Advances in Pediatric Neck Trauma: What’s New in Assessment and Management?
September 1, 2020
Reprints
AUTHOR
Jennifer Guyther, MD, Co-Director Combined Residency in Emergency Medicine and Pediatrics, Departments of Emergency Medicine and Pediatrics, University of Maryland School of Medicine, Baltimore; Deputy Medical Director Baltimore City Fire Department, Assistant Medical Director Baltimore County Fire Department, Associate Region III Medical Director, MIEMSS
PEER REVIEWER
Larry B. Mellick, MD, MS, FAAP, FACEP, Vice Chairman for Academic Affairs, Interim Section Chief of Pediatric Emergency Medicine, Assistant Residency Director, Professor of Emergency Medicine, University of South Alabama, Mobile
EXECUTIVE SUMMARY
• Neck injuries are uncommon in pediatrics, with cervical spine injuries occurring in only 1% to 2% of patients with blunt trauma.
• The neck can be divided into three anatomical zones. Zone I extends from the clavicle to the cricoid cartilage. Zone II extends from the cricoid cartilage to the angle of the mandible, and zone III extends from the angle of the mandible to the base of the skull.
• Children with penetrating neck trauma account for only 0.28% of pediatric trauma patients. In a review of National Trauma Data Bank records on patients younger than 15 years of age, Stone et al found the most common mechanisms of injury were stabbings and gunshot wounds.
• Selective neck exploration should be used based on the physical examination to evaluate penetrating neck trauma in children. Hard signs of injury that mandate surgical exploration are active hemorrhage, a pulsatile or expanding hematoma, pulse deficit, massive subcutaneous emphysema, respiratory distress, shock, or airway compromise.
• Children with syndromes associated with ligamentous laxity, cervical instability, or rheumatologic disorders are at higher risk for cervical spine injury.
• In children 2 to 7 years of age, atlantoaxial rotatory subluxation and atlantooccipital dislocations are more common.
• The Pediatric Emergency Care Applied Research Network conducted a retrospective case-control study looking at risk factors for cervical injury in blunt trauma patients and found that altered mental status, focal neurological findings, neck pain, torticollis, torso injury, diving, and high-risk motor vehicle collision were conditions that predisposed to cervical spine injury.
• The line of Swischuk, which is drawn between the anterior aspect of the C1 and C3 spinous processes, helps differentiate between subluxation and pseudosubluxation, the latter of which is related to the elasticity of cervical spine in pediatrics. The anterior aspect of the C2 spinous process should be within 2 mm of this line.
Although rare, pediatric neck trauma may have devastating consequences. The author provides current information on recognizing and managing pediatric neck trauma.
— Ann M. Dietrich, MD, Editor
Introduction
Pediatric neck trauma is a rare event, occurring in only 1% to 2% of patients. Understanding the anatomical changes that occur with age can illuminate the differences in injury patterns between adults and children. The vast majority of these injuries involve the cervical spine, but it is also important to recognize potential associated injuries to the airway, vasculature, and other body systems.
Obtaining an accurate and reliable history and physical exam can be difficult in children, especially those younger than 3 years of age. Awareness of the mechanisms of injury and risk factors that predispose children to neck trauma will be helpful in assessing the pediatric trauma patient. Such awareness, in addition to the physical examination looking for clues of injury, such as midline cervical pain or neurological deficits, will guide clinical care decisions, including the application of a cervical collar or appropriate imaging. Unlike adults, for whom there are validated criteria to clinically clear the cervical spine, currently there is no widely accepted, well-validated criterion for cervical spine clearance in children. The patient’s entire clinical picture must be weighed carefully to balance the risk of injury with the risk of radiation exposure.
Options for imaging the cervical spine include radiographs, computed tomography (CT) scan, and magnetic resonance imaging (MRI). Each imaging modality has its own advantages and disadvantages that should be taken into account. Ultimately, if the clinical exam or indicated imaging studies show no injuries, the patient can be referred for outpatient follow-up. Concerning physical exam findings or abnormalities on imaging should be managed in conjunction with a subspecialist. Although neck injuries do not occur often, it is important to maintain a high index of suspicion, collect all necessary information, and carefully consider the risks of any interventions to provide the best care for pediatric patients.
Neck injuries are uncommon in pediatric patients, with cervical spine injuries occurring in only 1% to 2% of patients with blunt trauma.1-4 However, despite the low incidence, injuries to the neck can cause significant morbidity and mortality, especially if the injury involves the airway or cervical spine. Cervical spine injuries can be fatal in up to 40% of cases, and morbidity can be as high as 60%.5 Penetrating injuries to the neck are an even rarer occurrence, but if the vasculature is injured, mortality has been reported as high as 66%.6
In children’s necks, several vital structures are compressed into a much smaller area compared to adults. The upper airway consists of the larynx, comprising the thyroid, cricoid cartilage, and semicircular cartilaginous rings.7 The common carotid arteries follow the trachea on both sides.7 The esophagus runs posterior to the trachea. The first seven vertebrae comprise the cervical spine. The neck also can be divided into three anatomical zones. Zone I extends from the clavicle to the cricoid cartilage. Zone II extends from the cricoid cartilage to the angle of the mandible, and zone III extends from the angle of the mandible to the base of the skull.8,9 These zones historically have been used to determine surgical management based on possible damage to the underlying organs. As CT technology has advanced, less of an emphasis has been placed on the specific zone, and imaging has played a larger role in the ultimate decision to go to the operating room.
Background
Anatomical Differences
The cervical spine undergoes growth and development during childhood, causing it to respond to and suffer injuries differently than the adult spine. One protective element against injury is that the neck is relatively shorter, allowing for less physical space for direct trauma. Along the same lines, the relatively larger mandible provides physical protection as well.7 The head is relatively larger than the neck, leading to a higher fulcrum of cervical spine flexion.1,10 In children younger than 8 years of age, maximal mobility of the cervical spine is in C1 to C3. In children 8 to 12 years of age, the fulcrum changes to C3 to C5, and generally after age 12 years, the fulcrum is from C5 to C6.11-13 This is one of the reasons why younger children tend to experience injuries at higher cervical levels compared to older children and adults.
Bones also continue to develop over the years. Growth plates are still developing, and ossification centers are not completely mineralized.14 There is natural anterior wedging of the ossifying vertebral bodies.10 This causes difficulty in interpreting fracture lines to the untrained eye, since skeletal growth in children may resemble fracture patterns in adults. Vertebral bodies tend to slide forward with flexion, and articular surfaces are more horizontal, allowing for easier movement.1,5,12 The vertebral facet joints are shallow and horizontally oriented, which causes increased flexion and extension. The uncinate processes that will limit lateral flexion in adults are underdeveloped in children.2 All this leads to increased mobility and flexibility of the bony structures. Herzenberg et al performed calculations from anthro-pometric data, which documented disproportionate rates of growth between the head and the chest of a child. They found the circumference of the head grew logarithmically, but the circumference of the chest grew linearly. This disproportionate growth results in young children having neck flexion when they lie supine.15
Ligamentous attachments in children are stronger than bone. The strength of the bone will increase as the child ages and the bones mature. The vertebral column is intrinsically elastic, which may result in immediate self-reduction following a dislocation injury.2 Therefore, with its elasticity, the pediatric cervical spine can stretch more than the spinal cord.10 The vertebral column can tolerate several centimeters of distraction, whereas the spinal cord can only tolerate millimeters.14 This may account for why radiographs and CT scans can be normal in a patient with neurological findings.2 The muscles that support the spine also are underdeveloped, increasing cervical mobility and decreasing neck control.2,7,10 At approximately 8 years of age, the pediatric cervical spine begins to resemble that of an adult.1
Aside from the cervical spine, the pediatric airway also is different than an adult’s. The larynx is anterior, funnel-shaped, and much narrower.16 With blunt injury, pediatric patients can develop respiratory distress much faster than adults can, and even a small amount of swelling can be catastrophic.17 To maintain proper airway alignment during resuscitation, the plane of the patient’s face needs to be parallel to the bed. This may require padding the torso to keep the entire torso in neutral alignment with the spinal column and the airway patent.18
Mechanisms of Injury
Penetrating. Children with penetrating neck trauma account for only 0.28% of pediatric trauma patients.9 In a review of National Trauma Data Bank records on patients younger than 15 years of age, Stone et al found the most common mechanisms of injury were stabbings and gunshot wounds. Other mechanisms included falls onto sharp objects and dog bites. The majority of the patients were male with a mean age of 7.8 years. Almost 25% of these patients went directly to the operating room, and intubation occurred in the emergency department (ED) in 7.2% of patients.6 Vascular injury or hypotension while in the ED was associated with death.8 The most common associated injuries were to the aerodigestive system, followed by blood vessel damage and spinal cord injury.6 Younger children (0 to 5 years of age) tended to injure the aerodigestive system more often than older children, and 5- to 14-year-olds injured the vasculature, nerves, and cervical spine more frequently.6 CT scan was the tool used most frequently to diagnose penetrating neck injuries in pediatric patients, followed by laryngoscopy and esophagoscopy.6,8
Selective neck exploration should be used based on the physical examination to evaluate penetrating neck trauma in children.8,9 Hard signs of injury that mandate surgical exploration are active hemorrhage, a pulsatile or expanding hematoma, pulse deficit, massive subcutaneous emphysema, respiratory distress, shock, or airway compromise.9 The management of penetrating neck injuries in both adult and pediatric patients was previously dependent on the zone of injury. Recent studies have supported selective operative management in adults, and this theory has been adapted to pediatrics.6,9 In all hemodynamically stable patients without hard signs of vascular injury, a computed tomography angiography (CTA) is recommended prior to operative exploration.8,9
Blunt. Blunt trauma accounts for 95% of cervical spine injuries. Motor vehicle collisions (MVCs) are the leading cause of neck injury, causing between 11% and 62% of cervical spine injuries.14 The deceleration and hyperflexion/extension injuries in these accidents affect the cervical spine between the dens and C2 body, causing significant injury, which is worse in children younger than 8 years of age.13,14
The next leading cause of injury is pedestrians struck by vehicles. Falls also account for a significant portion of cervical injuries in younger children. Sports-related injuries were more common in older children.2,14 Other risk factors include diving or an increased axial load.19 Always consider nonaccidental trauma in young children with cervical injuries.2 In cases of child abuse, reports show an incidence of cervical spine injury between 5.6% and 13%.14
Tracheal trauma can occur after a clothesline injury or hockey puck injury. Sudden hyperextension of the neck causes the trachea to stretch and compress against the cervical spine. The rapid trauma forces followed by deceleration produce a shearing force between the airway, carina, and cricoid cartilage.7 Prioritize the airway in these patients; swelling is expected and can occlude the airway over time.17
Risk Factors
Children with syndromes associated with ligamentous laxity, cervical instability, or rheumatologic disorders are at higher risk for cervical spine injury.14 Of patients with Down syndrome, 10% to 20% have increased ligament laxity that can result in atlantoaxial instability.20 These patients also may have other developmental abnormalities of the spine, such as occipitalization of the atlas, atlantal arch hypoplasia, and os odontoideum.20 Patients with 22q11.2 deletion syndrome also can have congenital anomalies of the cervical spine. The location of these anomalies varies, but they are found most commonly between C1 and C3.21,22 Patients with Klippel-Feil syndrome are more predisposed to spinal instability because this syndrome is characterized by a short neck and decreased cervical range of motion.23
Age and sex are risk factors for injury as well. Males have a greater predominance of neck injuries than females.2 Children younger than 8 years have different injury patterns than those between 8 and 18 years.24 The older age group presents more similarly to adults, and subaxial injuries are the most common.24 In children 2 to 7 years of age, atlantoaxial rotatory subluxation and atlantooccipital dislocations are more common. The most common cervical spine injury in children younger than 2 years of age is atlantooccipital dislocation.24 In a 10-year review of the National Pediatric Trauma Registry, injuries of the upper cervical spine were found among all age groups, whereas injuries of the lower cervical spine were more prevalent in children older than 8 years.2
Initial Assessment and Stabilization
History
Obtain a comprehensive history to identify preexisting conditions, mechanism of injury, and symptoms post-injury. Past medical problems can reveal risk factors that would raise suspicion for neck injuries. Determining the mechanism of injury is paramount. Include a thorough review of systems, looking for signs of head injury or neurological symptoms. A history of loss of consciousness or neck pain is a risk factor associated with cervical spine injuries.19 Do not dismiss transient symptoms, such as paresthesia, a burning sensation in the hands, and a subjective feeling of generalized weakness or a lightning sensation down the spine with neck movement. Central cord syndrome that results from hyperextension injuries may present only with a burning sensation in the hands.14
Physical Examination
Follow the normal pattern of a trauma assessment, first performing a rapid head-to-toe examination and prioritizing the airway, breathing, circulation, and disability; stabilizing any acute life-threatening injury; and then returning for a more thorough evaluation. Obtaining a reliable examination can be difficult, especially in children younger than 5 years of age or in those with developmental delays.4 Performing a physical examination on a child who is upset also can be difficult and might not produce much useful information.3 If the situation allows, parents or child life specialists can help to calm the patient and obtain valuable information.
Take care to maintain in-line cervical stabilization, either manually or with a cervical collar. When in doubt, continue spine immobilization while completing the remainder of the examination and consult a subspecialist if concerns arise. When examining the cervical spine, have someone maintain manual stabilization while the midline of the cervical spine is palpated. Each vertebra should be palpated to assess for bony tenderness. A 2001 study in which National Emergency X-Radiography Utilization Study (NEXUS) criteria were applied to pediatric patients showed that midline neck tenderness was the most common abnormality in patients both with and without cervical spine injury.25 Despite the fact that some children with neck pain ultimately do not have cervical injury, it is still important to maintain spine immobilization until a full evaluation can be completed.
Do not forget to evaluate the remainder of the neck while someone else maintains in-line stabilization. Look for any skin abnormalities or signs of swelling. The hard signs of vascular injury include arterial bleeding, hemorrhagic shock, expanding or pulsatile hematoma, and a thrill or bruit over the injured area.26 If there is a vascular injury, it could expand to the point of compressing the airway, causing trouble breathing or swallowing. Remember to replace the cervical collar while performing the rest of the physical examination.
Up to 35% of patients with a cervical spine injury have an associated neurological injury.27 An initial rapid assessment of the cervical spine nerves to assess for neurological deficit can include elbow flexion (C5), dorsiflexion of the wrist (C6), and extension of the elbow (C7).3 Test sensation in the area over the deltoid (C5), the thumb (C6), the middle finger (C7), and the little finger (C8). The supraclavicular nerves and C2 through C4 provide sensory innervation to the region overlying the pectoralis muscle. The upper cervical dome dermatome C1-C4 can be variable in cutaneous distribution.28 Disruption of the cervical sympathetic chain, which begins between C7 and T1, may cause Horner syndrome.3
If the patient is able to speak, a hoarse voice may indicate a laryngeal injury. Stridor can indicate an airway injury.17 A seesaw respiratory pattern may represent injury to the diaphragmatic (C3, C4, C5) or intercostal nerves. Closely monitor vital signs. Spinal shock is characterized by bradycardia and hypotension.3 Respiratory distress, decreased oxygen saturation, or the need for intubation have been associated with cervical spine injuries.19 If the patient needs intubation or other advanced airway intervention, use a jaw thrust rather than a head tilt/chin lift maneuver to minimize movement of the cervical spine.
Always look for other injuries. Altered mental status, signs of basilar skull fracture, torso injury, and thoracic injury are associated with patients who have cervical spine injury.19 One-third of patients with cervical spine injury will have an associated head injury.19 Other findings that may be associated with neck injury are chin trauma, posterior teeth fractures, and injury to the mandible.14
Emergency Medical Services
When emergency medical services (EMS) arrives at the patient’s side, the EMS clinician needs to decide if a cervical collar or a long backboard is indicated. A summary of high-risk criteria for cervical spine injury can be found in Table 1. A study conducted by the Pediatric Emergency Care Applied Research Network revealed inconsistent EMS application of spinal precautions, particularly in children younger than 2 years of age.29 EMS will follow jurisdictional protocols, but there is some suggestion that having a cervical collar or long backboard placed in the prehospital setting increases the probability that the patient will be imaged in the ED.19
Table 1. A Compilation of the Key High-Risk Criteria that Should Raise Suspicion for Cervical Spine Injury |
|
|
Mechanism |
|
|
History |
|
|
Physical Exam |
|
If the EMS clinician suspects cervical injury based on the history, mechanism of injury, or physical examination findings, place a cervical collar. Provide gentle in-line manual immobilization, then apply a rigid collar.30 To perform manual stabilization, place hands on both sides of the patient’s head, with fingertips touching or gently resting on the clavicle, to maintain the cervical spine in neutral position. Do not apply traction. Have a second clinician determine the appropriate size cervical collar for the patient. This is imperative to maintain the neutral position. A collar that is too tall can cause excessive cervical extension, while a collar that is too short can cause excessive flexion. Proper sizing depends on the brand of collar; follow the manufacturer’s recommendations on sizing. Kreinest et al evaluated prehospital personnel and emergency physicians’ ability to properly place a cervical collar and found that only 11% of participants were able to carry out the task without error. The most common area of deficiency was adjustment of size.31
Rigid collars may not fit children exactly. The cervical collar should provide points of support for the chin, angle of the jaw, mastoid process, and occiput. If a premade cervical collar is not available or the fit is improper, place a rolled towel around the neck, crossed in the front and secured with tape.2,32 Children may become agitated and fight having a cervical collar put on. Resisting may cause more harm than benefit. Depending on the child’s behavior, the provider may need to provide manual in-line stabilization initially while the child is able to find a comfortable position.2,32 If the patient presents with a deformity or torticollis, let the patient get into a comfortable position before immobilization; attempting to align such a patient’s spine for purposes of immobilization can cause pain or even spinal cord damage.30
For athletic injuries that occur while the patient is wearing a helmet and shoulder pads, leave this equipment on unless there is airway compromise. If an airway emergency requires helmet removal, direct close attention toward maintaining the cervical spine in a neutral alignment until the shoulder pads can be removed.
Studies examining the utility of cervical collars have been contradictory.33 Extension of the cervical spine in some conditions, such as ankylosing spondylitis, can cause significant harm.2 Cervical collars also may cause further atlantooccipital distraction and have the potential to worsen neurological injury in such cases.2 Cervical collars can increase intracranial pressure by compressing the jugular veins, which may cause additional harm to a patient with a head injury.34 Collars may restrict respiration and lead to compromised mouth opening, making airway management more challenging.33 Despite these recognized risks, cervical spine immobilization with cervical collars still is recommended when cervical spine trauma is suspected.
Full spine immobilization historically has included a cervical collar and a long backboard. Potential detriments of full spine immobilization include increased pain, airway compromise, and pressure ulcers.32,35 Positioning the patient completely flat can lead to a decrease in forced vital capacity. Also, given the relatively large head of a child, the spine board can cause cervical flexion of more than 10 degrees.14,32 Thoracic elevation may alleviate this iatrogenic flexion.18 Skin breakdown can occur in a relatively short amount of time.32 Also, the pain caused by spinal immobilization may be mistaken for pain related to the accident, thereby increasing diagnostic imaging and associated radiation exposure.32,33,36
The National Association of EMS Physicians (NAEMSP) and the American College of Surgeons Committee on Trauma (ACS-COT) developed a joint position paper on EMS spinal precautions.32 The benefits of long backboards have not been proven.32 A spine board is recommended for an adult patient who has suffered blunt trauma and has an altered level of consciousness, spine pain or tenderness, neurological complaints, spine deformity, or a significant mechanism of injury with intoxication, inability to ambulate, or a distracting injury.32 A long spine board or pediatric spine board should be used for pediatric patients in these scenarios as well. Patients with penetrating trauma to the head, neck, or torso and without evidence of spinal cord injury on initial EMS examination do not need to be immobilized on a backboard. Patients who are ambulatory but require spinal precautions can have a cervical collar applied and be secured appropriately to the EMS stretcher.32
The development and validation of spinal immobilization guidelines in the pediatric population have been identified as a priority area for prehospital research.35 Pediatric experts have argued that a rigid cervical collar alone with proper restraint to the stretcher may be sufficient for prehospital transport of children with a normal neurological examination.36 This expert opinion still does not align with the National Highway Traffic Safety Administration (NHTSA) guidelines for the transport of younger pediatric patients, which state that a long board properly restrained to the stretcher is the safest way to transport children with suspected spinal injuries.37 EMS clinicians ultimately will follow the jurisdictional protocol to determine how best to transport their patient, but alignment of NAEMSP, ACS-COT, and NHTSA on recommendations would be optimal. The question remains if it is necessary to use a backboard for a neurologically intact pediatric patient without spine pain or tenderness, intoxication, or a distracting injury.
ED Evaluation
Once the patient arrives in the ED, a thorough history and physical examination with an emphasis on the key points outlined previously should be completed. If the patient arrives on a long backboard, use log roll movements while maintaining cervical stabilization to transfer the patient to the hospital stretcher. The patient should be taken off the backboard as soon as possible to prevent complications.32
When children present with respiratory distress and tracheal injury, options for definitive airway management include flexible fiberoptic intubation or tracheostomy.7 There are case reports of posterior tracheal tears after blunt neck trauma.38 Occasionally, these can be treated conservatively with intubation and observation, but larger tears may require thoracoscopic repair.38
If the patient arrives to the ED in a cervical collar, leave the collar in place until all assessments are complete and an informed decision regarding collar removal can be made. If the patient did not arrive by EMS and there is concern for a cervical spine injury, then a cervical collar should be placed. If the cervical spine cannot be cleared clinically on the initial ED exam, the collar should be left on and the patient should be reevaluated at a later time.1 However, prolonged time in a cervical collar can lead to skin breakdown.4
Concerns exist that there is a small percentage of patients who have a reassuring initial evaluation and later show neurologic deterioration that may have been related to patient movement or inadequate immobilization.27 This shows the importance of maintaining cervical immobilization during the entire evaluation.27 Lapses in cervical spine immobilization during the initial ED resuscitation occurred in 71.4% of patients in one small, observational study.27 Coordination of team members can help to decrease lapses in immobilization. Children who received oxygen therapy had more lapses in immobilization compared to children who did not.27
Cervical spine clearance is also not an emergency.1 Once the patient has been stabilized and all life-threatening conditions have been addressed, a physician should determine if it is safe to remove the cervical collar or if imaging is warranted. Cervical spine clearance should be a clinical event, not a radiological event.1 Clearing the spine clinically involves having a reliable examination, no midline neck pain or tenderness, a normal neurological examination without distracting injuries, and no risk factors based on the history or mechanism of injury.
Clinicians may feel uncomfortable with their physical examination skills of the young child and rely heavily on imaging, including radiograph and CT scan.5 The risks and benefits of each imaging modality should be weighed carefully. Unfortunately, in pediatrics, there is no validated clinical decision tool or management strategy.1 Imaging recommendations also are variable.4 Current pediatric decision tools are based on expert consensus after consideration of adult guidelines.5
Clearing the Cervical Spine
Adult protocols for clearing the cervical spine have not been well validated in pediatrics.3 In adults, cervical spine protocols have been shown to reduce the number of missed injuries and limit the need for radiographs and CT scans, leading to decreases in both radiation exposure and time to removal of the cervical collar.4 The Pediatric Cervical Spine Study Group published that only 46% of pediatric level I trauma centers adhered to a written protocol for clearing the pediatric cervical spine.4 It also was noted that there was a wide variability in the protocols and in the use of CT scanning.3
There are two large, well-validated cervical spine clearance rules for adults: the NEXUS cervical spine criteria and the Canadian Cervical Spine Rule. All patients in a trial of the Canadian Cervical Spine Rule were older than 16 years, limiting the applicability of the rule’s findings to pediatrics.14 The NEXUS trial did include patients younger than 18 years, suggesting that the NEXUS criteria could be more applicable to children. In adults aged 18-55 years, the NEXUS criteria for cervical spine clearance have been well validated. The NEXUS criteria recommend that cervical spine radiography be obtained in trauma patients unless all of the following are present: no posterior midline cervical spine tenderness, no evidence of intoxication, normal level of alertness, no focal neurological deficits, and no painful, distracting injuries.24 It is important to note that distracting injury is a subjective variable. NEXUS is the best clinical guide that has been studied, but its use as a pediatric protocol is not recommended and has not been validated.24 The NEXUS criteria are potentially useful in children older than 8 years, but use caution in applying the criteria to younger children.
The problem with applying NEXUS criteria to the pediatric population is that only 2.5% of the entire study population were younger than 8 years and only 1.3% of the entire study population were both younger than 8 years and had cervical spine injury.14 Viccellio et al examined 3,065 pediatric patients prospectively looking to evaluate the NEXUS criteria. Only 30 children had cervical spine injury and all had at least one risk factor in the NEXUS criteria. However, none of the children with cervical spine injury were younger than 2 years of age, and only four children were younger than 9 years old.25 Adding into consideration that only 88 children total were younger than 2 years in the study, there is concern with extrapolating these findings.1 Of the NEXUS criteria, the two most common positive findings in children were cervical tenderness and the presence of distracting injuries.25
Rozzelle et al published guidelines that recommended clinical clearance if the child is alert and interactive without neurological deficit, neck tenderness, distracting injury, or intoxication.39 In children who did not meet those criteria, radiographs were recommended. In patients younger than 9 years, only anteroposterior (AP) and lateral views were suggested. Adding an odontoid view may increase sensitivity in children older than 9 years.1
The National Institute for Health and Care Excellence guidelines suggest avoiding CT scans unless any of the following are present40:
- Glasgow Coma Scale (GCS) less than 13 on initial assessment;
- intubated;
- focal neurological examination;
- paresthesia;
- a definitive diagnosis is needed urgently;
- the patient is having other body areas scanned for head injury or multisystem trauma;
- there is a strong clinical suspicion despite normal radiographs;
- plain radiographs are technically difficult or inadequate;
- plain films identify significant bony injury.
Children who have neck pain or tenderness and do not meet the CT criteria should have a three-view spine radiograph according to these guidelines.41 There is concern that the application of these guidelines may result in increased use of CT imaging without an apparent increase in specificity.5
Kavuri et al evaluated data from three separate cervical spine clearance protocols used by Drexel University College of Medicine over several years. Initially, there was liberal use of radiographs and CT scans. The protocol developed in 2014 placed more emphasis on repeat clinical examination and on decreasing CT use to the point where CT scans were not ordered without consultation with the spine service. The use of CT scans decreased from 90% to 28.7%. The Drexel team also proposed a “next day” examination to provide a more accurate and sensitive assessment before additional imaging was ordered.3
Arbuthnot and Mooney conducted a retrospective review of all children younger than 21 years who were admitted over a 10-year period and underwent cervical spine clearance using the institutional algorithm at Boston Children’s Hospital. In this algorithm, if the patient has a normal neurological examination, is cooperative with the examination, denies any neck tenderness or pain with palpation, and is able to range the head fully with no problems, the patient’s cervical spine is considered cleared. If the patient fails any of those criteria, a lateral cervical spine radiograph is obtained. If the lateral film is normal, an AP view is obtained, with an odontoid view added for children older than 5 years. The 5-year age cutoff for obtaining an odontoid view was specific to this institutional algorithm. If the radiographs are normal and the patient is still unable to pass the clinical examination, then the collar remains in place and the patient is reevaluated later. If at reevaluation, the child still is unable to be cleared clinically and there is a high suspicion of injury, a spine consult is obtained. If there is low suspicion for injury, the patient can be discharged with a cervical collar and outpatient follow-up at 7-14 days in the spine clinic. The patient also can be reevaluated sooner if they require admission for another reason.1
In the Boston algorithm, if the child is found to have a neurological deficit, an immediate spine or neurosurgical consult is obtained. If the child is unresponsive, clinicians obtain a lateral cervical spine film. If the lateral film is normal and the patient wakes up, then the cervical spine can be cleared in the same manner as if the child had presented alert. If the child is not expected to return to a normal mental status for a prolonged time period, an AP view is added and a spine MRI is considered, preferably within the first 48 hours after the injury. If the MRI is normal, the collar can be removed.1
The Boston algorithm showed 94.4% sensitivity and 99.9% negative predictive value. The injury that was missed was a spinous process tip fracture in a teenager who was kept in a cervical collar as treatment. Arbuthnot and Mooney also performed a subanalysis on children younger than 3 years and found that, of 135 children with an average age of 1.6 years, 43 (31.9%) were able to be cleared without imaging. One child had a CT scan. Ninety-one (67.4%) of the patients younger than 3 years had plain films done, with only one injury evident on radiograph.1
The Pediatric Emergency Care Applied Research Network conducted a retrospective, case-control study looking at risk factors for cervical injury in blunt trauma patients and found that altered mental status, focal neurological findings, neck pain, torticollis, torso injury, diving, and high-risk MVC were conditions that predisposed to cervical spine injury.42 Using these criteria as a study tool, Leonard et al found that imaging could have been decreased by at least 25%.42
Imaging
Rozzelle et al recommended no imaging in children older than 3 years if they are alert and neurologically intact, have no midline tenderness without distracting injury, and are not hypotensive or intoxicated. The group also recommended not imaging children younger than 3 years with GCS greater than 13, who are neurologically intact without posterior midline tenderness and no distracting injuries, are not hypertensive or intoxicated, and were not in an MVC, in a fall greater than 10 feet, or a victim of nonaccidental trauma.39
Children younger than 3 years present the most challenge for assessment since they may not be reliable to participate in the clinical examination and also have a higher susceptibility to radiation.1 Pieretti-Vanmarcke et al performed a retrospective review of children younger than 3 years with blunt injury. The rate of cervical spine injury was 0.66%.43 This group devised clinical criteria that were predictive of injury that included cumulative GCS less than 14, eye subset GCS 1, MVC, and age 2 years and older.1 The criteria were applied to 12,537 children, and the authors concluded that one-third of these children could be cleared without any imaging.14
Radiographs. Plain radiographs are sufficient to screen for cervical spine injuries.1,44 A previous study suggested that a cervical spine radiograph has a sensitivity up to 90% in detecting an abnormality after blunt trauma.45 Lateral or AP and lateral films should be done on patients who require imaging for cervical clearance. In children older than 8 years, the odontoid view can be added. The odontoid view requires a child to be able to fully open the mouth.41 In children younger than 8 years or who cannot open their mouth for an odontoid view, a Waters’ view through the foramen can be helpful to further visualize the odontoid and upper cervical spine.14 Other studies and institutional protocols have used 5 years, 8 years, or 9 years as age criteria for obtaining an odontoid view.1,14,41 Flexion and extension films do not have a role in the acute setting, but they are important at subspecialty follow-up evaluation to help determine the stability of the cervical spine.2
A good-quality radiograph requires visualization of all seven vertebrae. The changes seen radiographically related to growth can make plain films difficult to interpret without the appropriate training.4 Normal anatomical variations in children include absent lordosis, nonossified posterior spinal elements, ligamental laxity, and C2-C3 pseudosubluxation.2,14
When reviewing the cervical spine films, first check to make sure that the C7-T1 junction is visible. Typically, adults will have a slight forward arch in the cervical spine, which provides stability and helps bear the weight of the spine. This normal lordosis may be absent in children up to 16 years of age.
The atlas vertebrae develop from three distinct ossification centers: one for the anterior arch and two for the lateral masses. The ossification centers appear by 1 year and fuse by 7 years.14 The axis has five ossification centers: one for the centrum, two for the posterior arches, and two for the odontoid process.14 The odontoid is separated from the body of the axis at birth by cartilage.12 The tip of the odontoid process first appears at age 7 years and fuses to the dens at 12 years. The ossification centers of the dens fuse before birth and join the centrum at 5 to 7 years, causing a persistent synchondrosis.14 C2 consists of five ossification centers separated by six synchondroses which close between the ages of 7 and 13.5 years.2 The remainder of the cervical vertebrae have four ossification centers, which unite in the midline between 2 and 4 years and produce a neurocentral synchondroses between 3 and 6 years.14 Synchondroses can be mistaken for fractures, but remember that fractures also can occur in this area.2 The growth centers at the tip of the spinous process also can resemble fractures.12
The distance and alignment between vertebrae varies between adults and children. When interpreting a cervical spine radiograph, disruption of any of the four curvilinear alignment lines can raise concern for possible cervical spine injury. These lines include the anterior vertebral body line, posterior vertebral body line, spinolaminar line, and the line of the tips of the spinous process.14 The predental space (between the odontoid process and anterior arch of the atlas) is less than 3 mm in adults and 5 mm in children. A predental distance of greater than 5 mm implies rupture of the transverse ligament.46 Radiologists also can measure the interspinous ratio. This is the distance between C1 and C2 compared to the distance between C2 to C3. If the ratio is more than 2.5, there is a sensitivity of 87% and a specificity of 100% for tectorial membrane disruption.14 A basion-dental interval also can be measured. If the distance is 12 mm or greater, there is concern for disassociation.46 The line of Swischuk, which is drawn between the anterior aspect of the C1 and C3 spinous processes, helps differentiate between subluxation and pseudosubluxation, the latter of which is related to the elasticity of the cervical spine in pediatrics. The anterior aspect of the C2 spinous process should be within 2 mm of this line. If the distance is greater than 2 mm of displacement, then it is a true dislocation.14,46
All vertebrae should be examined for fracture, collapse, or avulsion. The disc spaces should be evaluated for symmetry.46 The cervical vertebrae are spherical at birth and over the years will develop the classical rectangular shape as the bone ossifies. This natural process of ossification causes the pediatric spine to have a wedge appearance, which can be mistaken for an anterior wedge fracture.2
Remember to look at all portions of the radiograph, not just the bone. When looking at the soft tissue, prevertebral swelling should be less than two-thirds of the adjacent vertebral width. Another way to remember this is that the prevertebral space should be less than 7 mm anterior to C2 and less than 2 cm anterior to C7.47 In adults, prevertebral soft tissue thickening could be indicative of injury, but in the pediatric patient, thickening may be seen during exhalation or flexion and is especially prominent during crying.2
Computed Tomography. In adults, CT scans detected 98% of cervical spine injuries; this could be increased to 100% when adding radiographs.1 A CT scan is indicated when there are inadequate radiographs in concerning situations, bony injury is seen on radiograph, or there is a high clinical suspicion of bony injury that requires a time-sensitive diagnosis.5,14 A survey of the Pediatric Cervical Spine Study Group showed that at 46% of participating institutions, CT imaging was the most common primary modality for cervical spine clearance. Only 12% of responding institutions used a combination of CT and radiographs.4
Because of radiation concerns, CT scans should be protocolized to use “as low as reasonably achievable” radiation doses.41 The thyroid glands are some of the most radiosensitive organs.48 The highest radiation risk is for children younger than 2 years.1 Jimenez et al concluded that the risk of developing thyroid cancer doubled in patients who had a CT scan and the highest risk was in children younger than 5 years.49 Another study cited a 24% increase in risk of developing malignancy after cervical CT scans.5 The rate ratios for solid tumors after a CT of the cervical spine is 1.13 and 1.78 for thyroid cancer.35 Studies also have shown that approximately one fatal cancer results for every 1,000 CT scans performed during childhood.3,4 Patients who are younger and those involved in higher-energy MVCs are exposed to greater radiation, likely because of CT scans being ordered more frequently on those patients.3 A CT scan of the neck delivers up to 200 times the radiation of the three-view cervical radiograph,25 further adding to the evidence that perhaps CT scans should be used judiciously in the pediatric neck trauma patient.
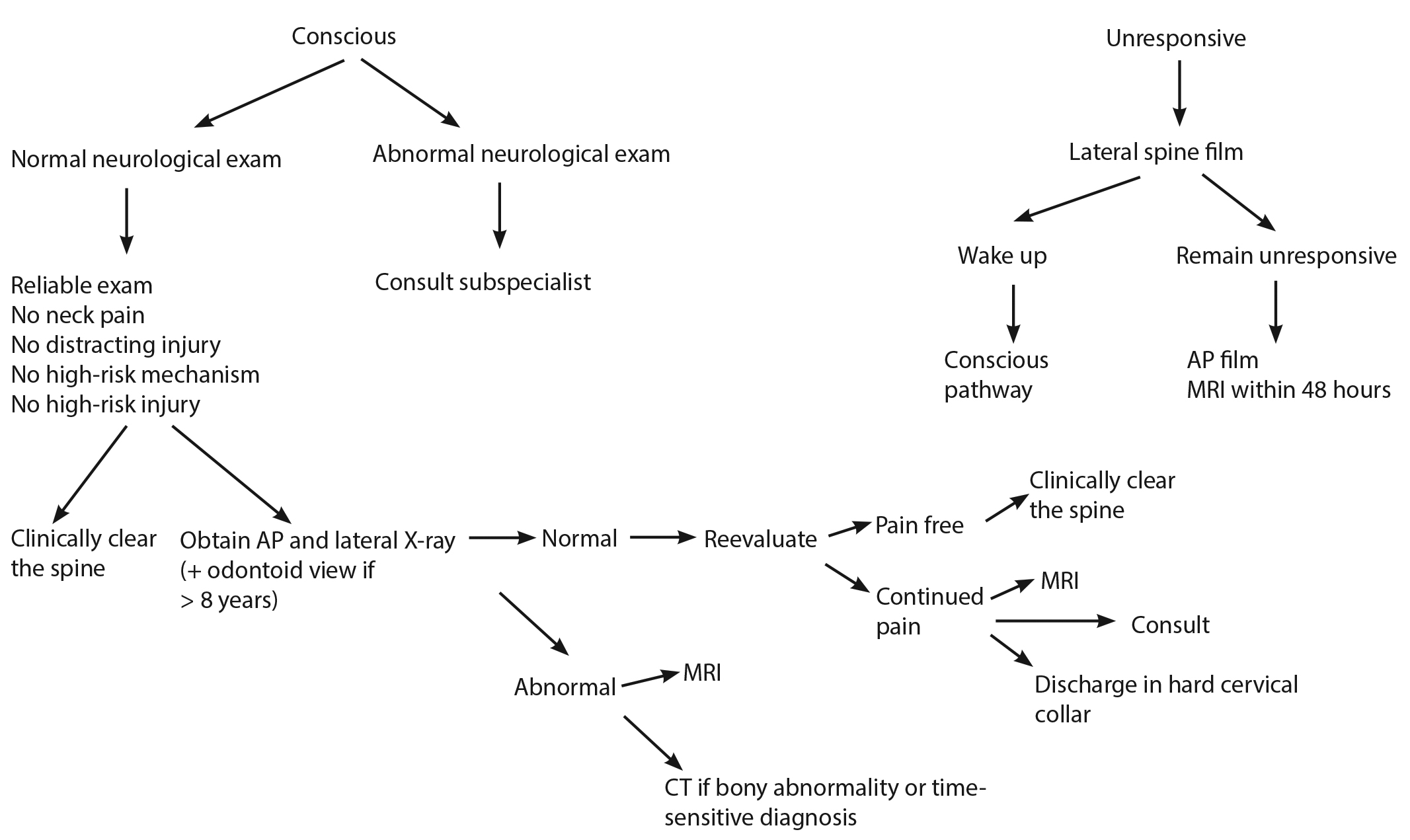
The incidence of pediatric cervical injuries in the neurologically intact child with a normal examination is lower than the incidence of radiation-induced malignancy.1 One published approach to decreasing radiation exposure is to obtain a CT down to C3 when a head CT is being obtained, which would reduce the overall radiation exposure approximately three-fold.14 Figure 1 provides a summary of all of the imaging studies recommended based on the patients mental status and exam.
Figure 1. A Proposed Flowchart for Clearance of the Pediatric Cervical Spine |
 |
|
This was developed based on the compilation of algorithms in this article. This is not meant to guide clinical care and has not been validated. This is only meant to be a summary of the articles presented here. |
Computed Tomography Angiography. A CTA should be obtained if there is concern for vascular injury. If there is concern for a blunt cerebrovascular injury in an adult patient, the Denver and Memphis screening criteria are applied to determine whether CTA is needed. The Denver criteria include arterial neck bleeding or expanding hematoma, bruit, neurological exam findings not consistent with head CT findings, stroke detected on subsequent CT scans, focal neurological deficits, diffuse axonal injury with a GCS of 6 or less, cervical spine fracture, LeFort II or III fractures, basilar skull fractures or soft tissue neck injuries, including seat belt injuries, hanging, or hematomas. The Memphis criteria add two additional criteria: Horner’s syndrome and previous cervical fracture. One positive finding using either of these criteria had an increased risk for blunt carotid artery injury in adults and CTA was recommended.50 Mallicote et al conducted a nine-year retrospective study looking at more than 80,000 pediatric trauma patients from the National Trauma Data Bank and found that, had the Denver and Memphis criteria been applied, there would have been negative CTAs in 97.4% of patients, suggesting that further criteria need to be defined for the pediatric setting.50 A study from 2009 showed that CTA is highly specific, sensitive, and accurate for detecting pediatric neck and vascular trauma.26 For blunt trauma, CTA was 88% sensitive and 100% specific and had a negative predictive value of 97%. For penetrating injuries, the sensitivity was 100% and specificity was 93%.26
Magnetic Resonance Imaging. MRI is superior to CT scan in examining the spinal cord and soft tissues.14 The imaging sequences should include a sagittal T1 and Short-TI Inversion Recovery and axial T2 weighted images at a baseline.2 An MRI should be obtained if the patient is nonverbal and obtunded with a concerning mechanism of injury, radiographs are equivocal, the patient has neurological findings, or there is an inability to clinically clear the cervical spine within three days of injury.1,2,10,14
Even if radiographs and CT scans are unremarkable, MRI still should be considered for patients with persisting neurologic symptoms after trauma. MRI can be helpful diagnostically as well as prognostically.10 Drawbacks of MRI include the time needed to perform the scan, the time the child is away from the ED, the possible need for sedation, and the limited availability of MRI in general. Despite these pitfalls, MRI does remain the gold standard for identifying injuries to the cervical spine.2
Spinal Cord Injury Without Obvious Radiologic Abnormality. Spinal cord injury without obvious radiologic abnormality (SCIWORA) was first defined in 1982 and included children in whom there were no abnormalities on plain films, CT scans, and even myelography at the time of admission but who had objective signs of spinal cord injury.10,51 SCIWORA is more common in young children, making up 17% to 20% of cervical spine injuries in children age 0-3 but only 5% of cervical spine injuries in teenagers. It is identified more frequently in the cervical spine than the thoracic or lumbar spine.10,51 Children with SCIWORA have other injuries in up to 50% of cases.10 SCIWORA injuries typically result from flexion/extension, rupturing the anterior longitudinal ligament and causing rapid dislocation/reduction of the vertebrae. The extension causes the ligamentum flavum to buckle and possibly compress the spinal cord.2 External fixation is the treatment for the majority of these injuries.2 Steroids are no longer indicated in the treatment of acute spinal cord injuries.1,10 The typical treatment for cervical spine SCIWORA is a hard collar for 12 weeks.10 As MRI has become more widely available and utilized, the incidence of SCIWORA has decreased.10,14 With the widespread use of MRI and increased injury detection, the term SCIWORA has become outdated.51 MRI images have been able to show soft tissue, ligamentous, and spinal cord injuries almost immediately. MRI is highly sensitive for cervical injury, but there also are a high number of falsely positive findings. An abnormal MRI does not necessarily correlate with cervical instability; however, an MRI showing no ligamentous instability in the cervical spine does strongly correlate with cervical stability.51
Specific Injury Patterns
Atlantooccipital dislocation occurs three times more often in children than in adults, likely due to the larger head and other previously described anatomical differences. Eighty percent of children with atlantooccipital dislocation will have an abnormal neurological examination at the time of presentation. High cervical cord injuries can cause flaccid paralysis, sensory changes, breathing problems, priapism, bowel and bladder incontinence, and neurogenic shock. Definitive treatment is controversial, but most likely will include internal fixation. If internal fixation is not possible, a halo is used.2
Atlantoaxial dislocation also can be seen in pediatrics and presents similarly to atlantooccipital dislocation. This injury will be seen on CT scan, but MRI is needed to assess the transverse atlantal ligament of C1. Early stabilization is key. Many of these injuries are treated with halo devices and heal without surgery.2
The shallow articulation of C1 and C2 and highly elastic ligaments predispose children to atlantoaxial rotary fixation. This can occur with minor trauma, spontaneously, or after an upper respiratory infection.2 In the setting of trauma, the ligaments can be disrupted and there is a larger degree of dislocation, which can manifest with neurological deficits.
Odontoid fractures have a different pathophysiology in children compared with adults. Fractures involving the synchondroses typically heal well with external fixation. Odontoid fractures in pediatrics typically are not associated with neurological deficit.2 Os odontoideum is characterized by separation of part of the odontoid process from the remaining part, which is associated with the body of the axis. In trauma, the os odontoideum can compress the spinal cord.2 Also, subaxial injuries are seen more commonly in children older than 8 years, with patterns resembling those in adult patients.2
Carotid artery dissection is seen most in the distal cervical carotid artery or in the proximal segments of the vertebral artery. Emboli can be thrown due to aneurysm or pseudoaneurysm and can cause transient ischemic attacks or stroke. If the sympathetic chain is damaged, Horner syndrome may develop. Treatment remains controversial but may include aspirin or clopidogrel. Endovascular management is continuing to develop. Follow-up for these injuries can be with ultrasound or magnetic resonance angiography.2
Disposition
Cervical spine injuries can have serious and long-lasting consequences. There is a balance between diagnosing these low-frequency injuries and being overly cautious. If a complete evaluation shows no significant injury, but the patient continues to have cervical pain and is at low risk for neurological injury, the patient may be discharged home in the hard cervical collar to be evaluated initially by the primary care doctor. If the patient continues to have persistent tenderness, neurologic symptoms, or concerning examination findings, then they would be referred to a subspecialist.52 If an injury to the neck is found, contact the institutionally appropriate consultant. If the patient has neurological symptoms that have since resolved and the MRI is normal, the patient typically is sent home in a hard collar for one to two weeks with close follow-up. Patients with an abnormal MRI, vascular injury, or trauma to other areas of the body require admission to a pediatric trauma center.
Prognosis
The mortality associated with pediatric cervical spine injuries ranges from 4% to 41%.1 The prognosis depends on the level of injury. The mortality is 33% with upper cervical spine injury vs. 8.3% in lower cervical spine injuries.2 Of patients with cervical spine injury, 30% to 67% will have neurological deficits and 66% will have associated injuries to the head or other major organ systems.1 In addition to the deficits caused by the initial injury, affected patients may develop paralytic scoliosis or cervical kyphosis secondary to laminectomy. All cervical spine injuries have high medical, social, and psychological costs.24
Conclusion
Pediatric neck trauma is a rare event, but with devastating consequences. The approach to a neck trauma patient should start — as with any trauma patient — with a history- and trauma-based physical examination looking for risk factors predisposing the patient to cervical injury and looking for neurological deficits. In patients who have suspected cervical trauma, a cervical collar should be placed. If the spine is unable to be cleared clinically, radiographs are a useful first test. CT scans should be limited to decrease pediatric radiation exposure. When there is an abnormal neurological examination, MRI should be performed. Future research is needed in developing a universal, comprehensive tool for clearing the pediatric spine and determining the appropriate imaging studies. In the meantime, having an institutional protocol may be beneficial in decreasing radiography, thereby decreasing exposure to radiation and improving patient care.
REFERENCES
- Arbuthnot M, Mooney DP. The sensitivity and negative predictive value of a pediatric cervical spine clearance algorithm that minimizes computerized tomography. J Pediatr Surg 2017;52:130-135.
- Copley PC, Tilliridou V, Kirby A, et al. Management of cervical spine trauma in children. Eur J Trauma Emerg Surg 2019;45:777-789.
- Kavuri V, Pannu G, Moront M, et al. “Next day” examination reduces radiation exposure in cervical spine clearance at a level 1 pediatric trauma center: Preliminary findings. J Pediatr Orthop 2019;39:e339-e342.
- Pannu GS, Shah MP, Herman MJ. Cervical spine clearance in pediatric trauma centers: The need for standardization and an evidence-based protocol. J Pediatr Orthop 2017;37:e145-e149.
- Davies J, Cross S, Evanson J. Radiological assessment of paediatric cervical spine injury in blunt trauma: The potential impact of new NICE guidelines on the use of CT. Clin Radiol 2016;71:844-853.
- Stone ME Jr, Farber BA, Olorunfemi O, et al. Penetrating neck trauma in children: An uncommon entity described using the National Trauma Data Bank. J Trauma Acute Care Surg 2016;80:604-609.
- Nicholson B, Dhindsa H, Seay L. Pediatric blunt neck trauma causing esophageal and complete tracheal transection. Prehosp Emerg Care 2017;21:257-262.
- Abdelmasih M, Kayssi A, Roche-Nagle G. Penetrating paediatric neck trauma. BMJ Case Rep 2019;12:e226436.
- Tessler RA, Nguyen H, Newton C, Betts J. Pediatric penetrating neck trauma: Hard signs of injury and selective neck exploration. J Trauma Acute Care Surg 2017;82:989-994.
- Farrell CA, Hannon M, Lee LK. Pediatric spinal cord injury without radiographic abnormality in the era of advanced imaging. Curr Opin Pediatr 2017;29:286-290.
- Mandadi AR, Koutsogiannis P, Waseem M. Pediatric spine trauma. In: StatPearls [Internet] 2019 Mar 4. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK442027/
- McAllister AS, Nagaraj U, Radhakrishnan R. Emergent imaging of pediatric cervical spine trauma. Radiographics 2019;39:1126-1142.
- Orenstein JB, Klein BL, Gotschall CS, et al. Age and outcome in pediatric cervical spine injury: 11-year experience. Pediatr Emerg Care 1994;10:132-137.
- Gopinathan NR, Viswanathan VK, Crawford AH. Cervical spine evaluation in pediatric trauma: A review and an update of current concepts. Indian J Orthop 2018;52:489-500.
- Herzenberg JE, Hensinger RN, Dedrick DK, Phillips WA. Emergency transport and positioning of young children who have an injury of the cervical spine. The standard backboard may be hazardous. J Bone Joint Surg Am 1989;71:15-22.
- Harless J, Ramaiah R, Bhananker SM. Pediatric airway management. Int J Crit Illn Inj Sci 2014;4:65-70.
- Abid ES, Miller KA, Nagler J. Blunt laryngeal injury in a teenage hockey player. J Emerg Med 2019;57:e58-e87.
- Mellick LB. Open airway, neutral cervical spine. Pediatr Emerg Care 2016;32:e7-e8.
- Leonard JC, Browne LR, Ahmed FA, et al. Cervical spine injury risk factors in children with blunt trauma. Pediatrics 2019;144:e20183221.
- Ali FE, Al-Bustan MA, Al-Busairi WA, et al. Cervical spine abnormalities associated with Down syndrome. Int Orthop 2006;30:284-289.
- Hamidi M, Nabi S, Husein M, et al. Cervical spine abnormalities in 22q11.2 deletion syndrome. Cleft Palate Craniofac J 2014;51:230-233.
- Ricchetti ET, States L, Hosalkar HS, et al. Radiographic study of the upper cervical spine in the 22q11.2 deletion syndrome. J Bone Joint Surg Am 2004;86:1751-1760.
- Kenna MA, Irace AL, Strychowsky JE, et al. Otolaryngologic manifestations of Klippel-Feil syndrome in children. JAMA Otolaryngol Head Neck Surg 2018;144:238-243.
- Slaar A, Fockens MM, Wang J, et al. Triage tools for detecting cervical spine injury in pediatric trauma patients. Cochrane Database Syst Rev 2017;12:1-28.
- Viccellio P, Simon H, Pressman BD, et al. A prospective multicenter study of cervical spine injury in children. Pediatrics 2001;108:e20.
- Hogan AR, Lineen EB, Perez EA, et al. Value of computed tomographic angiography in neck and extremity pediatric vascular trauma. J Pediatr Surg 2009;44:1236-1241.
- Ahmed OZ, Webman RB, Sheth PD. Errors in cervical spine immobilization during pediatric trauma evaluation. J Surg Res 2018;228:135-141.
- Lee MWL, McPhee RW, Stringer MD. An evidence-based approach to human dermatomes. Clin Anat 2008;21:363-373.
- Kim EG, Brown KM, Leonard JC, et al. Variability of prehospital spinal immobilization in children at risk for cervical spine injury. Pediatr Emerg Care 2013;29:413-418.
- American College of Surgeons (ACS). Advanced Trauma Life Support: Student Course Manual. 9th ed. ACS; 2012: 174-205; 246-269.
- Kreinest M, Goller S, Rauch G, et al. Application of cervical collars — an analysis of practical skills of professional emergency medical providers. PLoS One 2015;10:1-7.
- White CC 4th, Domeier RM, Millin MG, et al. EMS spinal precautions and the use of the long backboard — resource document to the position statement of the National Association of EMS Physicians and the American College of Surgeons Committee on Trauma. Prehosp Emerg Care 2014;18:306-314.
- Sundstrom T, Asbornsen H, Habiba S, et al. Prehospital use of cervical collars in trauma patients: A critical review. J Neurotrauma 2014;31:531-540.
- Lemyze M, Palud A, Favory R, Mathieu D. Unintentional strangulation by a cervical collar after attempted suicide by hanging. Emerg Med J 2011;28:532.
- Ward CE, Badolato GM, Breslin K, et al. Evaluation of a selective prehospital pediatric spinal protection protocol. Prehosp Emerg Care 2019;23:862-869.
- Chang CD, Crowe RP, Bentley MA, et al. EMS providers’ beliefs regarding spinal precautions for pediatric trauma transport. Prehosp Emerg Care 2017;21:344-353.
- Working Group Best-Practice Recommendations for the Safe Transportation of Children in Emergency Ground Ambulances. National Highway Traffic Safety Administration; September 2012. https://www.nhtsa.gov/staticfiles/nti/pdf/811677.pdf
- Mener DJ, Stewart FD, Tunkel DE. Tracheal tear from blunt neck trauma in children: Diagnosis and management. Int J Pediatr Otorhinolaryngol 2017;96:100-102.
- Rozzelle CJ, Aarabi B, Dhall SS, et al. Management of pediatric cervical spine and spinal cord injuries. Neurosurgery 2013;72:205-226.
- National Institute for Health and Care Excellence (NICE). Head injury: Assessment and early management. NICE; 2014. Updated September 2019. https://www.nice.org.uk/guidance/cg176/resources/head-injury-assessment-and-early-management-pdf-35109755595493
- Abela N, Herrieven E. Fifteen-minute consultation: Imaging in paediatric major trauma. Arch Dis Child Educ Pract Ed 2020. doi:10.1136/archdischild-2019-318247
- Leonard JR, Jaffe DM, Kuppermann N, et al. Cervical spine injury patterns in children. Pediatrics 2014;133:e1179-e1188.
- Pieretti-Vanmarcke R, Velmahos GC, Nance ML, et al. Clinical clearance of the cervical spine in blunt trauma patients younger than 3 years: A multi-center study of the American Association for the Surgery of Trauma. J Trauma 2009;67:543-549; discussion 549-550.
- Somppi LK, Frenn KA, Kharbanda AB. Examination of pediatric radiation dose delivered after cervical spine trauma. Pediatr Emerg Care 2018;34:691-695.
- Nigrovic LE, Rogers AJ, Adelgais KM, et al. Utility of plain radiographs in detecting traumatic brain injuries of the cervical spine in children. Pediatr Emerg Care 2012;28:426-432.
- Partyka C. C-spine x-ray interpretation. Don’t forget the bubbles; 2017. doi:10.31440/DFTB.13656
- Vermess D, Rojas CA, Shaheen F, et al. Normal pediatric prevertebral soft-tissue thickness on MDCT. AJR Am J Roentgenol 2012;199:W131-W133.
- Sinnott B, Ron E, Schneider AB. Exposing the thyroid to radiation: A review of its current extent, risks, and implications. Endocr Rev 2010;31:756-773.
- Jimenez RR, Deguzman MA, Shiran S, et al. CT versus plain radiographs for evaluation of c-spine injury in young children: Do benefits outweigh risks? Pediatr Radiol 2008;38:635-644.
- Mallicote MU, Isani MA, Golden J, et al. Screening for blunt cerebrovascular injuries in pediatric trauma patients. J Pediatr Surg 2019;54:1861-1865.
- Horn E, Theodore N, Sonntag VK. SCIWORA: An antiquated acronym. Semin Spine Surgery 2005;17:46-48.
- Dorney K, Kimia A, Hannon M, et al. Outcomes of pediatric patients with persistent midline cervical spine tenderness and negative imaging results after trauma. J Trauma Acute Care Surg 2015;79:822-827.
Although rare, pediatric neck trauma may have devastating consequences. The author provides current information on recognizing and managing pediatric neck trauma.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
