Evaluation and Management of Anaphylaxis in the Emergency Department
August 15, 2019
Reprints
AUTHORS
Kyley J. Wyss, MD, Resident, Department of Emergency Medicine, Wright State University, Boonshoft School of Medicine, Kettering, OH
Derek M. Sorensen, MD, FACEP, Assistant Professor, Departments of Emergency Medicine and Surgery, Wright State University, Boonshoft School of Medicine, Kettering, OH
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Assistant Clinical Professor of Emergency Medicine, Mt. Sinai, New York City
EXECUTIVE SUMMARY
• Anaphylaxis is a reaction to a trigger substance that leads to urticaria (90%), hypotension, bronchospasm, and laryngospasm. A large number of substances can be the trigger, but in about half the cases, no trigger can be identified. Food is the most common trigger, with peanuts, tree nuts, milk, and shrimp being the most common. While nearly all patients will have cutaneous signs, about 10% will not.
• Delay in administration of epinephrine is associated with death and biphasic reactions. It is now recommended that epinephrine is given intramuscularly. Intravenous epinephrine is reserved for patients who are refractory to many doses of intramuscular epinephrine (usually defined as three doses) or when the patient has cardiovascular collapse. Patients who remain refractory should have an epinephrine drip started.
• Angioedema is one of the presentations of an allergic reaction. However, angioedema also can be caused by ACE inhibitors. These drugs induce angioedema through bradykinin, which generally is not responsive to epinephrine. In addition, patients with hereditary angioedema have their reaction through complement and, in general, are not helped by epinephrine.
• Patients who are on beta-blockers and have anaphylaxis may be refractory to epinephrine. In such patients, glucagon may be beneficial.
Introduction
For emergency physicians, anaphylaxis can be a challenging diagnosis to make. International guidelines have been left intentionally vague because of the range of presentations that may occur with anaphylaxis. Unfortunately, the diverse manifestations of life-threatening anaphylaxis often lead to delays in life-saving treatment because there is not a specific set of criteria for diagnosis. The current knowledge gap is a major issue for patients, emergency providers, and the medical community at large.
Of course, anaphylaxis is not the only end of the hypersensitivity spectrum encountered in the emergency department (ED). Particularly if this is the first time the patient has had an anaphylactic reaction, he or she may not present with a chief complaint of an “allergic reaction.” This article also will discuss the often-uncertain treatment decisions that come with a presentation of urticaria or angioedema.
This article will present the most current information for diagnosing allergic reactions and anaphylaxis, and how to treat them properly. The diagnostic criteria for anaphylaxis, let alone the best course of treatment, are highly debated topics that require further research.
Epidemiology
The worldwide incidence of anaphylaxis is increasing.1 At least 1.6% of the population in North America will have an anaphylactic reaction in their lifetime, with a lifetime prevalence of 0.5-2.0% worldwide.2,3 The reason for the increase is not known precisely, but food allergy prevalence in North America is increasing more rapidly than in European countries.1 In the United States, the rate of anaphylaxis increased by 101% between 2005 and 2014.4 This increase was largest in children ages 5-17 years.4 It should be noted that due to the difficulty in correctly diagnosing anaphylaxis, epidemiological studies are often faulty.
Most cases of anaphylaxis are caused by exposure to an unknown trigger (57%). Identification of the trigger may take time and some detective work, especially in the case of food allergies. The most common identified triggers are food (27%), medications (12%), and insect venom (4%).4 (See Table 1.) Adults tend to have a more severe presentation than children, with features including hypotension and respiratory distress.5 Adults also are hospitalized after an anaphylactic reaction more frequently than children.4 Infants and toddlers who are unable to verbalize their symptoms often are treated less aggressively than older children.6
Mortality from food-induced anaphylaxis is rare, with 31 fatalities reported to a comprehensive registry maintained by members of the American Academy of Allergy, Asthma & Immunology (AAAAI) and the Food Allergy and Anaphylaxis Network between 2001-2006.7 In this registry, deaths from a high suspicion of anaphylaxis from a food allergen were more prevalent in males (61%) and in adolescents and young adults.7,8 Most patients had a known history of food allergies and asthma.7 In a study of drug-induced anaphylaxis, older patients with more cardiovascular comorbidities had a higher rate of fatal anaphylaxis reactions.8 Most deaths were associated with prolonged time from the start of the reaction to epinephrine administration.7
There seems to be a predilection for anaphylactic reactions in those with a medical history of asthma and eczema.9 Although the rate of fatal drug-induced anaphylaxis is on the rise, food- and venom-induced anaphylaxis rates are stable.8
Table 1. Most Common Triggers of Anaphylaxis |
|
Etiology
The most common identified triggers for anaphylaxis are foods, medications, insect stings, and allergen immunotherapy.10 (See Table 1.) In both adults and children, food is the most common trigger for anaphylaxis.5 Overall, studied risk factors for anaphylaxis in general include exercise, alcohol use, nonsteroidal anti-inflammatory drug (NSAID) use, acute infections, stress, and perimenstrual status.8 These factors are associated with anaphylaxis at highly variable rates among different studies. Still, about 20% of cases of anaphylaxis are idiopathic.11
Foods are the most common triggers for anaphylaxis, and are also the most common triggers for anaphylaxis resulting in death. The most common food triggers are peanuts, tree nuts, milk, and shrimp.7 Other common food allergens include soy, chickpeas, bananas, nectarines, wheat, eggs, and seeds.10 (See Table 2.) However, any food, seasoning, or spice can trigger an anaphylactic reaction. Patients can acquire an allergy to beef from a tick bite of the Lone Star tick. As our diet consists increasingly of store-bought over home-prepared food, it is more likely for those with known allergies to be exposed to their allergens in their homes than ever before.
Table 2. Common Food Allergens |
|
Any drug can lead to an allergic reaction. The most common drugs that cause allergic reactions are beta-lactam antibiotics, salicylates, sulfa drugs, vancomycin, and NSAIDs.10 (See Table 3.) Deaths were most frequently associated with beta-lactam and cephalosporin antibiotics, general anesthetics (namely neuromuscular-blocking agents), and radiocontrast agents.8
Table 3. Common Drugs That Cause Allergic Reactions |
|
The healthcare system predisposes patients to some other common allergens, such as latex, vaccines, radiographic contrast material, and blood products.10 Other common allergens include hymenoptera stings (i.e., bee and wasp stings), insect parts (i.e., ingested bugs, tick heads), mosquito bites, and molds.
Anaphylaxis to venom has a predilection to occur in men, typically of white race.8 Most deaths associated with venom anaphylaxis have occurred after honeybee stings,8 but insect parts, such as ingested insects, tick heads left under the skin after improper removal, or mosquito bites, also can present a risk for allergic reaction or anaphylaxis.
Exercise-induced anaphylaxis is a disorder in which individuals develop hypersensitivity with exercise.12 In 30-50% of cases, the reaction is food-dependent and occurs with a combination of certain foods and exercise.12 One theory is that exercise may increase absorption of certain food allergens through increased intestinal permeability.8 It also has been reported in combination with medications (namely NSAIDs), extreme temperatures, menstrual cycles, and environmental allergens.12 Anaphylaxis in the setting of exercise has been found to be as prevalent as milk allergy in some prospective studies.13
Pathophysiology
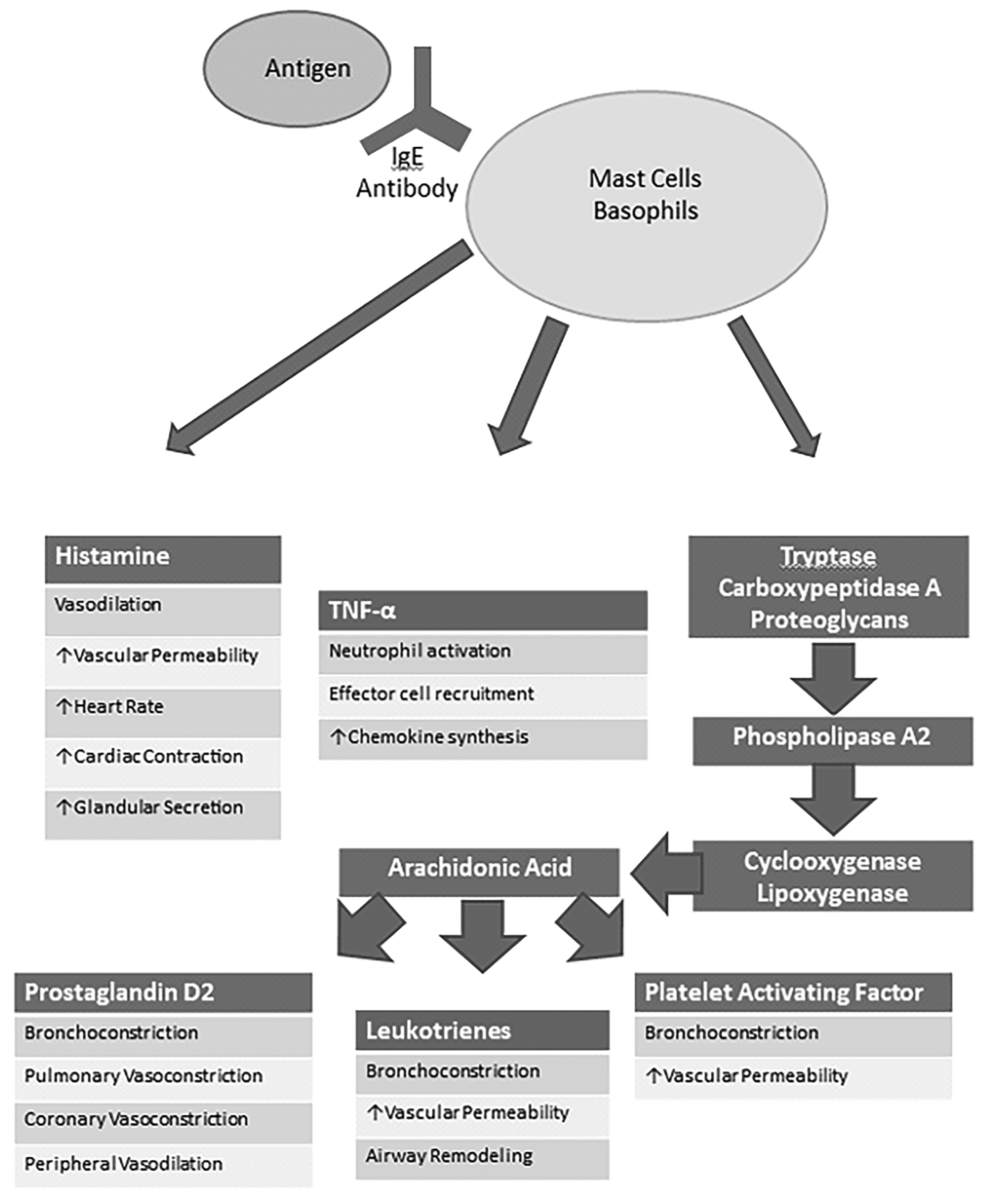
The body’s inappropriate response to a harmless antigen is referred to as hypersensitivity.10 Any agent that can produce a sudden degranulation of mast cells or basophils can induce anaphylaxis.10 The resulting symptoms are manifested in organ systems with high expressions of mast cells, namely the cutaneous, respiratory, cardiovascular, and gastrointestinal systems.11 (See Figure 1.)
In the gastrointestinal tract, mast cells coated with immunoglobulin E (IgE) are the chief mediators of food protein allergic reactions.10 There are non-IgE-mediated inflammatory reactions mediated by allergen-specific lymphocytes, such as in allergic contact dermatitis, as well as immunoglobulin G (IgG) antibodies such as in serum sickness.14
Figure 1. The Pathophysiology of Anaphylactic Reactions10 |
 |
|
Source: Rowe BH, Gaeta TJ. Anaphylaxis, allergies, and angioedema. In: Tintinalli JE, Stapczynski J, Ma O, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016. |
Angioedema is the acute onset of asymmetrical, nonpitting swelling of the skin, mucous membranes, or both.15 It typically involves the upper airway and digestive tract, but is not limited to these areas.15 It may be allergic and follows a similar pathological pathway as discussed earlier. Angioedema has become a well-known complication of angiotensin converting-enzyme (ACE) inhibitor medication use, occurring in 0.1-0.7% of patients taking ACE inhibitors, predominantly in African Americans.10 Hereditary angioedema can present in a similar manner, but the underlying cause is different. In these cases, the pathophysiology of angioedema is mediated by bradykinin, which will not be discussed here. A large portion of cases of angioedema are associated with ACE inhibitor use, which may account for this reaction typically appearing in an older age group than anaphylaxis.15
Clinical Features
Patients presenting with an allergic reaction can range from those with no or mild symptoms to those who arrive in extremis. Although it is recognized that systemic hypersensitivity reactions occur with a spectrum of severity, there has not been a well-studied classification system developed for the ED provider to aid in decision making.16 This makes allergic reactions difficult to recognize, report, and study. It is difficult to develop uniform treatment action plans for these rare events.
Urticaria and diffuse erythema are easily recognized early manifestations of an allergic reaction. However, 10% of patients will not develop any cutaneous signs, making the diagnosis more difficult and potentially missed. Only about half of health professionals could correctly identify anaphylaxis in one study.17,18
The presenting symptoms of anaphylaxis are varied. The clinical criteria for anaphylaxis are as follows:
Urticaria, generalized itching or flushing, or edema of the lips, tongue, uvula, or skin developing over minutes to hours and associated with at least one of the following:
- respiratory distress or hypoxia;
- hypotension or cardiovascular collapse; or
- associated symptoms of organ dysfunction (i.e., hypotonia, syncope, incontinence).
Two or more signs or symptoms that occur minutes to hours after allergen exposure, including:
- skin or mucosal involvement;
- respiratory compromise;
- hypotension; or
- persistent gastrointestinal cramps or vomiting. (See Table 4.)
Consider anaphylaxis with known allergen exposure and developing hypotension.10
A history may or may not be available. Ideally, a known exposure will have occurred to a known allergen at a known time. However, in most cases, a specific allergen is not found.4
Urticaria is a cutaneous hypersensitivity reaction to an allergen, and may be found both as one of a constellation of symptoms in anaphylaxis or as a single symptom with its own diagnosis. Angioedema, while certainly concerning for its impact on the patient’s ability to breathe, is not in itself anaphylaxis, but rather a mucocutaneous hypersensitivity reaction, usually of the upper airway.
Table 4. Clinical Signs of Anaphylaxis10 |
|
One of the following:
PLUS
Two or more signs or symptoms occurring minutes to hours after allergen exposure, including:
|
Diagnostic Studies
There are no specific diagnostic studies required to diagnose an allergic reaction, but physicians may choose to order indicated studies if the diagnosis is unclear. Elevations in tryptase and histamine levels may be present in the blood, but clinical utility for these studies remains poor.19 Testing for antigen sensitivity should be performed in the outpatient setting by an allergist after the initial anaphylactic reaction.20
Differential Diagnoses
Given the often vague presenting symptoms of allergic reactions and anaphylaxis, a broad differential is a good approach when considering the treatment and stabilization of the patient with suspected anaphylaxis. Vasovagal syncope is the most common presentation that can imitate the symptoms of anaphylaxis.20 Patients may present with symptoms similar to acute coronary syndrome, arrhythmia, airway obstruction or epiglottitis, seizures, and many other possibilities.10 Because patients present with sudden shortness of breath, pulmonary embolism may be considered. Especially when there is no historical information or a history of an inciting event, it is important not to anchor on anaphylaxis while keeping in mind that early intervention is extremely important in its management.
Management
Stabilization of the patient in anaphylactic shock requires removal of the allergen and administration of epinephrine. This should be done in conjunction with the usual priorities: evaluating the airway and assessing breathing and circulation. If it is helpful, consider using a similar mnemonic to the ABCDEs of trauma when assessing a patient with suspected anaphylaxis: airway, breathing, circulation, decontamination, and epinephrine. (See Table 5.)
Table 5. Primary and Secondary Management10 |
|
|
Primary Management |
|
|
Secondary Management |
|
|
IM = intramuscular; IV = intravenous |
|
The initial and most important treatment for recognized anaphylaxis with or without cardiovascular compromise or collapse is intramuscular (IM) epinephrine given in the lateral thigh.21 Previously, epinephrine was given subcutaneously, but it is better absorbed after IM injection. This should be repeated every 5-10 minutes according to response, or if a relapse occurs.10,22 If the clinician believes that another dosage is necessary, a shorter interval is permissible.23 The correct IM dosing is 0.01 mg/kg of 1:1,000 (1 mg/mL) solution, up to 0.3 mg in adults and 0.15 mg in children < 30 kg.10 Epinephrine is underutilized for treatment of anaphylaxis across the board in numerous studies, largely because of misdiagnosis and unfamiliarity with its use in this disease process.6,24,25,26
The route of administration is absolutely imperative to effective management; when compared to IM, blood concentrations of subcutaneously administered epinephrine take longer to reach peak blood levels. When epinephrine is injected intramuscularly into the lateral thigh, peak plasma levels of epinephrine are reached faster than when injections are given either subcutaneously or intramuscularly in the deltoid.23,27 The peak levels in the blood were higher, too.23
If the patient remains refractory to treatment with multiple doses of IM epinephrine (typically three, but there is not currently supported literature to recommend an exact number), or when the patient has signs of cardiovascular collapse, administer an intravenous (IV) bolus of epinephrine 5 to 10 mcg (or 0.2 mcg/kg) for hypotension and 0.1 to 0.5 mg for cardiovascular collapse.23 If the patient remains refractory, an infusion should be started at 1 mcg/min and titrated to effect.
If angioedema appears to be causing any signs of respiratory distress (uvular edema, audible stridor, hypoxia, etc.), intubate the patient early.10 Note that most patients with angioedema, especially those with mild symptoms, have self-limiting courses without airway compromise; most do not require intubation.28 Ventilator management in the anaphylactic patient should be patient-driven, keeping in mind that these patients may have significant bronchospasm and are at higher risk of barotrauma with large tidal volumes.
Another consideration in the intubated patient may be the use of propofol for sedation. Physicians may have heard that in patients with peanut allergies, the soya oil excipient of propofol can be cross-reactive. However, this oil is refined and is unlikely to contain enough soya protein to produce an allergic response. However, the product literature for propofol does list peanut allergy as a contraindication, so consideration for other sedating medications is strongly recommended.29
Removal of the offending agent may require a full body examination (i.e., in the case of bee stings, the stinger must be removed). Gastric lavage for ingestions is not recommended currently for foodborne allergens.10
Hypotension of anaphylaxis is related to distributive shock, and should be treated with IV isotonic crystalloids in standard bolus dosing; 1 to 2 L/hour in adults and 10 to 20 mL/kg/hour in children.10 Vasopressin should be considered in epinephrine- and fluid-resistant hypotension, at a dose of 0.01-0.04 IU/min IV titrated to response.20
It may also benefit the patient to keep him or her in a supine position, with legs in the air if possible, to improve venous return to the heart.11 In fact, in some studies, upright positioning in anaphylactic shock has been found to be associated with increased mortality.23 Refrain from having the patient lie flat if the patient is having shortness of breath or vomiting, but attempt to keep the legs elevated even if the patient cannot lie flat.23
Epinephrine administration prior to arrival in the ED, either from a home autoinjector or administered by EMS personnel, is associated with a decreased need for epinephrine in the hospital.9 In fact, there is evidence that once shock is fully developed in anaphylaxis, epinephrine administration does not have significant benefit on hemodynamics at all.30 This evidence again suggests benefits to patients for both early epinephrine administration as well as ensures that patients who present in anaphylaxis receive a prescription for an autoinjector after discharge.
Other pharmacological agents should be administered, most with more theoretical benefit than studied. These are considered second-line treatments, since most have a lengthy onset of action.
Nebulizer treatment with albuterol is recommended in patients with signs of bronchospasm.31 Consider the risk of exacerbating hypotension in patients in shock with further tachycardia. In patients with respiratory symptoms or those requiring multiple doses of epinephrine, supplemental oxygen should be administered.32 Racemic epinephrine is not currently recommended for use and should not be used as a substitute for intramuscular epinephrine because it is poorly tolerated prior to reaching satisfactory blood levels.33
H1 antagonists should be administered orally, intramuscularly, or intravenously.31 The onset of action is one to three hours. This class of medications likely has little benefit in controlling all but the cutaneous symptoms of anaphylaxis (urticaria and angioedema).11 It has very little effect on blood pressure.23 This medication should be given intravenously or intramuscularly at 25 to 50 mg in adults and 1 mg/kg, maximum 50 mg, in children.23 In some studies, H2 antagonists, such as ranitidine or cimetidine, used in combination with H1 antagonists have been shown to treat cutaneous symptoms better.23
Steroids should be given intravenously after the initial resuscitation.31 Oral steroids prescribed after discharge also are reasonable, and may be especially efficacious in patients with concomitant asthma.31 However, there is little to no evidence of their efficacy in treating allergic reactions or preventing biphasic reactions.11 Subsequently, there is high variability of their administration timing and dosing.34 Dosing should be 1.0 to 2.0 mg/kg/dose equivalent of methylprednisolone every six hours intravenously.23 Oral prednisone can be given in 1.0 mg/kg up to 50 mg for mild reactions.23
Glucagon has a theoretical benefit in patients taking beta-blocker medications with refractory hypotension and bronchospasm not responsive to epinephrine.23 The dosing for administration is 1.0 to 5.0 mg over five minutes, with an infusion of 5 to 15 mcg/min titrated to response.23 Because glucagon can cause emesis, ensure the patient’s airway is secured.23
In patients with a history of contrast or iodine allergy, pretreatment with IV crystalloid bolus and/or steroids (50 mg prednisone given 13, 7, and 1 hour prior to injection) and antihistamines (50 mg diphenhydramine and 300 mg ranitidine orally or intravenously one hour prior) has been shown to be beneficial in preventing allergic reaction.20 Although these regimens are not applicable to ED care, a clinician may consider the risks and benefits of the historical reactions, the ability to give any of these medications prior to contrasted studies, and the need for these diagnostic studies to be conducted.20
Treatment: Urticaria
The treatment of urticarial reaction involves the removal of the offending agent and symptomatic treatment.10 Patients can be treated with H1 antihistamines first line.10 Again, the use of steroids is common but is without significant supporting data, as is the use of H2 antihistamines.10 Epinephrine should be considered only in severe or refractory cases of urticaria.10
Treatment: Angioedema
The treatment of angioedema is similar to that of an urticarial reaction, unless there is suspicion that it is a nonallergic form of angioedema triggered by ACE inhibitor use or hereditary angioedema.10 Neither of these forms will respond to anaphylaxis treatment since their pathophysiology is bradykinin- or C1 esterase inhibitor-mediated, respectively.10 Treatment of both non-allergenic forms is largely supportive and expectant.
ACE inhibitor-mediated angioedema symptoms may last hours to days, with little data to support the use of either C1 esterase inhibitor at 1,000 U IV or icatibant (a bradykinin-2 receptor antagonist) at 30 mg subcutaneous (SC). The symptoms of hereditary angioedema may be shortened with the use of C1 esterase inhibitor at 20 U/kg IV, icatibant at 30 mg SC, or ecallantide at 30 mg SC.10 Fresh frozen plasma can be used in place of C1 esterase inhibitor.10
Complications
Death by anaphylaxis is rare, but certainly possible. Death from anaphylaxis typically occurs by means of circulatory collapse and/or respiratory arrest.32 One study of fatal anaphylactic reactions found that only 14% of patients who died from anaphylaxis had received epinephrine prior to arrest.13
Biphasic reactions, or a return of allergic symptoms after complete resolution of anaphylaxis without repeated exposure to the antigen, are a feared complication of anaphylaxis, with incidences of 1-23% of cases of anaphylaxis reported.16 Risk factors for the biphasic reaction include severe initial reactions (especially the symptoms of laryngeal edema or hypotension), delayed administration of epinephrine, or a delayed response to antigen exposure.16 However, the treatment for a biphasic reaction should be the same as for the initial anaphylactic reaction. Consider a patient’s risk factors for biphasic reactions when determining disposition. Most studies report a mean time to onset of the secondary reaction of more than eight hours, with a maximum of 72 hours, after resolution of the initial reaction.35
While epinephrine administration is the definitive treatment for anaphylaxis, it is not without complications. The safety profile of epinephrine use in anaphylaxis has been studied, with one paper showing an overall side effect rate of about 21.6%. In that study, the side effects largely included mild and transient effects, such as tremors, palpitations, and anxiety. These effects are more frequent in the adult population.36 More severe adverse events due to epinephrine administration, such as chest discomfort, elevated blood pressure, or electrocardiogram (ECG) changes, were associated with IV administration rather than IM administration.36 Coronary artery vasospasm inducing ST elevations and troponin elevations after administration have been reported.37 One feared effect is epinephrine use in the setting of nonselective beta-blocker medications, as this theoretically could cause coronary artery vasospasm.38 However, this potential and extremely rare complication should not delay epinephrine administration.38
The need for multiple doses of epinephrine in the ED has been found to have a higher association with delayed administration of epinephrine or administration in the ED rather than outside the hospital.4 The need for multiple doses also was associated with anaphylaxis after triggers with strong evidence for more severe anaphylactic reactions, including peanuts, tree nuts, and milk.39
Kounis syndrome occurs when anaphylaxis causes coronary artery spasm.40 Patients often present with chest pain, but this may be ignored in patients in extremis from anaphylaxis. All patients who have had an anaphylactic reaction should have an ECG prior to discharge. Patients with prolonged chest pain or an abnormal ECG should be observed and have troponin measured.
Disposition
The post-anaphylactic patient with a quick response to epinephrine administration should be observed for four to six hours.16 The patient should be monitored for signs and symptoms of continued or biphasic allergic response, and if these occur, should be treated appropriately. The patient with a delayed onset of allergic symptoms after allergen exposure, a delayed administration of epinephrine, or a poor response to treatment should be observed longer or observed in an inpatient setting because of the increased risk of biphasic reaction.16 Other considerations for inpatient observation may include access to medical care, uncertainty of the risk of allergen reexposure, or parental discomfort with discharge. If the patient is hospitalized, consider consulting an allergist early on if this is the hospital’s practice.
If there are ongoing signs of anaphylaxis despite treatment, if an epinephrine drip has been started for the patient, or if the patient is ventilated, ICU admission generally is appropriate.
After four hours of ED observation, patients who remain symptom-free can be discharged home with an epinephrine autoinjector and instructions for its use. Recent reports state that 60% of individuals who experienced anaphylaxis were not equipped with epinephrine at home.2 Epinephrine autoinjectors are not prescribed enough after discharge, with one paper finding that they were prescribed only 31.7% of the time after criteria for anaphylaxis on ED admission were met.41 There is much to be said for educating all patients on the use of their autoinjectors prior to discharge, since one study found that only 30-40% of patients with autoinjectors were able to use them properly.31 Also inform patients that autoinjectors typically expire after about one year, and their efficacy may be compromised after that date.
As noted in the media, the cost for autoinjectors is high, and supplies can be low in some geographic areas. Generic autoinjectors are available, although they also have been in short supply. Often, the autoinjector comes in a two-pack, which allows the patient to give a second dose if symptoms worsen while they seek medical help. Patients should be encouraged to carry the injectors in a place that is always accessible, such as a purse, camera bag, etc. Autoinjectors are permitted in carry-on luggage on airplanes.
Prescribing epinephrine autoinjectors to patients with allergic reactions but without anaphylaxis, such as those who arrive at the ED with urticaria only, is not recommended currently.17 The dose of epinephrine contained in autoinjectors is not without risk or side effects. Providers in the ED tend to prescribe oral antihistamines every six hours for the first 24 hours in such circumstances; however, there is little to no data to support this practice. H1 antihistamines may be prescribed on an as-needed basis for ongoing cutaneous symptoms.
Most emergency medicine providers continue to prescribe scheduled steroids and antihistamines after resolution of anaphylaxis despite the lack of evidence that steroids affect urticaria or other allergic symptoms, including repeat anaphylaxis.42 Steroids are theorized to decrease the risk of biphasic reactions, but studies have not shown actual benefit.16
Consultation with an allergist is strongly recommended, but referrals to allergists are made only about 45% of the time, and patients actually see an allergist much less often.41,43 Patients with anaphylaxis to bee stings can be successfully desensitized over a number of months. Those with food allergies and their families may benefit from dietetic consultation as well to assist in avoiding allergens in their diets.44 For children, requesting that parents share this education with schools and daycare facilities also will reduce the risk of anaphylactic reactions at these locations.44,45 Those with drug-induced allergies should receive written documentation of the likely medication, if possible, to assist with communication between patients and their future providers.
For likely exercise-induced anaphylaxis, there is inadequate evidence to suggest that taking antihistamines or H2 antagonists prior to exercise is protective.29 It has been estimated that about half of exercise-induced anaphylaxis has an association with ingesting certain foods, and it is recommended that delaying exercise for five hours after eating can prevent reactions.11 Physicians in the ED should recommend avoiding exercise as one would with any other trigger, prescribe an autoinjector to be carried at all times and when exercise cannot be avoided, and refer to an allergist.
Summary and the Future of Anaphylaxis in the Emergency Department
Current proposals for diagnostic criteria have been found to have good sensitivity but poor specificity, and they lack prospective validation.46 Currently, there is not a well-studied set of clinical criteria to delineate definitively between an acute allergic reaction and anaphylaxis. Therefore, ED physicians are without a standardized guideline for management. In the future, a more defined set of criteria for anaphylaxis and allergic reactions will be beneficial for patients and the physicians who treat them. This will allow for improved recognition of the disease and earlier treatment with epinephrine.
Underreporting due to the knowledge gap and subsequent misdiagnosis of anaphylaxis will continue to make research of this disease difficult.47 Interestingly, difficulty studying anaphylaxis is even hindered by discharge coding. One study found that half of their study population would have been missed for research if coded incorrectly.48 Providers can assist in future research by specifying a known allergen in a patient’s chart. The fluid language used when describing an “allergic reaction” vs. “anaphylaxis” and “anaphylactic shock” can be confusing to patients, can lead to miscommunication between providers, and can make studying the disease process difficult due to inappropriately named diagnoses. The allergy community has made the call to revise the current nomenclature to enhance the descriptive vocabulary.49
Further studies also are needed to help practitioners decide whether, when, and how much antihistamines and steroids to administer and prescribe. Allergic reactions often do not meet proposed criteria for anaphylaxis, and physicians are left with vague recommendations and data on treatment with antihistamines, steroids, or novel treatment modalities.
In general, the earlier epinephrine is administered, the better the outcome. Since first responders often are the first to see the patient during an allergic reaction, educating EMS personnel on the recognition of anaphylaxis and implementing protocols for early epinephrine administration are key to reducing overall morbidity, mortality, and length of hospital stays.
In a study on North American ED concordance with current guidelines in anaphylaxis, researchers found that epinephrine treatment occurred 49% of the time, epinephrine autoinjector prescriptions were given 57% of the time, referral to an allergist occurred 12% of the time, and instructions to avoid the offending allergen occurred 24% of the time.50 A patient presenting with anaphylaxis received three of four of the guideline recommendations only 16% of the time.50 A greater understanding of the proper approach to anaphylaxis recognition, treatment, and disposition is needed. While this article is unable to clearly state a straightforward approach to diagnosing and treating the spectrum of allergic presentations, understanding that the disease itself is not straightforward and still shrouded in mystery is imperative to the emergency practitioner. It is an important differential to consider in a number of possible presentations, and one of the most common presentations that remains undertreated.
References
- Simons FE, Ardusso LR, Bilò MB, et al. World Allergy Organization guidelines for the assessment and management of anaphylaxis. World Allergy Organ J 2011;4:13-37.
- Wood RA, Camargo CA Jr, Lieberman P, et al. Anaphylaxis in America: The prevalence and characteristics of anaphylaxis in the United States. J Allergy Clin Immunol 2014;133:461-467.
- Lieberman P, Camargo CA Jr, Bohlke K, et al. Epidemiology of anaphylaxis: Findings of the American College of Allergy, Asthma and Immunology Epidemiology of Anaphylaxis Working Group. Ann Allergy Asthma Immunol 2006;97:596-602.
- Lippner E, Dinakar C. Increasing emergency department visits for anaphylaxis, 2005-2014. Pediatrics 2017;140(Suppl 3):S188.
- Sundquist BK, Jose J, Pauze D, et al. Anaphylaxis risk factors for hospitalization and intensive care: A comparison between adults and children in an upstate New York emergency department. Allergy Asthma Proc 2019;40:41-47.
- Molloy JD, Gabrielli S, Clarke AE, et al. Anaphylaxis: Comparison of clinical characteristics and management between children less than 2 years of age and older children. J Allergy Clin Immunol 2019;143:AB145.
- Bock SA, Muñoz-Furlong A, Sampson HA. Further fatalities caused by anaphylactic reactions to food, 2001-2006. J Allergy Clin Immunol 2007;119:1016-1018.
- Turner PJ, Jerschow E, Umasunthar T, et al. Fatal anaphylaxis: Mortality rate and risk factors. J Allergy Clin Immunol Pract 2017;5:1169-1178.
- Hochstadter E, Clarke A, De Schryver S, et al. Increasing visits for anaphylaxis and the benefits of early epinephrine administration: A 4-year study at a pediatric emergency department in Montreal, Canada. J Allergy Clin Immunol 2016;137:1888-1889.e4.
- Rowe BH, Gaeta TJ. Anaphylaxis, allergies, and angioedema. In: Tintinalli JE, Stapczynski J, Ma O, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 8e New York, NY: McGraw-Hill; 2016.
- Sampson HA, Muñoz-Furlong A, Bock SA, et al. Symposium on the definition and management of anaphylaxis: Summary report. J Allergy Clin Immunol 2005;115:584-591.
- Minty B. Food-dependent exercise-induced anaphylaxis. Can Fam Physician 2017;63:42-43.
- Pumphrey RS. Lessons for management of anaphylaxis from a study of fatal reactions. Clin Exp Allergy 2000;30:1144-1150.
- Johansson SG, Bieber T, Dahl R, et al. Revised nomenclature for allergy for global use: Report of the Nomenclature Review Committee of the World Allergy Organization, October 2003. J Allergy Clin Immunol 2004;113:832-836.
- McCormick M, Folbe AJ, Lin HS, et al. Site involvement as a predictor of airway intervention in angioedema. Laryngoscope 2011;121:262-266.
- Kemp SF. The post-anaphylaxis dilemma: How long is long enough to observe a patient after resolution of symptoms? Curr Allergy Asthma Rep 2008;8:45-48.
- Sicherer SH, Simons FE. Quandaries in prescribing an emergency action plan and self-injectable epinephrine for first-aid management of anaphylaxis in the community. J Allergy Clin Immunol 2005;115:575-583.
- Wang J, Young MC, Nowak‐Wegrzyn A. International survey of knowledge of food‐induced anaphylaxis. Pediatr Allergy Immunol 2014;25:644-650.
- Lin RY, Schwartz LB, Curry A, et al. Histamine and tryptase levels in patients with acute allergic reactions: An emergency department–based study. J Allergy Clin Immunol 2000;106:65-71.
- Ward BR, Schwartz LB. Anaphylaxis and its management. In: Mahmoudi M, ed. Allergy and Asthma: Practical Diagnosis and Management. Switzerland: Springer International; 2016: 651-671.
- Chamberlain D. Emergency medical treatment of anaphylactic reactions. Project Team of the Resuscitation Council (UK). J Accid Emerg Med 1999;16:243-247.
- Järvinen KM, Sicherer SH, Sampson HA, Nowak-Wegrzyn A. Use of multiple doses of epinephrine in food-induced anaphylaxis in children. J Allergy Clin Immunol 2008;122:133-138.
- Sampson HA, Muñoz-Furlong A, Campbell RL, et al. Second symposium on the definition and management of anaphylaxis: Summary report — Second National Institute of Allergy and Infectious Disease/Food Allergy and Anaphylaxis Network symposium. Ann Emerg Med 2006;47:373-380.
- Estelle F, Simons R, Chad ZH, Gold M. Real-time reporting of anaphylaxis in infants, children and adolescents by physicians involved in the Canadian pediatric surveillance program. J Allergy Clin Immunol 2002;109:S181.
- O’Keefe A, Clarke A, St Pierre Y, et al. The risk of recurrent anaphylaxis. J Pediatr 2017;180:217-221.
- Sidhu N, Jones S, Perry T, et al. Evaluation of anaphylaxis management in a pediatric emergency department. Pediatr Emerg Care 2016;32:508-513.
- Simons FE, Roberts JR, Gu X, Simons KJ. Epinephrine absorption in children with a history of anaphylaxis. J Allergy Clin Immunol 1998;101:33-37.
- Worm M, Eckermann O, Dölle S, et al. Triggers and treatment of anaphylaxis: An analysis of 4,000 cases from Germany, Austria and Switzerland. Dtsch Arztebl Int 2014;111:367-375.
- Bradley AE, Tober KE, Brown RE. Use of propofol in patients with food allergies. Anaesthesia 2008;63:439.
- Mink SN, Simons FE, Simons KJ, et al. Constant infusion of epinephrine, but not bolus treatment, improves haemodynamic recovery in anaphylactic shock in dogs. Clin Exp Allergy 2004;34:1776-1783.
- Lack G, Penagos M. Recognition and management of anaphylaxis in children. Prescriber 2010;21:43-49.
- Shedd GC, Shaeri A. Drug-induced anaphylaxis in the emergency department. Adv Emerg Nurs J 2015;37:5-11.
- Simons FE, Gu X, Johnston LM, Simons KJ. Can epinephrine inhalations be substituted for epinephrine injection in children at risk for systemic anaphylaxis? Pediatrics 2000;106:1040-1044.
- Mo Y, Byrd AM, Stephens K, et al. Steroid management of allergic reactions and anaphylaxis in the emergency room. J Allergy Clin Immunol 2018;141:AB41.
- Pourmand A, Robinson C, Syed W, Mazer-Amirshahi M. Biphasic anaphylaxis: A review of the literature and implications for emergency management. Am J Emerg Med 2018;36:1480-1485.
- Cardona V, Ferré-Ybarz L, Guilarte M, et al; AdreSCAIC Research Group. Safety of adrenaline use in anaphylaxis: A multicenter register. Int Arch Allergy Immunol 2017;173:171-177.
- Shaver KJ, Adams C, Weiss SJ. Acute myocardial infarction after administration of low-dose intravenous epinephrine for anaphylaxis. CJEM 2006;8:289-294.
- Cunnington C, McDonald JE, Singh RK. Epinephrine-induced myocardial infarction in severe anaphylaxis: Is nonselective β-blockade a contributory factor? Am J Emerg Med 2013;31:759.e1-2.
- Lee J, Rodio B, Lavelle J, et al. The impact and safety of an updated anaphylaxis clinical pathway in a busy pediatric emergency department. J Allergy Clin Immunol 2017;139:AB222.
- Kounis NG. Kounis syndrome: An update on epidemiology, pathogenesis, diagnosis and therapeutic management. Clin Chem Lab Med 2016;54:1545-1559.
- Dubus JC, Lê MS, Vitte J, et al. Use of epinephrine in emergency department depends on anaphylaxis severity in children. Eur J Pediatr 2019;178:69-75.
- Duffey H, Egan MS, Maiorella A, Mistry R. Variation in discharge practices after resolution of allergic reactions among emergency medicine and allergy immunology providers. J Allergy Clin Immunol 2019;143:AB151.
- Wright CD, Longjohn M, Lieberman PL, Lieberman JA. An analysis of anaphylaxis cases at a single pediatric emergency department in over one year. J Allergy Clin Immunol 2017;139:AB223.
- Roberts G. Diagnosis of food allergy and practical management of anaphylaxis: Acute management. Clinical and Translational Allergy 2011;1(Suppl 1):S63.
- Greenberger PA, Rotskoff BD, Lifschultz B. Fatal anaphylaxis: Postmortem findings and associated comorbid diseases. Ann Allergy Asthma Immunol 2007;98:252-257.
- Loprinzi-Brauer CE, Li JTC, Hagan JB, et al. Prospective validation of National Institute of Allergy and Infectious Diseases/Food Allergy and Anaphylaxis Network clinical criteria for the diagnosis of anaphylaxis in emergency department patients. Ann Emerg Med 2014;64:S22-S23.
- Klein JS, Yocum MW. Underreporting of anaphylaxis in a community emergency room. J Allergy Clin Immunol 1995;95:637-638.
- Clark S, Gaeta TJ, Kamarthi GS, Camargo CA. ICD-9-CM coding of emergency department visits for food and insect sting allergy. Ann Epidemiol 2006;16:696-700.
- Johansson SG, Hourihane JO, Bousquet J, et al. A revised nomenclature for allergy: An EAACI position statement from the EAACI nomenclature task force. Allergy 2008;56:813-824.
- Hasegawa K, Clark S, Boggs KM, et al. Changes in emergency department concordance with guidelines for the management of insect sting-induced anaphylaxis: 1999-2001 versus 2013-2015. J Allergy Clin Immunol 2017;139:AB229.
For emergency physicians, anaphylaxis can be a challenging diagnosis to make. This article will present the most current information for diagnosing allergic reactions and anaphylaxis, and how to treat them properly.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
