What Is the Cause of This Regular WCT?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
Dr. Grauer reports no financial relationships relevant to this field of study.
The ECG in the figure below was obtained from an older woman who presented with hypotension. What is the rhythm?
The rhythm in the figure is a regular, wide complex tachycardia (WCT). The heart rate is approximately 220 beats/minute, and there is no clear sign of P waves. The principal differential diagnosis is between ventricular tachycardia (VT) and a supraventricular tachycardia (SVT) in which the reason for QRS widening is either pre-existing bundle branch block or aberrant conduction because of the rapid heart rate.
That said, there are several clues on this ECG that should allow one to rapidly arrive at the diagnosis of this tachyarrhythmia with near certainty. The odds in favor of VT when an older adult presents with a regular WCT rhythm, without clear sign of P waves, exceed 90%, even before one considers specific ECG features in the tracing. It is for this reason that the emphasis always should be on assuming the rhythm is VT (and treating the patient accordingly) until one can prove otherwise.
VT may be even likelier because the QRS complex is all negative in lead I. This means there is “extreme” axis deviation, which I define as complete negativity of the QRS complex in either lead I or lead aVF.
QRS morphology during the WCT rhythm does not resemble any known form of conduction disturbance. Whereas the QR pattern with predominant positivity in lead V1 resembles right bundle branch block (RBBB) conduction, the lack of any R wave at all in lead I and the lack of any S wave at all in lead V6 rules out RBBB conduction. The all-negative QRS complex in lead I, and the predominantly positive QRS in lead V1, rule out left BBB conduction.
There are wide and deep Q waves in virtually all chest leads. This suggests delay in the initial vector of ventricular depolarization. In contrast, the initial vector of ventricular depolarization tends to be more rapid when the rhythm is supraventricular (and traveling through organized conduction pathways). The rhythm in the figure almost is certain to be VT. The patient was treated accordingly. She responded to synchronized cardioversion by return to a sinus rhythm in which QRS morphology looked completely different to that seen during the WCT.
For more information about and further discussion of this case, please click here.
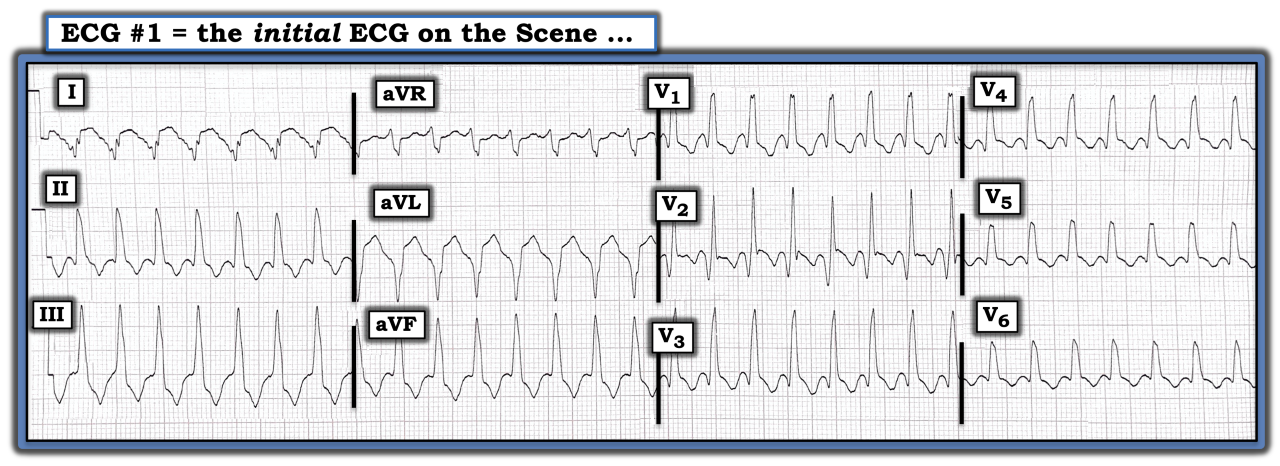
The ECG in the figure was obtained from an older woman who presented with hypotension. What is the rhythm?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
