Biventricular Hypertrophy in an Asymptomatic Patient?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
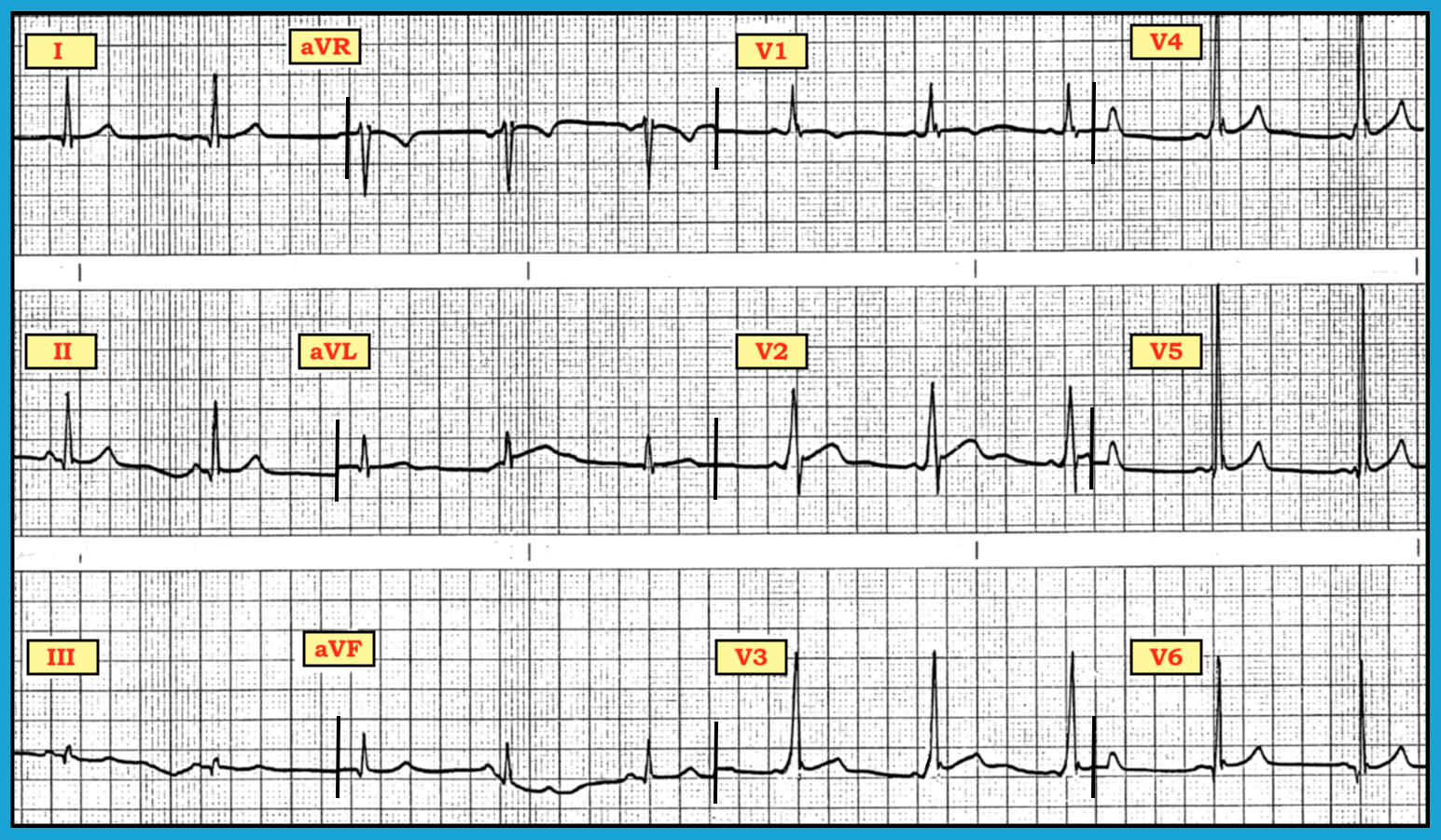
As part of a pre-employment physical, the ECG in the figure below was obtained from an asymptomatic, otherwise healthy 39-year-old male. How might one interpret this ECG? Is there right ventricular hypertrophy (RVH)? What about left ventricular hypertrophy (LVH)?
The rhythm is sinus at ~60-65/minute. But the PR interval appears short (i.e., < 0.12 seconds). When studying QRS complex in all 12 leads, one sees there is a slight QRS widening (especially in leads V2 and V3). There could be some slurring of the initial part of the QRS complex in a few precordial leads. Thus, this patient has Wolff-Parkinson-White (WPW) syndrome.
Usually, WPW is easily recognized on ECG when conduction completely uses the accessory pathway (AP). One should look for delta waves, a short PR interval, and QRS widening — even when conduction is over entirely of the AP (delta waves will not always be visible in every lead). Further, delta waves may appear and disappear, since conduction over the AP may be intermittent. Sometimes, conduction may happen at the same time over the AP and the normal. If this occurs, the WPW ECG characteristics may appear subtle because the contribution from conduction over the normal AV nodal pathway may predominate (and mask) ECG features of pre-excitation. Because of less-than-complete pre-excitation, it would be easy to overlook WPW in this case. Other than a slightly shortened PR interval, not much appears abnormal in the limb leads. One observes definite delta waves in leads V1, V2, V3, and V4 only. WPW may mimic other ECG conditions. Thus, the slightly widened and upright QRS complex in V1 mimics right bundle branch block and RVH. The markedly increased QRS amplitude observed in V5 imitates LVH. Still, one cannot diagnose these conditions on ECG because the patient has WPW. When viewing this ECG, we cannot determine if ventricular enlargement or bundle branch block also exist.
For more information about and further discussion on this case, please visit: https://bit.ly/2MKPl8U.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
