Management of Burn Injuries
January 1, 2019
Reprints
AUTHORS
Chad L. Mayer, MD, PhD, Resident Physician, Department of Emergency Medicine, The Ohio State University, Columbus
Howard A. Werman, MD, FACEP, Professor of Clinical Emergency Medicine, The Ohio State University College of Medicine, Columbus
PEER REVIEWER
Brian L. Springer, MD, FACEP, Department of Emergency Medicine, Wright State University, Kettering, OH
EXECUTIVE SUMMARY
- Three major risk factors have been shown to be predictive of burn mortality: age older than 60 years, burn size greater than 40%, and inhalation injury.
- Carbon monoxide and cyanide poisoning must be considered in burn patients who present with altered mental status, seizures, or cardiac arrest.
- Thermal burns can be classified as superficial, partial-thickness (formerly second-degree), or full-thickness (deep; formerly third-degree) burns.
- Any evidence of edema or blistering in the airway on fiberoptic view is a hard sign of inhalation injury and should warrant immediate intubation.
- An indirect measure of cyanide toxicity may be a severely elevated lactate in an enclosed-fire victim.
Burn injuries are complex injuries that the acute care physician must be prepared to assess and manage. In addition, an understanding of potential systemic effects from inhalation of toxic components in fires is critical to guide management. The authors provide a timely review of the critical aspects of assessment and management of burn patients.
— Ann M. Dietrich, MD, Editor
Introduction
Burn injuries are complex, secondary to tissue destruction and the inability of providers to reverse the pathology quickly, as can be accomplished with setting a bone or suturing a wound. Additionally, because of the varied mechanisms that produce burn injuries, providers must understand how to manage the many possible complications that can occur. Proper early management is essential in a severely burned patient because appropriate care can prevent downstream complications and reduce morbidity and mortality. Ultimately, patients with severe burns require complex, specialized management in a burn center.
Epidemiology
Burn injuries continue to be one of the leading causes of unintentional death and injury in the United States. Data from both the American Burn Association (ABA) and the National Fire Protection Association help lend scope to the problem: Between 2011 and 2015, approximately 486,000 fire or burn injuries were seen in emergency departments (EDs).1,2 In 2016, there were 3,390 civilian deaths from burns. More than 90% of patients who experience a burn injury are discharged from the ED. Burn injuries occur more commonly in males, and approximately one in four burns occurs in children. The mortality rate for burns has declined over the past several decades but has remained steady at about 4% in recent years. The majority of burn injuries originate from either home (73%) or work (8%),1 with other exposures, such as highway fires or environmental fires, making up the remainder.
A recent study identified three major risk factors predictive of burn mortality: age older than 60 years, burn size greater than 40%, and inhalation injury. The authors noted that as the number of factors increased from zero to three factors present, mortality increased 0.3%, 3%, 33%, and 90%, respectively.3 Inhalation injury is thought to elevate the mortality risk for any burn by an additional 50%.
Causes of Burn Injury
The vast majority of burns that healthcare providers encounter are thermal burns, either from a heated medium, such as burning materials, scalding water, super heated air, or direct contact with a hot object, or from a cold medium such as snow. Chemical burns occur from exposure to very acidic or alkaline sources, each of which has different management strategies, especially if the chemical is ingested. Finally, electrical burns from live wires, outlets, or other electrical sources are a third mechanism that providers may encounter.
According to the ABA, data from the National Burn Repository 2017 update showed that the most common causes for burn admissions were fire/flame (43%), scald (34%), contact (9%), electrical (4%), chemical (3%), and other (7%).4 Other causes include radiation injuries, which will not be discussed.
Burns as Presenting Complaints
Most patients with severe burns will present in the first few hours after injury, whereas those with smaller burns may present later. Chemical burns often occur in the workplace and disproportionately affect young males.5 Electrical burns are even less common, with only about 3-6% of all burn victims admitted to burn units experiencing an electric exposure.6 Carbon monoxide (CO) and cyanide (CN) poisoning must be considered in thermal burn patients who present with altered mental status, seizures, or cardiac arrest. In industrialized countries, domestic fires are the most common cause of CN poisoning and the second leading cause of CO toxicity. It has been shown that 50% of survivors of closed-space fires and 60% of fatalities have detectable CN levels.7
Pathophysiology
Thermal burn injuries occur primarily through conduction (direct transfer of heat or cold) or convection (heat carried to or away by a medium, such as air or water). These mechanisms prevail whether the patient suffers hyperthermic or hypothermic burns. Thermal burns cause tissue denaturation and charring in the most extensively injured portion of the wound. At the margins of a burn, the full spectrum of thermal injury, ranging from simple hyperemia, to increased vascular permeability with blister formation, to charred and insensate skin, may be seen. In the case of hypothermic injury, it is thought that although freezing injury is undesirable, the thawing event causes more damage through vasoconstriction, thrombosis, ischemia, and tissue necrosis.8
Initially, burns promote a systemic inflammatory response syndrome characterized by high levels of pro-inflammatory markers and cytokines, increasing permeability of vasculature, promoting inflammation, and in all respects mimicking sepsis, while placing the patient at much higher risk for this very condition. Increased vascular permeability can be seen in uninjured tissues as well as in the burn injury area. In the same way that sepsis can lead to multi-organ failure, burns are known to affect every major organ system. Loss of fluid into the burn and generalized edema can lead to burn shock if not managed properly. Unlike with traumatic injuries, the initial fluid losses do not contain significant red blood cells, thus producing a state of hemoconcentration. One additional effect that can exacerbate burn shock is depressed cardiac output, which is one of the earliest changes in severely burned patients. Careful supportive care in a comprehensive burn center is required for monitoring and responding to the many needs of the severely burned patient. Even recovery can be difficult, as the major burn injury sets up patients for complications, such as sepsis, renal failure, malnutrition, and graft failure. After the first 24-48 hours, burn patients typically develop a hyper-dynamic phase with increased cardiac output and metabolic rates far above normal, along with protein catabolism; thus, their nutritional needs and hemodynamic state can change dramatically.9
Inhalation injury in burns results from convection of super heated gases or chemical insult to the upper airway, lower airway, lung parenchyma, or through systemic effects. Super heated gases tend to affect the upper airways, whereas toxic chemicals released by combustion affect the lower airway and lungs. Damage to tissues causes a rapid release of cytokines and other inflammatory markers, and there is marked vasodilation, increased blood flow, and microvascular permeability, all of which lead to airway edema and secretions. Secretions in the airways may harden as time passes, causing significant casts to form and more drastically blocking small airways.10 Complications such as adult respiratory distress syndrome and hypoxemia due to ventilation/perfusion mismatch occur early in inhalation injuries.
Chemical burns, while occasionally causing an exothermic reaction and thus a thermal burn, propagate by chemical reaction. The type of chemical exposure often determines the severity of the burn. Acids generally cause a coagulative necrosis as a result of protein denaturation that quickly forms an eschar, limiting the penetration of the exposure. Thus, the severity of an acid burn is related to both the type of acid and the length of time it is in contact with the tissue. A notable exception is hydrofluoric acid, which produces both protons as well as fluoride that scavenges cations, sometimes leading to huge swings in cation concentrations and causing deep tissue burns. In some cases, systemic complications, such as arrhythmias, are seen as a result of the propensity of the free fluoride ion to scavenge magnesium and calcium cations. The Na+/K+ ATPase and Krebs cycle enzymes, which contribute to hypomagnesemia, hypocalcemia, and hypokalemia, also are affected.5 Unlike other acids that self-limit through eschar formation, hydrofluoric acid will continue to burn through mechanisms similar to alkali burns if left in contact with the skin. Prompt recognition and treatment are paramount to limiting sequelae.
Alternatively, alkali burns cause a liquefaction necrosis with saponification of fats that does less to contain the exposure than acid burns, and can cause ongoing burns if not addressed early. This is true for dermal exposure and ingestion.8 Alkali substances splashed in the eyes are more threatening to a patient’s vision than acids because of their hydrophilic and lipophilic properties. These properties allow ready penetration of alkali substances through the outer eye, causing damage to intraocular structures, while acid exposure causes quick precipitation of proteins, impeding progress and limiting damage.5 Chemical precipitates also can cause opacification of the cornea, and damage to underlying structures can cause intraocular pressures to rise.11
Electrical burns cause injury by the direct effect of current through the tissues, the conversion of electrical energy to thermal energy, and blunt trauma from intense muscle contraction or falls. These burns typically are divided into high voltage (> 1,000 V) and low voltage (< 1,000 V), although it is not clear that this classification is useful clinically. Low-voltage injuries are caused by alternating current (AC), whereas high-voltage injuries may be due to AC or direct current (DC). Generally, it is accepted that AC is the more dangerous exposure when compared to DC, in part because it can lead to tetany, causing the victim to maintain contact with the energy source. Tetany may not be seen with higher-voltage exposures, which can cause the victim to be thrown violently away from the contact. Although this may limit electrical exposure, the trauma from being thrown can lead to intracerebral hemorrhage, fractures, dislocations, and internal injuries.
The burn and associated thermal injury are proportional to the duration of contact and the resistance between entry and exit points of the current, as well as the cross-sectional area through which the current travels. As voltage is lost, heat is released, causing thermal injury. For this reason, current passing through an entry point in a limb, with a smaller cross-sectional area, or an arc injury, with a very large associated voltage drop, can produce worse thermal injuries than current passing through the larger area of the torso.12 Different tissues sustain injury based on their ability to conduct an electrical current. Skin, bone, and fat have higher resistance and, thus, a greater tendency to sustain injury. Nervous tissue and blood vessels are good conductors of electricity and are relatively spared, although they may be affected by localized thermal injury.
Environmental factors also can affect the injury. The resistance of skin, for example, may be lowered a thousand-fold when that skin becomes wet.6,12,13 Thus, a person exposed to an electric source in a bath may experience a fatal arrhythmia but may not sustain significant dermal burns, while a child who chews an electrical cord may have disfiguring oral commissure burns but no other systemic effects.12
A specific cause of mortality in electrical injury is fatal arrhythmia, with proposed mechanisms including electrical stimulation during ventricular repolarization leading to ventricular fibrillation, as well as direct induction of ventricular fibrillation.14 For patients with an electrical injury and absent pulses, such as at the scene of a lightning strike, early delivery of cardiopulmonary resuscitation and defibrillation of a shockable rhythm often results in good survival.13 An interesting and unique pattern seen in lightning strikes is Lichtenberg figures, a characteristic superficial pattern that may inform a provider of a lightning strike.13 (See Figure 1.)
Figure 1. Lichtenberg Figures |
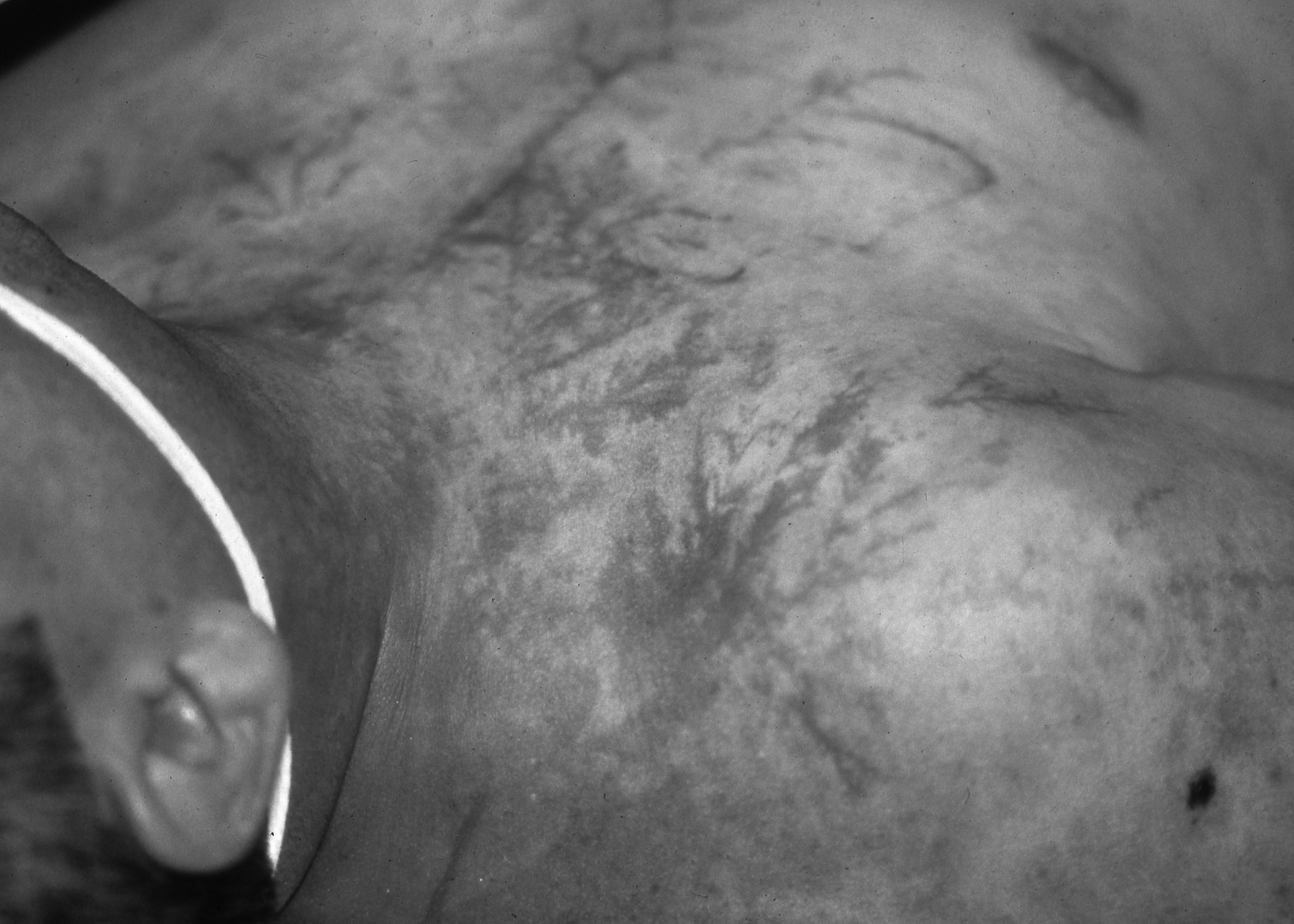 |
|
Source: Courtesy of David Effron, MD, Associate Professor, Case Western Reserve University, Attending Physician, Department of Emergency Medicine, MetroHealth Medical Center, Cleveland, OH |
Thermal injury may be accompanied by inhalation of toxic gases. CO is a clear, colorless gas that results from the incomplete combustion of materials found in many home and industrial fires. The CO molecule binds to the iron portion of the heme molecule with approximately 240 times greater affinity than oxygen. Fetal hemoglobin has an even greater affinity for the CO molecule. The binding of CO creates a conformational change in the hemoglobin that prevents the off-loading of oxygen in the peripheral tissues. CO also binds to other iron-containing enzymes, such as cytochromes, and prevents utilization of oxygen as well.15 Impaired cellular respiration leads to cellular stress, inflammation, apoptosis, and necrosis.16 The most significantly affected tissues are those of the central nervous system, because of the low energy stores, and the cardiovascular system in severe cases.
The combustion of materials such as upholstery, plastics, and synthetic rubber that contain both carbon and nitrogen leads to the release of CN. CN combines with iron found in cytochrome c oxidase, leading to inadequate utilization of oxygen by cells and resultant acidosis and hypoxia. This leads to a halt of cellular aerobic respiration and is rapidly fatal.17 CN is a compound with a short half-life in blood. Although people involved in closed-room fires always should be suspected of having CN exposure, CN levels in the ED may not reflect exposure accurately. The authors of one study found that plasma lactate values above 10 mmol/L correlated with CN intoxication of at least 40 µmol/L.18 CN is thought to be a significant contributor to morbidity and mortality in inhalation injury.19 As with CO poisoning, the central nervous system is most susceptible to these effects.
Clinical Features
The most common presentations encountered by healthcare providers are thermal burns. Thermal burns can be classified as superficial, partial-thickness (formerly second-degree), or full-thickness (deep; formerly third-degree) burns. For the purposes of triage and fluid management, only partial-thickness and full-thickness burns are counted toward total body surface area (TBSA). Several charts and rules are available for calculating TBSA. Classically, superficial burns are painful and erythematous. A mild sunburn is an appropriate example. Partial-thickness burns involve the dermis and may have blistering, which helps differentiate them from superficial burns. Unlike full-thickness burns, there is neurovascular preservation with partial-thickness burns and, as a result, bleeding and pain are complications. Burns can occur along a spectrum and, thus, deeper partial-thickness burns can be difficult to distinguish from full-thickness burns. Full-thickness burns classically are insensate, devoid of color, or “leathery.”20 Clinical examination is 70% accurate in determining the wound depth, and new technologies such as laser Doppler scanning may be more accurate in this determination.21,22 This technology has been shown to reduce hospital length of stay, improve the decision for grafting procedures, and generate lower costs,23 but it is not widely available.
If the burns are sustained in a closed space, a high suspicion for inhalation injury must be considered. High-risk features for inhalation injury include facial burns, perioral burns, or a burn to a large body surface area (BSA), as well as carboxyhemoglobin level. Although classically taught as a sign indicating the need for intubation, singed nasal hair was not shown to be an accurate predictor of the need for intubation in one retrospective study.24 The authors found significant predictive value in patients with facial/neck burns, carboxyhemoglobin concentration above 4%, or bronchial wall thickness greater than 3.5 mm on computed tomography (CT).
In another retrospective study conducted between 1998 and 2003, researchers found a lack of utility in the finding of singed nasal hair.24 Additionally, these authors confirmed the usefulness of fiberoptic examination, but the study was not powered to comment on symptoms such as stridor or hoarseness. Fiberoptic inspection, when available, should be considered to evaluate the vocal cords in patients not requiring immediate intubation because it can provide a much better assessment of the need for intubation and can help avoid unnecessary intubations.25 In another review of 879 patients intubated prior to arrival at a burn center, investigators found that about 40% could be extubated within the first two days of injury without a need for reintubation, suggesting that a significant portion of patients with burns may not require the procedure.26 However, the authors noted that in 27.9% of these patients, the reason given for intubation was “prophylaxis.” As such, it is not clear what hard signs of inhalational injury were present at the time of the procedure.
Any evidence of edema or blistering in the airway on fiberoptic view is a hard sign of inhalation injury and should warrant immediate intubation. Other findings, such as hoarseness, stridor, or drooling, although concerning, have not been shown consistently to be independent indicators of the need for immediate intubation. The authors of one paper pointed toward carboxyhemoglobin levels and significant
(> ~25%) TBSA burns as predictors of the need for intubation.27 If there is a suspicion for inhalation injury, concomitant CO or CN poisoning also should be considered and treated appropriately to help affect oxygenation as well.
In contrast to thermal and electrical burns, cold injuries follow a spectrum from “frostnip” and chilblains to full-blown frostbite and frozen limbs. As described later in this article, there is a fundamentally different approach to the treatment of frostbite. Although the features of frostbite may include a cold, hard limb with obvious signs of poor or no perfusion, real assessment cannot be undertaken until the affected body part has been rewarmed completely. Because frostbite often is a complication of environmental exposure, the first priority typically is to address the concomitant systemic hypothermia. Similar to thermal-induced injuries, there are “degrees” of cold-related injury with a worsening prognosis as the injury penetrates deeper into tissues. However, it is unclear whether these patients require the large volume resuscitation or early debridement that thermal burn victims require.28,29
A minority of burn center admissions involve chemical burns, which are discussed less in the literature.5 Chemical burns often are encountered as an ingestion, especially in pediatric patients,30 and the majority of the burn may not be visualized fully by the initial providers. The main clinical signs in cases of ingestion may be nausea and vomiting with abdominal pain. In the case of ocular burns, the signs are scleral injection and tearing. In surface burns, skin changes such as sloughing or discoloration occur.
Electrical burns, although rare as a presentation to burn centers, are devastating injuries. These burns often cause significant internal injury that is belied by the amount of external burns. Electrical injuries occur more frequently in adults as the result of an occupational exposure, and may produce fracture/
dislocations of bones, acute visceral injury, and cardiac arrest. A thorough history, including as much information as possible regarding the type of electrical exposure, is critical. As discussed earlier, electrical burns can differ greatly by type of current exposure, level of voltage, and resistance of tissues. Because severe occult damage can occur, standard TBSA calculations for resuscitation may not correlate with the extent of total damage and may underestimate fluid needs.12,13
In toddlers, a distinct form of an electrical burn is the oral commissure burn. (See Figure 2.) This injury occurs when a person, usually a toddler, bites an electrical cord or mouths the female end of a live cord. Most of these cases occur in children younger than 5 years of age, with half occurring in children younger than 3 years of age.31 Management of these particular burns will be discussed later, but recognizing this characteristic pattern of an oral burn with a history of wire exposure will greatly affect guardian education. A feared but uncommon complication of this rare burn is a severe bleed, which occurs once the eschar detaches.32,33 Parents whose children sustain such injuries should be counseled to return to the ED immediately for bleeding from the burn site.
Complications such as CO poisoning and CN poisoning have a wide variety of clinical presentations. Additionally, there is significant overlap between the symptoms produced by both toxins. Mild symptoms can include headache, nausea, vomiting, dizziness, palpitations, and malaise. Severe symptoms can range from cognitive dysfunction, confusion, flushing (“cherry red”) skin, seizures, coma, syncope, and cardiac arrest. Signs and symptoms of myocardial injury also have been reported in patients exposed to CO.34
Figure 2. Oral Commissure Burn |
 |
|
Source: Courtesy of Ann Dietrich, MD |
Laboratory/Radiology
For the most part, radiology is an adjunct in burn management, except in the case of electrical burns, in which convulsions can cause significant fractures and dislocations as well as intracranial injury that otherwise is not easily evaluated. CT also has been shown to be helpful in the case of inhalation injury for measuring bronchial wall thickness.27 Laboratory studies are an important part of burn management and should include a complete blood count, clotting studies, serum chemistries, and urinalysis. An electrocardiogram should be obtained in patients to detect arrhythmias from electrolyte disturbances. The most common findings identified in burns include signs of electrolyte abnormalities and renal dysfunction. Renal impairment simply may be the result of dehydration and significant volume losses, but massive burns and electrical injuries can produce rhabdomyolysis and myoglobinuria, leading to renal injury. The latter may be suspected when assessing a urinalysis that demonstrates the presence of blood on a dipstick but no red blood cells on microscopic urinalysis. With respect to electrical burns, the TBSA of any associated external burns, the peak level of creatine kinase, and the need for dialysis all were associated significantly with mortality.35
In patients with suspected inhalation injury, the initial chest radiograph often does not demonstrate the classic findings of atelectasis, inflammation, or infection. If CO or CN toxicity is suspected based on the history of an enclosed space fire, serum carboxyhemoglobin or CN levels should be ordered. Serum levels of carboxyhemoglobin do not correlate well with symptoms, especially if therapies, such as high-flow oxygen or hydroxocobalamin, have been administered. Remember that pulse oximetry cannot be used to distinguish oxyhemoglobin and carboxyhemoglobin, as both absorb the wavelength light emitted by the device. Noninvasive pulse co-oximeters are available as a screening tool for CO exposure, but the accuracy of such devices has been questioned.36 The diagnosis of CN poisoning often is made clinically, based on altered level of consciousness, elevated lactate levels, and profound acidosis. Serum CN levels are limited by long laboratory turnaround times and a short half-life of CN in the serum. Because of poor utilization of oxygen by tissues, venous blood may appear bright red. As stated before, an indirect measure of CN toxicity may be a severely elevated lactate in an enclosed-fire victim.18
Assessment and Management
Initial Assessment of the Burn
As with all ED evaluations, the evaluation of burns begins with the priorities established in Advanced Trauma Life Support of airway, breathing, circulation, disability, and exposure/environment. (See Figure 3.) Some would expand this to ABCDEF, in which “F” stands for fluid therapy. Late or inadequate fluid resuscitation has been shown to contribute to increased morbidity and mortality in burn patients. Burns have concomitant traumatic injuries in 5-7% of cases.37 Thus, an initial trauma survey for injuries should be conducted in the usual manner, particularly in patients with electrical injuries.38
Figure 3. Initial Management of Burns |
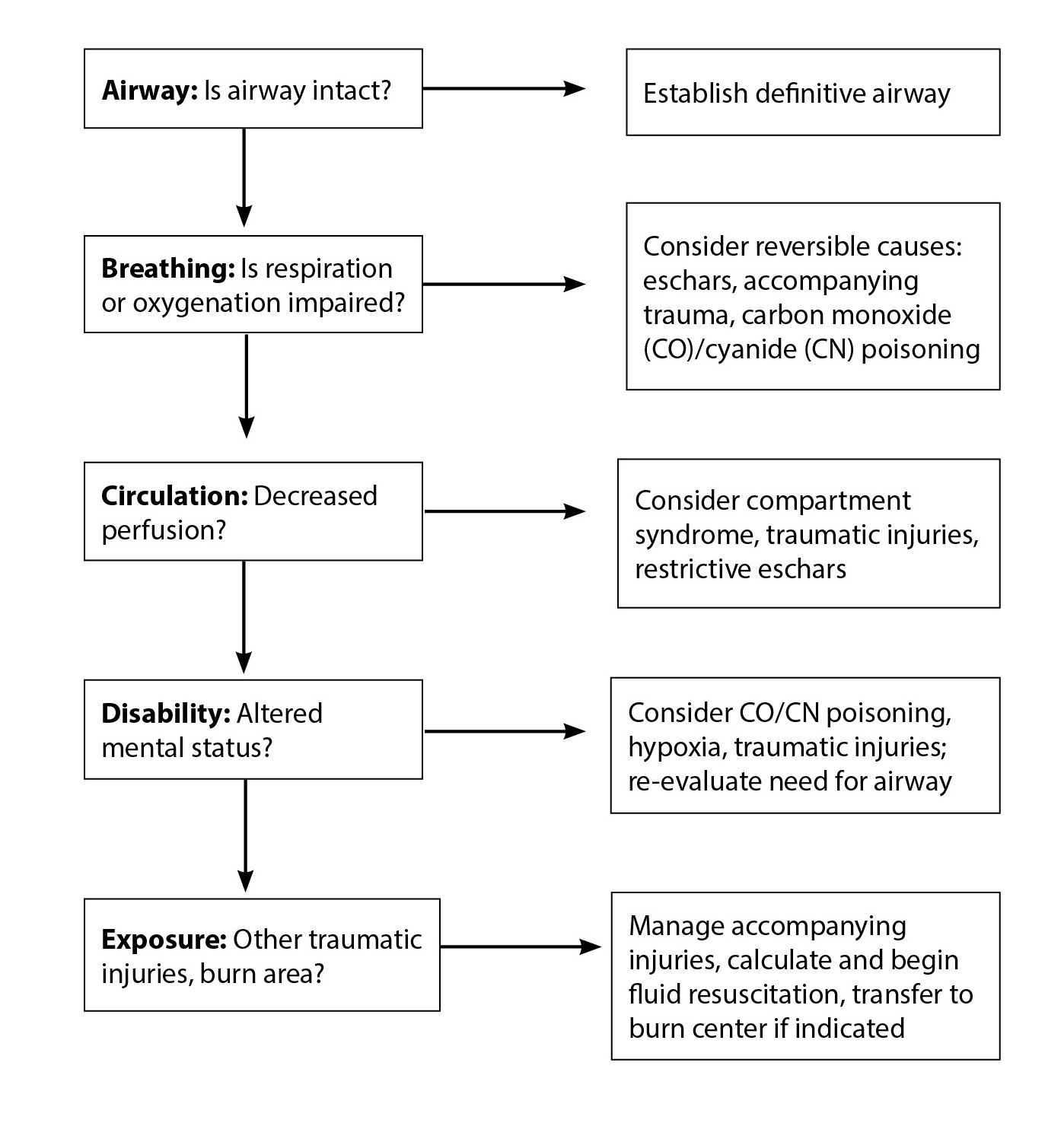 |
The most worrisome injury with a burn may not necessarily be the burn itself, which will lead to large fluid losses, a high risk of infection, and multiple surgeries, but the airway edema and respiratory compromise that may worsen dynamically during a patient’s evaluation. Because of this risk, the airway should be secured in those patients who are comatose, who have inadequate oxygenation, or who have burns involving the face or neck or significant TBSA (found in one paper to be a little more than 25% TBSA).27 Although classic teaching has discussed stridor and hoarseness as indications for immediate intubation, these conditions have not been found to be direct indicators of the need for intubation. However, they certainly may be signs of impending airway compromise and may indicate the need for close monitoring, since studies in the literature do not always have enough cases to reach statistical significance.24,27 Burns that involve the oropharynx and appear to put the airway at risk should be assessed carefully,39 as any change in respiratory status may be a sign of impending airway failure. Healthcare personnel should consider being aggressive in establishing a definitive airway, especially if they are planning to transfer a patient to a comprehensive burn center, although often a large portion of patients can be extubated quickly post-transfer.26 In at least one study, time to intubation has been associated with a more difficult intubation.40
It is important to remember that burns to the face may add another level of complexity to the airway assessment that should be performed before every intubation procedure. The clinician should anticipate a restricted mouth opening and distortion of the upper airway. Fiberoptic intubation or awake ketamine-assisted intubation should be considered if available. The laryngeal mask airway also has been used with success in burn patients. Remember that severe burns can change the pharmacologic properties of medications as well as the volume of distribution.
The use of paralytic agents involves several considerations. The most important factor is the altered airway anatomy, which might limit the use of these agents as an adjunct to intubation because edema or other structural damage may lead to an unsuccessful attempt at endotracheal intubation. In such cases, maintaining airway protective reflexes and avoiding paralysis may be prudent. Succinylcholine may produce an exaggerated hyperkalemic response, particularly after 48 hours in a severe burn patient. Alternatively, patients with severe burns may be resistant to non-depolarizing agents such as rocuronium, thus requiring higher doses (1.5 mg/kg) for rapid sequence induction. Burn patients may be resistant to the effects of sedatives (e.g., propofol) and opioid analgesic agents, mandating that higher dose requirements are needed. Ketamine frequently is used in EDs and by emergency medical services (EMS) and has several possible benefits in burn patients, including potential anti-inflammatory properties, which may make it a more desirable agent in these cases.41
Inhalation injury can be occult, occurring in the absence of significant burn injuries, and has been shown to correlate with extensive burns and facial burns, but not necessarily stridor or singed nasal hairs.24,27 If available, fiberoptic views of the airway at the bedside may be required to elicit its presence, but findings have not been shown to correlate consistently with significant clinical outcomes.27,42,43 As stated earlier, though, fiberoscopy may help avoid unnecessary intubations.
Treatment of inhalation injury primarily is supportive, with intubation, sedation/paralysis, and positive-pressure ventilation. Nebulization of anticoagulants, antioxidants, and anti-inflammatory agents currently is under investigation as adjunctive treatment.44,45 In patients with CO or CN poisoning, treatments such as intubation, high-flow oxygen therapy, hydroxocobalamin, and even hyperbaric oxygen therapy can be considered.20
Other important adjunctive measures in the initial assessment include cooling the wound, discarding all clothing, removing any circumferential jewelry, and updating tetanus as indicated. Decontamination of chemical burns, discussed in greater detail later, also is an initial priority. Finally, because the skin is the major organ of thermoregulation, patients should be kept warm and monitored for the development of hypothermia.
Management of the Burn Injury
Accurately estimating the size of a burn is crucial to the management of burn patients in the first 24-48 hours. Many providers may be familiar with the “rule of nines” or the use of the Lund and Browder chart. The Lund and Browder chart often is used to clarify TBSA in children because the “rule of nines” only applies to adults. The most common error in estimating the extent of the burn is to include superficial burns in the initial estimate of TBSA. A partial- or full-thickness burn covering as little as 15-20% TBSA can lead to hypovolemic shock from third spacing if adequate resuscitation is not undertaken rapidly.46 Remember that for smaller burn areas, the patient’s hand represents 1% of TBSA.
Once the extent of burn is determined, several formulas are available for estimating the initial fluid requirements in a severe burn.47 (See Table 1.) Volume resuscitation in burns usually is divided into blocks of time.48 For example, when using the Parkland formula or the modified Brooke formula, 50% of the calculated fluid requirement is given in the first eight hours, with the other half given over the remaining 16 hours of day 1. The first interval begins when the burn occurs, not when the patient presents for treatment. Chung proposed a simple rule (ISR Rule of Tens)49 that can be used to determine an initial fluid rate in milliliters per hour in an adult: % TBSA × 10. In the early phases of resuscitation, crystalloid solutions are appropriate for initial fluid replacement. Ideally, a balanced solution such as lactated Ringer’s is initiated for early resuscitation, as the use of 0.9% normal saline has been associated with hyperchloremic acidosis. Some burn centers use colloid solutions50 for larger burns, as with the West Penn51 or Brooke formula in the early phases of resuscitation. At least one small study showed a decreased rate of elevated intraabdominal compartment pressure and significantly lower volumes of resuscitation fluid when plasma was used for resuscitation.52
Early fluid resuscitation is among the most challenging aspects of burn care, especially for those patients with burns covering a large TBSA. In addition, inhalation injury can increase fluid requirements by as much as 50%, despite not being considered in most burn resuscitation formulas. These resuscitation formulas only provide guidance to determine adequate resuscitation, and clinical judgment may be needed to guide an individual burn patient’s resuscitation based on the entire clinical picture. The most important parameter used to monitor adequate resuscitation is urine output. With fluid resuscitation in burned adults, goal urine output (UOP) usually is about 30-50 mL/hour, with fluid resuscitation guided by either the Parkland or modified Brooke formulas. A resuscitative goal UOP should be greater than 0.5-1 mL/kg/hour in patients less than 30 kg and 1-2 mL/hour in infants.
Table 1. Resuscitative Formulas for Burns |
|
|
Parkland |
First 24 h: Lactated Ringer’s at 4 mL/kg/% TBSA burn, half in first 8 h, remaining over 16 h Second 24 h: Colloid at 20-60% calculated plasma volume targeting urine output |
|
Brooke |
First 24 h: Lactated Ringer’s at 1.5 mL/kg/% TBSA burn, colloid 0.5 mL/kg/% TBSA burn Second 24 h: switch to D5W 2,000 mL |
|
Modified Brooke |
First 24 h: Lactated Ringer’s at 2 mL/kg/% TBSA burn, half in first 8 h, remaining over 16 h Second 24 h: Colloid at 0.3-0.5 mL/kg/% TBSA burn + D5W targeting urine output |
|
Western Pennsylvania |
Fresh frozen plasma at 75 mL/kg/24 h for 48 h (target urine output 0.5 mL/kg/h) + lactated Ringer’s at 83 mL/h |
|
Cincinnati (older children) |
4 mL/kg/% TBSA burn + 1,500 mL/m2 % TBSA of lactated Ringer’s + 5% dextrose PRN, half first 8 h, remaining over 16 h |
|
Galveston |
5,000 mL/m2 % TBSA burn + 2,000 mL/m2 % TBSA of lactated Ringer’s + 12.5 g 25% albumin/L of crystalloid + 5% dextrose PRN, half first 8 h, remaining over 16 h |
|
Key: TBSA = total body surface area; D5W = dextrose 5% in water; PRN = as needed |
|
Although the most common error in burn management is under-resuscitation, there are real risks of over-resuscitation, including adult respiratory distress syndrome and abdominal compartment syndrome, which may necessitate surgical decompression in patients who receive more than 250 mL/kg in the first 24 hours. These complications often occur because providers generally overestimate burn size. A rare complication of over-resuscitation is ocular compartment syndrome, which is diagnosed by bedside tonometry and treated with lateral canthotomy. Another pitfall is to forget that these formulas apply to patients > 40 kg. Pediatric burn patients often are resuscitated with 3 mL/kg/TBSA burned and require additional dextrose maintenance fluids because of their smaller glycogen stores and increased risk of hypoglycemia.39 Several different formulas are available for pediatric resuscitation, with the Cincinnati and Galveston formulas cited as ones commonly used in burn centers that treat pediatric patients.53 One additional consideration is electrical injury, in which the goal UOP of 70-100 mL/h in adults or 2 mL/kg/h in pediatric patients must be achieved to avoid acute renal failure from myoglobinuria and rhabdomyolysis.
A potential complication of heat-induced thermal burns is the need for escharotomy. This procedure is used to relieve constricting pressure around a patient’s torso or limb, usually resulting from an encircling burn. (See Figure 4.) This constriction can lead to compartment syndrome from edema causing ischemia, hypoxia, myonecrosis, and possible loss of life or limb, if, for example, the eschar restricts chest wall expansion and respiration. The decision to proceed with escharotomy or even fasciotomy relies on a having high clinical suspicion for the condition and monitoring pulses and compartment pressures as well as respiratory status. Signs of compartment syndrome, such as absent pulses, often are late findings. Thus, prompt surgical consultation must be obtained when this syndrome is suspected, as a crucial window to preserve tissue already may be passing. Even when the procedure is performed, it may be done poorly and require further releasing of pressure at a burn center. Relief is accomplished by incising the eschar, allowing expansion of the underlying tissues.54
Figure 4. Circumferential Lower Extremity Burns Requiring Escharotomies |
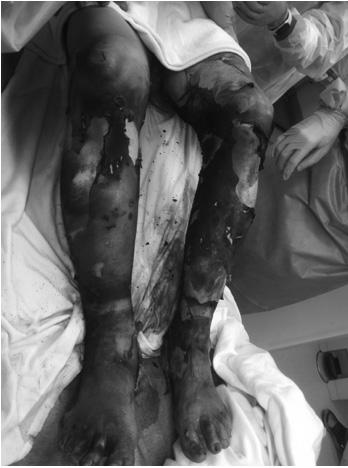 |
|
Source: Courtesy of Benjamin Ostro, MD |
Of note, in one study, pulses were present in 175 of 237 (74%) limbs requiring further decompression, and 20 limbs (8.4%) required decompression despite not having circumferential burns. In patients with inadequate or delayed decompression, complications ranged from foot drop to amputations.55 Therefore, maintaining a high clinical suspicion with a low threshold for checking compartment pressures or consulting a surgeon and carefully monitoring pulses are critical actions in any severely burned patient. It is generally accepted that a compartment pressure above 30 mmHg or a delta pressure (diastolic blood pressure – compartment pressure) less than 30 mmHg warrants surgical decompression. Any diminution or loss of pulse strength is a late finding.
With all burn wounds, the clinician must balance the risk of infection and the need to keep the wound moist for wound healing.21,56 There is extensive literature regarding the myriad choices in antibiotic and antiseptic dressings for burn wounds, with silver-based antiseptics among the most popular.57,58 Despite recent advancements in plastic surgery, silver-based antiseptics remain an important part of burn care. There are several reviews describing these agents in greater detail. In a Cochrane review, investigators found that honey and antimicrobials seemed to promote healing, but they failed to find high-quality evidence that any topical treatment has a positive effect on burn wound healing and other outcomes in burned patients.59 It is best to delay application of topical dressings beyond clean white sheets until the patient has reached a comprehensive burn center to allow the best evaluation and management of the wounds.
Special care is required with pediatric burns for several reasons. Children have larger BSA/mass ratio than adults, placing them at higher risk for hypothermia and increasing their fluid resuscitation requirements compared to adults.53,60 Additionally, pediatric burn patients also have thinner skin than adults, meaning that for any thermal exposure, children will have a deeper burn.60 Regarding the unique case of oral commissure burns, management mainly includes outpatient plastic surgery follow-up and guardian education, as there is a small but real risk of delayed arterial bleeding when the eschar detaches several days post-injury. There has been discussion in the literature about whether oral splinting is warranted and whether it helps reduce the need for surgery. Since this intervention usually occurs over a period of months post-injury, the decision about oral splinting is best decided in consultation with a local plastic surgeon within several days of injury.61-63
In evaluating cold-induced burns, the initial assessment is complicated by the fact that a cold or frozen limb cannot be evaluated adequately until thawed, at which point interventions can be considered. Once there is no risk of refreezing,28 limbs and other affected areas should be rewarmed in a moving liquid bath ideally between 40-42°C. Analgesia will be needed during this painful process. The risk to tissue increases with any refreezing; thus, it is ideal to thaw only once, and avoid rewarming in settings such as the battlefield or wilderness where re-exposure cannot be prevented. At this point, if the burn occurred within 24 hours and there are no contraindications, there is evidence of improved outcomes with early angiography or other advanced imaging and the use of iloprost/thrombolytics and heparin to help restore perfusion. Several treatment algorithms have been published.64-68 These interventions are best conducted at a tertiary care center in conjunction with a burn team. Advanced imaging may be helpful in guiding the level of amputation for those with contraindications to tissue plasminogen activator (tPA).66
When evaluating chemical burns, the priorities as outlined are unchanged. However, there are several special considerations when treating a chemical burn patient. Unlike the patient with an environmental exposure, the patient with a caustic burn may remain in contact with the offending agent in the ED through saturated clothes or the presence of the substance on the skin or the mucous membranes. Unless other immediate life threats, such as airway compromise, are identified, decontamination often is the first step in treating a chemical burn. This is performed by removing any contaminated garments or personal protective equipment (PPE) and ensuring the providers are wearing their own PPE. Flushing with copious amounts of water then is performed, unless the burn was caused by an elemental metal (which should be brushed off and irrigated with mineral oil) or phenol5 (which may benefit from irrigation with polyethylene glycol [PEG]), although evidence for this is weak. Any powder, such as lye, should be brushed off first, as water may react to form a strong alkali and expand the burn area.5
Special consideration also should be given to hydrofluoric (HF) acid exposures because this agent is associated with electrolyte abnormalities, such as hypocalcemia, hypomagnesemia, and often hypokalemia, which can lead to life-threatening arrhythmias. For a visible burn, treatment is with calcium gluconate, either injected subcutaneously or administered systemically, as topical calcium gluconate gel often does not penetrate deep enough to be effective. Even a very small HF acid burn can have significant complications.5 Intraocular burns are an important consideration with HF acid because it penetrates the corneal epithelium similarly to an alkali substance.69
When dealing with ocular chemical burns in the prehospital setting, irrigation with copious amounts of clean tap water, if close at hand, is better than delaying irrigation for a sterile irrigating solution. In the ED, topical anesthetics and prompt irrigation, preferably with a Morgan lens and sterile irrigation solution such as lactated Ringer’s, are mainstays of treatment. Irrigation should proceed for at least 20-30 minutes, with the goal of restoring a neutral pH in tears. Testing pH with litmus strips in areas such as the eye can help guide irrigation until pH has returned to a physiologic 7.4. Acidic burns progress through coagulative necrosis and may be somewhat self-limiting. Alkali burns progress through liquefaction necrosis, are not as self-limiting, and, therefore, are far more dangerous. One should not neutralize an alkali or acid with the opposite solution, as this causes an exothermic reaction. Prompt consultation with an ophthalmologist is appropriate because there are several therapies to consider. Cycloplegics often are used to prevent synechiae formation and provide analgesia. Topical antibiotics and steroids also are used. These therapies should be discussed with an ophthalmologist who should monitor for sequelae such as acute glaucoma.11,70
An important consideration in electrical burns is the possibility of rhabdomyolysis, which results from extensive muscle destruction beneath the exterior burns. Laboratory investigation may reveal elevated creatine kinase (CK) levels as well as a positive urinalysis for myoglobin. The major risk is kidney injury caused by obstruction of the renal tubules.
Finally, patients who do not achieve an adequate urine output, have repeated episodes of hypotension, or have an increasing base deficit should be reassessed for the adequacy of resuscitation. Reassess the ABCs and consider missed traumatic injuries. Recalculate the patient’s fluid requirements and compare them to those already administered. Consider a bedside ultrasound study to assess the inferior vena cava for fluid status and the heart for wall motion abnormalities.39
Treatment of coexisting CO poisoning involves placing the patient on a tight-fitting nonrebreather mask at 15 L per minute. Remember that the half-life of carboxyhemoglobin under room air conditions is four to six hours; breathing near 100% oxygen reduces the half-life to 90 minutes. If the patient is intubated, an inspired oxygen concentration of 100% should be used for the first several hours. Hyperbaric oxygen therapy (HBOT) is recommended to reduce mortality71 and long-term neurologic sequelae of CO poisoning, although this later point is controversial.72 HBOT is recommended for patients with a carboxyhemoglobin level > 25%, pregnant females with CO exposure, patients with altered level of consciousness or metabolic acidosis, and patients with electrocardiographic evidence of myocardial ischemia. One to two treatments at 2.5 to 3 ATA are recommended. Ideally, the treatment should be administered within the first six hours of CO exposure.73
Patients with inhalation injury who have suspected CN toxicity should be treated empirically because of the early onset of clinical symptoms and the current lack of an available rapid, specific diagnostic test. There is some evidence that empiric therapy for smoke-inhalation victims in cardiac arrest may improve outcomes.74 Some institutions still use the Cyanide Antidote Kit, but many have moved to using hydroxocobalamin, dosed at 70 mg/kg to a maximum of 5 grams, administered intravenously. In severe CN poisoning, a second dose may be given if there is no response after the first dose in 15 minutes. The drug binds to hydrogen cyanide to form cyanocobalamin or vitamin B12, which is excreted in the urine. Side effects include a reddish discoloration of the skin, headache, nausea, chest discomfort, and dysphagia. The drug interferes with accurate measurement of carboxyhemoglobin levels. It is also recommended that 25% sodium thiosulfate, dosed at 1.65 mL/kg, be administered empirically to a maximum dose of 12.5 grams. This drug is relatively safe and acts as a sulfur donor, resulting in the production of thiocyanate, which then is excreted in the urine.
Disposition
Most medical centers are not burn centers, and the decision to transfer a patient to a comprehensive burn center is an early decision point to guide care. The ABA provides specific guidance for referral to a burn center. Patients with large burns comprising > 10% BSA, inhalation injury, and associated trauma all should be referred to a burn center quickly. Additionally, burns to the face, hands, perineum, genitalia, or major joints, or full-thickness burns warrant referral. Other indications for transfer are pediatric burns; electrical, chemical, or lightning burns; patients with multiple comorbidities; or those who the provider believes may have special needs.20,39 Any suspicious burn should raise concern regarding child, intimate partner, or geriatric abuse. These patients should be transferred for evaluation to a facility where the appropriate social service providers are available. One additional consideration for transfer is the patient with a severe CO exposure, who should be considered for early HBOT.
The ABA has a verification process for burn centers. ABA Verified Burn Centers can provide comprehensive care for complicated burn patients who will have a long hospitalization, often with multiple surgeries and significant rehabilitation needs. The need for specialty consultants, such as for ophthalmology, renal replacement therapy, or evaluation of burn complications, including compartment syndrome, may necessitate transfer to a higher level of care if these services are not available at a provider’s center. Finally, telemedicine is gaining popularity for determining the need to transfer vs. outpatient evaluation in questionable cases.75
If patients with low-voltage electrical burns did not experience loss of consciousness or cardiac dysrhythmias and their ECG is otherwise reassuring, it may be appropriate to discharge the patients after a brief period of observation.6
Summary
Patients with significant burns require long-term care and a prolonged period of rehabilitation. Characterizing the extent of the burn and recognizing associated comorbidities and trauma is paramount in guiding initial management. Nonetheless, proper early management can reduce mortality and long-term morbidity. As with all other traumatic injuries, the initial focus is on assessing the airway, maintaining proper ventilation and oxygenation, and replenishing circulatory losses. Intubation should be performed early for those with evidence of upper airway compromise or the presence of factors that have been shown to predict the presence of inhalation injury, with fiberoptic inspection a helpful adjunct in determining the true presence of this condition. Proper fluid resuscitation is guided by the extent of the burn and is targeted to adequate urine output. However, over-resuscitation with fluids is as detrimental as under-resuscitation. Special considerations for chemical burns and electrical injuries must be considered, such as monitoring for compartment syndrome. Severe burns require transfer to a specialized burn center for long-term care.
REFERENCES
- American Burn Association. Burn Injury Fact Sheet. 2018. Available at: www.ameriburn.org. Accessed Nov. 28, 2018.
- Haynes HJG. Fire Loss in the United States During 2015. National Fire Protection Association; 2016:1-50.
- Ryan CM, Schoenfeld DA, Thorpe WP, et al. Objective estimates of the probability of death from burn injuries. N Engl J Med 1998;338:362-366.
- Mosier MJ, Bernal N, Faraklas I, et al. National Burn Repository 2017 Update: Report of Data from 2008-2017. 13 ed: American Burn Association; 2017.
- Friedstat J, Brown DA, Levi B. Chemical, electrical, and radiation injuries. Clin Plast Surg 2017;44:657-669.
- Waldmann V, Narayanan K, Combes N, Marijon E. Electrical injury. BMJ 2017;357:j1418.
- Grabowska T, Skowronek R, Nowicka J, Sybirska H. Prevalence of hydrogen cyanide and carboxyhaemoglobin in victims of smoke inhalation during enclosed-space fires: A combined toxicological risk. Clin Toxicol (Phila) 2012;50:759-763.
- Tintinalli JE, Stapczynski JS, Ma OJ, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th ed. New York: McGraw-Hill Education; 2016.
- Nielson CB, Duethman NC, Howard JM, et al. Burns: Pathophysiology of systemic complications and current management. J Burn Care Res 2017;38:e469-e481.
- Jones SW, Williams FN, Cairns BA, Cartotto R. Inhalation injury: Pathophysiology, diagnosis, and treatment. Clin Plast Surg 2017;44:505-511.
- Bunker DJ, George RJ, Kleinschmidt A, et al. Alkali-related ocular burns: A case series and review. J Burn Care Res 2014;35:261-268.
- Skoog T. Electrical injuries. J Trauma 1970;10:816-830.
- Spies C, Trohman RG. Narrative review: Electrocution and life-threatening electrical injuries. Ann Intern Med 2006;145:531-537.
- Kroll MW, Fish RM, Lakkireddy D, et al. Essentials of low-power electrocution: Established and speculated mechanisms. Conf Proc IEEE Eng Med Biol Soc 2012;2012:5734-5740.
- Ernst A, Zibrak JD. Carbon monoxide poisoning. N Engl J Med 1998;339:1603-1608.
- Weaver LK. Clinical practice. Carbon monoxide poisoning. N Engl J Med 2009;360:1217-1225.
- MacLennan L, Moiemen N. Management of cyanide toxicity in patients with burns. Burns 2015;41:18-24.
- Baud FJ, Barriot P, Toffis V, et al. Elevated blood cyanide concentrations in victims of smoke inhalation. N Engl J Med 1991;325:1761-1766.
- Antonio AC, Castro PS, Freire LO. Smoke inhalation injury during enclosed-space fires: An update. J Bras Pneumol 2013;39:373-381.
- Alharbi Z, Piatkowski A, Dembinski R, et al. Treatment of burns in the first 24 hours: Simple and practical guide by answering 10 questions in a step-by-step form. World J Emerg Surg 2012;7:13.
- Bezuhly M, Fish JS. Acute burn care. Plast Reconstr Surg 2012;130:349e-358e.
- Shin JY, Yi HS. Diagnostic accuracy of laser Doppler imaging in burn depth assessment: Systematic review and meta-analysis. Burns 2016;42:1369-1376.
- Hop MJ, Stekelenburg CM, Hiddingh J, et al. Cost-effectiveness of laser Doppler imaging in burn care in The Netherlands: A randomized controlled trial. Plast Reconstr Surg 2016;137:166e-176e.
- Madnani DD, Steele NP, de Vries E. Factors that predict the need for intubation in patients with smoke inhalation injury. Ear Nose Throat J 2006;85:278-280.
- Oscier C, Emerson B, Handy JM. New perspectives on airway management in acutely burned patients. Anaesthesia 2014;69:105-110.
- Eastman AL, Arnoldo BA, Hunt JL, Purdue GF. Pre-burn center management of the burned airway: Do we know enough? J Burn Care Res 2010;31:701-705.
- Onishi S, Osuka A, Kuroki Y, Ueyama M. Indications of early intubation for patients with inhalation injury. Acute Med Surg 2017;4:278-285.
- Handford C, Buxton P, Russell K, et al. Frostbite: A practical approach to hospital management. Extrem Physiol Med 2014;3:7.
- Handford C, Thomas O, Imray CHE. Frostbite. Emerg Med Clin North Am 2017;35:281-299.
- Alemayehu H, Tarkowski A, Dehmer JJ, et al. Management of electrical and chemical burns in children. J Surg Res 2014;190:210-213.
- Umstattd LA, Chang CW. Pediatric oral electrical burns: Incidence of emergency department visits in the United States, 1997-2012. Otolaryngol Head Neck Surg 2016;155:94-98.
- Thomson HG, Juckes AW, Farmer AW. Electric burns to the mouth in children. Plast Reconstr Surg 1965;35:466-477.
- Gifford GH Jr, Marty AT, MacCollum DW. The management of electrical mouth burns in children. Pediatrics 1971;47:113-119.
- Sward DG, Sethuraman KN, Wong JS, Rosenthal RE. Carbon monoxide and ST-elevation myocardial infarction: Case reports. Undersea Hyperb Med 2016;43:63-69.
- Saracoglu A, Kuzucuoglu T, Yakupoglu S, et al. Prognostic factors in electrical burns: A review of 101 patients. Burns 2014;40:702-707.
- Zaouter C, Zavorsky GS. The measurement of carboxyhemoglobin and methemoglobin using a non-invasive pulse CO-oximeter. Respir Physiol Neurobiol 2012;182:88-92.
- Rosenkranz KM, Sheridan R. Management of the burned trauma patient: Balancing conflicting priorities. Burns 2002;28:665-669.
- Hettiaratchy S, Papini R. Initial management of a major burn: I — overview. BMJ 2004;328:1555-1557.
- Cancio LC. Initial assessment and fluid resuscitation of burn patients. Surg Clin North Am 2014;94:741-754.
- Esnault P, Prunet B, Cotte J, et al. Tracheal intubation difficulties in the setting of face and neck burns: Myth or reality? Am J Emerg Med 2014;32:1174-1178.
- Bittner EA, Shank E, Woodson L, Martyn JA. Acute and perioperative care of the burn-injured patient. Anesthesiology 2015;122:448-464.
- Spano S, Hanna S, Li Z, et al. Does bronchoscopic evaluation of inhalation injury severity predict outcome? J Burn Care Res 2016;37:1-11.
- Liffner G, Bak Z, Reske A, Sjöberg F. Inhalation injury assessed by score does not contribute to the development of acute respiratory distress syndrome in burn victims. Burns 2005;31:263-268.
- Toon MH, Maybauer MO, Greenwood JE, et al. Management of acute smoke inhalation injury. Crit Care Resusc 2010;12:53-61.
- Miller AC, Elamin EM, Suffredini AF. Inhaled anticoagulation regimens for the treatment of smoke inhalation-associated acute lung injury: A systematic review. Crit Care Med 2014;42:413-419.
- Monafo WW. Initial management of burns. N Engl J Med 1996;335:1581-1586.
- Hettiaratchy S, Papini R. Initial management of a major burn: II — assessment and resuscitation. BMJ 2004;329:101-103.
- Alvarado R, Chung KK, Cancio LC, Wolf SE. Burn resuscitation. Burns 2009;35:4-14.
- Chung KK, Salinas J, Renz EM, et al. Simple derivation of the initial fluid rate for the resuscitation of severely burned adult combat casualties: In silico validation of the rule of 10. J Trauma 2010;69(Suppl 1):S49-S54.
- Cartotto R, Greenhalgh DG, Cancio C. Burn state of the science: Fluid resuscitation. J Burn Care Res 2017;38:e596-e604.
- Jones LM, Brown N, Phillips G, et al. Burn resuscitation with fresh frozen plasma: 5 years of experience with the West Penn Formula. Austin J Emergency & Crit Care Med 2015;2:1-4.
- O’Mara MS, Slater H, Goldfarb IW, Caushaj PF. A prospective, randomized evaluation of intra-abdominal pressures with crystalloid and colloid resuscitation in burn patients. J Trauma 2005;58:1011-1018.
- Romanowski KS, Palmieri TL. Pediatric burn resuscitation: Past, present, and future. Burns Trauma 2017;5:26.
- Davis TS, Graham WP 3rd. Escharotomies. J Trauma 1981;21:83-84.
- Brown RL, Greenhalgh DG, Kagan RJ, Warden GD. The adequacy of limb escharotomies-fasciotomies after referral to a major burn center. J Trauma 1994;37:916-920.
- Cambiaso-Daniel J, Boukovalas S, Bitz GH, et al. Topical antimicrobials in burn care: Part 1-Topical antiseptics. Ann Plast Surg 2018; doi: 10.1097/SAP.0000000000001297. [Epub ahead of print].
- Cartotto R. Topical antimicrobial agents for pediatric burns. Burns Trauma 2017;5:33.
- Greenhalgh DG. Topical antimicrobial agents for burn wounds. Clin Plast Surg 2009;36:597-606.
- Norman G, Christie J, Liu Z, et al. Antiseptics for burns. Cochrane Database Syst Rev 2017;7:CD011821.
- Palmieri TL. Pediatric burn resuscitation. Crit Care Clin 2016;32:547-559.
- Canady JW, Thompson SA, Bardach J. Oral commissure burns in children. Plast Reconstr Surg 1996;97:738-744; discussion 745; 746-755.
- Hoffman KA, Trigger CC. Pediatric oral commissure burn. Clin Pract Cases Emerg Med 2017;1:59-60.
- Vorhies JM. Electrical burns of the oral commissure. Angle Orthod 1987;57:2-17.
- Cauchy E, Davis CB, Pasquier M, et al. A new proposal for management of severe frostbite in the austere environment. Wilderness Environ Med 2016;27:92-99.
- Jones LM, Coffey RA, Natwa MP, Bailey JK. The use of intravenous tPA for the treatment of severe frostbite. Burns 2017;43:1088-1096.
- Kraft C, Millet JD, Agarwal S, et al. SPECT/CT in the evaluation of frostbite. J Burn Care Res 2017;38:e227-e234.
- Wagner C, Pannucci CJ. Thrombolytic therapy in the acute management of frostbite injuries. Air Med J 2011;30:39-44.
- Twomey JA, Peltier GL, Zera RT. An open-label study to evaluate the safety and efficacy of tissue plasminogen activator in treatment of severe frostbite. J Trauma 2005;59:1350-1354; discussion 1354-1355.
- Atley K, Ridyard E. Treatment of hydrofluoric acid exposure to the eye. Int J Ophthalmol 2015;8:157-161.
- Sharma N, Kaur M, Agarwal T, et al. Treatment of acute ocular chemical burns. Surv Ophthalmol 2018;63:214-235.
- Huang CC, Ho CH, Chen YC, et al. Hyperbaric oxygen therapy is associated with lower short- and long-term mortality in patients with carbon monoxide poisoning. Chest 2017;15:943-953.
- Buckley NA, Juurlink DN, Isbister G, et al. Hyperbaric oxygen for carbon monoxide poisoning. Cochrane Database Syst Rev 2011;(4):CD002041.
- Weaver LK, Hopkins RO, Chan KJ, et al. Hyperbaric oxygen for acute carbon monoxide poisoning. N Engl J Med 2002;347:1057-1067.
- Kaita Y, Tarui T, Shoji T, et al. Cyanide poisoning is a possible cause of cardiac arrest among fire victims, and empiric antidote treatment may improve outcomes. Am J Emerg Med 2018;36:851-853.
- Saffle JR, Edelman L, Theurer L, et al. Telemedicine evaluation of acute burns is accurate and cost-effective. J Trauma 2009;67:358-365.
Burn injuries are complex injuries that the acute care physician must be prepared to assess and manage. In addition, an understanding of potential systemic effects from inhalation of toxic components in fires is critical to guide management. The authors provide a timely review of the critical aspects of assessment and management of burn patients.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
