High Altitude Medicine: A Review for the Practicing Emergency Physician
December 15, 2018
Reprints
AUTHORS
Stephen Manganaro, MD, FACEP, FAAFP, FAWM, Core Faculty Attending Physician, Arnot Ogden Medical Center, Elmira, NY
Vincent B. Call, DO, PGY-4 Emergency Medicine, Arnot Ogden Medical Center, Elmira, NY
Daniel Manganaro, MS-3, Lake Erie College of Osteopathic Medicine
PEER REVIEWER
Daniel Migliaccio, MD, Clinical Assistant Professor, Assistant Director, UNC SOM Ultrasound Elective, University of North Carolina, Chapel Hill
EXECUTIVE SUMMARY
- High altitude illness (HAI) is a spectrum of conditions that ranges from acute mountain sickness (AMS) to high altitude cerebral edema (HACE) and high altitude pulmonary edema (HAPE).
- HAI is caused by failure to acclimatize in response to elevation ≥ 8,000 feet (2,500 m) in all three syndromes because of hypobaric hypoxia. Consequently, all three respond to the same essential therapy: descent and supplemental oxygen.
- Acetazolamide is useful to speed the acclimatization process and in treatment and prevention of HAI. Dexamethasone plays a role in the treatment of AMS and HACE.
- HAPE and HACE are severe, life-threatening manifestations of HAI and should be managed aggressively. Patients with HAPE should be evacuated unless good medical care is available. Patients with HACE always should be evacuated.
- Descent is the definitive management for all HAIs.
- Because hypoxemia is maximal during sleep, the sleeping altitude is the critical altitude to consider in assessing patients with HAI.
Introduction
The recognition and treatment of high altitude illness (HAI) is within the core content of emergency medicine practice. In the past five years, more than 100 million people have traveled to altitudes that can cause HAI, and more than 50% of people traveling to altitudes above 18,000 feet (5,500 m) experience some form of HAI. The disease spectrum varies from mild symptoms, such as headaches, to irreversible cerebral edema and even death. In general, acute HAIs result from hypobaric hypoxia, which is exposure to low oxygen states caused by low atmospheric pressure. Syndromes primarily affecting the brain are the primary clinical manifestations of HAI.
High altitude can be described as an altitude of 5,000 feet (1,500 m) to 11,500 feet (3,500 m). Very high altitude is defined as between 11,500 feet and 18,000 feet (3,500 m to 5,500 m), and extreme altitude is elevation greater than 18,000 feet (5,500 m). Elevations greater than 26,000 feet (8,000 m) are known as the “death zone” because they extend beyond the human body’s ability to acclimatize. (See Table 1.)
Table 1. Definitions of High Altitude and Physiologic Responses |
|||
|
Altitude |
Elevation (feet) |
Elevation (m) |
Response |
|
High Altitude |
5,000 to 11,500 |
1,500 to 3,500 |
Little to no symptoms Mild illness possible |
|
Very High Altitude |
11,500 to 18,000 |
3,500 to 5,500 |
O2 desaturation |
|
Extreme Altitude |
≥ 18,000 |
≥ 5,500 |
Acclimatization difficulty |
|
Death Zone |
≥ 26,000 |
≥ 8,000 |
Acclimatization impossible |
|
At the death zone, without supplemental O2, it is physiologically impossible to survive for any prolonged period of time. People are known to summit Mt. Everest (29,029 ft/8,848 m) without oxygen, but they must descend immediately afterward or risk significant illness. |
|||
High altitude syndromes usually are seen at elevations above 8,000 feet (2,500 m) and are caused by hypobaric hypoxia. Milder cases can be seen at ≥ 5,000 feet (1,500 m). HAI represents a spectrum of clinical entities, ranging from common and benign acute mountain sickness (AMS) to life-threatening high altitude pulmonary edema (HAPE) and rare but potentially lethal high altitude cerebral edema (HACE). (See Figure 1.) All three of these syndromes are considered to be caused by a failure of acclimatization. Gradual ascent is the safest method to facilitate acclimatization and prevent HAI. Acclimatization is the process of adapting to hypoxia at altitude; therefore, gradual ascent allows the human body to adapt physiologically. An ascent that is too rapid increases the risk of acclimatization failure, which can lead to severe HAI.
Figure 1. High Altitude Illness Spectrum Representation |
 |
Epidemiology
More than 40 million people worldwide live at altitudes higher than 8,000 feet (2,500 m) above sea level and do not experience acute altitude illness due to acclimatization. However, individuals recruited from lower elevations and brought to work at higher elevations, such as expedition porters, are at risk of HAI, such as life-threatening HAPE and HACE.1
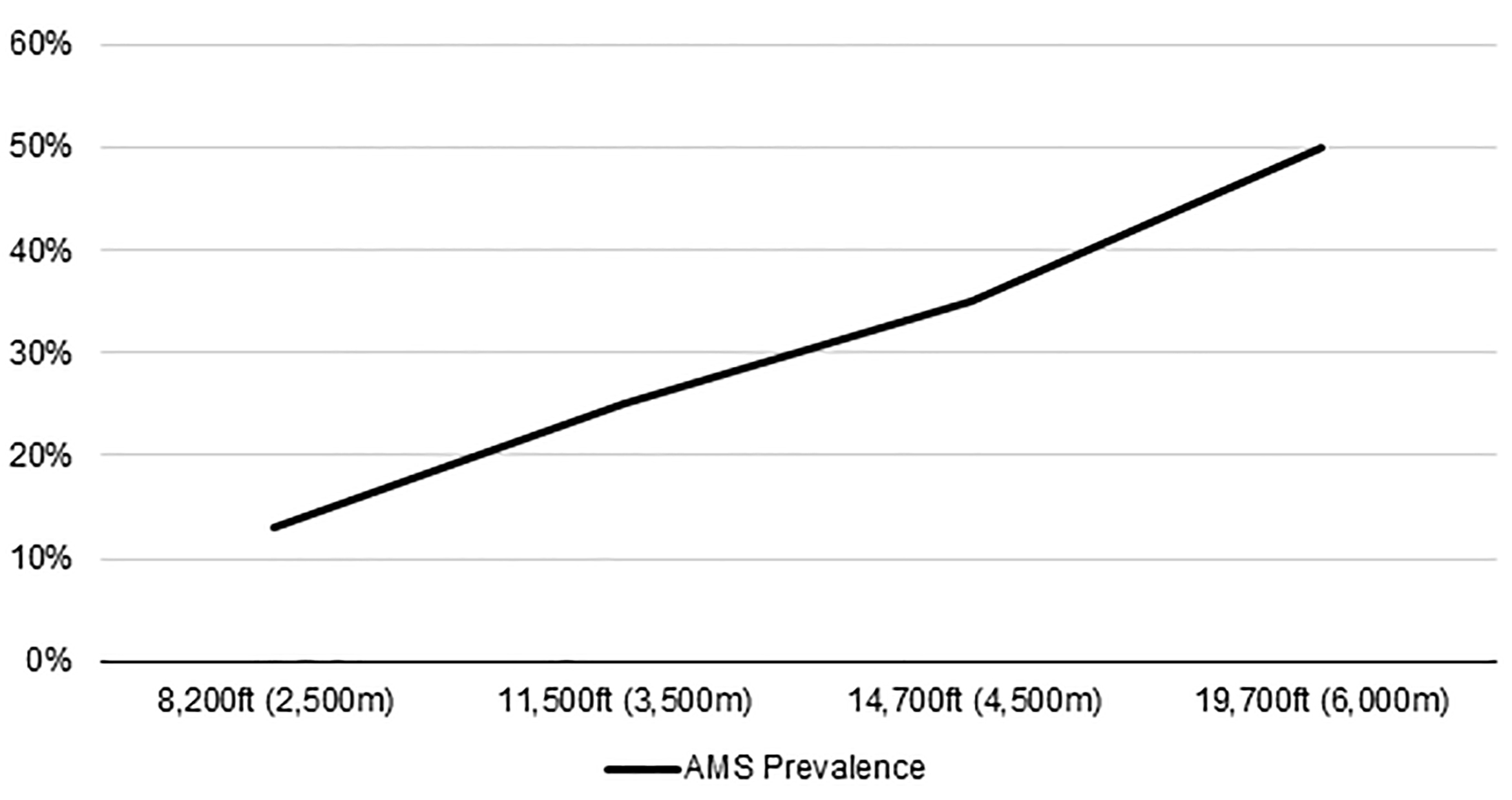
Millions of recreationalists travel to high altitudes for skiing, climbing, and other outdoor sports. Individuals who are not accustomed to living at such altitudes risk developing HAI. The incidence of HAI has been studied in individuals who make a sudden ascent, typically by aircraft. In one study of 3,628 unacclimatized individuals who were flown to an altitude of 12,000 feet (3,600 m), 57% experienced AMS, 1.9% developed HAPE, and none were found to have HACE.2 In a report of 401 participants at greater than 13,000 feet (4,000 m), 25% had symptoms of AMS, 25% had HACE, and 13% had HAPE.3 A meta-analysis found that the incidence of AMS is more frequent with higher elevations. For each 3,300 feet (1,000 m) increase in altitude above 8,000 feet (2,400 m), AMS prevalence increased by 13%.4 (See Figure 2.)
Figure 2. Acute Mountain Sickness Prevalence |
 |
|
The prevalence of acute mountain sickness increases as altitude increases. Source: Meier D, Collet TH, Locatelli I, et al. Does this patient have acute mountain sickness?: The rational clinical examination systematic review. JAMA 2017;318:1810-1819. |
Physiology
AMS occurs within hours to days of ascent and is considered the beginning of a continuum that ends with HACE. HAPE is the pulmonary form of HAI and can occur independently without AMS or concurrently with AMS and HACE. Of all types of HAI, HAPE is the most common cause of death. Both HAPE and HACE are medical emergencies, can be fatal, and require prompt recognition and aggressive treatment.
Hypobaric hypoxia results from a decrease in barometric pressure at altitude. Barometric pressure, often referred to as atmospheric pressure, decreases in a logarithmic manner as altitude increases. According to Dalton’s law of partial pressures, the total pressure in the system is equal to the sum of the partial pressures of all the gases in the system. At sea level, the partial pressure of oxygen is 160 mmHg, which is 20.9% of the total atmospheric pressure of 760 mmHg. As the atmospheric pressure decreases with increases in altitude, the partial pressure of all gases decreases. The fraction of oxygen remains at 20.9%; however, the partial pressure decreases. (See Table 2.) For example, at 10,000 feet (3,000 m), total atmospheric pressure is 522.6 mmHg, and 20.9% is equal 110 mmHg. At altitude, there are fewer molecules in the same volume, thus less oxygen available overall. This is known as hypobaric hypoxia. There is a 50% reduction in barometric pressure at 18,000 feet (5,500 m) compared to sea level. Mt. Everest, the world’s tallest mountain, reaches an elevation of 29,029 feet (8,848 m), where barometric pressure is only 33% of that found at sea level.
Table 2. Dalton’s Law of Partial Pressures |
|||||
|
Feet |
Meters |
Barometric Pressure |
PN2 mmHg (78.0%) |
PO2 mmHg (20.9%) |
PCO2 |
|
Sea level |
Sea level |
760 |
593 |
160 |
8 |
|
5,000 |
1,500 |
639 |
498 |
134 |
7 |
|
8,000 |
2,500 |
574 |
448 |
120 |
6 |
|
10,000 |
3,000 |
534 |
416 |
112 |
6 |
|
15,000 |
4,500 |
443 |
345 |
93 |
5 |
|
20,000 |
6,000 |
365 |
285 |
76 |
4 |
|
25,000 |
7,500 |
299 |
233 |
62 |
3 |
|
29,000 |
8,800 |
253 |
197 |
53 |
3 |
|
Dalton’s law of partial pressures where P (total) is barometric pressure and is equal to the sum of all partial pressures (pN2 + pO2 + p Other gases). |
|||||
AMS results from the effects of low oxygen saturation, referred to as hypoxemia.5 The human body must adapt to the stress of hypoxia through acclimatization, which is a series of complex cellular adjustments that improve oxygen delivery to tissues and enhance hypoxic tolerance. Acclimatization counteracts the hypobaric hypoxia but does not result in “normal physiology” as would be found at sea level.
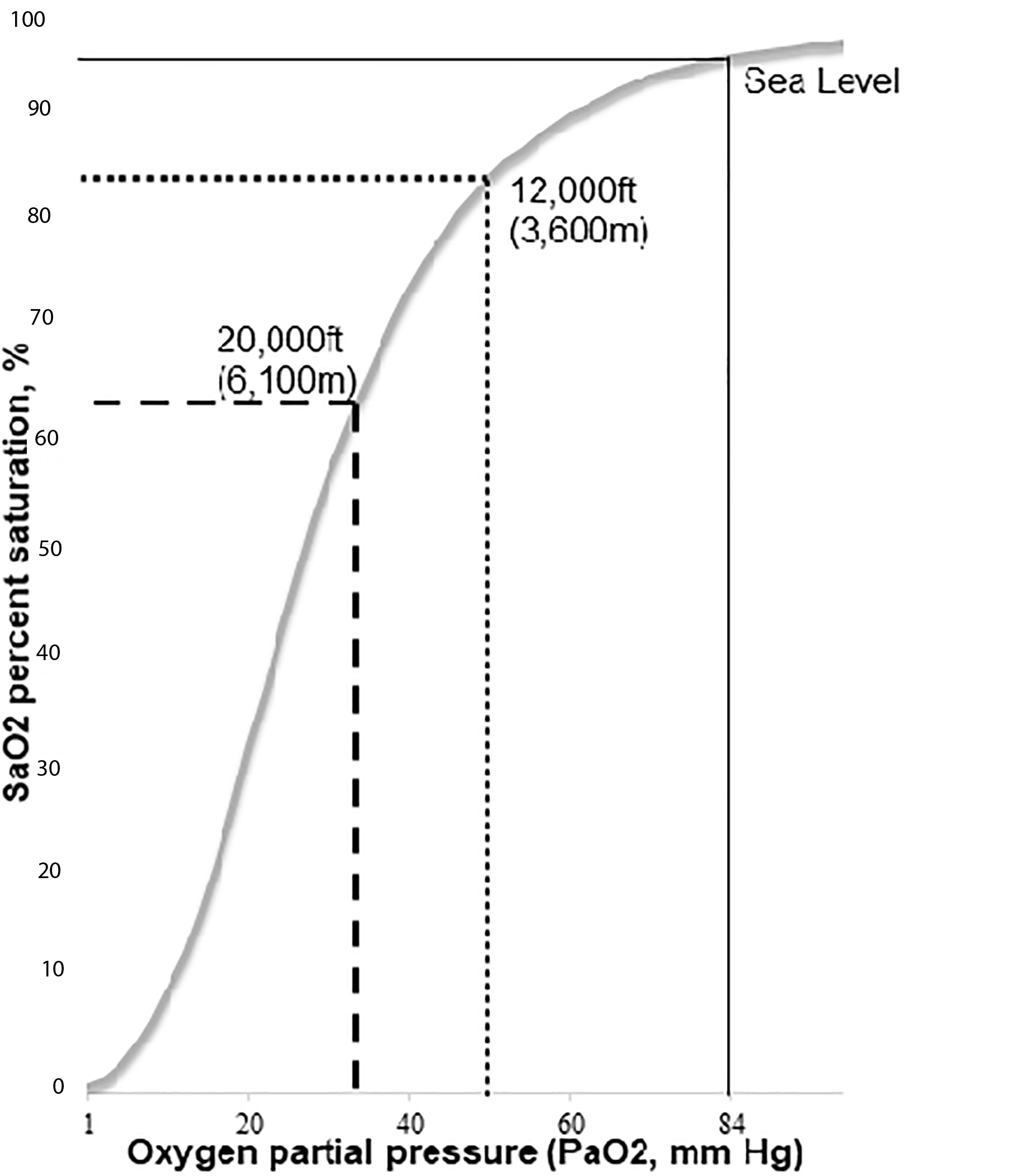
The hemoglobin dissociation curve represents the binding of oxygen to hemoglobin. (See Figure 3.) In the steep portion of the curve, a small change in partial pressure of oxygen in arterial blood (PaO2), caused by the change in altitude, can create a significant change in oxygenation. From sea level to elevation of 12,000 feet (3,600 m), oxygen saturation (SaO2) still is maintained at 85% despite the significant drop in PaO2 from 84 mmHg to 47 mmHg. At 20,000 feet (6,100 m) altitude, this change moves along the steep portion of the hemoglobin oxygenation dissociation curve, resulting in a relatively small change in PaO2 and a large change in SaO2.
The inspired partial pressure of oxygen (pO2) falls at altitude and may fall so sufficiently that the oxyhemoglobin dissociation curve is no longer in its upper flat portion. At moderate altitude, the oxyhemoglobin dissociation curve shifts rightward to assist in unloading of oxygen. This shift is caused by increases in 2,3-diphosphoglycerate resulting from metabolic alkalosis. With an increased rise in altitude, there is marked respiratory alkalosis, which shifts the curve leftward to assist in pulmonary oxygen loading. The body’s physiologic values for the PaO2, SaO2, and partial pressure of arterial carbon dioxide (PaCO2) are given in Table 3.
Figure 3. Hemoglobin Saturation and Dissociation Curve |
 |
|
From sea level to an increase in altitude to 12,000 ft (3,600 m), SaO2 is still maintained at 85% despite the significant drop in PaO2 down to 47 mmHg. At 20,000 ft (6,100 m) altitude, the change is moving along the steep portion of the hemoglobin oxygenation dissociation curve. The change is more significant with a SaO2 of 65% and a PaO2 at 35 mmHg. A small change in PaO2 at altitude causes a disproportionately larger change in SaO2. Source: Severinghaus JW. Simple, accurate equations for human blood O2 dissociation computations. J Appl Physiol Respir Environ Exerc Physiol 1979;46:599-602. |
Table 3. ABG Values of Oxygen and Carbon Dioxide at Various Altitudes |
|||
|
Altitude |
PaO2 (mmHg) |
SaO2 (%) |
PaCO2 (mmHg) |
|
0 ft (0 m) |
90-95 |
96 |
40 |
|
5,000 ft (1,500 m) |
80 |
95 |
36 |
|
8,000 ft (2,500 m) |
75 |
92 |
32 |
|
15,000 ft (4,500 m) |
50 |
86 |
25 |
|
20,000 ft (6,000 m) |
40 |
76 |
20 |
|
25,000 ft (7,500 m) |
35 |
68 |
13 |
|
29,000 ft (8,800 m) |
33 |
58 |
11 |
|
PaO2 = partial pressure of diatomic oxygen, SaO2 = oxygen saturation; PaCO2 = partial pressure of carbon dioxide. |
|||
|
Source: Wagner P. Operation Everest II. High Alt Med Biol 2010;11:111-119. |
|||
The major risk factors for AMS include the rate of ascent, the base altitude of acclimatization, the sleeping altitude, the final altitude reached, and the duration of stay at altitude. Other risk factors that are more individualized include individual genetic susceptibility and comorbidities, such as congenital heart disease, pulmonary hypertension, coronary artery disease, congestive heart failure, sickle cell trait, sickle cell disease, obstructive sleep apnea, and pregnancy.6,7 Anxiety also may be an independent risk factor.8
Traditionally, age was recognized as a risk factor; however, a recent meta-analysis concluded that there was no association between age and the risk of AMS. Prior studies failed to address certain differences that occur throughout the lifespan that account for a seeming association. For example, since sleep quality decreases with age and low-quality sleep increases the risk of AMS, elderly people are more likely to develop AMS. Older trekkers and climbers are likely to have more experience and better control of their ascent rate.9 Younger individuals may have a higher level of physical fitness, but this has not been proven to decrease the incidence of AMS. Males typically are more at risk than females. Alcohol and sedative use increases the risk of acquiring acute altitude sickness. Although smoking traditionally has been considered a risk factor, recent research suggests smoking has neither a positive nor a negative effect on the chance of developing AMS.10 Chronic lung disease such as chronic obstructive pulmonary disease (COPD) is a risk factor for severe altitude-related illness.
The incidence and severity of altitude illness are directly related to elevation and the rapidity of ascent. The pathophysiology effects of high altitude begin when oxygen saturation of arterial blood falls below 90%. Acclimatization is the body’s response to high-altitude hypoxia. It begins within minutes and may continue for months. Multiple organ systems, including respiratory, cardiovascular, renal, and hematologic, respond to hypoxia. The pharmacokinetics of some drugs appear to be altered by high altitudes. Notably, absorption and clearance are decreased, which may require dose adjustments and closer monitoring in acute high-altitude exposure.11
The primary benefit of acclimatization is increased oxygen delivery to the tissues, which protects against HAI and increases exercise capability at altitude. As a person ascends, the carotid bodies sense hypoxia by a decrease in partial pressure of O2 in the alveoli, and signal the respiratory center in the medulla to increase the respiratory rate. In turn, the increased respiratory rate increases minute ventilation, meaning there is a greater volume of total air inhaled and exhaled. By increasing the minute ventilation, more total oxygen is inhaled. This reaction is known as the hypoxic ventilatory response (HVR). The magnitude of the HVR varies among individuals and may be predetermined genetically. HVR may be inhibited by ethanol and sleep medications because they decrease respiratory rate and counteract the normal physiologic response of HVR. Although this initial response may begin within minutes, 80% of the total ventilatory compensation takes place over the course of about four days.
Under normal circumstances at or near sea level, the arterial partial pressure of carbon dioxide (PCO2) is maintained very close to 40 mmHg, even at the expense of arterial PO2. Thus, CO2 is the primary driver of ventilation. However, at around 8,000 feet elevation, because of the level of hypobaric hypoxia with oxygen’s partial pressure at only 75 mmHg, oxygen homeostasis is prioritized over carbon dioxide homeostasis and is achieved via HVR. When the change in altitude is acute, the HVR may cause a significant fall in arterial PCO2, with a concomitant rise in arterial pH resulting in respiratory alkalosis. This low PCO2 then acts on the central respiratory center and limits further increase in ventilation.
In response to hyperventilation and the associated respiratory alkalosis, the kidneys excrete bicarbonate. This induces a metabolic acidosis that allows hyperventilation to continue.
The body’s response to the stress of hypoxia due to ascent leads to a rapid release in catecholamines, which stimulates the circulatory system to increase cardiac output. In turn, there is an increase in heart rate, blood pressure, cardiac output, and venous tone. Over the course of days to weeks, the hematopoietic response includes an increase in erythropoietin levels and increased red blood cell mass. Athletes practice the “live high, train low” method because it leads to a small but significant improvement in sea level performance.12
Long-term adaptation with sustained presence at altitude causes arterial pH to return to normal. Arterial PO2, PCO2, and serum bicarbonate levels remain reduced. The body’s sensitivity to rises in PCO2 levels increases, and HVR increases chronically. Cardiac output returns to normal within a few days of acclimatization. Vital capacity and functional residual capacity are unchanged from baseline, but minute ventilation remains elevated.13,14 People who live at a high altitude have a 10% prevalence of high-altitude pulmonary hypertension.
Although living at a high altitude generally is considered cardioprotective, some high altitude dwellers become intolerant to chronic hypoxia and develop chronic mountain sickness (CMS). CMS is a progressive incapacitating syndrome characterized by excessive erythrocytosis (hemoglobin
≥ 21 g/dL in men and ≥ 19 g/dL in women), severe hypoxemia, headache, dizziness, breathlessness and/or palpitations, sleep disturbances, physical and mental fatigue, localized cyanosis, and distended veins. Among Andean highlanders in Peru who live at an altitude greater than 13,000 feet (4,000 m), 15-25% experience this disease. Furthermore, recent research suggests that individuals who develop CMS and excessive erythrocytosis are at increased risk for hypertension and elevated fasting glucose and are likely to have an increased risk of thrombotic events, such as cardiac thrombosis and stroke.15
Although discrete physiologic responses occur within minutes of exposure to acute hypoxia, the clinical syndromes of AMS develop within four to eight hours of acute exposure to hypobaric hypoxia. With AMS, a poor HVR leads to hypoventilation, which results in fluid retention. This can lead to peripheral edema, decreased urinary output, increased body weight, and increased intracranial pressure.
Centrally mediated periodic breathing (hypopnea) followed by brief periods of apnea (3-10 seconds) while sleeping at a high altitude further exacerbate the hypoxia. Generally, sleep is impaired at high altitude.16 Individuals tend to wake frequently, have unpleasant dreams, and report not feeling refreshed on waking. This sleep-disordered breathing and intermittent hypoxia are associated with excessive sleepiness during the day, difficulty with focusing, impaired memory, and difficulty with tasks requiring sustained attention.17,18,19,20 Periodic breathing occurs in most people at altitudes above 13,000 feet (4,000 m) and results from instability in the HVR. Low oxygen levels during sleep apnea can cause frequent awakenings. Experienced mountaineers recommend climbing high but sleeping low to decrease the incidence of these problems.21,22 Typically, sleep medications are discouraged at altitude because of the risk of further exacerbating impaired ventilation. An exception may be zaleplon and zolpidem, which have been observed to improve objective and subjective sleep quality without impairing ventilation.23 Acetazolamide was not found to help with sleep.23
HACE and HAPE typically occur within two to four days of exposure to high altitude. In HAPE, hypoxia leads to pulmonary vasoconstriction. Additionally, elevation in pulmonary artery pressures results in shear forces that cause plasma fluid to leak into the alveoli and cause a non-cardiogenic pulmonary edema. Pre-existing inflammation, such as autoimmune illness, also may be a risk factor of HAPE, particularly in children. Pre-existing respiratory infection during ascent increases susceptibility to HAPE.
With the cerebral edema seen in HACE, hypoxia induces cerebral vasoconstriction, which increases ICP and causes capillaries to become “leaky,” leading to a vasogenic edema. Within minutes of exposure to hypoxia, cerebral vasodilation occurs as an end effect of increased cerebral blood flow, leading to transcapillary leakage and vasogenic edema. In addition, systemic hypertension from strenuous exercise at high altitude causes increased transcapillary leakage and, therefore, is considered a risk factor for the development of HACE.24,25
Acute Mountain Sickness
AMS is primarily a clinical diagnosis. The Lake Louise scoring system is the accepted reference standard for diagnosis of AMS. A simpler approach is to ask one question: “Overall if you had any symptoms, how did they affect your daily activity?” Responses were scored 0-3, indicating no, mild, moderate, or severe (bed rest) decrease in function. Scores of 2 or higher had a sensitivity of 82% and specificity of 67% for detecting AMS.4
Mild AMS is common with people who experience a rapid ascent. There are no specific physical findings, and the disease varies from mild to severe. Symptoms typically include headache plus at least one of the following: dizziness, fatigue (weakness), insomnia, nausea, vomiting, and anorexia. The headache has been described as ranging from a mild headache to a severe bitemporal throbbing that is worse during the night, in the morning, or when sitting upright. Although some people can travel to locations that are 5,000 feet (1,500 m) or higher and experience symptoms, it is significantly more common once individuals ascend above 8,000 feet (2,500 m). At 8,000 feet (2,500 m), the partial pressure of oxygen decreases to 75 mmHg, which causes hypoxemia and some level of cerebral edema unless the person is acclimatized adequately. AMS typically starts within a few hours after arrival at high altitude and reaches a maximum intensity between 24-48 hours, followed by gradual spontaneous resolution. Provided there is no further ascent, acclimatization eventually will catch up. Patients report that they usually are symptom free by day three or four at altitude. Once symptoms resolve, then further ascent may be attempted. If symptoms haven’t resolved after three to four days, descent should be considered strongly.
Risk factors for AMS include prior history of AMS, low peripheral oxygen saturation (SpO2) from rapid or high ascents, obesity, high sleeping altitudes, sedative hypnotics, and low blood-urea-nitrogen levels.26 Prior history of migraines or headaches at low altitude does not appear to be a risk factor.27
Because there are no objective diagnostic physical findings, a broad differential should be maintained, including tension or migraine headache, caffeine withdrawal, carbon monoxide (CO) poisoning (from campfires), viral syndrome, hypothermia, alcohol intoxication/toxidrome, dehydration, infection (meningitis or encephalitis), intracranial hemorrhage, intracranial mass, venous sinus thrombosis, abdominal process, acute angle closure glaucoma, or other ocular processes.
AMS Treatment
All forms of HAI, including AMS, are treated effectively with cessation of ascent, rest, and supplemental oxygen by nasal cannula to achieve an oxygen saturation of greater than 90%. It is important to treat AMS adequately because the same underlying pathophysiology can lead to life-threatening HACE. In fact, 18 hours of being asymptomatic is recommended before resuming altitude ascent.
Pharmacologic therapy can be a useful adjunct in the treatment of AMS. A recent Cochrane review found that there is low-quality evidence regarding pharmacological and non-pharmacological interventions.28 Of the evidence that does exist, treatment of AMS has been studied the most because it is more prevalent than HACE/HAPE. Currently, acetazolamide is the only drug with an FDA indication for AMS.
Acetazolamide is a safe medication and is the most studied drug for treating AMS symptoms. The drug accelerates acclimatization and, if given early in the development of AMS, usually resolves symptoms within hours. The recommended dose is 250 mg orally twice daily. In some studies, researchers have found lower doses (125 mg or even 62.5 mg orally twice daily) to be just as effective. Acetazolamide may be discontinued as soon as symptoms reach full resolution or may be continued as the preventive dose until two or three days at the maximum altitude.
Acetazolamide is a carbonic-anhydrase inhibitor, which exerts its mechanism of action as a diuretic. It enhances renal bicarbonate diuresis and induces metabolic acidosis, correcting the respiratory alkalosis caused by hyperventilation. The medication also has been shown to decrease nocturnal periodic breathing and improve sleep. As a diuretic, it decreases fluid retention. It is theorized that there are beneficial chemoreceptor effects on ventilatory drive, alterations of cerebral blood flow that lower CSF volume and pressure, as well as relaxation of vascular smooth muscle leading to up-regulation of fluid resorption in the lungs. The most common adverse reactions are paresthesias and polyuria. Other side effects may include nausea, diarrhea, drowsiness, tinnitus, and transient myopia.
Acetazolamide is a sulfa-based compound, but it is a non-antibiotic one that carries a low risk of cross-reactivity for individuals with allergies to sulfa antibiotics.29 However, for patients with history of sulfa antibiotic allergies, trying acetazolamide in a controlled environment prior to any significant ascent is recommended. Acetazolamide is contraindicated in patients with a history of anaphylaxis or severe skin reactions to sulfa-containing medications. Acetazolamide should be avoided in breastfeeding mothers and pregnant women. Acetazolamide also should be avoided in patients with sickle cell disease because of an increased risk of sickling.
Dexamethasone (off-label use) is a safe and effective alternative treatment for AMS. The typical recommended dose for AMS is 4 mg every six hours orally. If the patient cannot tolerate oral administration because of gastrointestinal symptoms, an intramuscular medication can be considered.30 When used for moderate to severe AMS, dexamethasone reduces cerebral blood flow and decreases symptoms, but unlike acetazolamide, it does not enhance acclimatization. Individuals with AMS may resume their ascent after symptoms resolve and they likely would benefit from starting acetazolamide use when re-attempting ascent. Further ascent is discouraged if symptoms recur and persist.
Analgesics are used for symptomatic treatment of high-altitude headache. Aspirin, ibuprofen,31 and acetaminophen are useful to treat headaches. Avoid narcotic analgesics and sedative hypnotics because of depression of HVR.
The definitive treatment for AMS is descent. Because of the risk of developing HACE, descent is recommended when no improvement of symptoms occurs within 48 hours using the therapies mentioned. If descent is not feasible, then consider the use of a portable hyperbaric chamber or evacuation.
AMS Prevention
Prior to any ascent to a high altitude, some simple measures may prove helpful. People ascending to a high altitude should avoid the use of alcohol, caffeine, and sedatives. They should consider bringing acetazolamide to help with acclimatization and zolpidem to assist with sleep. They should obtain a medical evaluation prior to travel. People also should be well rested prior to starting a strenuous journey at altitude. Those taking a long flight to a high altitude should get as much rest as possible on the plane. Travelers should not overhydrate, but should be vigilant to not become dehydrated.
During a trek, sleeping at lower altitudes is beneficial. Because hypoxemia is maximal during sleep, the sleeping altitude is a critical altitude to consider in efforts to avoid AMS. Gradual ascent also will help by giving the body time to acclimatize adequately. Limiting ascent to no more than 2,000 feet (600 m) per day is recommended. There is little evidence that a high carbohydrate diet prevents AMS.
The authors of a 2017 Cochrane review found that acetazolamide is effective in preventing acute HAI, based on moderate evidence.
Dexamethasone has been shown to help with prevention of AMS in small studies and in a meta-analysis;33 however, the quality of evidence overall is weak to give it a strong recommendation.34 Dexamethasone dosing for prevention of AMS is 2 mg orally every six hours or 4 mg every 12 hours starting on the day of ascent. This may be discontinued after staying at the same elevation for two or three days or if descent is initiated. Do not exceed a 10-day course. In some situations, such as rapid ascent to altitudes higher than 3,500 m (for example, for rescue or military operations), 4 mg every six hours may be considered. Patients with COPD receive little to no AMS prevention benefit from taking dexamethasone, although dexamethasone was found to mitigate altitude-induced hypoxemia.35
Budesonide also has been shown to help, but the evidence is weak and the medication is not strongly recommended at this time.34
Nonsteroidal anti-inflammatory drugs (NSAIDs) have been studied and are probably a safe alternative for prevention of AMS, but studies have been small in sample sizes and have failed to have the adequate power to recommend NSAIDs.36
Others medications proposed to treat AMS include spironolactone, drug classes such as selective 5-hydroxytryptamine(1) receptor agonists, N-methyl-D-aspartate (NMDA) antagonist, endothelin-1 antagonist, and anticonvulsant drugs. There is scarce evidence to support or recommend any of these.37
High Altitude Pulmonary Edema
HAPE can occur above 8,000 feet (2,500 m), but it is more common at altitudes above 10,000 feet (3,000 m). HAPE is more severe than AMS and is the most common fatal manifestation of HAI. HAPE usually begins two to four days after arrival at high altitude and its onset may be subtle. Less commonly, it may develop rapidly within a few hours at altitude. If symptoms emerge at less than 10,000 feet (3,000 m) or after four days of altitude reached, consider an alternate diagnosis.
Hallmark symptoms include significant dyspnea on exertion and dyspnea at rest. It also may present as fatigue with minimal to moderate effort. This may be noticed because the rest of the team may have recovered from exertion, but the symptomatic patient still may be dyspneic. Shortness of breath at rest is considered a red flag. AMS symptoms can occur concurrently with the development of HAPE. Usually, the dyspnea causes further deterioration if left untreated. Often a patient may experience a dry cough that then may progress to the production of clear, watery sputum. Hemoptysis is seen in more severe cases. Nail bed cyanosis may occur, with central cyanosis sometimes occurring in severe cases. Further deterioration may be manifested by signs of central nervous system (CNS) dysfunction, indicating the possibility of coexistent HACE.
In these circumstances, urgent therapy is warranted. Patients may have rales, which can be unilobar early or bilateral multilobar later. Patients typically develop tachypnea and tachycardia as symptoms progress. They may experience associated peripheral edema from the AMS physiologic response, causing fluid retention.
HAPE is caused by hypoxia-induced pulmonary artery hypertension, which results in increased pulmonary vascular resistance. This increases the pulmonary capillary pressure, resulting in a transudative fluid and protein leak into the lungs. Inflammation typically is present. This may be caused, in part, by the transudate, but will worsen the pulmonary edema.
The differential diagnosis includes pneumonia, which may have a similar presentation, but often has fever and signs of systemic toxicity. High altitude may predispose individuals to bacterial infections because of impairment of T-lymphocytes. If patients present with symptoms consistent with pneumonia at high altitude, HAPE treatment also should be started. If there is uncertainty, treat both entities, including giving antibiotics for pneumonia.
Bronchitis and pharyngitis are common problems among mountaineers. As patients breathe large volumes of cold, dry air into the upper airway, it is not uncommon to experience some mucosal inflammation. Sputum production also may be present. Antibiotics usually are not helpful. Supportive care typically is sufficient, but care must be taken not to miss HAPE.
Pulmonary embolism (PE) is a consideration when patients have shortness of breath. Patients already have a risk factor, including decreased ambulation during long plane trips, making them more susceptible to thromboembolic disease. Altitude also causes hyperviscosity because of elevated hematocrit and dehydration, which is a known risk factor for hypercoagulability. Although HAPE may have a similar presentation to PE, usually HAPE will not feature an onset as rapid as the one for PE, nor will it involve pleuritic chest pain as may be seen in PE.
Other considerations that are possible depending on the patient’s comorbidities include carbon monoxide poisoning, pneumothorax, pleural effusion, acute coronary syndrome, acute congestive heart failure, congestive heart failure exacerbation, COPD exacerbation, pulmonary hypertension exacerbation, acute asthma exacerbation, and valvular disease exacerbations.
Imaging may be helpful. Thoracic ultrasonography may demonstrate B-lines indicating that there is pulmonary edema. High pulmonary artery pressures also may be measured via echocardiography and, when coupled with normal left ventricular ejection fraction, suggest HAPE. On chest radiography, HAPE may present with alveolar infiltrates, patchy in distribution, with areas of clearing between the patches. Mild cases may be unilateral. Bilateral infiltrates are seen in more severe cases, and right mid-lung field involvement is the most common finding. The degree of pulmonary edema seen on radiography seems to correlate with severity of the disease.
HAPE Treatment
Descent is the definitive therapy for HAPE and should be done in almost all cases. Descent will reverse the symptoms rapidly and is recommended in areas of limited medical therapy. Even a descent as little as 1,000 to 3,000 feet (300-900 m) could be lifesaving. If HAPE is mild, descent may not be necessary, but the patient still should be evacuated to a medical facility capable of treating HAPE.
Portable hyperbaric chambers are small, lightweight chambers that simulate descent by generating about 100 mmHg (2 psi) above the ambient pressure. The 100 mmHg of additional pressure effectively simulates a descent of 3,500-5,000 feet (1,000-1,500 m) when at moderate altitudes. These chambers may have a role in the treatment of HAPE, especially if descent or evacuation is not feasible. For example, if the patient is unable to ambulate or if severe weather conditions make descent unsafe, it may be reasonable to consider a portable hyperbaric chamber treatment. However, caution is advised because of the risks involved. Patients who are vomiting actively may not protect their airway adequately.
Hyperbaric chambers provide very high concentrations of oxygen for short periods of time. Care should be taken to monitor for signs of oxygen toxicity, such as CNS toxicity (e.g., facial twitching and behavioral changes), pulmonary toxicity (e.g., chest pain with inspiration), or visual toxicity (tunnel vision). Some patients can descend without significant assistance after a few hours in a portable hyperbaric chamber.
Patients must be symptom free for at least 72 hours before attempting further ascent. If any symptoms recur, then evacuation is recommended. If a patient plans to fly home, he or she should have adequate recovery time prior to a major airline flight at altitude with a cabin pressure near 8,000 feet (2,500 m) to prevent recurrence of the disease.
Oxygen therapy increases the rate of symptom improvement. In more severe cases, patients will be hypoxemic. Oxygen should be high-flow of 6-8 L/min by mask to achieve SpO2 greater than 95%. Positive pressure ventilation with bilevel positive airway pressure (BiPAP) or continuous positive airway pressure (CPAP) is preferred, when available, and may decrease pulmonary artery pressure and improve clearance of alveolar fluid.
Medications are adjunctive to the definitive therapy of descent. Nifedipine (off-label use) is a calcium channel blocker that may be effective in lowering pulmonary artery pressure, pulmonary blood volume, and pulmonary vascular resistance. The typical dosing would be extended-release 30 mg every 12 hours.
There is some controversy that nifedipine may increase the risk for developing HACE because of its effects on lowering systemic blood pressure. The cerebral perfusion pressure is equal to the mean arterial pressure minus the intracranial pressure (CPP = MAP – ICP). Since intracranial pressure tends to be fixed, lowering mean arterial pressure also would lower cerebral perfusion pressure. Nifedipine typically is reserved for situations in which descent is not possible or there is a lack of oxygen availability.
Diuretics do not help with pulmonary edema, as the cause is not cardiogenic in nature. Phosphodiesterase type 5 inhibitors (PDE-5; tadalafil, sildenafil) are known to be useful for HAPE prevention but lack sufficient evidence to strongly recommend their use. Their proposed mechanism is the inhibition of degradation of cyclic GMP. Increased levels of cGMP cause relaxation of the pulmonary vasculature, decreasing pulmonary artery pressure. Ultimately, this leads to a decrease in capillary leak into the alveoli. Inhaled long-acting beta-
agonists, such as salmeterol 125 mcg inhaled twice daily, have been used anecdotally. Salmeterol may increase fluid clearance from alveolar spaces.
HAPE Prevention
HAPE is more difficult to prevent than AMS or HACE. Once a patient experiences HAPE, he or she is more likely to experience HAPE in the future, and prophylaxis is indicated. Slow ascent of less than 1,200 feet (< 350 m) per day is recommended. Acetazolamide may help by increasing the speed of acclimatization. If a patient has had a prior episode of HAPE, prophylaxis is recommended with nifedipine and a PDE-5 inhibitor. The nifedipine dosage for prevention is extended-release 30 mg every 12 hours starting the day before ascent; nifedipine may be discontinued after staying at the same altitude for five days or when descent is initiated.
PDE-5 inhibitors dosing is as follows: sildenafil 40 mg every eight hours or tadalafil 10 mg every 12 hours. There are limited data regarding the use of dexamethasone to reduce the rate of HAPE, but it may be of help by decreasing the inflammatory cascade causing pulmonary capillary leak when given two days before ascent to prevent HAPE (8 mg every 12 hours).
High Altitude Cerebral Edema
HACE is a severe, but the least common, form of HAI. Severe symptoms usually develop within one to three days. Severe HACE with coma has been reported in as few as 12 hours after mild AMS was noted. Other reports indicate it did not occur until days 5-9. Cases of HACE have been reported only at moderate altitudes (> 8,500 feet or
> 2,500 m).
The hallmark symptom of HACE is global central nervous system effects. Ataxia is the most common and most sensitive finding associated with HACE. Ataxia is caused by cerebellar hypoxia as a result of cerebral edema. Ataxia testing with a simple heel-to-toe tandem walk and a Romberg test usually is clinically sufficient. One of these tests is insufficient to exclude the diagnosis of HACE, so both tests must be performed. No evidence supports the need for more sophisticated cerebellar testing.38
Other symptoms may include severe headache, nausea and vomiting, altered mentation, slurred speech, seizures, and coma. Focal neurologic deficits also may be seen but rarely occur. Ataxia alone is sufficient to indicate immediate descent and evacuation. Patients who experience coma have a mortality rate greater than 60%.
Intermittent CNS symptoms could be indicative of an alternative diagnosis, such as hypothermia, hypoglycemia, carbon monoxide poisoning, or transient ischemic attack (TIA). If symptoms are sudden in onset or focal in nature, consider acute stroke, TIA, and intracranial hemorrhage. Other considerations are meningitis, encephalitis, intracranial mass, vertebral dissection or stenosis, carotid dissection or stenosis, acute toxidrome or withdrawal such as in alcohol or drug use, seizure disorder, and transient global amnesia.
Advanced imaging may be required to differentiate between HACE and other acute pathologies. MRI of HACE shows white matter changes consistent with vasogenic edema.
HACE Treatment
As in all forms of AMS, definitive treatment is descent and evacuation with two assistants. If descent is not feasible because of weather or terrain considerations, portable hyperbaric chambers also are effective and may result in some temporary improvement, but evacuation still is necessary when feasible. CNS deficits may take days to resolve, even after descent. Recovery with prolonged sequelae, especially ataxia lasting for weeks, is common. Most survivors of HACE eventually have full neurologic recovery.
Oxygen at 2-4 L/min by vented mask or nasal cannula should be administered to a target SpO2 greater than 90%. Increased oxygen potentially reduces intracranial blood flow at high altitude. Over-oxygenation may cause acute toxicity resulting in CNS manifestations, such as twitching, vertigo, altered behavior, clumsiness, and convulsions. Oxygen toxicity also may result in pulmonary symptoms, such as tracheobronchitis, acute respiratory distress syndrome, pulmonary interstitial fibrosis, and absorption atelectasis due to washout of nitrogen causing lung collapse and air trapping. Oxygen toxicity occurs from free radical tissue damage and inhibition of oxygen-sensitive enzymes.39
Dexamethasone 8 mg should be given orally (if the patient can tolerate it) or intramuscularly/intravenously (in more severe cases or if the patient cannot safely swallow). This should be followed by dexamethasone 4 mg every six hours. Patients who have significant alterations of consciousness should be intubated to protect their airway. The increased cerebral pressure may benefit from hyperventilation, diuretics, and mannitol. Patients with HACE typically are volume depleted from poor fluid intake, so these efforts actually may decrease cerebral perfusion, and caution is advised.
HACE is an uncommon disease, so data are lacking about effective treatments, but survivors of HACE certainly benefited from oxygenation and descent.
HACE Prevention
Graded ascent is the safest method to facilitate acclimatization and prevent HAI. Two to three nights at 5,000-7,000 feet (2,500-3,000 m) before further ascent likely is beneficial. Increases of greater than 2,000 feet (600 m) per day should be avoided. Acetazolamide 125 mg orally twice per day starting two days before ascent helps in AMS prevention.
Table 4. High Altitude Illness Syndromes |
|||
|
Condition |
Severity |
Clinical Findings |
Treatment |
|
Acute Mountain Sickness |
Mild to moderate |
Headache, nausea, vomiting, weakness, dizziness, difficulty sleeping |
• Acetazolamide 125 mg to 250 mg twice per day, dexamethasone, ibuprofen, or acetaminophen • Antiemetics, supplemental O2 at night, descent |
|
High Altitude Pulmonary Edema |
Life-threatening |
Weakness, cough, exercise intolerance, cyanosis, dyspnea at rest, respiratory distress |
• Descent • Oxygen • Airway support • Evacuate |
|
High Altitude Cerebral Edema |
Life-threatening |
Ataxia, confusion, coma |
• Evacuation and descent • Oxygen • Airway support • Dexamethasone |
Altitude and Underlying Medical Conditions
Individuals with moderate to severe COPD, coronary artery disease (CAD), or congestive heart failure (CHF) should avoid high altitudes because these disease states may be made worse by the hypoxic environment. These patients may experience more difficulty with acclimatization. Patients with sickle cell anemia with a history of crises will experience additional stress from hypoxia and are at risk of a vaso-occlusive crisis at altitude; these patients also may develop splenic ischemia or infarction.
Caution is advised to all patients with any history of COPD, asthma, morbid obesity, CHF, CAD, history of cardiac arrhythmia, sickle cell trait, sickle cell disease, seizure disorders, and pregnancy. High altitude hypobaric hypoxia may exacerbate symptoms in these comorbid states. Pregnant patients who are permanent high-altitude residents have increased complications in maternal, fetal, and neonatal life.
Evacuation
With all high-altitude illness, the definitive treatment is descent. Descent is not the same as evacuation; evacuation implies removing the individual from altitude and bringing the individual to a medical facility where appropriate care may be given.
AMS does not necessarily require evacuation. Medical treatment for AMS should be initiated as soon as AMS is recognized. Patients should rest and may consider restarting a climb with extreme caution because AMS may progress to HACE.
HACE is life-threatening and when recognized even with mild ataxia, patients always should be evacuated to lower altitude.
If away from medical resources, patients with HAPE must be evacuated emergently. HAPE may have a rapid progression to life-threatening pulmonary edema and result in death. With appropriate medical resources and milder forms of HAPE, the patient may be treated at a medical facility that still is at moderate-high altitude. These patients must be supervised closely with O2 monitoring. Patients who do not improve then must descend and be evacuated to a medical facility at low altitude. If the patient is stable at altitude, he or she should be symptom free for at least three days and then may attempt climbing altitude again. If any respiratory symptoms arise again, the patient should be evacuated.
Conclusion
HAI is a spectrum of disorders, including AMS, HACE, and HAPE. AMS can present as mild as headache with accompanying symptoms such as nausea, lightheadedness, fatigue, anorexia, or sleep disturbance. Mild forms of AMS may not require treatment. However, HAPE and HACE are severe and potentially life-threatening illnesses that require prompt recognition and treatment to prevent morbidity and mortality.
HAI is caused by failure to acclimatize to elevation ≥ 8,000 feet (2,500 m) in all three syndromes and, thus, they all respond to the same essential therapy: descent and supplemental oxygen. Descent is the definitive therapy for all HAI. Acetazolamide is useful to speed the acclimatization process and is useful in treatment and prevention of HAI. Sleeping at lower altitudes may be useful to aid in acclimatization. Dexamethasone is a useful adjunct medication for treating AMS and HACE.
Because AMS can deteriorate and progress to HAPE or HACE, patients with AMS should be monitored carefully. HAPE is characterized by dyspnea, decreased exercise tolerance, cough, and tachycardia, and commonly presents as a non-cardiogenic pulmonary edema. HAPE is the most common cause of death related to HAI and requires aggressive management: supplemental oxygen, descent, and possibly nifedipine. HACE is the most severe form of AMS and usually presents with symptoms similar to AMS plus CNS changes such as ataxia, confusion, mood changes, coma, and papilledema. HACE requires descent and evacuation, dexamethasone, and supplemental oxygen.
Many chronic illnesses and comorbidities worsen at moderate to high altitude, and patients should seek medical evaluation before traveling to altitude.
REFERENCES
- Koirala P, Wolpin SE, Peterson JT. High altitude illness: Knowledge, practice, and attitudes of porters in Nepal. Wilderness Environ Med 2018;29:431-436.
- Ren Y, Fu Z, Shen W, et al. Incidence of high altitude illnesses among unacclimatized persons who acutely ascended to Tibet. High Alt Med Biol 2010;11:39-42.
- Croughs M, Van Gompel A, Rameckers S, Van den Ende J. Serious altitude illness in travelers who visited a pre-travel clinic. J Travel Med 2014;21:403-409.
- Meier D, Collet TH, Locatelli I, et al. Does this patient have acute mountain sickness?: The rational clinical examination systematic review. JAMA 2017;318:1810-1819.
- Guo G, Zhu G, Sun W, et al. Association of arterial oxygen saturation and acute mountain sickness susceptibility: A meta-analysis. Cell Biochem Biophys 2014;70:1427-1432.
- MacInnis MJ, Koehle MS, Rupert JL. Evidence for a genetic basis for altitude illness: 2010 update. High Alt Med Biol 2010;11:349-368.
- Luks AM, McIntosh SE, Grissom CK, et al. Wilderness Medical Society practice guidelines for the prevention and treatment of acute altitude illness: 2014 update. Wilderness Environ Med 2014;25(4 Suppl):S4-14.
- Boos CJ, Bass M, O’Hara J, et al. The relationship between anxiety and acute mountain sickness. PLoS One 2018;13:e0197147.
- Wu Y, Zhang C, Chen Y, Luo YJ. Association between acute mountain sickness (AMS) and age: A meta-analysis. Mil Med Res 2018;5:14.
- Vinnikov D, Blanc PD, Steinmaus C. Is smoking a predictor for acute mountain sickness? Findings from a meta-analysis. Nicotine Tob Res 2016;18:1509-1516.
- Bailey DM, Stacey BS, Gumbleton M. A systematic review and meta-analysis reveals altered drug pharmacokinetics in humans during acute exposure to terrestrial high altitude — clinical justification for dose adjustment? High Alt Med Biol 2018;19:141-148.
- Chapman RF. The individual response to training and competition at altitude. Br J Sports Med 2013;47(Suppl 1):i40-i44.
- West JB. Chapter 9: Respiratory system under stress. In: Respiratory Physiology: The Essentials. 9th ed. Baltimore: Lippincott Williams & Wilkins; 2012.
- Levitzky MG. Chapter 11. The respiratory system under stress. In: Pulmonary Physiology. 7th ed. New York: McGraw Hill Medical; 2007.
- Corante N, Anza-Ramírez C, Figueroa-Mujíca R, et al. Excessive erythrocytosis and cardiovascular risk in Andean highlanders. High Alt Med Biol 2018;19:221-231.
- Horiuchi M, Uno T, Endo J, et al. Impact of sleeping altitude on symptoms of acute mountain sickness on Mt. Fuji. High Alt Med Biol 2018;19:192-200.
- Morell MJ, Twigg G. Neural consequences of sleep disordered breathing: The role of intermittent hypoxia. Adv Exp Med Biol 2006;588:75-88.
- Dempsy JA, Veasey SC, Morgan BJ, O’Donnell CP. Pathophysiology of sleep apnea. Physiol Rev 2010;90:47-112.
- Beaudin AE, Hartmann SE, Pun M, Poulin MJ. Human cerebral blood flow control during hypoxia: Focus on chronic pulmonary obstructive disease and obstructive sleep apnea. J Appl Physiol 2017;123:1350-1361.
- Beaudin AE, Waltz X, Hanly PJ, Poulin MJ. Impact of obstructive sleep apnea and intermittent hypoxia on cardiovascular and cerebrovascular regulation. Exp Physiol 2017;102:743-763.
- West JB; American College of Physicians; American Physiological Society. The physiologic basis of high-altitude diseases. Ann Intern Med 2004;141:789-800.
- Weil JV. Sleep at high altitude. High Alt Med Biol 2004;5:180-189.
- Kong F, Liu G, Xu J. Pharmacological agents for improving sleep quality at high altitude: A systematic review and meta-analysis of randomized controlled trials. Sleep Med 2018;51:105-114.
- Harris NS. Chapter 136. High-altitude medicine. In: Walls RM, Hockberger RS, Gausche-Hill M. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia: Elsevier; 2018: 1787.
- Hackett PH, Davis CB. Chapter 221. High-altitude disorders. In: Tintinalli JE, Stapczynski JS, Ma OJ, et al. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th ed. New York: McGraw Hill; 2015:1429.
- Wang K, Zhang M, Li Y, et al. Physiological, hematological and biochemical factors associated with high-altitude headache in young Chinese males following acute exposure at 3700 m. J Headache Pain 2018;19:59.
- Schneider M, Bärtsch P. Characteristics of headache and relationship to acute mountain sickness at 4559 meters. High Alt Med Biol 2018; doi: 10.1089/ham.2018.0025. [Epub ahead of print].
- Simancas-Racines D, Arevalo-Rodriguez I, Osorio D, et al. Interventions for treating acute high altitude illness. Cochrane Database Syst Rev 2018;6:CD009567.
- Platt D, Griggs R. Use of acetazolamide in sulfonamide-allergic patients with neurologic channelopathies. Arch Neurol 2012;69:527-529.
- Luks AM, McIntosh SE, Grissom CK, et al. Wilderness Medical Society consensus guidelines for the prevention and treatment of acute altitude illness. Wilderness Environ Med 2010;21:146-155.
- Xiong J, Lu H, Wang R, Jia Z. Efficacy of ibuprofen on prevention of high altitude headache: A systematic review and meta-analysis. PLoS One 2017;12:e0179788.
- Tang E, Chen Y, Luo Y. Dexamethasone for the prevention of acute mountain sickness: Systematic review and meta-analysis. Int J Cardiol 2014;172:133-138.
- Sridharan K, Sivaramakrishnan G. Pharmacological interventions for preventing acute mountain sickness: A network meta-analysis and trial sequential analysis of randomized clinical trials. Ann Med 2018;50:147-155.
- Nieto Estrada VH, Molano Franco D, Medina RD, et al. Interventions for preventing high altitude illness: Part 1. Commonly-used classes of drugs. Cochrane Database Syst Rev 2017;6:CD009761
- Furian M, Lichtblau M, Aeschbacher SS, et al. Efficacy of dexamethasone in preventing acute mountain sickness in COPD patients: Randomized trial. Chest 2018;154:788-797.
- Pandit A, Karmacharya P, Pathak R, et al. Efficacy of NSAIDs for the prevention of acute mountain sickness: A systematic review and meta-analysis. J Community Hosp Intern Med Perspect 2014;4. doi: 10.3402/jchim.v4.24927.
- Gonzalez Garay A, Molano Franco D, Nieto Estrada VH, et al. Interventions for preventing high altitude illness: Part 2. Less commonly-used drugs. Cochrane Database Syst Rev 2018;3:CD012983.
- Bird BA, Wilson MH, Johnson BG, et al. High altitude ataxia – its assessment and relevance. Wilderness Environ Med 2011;22:172-176.
- Chawla A, Lavania AK. Oxygen toxicity. Med J Armed Forces India 2001;57:131-133.
The recognition and treatment of high altitude illness is within the core content of emergency medicine practice. High altitude illness represents a spectrum of clinical entities, ranging from common and benign acute mountain sickness to life-threatening high altitude pulmonary edema and rare but potentially lethal high altitude cerebral edema.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
