Subarachnoid Hemorrhage and Intracranial Hemorrhage
September 15, 2018
Reprints
AUTHORS
Brian L. Springer, MD, FACEP, Associate Professor, Director, Division of Tactical Emergency Medicine, Wright State University Department of Emergency Medicine, Dayton, OH
Adrienne Krysiak, MD, Resident, Wright State University Department of Emergency Medicine, Dayton, OH
PEER REVIEWER
Charles M. Andrews, MD, Assistant Professor, Departments of Emergency Medicine and Neurosurgery, Medical University of South Carolina, Charleston
EXECUTIVE SUMMARY
- The 16-slice or better computed tomography (CT) scan has virtually 100% sensitivity for subarachnoid hemorrhage if imaged within six hours after symptom onset.
- For patients presenting six hours after symptom onset with a normal noncontrast CT scan, lumbar puncture or CT angiography are acceptable techniques for further investigation in those at risk for subarachnoid hemorrhage.
- Risk factors for spontaneous intracranial hemorrhage include hypertension and cerebral amyloid angiopathy.
- For patients with subarachnoid hemorrhage or intracranial hemorrhage, supportive therapy with sedation, ventilatory support, prevention of hypotension, hypoxia, and hypoglycemia is important.
- Reversal of anticoagulant agents or antiplatelet agents should be discussed with a neurologist, as there is no strong evidence that such therapy increases functional outcomes.
Introduction
Spontaneous subarachnoid hemorrhage (SAH) and intracranial hemorrhage (ICH) are devastating diseases with significant mortality. For those who survive, long-term disability often is severe. The emergency physician almost exclusively will be the first doctor to lay eyes and hands on these patients. As with many other critical diagnoses, time is of the essence in management of ICH and SAH. The longer it takes to make the diagnosis and initiate treatment, whether it is surgical intervention or simply aggressive primary stabilization, the greater the risk to the patient regarding both morbidity and mortality. Identifying SAH poses additional challenges when a young and previously healthy patient appears with new-onset headache (or more challenging still, a “different” headache in a patient with chronic cephalalgia). Management of bleeding is complicated by the increasing number of patients taking anticoagulation, especially the direct-acting oral anticoagulants (DOACs), whose reversal remains challenging.
Subarachnoid Hemorrhage
Epidemiology
The epidemiology of spontaneous SAH is hard to establish because of variations in its presentation in patients of differing ethnicities and gender. In the United States, recent estimates of SAH demonstrate an incidence of 10-15 cases per 100,000 people, which is larger than previous estimates of six to eight per 100,000 in 2013. This extrapolates to a rough total of 30,000 people experiencing SAH annually. Rates are variable between populations; Japan and Finland have an estimated incidence of 22.7 and 19.7 per 100,000, respectively.1,2,3 Researchers have theorized that the higher incidence of SAH in Japan potentially is the result of the relatively older age of the Japanese population, higher rates of smoking, and genetic factors. The observed increase in SAH in the United States could be tied to the country’s aging population, with the highest incidence seen in patients younger than 25 years of age and those 85 years of age or older. Females have a higher incidence overall than males in the general population.3,4
Pathophysiology
Nontraumatic spontaneous SAH often is due to an underlying structural pathology, with approximately 85% caused by aneurysms. Other causes of spontaneous SAH include moyamoya disease, vasculitides, amyloid angiopathy, arteriovenous malformations, arterial dissection, and cerebral venous thrombosis.5,6 There is an increased incidence of cerebral aneurysms in patients with sickle cell disease and autosomal dominant polycystic kidney disease.
Nonaneurysmal SAH is much less common. Included in this category is perimesencephalic SAH, in which blood is present in the cisterns around the brainstem and there is no overt evidence of an aneurysm or structural pathology. This type of SAH has a much better prognosis. Patients often survive the initial insult and have improved neurologic and functional outcomes relative to aneurysmal SAH patients.6
There are several well-known modifiable risk factors for SAH. Cigarette smoking is strongly linked, with an associated pooled relative risk of 2-7. Hypertension leads to a 2.5 times increased risk of SAH. Excessive alcohol consumption (defined as > 150 g/week) increases risk by approximately two-fold.1,7 Of note, these modifiable risk factors lead to a measurably increased risk of disease in females relative to their male counterparts. As the population continues to age, the increased use of anticoagulants and antiplatelet agents is associated with increased risk for spontaneous SAH.8,9
Presenting Features
The presentation of SAH varies according to the amount of bleeding and its effect on the brain. Some patients present with an isolated headache; diagnosis in this group can be challenging. In patients with sudden, severe, and persistent neurologic depression, the presence of an intracranial catastrophe is obvious, and diagnosis is made more readily. Sentinel bleeds describe small leaks from aneurysms that precede overt rupture. Patients present with a headache, appear clinically well, and the symptoms often spontaneously resolve, allowing the underlying pathology of early aneurysmal bleeding to be easily missed. On subsequent presentation, patients may have a devastating bleed and significant neurologic insult. The sentinel bleed usually precedes overt SAH by one to three weeks.6,10
Studies evaluating the incidence of sentinel bleeding and headache vary widely in their conclusions, with prevalence ranging from as little as 11% to as high as 60%.4,11 There is likely a strong element of recall bias at play here; patients who end up being diagnosed with SAH may recall such a headache more readily. Most studies do not stratify incidence of sentinel bleeds based on gender, ethnicity, or age. There is a lower incidence of sentinel bleeds in elderly patients, theoretically because of age-related cerebral atrophy and concomitant enlargement of the subarachnoid space that could accommodate an increase in pressure without symptoms.4
The emergency physician should inquire about the onset and duration of headaches when patients present with them. Key features that increase the likelihood of SAH include headache reaching maximal intensity within one hour, neck stiffness, and loss of consciousness. Patients should be questioned to assess whether the headache is similar or dissimilar to previous headaches. Other concerning aspects include focal neurologic deficit and a headache combined with a decreased Glasgow Coma Scale (GCS) score.
Although asking patients if this is “the worst headache of your life” or describing a “thunderclap” headache still is common, the clinical utility in determining who requires further workup is limited. Studies have demonstrated wide confidence intervals, poor interrater reliability, and little evidence that a positive response actually will increase post-test probability of an SAH.12
The Ottawa Subarachnoid Hemorrhage Rule was developed to help differentiate SAH from more frequently encountered causes of headaches. It considers patient age, rapidity of headache onset, association with exertion, and associated neck pain/stiffness and witnessed loss of consciousness. Inclusion criteria for using the Ottawa Subarachnoid Hemorrhage Rule are alert patients ≥ 15 years of age with new severe atraumatic headache that reached maximum intensity within one hour. This rule is not valid for patients with new neurologic deficits, prior aneurysm, prior SAH, known brain tumors, or chronic recurrent headaches (three or more headaches of the same character and intensity for more than six months). (See Table 1.)
Table 1. Key Considerations in the Management of Suspected Subarachnoid Hemorrhage |
|
In appropriate patients, the Ottawa Subarachnoid Hemorrhage Rule essentially has 100% sensitivity, so patients who have none of the six criteria can be considered to have spontaneous SAH ruled out.13,14
To add to the diagnostic complexity, patients with chronic migraines (some 12% of the population) may present with headache symptoms that mimic those of SAH. Complex migraines can present with focal neurologic deficits along with marked elevation in blood pressure, nausea, vomiting, and photophobia or phonophobia. It is important to evaluate and document the character and features of patients’ headaches closely to avoid misdiagnosis of SAH as a complex migraine, especially in patients with a history of frequent migraine headaches. Given the range of stroke subtypes, avoid diagnosing any patients with a complex migraine if they have not had one previously.6
Physical examination findings consistent with SAH include the presence of focal neurologic deficits and meningeal symptoms (i.e., inability to flex the neck). Much like with historical findings, research has shown that the interphysician interpretation and documentation of findings such as neck rigidity are highly variable, and inconsistencies in grading such symptoms make systematic review difficult. Studies have failed to identify clinical features that have adequate predictive value for SAH; no single feature can include or exclude the diagnosis.6,12,13
SAH may cause sudden collapse and cardiac arrest, and both rescuers and treating physicians are likely to seek a primary cardiac etiology rather than consider a neurologic etiology. In patients with witnessed out-of-hospital cardiac arrests, features suggestive of SAH include sudden headache before collapse, an initial rhythm other than ventricular fibrillation, female gender, and normal serum cardiac troponin.15
Electrocardiogram (ECG) changes in relation to cerebral insult have been well-described. The mechanism behind the ECG findings is likely due to cerebral arteriolar spasm near the hypothalamus, which, via a feedback loop, causes sympathetic stimulation of the heart.16 The presence of ECG abnormalities also is linked strongly to the development of neurogenic pulmonary edema (NPE). NPE has a well-known association with SAH and its occurrence portends a poor outcome. Risk of NPE is linked to the severity of disease and of neurologic deficits, and to a history of diabetes.
Persistent hyperglycemia after SAH is an independent predictor for poor clinical outcomes.17,18 It is believed that hyperglycemia seen after SAH likely is multifactorial, in large part because of the direct effects of catecholamine release, and then worsened by catecholamine and cortisol’s role in enhancing insulin resistance. There is no evidence that treating the hyperglycemia with insulin is beneficial. Equally concerning, there is evidence that, in general, SAH patients and critically ill patients fare poorly when they become hypoglycemic, creating an additional concern of overshoot when attempting to treat hyperglycemia.19
Diagnosis and Imaging
Headache is one of the most common chief complaints of patients presenting to the emergency department (ED), accounting for more than 3 million visits annually. Roughly 27,000 to 30,000 cases of SAH are seen annually, making this a not-uncommon event, but one hidden among a vast number of headaches, most of which are benign. Given the prevalence of the complaint of headache and the relatively small number that actually are due to a life-threatening etiology, it is easy for the physician to fail to diagnose SAH as a potential cause. As a result, approximately 5% of the time, SAH is misdiagnosed during the initial ED visit. The younger average age of patients who experience SAH/hemorrhagic strokes also may lead to delayed diagnoses, given the lower overall incidence.12,20
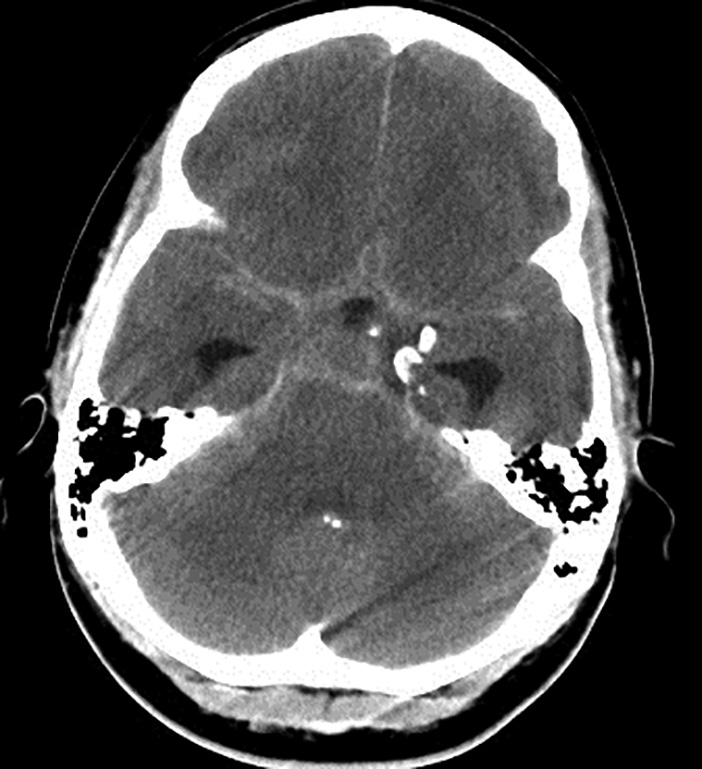
Radiographically, SAH is detected best within the first few hours of bleeding. (See Figure 1.) Diagnostic accuracy begins to decline once the hyperdense blood appears more similar to surrounding cerebral cortex because of the normal flow of cerebrospinal fluid (CSF).
Figure 1. Subarachnoid Hemorrhage |
 |
|
Image courtesy of J. Stephan Stapczynski, MD |
There are significant implications when SAH is not diagnosed on the initial visit, with an increased risk for death at three and 12 months (unadjusted odds ratio of 3.4 and 4.7, respectively) compared to patients diagnosed on the initial visit.20
To avoid missing an SAH, lumbar puncture (LP) has been adopted as the follow-up to a negative CT scan. Unfortunately, LPs come with their own host of complications. Post-LP headache is a well-known complication of the procedure and, although relatively benign in nature, it becomes a more worrisome and potentially complicating factor when SAH is suspected. It is worth noting that many of the studies that had demonstrated substandard detection of SAH on isolated CT scan were performed 10 or more years ago. The evolution of the CT scanner to include 32/64 slices, high resolution (also called thin-section), spectral imaging, and better correction of motion artifact has improved diagnostic accuracy drastically.6,12,20 In a meta-analysis of five studies using the 16-slice or greater CT scan, the sensitivity for detecting SAH within six hours after symptom onset was 98.7% (95% confidence interval [CI], 97.1-99.4%) in a neurologically normal patient with thunderclap headache presentation and a clear time of onset.21 Regardless of the CT protocol, it still generally is accepted that the time from symptom onset reduces CT sensitivity, and that the diagnosis of SAH by CT is best performed early, ideally within six hours.6,12,13,21,22
In a single-center study from the Netherlands of patients enrolled between 2005 and 2012, the sensitivity of the CT scan was 98.5% (95% CI, 92.1-100%) when performed within six hours and dropped to 90.0% (95% CI, 76.3-97.2%) if performed after six hours.22
Traditionally, LP is performed as a follow-up test when the CT is negative but the emergency physician still has a high clinical suspicion for SAH. An LP is performed to evaluate CSF for the presence of red blood cells and xanthochromia. The LP may be negative if performed very early (less than two hours) after SAH occurs and is most sensitive 12 hours after symptom onset.23 There is no established red blood cell (RBC) count that represents a positive tap. Additionally, a traumatic tap can complicate interpretation of the test.
Optimally, LP should be performed by the most experienced staff at least six hours (and ideally 12 hours) after symptom onset. A small (22-gauge) LP needle should be used to prevent a sudden drop in CSF pressure that theoretically could trigger aneurysm rupture.24
To differentiate between a traumatic and a positive tap, the first and last tubes may be compared, with an expected drop in RBC count in a traumatic tap and persistent elevation seen in SAH. Additionally, the specimen may be spun down and assessed for xanthochromia, a yellow discoloration caused by the breakdown of RBCs and the release of heme pigments into the CSF. It takes several hours for xanthochromia to occur, but it is present in almost all cases of SAH at 12 hours post-bleed, hence the high sensitivity for LP at that time. Spectrophotometry is the most reliable way to detect xanthochromia; unfortunately, it is used in as little as 1% of U.S. EDs.6,10
The LP may establish an alternative diagnosis in a small number (3%) of suspected SAH cases, although in the emergent setting, it alters the subsequent management of the patient in as little as 0.44% of cases.12
Along with a traumatic tap, the risks of LP include localized procedural pain, infection, and post-LP headache. A post-LP headache occurs in approximately one out of every six LPs, and the pain may be greater than that of the patient’s presenting headache.12,13,25
LPs appear to be truly effective at finding missed SAH when the CT-negative patient’s pre-LP probability of SAH is 5%, calculating a number needed to LP of 250 to find one aneurysmal SAH.12 A well-powered observational study found a low diagnostic yield for CT-negative patients who subsequently underwent LP. The findings were bolstered by the use of spectrophotometric analysis of CSF for xanthochromia, which, as noted earlier, is rarely used in the United States.26
A recent editorial published in Stroke addressed the question of whether LP is necessary in patients with suspected SAH who are CT-negative within six hours of headache onset.27 This has important implications in the busy ED: It potentially could relieve some of the burden on busy emergency physicians and could reduce risks to patients of potential infection, localized pain, and post-LP headache. There were multiple caveats if the LP is to be skipped: The less than six-hour timeline must be followed strictly; this only applies to patients presenting with headache, not dizziness, nausea, neurologic deficits, or other symptoms; and the CT must be read by an experienced neuroradiologist. Because of a large drop in sensitivity, emergency physicians still should consider obtaining an LP beyond six hours.
CT angiography (CTA) has gained popularity in recent years for its ability to detect small arterial pathology, including carotid dissections and intracranial aneurysms. CTA recently has been demonstrated to offer a pooled sensitivity of 98% and pooled specificity of 100% for the detection of aneurysm, with a miss rate of less than 1%.6,10 One possible approach to the patient presenting with concern for SAH is to obtain both a CT and a CTA. A drawback to this approach is that it is not possible to differentiate between bleeding and non-bleeding aneurysms on CTA. If the approach is to obtain a CTA in all possible SAH patients, emergency physicians eventually will uncover small, incidental aneurysms that may be unrelated to the patients’ symptoms. This creates a number of problems, including additional downstream testing and possible unnecessary surgery, as well as significant anxiety for the patients and their families. Some argue that finding any aneurysm is prudent in the prevention of SAH, as demonstrated by studies of patients with SAH in which 47-48% were less than 5 mm.28
Unfortunately, there are no strong comparative studies demonstrating superiority of CT/LP vs. CTA in the diagnosis of SAH. As discussed earlier, in the right patient presenting with a sudden onset of headache of less than six hours, a negative high-quality CT read by a qualified radiologist can be considered sufficient and testing can stop at that point. LP or CTA should be reserved for patients outside of the window or in whom pretest probability is high (strong family history, prior aneurysm or bleeding, etc.). Finding an aneurysm in a patient with high pretest probability of SAH should elicit consultation with neurosurgery. CT/CTA might be a reasonable approach in patients who are poor candidates for LP or who refuse the procedure and have a high pretest probability for SAH. As noted, the presence of an aneurysm does not confirm that the emergency physician has found the source of the headache and will require consultation for further evaluation in the hospital.
Acute Interventions
The primary goals in the management of patients with SAH are rapid stabilization, limitation of the effects of bleeding on the surrounding brain tissue, and the prevention of rebleeding, which is associated with poor neurologic outcomes. In early evaluation of patients presenting with suspected SAH, the primary focus is on the ABCs (airway, breathing, circulation), and emergency physicians should determine the need to intubate quickly. Prior to intubation, emergency physicians should optimize blood pressure and pre-oxygenation. Both profound hypotension and hypertension can worsen secondary injury, and physicians should use medications with which they are familiar to ensure adequate sedation while simultaneously not causing hypotension. In efforts to preserve the neurologic examination, medications with short half-lives, such as fentanyl and low doses of opioids, are preferred as sedative agents to optimize intubating conditions and minimize patient agitation. When possible, the most experienced physician should perform the intubation to limit multiple passes that can lead to hypoxia and secondary brain injury.29
The patient’s baseline GCS should be calculated to allow for tracking of neurologic status and to be used as a guide for potential surgical management. In addition, SAH severity can be rated using the Hunt and Hess scale (or similarly, the World Federation of Neurological Surgeons). Like the GCS, the Hunt and Hess scale is used by neurosurgeons to predict neurologic outcomes and guide the need for surgical intervention; ideally, the results should be calculated prior to administration of any sedating medications.30
Blood pressure management is critical, as both extremes of hypotension and hypertension can compromise cerebral perfusion pressure and exacerbate tissue injury. To date, there is no clear blood pressure goal, but rather a range that often is determined by premorbid blood pressure. The American Stroke Association’s 2012 guidelines recommend a systolic blood pressure less than 160 mmHg.31 However, overaggressive lowering of blood pressure can lead to underperfusion and resultant ischemia. Therefore, close monitoring in consultation with neurospecialists is necessary. Placement of an arterial line can help drive real-time management of blood pressure.
In cases of severely hypertensive patients, emergency physicians should use agents with predictable titratability and pharmacokinetics. Medications that fit this metric include labetalol, clevidipine, and nicardipine. Given their comparative ease of use and predictable effects, these three are the preferred agents according to American Heart Association guidelines.6,31 Nicardipine is easily titratable and has a short half-life, which can help avoid hypotension, and there is solid evidence backing its efficacy in preventing arterial vasospasm. Although beta-blockers may promote cardioprotective benefits via a decrease in the catecholamine surge thought to occur with SAH and elevated intracranial pressure (ICP), there is no evidence to suggest that beta-blockers be used in lieu of calcium channel blockers.32
Patients presenting with SAH who are on anticoagulants will need rapid reversal. It follows that reversal should be accomplished by the most effective and rapidly acting therapy. Patients on warfarin with a prolonged prothrombin time should receive 4-factor prothrombin complex concentrate and vitamin K. Reversal of the DOACs in patients with SAH has not been well studied, and reversal of antiplatelet agents in intracerebral bleeding is controversial. Both DOAC and antiplatelet reversal are discussed further in the section on ICH; the emergency physician should consult with the neurointensivist quickly after obtaining information on the specific DOAC or antiplatelet agent, dosing strength, and most recent dose taken.
In cases in which the neurosurgical intervention may be delayed because of prolonged transportation times, consideration should be given to administration of a 1 g dose of tranexamic acid (TXA). Matched with placebo controls, TXA administration decreased early rebleeding and reduced mortality. However, TXA is associated with potential cerebral ischemic complications in SAH, and neurosurgery should be consulted prior to administration.10,33
Regardless of initial presenting blood pressures, arterial vasospasm is a well-known consequence of subarachnoid bleeding and can lead to worsening neurologic outcomes. Vasospasm classically occurs three to 10 days after the initial bleed.10 Although vasospasm frequently is managed in the ICU or on the floor, patients with delayed presentations (days) of SAH should prompt emergency physicians to begin early treatment after consultation with neurospecialists. Nimodipine modulates vascular flow by preventing the influx of calcium into smooth muscle cells and is associated with improved outcomes. Routine use of nimodipine currently is recommended with level IA evidence by the American Stroke Association.6 Regimens include either oral or NG dosing.
Although seizures are seen in up to one-fourth of patients presenting with SAH, routine use of antiepileptic medications has questionable benefit. Neither phenytoin nor levetiracetam has been shown to reduce seizures significantly in SAH patients when administered prophylactically.6,34 Patients who seize while in the ED should be managed acutely as any patient with a seizure. Ensure the ABCs are maintained, start with administration of intravenous (IV) benzodiazepines, and consider loading with an antiepileptic in consultation with the neurosurgeon or intensivist.
Ultimately, SAHs caused by aneurysms are managed definitively with clipping/coiling of the lesion. This is managed best at high-volume tertiary care centers. Thus, early identification of SAH by ED physicians should prompt interhospital transfer as needed to better manage patients with suspected SAH. Most experts recommend that surgical intervention occur within 24 hours of symptom onset (of course, this may be delayed because of delayed patient presentation.) As previously noted, consideration should be given to TXA administration when transfer may be prolonged (12 hours or longer).35
Intracranial Hemorrhage
Epidemiology
Spontaneous ICH makes up only 10-20% of all strokes. Despite an overall decline in incidence of hemorrhagic and ischemic stroke (thought to be the result of better control of common risk factors for each), the case fatality and long-term fatality rates of ICH remain relatively unchanged. The incidence of ICH is estimated at 24.6 cases per 100,000 person years, with a case fatality rate of 40% at one month and 54% at one year. Decreases in in-hospital and 30-day mortality probably reflect improved neurocritical and stroke unit care, where there has been improvement in diagnostic and management strategies. Still, chances for meaningful recovery are grim, with only 12-39% of patients achieving long-term functional independence.35,36,37
The risk of ICH doubles every decade after the age of 35 years, with males 55 years of age and older at greatest risk. The incidence appears to be higher among Japanese and Afro-Caribbean populations.36
Pathophysiology
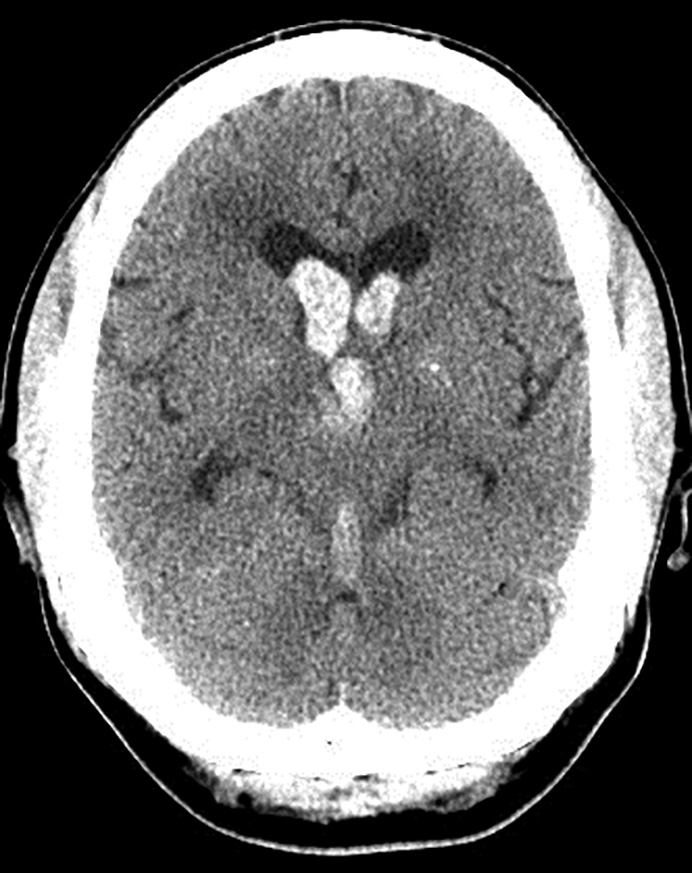
Primary spontaneous ICH results from the rupture of small blood vessels, most commonly those damaged by hypertension or cerebral amyloid angiopathy. Hypertension is the most common and important risk factor for the development of ICH, with 75% of hemorrhages occurring with a background of elevated blood pressure. Effective blood pressure control with antihypertensive medications has been shown to reduce the risk of spontaneous ICH significantly, and trends in improved control of hypertension likely account for the overall declining incidence of ICH.36,37 Long-standing hypertension results in damage to perforating arteries deep within brain structures, such as the thalamus, basal ganglia, and pons, with resultant deep hemorrhages that extend into the ventricles. Hypertension also is linked strongly to the development of idiopathic primary intraventricular hemorrhage, in which intraventricular bleeding occurs without parenchymal involvement or evidence of other structural cerebrovascular abnormalities (see Figure 2), accounting for about 3% of all ICH cases.38
Figure 2. Intraventricular Hemorrhage |
 |
|
Image courtesy of J. Stephan Stapczynski, MD |
Cerebral amyloid angiopathy results from deposition of beta-amyloid protein into the adventitia of cortical perforating vessels, leading to necrosis of the vessel wall and subsequent hemorrhage into the cortical and subcortical regions of the brain. Cerebral amyloid angiopathy is thought to be present in half of those older than 90 years of age and is the leading cause of lobar hemorrhage in people older than 70 years of age.35,36 Common risk factors include older age, history of ischemic stroke, heavy alcohol abuse, and abuse of sympathomimetic drugs such as cocaine and methamphetamine. Secondary causes of ICH include vascular malformations (arteriovenous malformation, cavernous hemangiomas, intracranial aneurysms, venous sinus thrombosis), hemorrhagic conversion of ischemic stroke, coagulopathy, tumors (primary or metastatic), and vasculitis.35,36
Use of anticoagulant medications is a risk factor for the development of ICH, especially in patients taking long-term warfarin or DOACs, with patients having a four-fold increase in risk for ICH. Concomitant use of aspirin and other antiplatelet medications increases the risk slightly, including in patients already receiving warfarin.35,36,39 Additional risk factors for ICH in anticoagulated patients include age older than 75 years, hypertension, history of cerebrovascular disease, and international normalized ratio (INR) > 4.0.
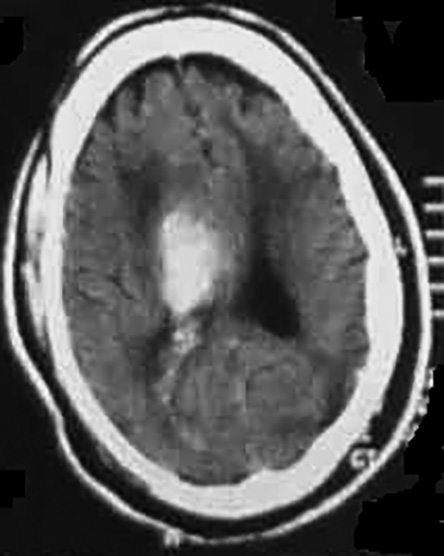
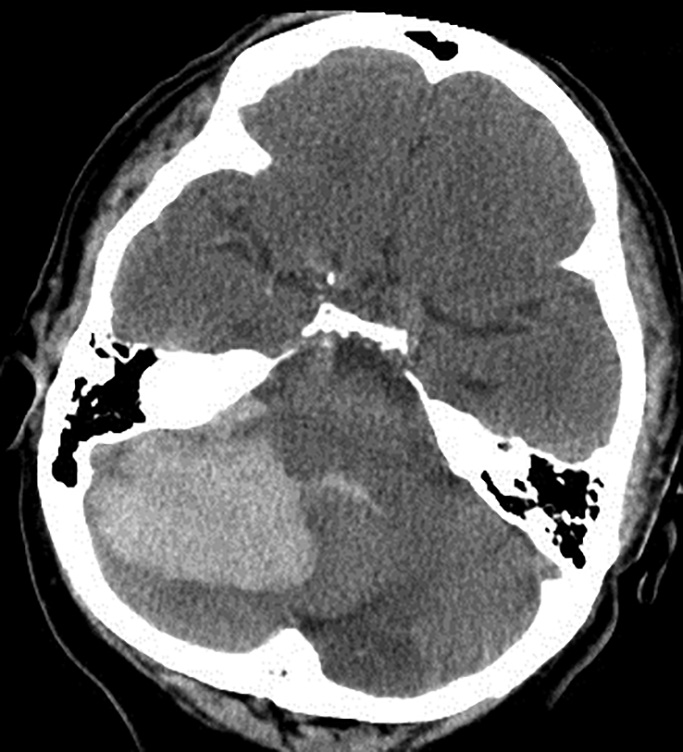
The most common locations for ICH are the basal ganglia (see Figure 3), thalamus, pons, and cerebellum (see Figure 4).2 Primary intraventricular hemorrhage occurs in approximately 2-3% of bleeds.38 Lobar hemorrhage is seen most often in the occipital lobes, followed by the frontal, temporal, and parietal lobes.
Figure 3. Basal Ganglia Hemorrhage |
 |
|
Image courtesy of J. Stephan Stapczynski, MD |
Figure 4. Cerebellar Hemorrhage |
 |
|
Image courtesy of J. Stephan Stapczynski, MD |
Primary brain injury occurs immediately from the rapid spread of the hematoma across white matter planes, causing direct and rapid tissue destruction. The next several days to weeks confer a risk of secondary injury from multiple mechanisms. Hematoma expansion commonly continues for 24 hours after symptom onset because of ongoing hemorrhage from the primary source, as well as vessel disruption and surrounding coagulopathy. The greatest risk occurs in the first few hours.
Perihematoma edema develops early and lasts days to weeks, reflective of the release of osmotically active serum proteins and other cytotoxic and vasogenic mechanisms. Severe edema is associated with poor outcomes, even in small-volume bleeds. Ventricular extension of the hematoma or ventricular obstruction from displaced brain tissue can cause hydrocephalus, which also is associated with worse outcomes.35,36
Presenting Features
ICH produces a multitude of possible presenting features, which are not specific for ICH and cannot be differentiated from ischemic stroke and other neurologic disorders without the use of neuroimaging.35 Clinical features of ICH may be generalized or location-dependent. The specific constellation of symptoms will depend on the location of the bleeding, as well as its effect on the surrounding brain tissue. As a general rule, ICH at least must be considered in any case of sudden onset of acute neurologic symptoms.
Generalized features resulting from increased intracranial pressure include headache, nausea and vomiting, reduced level of consciousness, seizures, and acute hypertension. Nuchal rigidity can occur when blood is present in the ventricles and may be seen in idiopathic primary intraventricular hemorrhage.
Location-dependent clinical features often are progressive focal neurological deficits, peaking during the first 24 hours because of previously discussed secondary mechanisms of injury. Supratentorial lesions can result in high cortical dysfunction, such as aphasia, hemianopia, and neglect. Infratentorial lesions result in contralateral motor deficits, gaze and cranial nerve abnormalities, or cerebellar dysfunction (ataxia, dysmetria).35,36
Although uncommmon, onset (upon initial presentation) and early seizures (occurring within the first seven days of bleeding) can occur in patients with ICH. Onset seizures are associated with both patient factors (younger age, prior ICH) and factors related to the bleed (cortical involvement, initial severity of neurologic deficits). However, neither onset seizures nor early seizures have been proven to be independent factors influencing patient outcomes at six months.40
Diagnosis and Imaging
The emergency physician should obtain a brief medical history from the patient, bystanders, or emergency medical services (EMS) in an attempt to elicit symptoms, time of onset, recent trauma, prior ischemic or hemorrhagic stroke, and use of oral anticoagulants.
Neuroimaging remains the hallmark of ICH diagnosis and should be obtained quickly. Delays in neuroimaging are associated with long-term mortality.35 The most commonly used imaging modalities in the diagnosis and management of ICH include CT, magnetic resonance imaging (MRI), and CT/MR angiography (MRA).
Noncontrast CT remains the imaging study of choice in the early assessment of ICH because of its availability, patient tolerability, cost, and scan duration.41 CT without contrast allows for rapid detection, determination of the bleed’s location and size, and assessment of the presence of intraventricular bleeding. Hemorrhage will appear as an interaxial, hyperdense area of consolidation, often with associated mass effect. (See Figures 2-4.) The presence of such a lesion is 98% sensitive and 100% specific for acute ICH.35,41
This appearance will last for several days, gradually losing its high attenuation signal until it becomes hypoattenuated relative to the brain parenchyma. Large hematomas and the presence of heterogenous attenuation of the hematoma are predictors of hematoma expansion.
The addition of IV contrast also has some prognostic value in risk for hematoma expansion. The presence of contrast extravasation into the hematoma (spot sign) with or without the presence of a linear density extending from the middle cerebral artery into the hematoma and toward the spot sign (spot-and-tail sign) are predictive for markedly greater risk of hematoma expansion and acute neurologic deterioration.35,41,42
Gradient-echo MRI is as sensitive as CT in detecting spontaneous ICH, and is more accurate in detecting structural abnormalities, brain edema, chronic bleeding, and herniation. However, in the acute setting, MRI is limited by patient factors, including depressed level of consciousness, airway control, hemodynamic instability, agitation, or metallic implants.36,41
In the emergent setting, CT angiography is less invasive and less resource intensive than traditional angiography and may be useful in detecting causal vascular anomalies and aneurysms, with a sensitivity 97% and specificity of 98%. Direct angiography remains the gold standard for vascular lesions and should be considered when clinical suspicion is high for secondary causes, such as in lobar or primary intraventricular hemorrhage.
Younger patients with normal blood pressure should be considered strongly for either direct angiography or MRI/MRA because of the increased risk for vascular pathology.35 Temporal imaging during direct angiography allows for identification of feeding branches and drainage pathways of vascular malformations and allows for possible interventional management by way of interventional radiology or neurosurgery.41
MRI/MRA in the subacute stage is almost as accurate as direct angiography in detecting vascular abnormalities and can detect other causes of hemorrhage, such as cavernoma, malignancy, and hemorrhagic transformation of an ischemic infarct.
Delayed intraventricular hemorrhage may occur in up to 21% of patients with ICH. As a general rule, repeat imaging should be obtained in any patient who experiences acute neurologic deterioration.35,42
Acute Interventions
Rapid decline is not uncommon in patients with ICH, so aggressive therapy must be instituted as early as possible. Between 15-23% of patients have hematoma expansion and neurological decline in the first several hours after presentation, and more than 20% of patients experience a decrease of two or more points in their GCS after initial assessment by EMS.
The initial focus always must be on the ABCs, and protection of the airway may need to precede neuroimaging. (See Table 2.) Obtunded or comatose patients or those with impaired gag reflex, severe respiratory distress, or excessive vomiting should receive prompt airway management with rapid sequence induction and intubation.35,42 Ventilatory management is required in up to 21% of ICH patients, usually because of inability to protect the airway, and is associated with high rates of in-hospital mortality.
Table 2. Key Considerations in the Management of Intracerebral Hemorrhage |
|
Acute respiratory distress syndrome (ARDS) occurs in about one-fourth of ventilated ICH patients, possibly because of neurogenic pulmonary edema. Traditional management of ARDS in these patients must balance the potential barotrauma benefits of permissive hypoxia/hypercapnia with the potential harms of worsening secondary brain injury, but there is not good evidence to break from the most recent recommendations of using lower tidal volumes to prevent acute lung injury.43
Once the primary survey has been completed, fully expose the patient and perform a detailed secondary survey looking for any focal neurologic deficits or traumatic injury, being especially vigilant for injury that may have occurred as a result of decreased level of consciousness and prolonged down time.36
Cardiac monitoring should be instituted and patients should be monitored carefully in the ED, especially when IV medications are instituted for blood pressure control. Electrophysiological findings in patients with deep ICH include bradydysrhythmias and tachydysrhythmias, ST abnormalities, and QT abnormalities, not unlike those seen in SAH, as discussed earlier. This is also likely from the same mechanism.15,16,44
Elevated blood pressure immediately following the onset of ICH has been linked to hematoma expansion, acute neurologic deterioration, and poor outcomes.45,46 Blood pressure management has not been shown definitively to reduce risks of death or major disability at 90 days, but may decrease hematoma size and improve functional outcomes (as defined by improved modified Rankin scores at 90 days).47,48 Controversy arises in the possible decrease in cerebral perfusion pressure and worsening of secondary injury that aggressive blood pressure reduction may exacerbate. In patients with rapid reduction of blood pressure, MRI sometimes detects small areas of subacute ischemia. This demonstrates how many interventions come at a cost: Aggressive blood pressure reduction must be balanced with prevention of ischemia.49
The most recent guidelines from the American Heart Association recommend the following: For patients with ICH who have a systolic blood pressure (SBP) between 150 and 220 mmHg and who do not have contraindications to acute blood pressure treatment, acute lowering of SBP to 140 mmHg is safe and can be effective for improving functional outcome. For SBP > 220 mmHg, initiate aggressive blood pressure control with a continuous and closely monitored IV infusion.50 The guidelines do not recommend any specific agent, noting that the most commonly used medications are beta-blockers (e.g., labetalol) and calcium channel blockers (e.g., nicardipine). Nitrates are associated with cerebral vasodilation, impaired autoregulation, and increased intracranial pressure and should be avoided. Patients must be monitored closely to avoid overshoot and maintain cerebral perfusion pressure.35
As noted earlier, the use of oral anticoagulant medications is associated with an increased risk of ICH as well as worse outcomes. Most bleeds occur at therapeutic levels; however, overanticoagulation is associated with an even greater risk of bleeding and complications.51 Current management strategies focus on the aggressive correction of coagulopathy in patients using vitamin K antagonists such as warfarin. However, there is limited evidence for optimal reversal of DOACs or for antiplatelet agents.50
Reversal of warfarin coagulopathy in the setting of ICH is a critical action that should be initiated immediately. The most common medical options for reversal are the use of IV vitamin K, fresh frozen plasma (FFP), or prothrombin complex concentrates (PCC). IV vitamin K takes more than six hours to normalize the INR, and thus should be administered as soon as possible in conjunction with either FFP or PCC. Vitamin K is administered slowly at doses of 5 to 10 mg. Patients should be monitored carefully for anaphylaxis during the infusion.35 A growing body of literature supports PCC vs. FFP for reversing the effects of warfarin in patients with ICH. Compared to FFP, PCC contains higher levels of vitamin K-dependent cofactors, can be administered more rapidly, requires a smaller volume of infusion, and reverses the INR more quickly. However, PCC is associated with high rates of thrombotic complications.51 Investigators for the International Normalised ratio normalisation in patients with Coumadin-related intracranial Haemorrhages (INCH) trial, a multicenter trial comparing the two agents, began recruiting subjects in 2009, but the trial was stopped early in 2015 because of safety concerns. The researchers concluded that in patients with vitamin K antagonist-related ICH, 4-factor PCC might be superior to FFP with respect to normalizing INR, and faster INR normalization was associated with smaller hematoma expansion. No clinical benefit to using PCC over FFP was demonstrated.52
Reversal of DOACs in patients with ICH has not been well studied. Dabigatran may be partially reversed by PCC, recombinant factor VIIa, or hemodialysis (especially in patients with renal insufficiency). If available, the reversal agent idarucizumab should be given in two 2.5 mg IV doses.42,53 Rivaroxaban and apixaban also may be partially reversed by 4-factor PCC. Hemodialysis is less likely to be effective for these medications because of greater protein binding. Consider the use of activated charcoal to reduce further absorption of any DOAC if the patient presents within two hours of ingestion.42,50 The FDA has just approved andexanet alfa, a factor Xa-inhibitor antidote indicated for patients treated with rivaroxaban and apixaban, but it is very costly and few hospitals have obtained it.54
In patients being treated with heparin or therapeutic (as opposed to prophylactic) low molecular weight heparin, a protamine sulfate should be administered, with the dosage tailored to the amount of heparin given and the timeframe of when it was administered last. For patients on aspirin, clopidogrel, or other antiplatelet therapy, there has not been a demonstrated mortality benefit from the use of platelet transfusions or desmopressin acetate (DDAVP).42,50,51 If a neurosurgical procedure is going to be done, perform platelet function testing, and if abnormal or such testing is not readily available, it is reasonable to transfuse platelets.55,56 DDAVP can be considered in patients on cyclooxygenase inhibitors such as celecoxib or ADP-receptor inhibitors such as clopidogrel and prasugrel.42
Once a patient has been identified as experiencing ICH, the emergency physician should consult with neurocritical care and neurosurgery immediately to facilitate management. Even the relatively stable, non-comatose patient with ICH runs the risk of rapid deterioration and will require close monitoring in the ICU. Risk factors for deterioration include elevated SBP (> 180 mmHg), hemorrhage at the brainstem level, presence of intraventricular hemorrhage, and larger hematoma size.57,58,59,60
Elevated ICP in patients with ICH may result from the hematoma, surrounding edema, or both.51 In comatose patients who present with signs of intracranial hypertension (intraventricular hemorrhage with hydrocephalus, mass effect, or herniation on imaging), early treatment should be focused on reducing intracranial pressure and enhancing cerebral blood flow. Ensure the patient is adequately sedated and that the sedatives used does not result in hypotension, which will compromise cerebral blood flow further. Elevate the head of the bed to 20-30 degrees, keeping the patient’s head midline. Consider the administration of an osmotic diuretic such as mannitol or hypertonic saline. Hyperventilation to a PaCO2 of 25 mmHg to 30-35 mmHg generally is not recommended, as the effect is transient and decreases cerebral blood flow. It should be considered only as a bridge to surgical decompression in patients who have failed other interventions and are at immediate risk of death from herniation.36,42,51,61
Fever is common after spontaneous ICH. The risk of fever is increased in patients who have a larger hematoma size and in those with intraventricular extension. Fever is a poor prognostic factor in patients with ICH. It is associated with higher mortality and worse neurologic outcomes.62 Maintenance of normothermia to limit secondary injury caused by hypothermia remains a reasonable strategy, with the American Heart Association recommending that febrile ICH patients be cooled to maintain a core temperature below 38° C. Techniques include the use of cooling blankets and acetaminophen.35,36,50
Up to 28% of ICH patients may develop seizures, with up to half being nonconvulsive (electrographic seen on continuous EEG monitoring) and most occurring within the first 24 hours after ICH. Seizures are seen most often in younger, intubated patients and are associated with surgical intervention and longer hospital length of stay. Prospective and population-based studies have not shown an association between clinical seizures and neurological outcome or mortality.50,51 Patients who have clinical seizures or electrographic seizures with a change in mental status should receive treatment with anticonvulsant drugs. Consider continuous EEG monitoring in patients who have a depressed mental status disproportionate to the degree of brain injury. These patients should receive a benzodiazepine, such as lorazepam or diazepam, immediately for rapid seizure control, accompanied by phenytoin, fosphenytoin, or levetiracetam loading for longer-term control. Prophylactic treatment is not recommended and, in fact, is associated with worse outcomes.35,50,51
REFERENCES
- Rammohan G, Kravchik L, Werman H. Spontaneous subarachnoid hemorrhage. Emerg Med Rep 2016;37:114-124.
- Bogason ET, Anderson B, Brandmeir NJ, et al. The epidemiology of admissions of nontraumatic subarachnoid hemorrhage in the United States. Neurosurgery 2014;74:227-229.
- de Rooij NK, Linn FH, van der Plas JA, et al. Incidence of subarachnoid haemorrhage: A systematic review with emphasis on region, age, gender and time trends. J Neurol Neurosurg Psychiatry 2007;78:1365-1372.
- Oda S, Shimoda M, Hirayama A, et al. Neuroradiologic diagnosis of minor leak prior to major SAH: Diagnosis by T1-FLAIR Mismatch. AJNR Neuroradiol 2015;36:1616-1622.
- Meurer WJ, Walsh B, Vilke GM, Coyne CJ. Clinical guidelines for the emergency department evaluation of subarachnoid hemorrhage. J Emerg Med 2016;50:696-701.
- Abraham MK, Chang WW. Subarachnoid hemorrhage. Emerg Med Clin North Am 2016;34:901-916.
- Feigin VL, Rinkel GJ, Lawes CM, et al. Risk factors for subarachnoid hemorrhage: An updated systematic review of epidemiological studies. Stroke 2005;36:2773-2780.
- García-Rodríguez LA, Gaist D, Morton J, et al. Antithrombic drugs and risk of hemorrhagic stroke in the general population. Neurology 2013;81:566-574.
- Konczalla J, Kashefiolasl S, Brawwanski N, et al. Increasing numbers of nonaneurysmal subarachnoid hemorrhage in the last 15 years: Antithrombic medication as a reason and prognostic factor? J Neurosurg 2016;124:1731-1737.
- Long B, Koyfman A, Runyon MS. Subarachnoid hemorrhage: Updates in diagnosis and management. Emerg Med Clin North Am 2017;35:803-824.
- Pereira JL, de Albuquerque LA, Dellaretti M, et al. Importance of recognizing sentinel headache. Surg Neurol Int 2012;3:162.
- Carpenter CR, Hussain AM, Ward MJ, et al. Spontaneous subarachnoid hemorrhage: A systematic review and meta-analysis describing the diagnostic accuracy of history, physical examination, imaging, and lumbar puncture with an exploration of test thresholds. Acad Emerg Med 2016;23:963-1003.
- Perry JJ, Stiell IG, Sivilotti ML, et al. Clinical decision rules to rule out subarachnoid hemorrhage for acute headache. JAMA 2013;310:1248-1255.
- Perry JJ, Siviolotti MLA, Sutherland J, et al. Validation of the Ottawa Subarachnoid Hemorrhage Rule in patients with acute headache. CMAJ 2017;189:E1379-E1385.
- Inamasu J, Miyatake S, Tomioka H, et al. Subarachnoid haemorrhage as cause of out-of-hospital cardiac arrest: A prospective computed tomography study. Resuscitation 2009;80:977-980.
- Chen WL, Huang CH, Chen JH, et al. ECG abnormalities predict neurogenic pulmonary edema in patients with subarachnoid hemorrhage. Am J Emerg Med 2016;34:79-82.
- Huang YH, Liao CC, Yang KY. Demographics and short-term outcomes of spontaneous subarachnoid hemorrhage in young adults. World Neurosurg 2017;102:414-419.
- Kruyt ND, Biessels GJ, DeVries JH, et al. Hyperglycemia in aneurysmal subarachnoid hemorrhage: A potentially modifiable risk factor for poor outcome. J Cereb Blood Flow Metab 2010;30:1577-1587.
- Okazaki T, Kuroda Y. Aneurysmal subarachnoid hemorrhage: Intensive care for improving neurological outcome. J Intensive Care 2018;6:28.
- Byyny RL, Mower WR, Shum N, et al. Sensitivity of noncontrast cranial computed tomography for the emergency department diagnosis of subarachnoid hemorrhage. Ann Emerg Med 2008;51:697-703.
- Dubosh NM, Bellolio MF, Rabinstein AA, Edlow JA. Sensitivity of early brain computed tomography to exclude aneurysmal subarachnoid hemorrhage: A systematic review and meta-analysis. Stroke 2016;47:750-755.
- Backes D, Rinkel GJ, Kemperman H, et al. Time-dependent test characteristics of head computed tomography in patients suspected of nontraumatic subarachnoid hemorrhage. Stroke 2012;43:2115-2119.
- Beckse T. Subarachnoid hemorrhage workup. Medscape, Oct. 13, 2017. Available at: https://emedicine.medscape.com/article/1164341-workup. Accessed Sept. 1, 2018.
- Uff CE. LP and the diagnosis of SAH: Response to Perry J, et al. High risk clinical characteristics for subarachnoid haemorrhage in patients with acute headache: Prospective cohort study. BMJ 2010;341:c5204. Available at: https://www.bmj.com/rapid-response/2011/11/03/lp-and-disgnosis-sah. Accessed Sept. 5, 2018.
- Shah KH, Richard KM, Nicholas S, Edlow JA. Incidence of traumatic lumbar puncture. Acad Emerg Med 2003;10:151-154.
- Sayer D, Bloom B, Fernando K, et al. An observational study of 2,248 patients presenting with headache, suggestive of subarachnoid hemorrhage, who received lumbar punctures following normal computed tomography of the head. Acad Emerg Med 2015;22:1267-1273.
- Edlow JA. Diagnosis of subarachnoid hemorrhage. Stroke 2007;38:1129-1131.
- Edlow JA. Managing patients with nontraumatic, severe, rapid-onset headache. Ann Emerg Med 2018;71:400-408.
- Nickson C. Intubation of the neurocritical care patient. Life in the Fastlane. March 29, 2017. Available at: https://lifeinthefastlane.com/ccc/intubation-of-the-neurocritical-care-patient/. Accessed Sept. 1, 2018.
- Mooji JJ. Editorial: Grading and decision-making in (aneurysmal) subarachnoid haemorrhage. Interv Neuroradiol 2001;7:283-289.
- Connolly ES Jr, Rabinstein AA, Carhuapoma JR, et al. Guidelines for the management of aneurysmal subarachnoid hemorrhage: A guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2012;43:1711-1737.
- Chalouhi N, Daou B, Okabe T, et al. Beta-blocker therapy and impact on outcome after aneurysmal subarachnoid hemorrhage: A cohort study. J Neurosurg 2016;125:730-736.
- Hillman J, Fridriksson S, Nilsson O, et al. Immediate administration of tranexamic acid and reduced incidence of early rebleeding after aneurysmal subarachnoid hemorrhage: A prospective randomized study. J Neurosurg 2002;97:771-778.
- Marigold R, Gunther A, Tiwari D, Kwan J. Antiepileptic drugs for the primary and secondary prevention of seizures after subarachnoid haemorrhage. Cochrane Database Syst Rev 2013;6:CD008710.
- Chan S, Hemphill JC 3rd. Critical care management of intracerebral hemorrhage. Crit Care Clin 2014;30:699-717.
- Gupta RK, Jamjoom AA, Nikkar-Esfahani A, Jamjoom DZ. Spontaneous intracerebral hemorrhage: A clinical review. Br J Hosp Med 2010;71:499-504.
- Zahuranec DB, Lisabeth LD, Sanchez BN, et al. Intracerebral hemorrhage mortality is not changing despite declining incidence. Neurology 2014;82:2180-2186.
- Guo R, Ma L, Shrestha BK, et al. A retrospective clinical study of 98 adult idiopathic primary intraventricular hemorrhage cases. Medicine 2016;95:e5089.
- Cervera A, Amaro S, Chamorrow A. Oral anticoagulant-associated intracerebral hemorrhage. J Neurol 2012;259:212-224.
- De Herdt V, Dumont F, Henon H, et al. Early seizures in intracerebral hemorrhage: Incidence associated factors, and outcome. Neurology 2011;77:1794-1800.
- Khosravani H, Mayer SA, Demchuk A, et al. Emergency noninvasive angiography for acute intracerebral hemorrhage. Am J Neuroradiol 2013;34:1481-1487.
- Dastur CK, Yu W. Current management of spontaneous intracerebral haemorrhage. Stroke Vasc Neurol 2017;2:21-29.
- Elmer J, Hou P, Wilcox SR, et al. Acute respiratory distress syndrome after spontaneous intracerebral hemorrhage. Crit Care Med 2013;41:1992-2001.
- Levis JT. ECG diagnosis: Deep T wave inversions associated with intracranial hemorrhage. Perm J 2017; doi: 10.7812/TPP/16-049.
- Fan JS, Huang HH, Chen YC, et al. Emergency department neurologic deterioration in patients with spontaneous intracerebral hemorrhage: Incidence, predictors, and prognostic significance. Acad Emerg Med 2012;19:133-138.
- Rajwani KM, Nor AM. Towards evidence based emergency medicine: Best BETs from the Manchester Royal Infirmary. BET 1: Targeted blood pressure management in the hyperacute and acute stages following spontaneous intracerebral hemorrhage. Emerg Med J 2016;33:159-162.
- Qureshi AI, Palesch YY, Martin R, et al. Effect of systolic blood pressure reduction on hematoma expansion, perihematomal edema, and 3-month outcome among patients with intracerebral hemorrhage: Results from the antihypertensive treatment of acute cerebral hemorrhage study. Arch Neurol 2010;67:570-576.
- Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure lowering in patients with acute intracerebral hemorrhage. N Engl J Med 2013;368:2355-2365.
- Butcher K, Selim M. Acute blood pressure management in intracerebral hemorrhage: Equipoise resists an attack. Stroke 2016;47:3065-3066.
- Hemphill JC 3rd, Greenberg SM, Anderson CS, et al. Guidelines for the management of spontaneous intracerebral hemorrhage: A guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2015;46:2032-2060.
- Liebeskind DS. Hemorrhagic stroke. Medscape, Jan. 22, 2017. Available at: https://emedicine.medscape.com/article/1916662. Accessed Sept. 1, 2018.
- Steiner T, Poli S, Griebe M, et al. Fresh frozen plasma versus prothrombin complex concentrate in patients with intracranial haemorrhage related to vitamin K antagonists (INCH): A randomised trial. Lancet Neurol 2016;15:566-573.
- Pollack CV Jr, Reilla PA, van Ryn J, et al. Idarucizumab for dabigatran reversal — full cohort analysis. N Engl J Med 2017;377:431-441.
- Connolly SJ, Milling TJ Jr, Eikelboom JW, et al. Andexanet alfa for acute major bleeding associated with factor Xa inhibitors. N Engl J Med 2016;375:1131-1141.
- Frontera JA, Lewin JJ 3rd, Rabinstein AA, et al. Guideline for reversal of antithrombotics in intracranial hemorrhage: Executive summary. A statement for healthcare professionals from the Neurocritical Care Society and the Society of Critical Care Medicine. Crit Care Med 2016;44:2251.
- Martin M, Conlon LW. Does platelet transfusion improve outcomes in patients with spontaneous or traumatic intracerebral hemorrhage? Ann Emerg Med 2013;61:58-61.
- Fan JS, Chen YC, Huang HH, et al. Interhospital transfer neurological deterioration in patients with spontaneous intracerebral hemorrhage: Incidence and risk factors. Postgrad Med J 2017;93:349-353.
- Ferrete-Araujo AM, Egea-Guerrero JJ, Vilches-Arenas A, et al. Predictors of mortality and poor functional outcome in severe spontaneous intracerebral hemorrhage: A prospective observational study. Med Intensiva 2015;39:422-432.
- Kuramatsu JB, Bobinger T, Volbers B, et al. Hyponatremia is an independent predictor of in-hospital mortality in spontaneous intracerebral hemorrhage. Stroke 2014;45:1285-1291.
- Saxena A, Anderson CS, Wang X, et al. Prognostic significance of hyperglycemia in acute intracerebral hemorrhage: The INTERACT2 Study. Stroke 2016;47:682-688.
- Stevens RD, Shoykhet M, Cadena R. Emergency neurological life support: Intracranial hypertension and herniation. Neurocrit Care 2015;23(Suppl 2):S76-S82.
- Honig A, Michael S, Eliahou R, Leker RR. Central fever in patients with spontaneous intracerebral hemorrhage: Predicting factors and impact on outcome. BMC Neurol 2015;15:6.
Time is of the essence in management of intracranial hemorrhage and subarachnoid hemorrhage. The longer it takes to make the diagnosis and initiate treatment, whether it is surgical intervention or simply aggressive primary stabilization, the greater the risk to the patient regarding both morbidity and mortality.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
