Shocking Injuries: Knowing the Risks and Management for Electrical Injuries
July 1, 2019
Reprints
AUTHORS
Anne Walker, MD, Clinical Instructor, Emergency Medicine, Stanford University School of Medicine, Palo Alto, CA
Alexis Salerno, MD, Clinical Instructor, University of Maryland School of Medicine, Baltimore
PEER REVIEWER
Dennis Hanlon, MD, FAAEM, Quality Director, Allegheny General Hospital, Pittsburgh
Executive Summary
- Alternating current is about three to five times more damaging than direct current of equal voltage and current.
- Patients with electrical injuries should be treated first as trauma patients.
- The two most dangerous electrical pathways are from hand to hand (most dangerous; potentially affecting the heart and the spinal cord) and from hand to foot (potentially affecting the cardiovascular system).
- The severity of burn wounds caused by the electrical current does not accurately predict the severity of the injury. Tissues such as nerves, blood vessels, mucous membranes, and muscles have the least resistance and, therefore, are most likely to be damaged during electrical exposure.
- Electricity has significant effects on the muscle tissues and may result in rhabdomyolysis, which may be assessed by a creatine kinase (CK) level. The CK levels correlate with the length of stay and the incidence of serious complications, such as amputation and need for skin grafting.
- Patients who have had contact with power lines or a high-voltage injury are at higher risk for developing compartment syndrome. During the examination and treatment of these patients, it is important to evaluate all extremities and joints through their full range of motion and perform serial neurovascular checks. If there is concern for compartment syndrome, the compartment pressures should be checked in these areas.
- Oral electrical burns resulting from children putting electrical cords into their mouths typically include injuries involving the lip commissures and can extend into the gums and tongue. In addition, saliva can be a thermic conductor, generating temperatures up to 2,500° C to 3,000° C and leading to thermal burn injuries. The injuries can range from superficial burns to serious injuries requiring multiple surgeries to gain cosmetic effect. Burns affecting the tongue and lip movement can cause functional impairment of speech requiring speech rehabilitation.
Approximately 5,000 patients present to the emergency department (ED) each year for evaluation and treatment of electrical injuries.1 The objective of this article is to discuss the different classifications of electrical exposures and describe the recommended initial evaluation, diagnostic workup, and treatment. In addition, it also will discuss special situations, such as lightning exposures, pediatric exposures, and electrical exposures during pregnancy.
— Ann M. Dietrich, MD, Editor
Introduction
Electrical exposures can be categorized in several different ways. They often are separated based on the source of the injury: alternating current (AC) or direct current (DC). Injuries may occur in a household, recreational, or occupational setting, and a trimodal age distribution of injury has been described. The first peak is in the pediatric age group, often from household appliances.2 The second peak is during the teenage years, often from risky behavior near power lines or other sources. By far, the most significant injuries occur in the occupational environment in the adult population, which makes up the third peak.3 Most homes and workplaces use AC as the electrical supply, whereas batteries, automobiles, and power lines generally use DC. Injuries generally are worse with AC exposures than with DC exposures at an equal voltage. This is because low-frequency AC tends to cause tetany, which makes it difficult for the individual to release the current source and prolongs the length of exposure. For this reason, AC is about three to five times more damaging than DC of equal voltage and current. See Table 1 for a comparison of AC and DC injuries.
Table 1. Types of Electricity and Their Typical Characteristics |
|||
Location of Injury |
Wound Appearance |
Treatment Considerations |
|
|
Alternating Current |
Home or office |
Large exit wound |
|
|
Direct Current |
Automobiles, batteries, powerlines |
Discrete entrance and exit wounds |
|
Electrical injuries also can be characterized based on the source, such as a low-voltage source, a high-voltage source, a flash burn (no current passes through the affected person), or lightning.2,3 Clinically, the most common classification is low vs. high voltage, a distinction that can affect the medical workup and disposition significantly. Traditionally, high voltage is considered more than 1,000 volts and low voltage is considered lower than 1,000 volts. However, some systems are now considering > 600 volts as the threshold for high voltage. High-voltage injuries make up approximately 38% to 50% of all electrical injuries; low-voltage injuries comprise approximately 20% to 44.7% of injuries; and flash burns make up about 33% to 45.5% depending on the study.3 In general, workplace injuries tend to involve high-voltage exposures. Up to 75% of high-voltage burns were work-related, and more than 50% of these were from contact with powerlines.4,5 As would be expected, higher voltage generally leads to more severe injuries. This is because of deeper penetration of the current, which can lead to muscle necrosis and the potential need for fasciotomy or amputation.3,6
Pathophysiology
Injuries from electricity occur as a result of the effects of the electrical current, electroporation, the thermal energy produced, and falls.
Current is the most important determinant of tissue damage from electrical injuries. Joule’s law states that thermal energy is the product of the current multiplied by the resistance and time of current flow.7,8 (See Figure 1.) It is thought that a higher-voltage electrocution produces a larger current and, therefore, a more devastating injury.7 Nerves and blood vessels are good conductors of electricity because of their low resistance and can sustain a widespread injury.8 Current crossing the chest can interfere with the neurological signals to the respiratory and cardiac systems, causing apnea or asystole. Injuries to the nerves can cause paresthesia and paralysis, while injury to the blood vessels can cause coagulation.
Figure 1. Joules Law of Thermal Energy |
Q = I2 RtWhere Q is in Joules, I is in Amps, R is in ohms, and t is in seconds |
Electroporation is defined as the electrical current disrupting the cell membranes by producing pores without significant thermal energy.8,9 This releases the contents of the cell and disrupts ion channels. If the cell is unable to repair the membrane, it will die. Disruption of the intimal layer of blood vessels from this mechanism can result in delayed bleeding or development of thrombosis. Because this most commonly happens in small vascular branches of muscles, it can result in the development of a perceived delayed “tissue necrosis.” Long traveling neurons are also at high risk of injury as a result of this mechanism and additionally can be affected by disruption of vascular supply to them.10 Structures such as bones, fat, and tendons that have the highest resistance produce large amounts of thermal energy. This causes coagulation of the surrounding muscles, which can be present even without external manifestations.8,11
After the initial electrocution, patients may experience injuries secondary to trauma, most commonly falls. These injuries occur often in power line workers who fall from a height after the electrocution.
General Approach to Patients With Electrical Injuries
In general, prehospital triage of patients with electrical burns should be directed toward a burn center or trauma center, especially for cases that involve the face, hands, eyes, ears, or genitalia.12 High-voltage injuries in particular have a high risk for complications and would benefit from the specialized resources available at a burn/trauma center.6
History
When obtaining a history from emergency medical services, the patient, or family members, it is important to ask where the event took place and what was the source of the electrocution. If the source of electricity is known, it is important to ask about the voltage amount. It is also important to ask about the duration of the event and whether the patient was propelled away from the initial contact site. Lastly, note whether any loss of consciousness, dysrhythmias, difficulty breathing, muscle tenderness, or neurologic deficits occurred. (See Table 2.)
Table 2. Questions to Ask Patients With Electrical Injuries |
|
Physical Examination
Patients with electrical injuries should be treated first as trauma patients. Spinal motion restriction should be maintained until spinal injury is excluded. A primary survey is critical. A respiratory arrest can occur from the electrical shock itself. This is because of the effects of the current on the respiratory center in the medulla or from tetany of the diaphragm and respiratory muscles causing temporary paralysis.13 If there are signs of progressive airway swelling, as with other burns, have a low threshold to intubate in the prehospital setting or initially on ED arrival.
If a dysrhythmia occurs, it will occur immediately after the electrical exposure in most cases. The majority of dysrhythmias are supraventricular, but exposure to high-voltage current is more likely to cause asystole or ventricular dysrhythmias.14 If a patient with an automated implantable cardioverter defibrillator or pacemaker has been affected by an electrical injury, the patient should be placed on continuous cardiac monitoring, and pads should be placed for potential external pacing. Later in the evaluation of these patients, the device should be interrogated because electrocution can damage the functionality of these devices.13
Examine the patient’s pupils for size and reactivity; fixed and dilated pupils may occur secondary to the effects of electricity on the autonomic nervous system and do not necessarily reflect anoxic brain injury. Therefore, this physical exam finding should not lead to termination of resuscitation.13
The likely pathway of the current may be determined by carefully examining the entrance and exit wounds. The most common entrance wound is through the hand and the most common exit wound is through the foot. A pathway through the body from hand to hand is the most dangerous because it is likely to affect the heart and the spinal cord. A pathway from the hand to the foot also potentially can affect the cardiovascular system, although this occurs less frequently than with the hand-to-hand pathway. Straddle injuries in which entrance and exit wounds both occur on the feet have a much lower mortality than the two pathways mentioned previously.15,16 Discrete exit wounds are found more commonly with DC injuries than with AC injuries.
It is also important to remember that the severity of burn wounds caused by the electrical current does not accurately predict the deeper damage that has occurred, in contrast to typical fire burns.13 In general, increased resistance of a tissue is associated with increased thermal injury. Tissues such as the nerves, blood vessels, mucous membranes, and muscles have the least resistance and, therefore, are most likely to be damaged during electrical exposure. In contrast, bone, fat, and skin have high resistance and, therefore, are poor conductors of the electrical current. Of note, because of dry skin’s high resistance, thermal burns can occur when electricity travels throughout it. Wet skin has less resistance than dry skin and dissipates energy quickly to deeper tissues, which results in decreased surface burns but greater injury to deeper tissues.17 High-voltage injuries generally cause deeper tissue injuries because of the thermal energy produced.6
Once the patient is stabilized, take an AMPLE history (allergies, medication, past medical history, last oral intake, events of injury) and assess if there are any specific areas of concern to the patient, taking special care to note areas of pain, numbness, or weakness.
Treatment of Patients With Electrical Injuries
All patients with high-voltage exposures should be evaluated with laboratory studies, an electrocardiogram (ECG), and imaging, as needed, to assess for any trauma they may have sustained.
Cardiovascular
The most common ECG arrhythmias are sinus tachycardia and premature ventricular contractions. However, atrial fibrillation, ventricular fibrillation, and ventricular tachycardia also have been reported.13 Many of these dysrhythmias will be present initially after the inciting event. Patients with exposure to high-voltage electricity or those with low-voltage electricity associated with chest pain, syncope, or palpitations should be placed on continuous cardiac monitoring to observe for any abnormalities.18
Direct damage to the heart muscle also can occur from the electrical injury and coronary vasospasm, producing a risk for myocardial infarction, which may present atypically without chest pain.13 The ECG may show the classic ST elevations or Q waves in these cases. A troponin is useful in cases involving chest pain or a suspicious abnormality on the ECG. However, more widespread use of troponin for general monitoring in electrical injuries has not been studied sufficiently.13
Vascular damage can be associated with high-voltage electrical injuries and primarily affects small vessels. This damage can lead to medial necrosis with aneurysm formation. If there is any concern for aneurysm based on the patient’s history or exam, a computed tomography (CT) angiography or magnetic resonance (MR) angiography can be ordered, depending on institution availability.13
Skin and Musculoskeletal
In general, external burns should be cleansed and covered with a clean dressing.12 Patients also should have receive tetanus immunizations if open wounds or external burns are present.12 Because of the effects of electricity on the muscle tissues, it is important to assess for signs of rhabdomyolysis by obtaining a creatine kinase (CK) level. The CK levels correlate with length of stay and incidence of serious complications, such as amputation and need for skin grafting.6 Patients with elevated levels should be treated with adequate fluid resuscitation. Intravenous fluids should be given to produce a urine output of at least 0.5 mL/kg/hour up to 2 mL/kg/hour. Unfortunately, standard burn formulas, such as the Parkland formula, do not adequately represent the fluid resuscitation needed for an electrical injury patient. This is because deep burns caused by electrical injuries may not be apparent on the skin surface and, therefore, the burn percentage is underestimated.8 If myoglobin levels remain high, the administration of mannitol should be discussed in collaboration with a burn specialist.6 Administration of bicarbonate to alkalinize the urine and prevent the toxic breakdown of myoglobin has been a proposed treatment for cases of rhabdomyolysis; however, no large randomized trials have shown a clear benefit.19
Patients who have had contact with power lines or a high-voltage injury are at higher risk for developing compartment syndrome. During the examination and treatment of these patients, it is important to evaluate all extremities and joints through their full range of motion and perform serial neurovascular checks. If there is concern for compartment syndrome, the compartment pressures should be checked in these areas.5 If pressures are found to be rising, patients benefit from early fasciotomies and potential surgical debridement of the tissue.
Disposition
Most patients with minor electrical injuries will be able to be discharged home. Asymptomatic patients with low-voltage injuries and a normal ECG can be discharged safely with primary care follow-up. Patients who have had a low-voltage injury associated with loss of consciousness or ECG changes should be observed with continuous cardiac monitoring for 24 hours.18 A few recent studies have shown no increased risk for dysrhythmias if they are not present originally. Therefore, 24-hour cardiac monitoring may not be required if the patient had a normal ECG and cardiac rhythm on arrival.20-24
All patients with exposure to high-voltage electricity should be admitted. Regardless of voltage type, all patients with burns involving the face or genitals, circumferential limb burns, and large percent body surface area burns should be transferred to the local burn center. As previously noted, patients with signs of compartment injury or deep tissue injury should be evaluated by a surgeon for early surgical debridement. (See Table 3.)
Table 3. Unique Features of Electrical Injuries |
|||
History |
Physical Exam |
Management |
|
|
Low Voltage |
|
|
|
|
High Voltage |
|
|
|
|
Lightning |
|
|
|
Long-Term Effects
Electrical injuries can have a delayed effect on patients. Some patients will develop ascending paralysis, transverse myelitis, cataracts, and even amyotrophic lateral sclerosis (ALS) later in their clinical course.7 It is critical to send patients home with strict return precautions for any new neurological symptoms. In addition, cataract formation occurs in 5% to 20% of patients who have had an electrical injury. Therefore, it is important to refer patients for ophthalmology follow-up.18
As providers, it is important to recognize that this is a traumatic event for patients. A study of 311 French workers who sustained high-voltage electrical injuries showed that a number of patients had psychological sequalae from their experience, including post-traumatic stress disorder (PTSD). Provide resources for psychological support.25
Oral Pediatric Burns
Children who chew on electrical cords represent a distinct group of electrical injuries. (See Figure 2.) These incidences occur mostly when children are between the ages of 6 months and 3 years and start to explore their surroundings. The incidence of these types of injuries has decreased because of improved product safety standards. It is now estimated that oral electrical burns represent 0.001% of all pediatric injuries.26
Figure 2. Oral Commissure Burn |
 |
|
Image courtesy of Ann Dietrich, MD |
The extent of injury depends on the duration of contact, electrical voltage, and location. Many of these patients will present with injuries involving the lip commissures and that can extend into the gums and tongue.27 In addition, patients can have thermal burn injuries from saliva being a thermic conductor with temperatures generated up to 2,500° C to 3,000° C.28 Therefore, burns can range from superficial injuries to serious injuries requiring multiple surgeries to gain cosmetic effect. Burns affecting the tongue and lip movement can cause functional impairment of speech requiring speech rehabilitation.26
In the ED, chlorhexidine or bacitracin can be applied to the wound for comfort. However, because the extent of these injuries requires multidisciplinary treatment, children presenting with any facial electrical or burn injuries should be transferred to the nearest pediatric burn center.26 These patients often require oral splinting for cosmetic reasons and often need plastic surgery follow-up, although there is no universal agreement on optimal management. In addition, one to two weeks after the initial injury, the eschar starts to slough off due to enzyme dissolution. This potentially can cause labial artery hemorrhage, although over the last 10 years, these types of injuries have been documented rarely.28,29 Apply pressure to the area to help stop the bleeding. Very rarely would the amount of bleeding require an intervention.
Lightning Injuries
Lightning strike injuries are a rare and specific type of electrical injury. (See Tables 3 and 4.) The incidence is estimated at nine out of every 10 million people.30 In the United States, the National Weather Service reported an average of 234 injuries from lightning strikes each year from 2004 to 2013.31,32 There is an estimated 32% mortality from lightning injuries, generally occurring immediately after exposure from cardiac or respiratory arrest.1,33 Agricultural workers and construction workers are at highest risk, as are as outdoor enthusiasts and active members of the military.30,31,34
Table 4. Neurologic Sequelae From Lightning Strikes |
||||
Condition |
Description and Symptoms |
Cause |
Timing |
Treatment |
|
Keraunoparalysis |
Transient paralysis after a lightning strike; involves weakness and sensory loss in extremities; most commonly affects lower extremities |
Thought to be caused by overstimulation of the autonomic nervous system |
Transient; should not last more than 24 hours |
Usually resolves without treatment |
|
Complex regional pain syndrome |
Pain, sweating, edema, sensitivity after trauma |
Believed to be caused by autonomic nervous system dysfunction |
Often delayed; occurs hours to days after trauma; not transient |
Rehabilitation, such as physical and occupational therapy; medications such as sympathetic antagonists, adrenergic agents, anticonvulsants, steroids, and tricyclic antidepressants may be useful |
Lightning can be thought of as a very brief, high-intensity, direct current. Mechanisms of injury in lightning events include direct strike injury (which accounts for approximately 5% of strike events), contact injury (the patient is touching an object that is struck), and injury from side flash or from ground current (in which the current first hits another object or the ground at a nearby point and then travels around the patient).30,33
Initial Evaluation
Nearly all people who are struck by lightning will survive if they do not succumb to an immediate cardiac or respiratory arrest. Therefore, reverse triage should be practiced in response to a multi-victim lightning strike scenario.35 First attend to patients who are without vital signs because their cardiac or respiratory arrest may be reversible. Arrests after lightning strikes can be cardiac from the depolarization of the electric shock or respiratory from inhibition of the respiratory center in the medulla. Often, it is a combination of the two. Because the heart recovers its automaticity prior to the medulla’s recovery, it is possible for the patient to have a secondary respiratory arrest.35 Lightning strike victims also may have dilated and unreactive pupils as a result of the electrical effects on the pupils. Therefore, in patients struck by lightning, unreactive pupils are not an accurate indicator of brain function.1
Lightning can cause a range of injuries. Since the duration of exposure is so short, if the victim is dry, the current is likely to pass over rather than through the patient, and deep burns and underlying tissue damage rarely are seen. Superficial thermal burns may occur from moisture vaporization on the skin itself.33 Patients who are wearing metal jewelry also may be affected by thermal burns in these areas. One well-known effect of lightning on skin moisture vaporization is sudden explosion. This can result in the patient being found without any clothes or shoes on at the scene. Therefore, patients also should be examined for signs of secondary blunt injuries from being thrown or falling after the blast.
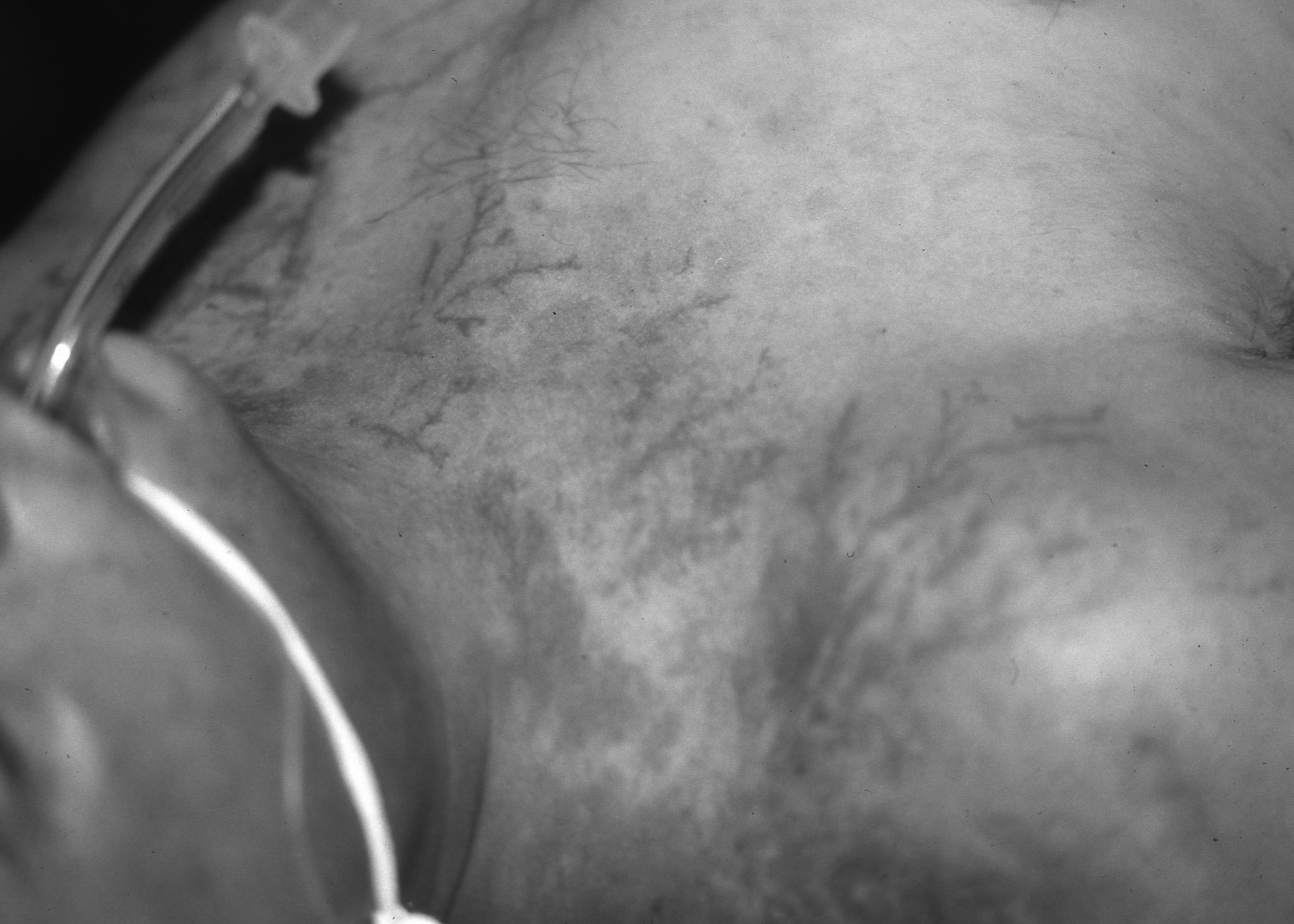
As opposed to other electrical injuries, lightning injuries rarely exhibit entry and exit wounds on physical exam. Because of the very short length of exposure with lightning injuries, tetanic muscle contractions are not seen. A characteristic feature of a lightning injury is Lichtenberg figures, which also are called “feathering” or “ferning” lesions based on their appearance.33 (See Figure 3.) These lesions technically are not burns but are caused by transient extravasation of blood in the subcutaneous areas where discoloration then occurs. These figures usually present within one hour and usually last for a matter of days followed by spontaneous resolution. Lichtenberg figures do not require any special treatment.33,35 Other findings may include loss of vision and loss of hearing (due to sensorineural hearing loss or ruptured tympanic membrane).31,35,36
Figure 3. Lichtenberg Figures |
 |
|
Image courtesy of David Effron, MD, Associate Professor, Case Western Reserve University, Attending Physician, Department of Emergency Medicine, MetroHealth Medical Center, Cleveland, OH |
Neurologic Sequelae
The nerves are the most conductive surface in the body and, thus, patients affected by lightning are prone to neurologic damage. This damage can range from brief to permanent and debilitating. Confusion, headache, seizure, or loss of consciousness may occur immediately and may be transient.35 A specific neurologic injury that can occur is keraunoparalysis or “Charcot’s paralysis.”37,38 (See Table 4.) This transient paralysis after a lightning strike is thought to be due to overstimulation of the autonomic nervous system from transient excessive catecholamine release and extreme vasoconstriction. It is the most common immediate neurologic sequela of a lightning strike.35,37,38 Keraunoparalysis often involves both weakness and sensory loss in the extremities. The condition affects the lower extremities most commonly and also can be associated with a transient loss of pulses and cyanosis.37 When initially checking for a pulse in patients who have been affected by lightning strikes, providers should be sure to check for central pulses so as not to assume incorrectly that there is no pulse in these patients.35 This phenomenon usually resolves without treatment over the course of several hours. It should not last more than 24 hours, and specific treatment is not needed.37
Complex regional pain syndrome also is a possible neurologic sequela. (See Table 4.) It is believed to be caused by autonomic nervous system dysfunction; however, this syndrome can be delayed and is not usually encountered on initial presentation.38 Patients present with pain, sweating, edema, and sensitivity hours to days after a trauma. Nerve conduction studies generally are not diagnostic; therefore, this is a clinical diagnosis. Unlike keraunoparalysis, the symptoms generally are not transient and should be treated. Rehabilitation with physical and occupational therapy should be arranged. Sympathetic antagonists, adrenergic agents, anticonvulsants, steroids, and tricyclic antidepressants also may be useful.38
Medical Workup and Treatment
Providers should order an ECG on any lightning strike victim who presents with chest pain, shortness of breath, or a high-risk feature such as a severe burn, evidence of trauma, loss of consciousness, suspected direct strike, focal neurologic strike, or pregnancy.35 ECG abnormalities include prolonged QT interval, atrioventricular block, sinus bradycardia, right bundle branch block, and other nonspecific ST changes.31 Most ECG changes resolve within three days, but pericarditis can be a late finding if a patient presents again weeks or months after a lightning strike.35 After a lightning strike, troponin testing has not been found to correlate with positive coronary angiography and, therefore, has limited clinical utility.35
As with other electrical burns, baseline laboratory testing, including myoglobin and CK levels, should be ordered. Because of the extremely short exposure, rhabdomyolysis is very rare in patients who experience lightning strikes. These patients do not need aggressive fluid resuscitation that other electrical injuries may require. In general, they should be admitted for 24 hours of cardiac monitoring, especially if they experienced a direct strike or if they have any positive ECG findings or screening tests.35
Follow-Up and Prevention
In addition to the various complications common to other electrical injuries, patients who have been struck by lightning often experience PTSD or extreme fear of thunder and lightning. They should be given adequate follow-up information and their family should be advised to look for any symptoms of PTSD. Additionally, patients should be advised to return if they experience any chest pain or shortness of breath because delayed cardiac injuries such as pericarditis and/or cardiomyopathies have been identified in some cases.35 Sometimes delayed neurologic sequelae, such as progressive myelopathy causing weakness and sensory loss months after the lightning strike, also can occur as well as cataracts and behavioral changes.
The National Weather Service states that the best treatment for lightning injuries is prevention. If one hears thunder, there is a risk of lightning. In thunderstorms avoid ridgelines, summits, metal objects, or tall objects such as isolated trees to prevent a lightning strike. Wait 30 minutes after the last sound of thunder to resume any outdoor activity. People who are in a wilderness setting and unable to go indoors should assume the lightning position: Sit or crouch with knees close together. People in a group should separate from each other by 20 feet or more.35
Pregnant Patients
Electrical exposure of the pregnant individual is a unique situation that raises concern for the well-being of the fetus. The rate of miscarriage following electrical exposures has been reported between 6% and 73%.14,35,39 It is postulated that the fetus is at greater risk because it is surrounded by amniotic fluid, which is a highly conductive substance.35 Another risk is the trauma of an electrical injury causing uterine rupture or premature rupture of membranes and labor induction.35 When caring for a pregnant patient with electrical injury, consultation with obstetrics and fetal heart monitoring would be appropriate if the gestation is greater than 20 weeks.13,35 If gestation is less than 20 weeks, the patient should be evaluated the same, but fetal monitoring is not necessary because the pregnancy is not considered viable.35
Lightning injuries in pregnant individuals are a rare occurrence. As of 2016, a review of the medical literature produced 14 case reports of pregnant patients struck by lightning. Of these, five reported intrauterine fetal demises, one died shortly after birth, one had long-term neurologic morbidity, and the remaining seven had no known reported sequelae.40-46 A lightning strike in the third trimester carries the greatest risk of morbidity and mortality for both mother and fetus. As in other serious traumas to a pregnant patient, optimizing care of the mother often is the best way to improve fetal outcomes.
Conclusion
Although the overall incidence of electric burns is low, there can be significant morbidity, mortality, and healthcare-related costs associated with this injury pattern. Potential complications of electrical injuries include rhabdomyolysis, compartment syndrome, gangrene due to intravascular thrombosis, dysrhythmias, infections, cataracts (especially if the current pathway involved the head and/or neck), seizures, memory loss, and peripheral nerve damage. Prompt recognition and treatment of the potentially life- and limb-threatening sequelae may reduce the morbidity and mortality associated with electrical burns.
REFERENCES
- Pujji O, Nizar B, Bechar J, et al. Burns Centre and fire services: What information can be exchanged to manage the burn patient? Burns 2018;44:573-581.
- Enoch S, Roshan A, Shah M. Emergency and early management of burns and scalds. BMJ 2009;338:b1037.
- Brandão C, Vaz M, Brito IM, et al. Electrical burns: A retrospective analysis over a 10-year period. Ann Burns Fire Disasters 2017;30:268-271.
- Patel BC. Emergency eye care in the accident and emergency department. Arch Emerg Med 1993;10:387-388.
- Hettiaratchy S, Papini R. Initial management of a major burn: II—assessment and resuscitation. BMJ 2004;329:101-103.
- Gille J, Schmidt T, Dragu A, et al. Electrical injury – a dual center analysis of patient characteristics, therapeutic specifics and outcome predictors. Scand J Trauma Resusc Emerg Med 2018;26:43.
- Primavesi R. A shocking episode: Care of electrical injuries. Can Fam Physician 2009;55:707-709.
- Spies C, Trohman RG. Narrative review: Electrocution and life-threatening electrical injuries. Ann Intern Med 2006;145:531-537.
- Bryan BC, Andrews CJ, Hurley RA, Taber KH. Electrical Injury, part I: Mechanisms. J Neuropsychiatry Clin Neurosci 2009;21:iv-244.
- Teodoreanu R, Popescu SA, Lascar I. Electrical injuries. Biological values measurements as a prediction factor of local evolution in electrocutions lesions. J Med Life 2014;7:226-236.
- Kidd M, Hultman CS, Van Aalst J, et al. The contemporary management of electrical injuries. Ann Plast Surg 2007;58:273-278.
- Schaefer TJ, Nunez Lopez O. Burns, Resuscitation And Management. StatPearls. Treasure Island, FL; StatPearls Publishing: 2018.
- Waldmann V, Narayanan K, Combes N, et al. Electrical cardiac injuries: Current concepts and management. Eur Heart J 2018;39:1459-1465.
- Waldmann V, Narayanan K, Combes N, Marijon E. Electrical injury. BMJ 2017;357:j1418.
- Foris LA, Huecker MR. Electrical Injuries. StatPearls. Treasure Island, FL; StatPearls Publishing: 2018.
- Thompson JC, Ashwal S. Electrical injuries in children. Am J Dis Child 1983;137:231-235.
- Fish RM, Geddes LA. Conduction of electrical current to and through the human body: A review. Eplasty 2009;9:e44.
- Friedstat J, Brown DA, Levi B. Chemical, electrical, and radiation Injuries. Clin Plast Surg 2017;44:657-669.
- Chavez LO, Leon M, Einav S, Varon J. Beyond muscle destruction: A systematic review of rhabdomyolysis for clinical practice. Crit Care 2016;20:135.
- Pawlik AM, Lampart A, Stephan FP, et al. Outcomes of electrical injuries in the emergency department. Eur J Emerg Med 2016;23:448-454.
- Searle J, Slagman A, Maaß W, Mockel M. Cardiac monitoring in patients with electrical injuries. An analysis of 268 patients at the Charité Hospital. Dtsch Arztebl Int 2013;110:847-853.
- Bailey B, Gaudreault P, Thivierge RL. Cardiac monitoring of high-risk patients after an electrical injury: A prospective multicentre study. Emerg Med J 2007;24:348-352.
- Purdue GF, Hunt JL. Electro-cardiographic monitoring after electrical injury: Necessity or luxury. J Trauma 1986;26:166-167.
- Blackwell N, Hayllar J. A three year prospective audit of 212 presentations to the emergency department after electrical injury with a management protocol. Postgrad Med J 2002;78:283-285.
- Piotrowski A, Fillet AM, Perez P, et al. Outcome of occupational electrical injuries among French electric company workers: A retrospective report of 311 cases, 1996–2005. Burns 2014;40:480-488.
- Umstattd LA, Chang CW. Pediatric oral electrical burns: Incidence of emergency department visits in the United States, 1997-2012. Otolaryngol Head Neck Surg 2016;155:94-98.
- Pontini A, Reho F, Giatsidis G, et al. Multidisciplinary care in severe pediatric electrical oral burn. Burns 2015;41:e41-e46.
- Yeroshalmi F, Sidoti EJ Jr, Adamo AK, et al. Oral electrical burns in children—A model of multidisciplinary care. J Burn Care Res 2011;32:e25-e30.
- Zubair M, Besner GE. Pediatric electrical burns: Management strategies. Burns 1997;23:413-420.
- Griggs C, Goverman J, Bittner EA, Levi B. Sedation and pain management in burn patients. Clin Plast Surg 2017;44:535-540.
- Thompson SN, Wilson ZW, Cole CB, et al. Case report: Mass casualty lightning strike at Ranger Training Camp. Mil Med 2017;182:e1803-e1806.
- US Department of Commerce, National Oceanic and Atmospheric Administration, National Weather Service. Lightning safety tips and resources. Available at: https://www.weather.gov/safety/lightning. Accessed Oct. 20, 2018.
- Eyerly-Webb SA, Solomon R, Lee SK, et al. Lightning burns and electrical trauma in a couple simultaneously struck by lightning. Clin Pract Cases Emerg Med 2017;1:246-250.
- Centers for Disease Control and Prevention (CDC). Lightning-associated injuries and deaths among military personnel--United States, 1998-2001. MMWR Morb Mortal Wkly Rep 2002;51:859-862.
- Davis C, Engeln A, Johnson EL, et al. Wilderness Medical Society practice guidelines for the prevention and treatment of lightning injuries: 2014 update. Wilderness Environ Med 2014;25(4 Suppl):S86-95.
- Ritenour AE, Morton MJ, McManus JG, et al. Lightning injury: A review. Burns 2008;34:585-594.
- ten Duis HJ, Klasen HJ, Reenalda PE. Keraunoparalysis, a “specific” lightning injury. Burns Incl Therm Inj 1985;12:54-57.
- Jost WH, Schönrock LM, Cherington M. Autonomic nervous system dysfunction in lightning and electrical injuries. NeuroRehabilitation 2005;20:19-23.
- Liu NT, Fenrich CA, Serio-Melvin ML, et al. The impact of patient weight on burn resuscitation. J Trauma Acute Care Surg 2017;83(1 Suppl 1):S112-S119.
- Rees WD. Pregnant woman struck by lightning. Br Med J 1965;1:103-104.
- Pierce MR, Henderson RA, Mitchell JM. Cardiopulmonary arrest secondary to lightning injury in a pregnant woman. Ann Emerg Med 1986;15:597-599.
- Galster K, Hodnick R, Berkeley RP. Lightning strike in pregnancy with fetal injury. Wilderness Environ Med 2016;27:287-290.
- Chan YF, Sivasamboo R. Lightning accidents in pregnancy. J Obstet Gynaecol Br Commonw 1972;79:761-762.
- Guha-Ray DK. Fetal death at term due to lightning. Am J Obstet Gynecol 1979;134:103-105.
- Weinstein L. Lightning: A rare cause of intrauterine death with maternal survival. South Med J 1979;72:632-633.
- Flannery DB, Wiles H. Follow-up of a survivor of intrauterine lightning exposure. Am J Obstet Gynecol 1982;142:238-239.
Approximately 5,000 patients present to the emergency department each year for evaluation and treatment of electrical injuries. This article will discuss the different classifications of electrical exposures and describe the recommended initial evaluation, diagnostic workup, and treatment. In addition, the authors also discuss special situations, such as lightning exposures, pediatric exposures, and electrical exposures during pregnancy.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
