
Olmesartan |
20 mg to 40 mg qd |
|
|
Telmisartan |
20 mg to 80 mg qd |
|
|
Valsartan |
80 mg to 320 mg qd |
|
Dihydropyridine calcium channel blockers (CCBs) |
||
|
Amlodipine |
2.5 mg to 10 mg qd |
|
|
Felodipine |
5 mg to 10 mg qd |
|
|
Isradipine |
5 mg to 20 mg qd or divided q12 |
|
|
Nicardipine SR |
20 mg to 40 mg q8hr |
|
|
Nifedipine LA |
30 mg to 120 mg qd or divided q12 |
|
|
Nisoldipine |
20 mg to 60 mg qd |
|
|
*Preferred |
||
Table 1. Antihypertensive Agents (continued) |
||
Drug |
Dose Range/Frequency |
Comments |
Nondihydropyridine calcium channel blockers (CCBs) |
||
|
Diltiazem SR |
60 mg to 180 mg bid (twice daily dosing) |
|
|
Diltiazem ER |
120 mg to 480 mg qd |
|
|
Verapamil IR |
40 mg to 120 mg tid (once daily dosing) |
|
|
Verapamil SR |
120 mg to 480 mg qd or divided q12 |
|
|
Verapamil PM |
400 mg qd |
|
Cardioselective beta-blockers (BB)† |
||
|
Atenolol |
25 mg to 100 mg qd |
|
|
Betaxolol |
5 mg to 20 mg qd |
|
|
Bisoprolol |
2.5 mg to 20 mg qd |
|
|
Metoprolol tartrate |
50 mg to 200 mg bid |
|
|
Metoprolol succinate |
50 mg to 200 mg qd |
|
Cardioselective and vasodilatory beta blockers (BB)† |
||
|
Nebivolol |
5 mg to 40 mg qd |
|
Non-cardioselective beta blockers (BB)† |
||
|
Nadolol |
40 mg to 320 mg qd |
|
|
Propranolol IR |
80 mg to 240 mg bid |
|
|
Propranolol LA |
80 mg to 320 mg qd |
|
Beta blockers (BB)† with sympathomimetic activity |
||
|
Carvedilol |
12.5 mg to 25 mg bid |
|
|
Carvedilol phosphate |
20 mg to 80 mg qd (extended release) |
|
|
Labetalol |
100 mg to 400 mg bid |
|
Diuretics (loop) |
||
|
Bumetanide |
0.5 mg to 2 mg bid |
|
|
Furosemide |
10 mg to 40 mg bid |
|
|
Torsemide |
2.5 mg to 10 mg qd |
|
Diuretics (potassium-sparing) |
||
|
Amiloride |
5 mg to 10 mg qd or divided q12 |
|
|
Triamterene |
100 mg to 300 mg qd or divided q12 |
|
|
† Avoid abrupt discontinuation as it can exacerbate angina and lead to myocardial infarction in those with underlying IHD. HFrEF, heart failure with reduced ejection fraction; IHD, ischemic heart disease; GFR, glomerular filtration rate; qd, once daily; bid, twice a day; tid, three times a day; qid, four times a day; q12, every 12 hours |
||
Table 1. Antihypertensive Agents (continued) |
||
Drug |
Dose Range/Frequency |
Comments |
Diuretics (aldosterone antagonists) |
||
|
Eplerenone |
50 mg qd or bid |
|
|
Spironolactone |
25 mg to 100 mg qd or divided q12 |
|
Direct renin inhibitor |
||
|
Aliskiren |
150 mg to 300 mg qd |
|
Central alpha-1 agonists and other centrally acting drugs |
||
|
Clonidine oral |
0.1 mg to 0.4 mg bid |
|
|
Clonidine patch |
0.1 mg to 0.3 mg q7days |
|
|
Methyldopa |
250 mg bid to qid |
|
|
Guanfacine |
0.5 mg to 2 mg qhs |
|
|
Vasoldilators |
||
|
Hydralazine |
10 mg to 50 mg bid to qid |
|
|
Minoxidil |
2.5 mg to 40 mg qd to bid |
|
Alpha-1 blockers |
||
|
Doxazosin |
1 mg to 16 mg qd |
|
|
Prazosin |
3 mg to 5 mg bid to tid |
|
|
Terazosin |
1 mg to 20 mg qhs |
|
|
qd, once daily; bid, twice a day; tid, three times a day; qid, four times a day; q12, every 12 hours; qhs, nightly at bedtime |
||
Monotherapy can be considered in patients with stage 1 HTN. Those with stage 2 HTN, average BP > 20/10 mmHg above their BP target, and high CVD risk should be initiated on two first-line agents of different classes, either as separate agents or fixed-dose combination therapy, as more than 60% of hypertensive patients require two ore more antihypertensive drugs to reach target BP.33,34
Combination therapy has been shown to lower BP more effectively with fewer side effects when compared with “stepped care” (optimization of monotherapy to maximal dosage and sequential addition of other antihypertensive drugs if BP control remains suboptimal).35
The lower adverse effects resulting from combination therapy may improve adherence. Several fixed-dose antihypertensive drug combinations are available and may help reduce pill burden in those who can afford them. Mechanisms of action of antihypertensive agents must be understood and considered for complementary pressor effects when choosing additional agents in those with uncontrolled BP. For example, initial pharmacotherapy with thiazide diuretics might lead to stimulation of the renin-angiotensin-aldosterone system (RAAS), and subsequent addition of an ACEI or ARB will help blunt these effects and lower BP. Drugs from the same class or with a similar mechanism of action should not be used in combination, as they provide no additional BP reduction and inevitably lead to more adverse effects. For example, an ACEI and ARB combination should be avoided. However, thiazide diuretics (e.g., chlorthalidone), a potassium-sparing diuretic (spironolactone), and/or loop diuretics (e.g., furosemide) can be used in combination, especially for those with renal disease and heart failure. There is no consensus on BP targets, especially for those with minimal CVD risk and elderly patients (> 65 years) who might be frail.36,37
Trials of optimal BP targets in the treatment of HTN have yielded mixed results. In the Action to Control Cardiovascular Risk in Diabetes (ACCORD) trial, more intensive BP treatment (SBP < 120 mmHg) failed to demonstrate a reduction in fatal and nonfatal cardiovascular events.38 More recently, the Systolic Blood Pressure Intervention Trial (SPRINT) investigated cardiovascular outcomes of more intensive BP (SBP < 120 mmHg) and standard BP treatment (SBP < 140 mmHg) in nondiabetic patients. The trial demonstrated a significant reduction in rates of nonfatal and fatal major cardiovascular events and all-cause mortality in those treated to SBP < 120 mmHg compared to SBP < 140 mmHg.39
Intensive BP treatment, as was seen in the SPRINT trial, may be associated with adverse effects including orthostatic hypotension. Patients who are frail, especially the elderly, must be evaluated for orthostatic hypotension, and intensification of therapy should be handled cautiously to avoid falls. A meta-analysis of the ACCORD and SPRINT trials showed fewer CVD events with SBP treatment to targets < 120 mmHg.
Therefore, clinicians should pay attention to patient-specific factors such as CVD risk, age, concurrent medications, comorbidities including presence of orthostatic hypotension, and potential for drug interactions to tailor BP targets.
Choice of Initial Therapy. Comorbid disorders play an important role in determining an appropriate choice for initial pharmacotherapy. A large head-to-head comparison trial (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial, ALLHAT) on initial pharmacotherapy showed that chlorthalidone was superior to amlodipine and lisinopril in preventing heart failure (HF).40
The ALLHAT trial also revealed that ACEIs were less effective than thiazide diuretics and CCBs in both BP reduction and stroke prevention. Furthermore, ACEIs have been found to be less effective than CCBs in preventing both HF41 and stroke in blacks.42,43 These studies have demonstrated that CCBs are just as effective as thiazide diuretics for reducing all CVD events except HF. Therefore, thiazide diuretics or CCBs may be the best first choice for initial single-drug therapy for hypertensive patients in general.
Pharmacotherapy in Patients With Comorbidities
HTN and Diabetes. The prevalence of HTN among adults with diabetes previously has been estimated to be 80%.44 The coexistence of HTN and diabetes is associated not only with increased incidence of CHD, HF, peripheral artery disease (PAD), stroke, and CVD mortality,45 but also with retinopathy and nephropathy.46
There is a paucity of data on optimal BP targets in diabetic patients. The ACCORD trial failed to demonstrate benefit in CVD outcomes from intensive BP control (SBP < 120 mmHg) among patients with diabetes. However, the results showed a tendency to reduced incidence of stroke (about 1.1% reduction in absolute risk), and there has been suggestion of significant benefit in the intensive BP/standard glycemic group in secondary analyses. A meta-analysis involving 73,913 patients with diabetes on intensive vs. standard BP treatment showed a 39% reduction in stroke among patients treated to an SBP < 130 mmHg, although there was no significant reduction in the incidence of myocardial infarction (MI).47 The United Kingdom Prospective Diabetes Study (UKPDS) demonstrated that a reduction in SBP by 10 mmHg was associated with an approximately 15% decrease in diabetes-related death.48
All antihypertensive drug classes, including thiazide diuretics, ACEIs, ARBs, and CCBs, are effective in the treatment of HTN in patients with diabetes.49 Notably, the study showed that diuretics had the lowest relative risk for development of HF than other antihypertensive agents, while CCBs appeared superior in reducing the risk for stroke. However, ACEIs or ARBs should be used in diabetic patients with albuminuria because of their proven benefit in reducing proteinuria and progression of diabetic nephropathy.50
Stable Ischemic Heart Disease. HTN is a major risk factor for ischemic heart disease. BP treatment to a target goal < 130/80 mmHg in patients with increased CVD risk has been shown to significantly lower CVD complications and overall mortality.39 ACEIs have a favorable effect on CVD outcomes. For example, ramipril demonstrated a 22% reduction in rates of MI, stroke, or CVD when compared with placebo in patients with high CVD risk.51 In an extension of these findings, perindopril also decreased CVD death, MI, or cardiac arrest by 20% compared with placebo in patients with established stable ischemic heart disease.52 Notwithstanding, the ALLHAT trial showed no additional benefit on CVD outcomes when ACEIs were compared to diuretics and CCBs. Beta-blockers may not be as effective as diuretics, CCBs, ACEIs, or ARBs in the treatment of HTN, but have been proven to improve symptoms of angina and can avert coronary events.53
Similarly, dihydropyridine CCBs are antianginal agents with BP-lowering effects. Unlike other hypertensive patients, those with stable ischemic heart disease can be managed initially with beta-blockers, given the added antianginal and mortality benefit. It is reasonable to add dihydropyridine CCBs to optimize BP in patients with persistent angina symptoms in whom BP control is suboptimal.
Heart Failure. Studies have shown that 75% of patients with chronic HF have antecedent HTN.54 Untreated HTN inevitably leads to HF.55 The SPRINT trial demonstrated that more intensive BP treatment to SBP < 120 mmHg significantly decreased the primary outcome (CVD composite), including the incidence of HF (hazard ratio, 0.62; 95% confidence interval, 0.45-0.84) in those with high CVD risk.39 Therefore, HTN can be managed with BP medications proven to have compelling indications for HF management. Guideline-directed medical therapy, including ACEIs, ARBs, angiotensin receptor-neprilysin inhibitors (ARNIs), guideline beta-blockers (carvedilol, metoprolol succinate, or bisoprolol), and mineralocorticoid receptor antagonists, is proven to reduce mortality and hospitalization.55
Nondihydropyridine CCBs (verapamil, diltiazem) may have deleterious effects on HF patients because of their negative inotropic effects.56 Therefore, they should be avoided in patients with HF with reduced ejection fraction (HFrEF).
There is a poorly understood subset of HF patients with preserved ejection fraction (HFpEF) in whom evidence-based therapies still are lacking. These patients are highly sensitive to pressure and volume loading, and commonly will present with pulmonary edema. Therefore, BP management with diuretic therapy may be effective in managing BP as well as volume overload. Suboptimally controlled BP can be managed further with the addition of an ACEI, ARB, beta-blocker, or mineralocorticoid antagonist. The beta-blocker nebivolol was associated with a 19% reduction in mortality or CVD hospitalization in patients with HFpEF.57 Aldosterone antagonists were shown to improve hospitalization rates in select patients.58
Chronic Kidney Disease. HTN and chronic kidney disease (CKD) commonly coexist, and each of these conditions can lead to the other. Their coexistence greatly increases the risk for adverse CVD and cerebrovascular events, especially in patients with proteinuria.59 About 67-92% of patients with CKD have HTN, and this prevalence increases with deterioration in renal function.60 About 30% of CKD patients may have masked HTN, and this might lead to accelerated CKD progression.61
Trials on optimal BP targets in CKD have yielded inconsistent results. The SPRINT trial demonstrated a benefit from intensive BP control (SBP < 120 mmHg) in those with high CVD risk. Intensive BP control demonstrated CVD and mortality benefit in 28% of the SPRINT study participants with CKD stages 3-4 (estimated glomerular filtration rate [GFR] 20 to < 60 mL/min/1.73 m2). Most CKD patients die of cardiovascular complications and, thus, may benefit from intensive BP control. Nonetheless, concerns have been raised about whether outcomes of the SPRINT trial can be generalized to all CKD patients, as previous studies showed a higher risk of mortality in CKD patients treated to lower SBPs, especially in the elderly.62,63
Even though no significant difference in adverse outcomes was noted between the intensive BP control and standard BP control groups of the SPRINT trial, caution must be exercised in applying the findings of this study to CKD patients. Many CKD patients have multiple comorbidities and might be frail, and intensive BP control inadvertently may cause harm. Slow optimization of medication doses and a “stepped-care” approach to BP management may be more appropriate and safer in elderly and frail patients.
ACEIs or ARBs (in those intolerant of ACEIs) are preferred in the treatment of BP in CKD patients with albuminuria (≥ 300 mg/day or ≥ 300 mg/g creatinine by first morning void), as they may slow progression of CKD.64,65 Those without albuminuria can be treated using any primary antihypertensive agent. Data on BP management post-renal transplant are less clear. Post-renal transplant patients have one functioning kidney and comprise a unique population of CKD patients. Typically, these patients have HTN because of their underlying CKD, use of calcineurin inhibitor-based immunosuppressive agents, and presence of allograft pathology. There are limited data on management of HTN in post-renal transplant patients. The immediate post-transplant period is especially complex and should be left to transplant physicians and nephrologists. HTN in the first month of renal transplantation can be managed with CCBs to maintain higher GFR and decrease graft loss.66 RAAS inhibitors may prove harmful, and should be used only after one month from transplantation in those with compelling indications like albuminuria and HF.
Cerebrovascular Disease. Stroke has high mortality, accounting for nearly 140,000 deaths among U.S. adults (one in every 20 deaths) annually, and is a leading cause of long-term disability and dementia.67 Most strokes (87%) result from ischemic damage from occlusion of blood flow to the brain.
Acute Intracerebral Hemorrhage. Data on optimal BP management in acute hemorrhagic stroke show conflicting results. Previous studies suggested safety and benefit from immediate (within six hours of presentation) SBP reduction to < 140 mmHg in patients with intracerebral hemorrhage (ICH).68,69 These studies suggested a decrease in hematoma growth and better functional recovery among ICH survivors. However, a more recent RCT showed no benefit in immediate lowering of SBP (within 4.5 hours of presentation) to 110-139 mmHg compared to SBP lowering to a goal of 140-179 mmHg.70 This study also showed more adverse renal events in those randomized to intensive BP control (SBP 110-139 mmHg). Significantly elevated BP (SBP 180 mmHg) is associated with hematoma growth and early neurological deterioration in patients with supratentorial ICH.71 Therefore, cautious control of blood pressure (SBP 140-179 mmHg) in ICH patients with significantly elevated SBP might be beneficial.
Acute Ischemic Stroke. About 80% of adult patients with acute ischemic stroke have elevated BP.72 Ischemic brain events are characterized by areas of infarction (if perfusion is not restored in a timely manner) that typically are surrounded by a rim of ischemic but viable tissue, referred to as penumbra, sustained by collateral arterial blood flow. There is abnormal cerebral autoregulation in the penumbra, and its viability depends on sustained systemic perfusion for delivery of oxygen. Thus, BP control in acute ischemic stroke aims to maintain cerebral perfusion pressure to the penumbra while minimizing worsening of tissue damage, ensuing cerebral edema, and hemorrhagic transformation of the infarct. Acute and drastic reductions in BP during acute ischemic stroke leads to brain injury and poor outcomes.73,74 Nonetheless, elevated BP in the first 24 hours in patients receiving intravenous thrombolysis with tissue plasminogen activator (tPA) has been associated with greater risk of symptomatic ICH.75 Given these considerations, the ACC/AHA 2017 BP guidelines recommend reduction of BP to < 185/110 mmHg before initiation of tPA. In patients who are not candidates for tPA, lowering BP ≤ 220/110 mmHg has no benefit and may cause harm. Therefore, BPs > 220/110 mmHg can be lowered gradually to 220/110 mmHg using intravenous agents.
Secondary Stroke Prevention. Recurrent strokes constitute 25% of all strokes among U.S. adults.67 Individuals who have an initial stroke or TIA have a 4% annual risk for a subsequent stroke,76 and mortality from recurrent stroke is twice as high as that from an initial stroke (21%).77 BP control with antihypertensive agents after an initial stroke results in 30% reduction in the risk of a recurrent stroke.78
Antihypertensive agents can be resumed within days (> 72 hours) in those with pre-existing HTN after an acute ischemic event, provided they have a stable neurologic status. Studies have suggested that CCBs, diuretics, and ACEI/ARBs may be superior to other drug classes for stroke prevention.79,80 Nevertheless, BP reduction to a target < 140/90 mmHg is more important than the specific choice of antihypertensive agent. The presence of other medical comorbidities, such as HF and CKD, may help with selection of appropriate therapy.
Peripheral Arterial Disease. No major difference exists in relative CVD risk reduction between hypertensive patients with PAD and without PAD,81 and no particular class of antihypertensive agents has demonstrated superiority over others in these patients.82 A recent analysis of ALLHAT data revealed a higher incidence of lower-extremity PAD events with lower and higher SBP (SBP < 120 mmHg and SBP ≥ 160 mmHg, respectively) compared with SBP 120-129 mmHg. Similarly, lower and higher BPs were associated with a higher rate of lower-extremity PAD events. In contrast, only lower DBP (< 60 mmHg) was associated with higher rates of lower-extremity PAD events.83 Given these findings, clinicians should exercise caution in managing BP in PAD patients.
Metabolic Syndrome. This refers to metabolic dysregulation characterized by increased abdominal adiposity, hypertriglyceridemia, low high-density lipoprotein, elevated fasting glucose, increased insulin resistance and hyperinsulinemia, and HTN.84 It is associated with significant CVD risk, and BP treatment with lifestyle modification and medications should be pursued. Previously, concerns have been raised about possible harm from the use of thiazide diuretics in patients with the metabolic syndrome because of their potential to increase insulin resistance, dyslipidemia, and hyperuricemia. There is no convincing clinical evidence to suggest this harm, and, in fact, the ALLHAT trial demonstrated only 1.5-4.0 mg/dL increase in fasting glucose levels that did not translate to meaningful increase in CVD risk with use of chlorthalidone.85 Traditional beta-blocker use in these patients may be associated with worsening of glucose tolerance, reduced ability to lose weight, and dyslipidemia, all of which might lead to overt diabetes.86 Interestingly, the newer vasodilating beta-blockers (e.g., carvedilol, labetalol, and nebivolol) seem to have favorable metabolic effects.87
Atrial Fibrillation. HTN is the most common comorbid condition in atrial fibrillation (AFib), occurring in more than 80% of patients. Uncontrolled HTN leads to left ventricular (LV) hypertrophy; impaired LV filling; and consequent left atrial hypertrophy, enlargement, and fibrosis, which in concert lead to electrophysiological remodeling and ectopy causing AFib.88 HTN also is common in ischemic and nonischemic cardiomyopathies that lead to AFib. Treatment of AFib in patients with LV dysfunction and HF can prevent new-onset AFib and recurrent AFib.89 However, similar ARB/ACEI effects on incident and recurrent AFib have not been demonstrated in those without LV dysfunction. Optimal BP control with primary antihypertensive agents (thiazide diuretics, ACEIs, ARBs, and CCBs), as opposed to the choice of initial antihypertensive, should be a focus of therapy.
Valvular Heart Disease
Aortic Stenosis. HTN is a risk factor for the development of aortic stenosis. In patients with asymptomatic aortic stenosis, systemic HTN results in increased LV afterload, structural damage, and increased morbidity and mortality.90 Improvements in stroke volume and LV end-diastolic pressure secondary to decreases in pulmonary and systemic resistance following nitroprusside infusion have been observed in hypertensive patients with severe aortic stenosis.91 This suggests a possible benefit from cautious BP lowering in patients with aortic stenosis. Unfortunately, trials comparing outcomes of different BP-lowering agents in patients with aortic stenosis are lacking. ACEIs and ARBs are preferred for treatment of HTN in patients with symptomatic aortic stenosis because of their favorable effect on dyspnea and effort tolerance.92 Beyond their effects on HTN, RAAS inhibitors can affect reverse remodeling and confer a mortality benefit in those with LV dysfunction and HF. However, caution should be exercised, given the potential to cause hypotension in patients with significant LV dysfunction and HF. Beta-blockers also may be advantageous in patients with prior MI, reduced ejection fraction, angina, and tachyarrhythmias. Diuretics can be harmful, especially in patients with small LV volume, as these patients often are preload-dependent.
Aortic Regurgitation. Vasodilator therapy leads to reduction in afterload, decrease in LV mass and volume, and improved LV function.93 Despite the hemodynamic effects noted in prior studies, long-term therapy with either nifedipine (CCB) or enalapril (ACEI) did not delay or reduce time to aortic valve replacement in patients with asymptomatic severe aortic regurgitation with no LV dysfunction. Beta-blockers lead to increases in diastolic filling with potential to worsen aortic regurgitation. Furthermore, rapid decreases in diastolic BP may compromise coronary perfusion in patients with chronic severe aortic stenosis.
Aortic Disease. An aortic aneurysm refers to localized or diffuse dilation of the aorta to a diameter at least > 50% its normal caliber. Aortic aneurysms mostly are asymptomatic until dissection or rupture, and inevitably lead to death in untreated cases of rupture.94,95 HTN is linked to changes in aortic wall mechanical properties (increased arterial wall stiffening), possibly related to elastin destruction, and increases the risk for aortic rupture.96 The goal of medical management in aortic dissection is to limit propagation of dissected wall components by control of BP. High BP variability has been associated with poor outcomes in patients with type B aortic dissections following endovascular repair surgery.97 Beta-blockers have been shown to lower operative repair risk98 and overall survival in patients with chronic aortic dissections.99
There is no evidence from clinical trials of appropriate BP treatment target goals. The European Society of Cardiology recommends lowering systolic BP to 100-120 mmHg.100
BP and Sexual Dysfunction. Sexual dysfunction is more common in hypertensive than normotensive individuals. Erectile dysfunction (ED) is an independent CVD risk factor, and may be an early sign of organ dysfunction.101
There is evidence to suggest that lifestyle modification may help improve ED.102 ACEI, ARB, CCB, and vasodilating beta-blocker (e.g., nebivolol) therapy appear to have neutral to beneficial effects on erectile function.103 Like beta-blockers, antihypertensive drugs with potential negative effects on sexual function must be avoided to improve adherence in those without compelling indications. Phosphodiesterase-5 inhibitors can be used safely in those with refractory ED after initial measures. However, caution must be exercised in those on multiple drugs because of the potential for adverse effects. These drugs are contraindicated in patients on alpha-blockers and nitrates.
Resistant HTN. Resistant HTN is defined as failure to achieve target BP with optimal doses of three antihypertensive agents with complementary mechanisms of action, including a diuretic, or when BP control is achieved but with at least four medications.104
Resistant HTN has been estimated to affect about 13% of hypertensive patients.105 Risk factors for resistant HTN include older age, obesity, diabetes, CKD, and black race. It is associated with markedly increased CVD morbidity and mortality, including all-cause death.106 Clinicians should ensure accurate office BP measurements, confirm with ambulatory BP measurements, and assess for medical adherence to exclude “pseudo resistance” before a diagnosis of resistant HTN is made. Also, it is important to identify reversible causes of poorly controlled HTN, such as obesity, obstructive sleep apnea, physical inactivity, dietary indiscretions like high salt intake, and excessive alcohol consumption. Clinicians also must conduct a detailed inquiry on possible use of nonsteroidal anti-inflammatory drugs, oral contraceptive therapy, nasal decongestants, excessive caffeine intake, use of illicit drugs, and other medications that might affect BP. Finally, patients suspected of having resistant HTN must be screened for secondary HTN.
Refractory HTN is another group of antihypertensive treatment failure that is defined as failure to control BP despite use of at least five different classes of antihypertensive agents, including a long-acting thiazide diuretic and a mineralocorticoid receptor antagonist.107 The addition of the mineralocorticoid receptor antagonist spironolactone to multidrug therapy, including primary agents (i.e., thiazide diuretics, CCBs, ACEI/ARBs), results in significant BP reduction.108 Furthermore, the addition of hydralazine and/or minoxidil may prove effective in controlling BP. Multidrug therapy also can be augmented by loop diuretic use in patients with CKD.
Hypertensive Crises. Hypertensive crises are divided into emergencies and urgencies. They constitute a large proportion of emergency department visits and may account for more than 25% of emergency department admissions.109
Hypertensive Emergencies. Defined as BP elevations > 180/120 mmHg with evidence of new or worsening end-organ damage,110 hypertensive emergencies are associated with a one-year mortality of almost 80% and a median survival of only 10.4 months if left untreated.111 Prompt control of BP may help prevent further end-organ damage. Examples of hypertensive emergencies include hypertensive encephalopathy, ICH, acute ischemic attacks, acute coronary syndromes, acute LV dysfunction and pulmonary edema, dissecting aortic aneurysm, and acute kidney injury. Hypertensive emergencies result in loss of autoregulation to tissues. Although prompt BP reduction helps prevent further end-organ damage from significantly elevated BP, cautious and gradual BP reduction may be required to maintain perfusion pressures to avoid ischemic tissue damage.
Management of hypertensive emergencies is based largely on clinical experience.112 Trial evidence suggests the superiority of nicardipine to labetalol in achieving short-term BP targets in hypertensive emergencies.113,114,115
Target BPs and choice of an intravenous antihypertensive agent depend on the end-organ involved, including the pathophysiology of the underlying HTN as well as present comorbid disorders. For example, aortic dissections and pheochromocytoma require rapid BP reduction to SBP < 140 mmHg within the first hour using short- and fasting-acting beta-blockers (e.g., esmolol) and non-selective alpha-blockers (e.g., phentolamine), respectively. Further reduction in BP to < 120 mmHg is required in aortic dissections. In general, management of other hypertensive emergencies requires prompt reduction of BP by a maximum of 25% in the first hour, then 160/100-110 mmHg over the next two to six hours, and then to normal in the next 24-48 hours.2
A cerebrovascular accident is another exception to this generalization, and whose management is discussed earlier.
Short-acting intravenous antihypertensive agents are titrated for BP easily, allow for more predictable and gradual reduction in BP than oral medications, and, therefore, are used in treating hypertensive emergencies.
Hypertensive urgencies are severe elevations in BP > 180/120 mmHg with no accompanying end-organ damage. Mostly, these are the result of nonadherence to medical therapy and can be managed safely on an outpatient basis. They are managed by reinstitution of antihypertensive drug therapy in those with nonadherence, and escalation of therapy in those with suboptimal control despite drug adherence.
Perioperative Management of HTN
Elevated BP is one of the common reasons for postponement of surgery. Evidence suggests increased cardiovascular complications including MI, dysrhythmias, neurological complications, and renal failure with preoperative DBP ≥ 110 mmHg.116 This relationship between BP and surgical risk is less clear for SBP. Postoperative HTN is associated with increased mortality and neurological deficits in patients undergoing carotid endarterectomy,117 and preoperative HTN appears to be the single most important risk factor for development of postoperative HTN. Isolated SBP is associated with increased CVD morbidity after coronary artery bypass graft surgery.118
Patients with poorly controlled HTN have BP lability with anesthesia.119 This can lead to markedly high BP with induction of anesthesia or intraoperative hypotension with further anesthesia. Because of the limited trial evidence on perioperative HTN, recommendations on BP management are based on observational data and clinical experience. Abrupt withdrawal of long-term beta-blockers and clonidine may precipitate rebound HTN and tachycardia and should be avoided. Patients taking these drugs can continue intravenous beta-blockers or transdermal clonidine if they cannot take anything by mouth. There is no indication to start beta-blockers on the day of surgery for patients who are beta-blocker naïve.120
Clevidipine, an ultra short-acting calcium channel antagonist, recently was shown to be an effective and safe drug for treatment of perioperative HTN, even in patients undergoing cardiac surgery.121,122 ACEIs and ARBs should be stopped 24 hours before noncardiac surgery, as recent evidence suggests potential harm including overall mortality, MI, stroke, and intraoperative hypotension in those continuing these medications until surgery.123 Diuretics should be avoided on the day of surgery because of potential adverse effects related to fluid depletion. It is important to remember that uncontrolled pain, anxiety, hypoxia, and fluid overload may contribute to perioperative HTN. Clinical evaluation focused on addressing these is crucial in the management of perioperative HTN.
Improvement of BP Control
Three major contributors to low rates of BP control include physician inertia, patients’ low therapeutic adherence, and healthcare system deficiencies.124
Adherence Strategies to Improve BP Control. Therapeutic nonadherence refers to failure to follow recommended medical or healthcare advice. It is a major barrier to effective control of HTN and reduction of CVD risk. Studies show that 25% of patients do not fill their initial prescription of antihypertensive medications,125 and the average hypertensive patient is in possession of their BP medication only 50% of the time in the first year of therapy.126 Nonadherence to therapy is complex and multifaceted, and requires a multipronged approach. Suggested solutions must be introduced at patient, provider, and healthcare system levels. Suggested methods to improve patient adherence are summarized in Table 2.
Table 2. Methods to Improve Patient Adherence to Therapy |
Patient level*
|
Drug treatment level†
|
Health system level
|
|
* Complex interventions combining more convenient care and supportive care, information, reminders, self-monitoring, reinforcement, counselling including family therapy and individual psychotherapy, crisis intervention, manual telephone follow-up, supportive care, and pharmacy-based programs were more effective. † Medication adherence is greatest (71-94%) with once-daily dosing, and lower with increased dose frequency. |
Clinicians should consider the benefits of a team-based approach as a means of enhancing care. A team-based approach involves collaboration between primary care physicians, specialists (e.g., nephrologists, cardiologists, and endocrinologists), nurses, pharmacists, dietitians, social workers, and community workers.2,124
CONCLUSION
HTN is a major public health problem in the United States and globally. Given the high mortality and morbidity associated with the disease, emphasis should be placed on prevention using lifestyle strategies including dietary measures and physical activity. Along with pharmacological interventions, tailored identification of patients’ global cardiovascular risk using existing risk stratification tools should be incorporated in treatment plans routinely.
REFERENCES
- Stone NJ, Robinson JG, Lichtenstein AH, et al. 2013 ACC/AHA guideline on the treatment of blood cholesterol to reduce atherosclerotic cardiovascular risk in adults: A report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. J Am Coll Cardiol 2014;63:2889-2934.
- Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the prevention, detection, evaluation, and management of high blood pressure in adults: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol 2018;71:e127-e248.
- Weber MA, Julius S, Kjeldson SE, et al. Blood pressure dependent and independent effects of antihypertensive treatment on clinical events in the VALUE Trial. Lancet 2004;363:2049-2051.
- Hajjar I, Kotchen TA. Trends in prevalence, awareness, treatment, and control of hypertension in the United States, 1988-2000. JAMA 2003;290:199-206.
- Whelton PK, He J, Appel LJ, et al. Primary prevention of hypertension: Clinical and public health advisory from the National High Blood Pressure Education Program. JAMA 2002;288:1882-1888.
- Whelton PK, Appel LJ, Espeland MA, et al. Sodium reduction and weight loss in the treatment of hypertension in older persons: A randomized controlled trial of nonpharmacologic interventions in the elderly (TONE). TONE Collaborative Research Group. JAMA 1998;279:839-846.
- Neter JE, Stam BE, Kok FJ, Geleijnse JM. Influence of weight reduction on blood pressure: A meta-analysis of randomized controlled trials. Hypertension 2003;42:878-884.
- Appel LJ, Moore TJ, Obarzanek E, et al. A clinical trial of the effects of dietary patterns on blood pressure. DASH Collaborative Research Group. N Engl J Med 1997;336:1117-1124.
- Svetkey LP, Simons-Morton D, Vollmer WM, et al. Effects of dietary patterns on blood pressure: Subgroup analysis of the Dietary Approaches to Stop Hypertension (DASH) randomized clinical trial. Arch Intern Med 1999;159:285-293.
- Bazzano LA, Hu T, Reynolds K, et al. Effects of low-carbohydrate and low-fat diets: A randomized trial. Ann Intern Med 2014;161:309-318.
- Nordmann AJ, Suter-Zimmermann K, Bucher HC, et al. Meta-analysis comparing Mediterranean to low-fat diets for modification of cardiovascular risk factors. Am J Med 2011;124:841-851.e2.
- Yokoyama Y, Nishimura K, Barnard ND, et al. Vegetarian diets and blood pressure: A meta-analysis. JAMA Intern Med 2014;174:577-587.
- He FJ, Li J, MacGregor GA. Effect of longer term modest salt reduction on blood pressure: Cochrane systematic review and meta-analysis of randomised trials. BMJ 2013;346:f1325.
- Graudal NA, Hubeck-Graudal T, Jürgens G. Effects of low-sodium diet vs. high-sodium diet on blood pressure, renin, aldosterone, catecholamines, cholesterol, and triglyceride (Cochrane Review). Am J Hypertens 2012;25:1-15.
- Sacks FM, Svetkey LP, Vollmer WM, et al; DASH-Sodium Collaborative Research Group. Effects on blood pressure of reduced dietary sodium and the Dietary Approaches to Stop Hypertension (DASH) diet. N Engl J Med 2001;344:3-10.
- Cook NR, Appel LJ, Whelton PK. Lower levels of sodium intake and reduced cardiovascular risk. Circulation 2014;129:981-989.
- Zhang Z, Cogswell ME, Gillespie C, et al. Association between usual sodium and potassium intake and blood pressure and hypertension among U.S. adults: NHANES 2005-2010. PLoS One 2013;8:e75289. doi: 10.1371/journal.pone.0075289.
- Kieneker LM, Gansevoort RT, Mukamal KJ, et al. Urinary potassium excretion and risk of developing hypertension: The prevention of renal and vascular end-stage disease study. Hypertension 2014;64:769-776.
- Whelton PK, He J, Cutler JA, et al. Effects of oral potassium on blood pressure. Meta-analysis of randomized controlled clinical trials. JAMA 1997;277:1624-1632.
- Geleijnse JM, Kok FJ, Grobbee DE. Blood pressure response to changes in sodium and potassium intake: A meta-regression analysis of randomised trials. J Hum Hypertens 2003;17:471-480.
- van Bommel E, Cleophas T. Potassium treatment for hypertension in patients with high salt intake: A meta-analysis. Int J Clin Pharmacol Ther 2012;50:478-482.
- World Health Organization. Guideline: Potassium Intake for Adults and Children. Geneva, Switzerland; 2012.
- Institute of Medicine. Dietary Reference Intakes for Water, Potassium, Sodium, Chloride, and Sulfate. Washington, DC: The National Academies Press; 2005.
- Cornelissen VA, Smart NA. Exercise training for blood pressure: A systematic review and meta-analysis. J Am Heart Assoc 2013;2:e004473. doi: 10.1161/JAHA.112.004473.
- Carlson DJ, Dieberg G, Hess NC, et al. Isometric exercise training for blood pressure management: A systematic review and meta-analysis. Mayo Clin Proc 2014;89:327-334.
- Cornelissen VA, Arnout J, Holvoet P, Fagard RH. Influence of exercise at lower and higher intensity on blood pressure and cardiovascular risk factors at older age. J Hypertens 2009;27:753-762.
- Klatsky AL, Friedman GD, Siegelaub AB, Gérard MJ. Alcohol consumption and blood pressure: Kaiser-Permanente Multiphasic Health Examination data. N Engl J Med 1977;296:1194-2000.
- Xin X, He J, Frontini MG, et al. Effects of alcohol reduction on blood pressure: A meta-analysis of randomized controlled trials. Hypertension 2001;38:1112-1117.
- Roerecke M, Kaczorowski J, Tobe SW, et al. The effect of a reduction in alcohol consumption on blood pressure: A systematic review and meta-analysis. Lancet Public Health 2017;2:e108-e120.
- Mukamal KJ. Understanding the mechanisms that link alcohol and lower risk of coronary heart disease. Clin Chem 2012;58:664-666.
- Hypertension Detection and Follow-up Program Cooperative Group. Five-year findings of the hypertension detection and follow-up program. I. Reduction in mortality of persons with high blood pressure, including mild hypertension. JAMA 1979;242:2562-2571.
- Fretheim A, Odgaard-Jensen J, Brørs O, et al. Comparative effectiveness of antihypertensive medication for primary prevention of cardiovascular disease: Systematic review and multiple treatments meta-analysis. BMC Med 2012;10:33.
- Cushman WC, Ford CE, Cutler JA, et al. Success and predictors of blood pressure control in diverse North American settings: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). J Clin Hypertens (Greenwich) 2002;4:393-404.
- Gradman AH, Basile JN, Carter BL, et al. Combination therapy in hypertension. J Clin Hypertens (Greenwich) 2011;13:146-154.
- Law MR, Wald NJ, Morris JK, Jordan RE. Value of low dose combination treatment with blood pressure lowering drugs: Analysis of 354 randomized trials. BMJ 2003;326:1427-1434.
- James PA, Oparil S, Carter BL, et al. 2014 evidence-based guideline for the management of high blood pressure in adults: Report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA 2014;311:507-520.
- Kaplan NM, Opie LH. Controversies in hypertension. Lancet 2006;367:168-176.
- Cushman WC, Evans GW, Byington RP, et al; ACCORD Study Group. Effects of intensive blood-pressure control in type 2 diabetes mellitus. N Engl J Med 2010;362:1575-1585.
- Wright JT Jr, Williamson JD, Whelton PK, et al; SPRINT Research Group. A randomized trial of intensive versus standard blood-pressure control. N Engl J Med 2015;373:2103-2116.
- ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: The Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA 2002;288:2981-2897.
- Ogedegbe G, Shah NR, Phillips C, et al. Comparative effectiveness of angiotensin-converting enzyme inhibitor-based treatment on cardiovascular outcomes in hypertensive blacks versus whites. J Am Coll Cardiol 2015;66:1224-1233.
- Leenen FH, Nwachuku CE, Black HR, et al. Clinical events in high-risk hypertensive patients randomly assigned to calcium channel blocker versus angiotensin-converting enzyme inhibitor in the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial. Hypertension 2006;48:374-384.
- Zanchetti A, Julius S, Kjeldsen S, et al. Outcomes in subgroups of hypertensive patients treated with regimens based on valsartan and amlodipine: An analysis of findings from the VALUE trial. J Hypertens 2006;24:2163-2168.
- Tarnow L, Rossing P, Gall MA, et al. Prevalence of arterial hypertension in diabetic patients before and after the JNC-V. Diabetes Care 1994;17:1247-1251.
- Stamler J, Vaccaro O, Neaton JD, Wentworth D. Diabetes, other risk factors, and 12-yr cardiovascular mortality for men screened in the Multiple Risk Factor Intervention Trial. Diabetes Care 1993;16:434-344.
- Estacio RO, Jeffers BW, Gifford N, et al. Effect of blood pressure control on diabetic microvascular complications in patients with hypertension and type 2 diabetes. Diabetes Care 2000;23(suppl 2):B54-64.
- Reboldi G, Gentile G, Angeli F, et al. Effects of intensive blood pressure reduction on myocardial infarction and stroke in diabetes: A meta-analysis in 73,913 patients. J Hypertens 2011;29:1253-1269.
- Adler AI, Stratton IM, Neil HA, et al. Association of systolic blood pressure with macrovascular and microvascular complications of type 2 diabetes (UKPDS 36): Prospective observational study. BMJ 2000;321:412-419.
- Emdin CA, Rahimi K, Neal B, et al. Blood pressure lowering in type 2 diabetes: A systematic review and meta-analysis. JAMA 2015;313:603-615.
- Palmer SC, Mavridis D, Navarese E, et al. Comparative efficacy and safety of blood pressure-lowering agents in adults with diabetes and kidney disease: A network meta-analysis. Lancet 2015;385:2047-2056.
- Yusuf S, Sleight P, Pogue J, et al. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N Engl J Med 2000;342:145-153.
- Fox KM. EURopean trial On reduction of cardiac events with Perindopril in stable coronary Artery disease Investigators. Efficacy of perindopril in reduction of cardiovascular events among patients with stable coronary artery disease: Randomised, double-blind, placebo-controlled, multicentre trial (the EUROPA study). Lancet 2003;362:782-788.
- Rosendorff C, Lackland DT, Allison M, et al. Treatment of hypertension in patients with coronary artery disease: A scientific statement from the American Heart Association, American College of Cardiology, and American Society of Hypertension. J Am Coll Cardiol 2015;65:1998-2038.
- Yancy CW, Jessup M, Bozkurt B, et al. 2016 ACC/AHA/HFSA focused update on new pharmacological therapy for heart failure: An update of the 2013 ACCF/AHA guideline for the management of heart failure: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Failure Society of America. J Am Coll Cardiol 2016;68:1476-1488.
- Butler J, Kalogeropoulos AP, Georgiopoulou VV, et al. Systolic blood pressure and incident heart failure in the elderly. The Cardiovascular Health Study and the Health, Ageing and Body Composition Study. Heart 2011;97:1304-1311.
- Goldstein RE, Boccuzzi SJ, Cruess D, et al. Diltiazem increases late-onset congestive heart failure in postinfarction patients with early reduction in ejection fraction. The Adverse Experience Committee; and the Multicenter Diltiazem Postinfarction Research Group. Circulation 1991;83:52-60.
- van Veldhuisen DJ, Cohen-Solal A, Bohm M, et al. Beta-blockade with nebivolol in elderly heart failure patients with impaired and preserved left ventricular ejection fraction: Data from SENIORS (Study of Effects of Nebivolol Intervention on Outcomes and Rehospitalization in Seniors With Heart Failure). J Am Coll Cardiol 2009;53:2150-2158.
- Pfeffer MA, Claggett B, Assmann SF, et al. Regional variation in patients and outcomes in the Treatment of Preserved Cardiac Function Heart Failure With an Aldosterone Antagonist (TOPCAT) trial. Circulation 2015;131:34-42.
- Matsushita K, van der Velde M, Astor BC, et al. Association of estimated glomerular filtration rate and albuminuria with all-cause and cardiovascular mortality in general population cohorts: A collaborative meta-analysis. Chronic Kidney Disease Prognosis Consortium. Lancet 2010;375:2073-2081.
- Muntner P, Anderson A, Charleston J, et al. Hypertension awareness, treatment, and control in adults with CKD: Results from the Chronic Renal Insufficiency Cohort (CRIC) Study. Am J Kidney Dis 2010;55:441-451.
- Drawz PE, Alper AB, Anderson AH, et al. Masked hypertension and elevated nighttime blood pressure in CKD: Prevalence and association with target organ damage. Clin J Am Soc Nephrol 2016;11:642-652.
- Kovesdy CP, Alrifai A, Gosmanova EO, et al. Age and outcomes associated with BP in patients with incident CKD. Clin J Am Soc Nephrol 2016;11:821-831.
- Weiss JW, Peters D, Yang X, et al. Systolic BP and mortality in older adults with CKD. Clin J Am Soc Nephrol 2015;10:1553-1559.
- Esnault VLM, Brown EA, Apetrei E, et al. The effects of amlodipine and enalapril on renal function in adults with hypertension and nondiabetic nephropathies: A 3-year, randomized, multicenter, double-blind, placebo-controlled study. Clin Ther 2008;30:482-498.
- Marin R, Ruilope LM, Aljama P, et al. A random comparison of fosinopril and nifedipine GITS in patients with primary renal disease. J Hypertens 2001;19:1871-1876.
- Cross NB, Webster AC, Masson P, et al. Antihypertensive treatment for kidney transplant recipients. Cochrane Database Syst Rev 2009;CD003598.
- Benjamin EJ, Blaha MJ, Chiuve SE, et al. Heart disease and stroke statistics — 2017 update: A report from the American Heart Association. Circulation 2017;135:e146-603.
- Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure lowering in patients with acute intracerebral hemorrhage. N Engl J Med 2013;368:2355-2365.
- Tsivgoulis G, Katsanos AH, Butcher KS, et al. Intensive blood pressure reduction in acute intracerebral hemorrhage: A meta-analysis. Neurology 2014;83:1523-1529.
- Qureshi AI, Palesch YY, Barsan WG, et al. Intensive blood-pressure lowering in patients with acute cerebral hemorrhage. N Engl J Med 2016;375:1033-1043.
- Rodriguez-Luna D, Pineiro S, Rubiera M, et al. Impact of blood pressure changes and course on hematoma growth in acute intracerebral hemorrhage. Eur J Neurol 2013;20:1277-1283.
- Qureshi AI, Ezzeddine MA, Nasar A, et al. Prevalence of elevated blood pressure in 563,704 adult patients with stroke presenting to the ED in the United States. Am J Emerg Med 2007;25:32-38.
- Castillo J, Leira R, Garcia MM, et al. Blood pressure decrease during the acute phase of ischemic stroke is associated with brain injury and poor stroke outcome. Stroke 2004;35:520-526.
- Vemmos KN, Tsivgoulis G, Spengos K, et al. U-shaped relationship between mortality and admission blood pressure in patients with acute stroke. J Intern Med 2004;255:257-265.
- Ahmed N, Wahlgren N, Brainin M, et al. Relationship of blood pressure, antihypertensive therapy, and outcome in ischemic stroke treated with intravenous thrombolysis: Retrospective analysis from Safe Implementation of Thrombolysis in Stroke-International Stroke Thrombolysis Register (SITS-ISTR). Stroke 2009;40:2442-2449.
- Dhamoon MS, Sciacca RR, Rundek T, et al. Recurrent stroke and cardiac risks after first ischemic stroke: The Northern Manhattan Study. Neurology 2006;66:641-646.
- Hardie K, Hankey GJ, Jamrozik K, et al. Ten-year risk of first recurrent stroke and disability after first-ever stroke in the Perth Community Stroke Study. Stroke 2004;35:731-735.
- Lakhan SE, Sapko MT. Blood pressure lowering treatment for preventing stroke recurrence: A systematic review and meta-analysis. Int Arch Med 2009;2:30.
- Webb AJ, Fischer U, Mehta Z, Rothwell PM. Effects of antihypertensive-drug class on interindividual variation in blood pressure and risk of stroke: A systematic review and meta-analysis. Lancet 2010;375:906-915.
- Lee M, Saver JL, Hong K-S, et al. Renin-angiotensin system modulators modestly reduce vascular risk in persons with prior stroke. Stroke 2012;43:113-119.
- Ostergren J, Sleight P, Dagenais G, et al. Impact of ramipril in patients with evidence of clinical or subclinical peripheral arterial disease. Eur Heart J 2004;25:17-24.
- Bavry AA, Anderson RD, Gong Y, et al. Outcomes among hypertensive patients with concomitant peripheral and coronary artery disease: Findings from the INternational VErapamil-SR/Trandolapril STudy. Hypertension 2010;55:48-53.
- Itoga NK, Tawfik DS, Lee CK, et al. Association of blood pressure measurements with peripheral arterial disease events: A reanalysis of the ALLHAT data. Circulation 2018. doi.org/10.1161/CIRCULATIONAHA.118.033348.
- Ruderman NB, Shulman GI. Metabolic syndrome. In: Jameson JL, ed. Endocrinology: Adult & Pediatric. Philadelphia: Elsevier Saunders; 2015:752-759.
- Wright JT Jr, Harris-Haywood S, Pressel S, et al. Clinical outcomes by race in hypertensive patients with and without the metabolic syndrome: Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). Arch Intern Med 2008;168:207-217.
- Owen JG, Reisin E. Anti-hypertensive drug treatment of patients with and the metabolic syndrome and obesity: A review of evidence, meta-analysis, post hoc and guidelines publications. Curr Hypertens Rep 2015;17:558.
- Reisin E, Owen J. Treatment: Special conditions. Metabolic syndrome: Obesity and the hypertension connection. J Am Soc Hypertens 2015;9:156-159; quiz 160.
- Healey JS, Connolly SJ. Atrial fibrillation: Hypertension as a causative agent, risk factor for complications, and potential therapeutic target. Am J Cardiol 2003;91:9G-14G.
- Healey JS, Baranchuk A, Crystal E, et al. Prevention of atrial fibrillation with angiotensin-converting enzyme inhibitors and angiotensin receptor blockers: A meta-analysis. J Am Coll Cardiol 2005;45:1832-1839.
- Rieck ÅE, Cramariuc D, Boman K, et al. Hypertension in aortic stenosis: Implications for left ventricular structure and cardiovascular events. Hypertension 2012;60:90-97.
- Eleid MF, Nishimura RA, Sorajja P, et al. Systemic hypertension in low-gradient severe aortic stenosis with preserved ejection fraction. Circulation 2013;128:1349-1353.
- Chockalingam A, Venkatesan S, Subramaniam T, et al. Safety and efficacy of angiotensin-converting enzyme inhibitors in symptomatic severe aortic stenosis: Symptomatic Cardiac Obstruction-Pilot Study of Enalapril in Aortic Stenosis (SCOPE-AS). Am Heart J 2004;147:E19.
- Scognamiglio R, Rahimtoola SH, Fasoli G, et al. Nifedipine in asymptomatic patients with severe aortic regurgitation and normal left ventricular function. N Engl J Med 1994;331:689-694.
- Masuda Y, Yamada Z, Morooka N, et al. Prognosis of patients with medically treated aortic dissections. Circulation 1991;84(5 Suppl):III7-13.
- Rampoldi V, Trimarchi S, Eagle KA, et al. Simple risk models to predict surgical mortality in acute type A aortic dissection: The International Registry of Acute Aortic Dissection score. Ann Thorac Surg 2007;83:55-61.
- Gaddum NR, Keehn L, Guilcher A, et al. Altered dependence of aortic pulse wave velocity on transmural pressure in hypertension revealing structural change in the aortic wall. Hypertension 2015;65:362-369.
- Zhang L, Tian W, Feng R, et al. Prognostic impact of blood pressure variability on aortic dissection patients after endovascular therapy. Medicine (Baltimore) 2015;94:e1591.
- Genoni M, Paul M, Jenni R, et al. Chronic beta-blocker therapy improves outcome and reduces treatment costs in chronic type B aortic dissection. Eur J Cardiothorac Surg 2001;19:606-610.
- Suzuki T, Isselbacher EM, Nienaber CA, et al. Type-selective benefits of medications in treatment of acute aortic dissection (from the International Registry of Acute Aortic Dissection [IRAD]). Am J Cardiol 2012;109:122-127.
- Erbel R, Aboyans V, Boileau C, et al; ESC Committee for Practice Guidelines. 2014 ESC Guidelines on the diagnosis and treatment of aortic diseases: Document covering acute and chronic aortic diseases of the thoracic and abdominal aorta of the adult. The Task Force for the Diagnosis and Treatment of Aortic Diseases of the European Society of Cardiology (ESC). Eur Heart J 2014;35:2873-2926.
- Dong JY, Zhang YH, Qin LQ. Erectile dysfunction and risk of cardiovascular disease: Meta-analysis of prospective cohort studies. J Am Coll Cardiol 2011;58:1378-1385.
- Gupta BP, Murad MH, Clifton MM, et al. The effect of lifestyle modification and cardiovascular risk factor reduction on erectile dysfunction: A systematic review and meta-analysis. Arch Intern Med 2011;171:1797-1803.
- Manolis A, Doumas M. Sexual dysfunction: The ‘prima ballerina’ of hypertension-related quality-of-life complications. J Hypertens 2008;26:2074-2084.
- Calhoun DA, Jones D, Textor S, et al. Resistant hypertension: Diagnosis, evaluation, and treatment: A scientific statement from the American Heart Association Professional Education Committee of the Council for High Blood Pressure Research. Hypertension 2008;51:1403-1419.
- Achelrod D, Wenzel U, Frey S. Systematic review and meta-analysis of the prevalence of resistant hypertension in treated hypertensive populations. Am J Hypertens 2015;28:355-361.
- Bangalore S, Fayyad R, Laskey R, et al. Prevalence, predictors, and outcomes in treatment-resistant hypertension in patients with coronary disease. Am J Med 2014;127:71-81.e1.
- Calhoun DA, Booth JN 3rd, Oparil S, et al. Refractory hypertension: Determination of prevalence, risk factors, and comorbidities in a large, population-based cohort. Hypertension 2014;63:451-458.
- Liu G, Zheng XX, Xu YL, et al. Effect of aldosterone antagonists on blood pressure in patients with resistant hypertension: A meta-analysis. J Hum Hypertens 2015;29:159-166.
- Zampaglione B, Pascale P, Marchisio M, Cavallo-Perin P: Hypertensive urgencies and emergencies: Prevalence and clinical presentation. Hypertension 1996;27:144-147.
- Papadopoulos DP, Sanidas EA, Viniou NA, et al. Cardiovascular hypertensive emergencies. Curr Hypertens Rep 2015;17:5. doi: 10.1007/s11906-014-0515-z.
- Keith NM, Wagener HP, Barker NW. Some different types of essential hypertension: Their course and prognosis. Am J Med Sci 1974;268:336-345.
- Gifford RW Jr. Current practices in general medicine. 7. Treatment of hypertensive emergencies including use of sodium nitroprusside. Proc Staff Meet Mayo Clin 1959;34:387-394.
- Peacock WF, Varon J, Baumann BM, et al. CLUE: A randomized comparative effectiveness trial of IV nicardipine versus labetalol use in the emergency department. Crit Care 2011;15:R157.
- Cannon CM, Levy P, Baumann BM, et al. Intravenous nicardipine and labetalol use in hypertensive patients with signs or symptoms suggestive of end-organ damage in the emergency department: A subgroup analysis of the CLUE trial. BMJ Open 2013;3:e002338. doi: 10.1136/bmjopen-2012-002338.
- Varon J, Soto-Ruiz KM, Baumann BM, et al. The management of acute hypertension in patients with renal dysfunction: Labetalol or nicardipine? Postgrad Med 2014;126:124-130.
- Wolfsthal SD. Is blood pressure control necessary before surgery? Med Clin North Am 1993;77:349-363.
- Towne JB, Bernhard VM. The relationship of postoperative hypertension to complications following carotid endarterectomy. Surgery 1980;88:575-580.
- Aronson S, Boisvert D, Lapp W. Isolated systolic hypertension is associated with adverse outcomes from coronary artery bypass grafting surgery. Anesth Analg 2002;94:1079-1084.
- Goldman L, Caldera DL. Risks of general anesthesia and elective operation in the hypertensive patient. Anesthesiology 1979;50:285-292.
- Devereaux PJ, Yang H, Yusuf S, et al. Effects of extended-release metoprolol succinate in patients undergoing noncardiac surgery (POISE trial): A randomised controlled trial. POISE Study Group. Lancet 2008;371:1839-1847.
- Espinosa A, Ripolles-Melchor J, Casans-Frances R, et al. Perioperative use of clevidipine: A systematic review and meta-analysis. PLoS ONE 2016;11:e0150625.
- Aronson S, Dyke CM, Stierer KA, et al. The ECLIPSE trials: Comparative studies of clevidipine to nitroglycerin, sodium nitroprusside, and nicardipine for acute hypertension treatment in cardiac surgery patients. Anesth Analg 2008;107:1110-1121.
- Roshanov PS, Rochwerg B, Patel A, et al. Withholding versus continuing angiotensin-converting enzyme inhibitors or angiotensin II receptor blockers before noncardiac surgery: An analysis of the Vascular events In noncardiac Surgery patIents cOhort evaluatioN Prospective Cohort. Anesthesiology 2017;126:16-27.
- Mancia G, Fagard R, Narkiewicz K, et al. 2013 ESH/ESC Guidelines for the management of arterial hypertension. Eur Heart J 2013;34:2159-2219.
- Holland N, Segraves D, Nnadi VO, et al. Identifying barriers to hypertension care: Implications for quality improvement initiatives. Dis Manag 2008;11:71-77.
- Gwadry-Sridhar FH, Manias E, Lal L, et al. Impact of interventions on medication adherence and blood pressure control in patients with essential hypertension: A systematic review by the ISPOR medication adherence and persistence special interest group. Value Health 2013;16:863-871.
This article on hypertension will cover treatments (pharmacological and nonpharmacological), initial therapy, relationship to various disease conditions (diabetes, ischemic heart disease, heart failure, chronic kidney disease, cerebrovascular disease, ischemic stroke, stroke prevention, atrial fibrillation, valvular heart disease, aortic regurgitation, sexual dysfunction), resistant hypertension, hypertensive crises and emergencies, preoperative management, and adherence strategies.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
