Sleep Tight, and Don’t Let the Ectoparasites Bite: Part 2
June 1, 2019
Reprints
AUTHOR
Trahern W. (TW) Jones, MD, Fellow, Division of Pediatric Infectious Diseases, Adjunct Instructor, Department of Pediatrics, University of Utah Health, Salt Lake City
PEER REVIEWER
Sandra L. Werner, MD, FACEP, Medical Staff President, MetroHealth Medical Center; Clinical Operations Director, Department of Emergency Medicine; Associate Program Director, Emergency Medicine Residency Program; Associate Professor, Case Western Reserve University, Cleveland
Executive Summary
- Bedbug infestations peak seasonally, with activity in the late summer and early fall. Although classically attributed to poor hygiene, unwashed sheets, and dilapidated housing, infestations may occur in almost any setting, ranging from family homes to apartments, dormitories, schools, hospitals, outpatient clinics, nursing homes, office buildings, theaters, retail stores, and public transportation.
- Patients with bedbug bites may note the presence of itchy or painful erythematous macules, papules, or welts. Several lesions may develop in a closely spaced linear arrangement, the so-called “breakfast, lunch, and dinner” sign.
- Typically, treatment for bite lesions is symptomatic, with the use of topical antiseptic creams to prevent infection, and topical corticosteroids and oral antihistamines to reduce itching and inflammation.
- Exposing bedbugs to temperatures > 113° F (> 45° C) for at least an hour, or > 140° F (> 60° C) for any length of time, will kill all adults and eggs. This may be accomplished with steaming or laundering.
- Both hard- and soft-bodied ticks progress through larval and nymphal stages before achieving adulthood. However, feeding patterns between species differ. Adult hard-bodied ticks may attach and feed on hosts for as long as one to four weeks, eventually engorging themselves with a substantial blood meal and dropping off the host. Soft-bodied ticks more typically inhabit mammalian burrows and nests, emerging at regular intervals to feed on their hosts for short periods.
- Patients may present with the tick still attached and feeding from the skin. However, the bite itself is painless, and patients usually discover the attached arthropod incidentally or by checking themselves after walking through an endemic area.
- Tick paralysis is caused by a neurotoxic salivary component released in some hosts during feeding. The syndrome typically manifests two to six days after the tick attaches itself to the host. Initially, patients experience irritability and restlessness, followed by paresthesias, ascending flaccid paralysis, ataxia, loss of deep tendon reflexes, eventual cranial nerve palsies, including oculomotor weakness, dysarthria, dysphagia, and, ultimately, respiratory failure and death.
- Erythema migrans frequently is described as the presenting rash of Lyme disease. This skin lesion develops at the site of the tick bite in 70-80% of cases. It begins as a red macule or papule, and spreads outward in the course of days or weeks. It is an expanding, round lesion with central clearing, growing to at least 5 cm, but up to a median 15 cm in size.
- Patients should be advised to remove ticks when they are spotted on their person. This always should be performed as soon as possible, since ticks are more likely to transmit vector-borne disease the longer they are attached.
- Patients or providers should use a pair of forceps or tweezers to grasp the tick firmly where the head is attached to the skin, and pull directly outward with gentle, steady axial traction.
Providers in the pediatric emergency department frequently encounter ectoparasitic infestations. Infestations require early recognition and knowledge of effective treatment strategies. Last month, the author reviewed scabies, chiggers, and lice. This month, the bedbugs and ticks will come biting!
— Ann M. Dietrich, MD, FAAP, FACEP, Editor
Introduction
As discussed last month, ectoparasites constitute parasitic infectious agents characterized by their size and host habitat. All medically significant ectoparasites are arthropods that reproduce and feed at the level of the epidermal or dermal strata in the skin, or on closely related structures, such as the hair, sebaceous glands, and external orifices like the ears, nares, and orbits.1
Part 1 of this review covered such ectoparasites as lice and scabies. Part 2 part will focus on bedbugs and ticks.
Bedbugs
Description and Epidemiology
Bedbugs, or Cimicidae, are 5 mm to 7 mm in length, with an oval, flattened shape dorsoventrally.2 (See Figure 1.) Their coloration may range from pale yellow to dark brown, depending on how recently they have consumed a blood meal.
Figure 1. Bedbug |
 |
|
Source: Getty Images |
The family Cimicidae includes two relevant species of bedbugs that feed on human hosts: Cimex lectularius, which is distributed globally, and Cimex hemipterus, which is largely restricted to the tropics.2 Between the two species, bedbugs enjoy a global distribution, and their prevalence may be increasing overall. After a drop in infestation rates throughout the 20th century, the United States has experienced a major resurgence in reported bedbug complaints from local health departments.3 This is believed to be due to new mechanisms of insecticide resistance among bedbugs.4 In a 2018 survey of U.S. and international pest control companies, more than 97% reported managing a bedbug infestation in the past year, and rates of infestation appeared to be increasing.5
Seasonal peaks in infestations and activity may occur in the late summer and early fall.5,6 Although classically attributed to poor hygiene, unwashed sheets, and dilapidated housing, infestations may occur in almost any setting, ranging from family homes to apartments, dormitories, schools, hospitals, outpatient clinics, nursing homes, office buildings, theaters, retail stores, and public transportation.3,5
Life Cycle and Pathophysiology
Bedbugs feed on human hosts with an often painless bite, usually at night. Because of this, victims may be unaware of the burden of infestation, simply presenting instead with a dermatitis of unknown origin.2
Female bedbugs may lay two to three eggs per day along cracks and crevices in walls and furniture.2 After eight to 11 days, these eggs hatch into nymphal forms, which require regular blood meals and warm temperatures to mature. This may require anywhere from two to seven weeks, depending on whether hosts are easily available. Between stages of growth, these nymphs may shed their skin, which can be found along cracks and crevices in households with active infestations.
Bedbug infestations generally are apparent by visualizing adults, eggs, nymphal skins, or excreta, which consists of dark brown marks or smears along crevices in walls and furniture or among bedsheets.2 Houses with severe infestations may take on a sickly sweet smell.
Transmission occurs primarily through the direct spread of adults, nymphs, or eggs from infested bedding, furniture, or even clothing and personal items, such as handbags.2 Purchases of secondhand furniture can lead to transmission of bedbugs from different households. Adults may survive more than a year without a blood meal, thus aiding their portability between habitations.
Clinical Manifestations and Diagnosis
To take a blood meal from human hosts, bedbugs inject victims with their saliva, which has an anticoagulating effect.2 These salivary components may cause later irritation, leading to a variety of dermatologic manifestations.7 Most often, patients may note the presence of itchy or painful erythematous macules, papules, or welts. Several lesions may develop in a closely spaced linear arrangement, the so-called “breakfast, lunch, and dinner” sign.8 (See Figure 2.) Bites typically occur on exposed parts of the skin. Because of the variability in inflammatory response, individuals who sleep in the same bed may not have the same dermatologic manifestations, or even may be asymptomatic.
Figure 2. Bedbug "Breakfast, Lunch, Dinner" Sign |
 |
|
Source: Getty Images |
Bites may become superinfected, particularly with scratching. Some have noted that patients who have endured bedbug infestations may experience severe emotional or psychological symptoms from their experience.9,10 In massive infestations, patients have been reported to develop anemia from an overwhelming bite burden, particularly among infants or disabled patients in neglectful circumstances, or adults with substance abuse problems.11-13
Bedbugs never have been demonstrated to transmit human pathogens between individuals or households.14,15 However, methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant enterococcus (VRE) have been found to colonize bedbugs from impoverished communities,16 suggesting their capacity as vectors is still incompletely understood.
Treatment
Treatment for bite lesions typically is symptomatic, with the use of topical antiseptic creams to prevent infection, and topical corticosteroids and oral antihistamines to reduce itching and inflammation.17,18 However, more worrisome is addressing control and elimination of bedbugs from the environment. Because of the propensity of bedbugs to hide in cracks and crevices and the nonspecific nature of bite reactions, infestations may become quite severe before the inhabitants become aware of their presence. Detection of infestations can require expertise, and technologies under development include pheromone-sensing systems, and bug-sniffing canines have been used to assist elimination efforts.19
First, homes should be cleaned thoroughly and decluttered, and furniture should be scrubbed and vacuumed to remove the pests and their eggs.20 Over-the-counter insecticides may be used, but professional services most likely will be needed because of resistance rates and the difficulty of thorough spraying, since insecticidal smoke generators may be needed to fumigate the premises.2,7 The expense of professional services can be a point of contention between renters and landlords, and physicians may be asked to document the suspicion of bedbug infestation to aid tenants in this conflict. Starving bedbugs by keeping infested rooms vacant is not a viable solution, as they may survive for nearly a year without a human blood meal.21
In all situations, infant bedding should not be sprayed with insecticides, but rather should be treated with high heat or steam. High heat is a practicable solution to decontaminaeclothing and bedding. Exposing bedbugs to temperatures > 113° F (> 45° C) for at least an hour, or > 140° F (> 60° C) for any length of time, will kill all adults and eggs.21 This may be accomplished with steaming or laundering.
For hospitalized patients or those presenting in the emergency department with known or suspected bedbug infestations at home, infection control services always should be contacted for assistance in activating isolation and preventing transmission to bedding and furniture in patient rooms. The direct and indirect costs of decontamination of clinical areas can pose a significant burden on operational expenditures.22 Emergency departments, clinics, and inpatient units should collaborate with hospital infection control to devise appropriate protocols for their clinical areas in the eventuality that bedbugs are discovered in furniture or on patient clothing.23
Ticks
Description and Epidemiology
As arachnids, ticks are classified alongside mites in the subclass Acari.2 Ticks then are divided further into two separate families of medical significance, the hard-bodied (Ixodidae) and soft-bodied (Argasidae) ticks, differentiated by the presence or absence of a sclerotized plate (scutum) that covers the dorsal aspect of the body. (See Figures 3 and 4.)
Figure 3. Hard-Bodied Tick |
|
Adult tick of genus Ixodes scapularis on blade of grass |
 |
|
Source: Getty Images |
Figure 4. Soft-Bodied Tick |
|
Ornithodoros kelleyi |
 |
|
Source: Jim Gathany, CDC Public Health Image Library. |
In the United States, certain species of hard-bodied ticks predominate in terms of medical significance, although both families may serve as vectors for a variety of infectious agents. Of these, Ixodes ticks, such as the Blacklegged tick, may harbor and transmit Lyme disease, anaplasmosis, and babesiosis; Dermacentor species, such as the American dog tick, the Rocky Mountain wood tick, and the brown dog tick, may carry Rocky Mountain spotted fever, tularemia, ehrlichiosis, and Colorado tick fever; and Amblyomma species, such as the Lone Star tick, also may carry tularemia and ehrlichiosis.24,25 Any of these taxons also may cause tick paralysis. Of the soft-bodied ticks, Ornithodoros may transmit certain borrelial relapsing fevers. (See Table 1.)
Table 1. Tickborne Diseases, Symptoms, Tick Vectors, and Typical Range Within the United States |
|||
Disease |
Hallmark Symptoms, Signs, and Findings |
Known Vectors |
Range |
|
Anaplasmosis |
Fever, chills, rigors, severe headache, malaise, myalgias, anemia, thrombocytopenia, leukopenia, elevations in hepatic transaminases |
Blacklegged tick (Ixodes scapularis), Western blacklegged tick (Ixodes pacificus) |
Upper Midwest and Northeastern United States |
|
Babesiosis |
Fever, chills, sweats, headache, malaise, myalgias, arthralgias, hemolytic anemia, elevated creatinine and BUN, splenomegaly or hepatomegaly, leukopenia, elevations in hepatic transaminases |
Blacklegged tick (Ixodes scapularis) |
Northeastern and Upper Midwestern United States |
|
Ehrlichiosis |
Fever, chills, rigors, severe headache, malaise, myalgias, anemia, thrombocytopenia, leukopenia, elevations in hepatic transaminases |
Blacklegged tick (Ixodes scapularis), Lone Star tick (Amblyomma americanum) |
Southeastern and South-central United States, from the East Coast extending westward to Texas, especially Oklahoma, Missouri, and Arkansas |
|
Colorado Tick Fever |
Fever, chills, rigors, headache, myalgias, lethargy, conjunctival injection, pharyngeal erythema, lymphadenopathy, thrombocytopenia, leukopenia |
Rocky Mountain wood tick (Dermacentor andersoni) |
Western United States, especially Colorado, Utah, Montana, and Wyoming |
|
Heartland Virus Disease |
Fever, fatigue, headache, arthralgias, myalgias, thrombocytopenia, leukopenia, elevations in hepatic transaminases |
Lone Star tick (Amblyomma americanum) |
Midwestern and Southern United States |
|
Powassan Virus Disease |
Fever, headache, weakness, fatigue, meningoencephalitis, seizures, altered mental status, aphasia, paresis |
Groundhog tick (Ixodes cookei) |
Northeastern and Great Lakes regions of United States |
Table 1. Tickborne Diseases, Symptoms, Tick Vectors, and Typical Range Within the United States (continued) |
|||
Disease |
Hallmark Symptoms, Signs, and Findings |
Known Vectors |
Range |
|
Lyme Disease |
Localized stage: erythema migrans, flu-like symptoms, lymphadenopathy Disseminated stage: multiple secondary annular lesions, flu-like symptoms, lymphadenopathy Later manifestations: migratory arthritis, conduction abnormalities, myocarditis, pericarditis, cranial neuropathy (including Bell’s palsy), radiculoneuropathy, meningitis, encephalitis |
Blacklegged tick (Ixodes scapularis), Western blacklegged tick (Ixodes pacificus) |
As of 2015, 95% of cases have been reported from the following states: Connecticut, Delaware, Maine, Maryland, Massachusetts, Minnesota, New Hampshire, New Jersey, New York, Pennsylvania, Rhode Island, Vermont, Virginia, and Wisconsin |
|
Rocky Mountain Spotted Fever |
High fever, severe headache, malaise, myalgia, extremity edema, maculopapular to petechial evolving rash, altered mental status, cerebral edema, multi-organ failure |
American dog tick (Dermacentor variabilis), brown dog tick (Rhipicephalus sanguineus), Rocky Mountain wood tick (Dermacentor andersoni) |
Five states account for more than 60% of cases: North Carolina, Oklahoma, Arkansas, Tennessee, and Missouri, with increasing numbers of cases in Arizona |
|
Tickborne Relapsing Fever |
Febrile episodes lasting ~3 days, separated by afebrile periods lasting ~7 days, headache, myalgias, chills |
Soft-bodied ticks (Ornithodoros spp.) |
Found most commonly in 14 Western states: Arizona, California, Colorado, Idaho, Kansas, Montana, Nevada, New Mexico, Oklahoma, Oregon, Texas, Utah, Washington, and Wyoming |
|
Tularemia |
Fever, chills, headache, malaise, fatigue, myalgias Ulceroglandular: localized lymphadenopathy, cutaneous ulcer at inoculation site Oculoglandular: conjunctivitis; photophobia; tearing; preauricular, submandibular, or cervical lymphadenopathy |
American dog tick (Dermacentor variabilis), Rocky Mountain wood tick (Dermacentor andersoni) |
Cases have been reported in all states except Hawaii, but especially high prevalence may be found in Missouri, Arkansas, Kansas, and Oklahoma |
However, the range and distribution where hard- and soft-bodied ticks may carry these individual agents vary considerably, and may evolve over time. (See Figures 5 and 6.) The seroprevalence and distribution of tickborne diseases among transplant donors has been observed to expand and increase throughout the continental United States in the last few decades.26 Some pathogens have found their way into unexpected tick vectors, opening new ranges of disease transmission. This occurred when Rocky Mountain spotted fever found its way into the Southwestern United States by way of the brown dog tick, leading to an ongoing epidemic on certain Native American reservations in Arizona and in parts of the Mexican state of Sonora.27,28
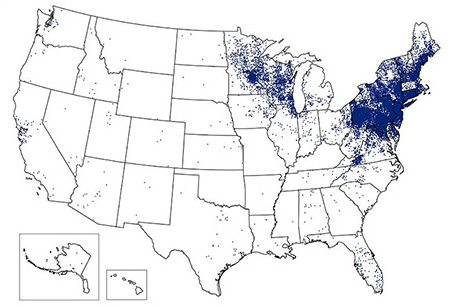
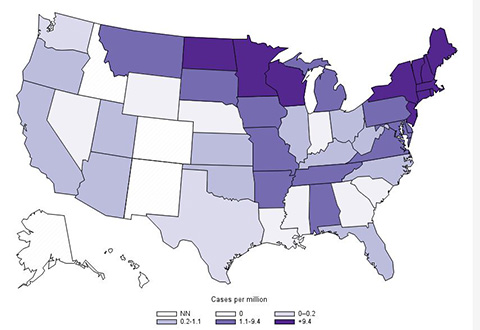
Figure 5. CDC Distribution Maps of Anaplasmosis and Lyme Disease in the United States |
Annual reported incidence (per million population) for anaplasmosis – United States, 2017 |
 |
Reported Cases of Lyme Disease — United States, 2017 |
|
One dot placed randomly within county of residence for each confirmed case
|
|
Source: Centers for Disease Control and Prevention |
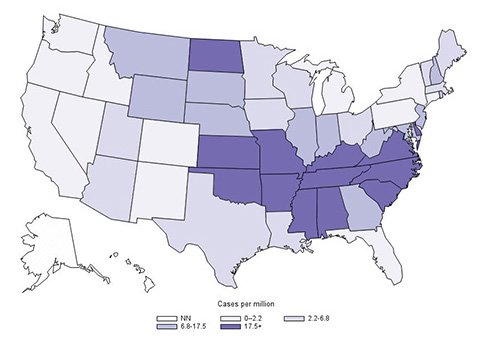
Figure 6. CDC Distribution Maps of Rocky Mountain Spotted Fever and Ehrlichiosis in the United States |
Annual incidence (per million persons) for Rocky Mountain spotted fever in the United States, 2017 |
 |
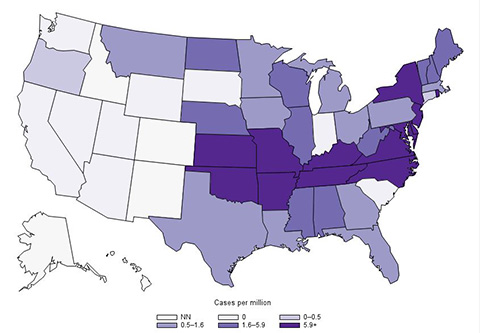
Annual reported incidence (per million population) for E. chaffeensis in the United States for 2017 |
 |
|
Source: Centers for Disease Control and Prevention |
On the other hand, practitioners should be skeptical of popular concerns of tickborne disease, such as Lyme disease, if patients present from regions without reported cases of endemically transmitted Borrelia burgdorferi.29 In short, whenever concern for tickborne disease arises, practitioners should consult resources from the Centers for Disease Control and Prevention.
Life Cycle and Pathophysiology
Both hard- and soft-bodied ticks progress through larval and nymphal stages before achieving adulthood. However, feeding patterns between species differ. Adult hard-bodied ticks may attach and feed on hosts for as long as one to four weeks, eventually engorging themselves with a substantial blood meal and thereafter dropping off the host.2 Soft-bodied ticks more typically inhabit mammalian burrows and nests, emerging at regular intervals to feed on their hosts for short periods of time.30
Because of these differences, patients usually are bitten by soft-bodied ticks while they sleep and rarely take notice, whereas patients sometimes may discover hard-bodied ticks still attached and feeding on the skin.25
Days to weeks after feeding, female hard-bodied ticks begin the process of laying thousands of eggs. These eggs hatch within days to weeks, releasing six-legged larvae only 0.5 mm to 1.5 mm long, small enough to be mistaken for mites.2,30 These larvae then begin the process of “questing,” wherein swarms of immature ticks climb to the tips of grasses and leaves, positioning themselves and latching onto passing hosts. After feeding for several days, the larval ticks then will drop to the ground, take shelter in leaf litter or soil, and emerge again as nymphs. These nymphs repeat the same questing behavior, sometimes for several cycles, before fully developing as adults. Importantly, most humans are bitten by larval or nymphal stage hard-bodied ticks, while adults more typically latch onto cattle, deer, horses, or other large mammals. Soft-bodied ticks inadvertently may feed on humans who sleep or stay close to rodent nests, such as when vacationing in rustic cabins.25
Although most hard-bodied ticks require two to three years to fully progress through larval, nymphal, and adult stages, feeding and questing behaviors typically manifest during spring and summer, while development usually slows or arrests in the winter.2 However, in warmer climates, some ticks may quest, feed, and breed throughout the year.
Clinical Manifestations and Diagnosis
Patients may present with the tick still attached and feeding from the skin. However, the bite itself is painless, and patients usually discover the attached arthropod incidentally or by checking themselves after walking through an endemic area. Hard- and soft-bodied ticks inject anticoagulant agents into the host, and salivary components may lead to local inflammation after the tick has become detached.31 Thus, it is not unusual for the patient to mount a local reaction, including erythema, induration, urticaria, or itching at the site of a bite.
Tick Paralysis
Tick paralysis is caused by a neurotoxic salivary component released in some hosts during feeding. The syndrome typically manifests two to six days after the tick attaches itself to the host.32 Initially, patients experience irritability and restlessness, followed by paresthesias, ascending flaccid paralysis, ataxia, loss of deep tendon reflexes, eventual cranial nerve palsies, including oculomotor weakness, dysarthria, dysphagia, and, ultimately, respiratory failure and death.32,33,34 Girls have been reported to be at greater risk, since longer hair makes locating a tick attached to the scalp more challenging. Patients may be misdiagnosed with Guillain-Barré syndrome. Focal deficits have been reported, such as facial nerve paralysis in the presence of ticks attached behind the ear or arm weakness due to a tick attached in the region of the brachial plexus, but these cases appear relegated to Australia.33
Cutaneous Manifestations of Lyme Disease
While an in-depth discussion of tickborne illnesses is beyond the scope of the current review, the cutaneous aspects of Lyme disease are worth addressing briefly.
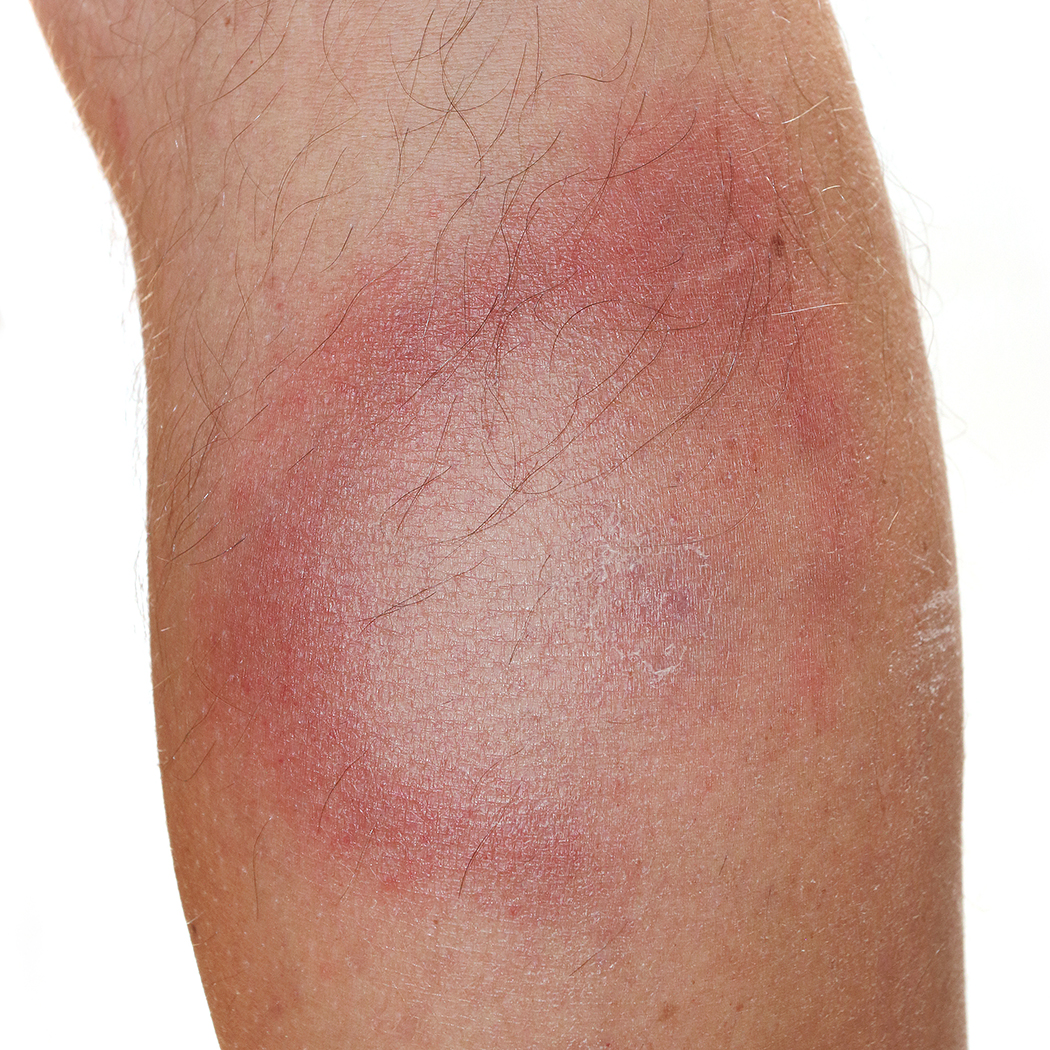
Erythema migrans frequently is described as the presenting rash of Lyme disease. This skin lesion develops at the site of inoculation (the tick bite) in 70-80% of cases, begins as a red macule or papule, and spreads outward in the course of days or weeks.35 Classically, it is an expanding, round lesion with central clearing, growing to at least 5 cm, but up to a median 15 cm in size.36 (See Figure 7.) The lesion may have an intensely erythematous, vesicular, or necrotic center, or even another annular lesion within it.35 Secondary lesions also can occur at other locations spared from tick bites. If the lesion has had enough time to spread, its annular nature may not be appreciated, resembling instead a diffuse, serpiginous (yet ill-defined) whole-body rash.35,36 An additional consideration is that erythema migrans often is accompanied by intermittent fever, fatigue, headaches, and myalgias, and lack of these symptoms may argue against the diagnosis.
Figure 7. Classic Bull’s-Eye Rash of Erythema Chronicum Migrans on the Lower Extremity |
 |
|
Source: Getty Images |
New Concerns Regarding Red Meat Allergy
A relatively new development is that some tick bites may be associated with new-onset allergy to red meat. Increasing reports have identified patients who experience a constellation of delayed allergic symptoms a few hours after consumption of red meat (beef, pork, or lamb), including rash, urticaria, pruritus, and gastrointestinal upset, in association with a history of tick bites and exposure.37,38,39 This association was first described in the New South Wales region of Australia, where allergic reactions to red meat were linked to individuals who had experienced tick bites in the bush.40 Since then, numerous other reports have been made of the same association in the United States, France, Sweden, Germany, Japan, and Central America.41-48 This association is not yet conclusive epidemiologically, but the association is thought to be due to a host reaction to tick salivary components, leading to the production of IgE antibodies against the oligosaccharide galactose-alpha-1,3-galactose (alpha-gal), which is present on many mammalian cells.38,49 The Lone Star tick (Amblyomma americanum) particularly has been implicated, and its recently spreading range is thought to be associated with growing deer populations, potentially explaining the rash of new cases.38 For now, cases with mild allergic-type symptoms should be treated with antihistamines, with appropriate referral to an allergy specialist for potential alpha-gal IgE antibody testing.39
Treatment
Patients should be advised to remove ticks when they are spotted on their person. This always should be performed as soon as possible, since ticks are more likely to transmit vector-borne disease the longer they are attached.50 Although numerous folk methods exist (suffocation with petroleum jelly, the use of matches, or covering with fingernail polish, etc.), these approaches may cause the tick to regurgitate and increase the likelihood of disease transmission. Instead, patients or providers should use a pair of forceps or tweezers to grasp the tick firmly where the head is attached to the skin, and pull directly outward with gentle, steady axial traction.50,51 Patients and providers should be cautious not to twist the tick or crush any body components; otherwise, blood may be regurgitated or parts of the head and jaws may be left in the skin. If any mouth parts remain embedded, forceps should be used to remove them or excision with a scalpel may be necessary.50
Local reactions from tick bites may be treated symptomatically with topical corticosteroids and oral antihistamines. Superinfection of a bite site with S. aureus is a consideration, and may be treated as any other cellulitis or folliculitis.
Patients may be concerned for the transmission of tickborne disease after tick removal, and may ask if prophylactic antibiotics are necessary. The Infectious Diseases Society of America does not recommend universal prophylaxis after tick bites.52 Similarly, the Centers for Disease Control and Prevention does not recommend universal prophylaxis, but it may be considered in areas highly endemic for Lyme disease.53 Providers may elect to prescribe a single dose of doxycycline to non-pregnant adults (200 mg) and to children older than 8 years of age (4 mg/kg up to 200 mg) who meet the following criteria:
- The patient is not pregnant, not younger than 8 years of age, or does not have any other contraindication to doxycycline (e.g., allergy).
- The offending tick can be identified positively as an I. scapularis adult or nymph.
- The offending tick has been attached for 36 hours or longer, which may be estimated depending on the degree of tick engorgement, or likely time when the patient was in a tick-endemic area (e.g., hiking in the woods).
- The provider can start the patient on prophylaxis within 72 hours of tick removal.
- Lyme disease is a pertinent consideration where the patient was bitten (CT, DE, MA, MD, ME, MN, NH, NJ, NY, PA, RI, VA, VT, WI).
It should be noted that there is no practicable prophylactic regimen for other tickborne illnesses, such as Rocky Mountain spotted fever, ehrlichiosis, babesiosis, anaplasmosis, etc.53 Patients in regions at risk for these illnesses should be advised to avoid tick bites, remove attached ticks as soon as possible, and watch vigilantly for symptoms of these diseases.
Prevention
Those at risk should be counseled on prevention of tick bites, such as avoiding high grass, brush, and leaf litter when outdoors, since questing nymphs and adults may perch in these locations awaiting a potential host.54 Wearing light-colored, long-sleeved shirts and pants with closed-toed shoes will help prevent ticks from attaching to the skin.55 Clothing may be impregnated with permethrin, a contact insecticide, to provide an additional layer of protection.54 The use of topical arthropod repellents should be advised. DEET is the best-studied and most commonly used repellent, and toxicity and side effects are rare.2,55 Depending on the concentration used (up to 30%), the duration of repellent activity may provide protection for up to six hours.55 Patients should be sure to follow the manufacturer’s directions and avoid its use in young infants. After traveling through a tick-endemic area, patients should check their clothing, gear, pets, and bodies for ticks, especially difficult-to-reach regions, such as the scalp, behind the ears, under the arms, around the waist, behind the knees, and between the legs.54
Patients also should be mindful of transmission of tickborne illnesses among pets. The brown dog tick has been discovered to serve as a vector of Rocky Mountain spotted fever in certain parts of the Southwest.27 Over-the-counter flea and tick shampoo and regular “tick checks” should be encouraged for families with dogs.
Conclusion
Providers in the emergency department frequently may see patients with concerns for ectoparasitic infestations and bites. In considering all of the above host-parasite interactions, a major caveat is the nonspecificity of many bites and biting patterns. And, as previously discussed, providers should remember that some patients experience more severe hypersensitivity responses than others. Infestations may plague an entire household, even if only one member of the family seems to manifest bite marks.
A wide variety of infestations from different organisms may present in the pediatric emergency department. With ongoing outbreaks of lice in different communities, growing bedbug infestations, and expanding populations of ticks in the United States, providers should ensure they are familiar with the diagnosis and treatment of such entities.
REFERENCES
- Diaz JH. Introduction to Ectoparasitic Diseases. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. New York: Elsevier Saunders; 2015.
- Service M. Medical Entomology for Students. 3rd ed. Cambridge, UK: Cambridge University Press; 2004.
- Centers for Disease Control and Prevention and U.S. Environmental Protection Agency. Joint statement on bed bug control in the United States from the U.S. Centers for Disease Control and Prevention (CDC) and the U.S. Environmental Protection Agency (EPA). Atlanta: U.S. Department of Health and Human Services; 2010.
- Dang K, Doggett SL, Veera Singham G, Lee CY. Insecticide resistance and resistance mechanisms in bed bugs, Cimex spp. (Hemiptera: Cimicidae). Parasit Vectors 2017;10:318.
- National Pest Management Association. Pest Control Professionals See Summer Spike in Bed Bug Calls. June 4, 2018. Available at: https://www.pestworld.org/news-hub/press-releases/pest-control-professionals-see-summer-spike-in-bed-bug-calls/. Accessed Jan. 17, 2019.
- Kantor J. Seasonal variability in bed-bug (Cimex lectularius) activity in Western Europe, the United States, and Australia using search engine query data as a surrogate outbreak measure. J Am Acad Dermatol 2016;75:627-629.
- Habif TP. Infestations and bites. In: Habif TP. Clinical Dermatology: A Color Guide to Diagnosis and Therapy. 6th ed. Philadelphia: Elsevier; 2016.
- Elston D. Bites and Stings. In: Bolognia JL, Schaffer JV, Cerroni L. Dermatology. 4th ed. Philadelphia: Elsevier; 2018.
- Goddard J, de Shazo R. Psychological effects of bed bug attacks (Cimex lectularius L.). Am J Med 2012;125:101-103.
- Ashcroft R, Seko Y, Chan LF, et al. The mental health impact of bed bug infestations: A scoping review. Int J Public Health 2015;60:827-837.
- Pritchard MJ, Hwang SW. Cases: Severe anemia from bedbugs. CMAJ 2009;181:287-288.
- Paulke-Korinek M, Széll M, Laferl H, et al. Bed bugs can cause severe anaemia in adults. Parasitol Res 2012;110:2577-2579.
- Venkatachalam PS, Belavady B. Loss of haemoglobin iron due to excessive biting by bed bugs. A possible aetiological factor in the iron deficiency anaemia of infants and children. Trans R Soc Trop Med Hyg 1962;56:218-221.
- Goddard J, deShazo R. Bed bugs (Cimex lectularius) and clinical consequences of their bites. JAMA 2009;301:1358-1366.
- Ho D, Lai O, Glick S, Jagdeo J. Lack of evidence that bedbugs transmit pathogens to humans. J Am Acad Dermatol 2016;74:1261.
- Lowe CF, Romney MG. Bedbugs as vectors for drug-resistant bacteria. Emerg Infect Dis 2011;17:1132-1134.
- Fallen RS, Gooderham M. Bedbugs: An update on recognition and management. Skin Therapy Lett 2011;16: 5-7.
- Lavery MJ, Parish LC. Bed bugs revisited. Skinmed 2011;9:6-8.
- Vaidyanathan R, Feldlaufer MF. Bed bug detection: Current technologies and future directions. Am J Trop Med Hyg 2013;88:619-625.
- Heymann WR. Bed bugs: A new morning for the nighttime pests. J Am Acad Dermatol 2009;60:482-483.
- Doggett SL, Dwyer DE, Peñas PF, Russell RC. Bed bugs: Clinical relevance and control options. Clin Microbiol Rev 2012;25:164-192.
- Totten V, Charbonneau H, Hoch W, et al. The cost of decontaminating an ED after finding a bed bug: Results from a single academic medical center. Am J Emerg Med 2016;34:649.
- Ruckriegel C, Pascarella L, Harmon P, et al. Bed bugs? Preventing mayhem with a protocol. Am J Infect Control 2011;39:E65
- US Department of Health and Human Services, Centers for Disease Control and Prevention. Tickborne Diseases of the United States: A Reference Manual for Healthcare Providers. 5th ed. 2018.
- US Department of Health and Human Services, Centers for Disease Control and Prevention. Tick ID. Available at: https://www.cdc.gov/ticks/tickbornediseases/tickID.html. Accessed Jan. 22, 2019.
- Diaz JH. Ticks, Including Tick Paralysis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. Philadelphia: Elsevier Saunders; 2015.
- Demma LJ, Traeger MS, Nicholson WL, et al. Rocky Mountain spotted fever from an unexpected tick vector in Arizona. N Engl J Med 2005;353:587-594.
- Álvarez-Hernández G, Roldán JFG, Milan NSH, et al. Rocky Mountain spotted fever in Mexico: Past, present, and future. Lancet Infect Dis 2017;17:e189-e196.
- Halperin JJ, Baker P, Wormser GP. Common misconceptions about Lyme disease. Am J Med 2013;126:264.e1-7.
- Vredevoe L. Background Information on the Biology of Ticks. UC Davis Department of Entomology and Nematology. Available at: http://entomology.ucdavis.edu/Faculty/Robert_B_Kimsey/Kimsey_Research/Tick_Biology/. Accessed Jan. 22, 2019.
- Paller AS, Mancini AJ. Infestations, Bites, and Stings. In: Paller AS, Mancini AJ, eds. Hurwitz Clinical Pediatric Dermatology: A Textbook of Skin Disorders of Childhood and Adolescence. 5th ed. Philadelphia: Elsevier; 2016.
- Vedanarayanan V, Sorey WH, Subramony SH. Tick paralysis. Semin Neurol 2004;24:181-184.
- Edlow JA, McGillicuddy DC. Tick paralysis. Infect Dis Clin North Am 2008;22:397-413.
- Bolgiano EB, Sexton J. Tickborne Illnesses. In: Walls R, Hockberger R, Gausche-Hill M. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia: Elsevier; 2018.
- Steere AC. Lyme Disease (Lyme Borreliosis) due to Borrelia burgdorferi. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases. 8th ed. Philadelphia: Elsevier Saunders; 2015.
- Michaels MG, Williams JV. Infectious Diseases. In: Zitelli BJ, McIntire SC, Nowalk AJ. Zitelli and Davis’ Atlas of Pediatric Physical Diagnosis. 7th ed. Philadelphia: Elsevier; 2018.
- Commins SP, Platts-Mills TA. Tick bites and red meat allergy. Curr Opin Allergy Clin Immunol 2013;13:354-359.
- Platts-Mills TA, Schuyler AJ, Tripathi A, Commins SP. Anaphylaxis to the carbohydrate side chain alpha-gal. Immunol Allergy Clin North Am 2015;35:247-260.
- Khoury JK, Khoury NC, Schaefer D, et al. A tick-acquired red meat allergy. Am J Emerg Med 2018;36:341.e1-341.e3.
- Van Nunen SA, O’Connor KS, Clarke LR, et al. An association between tick bite reactions and red meat allergy in humans. Med J Aust 2009;190:510-511.
- Jacquenet S, Moneret-Vautrin DA, Bihain BE. Mammalian meat-induced anaphylaxis: Clinical relevance of anti-galactose-alpha-1,3-galactose IgE confirmed by means of skin tests to cetuximab. J Allergy Clin Immunol 2009;124:603-605.
- Morisset M, Richard C, Astier C, et al. Anaphylaxis to pork kidney is related to IgE antibodies specific for galactose-alpha-1,3-galactose. Allergy 2012;67:699-704.
- Nunez R, Carballada F, Gonzalez-Quintela A, et al. Delayed mammalian meat-induced anaphylaxis due to galactose-alpha- 1,3-galactose in 5 European patients. J Allergy Clin Immunol 2011;128:1122-1124.
- Takahashi H, Chinuki Y, Tanaka A, Morita E. Laminin y-1 and collagen x-1 (VI) chain are galactose-a-1, 3-galactose-bound allergens in beef. Allergy 2014;69:199-207.
- Caponetto P, Fischer J, Biedermann T. Gelatin-containing sweets can elicit anaphylaxis in a patient with sensitization to galactose-a-1,3-galactose. J Allergy Clin Immunol Practice 2013;1:302-303.
- Fischer J, Hebsaker J, Caponetto P, et al. Galactose-alpha-1,3-galactose sensitization is a prerequisite for pork-kidney allergy and cofactor-related mammalian meat anaphylaxis. J Allergy Clin Immunol 2014;134:755-759.e1.
- Hamsten C, Tran TAT, Starkhammar M, et al. Red meat allergy in Sweden: Association with tick sensitization and B-negative blood groups. J Allergy Clin Immunol 2013;132:1431-1434.
- Wickner PG, Commins SP. The first 4 Central American cases of delayed meat allergy with galactose-alpha-1, 3-galactose positivity clustered among field biologists in Panama. J Allergy Clin Immunol 2014;133(Supp): AB212.
- Cabezas-Cruz A, Mateos-Hernández L, Chmelar J, et al. Salivary prostaglandin E2: Role in tick-induced allergy to red meat. Trends Parasitol 2017;33:495-498.
- Stone DB, Scordino DJ. Foreign Body Removal. In: Roberts JR, Custalow CB, Thomsen TW, eds. Roberts and Hedges’ Clinical Procedures in Emergency Medicine and Acute Care. 7th ed. Philadelphia: Elsevier; 2019.
- US Department of Health and Human Services, Centers for Disease Control and Prevention. Tick Removal. Available at: https://www.cdc.gov/ticks/removing_a_tick.html. Accessed Jan. 24, 2019.
- Wormser GP, Dattwyler RJ, Shapiro ED, et al. The clinical assessment, treatment, and prevention of Lyme disease, human granulocytic anaplasmosis, and babesiosis: Clinical practice guidelines by the Infectious Diseases Society of America. Clin Infect Dis 2006;43:1089-1134.
- US Department of Health and Human Services, Centers for Disease Control and Prevention. Tick Bite Prophylaxis. Available at: https://www.cdc.gov/ticks/tickbornediseases/tick-bite-prophylaxis.html. Accessed Jan. 24, 2019.
- US Department of Health and Human Services, Centers for Disease Control and Prevention. Preventing Tick Bites. Available at: https://www.cdc.gov/ticks/avoid/on_people.html. Accessed Jan. 24, 2019.
- Sood SK, Krause PJ. Lyme Disease. In: Cherry JD, Harrison GJ, Kaplan SL, et al, eds. Feigin and Cherry’s Textbook of Pediatric Infectious Diseases. 8th ed. Philadelphia: Elsevier; 2019.
Providers in the pediatric emergency department frequently encounter ectoparasitic infestations. Infestations require early recognition and knowledge of effective treatment strategies. Last month, the author reviewed scabies, chiggers, and lice. This month, the bedbugs and ticks will come biting!
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.