Is There AV Block?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The long lead II rhythm strip in the figure below was recorded at the standard 25 mm/second speed. This tracing was obtained from a middle-aged woman who presented to an outpatient clinic with noncardiac chest pain. How would one interpret this rhythm? Are there signs of AV block? Is it apparent if there is a cardiac problem?
The QRS complex is narrow in this single monitoring lead. The rhythm appears to be supraventricular. The rhythm is almost (but not completely) regular. P waves are present, but the PR interval does not remain constant throughout the tracing. When confronted with a difficult-to-interpret arrhythmia, it may be easiest to start with what one knows. In this case, the PR interval preceding beat 3 is too short to conduct. The PR interval preceding beats 2 and 6 also appears to be too short to conduct.
Is there an underlying sinus rhythm? Note that the PR interval preceding all other beats on this tracing (i.e., the PR interval before beats 1, 4-5, and 7-9) is longer than the PR interval preceding beats 2, 3, and 6.
Since the PR interval is equal and normal (~0.14/second) preceding beats 1, 4-5, and 7-9, and since P waves all are upright in this lead II monitoring strip, the underlying rhythm is sinus arrhythmia, with an overall ventricular rate less than 50 beats/minute.
Because the three beats that are preceded by a PR interval too short to conduct all feature a narrow QRS complex, and all look similar in morphology to the six sinus-conducted beats on this tracing, these three beats (i.e., beats 2, 3, and 6) must be junctional escape beats. Although the R-R interval varies slightly during this rhythm strip, the R-R interval preceding each of these three junctional beats is identical (6.6 large boxes in duration). This corresponds to a junctional escape rate of ~45 beats/minute.
The underlying rhythm is sinus bradycardia and arrhythmia. When the SA node slows to a rate below 45 beats/minute, the junctional escape rhythm takes over. When this happens, there is transient AV dissociation until the sinus rate speeds up to more than 45 beats/minute. A helpful clue that P waves are conducting again is when the R-R interval shortens. Thus, beats 4 and 5 are sinus-conducted beats. After junctional beat 6, the R-R interval again shortens, with resumption of sinus-conducted P waves for beats 7, 8, and 9.
There is no evidence of AV block on this tracing. There never are P waves that fail to conduct when given a chance to do so (i.e., the P waves just before beats 2, 3, and 6 never have a chance to conduct because the PR interval is just too short). Clinically, without more information (and a longer period of monitoring), there is no way to know whether the rhythm in the figure is pathologic. This could be a normal physiologic response if the patient was a healthy, endurance athlete with a baseline rhythm of sinus bradycardia. On the other hand, it could be a pathologic rhythm if this patient had sick sinus syndrome.
For more information about and further discussion on this case, please visit: https://bit.ly/2Joo2Vs.
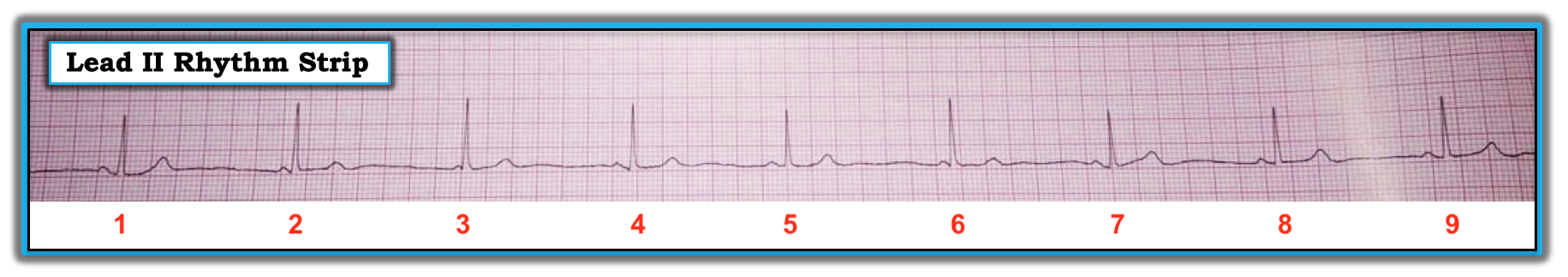
The long lead II rhythm strip in the figure was recorded at the standard 25 mm/second speed. This tracing was obtained from a middle-aged woman who presented to an outpatient clinic with noncardiac chest pain. How would one interpret this rhythm? Are there signs of AV block? Is it apparent if there is a cardiac problem?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
