Can You Predict the Anatomy?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below was recorded from an elderly woman with new-onset chest pain. How would one assess this ECG? Is there a “culprit” artery?
Because this ECG was recorded in the ambulance on the way to the hospital, there is significant baseline artifact, which is most notable in the inferior leads. Despite this artifact, it is still possible to interpret this ECG. The rhythm is sinus at a rate between 70 beats/minute and 75 beats/minute. The three intervals (the PR interval, QRS duration, and the QTc) are normal. The frontal plane axis is ~ +40 degrees.
Regarding QRST changes: Q waves are absent; R wave progression in the chest leads is normal, with transition occurring between lead V3 to V4; the lateral chest leads (V4, V5, and V6) manifest 1-2 mm of J-point ST elevation. Although difficult to ascertain because of the artifact, T waves in the three inferior leads (leads II, III, aVF) look larger, wider at their base, and appear to be more peaked than they should be. These are hyperacute T waves. Although subtle, there is some ST-T wave depression in lead aVL and also in leads V1 and V2.
In view of the history of new-onset chest pain in this elderly woman, this ECG strongly suggests acute lateral ST-segment elevation myocardial infarction (STEMI). The ST-T wave depression in leads V1 and V2 makes posterior involvement likely. The hyperacute inferior lead T wave changes suggest inferior wall involvement.
Most acute inferior MIs result from acute occlusion of the right coronary artery (RCA). That said, this patient is much more likely to represent the 10-15% of patients with acute inferior STEMI for whom the “culprit” artery is the left circumflex artery (LCx). This is because the relative amount of ST-segment elevation is higher in the lateral chest leads (V4, V5, and V6) than in the inferior leads. When the RCA is not the dominant vessel, the LCx tends to supply the lateral, posterior, and inferior walls of the left ventricle. This corresponds exactly to the areas of the heart that manifest acute changes in this ECG.
Acute occlusion of the RCA results most commonly in: ST-segment elevation in lead III > lead II; marked reciprocal ST-segment depression in lead aVL that looks like the mirror image of the ST elevation in lead III; ECG evidence that suggests acute RV involvement, such as less ST depression in right-sided lead V1 compared to lead V2 (or even slight ST-segment elevation in lead V1); and not as much ST-segment elevation in lead V6 vs. lead III. None of these features are seen in this case.
Although the relative amount of ST-segment deviation in any given lead in this ECG is modest, it is the composite picture of ST-T wave changes in almost every lead of this ECG that makes the diagnosis of acute LCx occlusion with resultant infero-postero-lateral STEMI in this patient with new-onset chest pain. For optimal treatment, perform cardiac catheterization as soon as possible, with the goal of reperfusion therapy. Repeat ECG within the next half hour should further clarify the clinical picture.
For more information about and further discussion on this case, please visit: http://bit.ly/2Zheqjh.
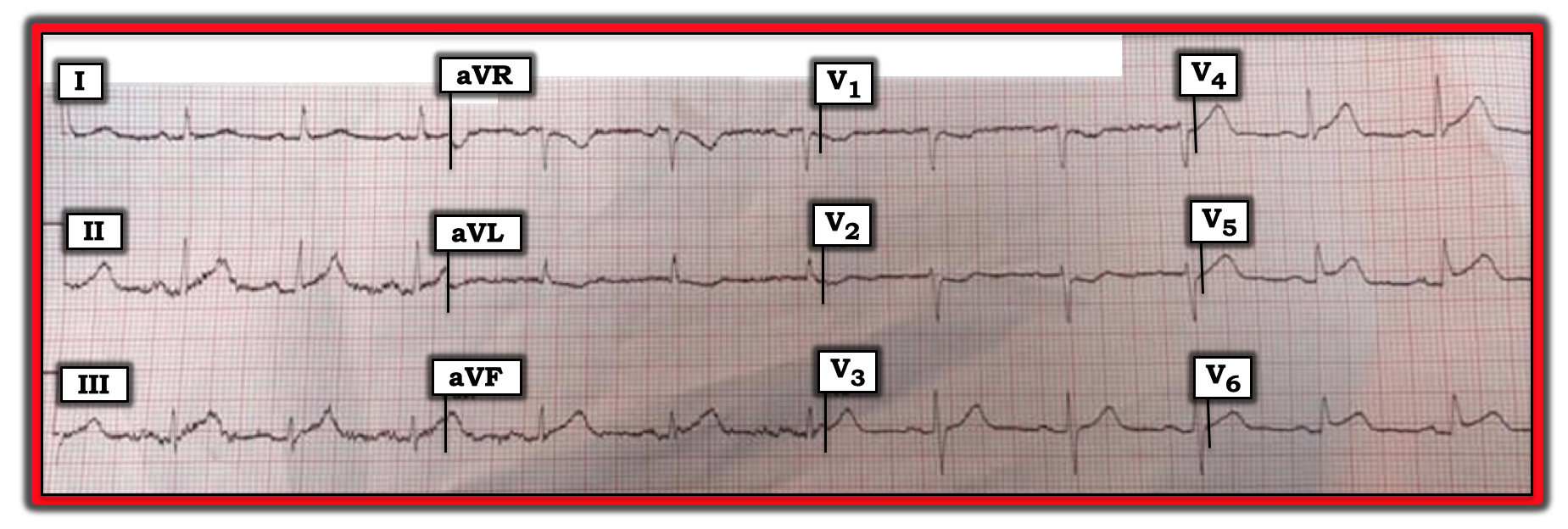
The ECG in the figure was recorded from an elderly woman with new-onset chest pain. How would one assess this ECG? Is there a “culprit” artery?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
