Is This Acute?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
There is a stack of ECGs in need of interpretation. The tracing in the figure below is among those tracings. No clinical information is available. How would one interpret this ECG? Are the changes acute?
The rhythm is sinus at about 85 beats per minute. All intervals and the axis are normal. There is no chamber enlargement. The most remarkable findings relate to assessment of Q-R-S-T changes.
Considering the tiny size of the QRS complex in lead III, the Q wave in this lead is large. There also appears to be a small q wave in lead aVF, although the tiny size of the QRS complex in this lead makes it difficult to be certain of this.
Regarding R wave progression, transition is delayed slightly (i.e., the R wave does not become greater than the depth of the S wave until lead V5).
Each inferior lead manifests ST segment elevation. Compared to the size of the QRS complex in leads II, III, and aVF, the relative amount of ST elevation is considerable. This is followed by beginning T wave inversion in each inferior lead. Reciprocal changes to the inferior ST elevation are seen in the form of ST depression in lead aVL. The rest of the ECG looks nonspecific. ST segments are coved but not elevated in the lateral chest leads. There is no ST depression in the anterior leads.
ECG findings in the limb leads are diagnostic of inferior infarction. The fact that ST segments in each inferior lead are significantly elevated, with mirror-image reciprocal ST depression in lead aVL, suggests that infarction is most probably recent, if not still ongoing. At this point, someone needs to learn the patient’s history. Was this patient admitted to the hospital? Was potential acuity of these ECG findings recognized? Was appropriate treatment initiated?
Further research reveals the patient had been admitted. The possibility of an infarction that still was acutely evolving was not appreciated. The patient died before referral was made.
For more information about and further discussion in this case, please visit: http://bit.ly/35SYzKT.
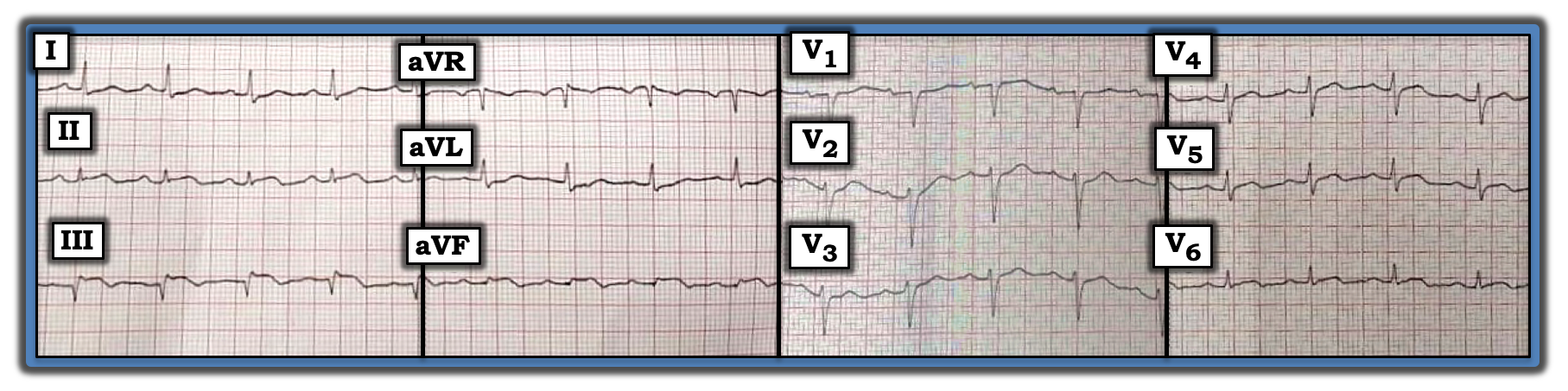
There is a stack of ECGs in need of interpretation. The tracing in the figure is among those tracings. No clinical information is available. How would one interpret this ECG? Are the changes acute?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
