Are the Changes Acute?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Imagine the ECG in the figure below was obtained from a previously healthy, middle-aged man who presented to an ambulatory clinic for “indigestion.” How might one interpret this ECG? Are there acute changes?
The rhythm is sinus at a rate of ~70 beats/minute. All intervals and the mean QRS axis are normal. There is no chamber enlargement. A large Q wave is seen in lead III and small Q waves are present in leads II and aVF. Transition is normal (occurs between V3 to V4). There is coved ST elevation in leads III and aVF, with a hint of early T-wave inversion in these leads. There also appears to be slight-but-real ST elevation in lead II. ST depression is seen in lead I (slightly), in lead aVL (more definite), and probably also in lead V2. The T wave is relatively flat in leads V5 and V6 (normally, the T wave is clearly upright in these lateral chest leads). The combination of these findings suggests we should assume inferior myocardial infarction (MI) has occurred at some point, probably in the recent past (at least until proven otherwise). The challenge is to determine the relative age of this MI, since treatment recommendations will vary dramatically depending on the answer.
ECG findings suggesting a more acute MI: There is ST elevation in each of the inferior leads; there is reciprocal ST depression in lead aVL, best appreciated by the fact that ST-T wave appearance in lead aVL is the mirror image picture of the ST-T wave in lead III.
ECG findings suggesting a less acute picture: The amount of ST elevation is relatively modest, a huge Q wave has formed already in lead III, the amount of reciprocal ST depression is extremely modest, and the patient presented to an ambulatory clinic instead an ED. Further, there is no specific history for acute-onset chest pain. Although patients with acute MI certainly can present to an ambulatory clinic, there seems to be a “self-selection” process, whereby statistical likelihood of an acute event appears to be greatly enhanced when patients call 911 and present with their symptoms to the ED instead of to an outpatient clinic. Pending additional historical information, the overall picture suggests a less acute onset for this MI. Whether this dates this infarct to 12 to 24 hours ago (or even longer ago than that) is uncertain from the information available.
For more information about and further discussion on this case, please visit: https://bit.ly/2S31iZW.
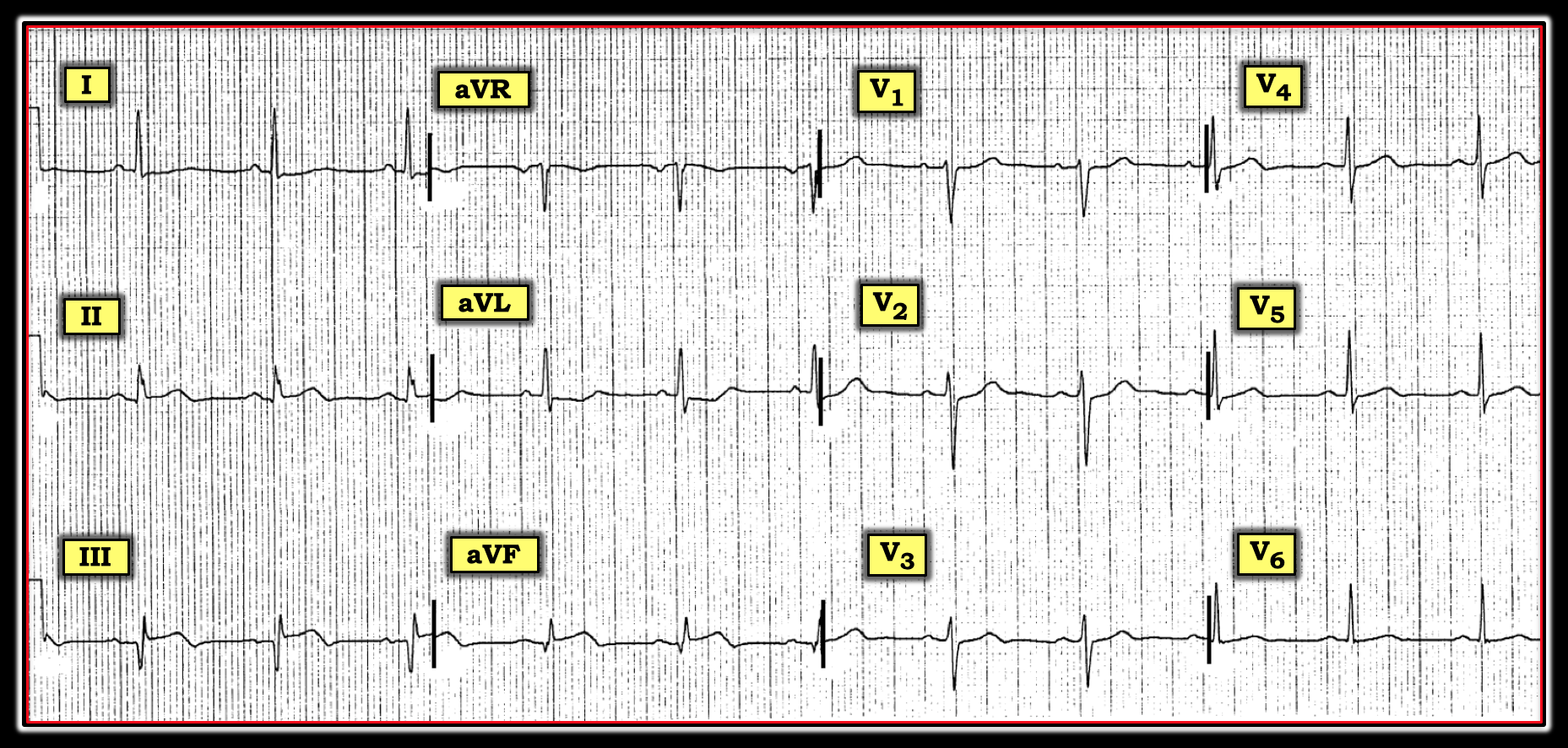
Imagine the ECG in the figure was obtained from a previously healthy, middle-aged man who presented to an ambulatory clinic for “indigestion.” How might one interpret the ECG?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
