This ECG Was in Your ‘Pile to be Read’
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
Imagine the ECG in the figure below was one of many tracings you received to read from a group of patients seen by other providers in your clinic. Unfortunately, no clinical information about this patient was available. How would one interpret this tracing? Considering no clinical information regarding what happened to the patient was available, what is the next step?
Clearly, this tracing is of concern. The rhythm is sinus bradycardia at a rate just under 60 beats/minute. All intervals (PR/QRS/QTc) are normal. The axis is normal at +75 degrees. There is no chamber enlargement. Small q waves are seen in the inferolateral leads.
Regarding R wave progression, transition occurs normally here (i.e., between leads V2 and V3), although R wave amplitude in lead V2 is taller than is usually seen in this anterior lead. However, the most concerning findings relate to ST-T wave changes. In addition to those narrow inferior lead q waves, there is 1-1.5 mm of upward concavity ST segment elevation in each inferior lead.
There are several reasons to suspect this represents an acute (or at least recent) inferior infarction. One, there is mirror-image opposite ST segment depression in lead aVL. Two, there is 1 mm of flat ST depression in lead I. Three, there also is ST depression in lead V2 in association with a taller-than-expected R wave in this anterior lead.
The ECG findings described so far strongly suggest recent (if not acute) inferoposterior myocardial infarction (MI). There is a “magic,” mirror-image opposite relationship that is seen commonly in acute inferior MI between the appearance of the ST segment and T wave in lead III, compared to the ST-T wave in lead aVL. If one mentally “flips” the shape of the elevated ST-T wave seen in lead III, the result closely resembles the J-point depression and sagging ST segment seen in lead aVL. The finding of a taller-than-expected R wave in anterior lead V2, in association with the depressed ST segment in this anterior lead, strongly suggests recent posterior MI. Putting these findings together makes for no fewer than six leads (i.e., leads I, II, III; aVL, aVF; and V2) that suggest recent (if not acute) inferoposterior MI has occurred. Immediately search for the chart of the patient whose ECG is shown in the figure to find out whether the caring provider recognized these ECG changes. If not, find the patient.
NOTE: For more information about and further discussion on this case, please click here.
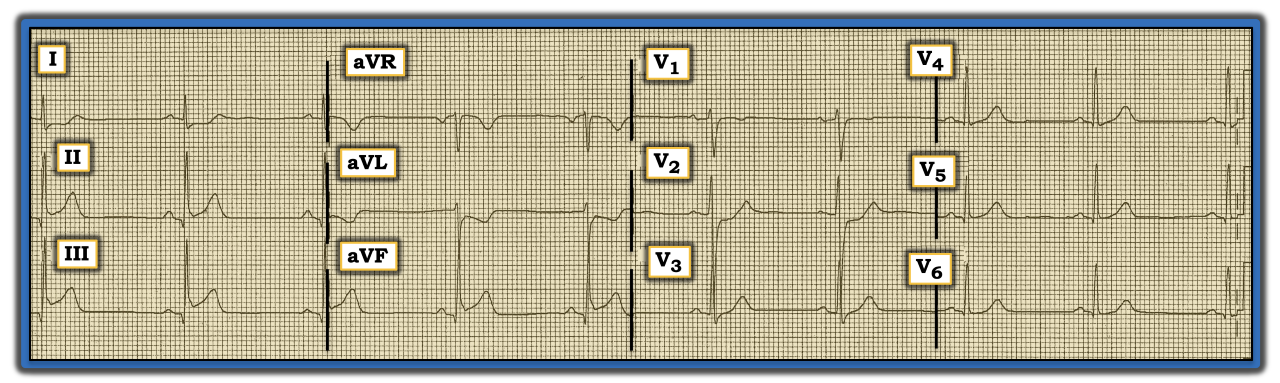
Imagine the ECG in the figure was one of many tracings you received to read from a group of patients seen by other providers in your clinic. Unfortunately, no clinical information about this patient was available. How would one interpret this tracing? Considering no clinical information regarding what happened to the patient was available, what is the next step?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
