Spinal Cord Compression: Evaluation and Management
September 1, 2021
Reprints
AUTHORS
Guhan Rammohan, MD, FACEP, Assistant Professor of Emergency Medicine, St. Luke’s University Health Network, Bethlehem, PA
Matthew Meyers, DO, Emergency Medicine Resident, St. Luke’s University Health Network, Bethlehem, PA
PEER REVIEWER
Catherine Marco, MD, Professor of Emergency Medicine, Wright State University, Dayton, OH
EXECUTIVE SUMMARY
- Spinal cord compression is an emergency. Delay in treatment can lead to permanent deficits. However, the diagnosis can be difficult. There are many patients with low back pain who seek care in an emergency department, yet few of them will have this complication.
- Spinal cord compression can occur from a variety of causes, ranging from degenerative disc disease, metastatic disease, hematoma, infection, and traumatic injury. Most will cause new, usually acute onset of pain, often with new motor or sensory changes, and/or loss of bowel or bladder control.
- Computed tomography is a reasonable screening test for spinal cord compression, but, since it does not image the cord itself, it can miss compression from non-bony sources. Magnetic resonance imaging is the preferred test, but it is not readily accessible in many emergency departments.
- Patients diagnosed or suspected to have spinal cord compression should have a consult with a spinal surgeon if possible. Treatment choices will vary depending on the cause of the compression. The literature is not definitive for many causes of compression, and local treatment preferences may vary.
- Corticosteroids have been shown to be of little to no value in traumatic spinal cord injures, but they continue to be used by some specialists.
Case
A 59-year-old male with a past medical history significant for chronic low back pain presents to the emergency department for low back pain and lower extremity weakness. Over the past five days, the patient reports worsening pain in the lumbar spine region, which radiates into both lower extremities. The symptoms are intermittent, and the pain is rated as a 10/10 at worst. The patient also notes worsening weakness in hip flexion, which has affected his ability to walk. Additionally, the patient reports episodes of bowel incontinence. This has been present intermittently for several months. One day prior, the patient experienced a transient episode of numbness in his genital region, which has since resolved.
The patient has a long-standing history of low back pain and was previously diagnosed with a herniated intervertebral disc on magnetic resonance imaging (MRI). The patient has completed a course of outpatient physical therapy and continues with home stretching exercises. The patient denies recent trauma to the area, fevers or night sweats, unexplained weight loss, and urinary retention. There is no history of intravenous drug use, chronic steroid use, or cancer (prostate, renal, lung). The patient has taken acetaminophen and applied a lidocaine patch at home to attempt to alleviate the symptoms.
On exam, the patient is in no acute distress and appears comfortable in the room. Vital signs demonstrate a temperature of 97.9°F, heart rate 86 beats per minute, respiratory rate 18 breaths per minute, and blood pressure 118/76 mmHg. The patient demonstrates an antalgic and wide-based gait. He has 4/5, symmetric strength in bilateral lower extremities. The patient has symmetric, though diminished, patellar and Achilles reflexes in bilateral lower extremities. Rectal tone is noted to be intact. Based on the history and physical exam, basic laboratory tests and imaging of the lumbar spine and spinal cord are ordered. Initially, providers considered obtaining a computed tomography (CT) scan of the lumbar spine, although because of a high index of suspicion for acute spinal cord compression, the radiologist approved an MRI of the lumbar spine. The MRI demonstrates a large extrusion type disc herniation at L4-5 superimposed on facet arthropathy and congenital stenosis, resulting in severe spinal canal stenosis and severe compression of the thecal sac. The patient is admitted, given 10 mg intravenous dexamethasone, and neurosurgery is consulted.
Introduction
Diagnosis and management of acute spinal cord compression can be a challenge for the emergency physician. A 2012 systematic review determined the global point prevalence of low back pain to be 11.9%.1 While low back pain is a common complaint, only 0.27% of patients presenting for low back pain were diagnosed with cauda equina syndrome in one study.2
The etiology of spinal cord compression is multiple. Likewise, the clinical presentation can range from intermittent, subtle symptoms to acute loss of motor sensory function. One retrospective chart review of 63 patients diagnosed with atraumatic spinal cord compression found that pain was present in 70% of patients, while subjective weakness was only present in 56% of patients.3 Diagnosis often requires advanced imaging, such as magnetic resonance imaging (MRI), which is not always readily available to emergency clinicians.
Prompt diagnosis and definitive intervention are crucial to preventing long-term neurologic deficit. This article will focus on conditions causing sudden spinal cord compression, as in the setting of traumatic injury. It also will focus on those pathologies that progress over days to weeks, such as cauda equina syndrome, spinal epidural abscess, and spinal epidural hematoma. Causes of chronic spinal cord compression, such as spinal stenosis or syringomyelia, are outside the scope of this article and will not be discussed here.
Anatomy
The spinal cord is composed of 31 segments of gray and white matter material spanning the cervical, thoracic, and beginning lumbar segments of the spine. (See Figure 1. ) The spinal cord contains afferent and efferent tracts that transfer neuronal signals between the peripheral and central nervous system. Afferent tracts include the corticospinal tract, which controls axial body and proximal limb movements; the rubrospinal tract, which controls flexor muscles of the upper extremity; and the vestibulospinal fasciculus, which controls extensor muscles as well as tone and posture.4 Ascending tracts include the dorsal column, which controls proprioception and vibration sense; the fasciculus gracilis, which carries sensory signals from the lower half of the body; the fasciculus cuneatus, which carries sensory information for the upper thorax and back of the head; and the spinothalamic tract, which transmits pain and temperature signals.4
Figure 1. Spinal Cord Anatomy |
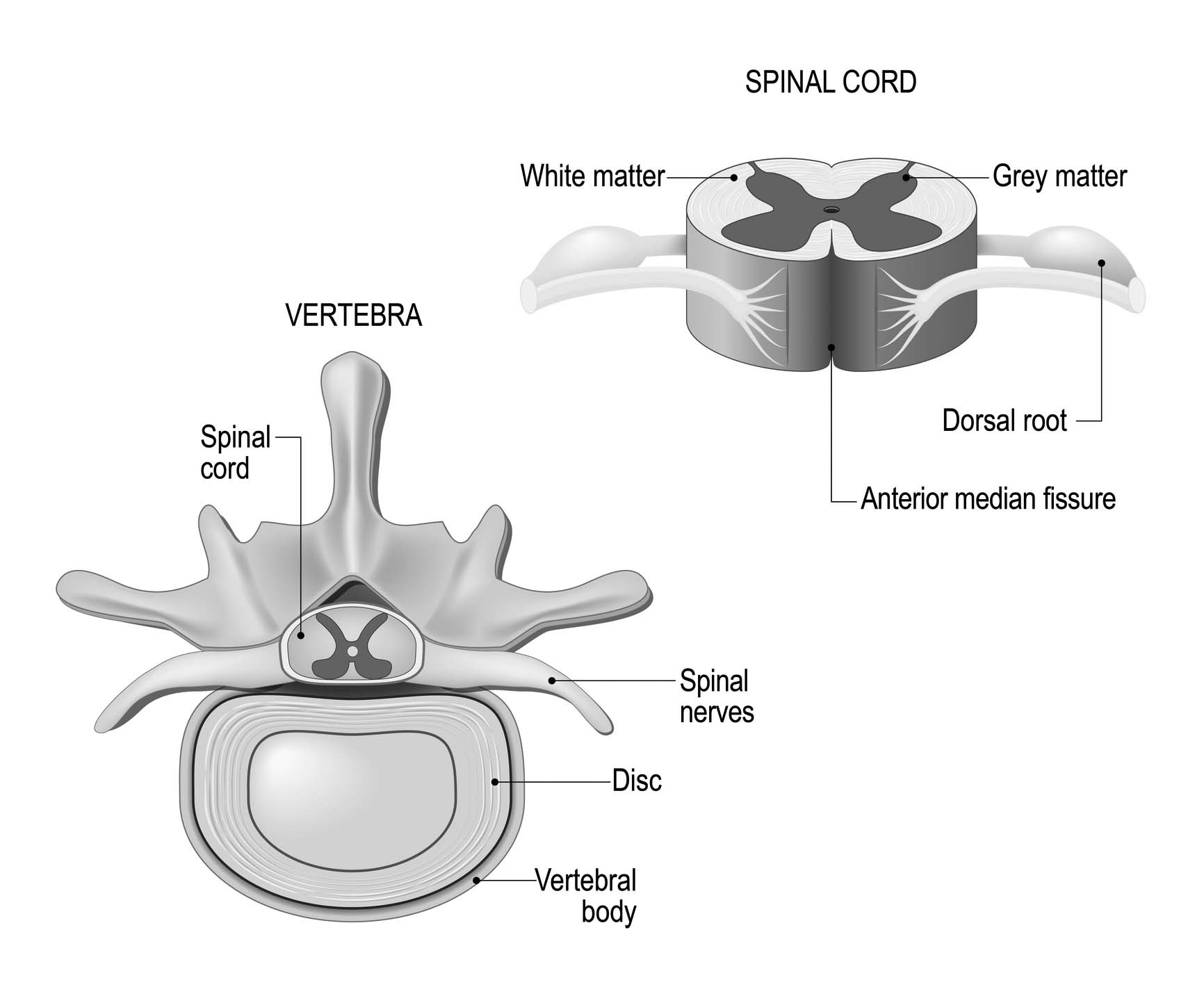
|
|
Source: Getty Images |
The spinal epidural space is a potential space that lies between the vertebral bones and the dura mater. This area contains fatty tissue and a venous plexus. This venous plexus communicates to the central venous circulation via the valveless Batson plexus. The epidural space is larger in the thoracolumbar region and, thus, is more prone to pathology. The spinal cord tapers at the end into a structure known as the conus medullaris. The conus medullaris is usually located at the level of the L1 vertebral body.5
Clinical Approach to Acute Spinal Cord Compression
A thorough history and physical exam are very helpful when evaluating all patients with acute low back pain. Important aspects of the history should focus on any new or worsening deficits in motor function, sensory function, or involuntary loss of sphincter reflexes. The history should focus on red flag historical elements, such as a history of low back pain, current or prior cancer diagnosis, intravenous drug use, prior spinal procedures, recent trauma, or other systemic symptoms.6,7
On physical exam, fever in the context of acute low back pain should raise concern for an infectious etiology of symptoms. The physical examination should focus on a thorough evaluation of the spinal reflexes, including L4, L5, and S1. Anal tone also should be evaluated in certain clinical settings. Thorough evaluation of muscle strength in the lower extremities is helpful, with an emphasis placed on comparing strength across both extremities. Upper motor neuron compression usually generates bilateral deficits, while lower motor neuron injury generally manifests as unilateral deficits.8 Sensation along dermatomal distributions is important and is best assessed using pinprick testing.7 If there is concern for acute spinal cord compression causing impairment of viscerosomatic reflexes, a post-void residual bladder volume > 100 mL raises the concern for acute spinal cord compression.9
Diagnostic evaluation for acute spinal cord compression is appropriate if the patient has red flag symptoms or unexplained deficits on physical exam. Laboratory testing may support or refute certain etiologies of low back pain. Coagulopathy can be associated with spinal epidural hematoma. A leukocytosis and elevated erythrocyte sedimentation rate/C-reactive protein (CRP) can be seen in cases of spinal epidural abscess.
Although laboratory tests may suggest a source of spinal cord compression, direct visualization in the form of imaging is necessary to confirm the diagnosis and assist in determining the best course of therapy. CT or plain radiographs may reveal traumatic injuries or other sources of spinal cord compression, but MRI is most commonly the test of choice for evaluation of acute spinal cord compression.7 The appropriate consultant to treat acute spinal cord compression depends on the etiology. Most cases benefit from discussion with a spine surgeon, if available. In select cases, interventional radiology and radiation oncology also may need to be involved to best manage spinal cord compression.
In patients without neurologic deficit and low clinical suspicion for acute spinal cord compression, a normal CT scan may provide reassurance to providers. Patients without neurologic deficit and with normal CT imaging may be able to be evaluated further with outpatient consultation. However, when clinical suspicion is high, urgent MRI is needed. If MRI capabilities are not readily available, then the patient should be transferred to a hospital with MRI capabilities and neurosurgery consultation regardless of CT imaging results.
Degenerative Disc Disease
Spinal cord compression can result from acute exacerbation of chronic spine disease. Degeneration of intervertebral discs causes changes in the ligaments, joints, and muscles surrounding the spine, which leads to progressive narrowing of the spinal canal.10 Advanced age and increased body mass index are known risk factors for developing degenerative disc disease.11 Herniation of intervertebral discs or stenosis of the spinal canal can extend to cause compression of the spinal cord. Degenerative disc disease is common, and, fortunately, most patients do not suffer cord compression. However, distinguishing between a patient with severe disc disease and acute pain and cord compression can be challenging.
Presentation
Providers should be concerned about any new or worsening symptoms that differ from the patient’s chronic low back pain. Degenerative disc disease and foraminal stenosis can cause nerve root compression resulting in intermittent radiculopathy. However, any patients with signs or symptoms of new motor, sensory, or autonomic dysfunction should prompt further investigation.
Diagnostic Evaluation
Many patients with chronic degenerative disc disease improve with conservative measures. Therefore, imaging is not routinely required in the emergency department evaluation of degenerative disc disease.
Imaging should be considered in any patient with a history of degenerative disc disease and signs or symptoms of new neurologic deficit. MRI is valuable for evaluating the intervertebral discs, nerve and spinal cord impingement, and intraspinal structures, while CT is more valuable for visualizing vertebral anatomy and is useful for preoperative planning.12
Management
In cases of acute spinal cord compression due to intervertebral disc herniation, surgical decompression is warranted. This commonly is performed using laminectomy and/or microdiscectomy to relieve spinal cord impingement.
The use of corticosteroids is a point of debate in cases of acute spinal cord compression. Their use varies among specialists, but they should be considered as a temporizing measure while plans for definitive therapy are arranged.
Disposition
Most patients with degenerative disc disease do not require admission to the hospital. Patients with isolated radicular symptoms can be managed with conservative measures and outpatient follow-up. In patients who have new motor or sensory deficits prompting imaging, decisions regarding disposition should be made in concert with neurosurgical consultation.
Metastatic Spinal Cord Compression
In patients with a history of prior or current cancer diagnosis and new-onset back pain, providers should consider the possibility for metastatic disease. The incidence of metastatic spinal cord compression in the last five years of life has been reported in 2.5% of cases, with a median survival of 2.9 months from the date of initial episode of spinal cord compression.13 Lung, prostate, and breast cancer were the primary tumors in 61.2% of cases of metastatic spinal cord compression.13 Cancers can spread to the structures surrounding the spinal cord or within the spinal cord itself. Compression of the spinal cord in the setting of malignancy can occur via external compression by metastatic lesions or via intramedullary growth of cancerous tissue.
Presentation
Patients with any history of cancer and acute low back pain should raise suspicion for metastatic spinal cord compression. The pain often is worse at night and can be localized to one area of the spine or cause referred pain to other areas of the spine. Often, pain is the first symptom and can precede frank neurologic deficit. Compression of the spinal cord or cauda equina results in motor weakness, numbness, paresthesia, ataxia, or loss of autonomic function in the form of bowel or bladder incontinence or retention.
Diagnostic Evaluation
Although CT can diagnose metastatic lesions to vertebrae, MRI is the gold standard for diagnosing spinal cord compression. Previous studies have demonstrated a 95% sensitivity and 88% specificity using CT compared to a 92% to 93% sensitivity and 90% to 97% specificity for MRI in diagnosing metastatic spinal cord compression.14,15 MRI should be performed of the entire spine, since 20% to 35% have metastasis and compression of multiple levels of the spinal cord.8 If MRI is contraindicated because of allergy or incompatible implanted devices, CT myelography or positron emission tomography can be used to make the diagnosis.16
Management
Classically, corticosteroids have been recommended to decrease perispinal inflammation to minimize spinal cord compression. Steroids are thought to reduce edema and also can decrease tumor size.17 Despite a paucity of randomized controlled trials supporting their use, steroids, commonly dexamethasone, are recommended by some as a temporizing measure while awaiting definitive management in the form of radiation or surgical management.17
One study comparing epidural spinal cord compression showed a decreased presence of paralysis in patients managed with surgical stabilization with and without decompressive laminectomy compared to patients managed with radiation therapy alone, although this difference did not achieve statistical significance.18 Radiation therapy in combination with surgery is a point of debate. Some studies have demonstrated improved ambulatory status in patients managed with surgery followed by radiation therapy compared to radiation therapy alone.19 Subsequent studies have failed to demonstrate a difference in ambulatory status comparing surgery followed by radiation therapy and radiation therapy alone.20
Radiation therapy is used as a palliative measure in patients with a poor prognosis, defined as having less than six months of life expectancy, poor baseline functional status, and preexisting paraplegia.21
The Spine Instability Neoplastic Score (SINS) is used to determine the need for surgical intervention.16,22 The components of the SINS scoring system are location, presence or absence of pain, type of bone lesion, degree of spinal misalignment, percentage of vertebral body collapse, and degree of posterolateral spine involvement.22 A score of 0-6 is considered stable, 7-12 is potentially unstable, and 13-18 is considered unstable. Patients with a score greater than 7 should have neurosurgical consultation.
Disposition
Patients with acute spinal cord compression due to metastatic disease should be admitted to the hospital. Decisions regarding care are made in coordination with subspecialists. In cases for which subspecialists recommend conservative management, many patients with metastatic cancer benefit from pain control and physical and occupational therapy, as well as coordination of postdischarge resources that can be arranged while the patient is admitted to the hospital.
Spinal Epidural Abscess
As in many cases of acute spinal cord compression, the diagnosis of spinal epidural abscess can be a difficult diagnosis to make. Risk factors for spinal epidural abscess include increased age, immunocompromised state, intravenous drug use, and history of spinal procedures.23 Infection can occur through local extension or through systemic seeding through bidirectional flow through the Batson plexus. Local spread can occur through a paraspinal abscess, spinal osteomyelitis, or discitis. Infection arising from local bacterial spread occurs in one-third of cases, whereas half of cases are attributed to hematogenous spread.24 Injury occurs through direct mechanical compression of the spinal cord, compression of the arterial blood supply, thrombus, or from septic thrombophlebitis.24,25
Presentation
When entertaining the diagnosis of spinal epidural abscess, it is important to consider risk factors for infection. Diabetes mellitus, history of spinal trauma, intravenous drug use, and alcoholism all predispose patients to developing spinal epidural abscess.26 The classic triad of fever, back pain, and neurologic deficit is a late finding and is unreliable.
The long-term prognosis largely depends on the severity of neurologic deficit at the time of diagnosis. The severity of neurologic deficit also is predictive of mortality. Therefore, early diagnosis is important.
Diagnostic Evaluation
Routine laboratory analysis should include a complete blood count with differential, blood cultures, CRP, and erythrocyte sedimentation rate testing, while MRI with gadolinium contrast is considered the gold standard for confirming the diagnosis.25 CT with intravenous (IV) contrast has been studied as an alternative for diagnosis, although it does not meet the > 90% sensitivity and specificity of MRI for detecting spinal infections.27 Contrast allows for discerning phlegmonous change resulting from abscess formation.
A grading system developed by Shah et al is used to determine the degree of spinal cord compression in cases of spinal epidural abscess. The five-point scale represents the progressing degrees of spinal cord impingement on MRI. The scale starts at grade 1, which is epidural impingement without deformity of the thecal sac, and ranges to grade 5, which is spinal cord compression without cerebrospinal fluid (CSF) visible around the spinal cord.28 However, it is notable that a higher grade compression did not correlate with failure of nonoperative management, residual neurologic deficit, or mortality.
CT myelography also has been used to diagnose epidural abscess, although it is more invasive and cumbersome when compared to MRI with IV contrast. Because of the risk of subdural infection or meningitis, lumbar puncture is not recommended. Cerebrospinal fluid analysis in cases of confirmed epidural abscess are consistent with paraspinal inflammation, although they usually are not specific for diagnosing epidural abscess. Additionally, cerebrospinal fluid culture is positive in only 25% of cases.24
Management
As with most abscesses, source control in the form of surgical drainage is the standard of care. Drainage can be performed through open surgical procedures or through interventional radiology drainage. Spine surgeons consider the location of the abscess and the degree to which the vertebral body is involved when determining an operative approach.23 Surgery may be contraindicated in patients with multiple medical comorbidities, diffuse spinal infection, no neurologic deficits, or neurologic deficits lasting greater than 48 hours.29
To our knowledge, no randomized controlled trial comparing surgical and nonsurgical (i.e., antibiotics-only) management of spinal epidural abscess has been completed. The timing of antibiotic initiation is a point of debate. In patients without neurologic deficit or sepsis, many experts recommend withholding antibiotics until blood cultures or, preferably, an aspirate is obtained.30,31 Other providers will initiate empiric antibiotic therapy as soon as the diagnosis of spinal epidural abscess is made. In this scenario, antibiotics can be in process or completed prior to MRI-confirmed diagnosis and surgical drainage.32
Two-thirds of cases are attributed to infections with Staphylococcus aureus.24,25 Therefore, initial antibiotics should cover methicillin-resistant S. aureus (MRSA), usually in the form of vancomycin. Third- or fourth-generation cephalosporins also should be considered to cover gram-negative bacilli. See Table 1 for specific antibiotic dosing. If a causative organism is isolated from blood or abscess cultures, antibiotic coverage should be narrowed accordingly. The duration of antibiotic therapy often is determined in conjunction with infectious disease guidance. Published guidelines recommend at least a six-week course of antibiotics in the setting of spinal epidural abscess.30,31
Table 1. Spinal Epidural Abscess Antibiotic Options | ||
|
Drug |
Initial Dose |
Route |
|
Vancomycin |
15-20 mg/kg |
IV |
|
Ceftriaxone |
2 grams |
IV |
|
Cefepime |
2 grams |
IV |
|
Meropenem |
2 grams |
IV |
|
Moxifloxacin |
400 mg |
IV |
|
IV: intravenous | ||
Disposition
All cases of spinal epidural abscess should be admitted for definitive care. As discussed earlier, patients require IV antibiotics and most cases also require surgical drainage of the spinal abscess. Patients receive physical and occupational therapy during hospitalization, and most cases require a peripherally inserted central catheter (PICC) to complete several weeks of IV antibiotics after discharge.
Traumatic Spinal Cord Compression
Both blunt and penetrating trauma can result in acute spinal cord compression. In the United States, the most common etiology of spinal cord injury is motor vehicle collisions.33 Injury can result from damage to the spinal cord itself or through damage to the surrounding spinal structures. Damage to the vertebrae can cause displacement of bony fragments, which migrate to cause cord compression. Anterolisthesis or retrolisthesis are the results of spinal instability caused by the loss of integrity to the soft tissue structures that provide support to the spinal column.
Presentation
Providers should have a high index of suspicion for spinal cord compression in patients who present with motor or sensory deficits following traumatic injury. A thorough neurologic exam should be performed, including examination of sensation along dermatomes, motor function, lower motor neuron reflexes, and anal sphincter tone.
Diagnostic Evaluation
Diagnostic imaging confirms the location and nature of injury while also allowing for preoperative planning. Over the past several decades, CT has become the preferred imaging modality for the evaluation of trauma patients.34,35 Although the sensitivity of identifying vertebral fractures on CT has been reported as high as 97%, only MRI allows for direct imaging of the spinal cord itself.36,37 CT of the spine has demonstrated better sensitivity and specificity compared to traditional radiographs for evaluation of blunt trauma injury in trauma patients with symptoms concerning for spinal injury.38 In patients with subjective or objective findings concerning for injury despite a negative CT scan, continued cervical spine immobilization and MRI should be considered.
In severe trauma patients requiring intubation, a full neurologic exam cannot be assessed. In this setting, the best practice for clearing the cervical spine of acute injury is debated. Current Eastern Association for the Surgery of Trauma (EAST) guidelines recommend cervical collar removal after a negative high-quality CT of the cervical spine.39 However, this recommendation is based on low quality of evidence. Other literature supports obtaining an MRI of the cervical spine to clear the cervical spine of traumatic injury. One study of trauma patients demonstrated abnormal findings on MRI after a negative CT of the spine in 12% of patients, of which 47% had spinal ligamentous injuries.40 This is a point of debate among clinicians, and practice may differ between providers.
The American Spinal Injury Association Impairment Scale (AIS) created by the International Standards Committee of the American Spinal Injury Association is a commonly used scoring system to quantify traumatic spinal cord injury.41 These criteria are described further in Table 2. The grading system ranges from Grade A, denoting complete loss of motor and sensory function, to Grade E, representing no motor or sensory deficit on exam.
Table 2. American Spinal Injury Association Impairment Scale (AIS) | |
|
A: Complete |
No sensory or motor function is preserved in the sacral segments S4-5. |
|
B: Sensory Incomplete |
Sensory but not motor function is preserved below the neurological level and includes the sacral segments S4-5 (light touch or pin prick at S4-5 or deep anal pressure) AND no motor function is preserved more than three levels below the motor level on either side of the body. |
|
C: Motor Incomplete |
Motor function is preserved at the most caudal sacral segments for voluntary anal contraction (VAC) OR the patient meets the criteria for sensory incomplete status (sensory function preserved at the most caudal sacral segments S4-5 by LT, PP or DAP), and has some sparing of motor function more than three levels below the ipsilateral motor level on either side of the body. (This includes key or non-key muscle functions to determine motor incomplete status.) For AIS C – less than half of key muscle functions below the single NLI have a muscle grade ≥ 3. |
|
D: Motor Incomplete |
Motor incomplete status as defined above, with at least half (half or more) of key muscle functions below the single NLI having a muscle grade ≥ 3. |
|
E: Normal |
If sensation and motor function as tested with the ISNCSCI are graded as normal in all segments, and the patient had prior deficits, then the AIS grade is E. Someone without an initial SCI does not receive an AIS grade. |
|
Using ND |
To document the sensory, motor and NLI levels, the ASIA Impairment Scale grade, and/or the zone of partial preservation (ZPP) when they are unable to be determined based on the examination results. |
|
LT: light touch; PP: pin prick; DAP: deep anal pressure; NLI: neurological level of injury Reprinted with permission: American Spinal Injury Association: International Standards for Neurological Classification of Spinal Cord Injury, revised 2019; Richmond, VA. | |
Management
The management of traumatic spinal cord injury primarily is surgical. The goal of surgical correction is to remove any bony fragments causing compression of the spinal cord and restore proper anatomic alignment of the spinal column.35 The use of corticosteroids as a neuroprotective agent in the setting of acute spinal cord injury has been a point of much debate. At present, a level 1 recommendation exists against the routine use of methylprednisolone in the setting of acute spinal cord injury.34
Disposition
Patients with acute spinal trauma and subsequent spinal cord compression require admission to the hospital for evaluation by neurosurgery. Many patients require surgical management. Subsequent management includes frequent motor and sensory checks. Patients require physical and occupational therapy during hospitalization, and many patients require coordination of post-acute rehabilitation services on discharge.
Spinal Epidural Hematoma
Epidural hematoma is the result of blood accumulation within the epidural space. Spinal epidural hematoma occurs in the presence of coagulopathy, trauma, spinal surgery, or vascular lesions.42 Multiple cases of spinal hematoma occurring spontaneously or after minimal spinal trauma also have been reported.43-45 Spontaneous epidural hematoma represents less than 1% of all spinal epidural space-occupying lesions.46 Spinal epidural hematoma is thought to be the result of bleeding from the spinal epidural veins, spinal epidural arteries, or vascular malformations.
Presentation
Patients classically describe acute onset of back pain and a wide range of neurologic deficits, depending on the location of the hematoma.47 As the epidural hematoma expands to compress the spinal cord or nerve roots, patients can experience radiation of pain to the extremities. Progression occurs at variable rates, with the time between the onset of symptoms and progression to neurologic deficit occurring over hours to days.42
Diagnostic Evaluation
Evaluation of patients with presumed spinal epidural hematoma should include a thorough history and physical exam. Laboratory work should include coagulation studies, such as international normalized ratio (INR), prothrombin time (PT), activated thromboplastin time (aPTT), and platelet count, both to identify coagulopathy predisposing to the development of an epidural hematoma and to guide appropriate reversal therapy if indicated. Diagnosis also requires imaging of the affected spinal region. Although CT can diagnose spinal epidural hematoma, more false-negative results are attributed to CT, and CT poorly demonstrates the size of hematoma.46 The preferred form of imaging to evaluate for spinal hematoma is MRI, since it is noninvasive and discerns between hematoma and other causes of spinal cord compression.46,48 Magnetic resonance arteriography can be performed if there is concern for a spinal arteriovenous malformation causing spinal epidural hematoma.
Management
For patients with symptomatic epidural hematoma, the management is surgical decompression.35,42,47 This should be performed as quickly as possible to prevent permanent neurologic deficit. Previous studies have demonstrated improved neurologic outcomes in patients who underwent decompressive surgery within six hours from the onset of neurologic deficit.49 If the spinal epidural hematoma is determined to be secondary to coagulopathy, providers should strongly consider targeted correction so long as there are no contraindications precluding reversal.
Disposition
Patients with spinal epidural hematoma and subsequent spinal cord compression require admission to the hospital for definitive care. Following surgical decompression, patients are monitored with frequent neurologic exams and receive ongoing physical and occupational therapy.
Conus Medullaris Syndrome
Conus medullaris syndrome can be the result of traumatic injury, epidural abscess or hematoma, or metastatic compression. As discussed earlier, the conus medullaris is the terminal end of the spinal cord and is usually located at the level of L1. Conus medullaris syndrome is considered an incomplete spinal cord injury. The clinical presentation can be similar to cauda equina syndrome, although compression usually occurs in the upper lumbar nerve roots secondary to injury at the level of the thoracolumbar spine.41 Compression of the sacral nerve roots S2-S4 affect autonomic genitourinary and bowel function. Sphincter dysfunction causes flaccid paralysis of the bladder and rectum. Compression of afferent nerve fibers along the S3-S5 nerve root causes the classic absence of sensation in the perianal region referred to as “saddle anesthesia.” Patients with conus medullaris will present with back pain combined with upper and lower motor neuron deficits.
Cauda Equina Syndrome
The collection of nerve roots emanating from the spinal cord below the L1-L2 level is referred to as the cauda equina. While these nerve roots are separate from the spinal cord, compression of the cauda equina generates a clinical presentation similar to spinal cord compression. Compression of these nerve roots causes loss of motor and sensory function to the lower extremities, bowel and bladder incontinence, impotence, and loss of perianal sensation.50 Providers should have a high index of suspicion for cauda equina syndrome in any patient with back pain and any of these red flag symptoms.
Any of the disease processes discussed previously can cause clinically significant compression of the cauda equina. A thorough history and physical exam are crucial for rapid diagnosis and management. Cauda equina syndrome is attributed to intervertebral disc herniation at L4/L5 or L5/S1 in 45% of cases, although only 1% to 2% of disc herniations result in cauda equina syndrome.51 As mentioned previously, MRI is the gold standard to best visualize the intervertebral discs and resultant compression on the spinal cord.52 When clinical suspicion is high, analysis of a post-void residual bladder volume is a rapid screening test for urinary retention. Prior studies have demonstrated a 4.0 odds ratio for cauda equina syndrome in patients with a post-void volume > 500 mL in the right clinical scenario.53 Management of cauda equina syndrome includes surgical intervention aimed at relieving spinal cord compression, although the timing of surgery has been a point of debate depending on the source of compression and degree of neurologic compromise.50,54
Summary
Acute compression of the spinal cord can occur through several different mechanisms. The presentation can range from insidious progression of back pain and neurologic deficit to frank, instantaneous injury. Understanding the clinical context in which acute spinal cord compression can arise is crucial for reducing morbidity. Regardless of the cause of spinal cord compression, rapid diagnosis and treatment are crucial. Interventions aimed at relieving spinal cord compression should be undertaken as soon as possible. Delays in treatment adversely affect long-term prognosis.
Case Conclusion
The patient is admitted to the hospital and taken to the operating room urgently to undergo L4-5 microdiscectomy and laminectomy. Following surgery, the patient demonstrates residual weakness in the lower extremities. Postoperative day one, the patient has resolution of urinary retention and can void spontaneously. The patient remains in the hospital for several days and is discharged to a rehabilitation facility. At his one-month follow-up visit in the neurosurgery clinic, the patient reports a return to baseline strength and normal bowel and bladder function.
REFERENCES
- Hoy D, Bain C, Williams G, et al. A systematic review of the global prevalence of low back pain. Arthritis Rheum 2012;64:2028-2037.
- Hoeritzauer I, Wood M, Copley PC, et al. What is the incidence of cauda equina syndrome? A systematic review. J Neurosurg Spine 2020;32:832-841.
- Dugas AF, Lucas JM, Edlow JA. Diagnosis of spinal cord compression in nontrauma patients in the emergency department. Acad Emerg Med 2011;18:719-725.
- Bican O, Minagar A, Pruitt AA. The spinal cord: A review of functional neuroanatomy. Neurol Clin 2013;31:1-18.
- Chiu P-Y, Liao J-C. Surgical outcomes in thoracolumbar fractures with pure conus medullaris syndrome. Biomed J 2019;42:277-284.
- Della-Giustina D. Evaluation and treatment of acute back pain in the emergency department. Emerg Med Clin North Am 2015;33:311-326.
- Corwell BN. The emergency department evaluation, management, and treatment of back pain. Emerg Med Clin North Am 2010;28:811-839.
- Lawton AJ, Lee KA, Cheville AL, et al. Assessment and management of patients with metastatic spinal cord compression: A multidisciplinary review. J Clin Oncol 2019;37:61-71.
- Podnar S, Tršinar B, Vodušek DB. Bladder dysfunction in patients with cauda equina lesions. Neurourol Urodyn 2006;25:23-31.
- Kos N, Gradisnik L, Velnar T. A brief review of the degenerative intervertebral disc disease. Med Arch 2019;73:421-424.
- Gübitz R, Lange T, Gosheger G, et al. Influence of age, BMI, gender and lumbar level on T1ρ magnetic resonance imaging of lumbar discs in healthy asymptomatic adults. Rofo 2018;190:144-151.
- Ailon T, Smith JS, Shaffrey CI, et al. Degenerative spinal deformity. Neurosurgery 2015;77(Suppl 4):S75-S91.
- Loblaw DA, Laperriere NJ, Mackillop WJ. A population-based study of malignant spinal cord compression in Ontario. Clin Oncol 2003;15:211-217.
- Carmody RF, Yang PJ, Seeley GW, et al. Spinal cord compression due to metastatic disease: Diagnosis with MR imaging versus myelography. Radiology 1989;173:225-229.
- Li KC, Poon PY. Sensitivity and specificity of MRI in detecting malignant spinal cord compression and in distinguishing malignant from benign compression fractures of vertebrae. Magn Reson Imaging 1988;6:547-556.
- Patnaik S, Turner J, Inaparthy P, Kieffer WK. Metastatic spinal cord compression. Br J Hosp Med 2020;81:1-10.
- Kumar A, Weber MH, Gokaslan Z, et al. Metastatic spinal cord compression and steroid treatment: A systematic review. Clin Spine Surg 2017;30:156-163.
- Maseda M, Uei H, Nakahashi M, et al. Neurological outcome of treatment for patients with impending paralysis due to epidural spinal cord compression by metastatic spinal tumor. J Orthop Surg Res 2019;14:291.
- Patchell RA, Tibbs PA, Regine WF, et al. Direct decompressive surgical resection in the treatment of spinal cord compression caused by metastatic cancer: A randomised trial. Lancet 2005;366:643-648.
- Rades D, Huttenlocher S, Dunst J, et al. Matched pair analysis comparing surgery followed by radiotherapy and radiotherapy alone for metastatic spinal cord compression. J Clin Oncol 2010;28:3597-3604.
- Al-Qurainy R, Collis E. Metastatic spinal cord compression: Diagnosis and management. BMJ 2016;353:i2539.
- Fourney DR, Frangou EM, Ryken TC, et al. Spinal instability neoplastic score: An analysis of reliability and validity from the Spine Oncology Study Group. J Clin Oncol 2011;29:3072-3077.
- Schwab JH, Shah AA. Spinal epidural abscess: Diagnosis, management, and outcomes. J Am Acad Orthop Surg 2020;28:e929.
- Darouiche RO. Spinal epidural abscess. N Engl J Med 2006;355:2012-2020.
- LaPenna PA, Roos KL. Bacterial infections of the central nervous system. Semin Neurol 2019;39:334-342.
- Reihsaus E, Waldbaur H, Seeling W. Spinal epidural abscess: A meta-analysis of 915 patients. Neurosurg Rev 2000;23:175-204.
- Sendi P, Bregenzer T, Zimmerli W. Spinal epidural abscess in clinical practice. QJM 2008;101:1-12.
- Shah AA, Yang H, Harris MB, Schwab JH. A classification system for spinal cord compression and its association with neurological deficit in spinal epidural abscess. Clin Spine Surg 2019;32:E126-E132.
- Rigamonti D, Liem L, Sampath P, et al. Spinal epidural abscess: Contemporary trends in etiology, evaluation, and management. Surg Neurol 1999;52:189-196.
- Berbari EF, Kanj SS, Kowalski TJ, et al. 2015 Infectious Diseases Society of America (IDSA) clinical practice guidelines for the diagnosis and treatment of native vertebral osteomyelitis in adults. Clin Infect Dis 2015;61:e26-e46.
- Babic M, Simpfendorfer CS, Berbari EF. Update on spinal epidural abscess. Curr Opin Infect Dis 2019;32:265-271.
- Tompkins M, Panuncialman I, Lucas P, Palumbo M. Spinal epidural abscess. J Emerg Med 2010;39:384-390.
- Devivo MJ. Epidemiology of traumatic spinal cord injury: Trends and future implications. Spinal Cord 2012;50:365-372.
- Shank CD, Walters BC, Hadley MN. Current topics in the management of acute traumatic spinal cord injury. Neurocrit Care 2019;30:261-271.
- Ropper AE, Ropper AH. Acute spinal cord compression. N Engl J Med 2017;376:1358-1369.
- Moutinho R, Tyrrell P, Cassar-Pullicino VN. Emergency and trauma imaging of the thoracolumbar spine. Semin Musculoskelet Radiol 2017;21:199-209.
- Expert Panel on Neurological Imaging and Musculoskeletal Imaging; Beckmann NM, West OC, Nunez D, et al. ACR Appropriateness Criteria suspected spine trauma. J Am Coll Radiol 2019;16:S264-S285.
- Ryken TC, Hadley MN, Walters BC, et al. Radiographic assessment. Neurosurgery 2013;72(Suppl 2):54-72.
- Patel MB, Humble SS, Cullinane DC, et al. Cervical spine collar clearance in the obtunded adult blunt trauma patient: A systematic review and practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2015;78:430-441.
- Schoenfeld AJ, Bono CM, McGuire KJ, et al. Computed tomography alone versus computed tomography and magnetic resonance imaging in the identification of occult injuries to the cervical spine: A meta-analysis. J Trauma 2010;68:109-113.
- Kirshblum SC, Burns SP, Biering-Sorensen F, et al. International standards for neurological classification of spinal cord injury (revised 2011). J Spinal Cord Med 2011;34:535-546.
- Al-Mutair A, Bednar DA. Spinal epidural hematoma. J Am Acad Orthop Surg 2010;18:494-502.
- Carlhan-Ledermann A, Laubscher B, Steinlin M, et al. Spinal epidural hematoma without significant trauma in children: Two case reports and review of the literature. BMC Pediatr 2020;20:77.
- Zheng H-X, Nyam T-TE, Liu C-A, et al. Spontaneous spinal epidural hematoma after normal spontaneous delivery with epidural analgesia: Case report and literature review. World Neurosurg 2020;137:214-217.
- Vanichkulbodee A, Issaragrisil S, Inboriboon PC. Massage-induced spinal epidural hematoma presenting with delayed paraplegia. Am J Emerg Med 2019;37:797.e1-797.e4.
- Alexiadou-Rudolf C, Ernestus RI, Nanassis K, et al. Acute nontraumatic spinal epidural hematomas: An important differential diagnosis in spinal emergencies. Spine 1998;23:1810-1813.
- Scott BB, Quisling RG, Miller CA, Kindt GW. Spinal epidural hematoma. JAMA 1976;235:513-515.
- Kou J, Fischgrund J, Biddinger A, Herkowitz H. Risk factors for spinal epidural hematoma after spinal surgery. Spine 2002;27:1670-1673.
- Kebaish KM, Awad JN. Spinal epidural hematoma causing acute cauda equina syndrome. Neurosurg Focus 2004;16:e1.
- Spector LR, Madigan L, Rhyne A, et al. Cauda equina syndrome. J Am Acad Orthop Surg 2008;16:471-479.
- Long B, Koyfman A, Gottlieb M. Evaluation and management of cauda equina syndrome in the emergency department. Am J Emerg Med 2020;38:143-148.
- Gitelman A, Hishmeh S, Morelli BN, et al. Cauda equina syndrome: A comprehensive review. Am J Orthop 2008;37:556-562.
- Domen PM, Hofman PA, Van Santbrink H, Weber WEJ. Predictive value of clinical characteristics in patients with suspected cauda equina syndrome. Eur J Neurol 2009;16:416-419.
- Lavy C, James A, Wilson-MacDonald J, Fairbank J. Cauda equina syndrome. BMJ 2009;338:b936.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
