Acute Myocardial Infarction, or Related to COVID-19?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below was obtained from a man in his 30s. How would one interpret this tracing if told the patient’s only symptom was recent shortness of breath on exertion that he had not experienced?
Notably, the patient’s spouse has tested positive for COVID-19. Would one’s interpretation of this ECG be different if told this patient reported new-onset chest pain instead of dyspnea? The ECG in the figure shows sinus rhythm with normal intervals and axis. There is no chamber enlargement. There are small septal q waves, and reasonable R wave progression. The remarkable findings relate to ST-T wave abnormalities in several leads.
There is subtle-but-real ST segment coving with slight elevation in high lateral leads I and aVL. Reciprocal ST-T wave depression is seen in leads III and aVF, with slight ST segment flattening in the remaining inferior lead (lead II). In a patient with new chest pain, these findings should suggest recent or acute infarction.
An additional abnormal finding in this ECG relates to the relative amplitude of the upright T waves in the six chest leads. In the absence of left ventricular hypertrophy, it is uncommon for an upright T wave in lead V1 to be taller than the upright T wave in lead V6. In a patient with new chest pain, the clearly more voluminous (i.e., taller in height and wider at its base) T wave in lead V1 compared to the T wave in lead V6 suggests there may be an ongoing ischemic process.
It turns out the history in this case was exactly as described in the opening paragraph. That is, this patient reported dyspnea on exertion of recent onset — and close exposure to a COVID-19-positive individual. This patient experienced no chest pain.
Unfortunately, a full evaluation was not performed at the time the patient was seen initially, so diagnostic considerations are presumptive. That said, the combination of a clearly abnormal ECG in this otherwise-healthy younger adult with COVID-19 exposure and recent dyspnea on exertion should suggest COVID-19-related myocarditis as the most likely explanation. Subsequent follow-up supported this presumption.
For more information about and further discussion of this case, please click here.
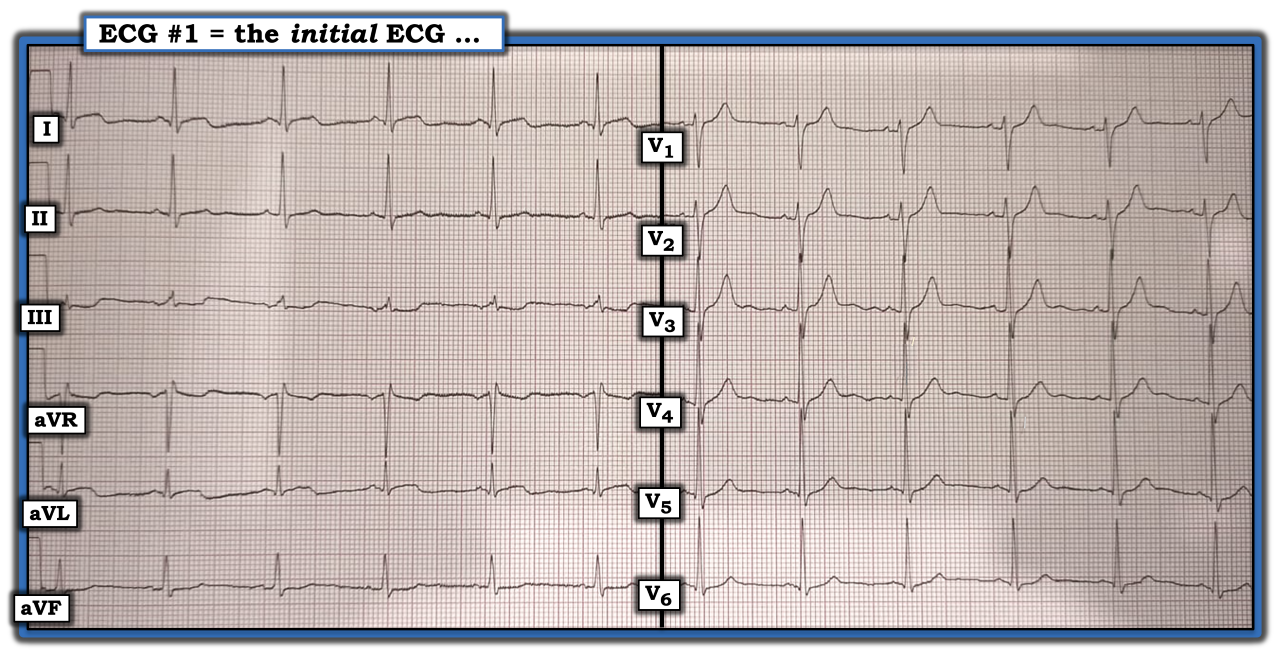
The ECG in the figure was obtained from a man in his 30s. How would one interpret this tracing if told the patient’s only symptom was recent shortness of breath on exertion that he had not experienced?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
