How Can This Patient Be Stable?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The ECG in the figure below was obtained from a young adult who presented to the emergency department with palpitations, but who otherwise was hemodynamically stable. What is the diagnosis?
The rhythm in this ECG is rapid and irregularly irregular. The QRS complex is obviously wide. P waves are absent. Therefore, this rhythm qualifies as an irregular wide complex tachycardia rhythm. The finding of an irregularly irregular tachycardia without clear sign of P waves on any of the 12 leads suggests the rhythm to be atrial fibrillation (AF).
The key to interpretation of this tracing lies with determination of the heart rate. Note the R-R interval for more than a few of the complexes in the long lead II rhythm strip is barely the length of one large box long. This corresponds to a ventricular rate that at times exceeds 220 (if not 250) beats per minute.
Normally with AF, the AV node refractory period limits the number of fibrillation impulses that can be conducted to the ventricles to less than 200 beats per minute. The fact that the ventricular response is at times much faster than this indicates that AF impulses cannot be conducting over the normal AV nodal pathway. Instead, fibrillation impulses must be conducting over an accessory pathway. This tells us that the patient must have Wolff-Parkinson-White (WPW) syndrome. Several additional features support the conclusion that this patient has WPW. There is marked variation in the duration of R-R intervals on this tracing. There is variation in QRS morphology. Both of these ECG findings are in contrast to what happens with monomorphic ventricular tachycardia (VT), in which the rhythm will not be this irregular, and will not manifest this degree of variation in QRS morphology. Finally, a characteristic feature seen in younger adults with WPW, who otherwise do not have underlying heart disease, is that they often remain hemodynamically stable for surprisingly long periods, despite attaining heart rates as rapid as we see in this figure. Patients with VT are far less likely to remain hemodynamically stable for a sustained period with heart rates that exceed 220 beats per minute.
For more information about and further discussion on this case, please click here.
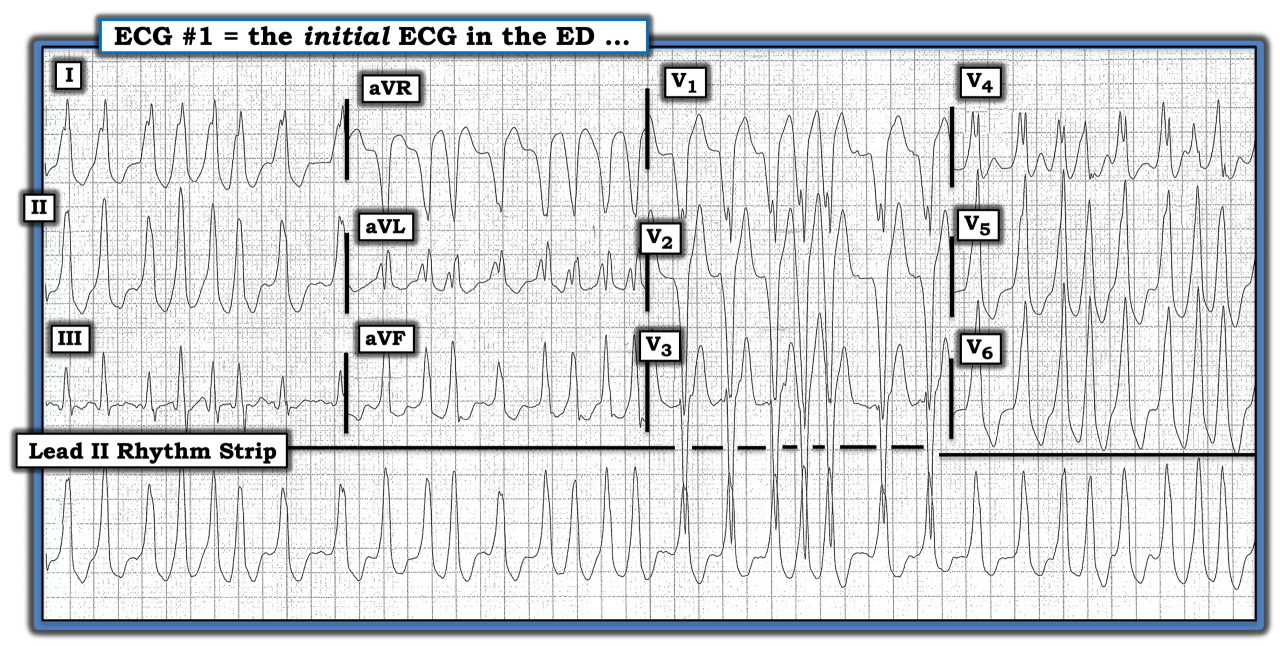
The ECG in the figure was obtained from a young adult who presented to the emergency department with palpitations, but who otherwise was hemodynamically stable. What is the diagnosis?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
