Are the Changes New, Recent, or Old?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
Imagine examining the ECG in the figure below without any accompanying clinical information. How would one interpret this tracing? What might one suspect is going on?
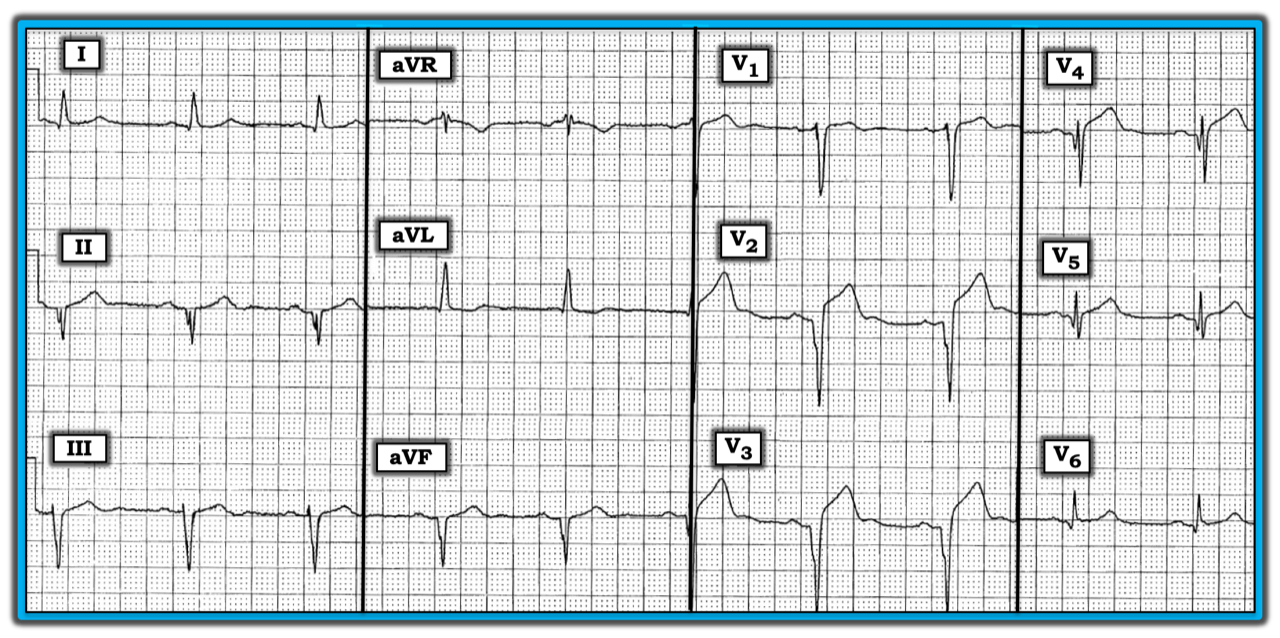
The rhythm is sinus at 60 beats/minute to 65 beats/minute. The PR, QRS, and QTc intervals are normal. There is marked left axis deviation. There is no chamber enlargement. But the most remarkable ECG findings relate to the assessment of the Q-R-S-T changes.
Large Q waves with fragmentation are visible in leads II and aVF. This strongly suggests there has been inferior myocardial infarction (MI) at some point. Preservation of an initial r wave in lead III suggests that in addition to inferior MI, there is left anterior hemiblock. Lack of ST elevation in any of inferior lead suggests that the inferior MI is old.
In the chest leads, large QS complexes in lead V2 and lead V3, together with Q waves in leads V4, V5, and V6, suggest there has been extensive anterolateral MI. Despite this, preservation of the initial r wave in lead V1 suggests the septum remains intact. There is significant anterior ST elevation. This begins in lead V1, and attains 2-3 mm in leads V2, V3, and V4. Does the anterolateral MI represent acute injury or old infarction? A third possibility might be prior MI with a superimposed new or recent infarction.
Clinical correlation will be needed to determine whether the changes seen in the chest leads represent acute or recent MI (prior MI with superimposed new injury) or longstanding changes of left ventricular (LV) aneurysm that has developed some time after extensive anterolateral MI.
Learning the history is essential. If the patient is experiencing new chest pain, repeating the ECG a short time later may show evolution if an acute event is in progress. Finding a prior ECG would be invaluable for telling if ECG changes in the tracing with this article are new. If the patient is in the hospital or ED, serum troponin should be increased if this is an acute or recent event. Finally, echocardiogram may be helpful if it shows a large LV aneurysm.
The ECG with this article could reflect development of LV aneurysm following a previous extensive anterolateral MI. That said, it is difficult to prove this without additional clinical correlation. For further discussion on and additional information about this case, please visit: http://bit.ly/2YXA8wh.
Imagine examining the ECG in the figure below without any accompanying clinical information. How would one interpret this tracing? What might one suspect is going on?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
