Healthcare Personnel Hospitalizations and COVID-19 — with Possible Implications for Vaccine Prioritization
By Stan Deresinski, MD, FACP, FIDSA
Clinical Professor of Medicine, Stanford University
Dr. Deresinski reports no financial relationships relevant to this field of study.
SYNOPSIS: During the period of study, 5.9% of individuals hospitalized for COVID-19-related reasons were healthcare providers (HCP), with approximately one-third involving HCP who were not expected to have direct patient contact in the course of their work.
SOURCE: Kambhampati AK, O’Halloran AC, Whitaker M, et al. COVID-19-associated hospitalizations among health care personnel — COVID-NET, 13 States, March 1-May 31, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1576-1583.
Kambhampati and colleagues used data collected by the COVID-NET population-based survey to evaluate the proportion and characteristics of healthcare personnel (HCP) who had COVID-19-associated hospitalizations in 98 counties of 13 states during March 1 to May 31, 2020. HCP were broadly defined to include anyone in a healthcare occupation with potential exposure to patients or infectious materials. In-depth medical chart abstractions were performed on a subset, and 438 (5.9%) of the 6,760 for whom documentation was available were HCP. (See Figure.)
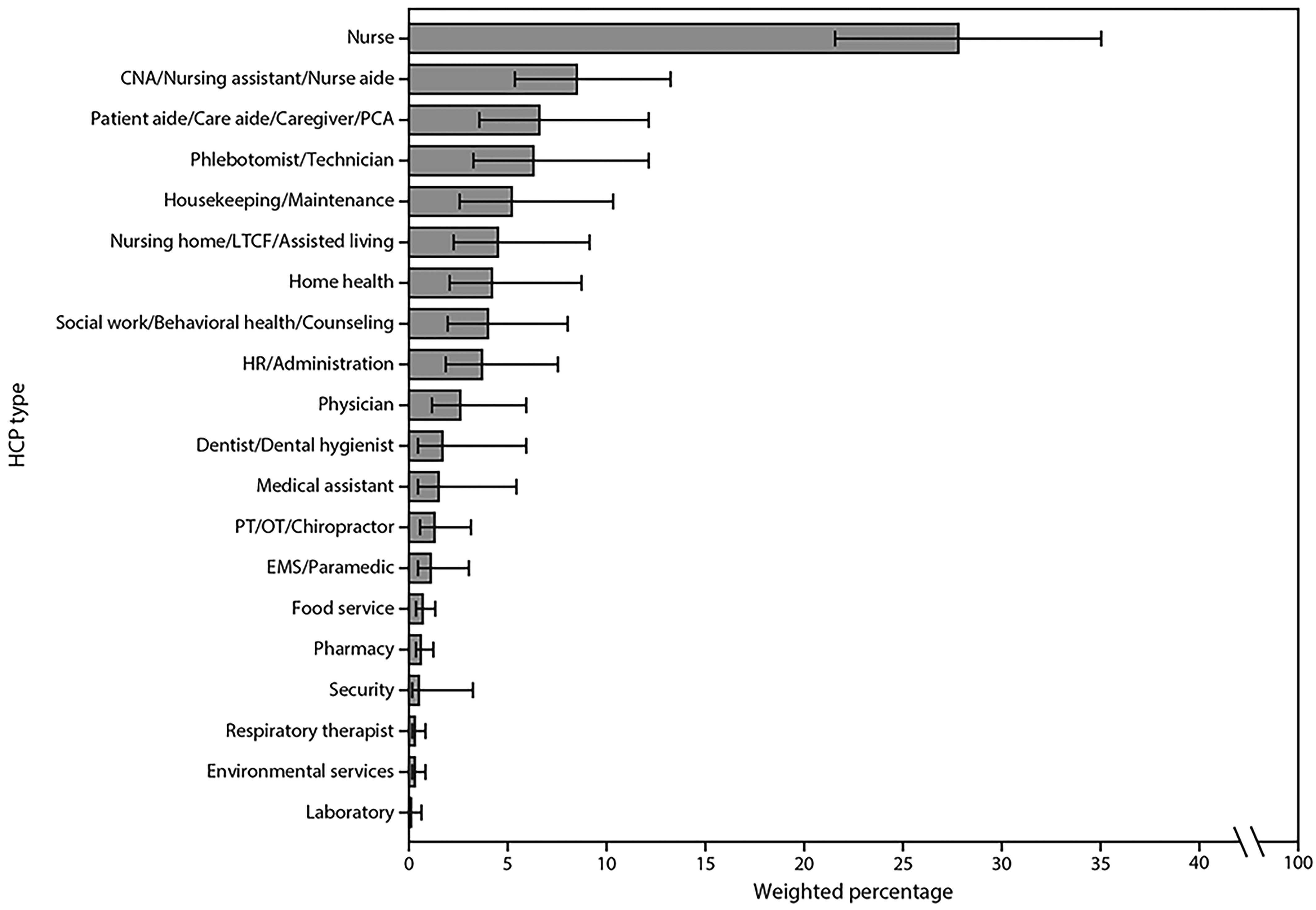
Figure 1: Weighted Percentage of Personnel Types*,† Among Reported Health Care Personnel (HCP) with COVID-19-Associated Hospitalizations (N = 438) — COVID-NET, 13 States,§ March 1-May 31, 2020 |
 |
|
Abbreviations: CNA = certified nursing assistant; COVID-19 = coronavirus disease 2019; * HCP categorized as “unspecified” or “other” have not been included in the figure but are included in the denominator. † Error bars represent 95% confidence intervals. § Sites located in the following 13 states: California, Colorado, Connecticut, Georgia, Maryland, Michigan, Minnesota, New Mexico, New York, Ohio, Oregon, Tennessee, and Utah. Source: Kambhampati AK, O’Halloran AC, Whitaker M, et al. COVID-19-associated hospitalizations among health care personnel — COVID-NET, 13 States, March 1-May 31, 2020. MMWR Morb Mortal Wkly Rep 2020;69:1576-1583. |
The median age of the HCP hospitalized with COVID-19 was 49 years and 71.9% were female. Approximately one-half were categorized as non-Hispanic Black, one-fourth as non-Hispanic white, and one-tenth as Hispanic or Latino. Just more than two-thirds (67.4%) had occupations for which direct patient contact was expected to occur, with 36.3% of the total in nursing-related categories. Almost nine in 10 had an underlying condition: obesity (72.5%), hypertension (40.6%), or diabetes mellitus (30.9%). Among the women who were 18-49 years of age, 9.6% were pregnant. Intensive care unit care was required for 27.5%, 15.9% received mechanical ventilation, and 4.2% died.
COMMENTARY
Kambhampati et al provide useful information regarding the burden of COVID-19 on HCP. However, the study examines data from relatively early in the U.S. pandemic and some of the results may be different currently because of changing and improved approaches to the disease. During the time studied, some institutions may have had limited supplies of personal protective equipment.
Although nursing occupations make up the largest single proportion of cases, no denominator data were presented. Thus, it must be recognized, e.g., that registered nurses are reported to account for one-third of U.S. healthcare practitioners. The broad range of occupational categories presented in the figure provides an overall picture across all types of HCP.
The picture presented in this study provides some useful input into initial strategies for COVID-19 vaccination which will be constrained by limited availability at the outset. Although national recommendations for vaccine prioritization have been published, these will have to be adapted to circumstances at the level of healthcare organizations, including hospitals, something which has been addressed, to an extent, by the Society for Healthcare Epidemiology of America.1
The difficulties of vaccination prioritization will be dictated by the extent of vaccine availability. Many recommendations suggest that the first target should be individuals who provide direct care to COVID-19 patients on a regular basis. However, the study reviewed here found that approximately one-third of the hospitalized HCP had occupations in which direct patient contact was not expected to occur. Other data from serosurveys suggest that direct care givers are not the HPC at greatest risk for infection. Thus, a recent survey at our institution found low levels of seropositivity overall, and the highest rates were not in HCP but in, e.g., environmental and food workers. Others have reported that the seroprevalence was not significantly different among direct-care providers when compared to others.2,3
These data, as well as those of Kambhampati et al, do not address the issue of where the infections occur. It is almost certain that the most infections occur in the community, rather than in the healthcare setting. Although different arguments can be made, I believe the data indicate that HCP such as environmental and food workers should be, at a minimum, at the same priority level as those providing direct care to COVID-19 patients.
A last note: the finding that three-fourths of HCP hospitalized for COVID-19-related reasons are obese suggests that healthcare institutions should be directly addressing this problem among their employees.
REFERENCES
- SHEA Statement for Healthcare Settings Preparing for COVID-19 Vaccination. https://shea-online.org/images/resources/101420_VaccinePlanningConsiderations.pdf
- Dimcheff DE, Schildhouse RJ, Hausman MS, et al. Seroprevalence of severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) infection among Veterans Affairs healthcare system employees suggests higher risk of infection when exposed to SARS-CoV-2 outside the work environment. Infect Control Hosp Epidemiol 2020 Sep 23;1-7. doi: 10.1017/ice.2020.1220. [Online ahead of print].
- Hunter BR, Dbeibo L, Weaver CS, et al. Seroprevalence of severe acute respiratory coronavirus virus 2 (SARS-CoV-2) antibodies among healthcare workers with differing levels of coronavirus disease 2019 (COVID-19) patient exposure. Infect Control Hosp Epidemiol 2020 Aug 3;1-2. doi: 10.1017/ice.2020.390. [Online ahead of print].
During the period of study, 5.9% of individuals hospitalized for COVID-19-related reasons were healthcare providers (HCP), with approximately one-third involving HCP who were not expected to have direct patient contact in the course of their work.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
