Making Sense of Delirium in the Emergency Department
February 1, 2019
Reprints
Related Articles
-
Is Artificial Intelligence Coming for Your Job?
-
Can Pulmonary Artery Pressure Help in the Decision to Operate in Chronic Aortic Regurgitation?
-
Combined TAVR and LAAO Studied in a Randomized Controlled Trial
-
Another Hemodynamic Variant of Aortic Stenosis
-
Clinical Features of Tachyarrhythmia-Induced Cardiomyopathy
AUTHORS
Gregory Sugalski, MD, Associate Professor, Department of Emergency Medicine, Rutgers New Jersey Medical School, Newark
Michael Ullo, MD, Resident Physician PGY-3, Department of Emergency Medicine, Rutgers New Jersey Medical School, Newark
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Attending Physician, Mt. Sinai Queens Hospital Center, Assistant Clinical Professor of Emergency Medicine, Mt. Sinai Medical School, Jamaica Queens, NY
EXECUTIVE SUMMARY
- Delirium is a process that develops over hours to a few days.
- The primary cognitive impairment in delirium is that of inattention to the circumstances and environment surrounding the patient, as opposed to memory impairment seen in the patient with dementia.
- Clinical features of delirium fluctuate throughout the day; the patient may appear normal in between episodes.
- The most common patient with delirium is an elderly individual with comorbidities taking multiple medications.
- The ED assessment focuses on identifying common precipitating conditions, such as infections, metabolic abnormalities, or adverse drug effects.
- Neuroleptics (e.g., haloperidol, risperidone) are the preferred agents when chemical restraint is required.
- Admission to the hospital for further investigation, treatment, and monitoring of response almost always is required.
Editor’s Note
While it may be true that a rose by another name would still smell as sweet, there is value to calling things by their correct names. What is a good word to describe the agitated and confused patient? There are many possible terms, more than 25 by one count, but let us consider the term delirium. The word has been in use since the mid-16th century. It was derived from two Latin words, de (“away”) and lira (“ridge between furrows”). The combination “delirare” literally means to “deviate from the furrow.” As used, it meant to deviate or be deranged. Use of the word peaked in the second half of the 19th century and declined in the 20th century as descriptive terms, such as altered mental status, acute confusional state, or encephalopathy, came into common use. This is partly a shame. The word delirium packs a wallop’s worth of meaning into just eight characters. Fortunately, it never went away completely, being established in 1966 within the Medical Subject Heading structure developed by the National Library of Medicine. The word is undergoing something of a rebirth as clinical investigators are rediscovering its utility. The European Delirium Association, the American Delirium Society, and the Australasian Delirium Association, professional organizations formed to study this syndrome, have embraced the term delirium.
Delirium and encephalopathy often are used interchangeably in the clinical setting as well as in the research and literature. Unfortunately, medical diagnosis coding using either ICD-9 or ICD-10 has not kept up with modern understanding of this syndrome. Instructions for medical diagnosis coders often direct using delirium when the symptoms result from psychiatric origin and reserve the use of encephalopathy for a brain malfunction that is a result of an acute or chronic medical disease state. This should not be of importance, but the Centers for Medicare & Medicaid Services gives the nonspecific behavioral diagnosis of delirium a lower severity than the pathophysiological diagnosis of encephalopathy. Doing this often enough can begin to affect things like risk adjustment, hospital profiling, and payment. How many of you have been advised by your coders to use the diagnosis of “acute toxic encephalopathy” as a diagnosis for the agitated and confused patient? I have.
So back to the beginning. Delirium is a great term. Use it wisely and appropriately. You and your consultants know what it means and what it implies. Until the medical diagnosis coding and reimbursement system gets up to date, use acute toxic encephalopathy to ensure appropriate risk adjustment, hospital profiling, and reimbursement occurs. And when selecting fragrant roses, I have been told to seek out the English rose “Lady Emma Hamilton.”
— J. Stephan Stapczynski, MD, Editor
Background
On a routine basis, emergency physicians are charged with the complex task of appropriately recognizing and managing patients who present for medical care with an acute change in mental status. Although the differential diagnosis for altered mental status is broad, the diagnosis of delirium poses a unique challenge to medical personnel. Despite being poorly understood, delirium poses a significant clinical burden with an estimated prevalence of nearly 10% in patients 65 years and older presenting to the emergency department (ED).1,2
Delirium is characterized by a change in mental status accompanied by inattention with an associated fluctuating course. Although no strict definition exists, the diagnostic criteria for delirium as outlined in the 5th edition of the Diagnostic and Statistical Manual of Mental Disorders include:3
- difficulty with attention; the person has decreased ability to focus, sustain, or shift attention;
- difficulty with awareness; the person is not oriented to surroundings, circumstance, or environment;
- difficulty with cognition; the person has impaired memory, language, or perception, or trouble performing visuospatial tasks;
- difficulties in attention, awareness, or cognition that are not explained better by existing dementia and not associated with decreased level of arousal, such as stupor or coma (these difficulties represent an acute change from baseline function, typically develop over a few hours to days, and fluctuate in intensity over the course of the day).
- The history, physical examination, or laboratory findings indicate that the cause is a direct physiologic consequence of a general medical condition, an intoxicating substance, medication use, or is associated with more than one cause.
Epidemiology
Delirium affects a large number of patients within the healthcare system, affecting 7-20% upon ED arrival and 11-42% during hospitalization.4,5 The financial burden on healthcare expenditures related to delirium in the United States ranges between $38 billion and $152 billion, further demonstrating the importance of this clinical entity.6
Understanding the prevalence of delirium remains a challenge because it often is misdiagnosed and underrecognized. Studies evaluating physician identification of delirium in the ED demonstrate accurate diagnosis in only 16-35% of cases. Furthermore, research is fairly limited, because it often excludes a significant number of delirious patients who are unable to communicate or cooperate with research protocols.7,8
The inpatient hospital setting reflects the primary source of epidemiologic data for delirium. Upwards of 30-40% of hospitalized elderly patients will develop delirium at some point during their hospitalization.9 This estimate significantly increases in the intensive care unit (ICU) setting, with delirium affecting nearly 70% of ICU patients.10 Notably, the disease state persists outside of the hospital, as elderly patients typically receive continued medical care after discharge from hospitalization. Prospective data indicate that delirium is diagnosed routinely in hospice units and post-acute care facilities.11,12
Etiology
Delirium is widely accepted as a multifactorial process that represents a unique interaction between vulnerable patients, typically older with a number of comorbid chronic diseases, and exposure to precipitating factors or noxious stimuli.13 Because delirium manifests as a sudden change in brain function potentially due to multiple factors, it is also known as “acute toxic-metabolic encephalopathy.” Although the acute confusional state may occur in the younger, healthier patient population, it is important to recognize that these patients frequently are subject to higher amounts of noxious stimuli before the development of delirium.
Prospective data from validated studies exploring the precipitating factors for delirium have identified many risk factors. Table 1 illustrates the most common predisposing factors in patients diagnosed with delirium on admission in the clinical setting.14
Because delirium remains a diagnostic challenge, physicians should remember the complex interplay between patient risk factors and exposure to adverse stimuli. Identifying high-risk and vulnerable patients (i.e., those with risk factors for delirium) on presentation can heighten suspicion for making the appropriate diagnosis.
Table 1. Leading Risk Factors for Delirium From Validated Predictive Models |
|
Pathophysiology
The mechanism by which delirium occurs is poorly understood and highly variable, as multiple disparate etiologies may lead to a confused state. Therefore, it is unlikely that there is one common pathway that helps to explain the events that precipitate the acute confusional state. It has been difficult to elucidate the biological basis for delirium. Human studies are challenging to perform because of the variable nature of the disorder. Furthermore, animal models have been unable to clarify the mechanism behind delirium. Despite this, several conventionally accepted theories help form the basis of our limited understanding of the pathophysiology behind delirium.
Neuronal Aging Hypothesis
As people age, their brains undergo significant changes, including alterations in neurotransmitter levels, decreased cerebral blood flow, changes in intracellular conduction, and neuronal loss.15 Age alone is a clear independent risk factor for delirium in a hospitalized setting, with a 3% risk for patients younger than 65 years of age to 36% risk for patients older than 75 years of age.16 Compounding this risk is the increased prevalence of dementia with age, which may be the strongest risk factor for the development of delirium, specifically in hospitalized patients.17
Neuroinflammatory Hypothesis
At its core, delirium is a disruption in a patient’s ability to maintain proper attention to his or her surroundings. Activation of the inflammatory cascade due to systemic illness results in release of mediators of inflammation throughout the bloodstream that activate downstream inflammatory changes within the brain. These alterations in the central nervous system induce neuronal dysfunction, which manifests clinically as the behavioral and cognitive changes seen in delirium.18
Neurotransmitter Hypothesis
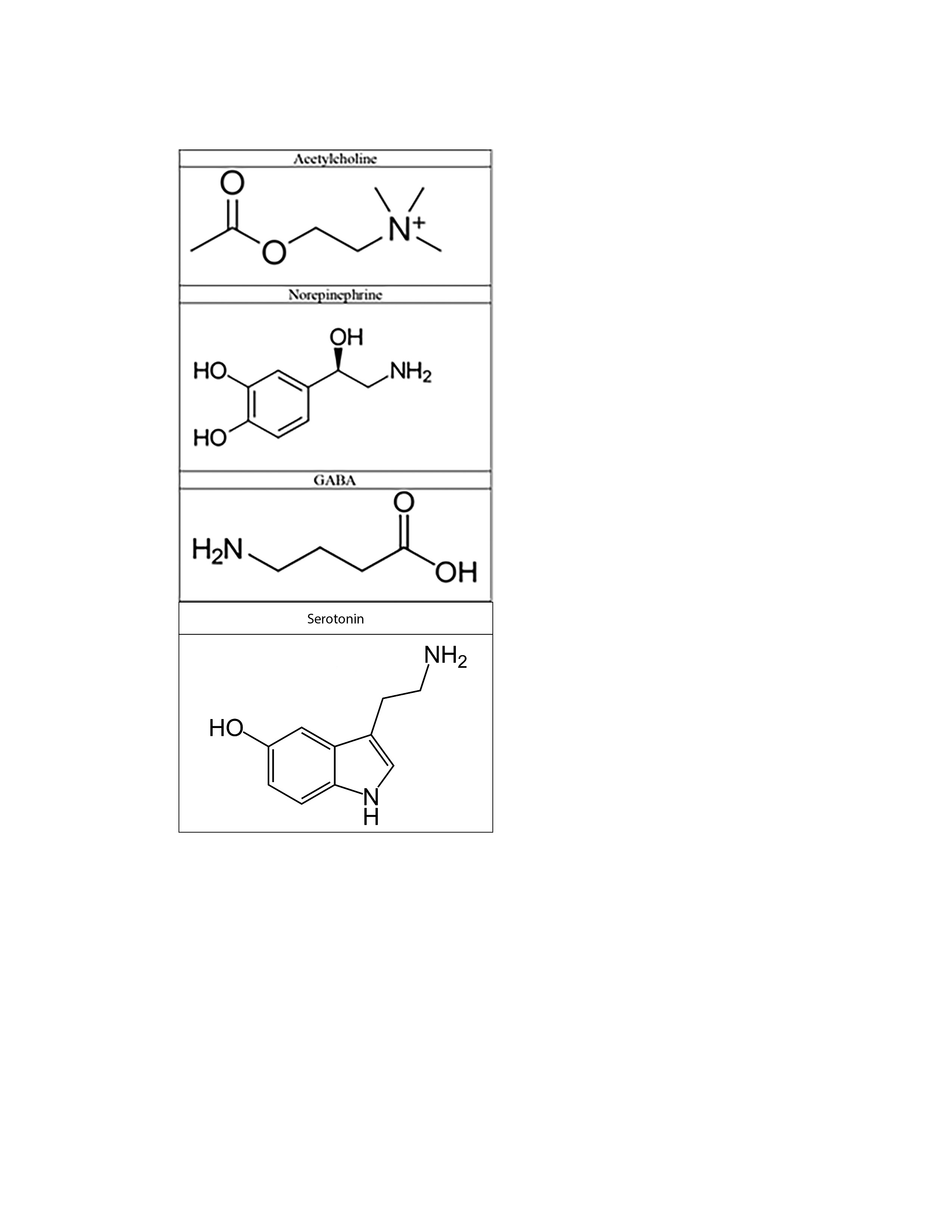
Data from limited animal and clinical studies have supported the notion that neurotransmitter abnormalities result in the delirious state. (See Figure 1.) Acetylcholine has been implicated as a critical neurotransmitter involved, as reduced levels of cholinesterase have been correlated with the development of an acute confusional state.19,20 Anticholinergic medications are well known to have an adverse effect of confusion, particularly in the elderly. This further supports the notion that impaired acetylcholine transmission may result in the cognitive deficits seen in delirium.
Although acetylcholine remains the most well-studied neurotransmitter involved in delirium, other neuronal systems have been implicated. Cerebrospinal fluid of patients with delirium has demonstrated alterations in the expected amount of serotonin, norepinephrine, and gamma-aminobutyric acid (GABA).21
Figure 1. Commonly Implicated Neurotransmitters in Delirium |
 |
Risk Factors
Given the complexity behind the pathogenesis of delirium, it is not surprising that there is a wide array of risk factors. Underlying brain disease remains the most common predisposing risk factor. Dementia, stroke, and Parkinson’s disease have been reported in nearly half of diagnosed delirium cases in older patients.22
In addition to risk factors, several precipitating factors of delirium have been identified. (See Table 2.) Importantly, elderly patients are at highest risk because they often are subject to several predisposing risk factors and precipitating factors simultaneously.
Table 2. Common Precipitating Factors of Delirium |
|
Clinical Presentation
The complexity of the pathogenesis behind delirium results in a clinical presentation that is varied and sometimes difficult to recognize. Because no diagnostic imaging or laboratory test exists, historical features and physical exam are the basis for clinical diagnosis.
Delirium is marked by a disturbance of consciousness with altered cognitive functioning. In contrast to other neurobehavioral syndromes, delirium typically presents with acute onset and fluctuation of symptoms throughout the day. Delirium typically develops over hours to days, making the temporal nature of symptoms important to evaluate during history taking.
The earliest presentation of delirium will be a change in the level of awareness of a patient. Disturbances in cognition and executive functioning can present on a spectrum from subtle changes to profound deterioration of a patient’s baseline mental status. This poses a unique challenge to emergency physicians, as patients typically are not well known to them from previous clinical encounters.
Cognitive difficulties, such as disorientation and memory loss, often are evident when examining mental status. Perceptual changes, such as hallucinations or delusions, can make eliciting pertinent historical features of the syndrome difficult to assess. Although time in the ED is limited, providers may need to employ frequent re-evaluations and assessments of mental status to assess for any dynamic changes.
History taking from patients may be severely limited because of depressed mental status, confusion, or disorganized thought processes. Therefore, collateral information from family, caregivers, or other individuals well known to the patient is incredibly important to understanding the patient’s clinical presentation when delirium is suspected.
Experts typically characterize delirium as having three subtypes: hyperactive, hypoactive, and mixed. Hyperactive delirium is marked by heightened arousal with concomitant agitation, restlessness, and increased motor activity. In contrast, hypoactive delirium is characterized by lethargy, and incoherent and slowed speech, with associated psychomotor slowing. A mixed state delirium combines features of hyperactive and hypoactive delirium.23-25
Differential Diagnosis
Although most frequently seen in the elderly or critically ill, delirium can present in any patient regardless of medical or psychiatric comorbidities. Careful evaluation of history and physical findings can point in the direction of delirium, but physicians should maintain a broad differential of other medical conditions that may present with a similar acute confused state. While beyond the scope of this review, physicians should methodically consider treatable and reversible causes that may have precipitated the delirium with a patient-centered approach.
After consideration of etiologies such as underlying infection, intoxication/withdrawal syndromes, medication adverse effects, and other metabolic derangements, the clinician should consider additional neurocognitive disorders that present similarly to delirium but are distinct entities.
Dementia
Dementia shares many similar features with delirium, and distinguishing the two disorders is of significant clinical importance. Since both diagnoses present with cognitive dysfunction and limited physical exam findings, key elements of the history can help guide the diagnosis. Table 3 compares important findings that can help distinguish delirium from dementia.
It is important for physicians to recognize and be familiar with the different types of dementia syndromes. Cognitive impairments, such as disturbances in memory, along with difficulties in executive functioning hallmark each, which are briefly described below.
Alzheimer’s Disease
Most cases of dementia are caused by Alzheimer’s disease, which typically occurs in adults older than 65 years of age. Insidious changes in memory prevail as the initial clinical manifestation. As the disease progresses, other cognitive disturbances, including impaired executive functioning and neuropsychiatric changes, tend to develop. The disease is progressive, although rates of progression are highly variable. The pathophysiology remains elusive, but prevailing theories involve abnormal protein deposition within the brain.
Vascular Dementia
Damage to the vasculature of the small vessels that supply the brain serves as the antecedent event for vascular dementia. The disease course tends to be step-wise, with a gradual loss of cognitive functioning after continued ischemic damage to the brain. Symptoms typically begin after the first clinically significant stroke and tend to progress gradually thereafter.
Lewy Body Dementia
Classically, this type of dementia is found in patients with Parkinson’s disease and is the result of abnormal deposition of the alpha-synuclein protein in the brain. This dementia syndrome features prominent visual hallucinations in addition to memory impairment.
Table 3. Key Clinical Features of Delirium and Dementia |
||
|
Feature |
Delirium |
Dementia |
|
Temporality of symptoms |
Acute (hours to days) |
Gradual (months to years) |
|
Attention |
Impaired |
Normal (impairment seen in severe cases) |
|
Alertness |
Fluctuates |
Normal |
|
Psychomotor changes* |
Present |
Absent |
|
Orientation |
Impaired |
Impaired |
|
Memory |
Impaired |
Impaired |
|
Perception |
Hallucinations |
Generally intact (impairment seen in severe cases) |
|
* Either a slowing down of thought and a reduction of physical movements, or accelerated thoughts and speech often accompanied by unintentional and purposeless motions Adapted from: Rosen’s Emergency Medicine: Concepts and Clinical Practice26 |
||
Psychiatric Disorders
Psychiatric illness may present similarly to delirium, and historical features can help differentiate the two. Depression can manifest with considerable deficits in attention and concentration that often cause impairment in the daily functioning of affected patients. Additionally, psychotic features associated with mood disorders may mimic the hallucinations seen in delirium. Changes in motor activity can be seen in major depressive disorder, with psychomotor slowing being a common physical manifestation. Although depression may not be diagnosed by emergency physicians frequently, knowledge of the diagnostic criteria for depression is important. (See Table 4.)
Table 4. Criteria for Depression |
|
Five or more of these clinical features occurring most every day over a two-week period:
AND/OR
PLUS
|
Sundowning is a phenomenon that has been described in institutionalized patients or those who have been hospitalized for prolonged periods of time. Patients exhibiting sundowning will have behavioral deterioration similar to delirium in the evening hours that appears to improve during the daytime.27
Diagnostic Strategies
Delirium can be the clinical manifestation of numerous medical conditions, medication effects, or toxic ingestions. The physician must consider the patient’s known medical history and precipitating events leading to the mental status change to determine which diagnostic workup will be appropriate and cost effective.
Laboratory data can be useful in discovering the potential etiology of delirium. The undifferentiated, confused patient who does not have an obvious inciting event may require an extensive workup. Physicians should obtain vital signs and review them for any significant abnormalities that may point to a potential precipitating factor, such as hypoxia or hypoglycemia. Fever and tachycardia, when combined with clinical context, may shift the initial diagnostic focus toward an infectious or toxicological etiology. Physicians should use caution when reviewing the vital signs of elderly and immunocompromised patients, as the signs may be falsely reassuring because of an impaired immune system or polypharmacy.
A complete blood count, comprehensive metabolic profile, and urinalysis generally are included in the initial laboratory investigation. Point-of-care glucose testing can be used to evaluate for derangements in blood glucose control quickly. Collateral information and previous medical records may help guide decisions about obtaining medication levels, urine drug screens, thyroid stimulation hormone, or cortisol levels.
When the initial workup and careful review of past medical history do not yield an identifiable cause for the patient’s change in mental status, diagnostic imaging may provide valuable information. Although a chest X-ray is included routinely in the initial radiologic workup for delirium, advanced neuroimaging should be reserved for cases in which the etiology remains unclear despite an unremarkable broad workup. Most pathology seen on head computed tomography (CT) represents chronic conditions that do not relate directly to the inciting agent for an acute change in mental status.28
Although magnetic resonance imaging (MRI) is costly and resource extensive, it may be reserved for cases in which additional advanced imaging is considered to be of diagnostic benefit. MRI can identify acute stroke or other lesions that are not always identifiable through CT. Although MRI potentially is useful, most findings on MRI do not identify treatable causes for the acute change of mental status seen in the critically ill.29
Although cerebrospinal fluid is not examined routinely in the evaluation for altered mental status, it can provide clinicians with useful information about potential etiologies of the delirious state. In the context of fever and mental status changes, meningitis may serve as the possible inciting event.30
Electroencephalogram (EEG) studies are not routine in the ED, but they can provide additional clues about the cause of mental status changes. Although EEG is neither sensitive nor specific, delirium demonstrates a characteristic EEG pattern of diffuse slowing. Metabolic encephalopathy due to severe liver disease also exhibits EEG findings of diffuse slowing. In contrast, increased fast-wave activity can be seen in alcohol/GABA antagonist withdrawal syndromes. Continuous discharges may represent nonconvulsive status epilepticus.31,32
Cognitive Screening Tools
The delirium triage screen (DTS) is a 20-second assessment designed to rule out delirium rapidly in busy clinical environments such as the ED. With a sensitivity of 98%, this screen serves as a tool to reduce the need for additional, more time-consuming assessments. The DTS is a two-step procedure. First, the patient’s level of consciousness is assessed. If the patient is alert and calm, the second step is asking the patient to spell the word “LUNCH” backward. An alert and calm patient who can spell the word “LUNCH” backward with zero or one error is considered normal, and the DTS is negative (no delirium). Patients with heightened (restlessness, agitation, aggressiveness, or combativeness) or reduced (drowsy, reduced response to physical stimulation or voice) consciousness or who make two or more errors in spelling the word “LUNCH” backward are considered DTS positive, and further assessment is indicated.33
After a positive screening test for delirium, further assessment is needed to aid in diagnosis. The Confusion Assessment Method (CAM) has been shown to have up to a 100% sensitivity and 95% specificity for the diagnosis of delirium. (See Table 5.) The CAM can be administered in less than five minutes and has been shown to be the best instrument to support the diagnosis of delirium. The diagnosis of delirium requires the presence of features 1 and 2 plus either 3 or 4.34,35
Additional tools that have been validated in an ICU setting are available for intubated patients. The CAM-ICU can be used for patients who are not able to verbalize, and it relies on nonverbal cues and observations of the patient.36 One review of multiple bedside tools for the diagnosis of delirium found that the CAM was the most reliable, and that the frequently used Mini-Mental State Exam was the least accurate tool.37
Table 5. Confusion Assessment Method (CAM) |
|
Information obtained from observation or from a family member or caretaker Feature 1 Acute Onset and Fluctuating Course: Is the patient’s current mental state a change from baseline AND has it fluctuated in intensity over the past 24 hours? Feature 2 Inattention: Does the patient have difficulty following conversation or are they easily distracted? Feature 3 Disorganized Thinking: Is the patient’s conversation disorganized, incoherent, rambling, or illogical? Feature 4 Altered Level of Consciousness: Is the patient’s level of consciousness something other than alert and calm (such as hypervigilant or lethargic)? |
Management
As with most ED encounters, evaluation of presenting vital signs with prompt attention to the ABCs (airway, breathing, and circulation) of the patient will allow for quick assessment of the need for critical interventions, such as securing an airway through orotracheal intubation.
Initial management plans for a patient who presents with an acute change in mental status include establishing a safe environment for both the patient and staff. Because patients may present as uncooperative and agitated, methods of verbal de-escalation or redirection may be unsuccessful because of an altered sensorium. Consideration should be given to the least restrictive restraint method possible while also ensuring safe and prompt medical evaluation of the acutely altered patient.
The ultimate goal in the management of delirium is to identify and appropriately manage any treatable or reversible causes for delirium. Supplemental oxygen, antidote administration, and antibiotic therapy are examples of interventions the emergency physician may use to manage delirium in the appropriate clinical context.
Unfortunately, despite a broad workup inclusive of laboratory data and diagnostic imaging, the etiology of the confusional state might not be elucidated in the ED. These patients will require continued hospitalization and observation in the inpatient setting.
Until the underlying medical condition can be recognized and treated, patients with delirium ultimately may require medication for symptom control. Initial attempts to control agitation should involve nonpharmacologic interventions and the focus should be placed on verbal redirection. Attempts should be made to re-orient the patient, provide a calm and quiet setting, and ensure a safe environment with bed rails and professional sitters.
When initial supportive interventions fail, escalation to medication therapy should be considered. Medication classes frequently used in the management of agitation associated with delirium include neuroleptic agents and benzodiazepines.
Neuroleptic Agents
Neuroleptic antipsychotic medications are used in the management of severe agitation; however, there are limited data to support their use.38,39 This class of medications frequently is used largely because there are limited alternative agents that have shown efficacy. Haloperidol remains the most frequently used antipsychotic; however, recent studies have demonstrated similar efficacy with the newer atypical antipsychotics (e.g., quetiapine, risperidone, or olanzapine).40-42 Caution should be exercised when administering haloperidol in patients with underlying coronary artery disease or with prolonged QTc intervals, as this medication may induce dysrhythmias. Neuroleptics are the preferred agents if chemical restraint is required for patients with delirium.
Benzodiazepines
Benzodiazepines (e.g., lorazepam or midazolam) offer a more rapid onset than antipsychotics through GABA antagonism in the central nervous system. Although they are readily available and are a familiar medication class to emergency physicians, benzodiazepines have been demonstrated to worsen confusion and sedation and, thus, should be avoided in most patients with delirium.43 When treating delirium thought to be caused by alcohol or sedative withdrawal, benzodiazepines are preferred to neuroleptic agents.
Disposition
The overwhelming majority of patients presenting to the ED with delirium will require admission to the hospital for continued symptom control while performing evaluation and treatment of underlying conditions. Escalating care to an intensive care setting may be required for severe cases of delirium, although no strict admission criteria exist.
Physicians should use clinical judgment on a case-by-case basis to determine if discharging a patient will be safe after the mental status change has been reversed. Typically, young, otherwise healthy patients with drug-induced delirium may be suitable candidates for discharge after the altered sensorium has dissipated and clinical sobriety is assessed.
Outcomes
The elderly, who represent most patients presenting with delirium, tend to have a poor prognosis, with persistent decline in neurobehavioral functioning. Delirium in the elderly has been associated with prolonged hospital stays, an elevated long-term mortality risk, and loss of activities of daily living.44,45
Elements of delirium, including cognitive dysfunction, may persist in the elderly long after the initial confusion resolves. Research has demonstrated that patients admitted to the intensive care setting with delirium had follow-up deficits at one year similar to patients with moderate traumatic brain injury.46
Summary
Delirium is a complex disorder marked by the acute onset of mental status change with an associated fluctuating course. Despite the fact that delirium is a common clinical entity in elderly hospitalized patients, the condition may present in any patient regardless of medical comorbidities. Recognition within the emergency setting is becoming increasingly important, as the diagnosis frequently is missed. The interplay between predisposing risk factors and precipitating events can lead to the delirious state, which is marked by inattentiveness, impaired concentration, and significant confusion. Although the exact mechanism is unknown, several theories point to alterations in neuronal functioning as a likely mechanism.
Emergency physicians must maintain a broad differential when considering the etiology of acute change in mental status. Historical features and collateral information will help guide the diagnostic workup for the underlying cause of delirium. Management of symptoms in the ED begins with supportive measures but pharmacotherapy may be required to control agitation and ensure a safe environment. Neuroleptic agents, including the newer atypical antipsychotics, generally are regarded as first-line management for undifferentiated delirium.
Although delirium classically is regarded as a reversible entity, it carries significant morbidity and mortality. Long-term outcomes, particularly in elderly patients with delirium, include significant cognitive decline with associated impairments in daily functioning. Although not demonstrated to reliably prevent delirium, preventive measures include interventions targeted toward decreasing exposure to modifiable risk factors.47
REFERENCES
- Elie M, Rousseau F, Cole M, et al. Prevalence and detection of delirium in elderly emergency department patients. CMAJ 2000;163:977-981.
- Hustey FM, Meldon SW. The prevalence and documentation of impaired mental status in elderly emergency department patients. Ann Emerg Med 2002;39:248-253.
- American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, 5th Edition. Washington, DC: American Psychiatric Publishing; 2013.
- Barron EA, Holmes J. Delirium within the emergency care setting, occurrence and detection: A systematic review. Emerg Med J 2013;30:263-268.
- Siddiqi N, House AO, Holmes JD. Occurrence and outcome of delirium in medical in-patients: A systematic literature review. Age Ageing 2006;35:350-364.
- Leslie DL, Marcantonio ER, Zhang Y, et al. One-year health care costs associated with delirium in the elderly population. Arch Intern Med 2008;168:27-32.
- Hustey FM, Meldon SW, Smith MD, Lex CK. The effect of mental status screening on the care of elderly emergency department patients. Ann Emerg Med 2003;41:678-684.
- Han JH, Zimmerman EE, Cutler N, et al. Delirium in older emergency department patients: Recognition, risk factors, and psychomotor subtypes. Acad Emerg Med 2009;16:193-200.
- Inouye SK, Rushing JT, Foreman MD, et al. Does delirium contribute to poor hospital outcomes? A three-site epidemiologic study. J Gen Intern Med 1998;13:234.
- McNicoll L, Pisani MA, Zhang Y, et al. Delirium in the intensive care unit: Occurrence and clinical course in older patients. J Am Geriatr Soc 2003;51:591.
- Lawlor PG, Gagnon B, Mancini IL, et al. Occurrence, causes, and outcome of delirium in patients with advanced cancer: A prospective study. Arch Intern Med 2000;160:786.
- Kiely DK, Bergmann MA, Murphy KM, et al. Delirium among newly admitted postacute facility patients: Prevalence, symptoms, and severity. J Gerontol A Biol Sci Med Sci 2003;58:M441.
- Inouye SK, Charpentier PA. Precipitating factors for delirium in hospitalized elderly persons. Predictive model and interrelationship with baseline vulnerability. JAMA 1996;275:852-857.
- Inouye SK. Delirium in older persons. N Engl J Med 2006;354:1157-1165.
- Maldonado JR. Delirium pathophysiology: An updated hypothesis of the etiology of acute brain failure. Int J Geriatr Psychiatry 2018;33:1428-1457.
- Pendlebury ST, Lovett NG, Smith SC, et al. Observational, longitudinal study of delirium in consecutive unselected acute medical admissions: Age-specific rates and associated factors, mortality and re-admission. BMJ Open 2015;5:e007808.
- Umesh SR, Chacko ST, Lucas A, Sundararaj A. Delirium and its risk factors among elderly patients. International Journal of Science and Research (IJSR) 2017;6:458-461.
- Cerejeira J, Firmino H, Vaz-Serra A, Mukaetova-Ladinska EB. The neuroinflammatory hypothesis of delirium. Acta Neuropathol 2010;119:737-754.
- White S. The neuropathogenesis of delirium. Rev Clin Gerontol 2002;12:62-67.
- Cerejeira J, Batista P, Nogueira V, et al. Low preoperative plasma cholinesterase activity as a risk marker of postoperative delirium in elderly patients. Age Ageing 2011;40:621-626.
- Trzepacz PT. The neuropathogenesis of delirium. A need to focus our research. Psychosomatics 1994;35:374.
- Fick DM, Agostini JV, Inouye SK. Delirium superimposed on dementia: A systematic review. J Am Geriatr Soc 2002;50:1723.
- Potter J, George J; Guideline Development Group. The prevention, diagnosis and management of delirium in older people: Concise guidelines. Clin Med 2006;6:303-308.
- Gupta N, de Jonghe J, Schieveld J, et al. Delirium phenomenology: What can we learn from the symptoms of delirium? J Psychosom Res 2008;65:215-222.
- Meagher DJ, Leonard M, Donnelly S, et al. A longitudinal study of motor subtypes in delirium: Frequency and stability during episodes. J Psychosom Res 2012;72:236-241.
- Marx JA, Rosen P. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 8th ed. Philadelphia: Elsevier/Saunders; 2006.
- Bliwise DL. What is sundowning? J Am Geriatr Soc 1994;42:1009.
- Koponen H, Hurri L, Stenbäck U, et al. Computed tomography findings in delirium. J Nerv Ment Dis 1989;177:226.
- Morandi A, Gunther ML, Vasilevskis EE, et al. Neuroimaging in delirious intensive care unit patients: A preliminary case series report. Psychiatry (Edgmont) 2010;7:28.
- Marcantonio ER. In the clinic. Delirium. Ann Intern Med 2011;154:ITC6-15.
- Jacobson S, Jerrier H. EEG in delirium. Semin Clin Neuropsychiatry 2000;5:86-92.
- Jenssen S. Electroencephalogram in the dementia workup. Am J Alzheimers Dis Other Demen 2005;20:159-166.
- Han JH, Wilson A, Vasilevskis EE, et al. Diagnosing delirium in older emergency department patients: Validity and reliability of the delirium triage screen and the brief confusion assessment method. Ann Emerg Med 2013;62:457-465.
- Inouye SK, van Dyck CH, Alessi CA, et al. Clarifying confusion: The confusion assessment method. A new method for detection of delirium. Ann Intern Med 1990;113:941-947.
- Wei LA, Fearing MA, Sternberg EJ, Inouye SK. The Confusion Assessment Method: A systematic review of current usage. J Am Geriatr Soc 2008;56:823-830.
- Ely EW, Inouye SK, Bernard GR, et al. Delirium in mechanically ventilated patients: Validity and reliability of the confusion assessment method for the intensive care unit (CAM-ICU). JAMA 2001;286:2703-2710.
- Wong CL, Holroyd-Leduc J, Simel DL, Straus SE. Does this patient have delirium?: Value of bedside instruments. JAMA 2010;304:779-786.
- Flaherty JH, Gonzales JP, Dong B. Antipsychotics in the treatment of delirium in older hospitalized adults: A systematic review. J Am Geriatr Soc 2011;59 Suppl 2:S269.
- Girard TD, Pandharipande PP, Carson SS, et al; MIND Trial Investigators. Feasibility, efficacy, and safety of antipsychotics for intensive care unit delirium: The MIND randomized, placebo-controlled trial. Crit Care Med 2010;38:428-437.
- Gilchrist NA, Asoh I, Greenberg B. Atypical antipsychotics for the treatment of ICU delirium. J Intensive Care Med 2012;27:354.
- Skrobik YK, Bergeron N, Dumont M, Gottfried SB. Olanzapine vs haloperidol: Treating delirium in a critical care setting. Intensive Care Med 2004;30:444-449.
- Lonergan E, Britton AM, Luxenberg J, Wyller T. Antipsychotics for delirium. Cochrane Database Syst Rev 2007;(2):CD005594.
- Breitbart W, Marotta R, Platt MM, et al. A double-blind trial of haloperidol, chlorpromazine, and lorazepam in the treatment of delirium in hospitalized AIDS patients. Am J Psychiatry 1996;153:231-237.
- Pisani MA, Kong SYJ, Kasl SV, et al. Days of delirium are associated with 1-year mortality in an older intensive care unit population. Am J Respir Crit Care Med 2009;180:1092-1097.
- Smith J, Seirafi J. Delirium and dementia. In: Marx JA III, Hockberger RS, Walls RM, editors. Rosen’s Emergency Medicine Concepts and Clinical Practice. 7th ed. Philadelphia: Elsevier; 2010:1367-1373.
- Pandharipande PP, Girard TD, Jackson JC, et al. Long-term cognitive impairment after critical illness. N Engl J Med 2013;369:1306-1316.
- Clegg A, Siddiqi N, Heaven A, et al. Interventions for preventing delirium in older people in institutional long-term care. Cochrane Database Syst Rev 2014;(1):CD009537.
Delirium is a complex disorder marked by the acute onset of mental status change with an associated fluctuating course. Despite the fact that delirium is a common clinical entity in elderly hospitalized patients, the condition may present in any patient regardless of medical comorbidities. Recognition within the emergency setting is becoming increasingly important, as the diagnosis frequently is missed.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
