Common Foot Problems
August 1, 2019
Reprints
AUTHORS
Kevin F. Sunshein, DPM, Fellow, American College of Foot and Ankle Surgeons; CEO, Sunshein Podiatry Associates, Centerville, OH
Anastasia Samouilov, DPM, Sunshein Podiatry Associates, Centerville, OH
PEER REVIEWER
Robin Lie, DPM, Sports and General Podiatry, Loma Linda, CA
EXECUTIVE SUMMARY
• Calluses and corns are abnormal thickening and hardening of the skin in areas of excessive pressure or friction.
• Warts are distinguished from calluses by appearance under magnification (absent skin lines and capillary bud formation) and pain on lateral compression.
• The American Academy of Dermatology recommends, “Don’t prescribe oral antifungal therapy for suspected nail fungus without confirmation of fungal infection” because treatment is long and potentially expensive, and the nonfungal mimics are common.
• For infected ingrown toenails, a partial or total nail avulsion is recommended.
• Plantar fasciitis typically presents with intense pain along the bottom of the heel with initial weight-bearing in the morning that usually subsides after a few steps as the plantar fascia and plantar intrinsic muscles stretch out. However, the pain frequently progresses throughout the day with prolonged weight-bearing.
• Baxter’s neuritis is misdiagnosed commonly as plantar fasciitis.
• Achilles tendinitis can occur at either the non-insertional area (middle portion of the tendon) or at the insertional area (lower portion of the tendon where it inserts into the heel).
• Metatarsalgia, capsulitis, and Morton’s neuroma are differential diagnoses of one another that often are difficult to differentiate.
• The initial X-ray of metatarsal stress fractures may be negative. In such circumstances, treatment is rest and protection, with a repeat X-ray in one to two weeks.
The foot usually does not get much respect; the hand has it beat in the prestige department. While there are specialists devoted to both body parts, hand surgeons get more acclaim than podiatrists. Remember the subplot in the Seinfeld episode “The Conversion” where Jerry and Elaine argue about whether Elaine’s podiatrist boyfriend is really a doctor. To quote Rodney Dangerfield, “no respect.” But the foot can cause mischief, and, when acting up, limit activity and function. So then, we’re glad there are specialists to help. This issue discusses some common foot conditions that, while not emergencies, may come into the emergency department (ED). In these situations, it is helpful if the emergency physician is knowledgeable and can provide the patient with appropriate directions and referral. Hope this issue is useful to you.
— J. Stephan Stapczynski, MD, Editor
Introduction
Foot problems are a common chief complaint. Patients may present to the ED when they do not have access to other sources of care or when an exacerbation becomes painful enough. Although these foot problems rarely are considered emergencies, it is useful for the emergency physician to be knowledgeable about these conditions to provide sound advice to patients and appropriate referral. They can be the first sign of more serious medical problems. The feet mirror one’s general health. Autoimmune disorders, endocrine disorders, neuropathies, and vasculopathies can present initially as symptoms in the lower extremity.
Anatomy of the Foot
The foot contains 26 bones, 33 joints, 107 ligaments, and 19 muscles.1 A basic review of foot anatomy will provide physicians with a good perspective on the foot’s complexity. The foot is divided into three different regions: forefoot, midfoot, and rearfoot. Tendons control the orientation of various joints to work together and propel the body forward.2
Pathology affecting the forefoot includes fractures, dislocations, hammertoes, and mallet toes. The forefoot has five metatarsals articulating with the proximal phalanges of each respective toe. The hallux has two phalanges and only has one interphalangeal joint. The other four toes have three phalanges with two interphalangeal joints.
Hammertoes occur at the proximal interphalangeal joints and mallet toes are contracted at the distal interphalangeal joints. This conditions result from muscle imbalances that occur both from a pronated or flat foot and from a supinated or high arched foot. The mechanism of deformity is different, but the result can appear similar. From there, contracted digits affect the distribution of pressure across the weight-bearing surface of the foot. The heads of the five metatarsal bones are weight-bearing structures, and any toe contracture will place retrograde pressure on the metatarsal heads, which often leads to painful conditions.3 These manifest in different ways, including calluses, capsulitis, and metatarsalgia. The conditions are not mutually exclusive and often present with overlapping symptoms. It is important to identify the cause of symptoms to alleviate the pain and prevent long-term progression.
The midtarsal or midfoot area is located proximally to the forefoot and is comprised of five bones: three cuneiforms, the navicular, and the cuboid bones.1 These bones contribute to the stability of the foot through coronal and transverse planes that work together during various phases of gait to absorb shock and transfer load throughout the body. The hindfoot or rearfoot consists of the talus and the calcaneus. The subtalar joint is instrumental in stabilization and is the first joint to connect the foot to the ankle.
Capsular and ligamentous structures crossing the metatarsophalangeal joints are susceptible to injury from abnormal and excessive weight bearing localized in a concentrated area. Likewise, tendon attachments are all common sites of inflammation when excessive or abnormal motion is involved. They present as Achilles tendinitis, posterior tibial tendinitis, or tendinitis of any other ankle tendon, and are not always isolated to one location. Likewise, the plantar aponeurosis is extremely susceptible to injury, usually at the medial attachment to the plantar calcaneal tuberosity.2
Common Skin Conditions of the Foot
Hyperkeratoses or calluses are abnormal thickening and hardening of the skin from excessive pressure or friction on an area of the epidermis, specifically the stratum corneum. These lesions appear to be diffuse or can be nucleated with a central core of skin embedded in the center of the lesion. This skin is avascular but may be infiltrated with nerve fibers. If the lesions are on the toes either dorsally or interdigitally, they usually are referred to as hard “corns” or heloma durum. A hard corn is usually on the dorsal aspect of the interphalangeal joints or the sides of the joints and results from pressure of a prominent joint on a shoe. Soft “corns” or heloma molle frequently are between the fourth and fifth toes in the sulcus and result from pressure between two prominent joints or a prominent bone rubbing on adjacent skin.4
Treatment of these lesions is accomplished via sharp debridement with surgical blades and topical keratolytics. It is important to understand the underlying etiology of callus and corn formation for long-term symptom relief. Appropriate counseling on shoe type usually is necessary. Accommodative padding of the digits can prevent frequent recurrence of these lesions. If conservative treatment fails, surgery is required to address the underlying bony pathology.
Excessive pressure on underlying skin can produce ulcerations from calluses, and is most commonly but not exclusively found in patients with a peripheral neuropathy. A simple flexor tenotomy can be performed to release the pressure on the toe by releasing the contracted flexor tendon and rebalancing both the intrinsic and extrinsic tendons and muscles on the toe.5 Flexor tenotomy is not effective for rigidly contracted digits, but it effectively prevents re-ulceration in flexibly contracted digits. This can be performed easily in an office or outpatient setting.
Verruca
Warts on the foot are caused by the human papillomavirus (HPV). They are the most common viral infection of the skin affecting 7% to 10% of the general population. Different viral strains produce varying wart presentations in individual areas. Verruca plantaris refers to warts located on the plantar surface of the foot. Verruca vulgaris refers to lesions on the other surfaces of the foot, including the toes. This common skin infection affects children, adolescents, and young adults, and can occur in older adults as well. Prevalence is equal in both sexes.6 Risk factors include immunosuppression, repeated trauma to the skin, swimming in public pools, use of communal showers, contact with HPV-infected individuals, and excessive sweating.6
Signs and symptoms include single or multiple papules on the skin varying in size from 2 to 20 mm. The lesions may occur as a cluster called mosaic warts. The lesions can be painful or painless to direct pressure, but oftentimes are painful on lateral compression. They may appear to be white dots or have dark spots indicating capillary infiltration. Inspection of the skin under magnification (dermoscopy) often is beneficial in determining the difference between a wart and a callus. Features that distinguish warts from calluses include absent skin lines, capillary bud formation, and pain with lateral compression. The differential diagnosis of warts on the feet includes molluscum contagiosum, seborrheic keratosis, and squamous cell carcinoma. If left untreated, warts can progress to verrucous carcinoma. Skin biopsy is the gold standard for diagnosis and is recommended for chronic warts.7
Treatment modalities are numerous and can be time-consuming, costly, and painful. Treatments include surgical excision, cryotherapy, laser ablation, immunomodulatory agents, topical keratolytics (salicylic acid), and intralesional injections (bleomycin).8 Some evidence suggests that oral cimetidine exhibits immunomodulatory activity through increased mitogen-induced lymphocyte proliferation and inhibition of T-cell function at histamine receptor sites.9 No one specific treatment works best, and many warts may be recalcitrant to any therapy. Treatment can last weeks to many months, and there is a risk of recurrence and spread.
Tinea Pedis
Tinea pedis is a common fungal infection of the foot. It is manifested as a pruritic, erythematous, scaly eruption of the foot. Depending on its location, it has three variant forms: moccasin or dry tinea pedis (the most common variant), interdigital, and vesiculobullous type. The most common tinea pedis infections are caused by dermatophytic fungi including Trichophyton spp. and Epidermophyton spp.10
Tinea pedis occurs in moist environments, most commonly due to occlusive shoe gear. Often, it occurs with coexistent atopic dermatitis or allergic eczema. Tinea pedis usually responds to regular application of topical antifungal medications, such as ciclopirox, terbinafine, econazole, or ketoconazole creams. There is a high risk of recurrence. A comprehensive treatment plan includes treating the environment in which fungus is found to prevent self-inoculation.
The most common treatment for tinea pedis is a topical medication. The two main groups of antifungal therapy are azole and allylamine medications. Azoles are fungistatic and include ketoconazole and clotrimazole. Allylamines are fungicidal and include naftifine and terbinafine. The advantage of using an allylamine is the duration of treatment is shorter.
Onychomycosis
Tinea unguium (onychomycosis) is a fungal infection on the matrix, plate, or nail bed commonly associated with tinea pedis. The typical presentation of fungal infected nails includes abnormal thickening with lysis; yellow, white, or brown discoloration; malodor; and hyperkeratosis of the underlying nail bed. The most common cause is a dermatophyte. Non-dermatophyte molds and Candida species are less common. Onychomycosis is more prevalent in older populations, and men are affected more commonly than women.11 Toenails are involved more frequently than fingernails.11 (See Table 1.)
Table 1. Common Foot Complaints |
||
|
Condition |
Definition |
Symptoms |
|
Onychomycosis |
|
|
|
Onychocryptosis |
|
|
|
Plantar fasciitis |
|
|
|
Baxter’s neuritis |
|
|
|
Achilles tendinitis |
|
|
|
Stress fractures |
|
|
Common mimics of onychomycosis include chronic trauma and psoriasis. Repeated sudden-stop trauma associated with basketball, soccer, and tennis can produce dystrophic toenails. Onychomycosis and trauma-related dystrophy most commonly affect the great toe, but when only the little toe is involved, it is likely related to trauma.
As part of the Choosing Wisely Campaign, the American Academy of Dermatology recommends, “Don’t prescribe oral antifungal therapy for suspected nail fungus without confirmation of fungal infection,” because treatment is long and potentially expensive, and the nonfungal mimics are common. If multiple toenails are involved or there is accompanying tinea pedis, treatment without confirmation of a fungal infection may be considered. The most accurate diagnostic test for onychomycosis is the Periodic acid-Schiff stain, performed by placing toenail clippings in 10% formalin and sending to the laboratory. Potassium hydroxide preparation has variable accuracy, while fungal culture has low sensitivity but good specificity.
Treatment for onychomycosis involves long courses (three to six months) with high failure rates and common recurrences. Treatment is optional but often is desired by adolescents and young adults for cosmetic appearance or discomfort from shoes. Topical therapy is usually ineffective, but for patients who decline oral systemic treatment, ciclopirox nail lacquer can be offered along with caution about the low cure rate. Assessment of cure takes nine to 12 months because toenails grow slowly.
The most effective treatment of onychomycosis is an oral antifungal agent, such as terbinafine or itraconazole.12 The duration of treatment usually is 90 days either with daily intake or through pulse dosing. Concomitant use of topical antifungal medication for long duration may prevent recurrences, although there is a high recurrence rate.
Onychocryptosis (Ingrown Toenails)
Ingrown toenails are the most common nail problem.13 Ingrown toenails occur from improper trimming, tight or ill-fitting shoes, blunt trauma, repetitive trauma sustained especially by athletes, and hereditary nail shapes such as pincer nails with increased, transverse over-curvature. They occur most commonly in those 15 to 40 years of age, but patients of all ages can experience this condition. Studies are conflicting regarding the incidence in males vs. females.13
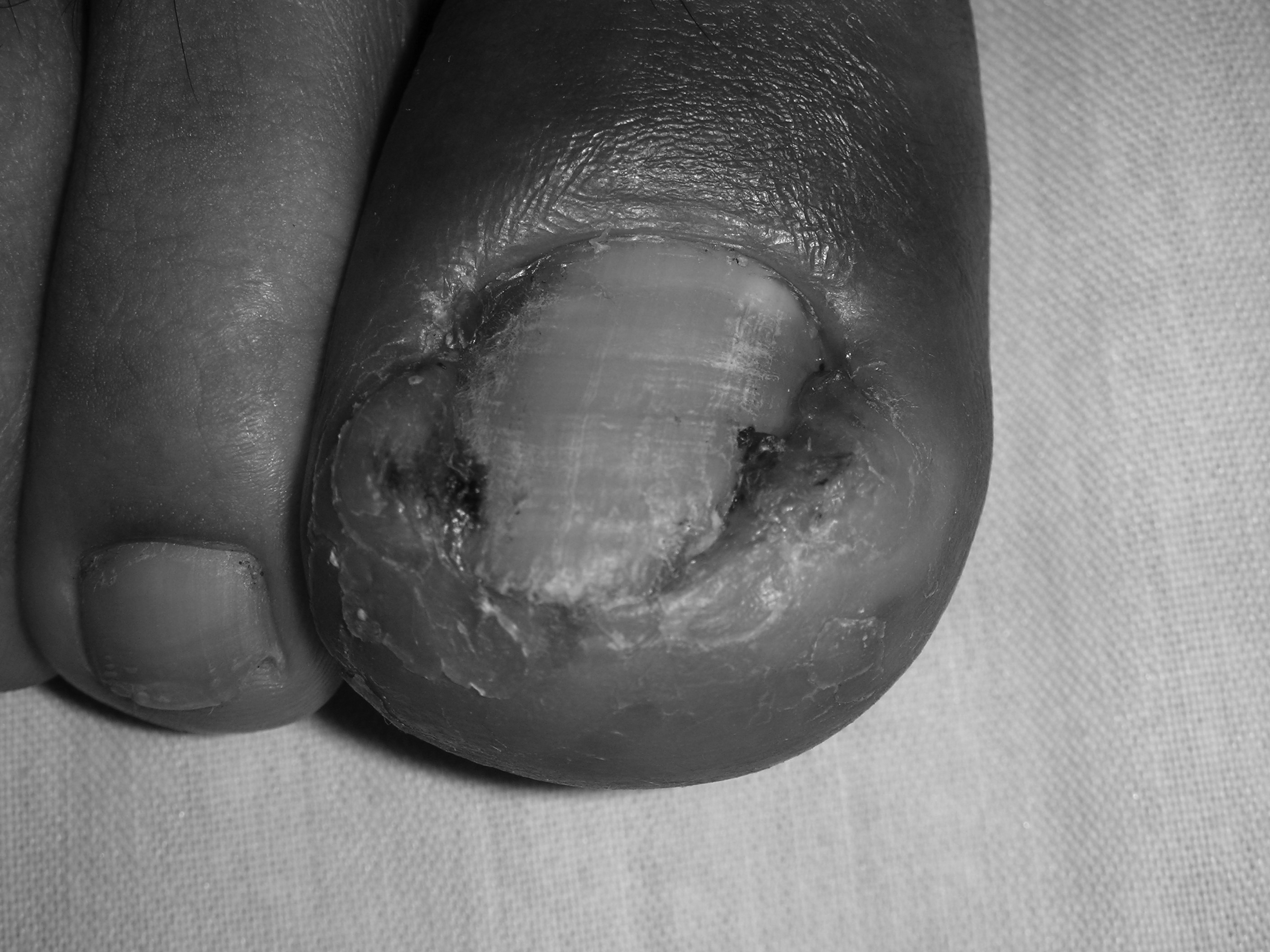
Ingrown toenails can be infected or non-infected, and occur most frequently in the great toes. The usual presentation is progressive pain along the medial or lateral nail border with periungual inflammation and edema. In later stages, purulent discharge and formation of granulation tissue is noted. (See Figure 1.)
Figure 1. Ingrown Toenail |
 |
|
Image courtesy of J. Stephan Stapczynski, MD |
In the early presentation, cutting the distal offending nail border may relieve pain, but more progressive conditions require surgical excision of the offending nail border under a local anesthetic. If the nail is not infected, a permanent partial nail resection (partial matricectomy) can be performed to prevent recurrence of the ingrown toenail. Typically, destruction of the nail root is performed using 85% phenol or 10% sodium hydroxide. Other surgical methods are available, but chemical matricectomy is one of the easiest and most economical procedures.14
In the presence of severe periungual inflammation and drainage, oral antibiotics can alleviate clinical signs of infection but seldom cure this problem, as an ingrown toenail is a foreign body reaction. Staphylococcus aureus is the most common pathogen causing paronychial infections.13,14
A partial or total nail avulsion is recommended in this situation. This procedure does not destroy the nail root. Under local anesthesia, the offending border is split back under the hyponychium with a nail splitter, and the nail spicule is removed from the soft tissue borders. Any granulation tissue present is sharply excised. A compression dressing is applied and changed daily until the infection and inflammation have resolved, usually within 48 to 72 hours. Epsom salt foot soaks twice daily for 10 to 15 minutes will help resolve the inflammation. Postsurgical oral antibiotics are indicated depending on the severity of the inflammation of the affected area.
Heel Pain
Up to 15% of all foot complaints are related to heel pain.15 Plantar fasciitis is defined as inflammation of the plantar fascial tissue at the plantar aspect of the heel, and is characterized by intense pain localized to the inferior portion of the calcaneus, most commonly along the plantar medial tuberosity. Any portion of the plantar fascia can be affected. The plantar fascia is a thick, broad, and dense band of longitudinally arranged collagen fibers that begins as an attachment to the anterior aspect of the calcaneal tuberosity.16 The plantar fascia is divided into three bands: medial, central, and lateral. Heel spur formation has been associated with the proximal plantar fascia, but the spur actually is deep to the plantar fascia and lies within the origin of the flexor digitorum brevis muscle. Most often, heel spurs exist without producing symptoms, although in some selected patients, heel spurs may become a source of symptoms.17 (See Figures 2 and 3.)
Figure 2. Image Showing Plantar and Posterior Spur |
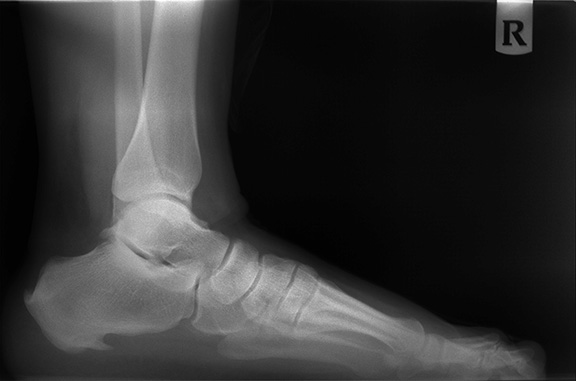 |
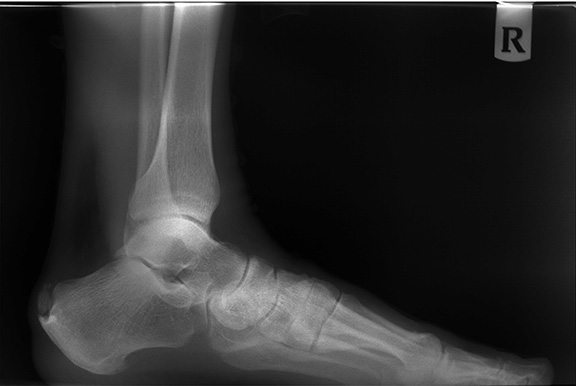
Figure 3. Image Showing Posterior Spur |
 |
Conventional plantar fasciitis is consistent in its initial presentation. Signs and symptoms include intense pain along the bottom of the heel with initial weight-bearing in the morning, commonly referred to as post-static dyskinesia.16 The pain typically subsides after a few steps, until the plantar fascia and plantar intrinsic muscles stretch out, but the pain frequently progresses throughout the day with prolonged weight-bearing. In severe cases, associated signs and symptoms include heel edema and thickening of the plantar heel pad. Plantar fasciitis can progress to complete or partial rupture of the plantar fascia. Chronic or recalcitrant plantar fasciitis may be confused with plantar fasciosis, which is a natural thickening and age-related degenerative process of the plantar fascia.
Initial treatment should focus on alleviating the pain and attempting to neutralize the cause. More than 90% of patients with plantar fasciitis can be treated conservatively.15 Nonsteroidal anti-inflammatory drugs or oral corticosteroid medications alleviate the intense pain initially, but do not prevent recurrence if the underlying etiology is left untreated. Corticosteroid injections may be used at the insertion point of the plantar fascia, but caution should be used because multiple injections in a short time period have been associated with rupture. Effective conservative treatment options include supporting the foot with over-the-counter arch supports and night splints.
Foot gear is a very important feature of treating any heel pain disorder. A raised heel with a stiffer sole shoe will offload the weight from the plantar surface of the foot. Calf stretches and strengthening exercises are beneficial in alleviating pressure from the plantar fascia by reducing tension of the Achilles tendon. Custom foot orthotics are the most effective in addressing the biomechanical faults in patients’ feet and there is a lot of variability in both orthotic material and quality. There are many different casting techniques to mold a foot orthotic, with little agreement on which method is optimal. Recent studies have looked at the efficacy between over-the-counter arch supports and custom foot supports and relate no significant difference. Most of these studies do not address the prescription elements that the researchers used nor the biomechanical variances in their patient population. Despite these studies, investigators have had overwhelming success in treating not only heel disorders, but any other foot disorder that is related to biomechanics instability.
Baxter’s Neuritis
Baxter’s neuritis is an entrapment neuropathy of the first branch of the lateral plantar nerve.18 Baxter’s neuritis commonly is misdiagnosed as a differential of plantar fasciitis. Differences in presentation include pain after activity vs. on initial weight bearing as seen in plantar fasciitis. A common presentation is pain with increased activity, a bulky abductor hallucis muscle on physical exam, paresthesias, and pain that is sharp, shooting, and reproducible with palpation along the medial heel as opposed to the plantar medial heel. Edema is not associated with this condition.
Conservative treatment is much the same as with plantar fasciitis, but if conservative care fails, then surgical decompression of the nerve is the procedure of choice.
Retrocalcaneal Heel Pain
Retrocalcaneal exostoses occur at the insertion of the Achilles tendon and often are associated with intratendinous calcifications. Conservative treatment includes many of the same treatment options as with plantar fasciitis with the exception of corticosteroid injections, which never should be attempted because of the high risk of tendon rupture. As with plantar heel pain, posterior heel pain usually responds to conservative therapies. If conservative care fails, detachment of the insertion of the Achilles tendon and exostectomy with debridement and repair of the tendon is required.19
Haglund deformity (pump bump) is a painful bony prominence at the posterior superior or posterior superior lateral aspect of the calcaneus above the attachment of the Achilles tendon. This condition is more common in females and the pain is caused from an impingement of the Achilles tendon over the posterior superior aspect of the calcaneus. This impingement may be related to an enlarged bony prominence or from a high calcaneal inclination angle. Conservative care includes heel lifts, nonsteroidal anti-inflammatory agents, orthotics, and physical therapy. Surgical options include excision of the bony prominence and removal of any inflamed bursa or a calcaneal osteotomy to advance the posterior portion of the calcaneus to offload the Achilles tendon insertion.20
Achilles Tendinitis
Achilles tendon injuries are among the three most frequent sports-related injuries of the foot and ankle. Injuries of the Achilles tendon are classified by anatomical location occurring at either the non-insertional area (middle portion of the tendon) or at the insertional area (lower portion of the tendon where it inserts into the heel).19,20
Achilles tendinitis affecting the non-insertional area is characterized by pain to palpation, localized edema, and increased warmth. Chronic thickening of the distal Achilles tendon in a fusiform pattern may represent tendinosis or degeneration of the tendon. Initial treatment for acute Achilles tendinitis should begin with RICE (rest, ice, compression, elevation) and nonsteroidal anti-inflammatory medications. Adding a one-fourth inch heel lift can alleviate tension on the tendon. Any abnormal biomechanical instability of the foot may be addressed with good supportive shoes and a semi-rigid over-the-counter orthotic device. Physical therapy modalities may be used for recalcitrant injuries. Chronic Achilles tendinosis may require surgical debridement and immobilization if all conservative treatment fails.20
Acute Achilles bursitis (also known as retrocalcaneal bursitis) affects the insertion point of the tendon and is diagnosed on physical exam by pain on squeezing the tendon at its most distal point. The pain is usually anterior to the tendon insertion point, as the bursa is located between the Achilles tendon and the calcaneus. Treatment is the same as for the non-insertional type.
Hallux Limitus and Hallux Rigidus
Hallux limitus is a condition in which there is limited dorsiflexion of the first metatarsal phalangeal joint to typically less than 20 degrees. Hallux rigidus is the end stage of hallux limitus when the joint undergoes degenerative changes. Common presenting symptoms include pain with limited range of motion. Hallux limitus has many causes, and multiple factors influence the loss of motion in the joint. Some causes include acute trauma, arthritis of the sesamoids, abnormal subtalar joint pronation, long first metatarsal, long proximal phalanx of the great toe, metatarsus primus elevatus, square first metatarsal head, and impingement of the sesamoid apparatus and flexor hallucis longus tendon in the retromalleolar region.
Hallux rigidus is the second most frequent site of arthrosis, after the knee.23 There are few or no preventive measures readily available. Symptomatic treatment includes offloading the first metatarsal phalangeal joint and limiting abnormal biomechanical forces with foot orthotics, shoe modifications including a stiffer sole shoe or one with a rocker bottom, nonsteroidal anti-inflammatory medications, short-acting corticosteroid intra-articular injections, and physical therapy. Surgeries include cheilectomy or debridement of the first metatarsal phalangeal joint of ankylosed bone, implant arthroplasty, and various osteotomies of the proximal phalanx or first metatarsal to decompress the joint. Salvage procedures include arthrodesis of the first metatarsal phalangeal joint. Early detection and diagnosis is paramount to limiting the progression of this disorder.
Hammertoes
Typical deformities affecting the lesser toes include hammertoe and claw toe deformities. These deformities are reported in the literature to affect 20% of the population.24 Surgeries for these deformities are among the most commonly performed procedures in foot and ankle practices.
Claw toe deformity is characterized by dorsiflexion of the metatarsophalangeal joint and plantar flexion of the proximal interphalangeal joint and distal interphalangeal joint. Similarly, hammertoe deformity is characterized by dorsiflexion of the metatarsophalangeal joint and plantar flexion of the proximal interphalangeal joint but dorsiflexion of the distal interphalangeal joint.
Clinically, the metatarsophalangeal joint dorsiflexion causes the head of the proximal phalanx to push against the internal surface of shoes, exerting abnormal pressures on the head of the proximal phalanx. Abnormal contractures at the proximal interphalangeal and distal interphalangeal joints cause abnormal skin irritation, creating painful hyperkeratoses, nail disorders, and ulcerations.
Conventional conservative care includes sharp debridement of the clavus along with accommodative padding, larger shoes, or a change in shoes to ones with a deeper toe box. Caustic callus removers should be discouraged because of the potential for severe skin burns, especially in the neuropathic foot. If the digital deformities are flexible and there are signs of abnormal foot mechanics, foot orthotics may be beneficial.24
Complex hammertoe deformities exhibit biplane instability with dorsiflexion of the toe and either adduction or abduction at the metatarsophalangeal joint. If this occurs in the second toe, it typically is referred to as a classic overlapping toe. It can present with a hallux valgus deformity. This is a much more difficult type of hammertoe to treat surgically.25
In advanced digital deformities, surgery often is indicated with either resectional arthroplasty of the affected proximal interphalangeal joint and distal interphalangeal joint. Arthrodesis of the proximal interphalangeal joint is used as a more stabilizing procedure. In the case of painful, semi-rigid hammertoes or toes with distal hyperkeratoses that exhibit potential ulceration, a simple flexor tenotomy may be beneficial for relieving pressure from the distal end of the toe. This is especially useful in neuropathic patients with digital deformities to prevent recurrent ulcerations.26
Metatarsalgia, Capsulitis, and Morton’s Neuroma
Metatarsalgia, capsulitis, and Morton’s neuroma are grouped together because they usually are differential diagnoses of one another. These three conditions are harder to differentiate, and the history and physical exam are critical in proper diagnosis.27
Metatarsalgia is a nonspecific term used to describe pain along the plantar aspect of the lesser metatarsal heads. Increased and uneven pressure under the metatarsal heads is thought to be the causative factor. Lesser metatarsal overload is thought to lead to a variety of pathologies, ranging from isolated metatarsal pain to complete dislocation of the metatarsophalangeal joint. Initial plantar metatarsal head pain may be a precursor to dislocation of the metatarsophalangeal joint.
Capsulitis or metatarsophalangeal joint synovitis of the lesser metatarsal heads is characterized by localized edema and inflammation plantarly; however, there may be periarticular edema noted dorsally. A less common differential diagnosis in this case may represent early osteochondrosis of the metatarsal head.
Morton’s neuroma is a painful condition that affects the intermetatarsal spaces. Typically, it affects the second or third intermetatarsal spaces. Its cause is the subject of debate. Currently, pathophysiology is thought to be from either a degenerative process or damage to the common digital nerve resulting from ischemia. Symptoms in its early stages present similarly to metatarsalgia. A positive Mulder’s sign (clicking with lateral compression of the forefoot) is not always present and is not pathognomonic for this condition, although it is present in a large number of cases.
The key physical finding in Morton’s neuroma is pain with palpation of the affected intermetatarsal space. Usually, there is no pain on palpation of the metatarsal head. Deliberate and thorough palpation of the forefoot is critical in diagnosing this condition. Typically, this condition worsens with wearing shoes, and removing shoes relieves the pain. Symptoms commonly are described as a burning or stabbing radiating pain to the toes. Radiographic evaluation of the foot is necessary to assess any early signs of metatarsophalangeal subluxations or contractures.
The most common ways to treat these conditions are with metatarsal padding and foot orthotics. Intra- or periarticular corticosteroid injections can exacerbate these conditions by causing rupture of the periarticular capsular ligaments. Although corticosteroid injections may relieve neuroma symptoms, they therefore should be used judiciously and infrequently. Oral anti-inflammatory medications have limited efficacy in treating neuromas but can be quite useful for capsulitis or metatarsalgia. Wider shoes play a significant role in treating interdigital neuromas.
Metatarsal Stress Fractures
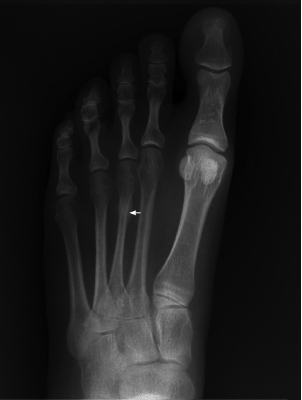
The most frequent location of stress fractures in the foot is in the metatarsals.28 (See Figure 4.) The second and third metatarsals are affected the most along the distal shaft and neck region of the metatarsal bone. Stress fractures result from a sudden increase in physical activity or from repetitive stress on the affected area. Initial signs and symptoms are pain, localized edema, and sometimes an increase in warmth and localized redness along the dorsal distal part of the foot.
Figure 4. Stress Fracture of the Third Metatarsal Shaft |
 |
Initial X-rays may be negative, and it may take several weeks to see the callus formation at the fracture site on subsequent X-rays. If initial X-rays are negative, which is common, applying a tuning fork to the appropriate metatarsal will be painful to the patient, indicating movement in the cortical margins of the bone. This is a good indicator that the patient has a stress fracture.29 However, if in doubt, an MRI or technetium Tc 99 bone scan may be performed to help in the diagnosis.
Treatment consists of the PRICE protocol (protection, rest, ice, compression, elevation) through offloading in either a very stiff-soled athletic shoe or surgical shoe. The fracture usually will heal in six to eight weeks, and physical activities should be moderated until symptoms abate.
Conclusion
Many foot problems can be averted with proper shoe gear and patient education. Foot type and biomechanical instability are the root causes of many foot and ankle problems. Even proximal joint pain and lower back pain can be improved if the foot is evaluated for any structural instability. The foot is the foundation for the rest of the body, and proper and timely diagnosis can alleviate a lifetime of problems.
REFERENCES
- Netter FN. Section 8: Lower Limb Ankle and Foot. In: Atlas of Human Anatomy. Philadelphia: Elsevier; 2018: 515-528.
- Root ML, Weed JH, Orien WP. Normal and Abnormal Function of the Foot. Clinical Biomechanics. Clinical Biomechanics Corp. 1977.
- Myerson MS, Shereff MJ. The pathological anatomy of claw and hammer toes. J Bone Joint Surg Am 1989;71:45-49.
- Bonavilla EJ. Histopathology of the heloma durum: Some significant features and their implications. J Am Podiatry Assoc 1968;58:423-427.
- Laborde JM. Neuropathic toe ulcers treated with toe flexor tenotomies. Foot Ankle Int 2007;28:1160-1164.
- Witchey DJ, Witchey NB, Roth-Kauffman MM, Kauffman MK. Plantar warts: Epidemiology, pathophysiology, and clinical management. J Am Osteopath Assoc 2018;118:92-105.
- Wright PK, Vidyadharan R, Jose RM, Rao GS. Plantar verrucous carcinoma continues to be mistaken for verruca vulgaris. Plast Reconstr Surg 2004;113:1101-1103.
- Chen J, Wu Y. Local Treatments for Cutaneous Warts. In: Williams HC, Bigby M, Herxheimer MB, et al, eds. Evidence-Based Dermatology. Hoboken, NJ: John Wiley & Sons; 2014: 320-328.
- Ronna T, Lebwohl M. Cimetidine therapy for plantar warts. J Am Podiatr Med Assoc 1995;85:717-718.
- Leyden JL. Tinea pedis pathophysiology and treatment. J Am Acad Dermatol 1994;31(3 Pt 2):S31-S33.
- Scher RK, Rich P, Pariser D, Elewski B. The epidemiology, etiology, and pathophysiology of onychomycosis. Semin Cutan Med Surg 2013;32(2 Suppl 1):S2-S4.
- Lipner SR, Scher RK. Onychomycosis: Treatment and prevention of recurrence. J Am Acad Dermatol 2018;80:853-867.
- Haneke E. Controversies in the treatment of ingrown nails. Dermatol Res Pract 2012;2012:783924.
- Espensen EH, Nixon BP, Armstrong DG. Chemical matrixectomy for ingrown toenails. J Am Podiatr Med Assoc 2002;92:287-295.
- Crawford F, Thomson C. Interventions for treating plantar heel pain. Cochrane Database Syst Rev 2003;CD000416.
- The Podiatry Institute; Southerland J, Alder D, Boberg J, et al, eds. McGlamry’s Comprehensive Textbook of Foot and Ankle Surgery. Philadelphia: Wolters Kluwer Health/Lippincott Williams & Wilkins; 2013: 494.
- Johal KS, Milner SA. Plantar fasciitis and the calcaneal spur: Fact or fiction? Foot Ankle Surg 2012;18:39-41.
- Schon LC, Glennon TP, Baxter DE. Heel pain syndrome: Electrodiagnostic support for nerve entrapment. Foot Ankle 1993;14:129-135.
- Rufai A, Ralphs JR, Benjamin M. Structure and histopathology of the insertional region of the human Achilles tendon. J Orthop Res 1995;13:585-593.
- Gould JS. Chapter 33: Haglund Deformity, Retrocalcaneal Bursitis and “Pump Bumps.” In: The Handbook of Foot and Ankle Surgery: An Intellectual Approach to Complex Problems. New Delhi: Jaypee Brothers Medical Publishers (P) Ltd.; 2013: 205-207.
- Chang TJ. Master Techniques in Podiatric Surgery: The Foot and Ankle. Philadelphia: Lippincott Williams & Wilkins; 2005.
- Nix S, Smith M, Vicenzino B. Prevalence of hallux valgus in the general population: A systematic review and meta-analysis. J Foot Ankle Res 2010;3:21.
- Coughlin MJ, Shurnas PS. Hallux rigidus: Demographics, etiology, and radiographic assessment. Foot Ankle Int 2003;24:731-743.
- Schuberth JM. Hammer toe syndrome. J Foot Ankle Surg 1999;38:166-178. doi:10.1016/s1067-2516(99)80032-5.
- Coughlin MJ. Lesser-toe abnormalities. J Bone Joint Surg 2002;84:1446-1469.
- Laborde JM. Neuropathic toe ulcers treated with toe flexor tenotomies. Foot Ankle Int 2007;28:1160-1164.
- Thomas JL, Blitch EL IV, Chaney DM, et al. Diagnosis and treatment of forefoot disorders. Section 2. Central metatarsalgia. J Foot Ankle Surg 2009;48:239-250.
- Thomas JL, Blitch EL IV, Chaney DM, et al. Diagnosis and treatment of forefoot disorders. Section 5. Trauma. J Foot Ankle Surg 2009;48:264-272.
- Schneiders AG, Sullivan SJ, Hendrick PA, et al. The ability of clinical tests to diagnose stress fractures: A systematic review and meta-analysis. J Orthop Sports Phys Ther 2012;42:760-771.
Foot problems are a common chief complaint. Patients may present to the ED when they do not have access to other sources of care or when an exacerbation becomes painful enough. Although these foot problems rarely are considered emergencies, it is useful for the emergency physician to be knowledgeable about these conditions to provide sound advice to patients and appropriate referral.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
