Is There RBBB, Acute Ischemia, or Both?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below was obtained from a 35-year-old man with a 20-year history of smoking. He presented to the ED with new-onset chest discomfort. He was hemodynamically stable at the time this tracing was obtained. How would one interpret his ECG? Is there right bundle branch block (RBBB)? Is there evidence of acute posterior ischemia or infarction?
There is a regular sinus rhythm at ~90 beats/minute. At first glance, the PR interval looks normal and the QRS looks wide with a pattern in lead V1 that suggests RBBB. That said, this is not RBBB. Delta waves with a short PR interval are visible in several leads, most notably in leads V2, V3, and V4. Instead of RBBB, this patient has Wolff-Parkinson-White (WPW) syndrome.
Once one realizes this patient has WPW, it becomes clear that the negative initial deflection in lead III is not a Q wave but rather a negative delta wave. Other examples of “retrospective recognition” of delta waves on this tracing are visible in leads II, aVL, and aVF. Thus, the suggestion of a tiny “extra little bump” on the baseline in leads II and aVF probably represents subtle delta waves that are almost entirely isoelectric.
The other remarkable finding on this tracing is the marked ST segment depression in leads V2-V5. Most of the time, one cannot appreciate ischemia or acute infarction in a patient with WPW. That said, on occasion ST-T wave changes may be so marked as to suggest acute disease, necessitating cardiac catheterization to define the anatomy. This was the situation in this case. Suffice it to say that the cardiologist also was uncertain as to whether the ST segment depression in multiple chest leads was a marker of acute ischemia or simply an accompaniment of this patient’s WPW. As a result, prompt cardiac catheterization was performed. It turned out that the coronary arteries were free of significant disease.
For more information about and further discussion on this case, please visit: https://bit.ly/2FR4LbS.
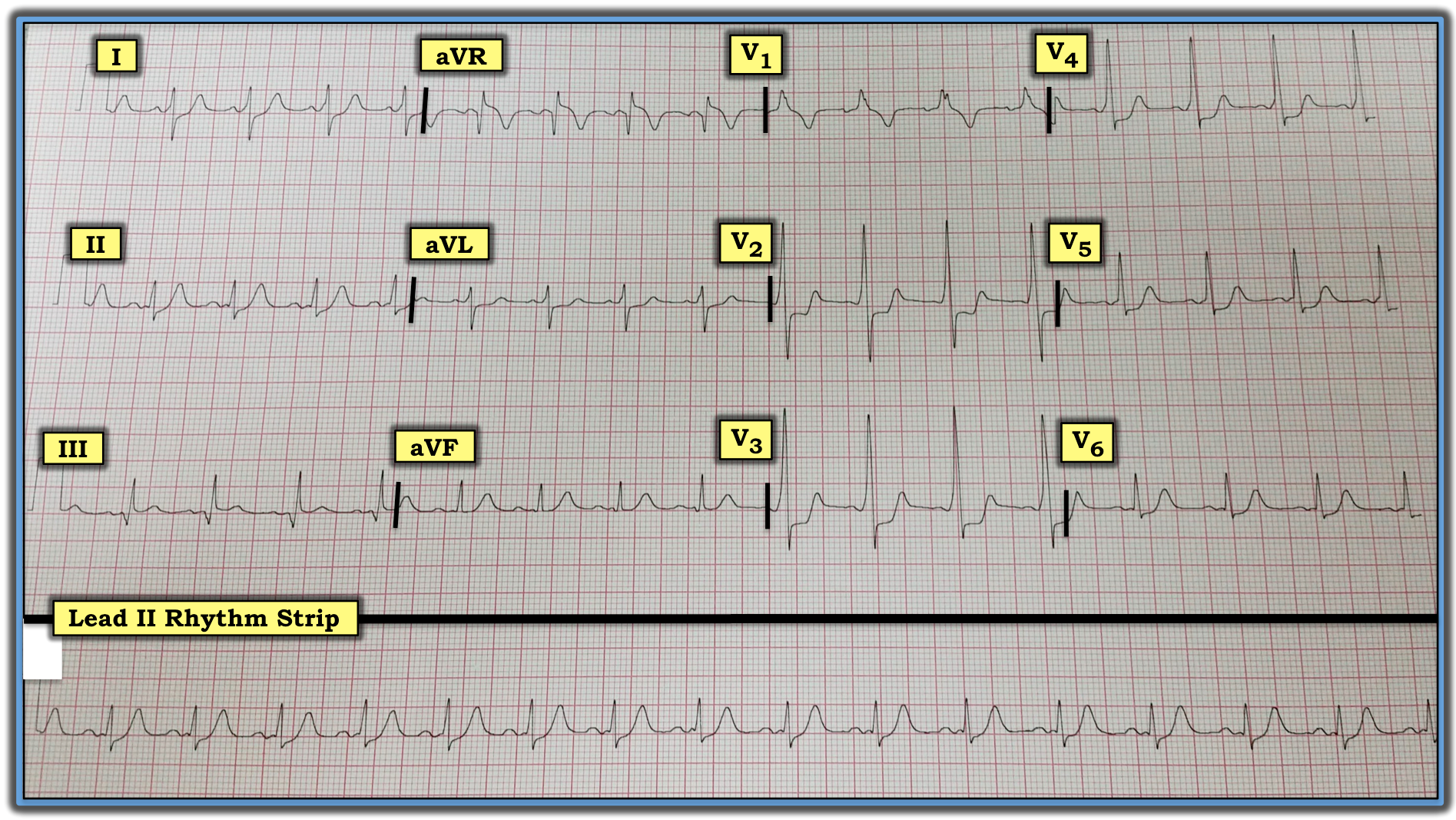
The ECG in the figure was obtained from a 35-year-old man with a 20-year history of smoking. He presented to the ED with new-onset chest discomfort. He was hemodynamically stable at the time this tracing was obtained. How would one interpret his ECG? Is there right bundle branch block (RBBB)? Is there evidence of acute posterior ischemia or infarction?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
