Necrotizing Soft Tissue Infections
October 1, 2021
Reprints
AUTHORS
Chadd Nesbit, MD, PhD, System EMS Medical Director, Allegheny Health Network, Pittsburgh, PA
Stephanie Carlson, MD, Good Shepherd Medical Center, Hermiston, OR
PEER REVIEWER
Catherine Marco, MD, FACEP, Professor, Emergency Medicine and Surgery, Wright State University, Dayton, OH
EXECUTIVE SUMMARY
- Necrotizing soft tissue infections (NSTIs) are serious and potentially life-threatening.
- NSTIs initially can appear similar to simple superficial skin infections.
- NSTIs can be initially indolent, then rapidly progress.
- Extensive pain that appears to be out of proportion to the amount of tissue involved is a useful finding.
- Full-blown NSTIs are accompanied by sepsis and multisystem organ failure.
- Rapid recognition and early surgical debridement are the keys to successful treatment.
- Imaging may detect soft tissue gas formation but should not delay surgical debridement.
- Initially, antibiotic coverage should be broad spectrum, covering gram-positive, gram-negative, and anaerobic organisms.
- Clindamycin should be added in cases where group A streptococci are suspected.
- There is little or no proven benefit for adjunctive therapy with either hyperbaric oxygen therapy or intravenous immunoglobulin administration.
My most powerful memory of patients with necrotizing soft tissue infections is the smell. That sickening, gag-inducing smell as you approach the room. The experienced nurses would hand you a surgical mask with a dab of scented oil inside before you entered the room. Even then, you may pause as you enter to adjust to the overwhelming smell. Years of allergies and overuse of nasal decongestant sprays have burned out my olfactory sense, so I am not so affected by the odor. Such full-blown malodorous cases are obvious, prompting rapid treatment. As this article describes, the challenge is to identify the more subtle or indolent cases before they progress into extensive skin and soft tissue necrosis. As noted, there is no test or decision tool that can replace clinical judgment. So, don’t wait for the white count; if it looks suspicious, consult early.
— Joseph Stephan Stapczynski, MD, Editor
Introduction
Necrotizing soft tissue infections (NSTIs) produce an intensive inflammatory state that can injure and necrose the skin and subcutaneous tissues.1 These infections typically are associated with systemic toxicity.2 These infections are at one end of the skin and soft tissue infection spectrum, from erysipelas, an inflammation of the epidermis, to necrosis of the deeper tissue. NSTIs are life-threatening, requiring surgical debridement and cardiopulmonary support, in addition to intravenous (IV) antibiotics.
A characteristic of NSTIs is their tendency to spread along subcutaneous tissue planes. These planes can include the dermis, subcutaneous fat, and connective tissue, as well as the fascia and even the muscle.
Terms such as “hospital gangrene” or “gas gangrene” were used historically, but now have been replaced by more specific terms that denote the depth of involvement, such as synergistic necrotizing cellulitis, necrotizing adipositis, necrotizing fasciitis, and myonecrosis.3 The term NSTI encompasses all of these infections. Because of the high morbidity and mortality associated with NSTIs, the emergency physician should be prepared to identify these infections early in the assessment of the patient and initiate rapid, aggressive, and appropriate treatment. The overarching principle in the management of these infection is broad-spectrum IV antibiotics and early surgical debridement produces the best outcome; delays in both diagnosis and treatment lead to worsened outcomes.
NSTIs affect patients of all ages; however, they are more fatal in adults than children.4 NSTIs were thought to be relatively rare, with an estimate from an article in 2014 that most physicians will see only one NSTI in their career.5 In an article from 2006, the estimated annual incidence in the United States was only 500-1,500 cases.4
However, NSTIs are likely more common than reported, since there is a lack of standardized reporting, aside from the Centers for Disease Control and Prevention (CDC) surveillance reporting of Group A Streptococcus-related NSTIs.6 A study published in 2021 used the National Inpatient Sample (NIS) for the years 2012-2016 and the Watson Health (WH) data set for 2009-2013 to estimate the incidence of NSTIs for 2018. Both data sets noted increasing annual incidence and estimated the incidence of NSTIs to be 33,600 for the NIS and 28,500 for the WH in 2018, yielding an estimated annual incidence of 8.7 to 10.3 per 100,000 persons.7 The incidence also varies greatly depending on time of year, geographic location, and specific patient populations.6
The mortality from NSTIs is high; reported mortality rates are between 6% and 33%, and now are thought to average around 20%,8 which is an improvement from previously reported higher averages.6 Mortality is influenced by the presence of comorbidities, such as severe shock, immunocompromise, and advanced age of the patient.6 In addition to high mortality, NSTIs carry significant morbidity as well. One study reported limb loss in 15% of patients, while another study noted that 21% of patients with extremity NSTIs ultimately required amputation.9,10
Etiology
Multiple studies have shown that major risk factors for the development of NSTIs include diabetes, obesity, immunocompromised state, peripheral vascular disease, alcohol abuse, cirrhosis, chronic renal disease, IV drug use, history of abscess (especially at the onset of symptoms), blunt or penetrating trauma, and age.5,11,12 Even though advanced age and chronic diseases are noted risk factors, young, healthy patients still can be affected as well.5 (See Table 1.)
Table 1. Risk Factors Regarding Necrotizing Soft Tissue Infections | |
|
Developing NSTI |
Mortality Related to NSTI |
|
|
|
NSTI: necrotizing soft tissue infection Information gathered from multiple references, including Hakkarainen 2014,5 Wallace 2021,11 Bonne 2017,6 and VK 201312 | |
In a study of 60 patients with NSTI, 34 (57%) had lower extremity involvement, four (7%) had upper extremity involvement, 15 (25%) had involvement of the perineum, and seven (12%) had involvement of the abdominal wall.12 In the 60 cases, diabetes was the most common comorbidity. Increased mortality was seen in patients older than 50 years of age and with and initial serum creatinine > 1.2 mg/dL.12 In the cases with NSTI of the perineum — termed Fournier’s gangrene — all had a history of abscess or minor wound at disease onset. Diabetes was the most common chronic disease, and other comorbid factors included peripheral vascular disease, chronic obstructive pulmonary disease (COPD), chronic renal failure, and paraplegia.12
NSTI can follow trauma or surgery, and there is some evidence that damaged skeletal muscle may render the patient more susceptible to these infections.6 Skin barrier compromise or a break in the epithelium is associated with about 80% of NSTIs, with hematogenous spread accounting for the other cases.11 Obviously, there must be some exposure to the causative organism, but some of these bacteria and yeast are found in skin flora. NSTIs can occur anywhere, but the more commonly affected sites include the extremities or the perineum/genitalia.5 In the study noted earlier, a lower limb was involved in more than 50% of infections, followed by perineal involvement in another 25% of cases, with post-operative abdominal wall infection and then upper limb involvement noted least often in this series of 60 patients.12
Pathophysiology
NSTIs tend to progress over several days but may exhibit rapid progression over a matter of hours.11,13 This complex process is mediated by toxins produced by the involved organisms and cytokine activation, which leads to ischemia of tissue, ultimately culminating in cell death by necrosis.
NSTIs can be classified according to clinical features, location, tissues involved, and microbiology. Historically, a variety of names were attached to these infections based primarily on clinical features. To provide order and structure to classification, Giuliano and colleagues proposed two types of NSTI based on microbiology in 1977.14 Since then, the classification scheme has increased to four types.6,15 (See Table 2.) Type I is most common, involving mixed anaerobes and aerobes, with a more indolent course and abundant gas formation making the diagnosis easier to identify. Type III is the least common, leading to gas-forming myonecrosis, often related to aquatic gram-negative bacteria such as Vibrio spp. Type IV is caused by fungal pathogens and is associated with traumatic injuries.2,13
Polymicrobial NSTIs are more common because of the presence of gram-negative and anaerobic agents in and on the body as well as in the environment.2,11
Table 2. Microbiologic Classification of Necrotizing Soft Tissue Infections | |||
|
Category |
Cause |
Microbiology |
Clinical Features |
|
Type I (70% to 80% of cases) |
Polymicrobial or synergistic, often derived from bowel flora |
Mixed anaerobes and aerobes |
More indolent, easier to detect |
|
Type II (20% to 30% of cases) |
Often monomicrobial, derived from skin flora or the respiratory tract |
Usually Group A beta-hemolytic Streptococcus, occasionally
|
Aggressive, diagnosis often missed |
|
Type III (rare in United States, more common in Asia) |
Gram-negative aquatic bacteria |
Vibrio spp. |
Seafood ingestion or wounds contaminated with sea water |
|
Type IV (fungal) |
Trauma-associated |
Candida spp. (immunocompromised patients); Zygomycetes (immunocompetent patients) |
Aggressive, especially if immunocompromised |
|
Source: Adapted from: Morgan MS. Diagnosis and management of necrotising fasciitis: A multiparametric approach. J Hosp Infect 2010;75:249. | |||
Streptococcus pyogenes (group A streptococci) can invade tissues via manipulation of host cytoskeleton using CD44, which is a hyaluronic acid binding protein cellular receptor.16,17 S. pyogenes produce Streptolysin S, a cytotoxin that causes damage to tissue membranes and white blood cells.18 The S. pyogenes cell envelope contains a proteinase that can cleave and inactivate interleukin 8, a cytokine necessary for neutrophil recruitment, one mechanism for S. pyogenes to evade host immune response.19 Staphylococcus, specifically methicillin-resistant Staphylococcus, can cause toxin-mediated tissue damage.20 Clostridium species also cause tissue damage via toxins.2 The ensuing tissue destruction and necrosis prompts massive cytokine release, kicking off a vicious cycle, eventually leading to shock and multisystem organ failure.2
Clinical Features
The initial presentation of an NSTI can be quite subtle. Common findings of swelling and erythema do not distinguish NSTIs from more benign skin infections or inflammation. A useful characteristic is that NSTIs often have pain out of proportion to the degree of tissue involvement. Thus, clinical suspicion is the key to making the diagnosis in a timely fashion.21 Vital signs may be deceptively normal, especially at first.21 As stated, the initial presentation most often will consist of erythema, tenderness, warmth, and edema, although blistering frequently is noted.22 Signs such as crepitus, necrosis, and loss of sensation rarely are seen at the time of presentation, but these often will become apparent within a few days (average around four days), although sometimes within a few hours.22 (See Figure 1.)
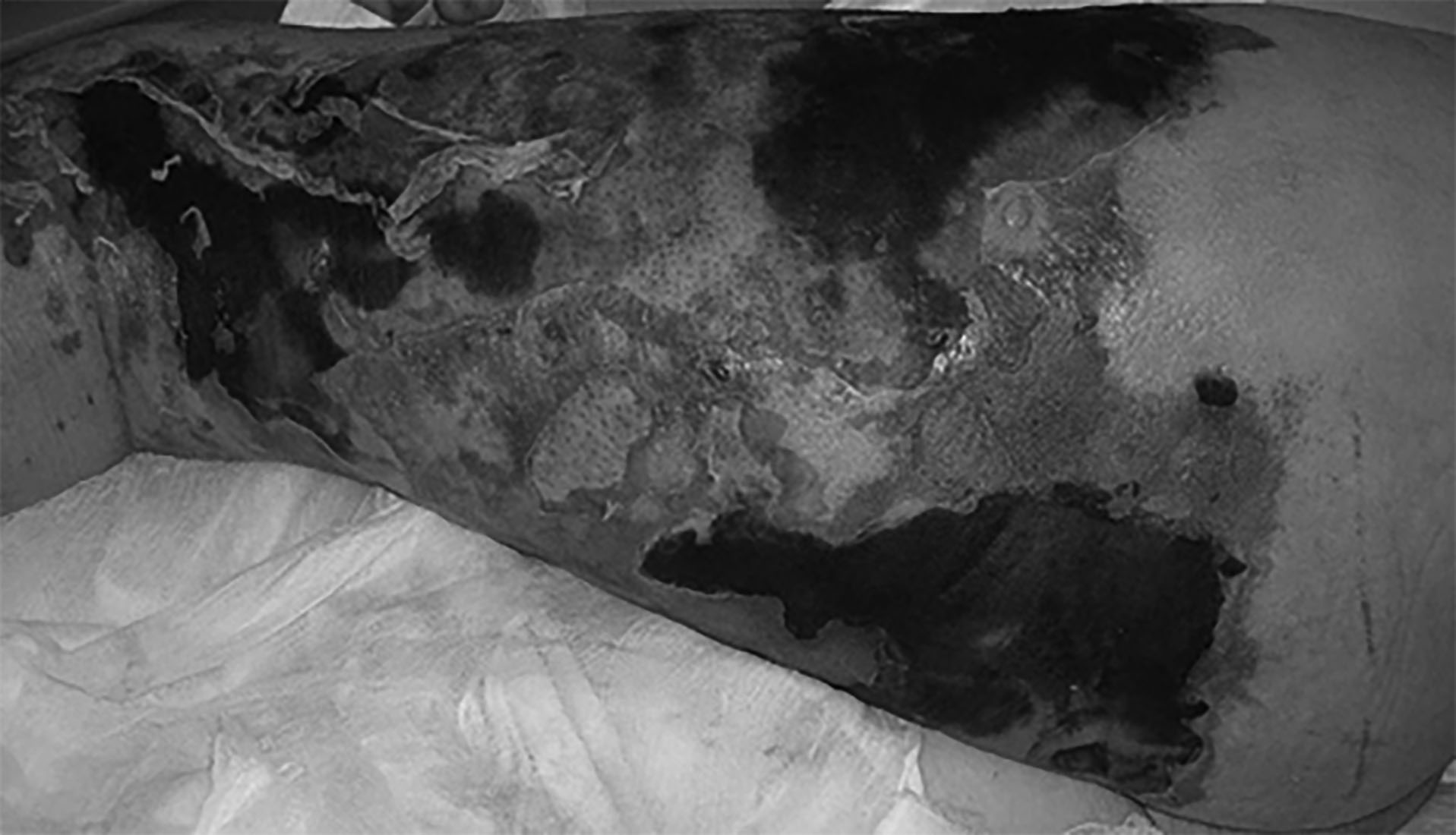
Figure 1. Necrotizing Fasciitis |
 |
|
43-year-old Caucasian male with necrotizing fasciitis. Preoperative photograph on the day of admission. Extensive erythema and necrosis of the left leg. Source: Smuszkiewicz P, Trojanowska I, Tomczak H. Late diagnosed necrotizing fasciitis as a cause of multiorgan dysfunction syndrome: A case report. Cases Journal 2008;1:125. doi:10.1186/1757-1626-1-125. Creative Commons. |
In addition to a high index of suspicion, the patient may provide historical information. The physician should ask about comorbidities, blunt or penetrating trauma, recent procedures, and disorders or medications associated with immunocompromise or immunosuppression, since these all are known to be risk factors for NSTI. A thorough physical exam also is crucial, looking at all body surfaces,especially since a significant percentage of NSTIs occur in the perineum.23
Because an NSTI may not be apparent on initial evaluation, it is important to pay special attention to patients who report worsening skin infection prompting a return visit to the ED. These patients should be reassessed thoroughly with suspicion for an NSTI.
Diagnosis
As previously stated, the key to diagnosis of NSTI is clinical suspicion. The aforementioned physical signs of skin necrosis and crepitus found on examination can be helpful, but they are not reliably present. Clinical suspicion for an NSTI should rely on “careful clinical examination and signs of local or systemic severity.”24 Blood tests and imaging studies may help guide diagnosis, but there is no diagnostic test that will rule in or rule out a diagnosis of NSTI. The gold standard for diagnosis remains tissue biopsy obtained at the time of debridement.23
Patients with NSTIs can exhibit leukocytosis, anemia, renal insufficiency, and, less commonly, hyponatremia and liver function disturbance.12 But these abnormal laboratory studies can appear in other infectious and inflammatory states, and so they are not specific to NSTIs.24 Imaging the affected area with plain radiographs, ultrasound, computed tomography (CT), and magnetic resonance (MR) looking for soft tissue gas all can be helpful, but gas formation is not specific for NSTIs, and some cases of NSTI will have very little to no detectable gas formation.21 (See Figure 2.) An important principle of imaging in the setting of NSTI is that it should never delay prompt surgical intervention.24
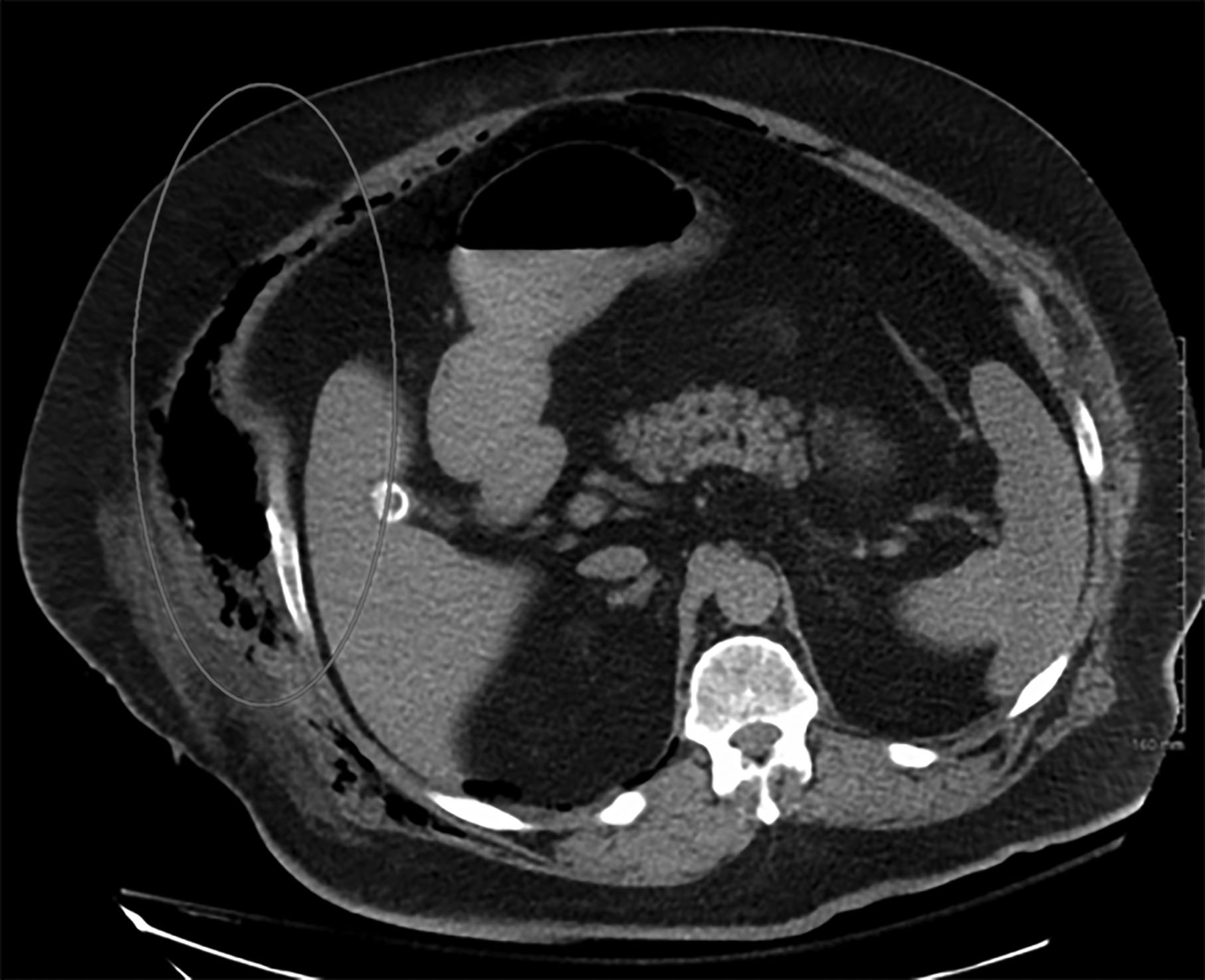
Figure 2. Necrotizing Fasciitis Computed Tomography Scan |
 |
|
Necrotizing fasciitis producing gas in the soft tissues as seen on computed tomography scan Source: James Heilman, MD, 2011, Creative Commons. |
Definitive NSTI diagnosis relies on tissue biopsy, which is obtained at the time of surgical debridement. In cases that are equivocal, a bedside biopsy by a surgeon, done under local anesthesia of the area of interest, can be done without the need for movement to the operating room. This bedside biopsy may reveal a “positive finger sign” in which a finger inserted along the fascial planes easily causes dissection of the tissues; this finding is considered diagnostic of NSTI.6 Other findings of NSTI during surgical intervention include necrotic or gray-appearing tissue, lack of blood flow, thrombosed vessels, gray “dishwater” drainage, muscles that do not contract, and weak tissue that does not resist blunt dissection with a finger.21 Tissue Gram stain and culture should be performed at the time of surgical intervention. Frozen tissue sections are not recommended for diagnosis in equivocal cases because of sampling error.25
Attempts have been made to construct and validate predictive algorithms for NSTIs with varying degrees of success. Perhaps the best known of these algorithms is the Laboratory Risk Indicator for Necrotizing Fasciitis, or LRINEC, score.26 This is a multi-component scoring system that includes white blood cell count, hemoglobin, sodium, glucose, creatinine, and C-reactive protein (CRP) level. (See Table 3.) Points are given for derangement of those specific laboratory results mentioned previously, with a maximum score of 13. The LRINEC score was then used to assign risk categories: ≥ 8 for high risk, 6-7 for moderate risk, and ≤ 5 for low risk.
Table 3. LRINEC and Two Proposed Modified LRINEC Scoring Systems | |||||
|
LRINEC |
Scoring |
mLRINEC Wu |
Scoring |
mLRINEC Borschitz |
Scoring |
|
WBC < 15 15-25 > 25 |
0 +1 +2 |
WBC > 15 |
+2 |
WBC < 15 15-25 > 25 |
0 +1 +2 |
|
Hgb > 13.5 11-13.5 < 11 |
0 +1 +2 |
Hgb < 11 |
+2 |
Hgb > 13.5 11-13.5 < 11 |
0 +1 +2 |
|
Na > 135 < 135 |
0 +2 |
Na < 135 |
+1 |
RBC < 4 |
+1 |
|
Glu < 180 mg/dL > 180 mg/dL |
0 +1 |
Glu > 180 |
+2 |
Fibrinogen > 750 mg/dL |
+2 |
|
Cr < 1.6 mg/dL > 1.6 mg/dL |
0 +1 |
Cr > 1.6 |
+3 |
Cr >1.35 |
+2 |
|
CRP < 15 mg/dL > 15 mg/dL |
0 +4 |
CRP > 30 mg/L |
+4 |
CRP > 15 mg/dL |
+4 |
|
|
|
Lactate > 18 mg/dL |
+4 |
Pain mild/none intermediate strong |
0 +1 +2 |
|
|
|
Comorbid liver disease |
+3 |
Fever < 37.5°C 37.6-37.9°C > 38°C |
0 +1 +2 |
|
|
|
|
|
Tachycardia > 100 bpm |
+1 |
|
|
|
|
|
AKI no yes |
0 +1 |
|
|
12 maximum; < 6 low risk |
|
> 12 high risk |
|
> 8 strong suspicion; 6-7 suspect; < 5 no suspicion |
|
LRINEC: Laboratory Risk Indicator for Necrotizing Fasciitis; mLRINEC: modified Laboratory Risk Indicator for Necrotizing Fasciitis; WBC: white blood cell count; Hgb: hemoglobin; Na: sodium; RBC: red blood cell; Glu: glucose; Cr: creatinine; CRP: C-reactive protein; bpm: beats/minute; AKI: acute kidney injury; NSTI: necrotizing soft tissue infection Information extracted from MDCalc LRINEC Score for Necrotizing Soft Tissue Infection, Hsiao et al 2020,27 Wu et al 2021,29 Borschitz et al 2015.30 | |||||
However, a study by Hsiao and colleagues from 2020 found the LRINEC score not to be a very useful tool in a study of 106 patients with NSTI and 825 patients with severe cellulitis.27 Using a LRINEC score of ≥ 6, this study found a sensitivity of 43%, a specificity of 83%, a positive likelihood ratio (LR+) of 2.56, and a negative likelihood ratio (LR-) of 0.68 for NSTI. Increasing the threshold to an LRINEC score of ≥ 8 produced a sensitivity of 27%, specificity of 93%, an LR+ of 3.76, and an LR- of 0.78 for NSTI. As with many decision tools, scores at the extreme are more useful in distinguishing those with disease from those without than scores in the middle range.
As the previously mentioned study found, the LRINEC score has not held up with external validation. There are high false-positive rates in the setting of cellulitis and high false-negative rates in the setting of confirmed NSTI.28 However, the study by Neeki and colleagues found the LRINEC to be more accurate in NSTI patients with diabetes; an LRINEC score of ≥ 8 had a sensitivity of 56% and a specificity of 97% in their diabetic patients.28
Modified versions of the LRINEC score have been developed in which researchers added additional variables in an attempt to increase sensitivity and specificity of the original score. One such study included the presence of liver disease and lactate and changed the parameters of the other laboratory markers.29 Under this system, a score of 12 or greater puts a patient in the high-risk category. Another study added fibrinogen levels greater than 750 mg/dL as well as pain rating and fever.30 A very recent paper by Wu et al redefined the cut-off values for the original LRINEC score, substituted high-sensitivity CRP for regular CRP, and added the comorbidities of diabetes and kidney disease to derive another modified LRINEC score.31 All these modifications appear to have yielded a much higher sensitivity and specificity, but further validation is needed before they can be relied upon in routine clinical use.
As with any scoring system, the clinician’s gestalt should serve as a guide. Patients with low LRINEC or mLRINEC scores may have an NSTI, and delayed surgical consultation may be detrimental to patient outcome. There is some suggestion that an mLRINEC score could be trended to monitor for progression along the spectrum of NSTI, but, again, more confirmatory studies need to be done.
Differential Diagnosis
The differential diagnosis of NSTI includes many other skin and soft tissue conditions, some of which could be considered part of the NSTI spectrum. Possible diagnoses include other staphylococcal infections, such as impetigo, furuncle, carbuncle, folliculitis, scalded skin syndrome, bacteremia, and insect bites — especially brown recluse spider bites, which are associated with methicillin-resistant S. aureus (MRSA).23 Some of these can be purulent infections, and some can be streptococcal. Other possible conditions, such as disseminated intravascular coagulation, toxic shock syndrome, purpura fulminans, fungemia, certain toxidromes, and primary dermatologic disease, may be mistaken for an NSTI.32 Epididymitis, orchitis, and testicular torsion can cause genital pain and swelling in men and may mimic an NSTI, such as Fournier’s gangrene.
Management of Necrotizing Soft Tissue Infections
As noted previously, management of NSTIs is predicated on the timely recognition that this type of infection may be the diagnosis. A high index of suspicion based on examination of the patient, risk factors and predisposing conditions, laboratory data, and perhaps imaging studies should prompt the provider to initiate treatment immediately. Even with aggressive treatment, there still is significant morbidity associated with these infections. Administration of antibiotics without aggressive surgical debridement of dead and devitalized tissue has an associated mortality of nearly 100%.33
The treatment of necrotizing infections is a three-part process consisting of early and aggressive surgical debridement of dead and devitalized tissues coupled with appropriate empiric antibiotic treatment and hemodynamic support of the critically ill patient in an intensive care unit (ICU) setting by a multidisciplinary team.
Surgical Debridement
Necrotizing skin infection is a surgical emergency requiring rapid and decisive intervention. Patients in whom there is a high index of suspicion, rapid progression of systemic manifestations of disease, or a positive finger test warrant early surgical intervention as part of a multimodal treatment plan.33 Source control likely should take place as soon as possible, and certainly within 12 hours of admission.34 Early and complete debridement is associated with higher rates of survival than debridement that was either delayed or incomplete.34 Patients with delayed debridement also have been shown to have a higher number of trips to the operating room for re-debridement, as well as more complications, such as septic shock and renal failure.35
The goal of operative management of necrotizing infection is to excise all dead and devitalized tissues, sometimes referred to as “cut until it bleeds.” This will necessitate debridement, possibly on multiple occasions, until all devitalized tissue has been excised.33 Removal of tissue of questionable viability should be delayed and reassessed during a second look.34 The exact timing of repeat debridement has not been well studied and commonly takes place in 12 to 24 hours. However, a clinical picture of worsening infection, rising white blood cell count, and worsening shock may prompt earlier repeat exploration.34 Delayed repeat debridement has been shown to result in worsened survival.36 If possible, cultures should be collected from deep tissue spaces or abscesses, since these may help to guide antibiotic therapy.6
Empiric Antibiotic Therapy
As mentioned earlier, simply treating a necrotizing skin infection with IV antibiotics is not adequate. Empiric, broad-spectrum antibiotics with activity against gram-positive, gram-negative, anaerobic, and MRSA isolates are necessary to cover the most likely pathogens. As culture data become available, antibiotic therapy can be tailored. However, the initial approach must be timely and cover all possible sources of infections.6
There are many possible choices for empiric antibiotic therapy. A typical empiric regimen usually consists of vancomycin, linezolid, or daptomycin used in combination with one of the following options:
• piperacillin-tazobactam;
OR
• a carbapenem, such as meropenem, ertapenem, or imipenem-cilastatin;
AND
• clindamycin.
Local patterns of resistance and hospital antibiograms should help to guide therapy as well. If there is a high prevalence of local resistance to ceftriaxone and fluoroquinolones, these agents should be avoided, since they are sometimes used in empiric therapy regimens. Similarly, the use of ampicillin-
sulbactam and ticarcillin-clavulanate is no longer recommended as empiric therapy because of resistance.33 Tigecycline has been suggested as a possible monotherapy in patients who have been hospitalized recently and may be colonized with resistant bacteria.37 Empiric therapy with antifungal agents is likely not necessary unless there is evidence in culture growth or on stains.6
Clindamycin is an important addition to the initial empiric therapy. Clindamycin has antitoxin effects against toxin-producing strains of Streptococcus and Staphylococcus. Clindamycin is a lincosamide antibiotic that acts as an inhibitor of ribosomal translocation, thus inhibiting the translation of ribonucleic acid (RNA) into protein.6 The addition of clindamycin suppresses cytokine and toxin production. Penicillin should be used along with clindamycin to cover for possible resistance of group A streptococci to clindamycin. (See Table 4.)
Table 4. Empiric Antibiotics for Necrotizing Soft Tissue Infection | ||
|
Organism |
Medication |
Dosage |
|
Methicillin-resistant Staphylococcus aureus |
Vancomycin Linezolid Tedizolid Daptomycin |
15 mg/kg IV q 12 h 600 mg IV q 12 h 200 mg IV q 24 h 4 mg/kg IV q 24 h |
|
Gram-negative
|
Piperacillin/tazobactam Imipenem/cilastatin Meropenem Ertapenem Ceftriaxone plus metronidazole Ciprofloxacin plus metronidazole Levofloxacin plus metronidazole Gentamycin or tobramycin plus metronidazole |
3.375 g IV q 6-8 h 1 g IV q 6-8 h 1 g IV q 8 h 1 g IV q 24 h 2 g IV q 24 h 500 mg IV q 6 h 400 mg IV q 12 h 500 mg IV q 6 h 750 mg IV q 24 h 500 mg IV q 6 h 4-7 mg/kg IV q 24 h 500 mg IV q 6 h |
|
Group A streptococci |
Clindamycin plus penicillin |
600-900 mg IV q 8 h 2-4 million units IV q 4-6 h |
|
IV: intravenous; h: hours Used with permission from Lamb M, Lloyd A. Necrotizing soft-tissue infection: Disease overview and updated treatment strategies. US Pharm 2017;42:HS16-HS20. | ||
Antibiotic therapy should be tailored to the specific cause of the infection once culture data are available. Firm data regarding the duration of treatment are lacking. It is reasonable to think that antibiotic therapy likely should be continued for a total of 48-72 hours after the patient meets the following three criteria:
1. The patient should no longer require surgical debridement.
2. The patient should not be febrile.
3. The patient should be hemodynamically stable.25
Additional Considerations
Care of the patient with a necrotizing infection should be undertaken by a team consisting of surgeons, infectious disease specialists, and critical care intensivists. This team will need to work closely to coordinate the need for early surgical debridement with the need for appropriate IV antibiotic therapy and hemodynamic support of these critically ill patients. Depending on the area that is infected, urological, gynecological, or colorectal surgical subspecialists may need to be involved. Orthopedic surgeons will play a role if there is bone involvement or an amputation is needed due to devitalization of a limb.
Once stabilized and out of the immediate life-threatening stage, these patients may require the services of multiple other specialties, such as dietary specialists, physical and occupational therapists, wound care specialists, plastic/reconstructive surgeons, and physiatrists. Long periods of intensive rehabilitation may be necessary to help these patients regain as much of their former functional independence as possible.5 Patients who do survive often have significantly altered body appearance and functional deficits. They may require long-term pain medication or assistive devices and frequently have decreased physical, social, and emotional functioning.38
Adjunctive Therapies
Intravenous immunoglobulin (IVIG) has been postulated to be of benefit in cases of necrotizing infection based on the ability of the antibodies to neutralize extracellular toxins produced by some strains of bacteria causing these types of infections.39 There have been multiple studies investigating the use of IVIG in the setting of necrotizing infections, but they have been fraught with significant limitations, making it difficult to draw conclusions regarding the effectiveness of this therapy.39 The 2014 guidelines from the Infectious Diseases Society of America (IDSA) did not recommend the use of this therapy for necrotizing infections caused by group A Streptococcus species.25
In 2018, Parks et al published a meta-analysis of patients treated with clindamycin and IVIG who had streptococcal toxic shock syndrome.40 In this analysis, the use of IVIG was associated with a significant reduction in 30-day mortality from 33.7% to 15.7%. A very recent prospective study of necrotizing infections caused by group A Streptococcus (GAS) showed that IVIG was associated with a reduction in mortality at 90 days; Lasso regression analysis of the GAS cases identified increased age (odds ratio [OR], 1.15, per year), male sex (OR, 5.09), septic shock (OR, 1.96), and IVIG not administered (OR, 3.15) as independent variables associated with mortality.41 Given these recent findings, it likely is reasonable to consider the use of IVIG as an adjunctive treatment of necrotizing fasciitis where streptococci are likely. However, IVIG administration should not delay surgery or treatment with broad-spectrum antibiotics.
Hyperbaric oxygen (HBO) is the delivery of 100% oxygen at increased atmospheric pressure, usually two to three times normal atmospheric pressure. Increasing atmospheric pressure allows for more oxygen to be dissolved in the blood, leading to greater availability of oxygen to the tissues. At higher concentrations of oxygen, a number of potentially beneficial effects may be seen, including improved leukocyte function.
The use of hyperbaric therapy as an adjunctive treatment for necrotizing fasciitis has been explored as a potential means of reducing the morbidity and mortality associated with necrotizing soft tissue infections. A Cochrane review from 2015 did not find any trials that met inclusion criteria for review.42 A 2019 review using PRISMA guidelines identified 21 studies that evaluated the efficacy for hyperbaric oxygen therapy for NSTI, 19 of them case studies with control groups. The majority of the studies were judged as being of poor quality with a high to critical risk of bias.43 The authors concluded that there is a need for randomized controlled trials to shed light on what may be a life-saving therapy. If the decision is made to use HBO therapy, it must be viewed as an adjunctive treatment and should not delay surgical intervention or the administration of antibiotics.
Wound care is a vital part in the healing process for a patient who has survived the initial debridement and hemodynamic insult of a necrotizing soft tissue infection. These patients may be left with large, open wounds due to the initial debridement of dead and devitalized tissues, followed by re-exploration of the wound and possible repeat debridement of tissues.34
Negative pressure wound therapy (NPWT), also known as vacuum-assisted wound closure, is a wound dressing system that applies less-than-atmospheric pressure to a wound in a constant or intermittent fashion that is designed to remove fluid from the wound and promote healing.44 These systems were developed in the 1990s and typically consist of an open-cell foam sponge that is placed into the wound cavity. The cavity then is covered by a membrane that is connected to a closed vacuum circuit, which can be evacuated, creating negative pressure in the wound.
Many types of wounds commonly are treated with NPWT, and multiple beneficial direct and indirect effects on wound healing have been shown in animal and human studies.45,46 However, studies evaluating the benefits of NPWT in the setting of NSTIs are lacking. A systematic review published in 2020 of 48 studies did not show clear evidence for the use of NPWT over standard therapies, although only three of the studies reviewed included patients with necrotizing wounds.44 This recent review found that low-quality data showed a benefit for NWPT compared to standard therapies for wound closure in patients with wounds healing by secondary intention.44 However, only two papers in this meta-analysis looked at wounds specifically from necrotizing fasciitis, and both were found to have a high risk of bias relative to outcomes.44
A case series of seven patients by Chen et al in 2019 reported the use of NPWT immediately after surgical debridement in cases of head and neck cancers.47 The device was left in place until the infection was controlled and then it was removed and replaced by conventional drainage therapy approach. They reported “various advantages” and “excellent clinical outcomes” in this series.47
New Agents
The last three to five years have seen the development of new antimicrobial and other biologic agents for use in the treatment of NSTI. There have been three new antibiotics and one non-antibiotic agent described in the literature that may have use in the treatment of NSTI.
Tedizolid is an oxazolidinone-class antibiotic related to linezolid. It is approved for use against MRSA and other gram-positive organisms that are multidrug-resistant. Unlike linezolid, tedizolid requires only once-daily dosing, which may be either IV or oral.48 There is evidence as well that tedizolid has a lower rate of myelotoxicity.49 Although effective against MRSA and gram-positive organisms, tedizolid has not been studied in the management of NSTI.
Dalbavancin and oritavancin are both lipoglycopeptides that have very long half-lives, allowing for single or weekly dosing of these agents. Both of these agents have been approved for use in the management of skin infections, but they have some limitations. The dosing of dalbavancin must be reduced in patients with a creatinine clearance less than 30 mL/minute.48 Oritavancin does not have any modifications for dosing in renal failure. However, it may increase the effects of warfarin and it prolongs coagulation tests in patients receiving heparin.48 Again, like tedizolid, there have been no specific trials evaluating the effectiveness of the lipoglycopeptides against NSTI.
Reltecimod is not an antibiotic, but rather an immunomodulatory peptide. This molecule, formerly known as AB103, is an octapeptide that has homology with part of the CD28 T-lymphocyte receptor.50 It acts as an antagonist of superantigen exotoxins and prevents them from binding to the CD28 receptor on T-lymphocytes. By binding to this receptor, it modulates the inflammatory process seen in NSTI. Reltecimod was tested in a Phase II trial for NSTI at two different doses vs. placebo.51 In this trial, reltecimod showed an improvement in sequential organ failure assessment score at two weeks, but no difference in the number of debridements, ICU or ventilator-free days, or any significant differences in plasma or tissue cytokine levels.51
The ACCUTE trial was a Phase III trial of reltecimod that was conducted as a multicenter trial enrolling 290 patients with necrotizing soft tissue infections.50 Although the trial did not reach statistical significance for the primary composite endpoint for those in the modified intention-to-treat analysis, the patients in the per-protocol group, a group that had 17 patients excluded for protocol violations, did reach statistical significance regarding improvement in resolution of organ dysfunction and hospital discharge status.50 Further study is necessary to determine optimal usage of this novel immune modulator in the setting of NSTI.
Additional Considerations and Potential Pitfalls
By far, the greatest potential pitfall in the management of NSTI is delay in diagnosis. Because this is a rapidly progressing disease, a delay of even a few hours may lead to significant deterioration of the patient. As discussed earlier, there is no single reliable test for this disease, meaning this diagnosis requires a high index of suspicion. Relying on laboratory analysis, imaging, or physical examination in isolation may lead to missing the diagnosis and a worsened outcome for the patient. However, when taken together, and examined in light of predisposing factors or comorbid conditions of the patient, the clinical picture may be somewhat clearer as to the diagnosis.
It is critical to remember that a low LRINEC or modified LRINEC score does not exclude this diagnosis, and if the clinical suspicion for NSTI remains high, it is imperative that the emergency department (ED) clinician advocate for early surgical evaluation and possible intervention on behalf of the patient. A low LRINEC score may be uncommon in a patient with NSTI, but it does not eliminate the possibility of the condition in the patient.
Disposition
The disposition of most of these patients is transfer to the operating room for urgent debridement with initiation of broad-spectrum antibiotic therapy. Postoperatively, these patients likely should be admitted to the ICU as mentioned previously. Re-exploration is recommended 12 to 36 hours following initial debridement, and this may need to be repeated until no more necrosis is found.32,34 Some patients may even benefit from transfer to a burn center. Patients treated at these specialty centers had more procedures and longer lengths of stay.52
Physical/occupational therapy and rehabilitation are crucial parts of recovery following an extended hospital stay, which often is the case with NSTI patients.34 Factors such as age older than 60 years, female, nonwhite, perineal involvement, and amputation all are independently associated with discharge to a skilled nursing facility.10 The risk of readmission within 90 days ranged from 24% to 29%, the majority of which were unplanned.7 The median cost of these readmissions was $13,590, adding to an already expensive initial admission with one or more operating room cases and ICU level of care.7 The most common associated diagnoses for readmission were infection, acute kidney injury, and shock.7 Even with appropriate treatment, the mortality of NSTI also remains high. As mentioned previously, it is estimated to be around one-fifth to one-fourth of patients affected.
Summary
Soft tissue infections span a spectrum from superficial infections, such as erysipelas, to deep infections, such as the NSTIs discussed in this review. Many soft tissue infections are diagnosed easily, treated with appropriate oral antibiotics, and do not cause significant morbidity and mortality. Some soft tissue infections may cause disease that is severe enough to require hospitalization of the patient and treatment with IV antibiotics. An even smaller number of infections, the NSTIs, cause severe illness and, even with appropriate treatment, cause significant morbidity and mortality.
The key to diagnosis of NSTIs is to consider the possibility of the infection when examining the patient. If NSTI is a possible diagnosis when the patient presentation along with physical findings, history, comorbidities, and laboratory workup are considered jointly, then prompt surgical evaluation of the patient is necessary. Laboratory workup, imaging, and administration of antibiotics all may occur concurrently, but they should not delay the evaluation of the patient by a surgeon. There is no single laboratory test that will diagnose NSTI. The diagnosis is based on findings at surgical exploration, but it may be suggested by comorbid conditions of the patient, physical examination, and laboratory and imaging studies. The emergency physician must advocate for the patient if the physician believes that NSTI is the diagnosis.
Patients may progress from looking relatively well to displaying signs of septic shock in a short period of time. They may need administration of aggressive amounts of fluid and blood pressure support with vasoactive agents, as well as treatment with antibiotics. They likely will require ICU-level care.
Post-operative management is a multidisciplinary process and will include surgeons, intensivists, infectious disease specialists, wound care specialists, nutritionists, plastic and reconstructive surgeons, and rehabilitation physicians. Even if the patient survives surgery, they likely will face months of rehabilitation because of the significant soft tissue loss due to debridement that often is necessary to save the life of the patient.
REFERENCES
- Baiu I, Staudenmayer K. Necrotizing soft tissue infections. JAMA 2019;321:1738.
- Mishra SP, Singh S, Gupta SK. Necrotizing soft tissue infections: Surgeon’s prospective. Int J Inflam 2013;2013:60962
- Puvanendran R, Huey JC, Pasupathy S. Necrotizing fasciitis. Can Fam Physician 2009;55:981-987.
- Ellis Simonsen SM, van Orman ER, Hatch BE, et al. Cellulitis incidence in a defined population. Epidemiol Infect 2006;134:293-299.
- Hakkarainen TW, Kopari NM, Pham TN, Evans HL. Necrotizing soft tissue infections: Review and current concepts in treatment, systems of care, and outcomes. Curr Probl Surg 2014;51:344-362.
- Bonne SL, Kadri SS. Evaluation and management of necrotizing soft tissue infections. Infect Dis Clin North Am 2017;31:497-511.
- May AK, Talisa VB, Wilfret DA, et al. Estimating the impact of necrotizing soft tissue infections in the United States: Incidence and re-admissions. Surg Infect (Larchmt) 2020;22:509-515.
- Nawijn F, Smeeing DPJ, Houwert RM, et al. Time is of the essence when treating necrotizing soft tissue infections: A systematic review and meta-analysis. World J Emerg Surg 2020;15:4.
- Hua C, Bosc R, Sbidian E, et al. Interventions for necrotizing soft tissue infections in adults. Cochrane Database Syst Rev 2018;5:CD011680.
- Horn DL, Shen J, Roberts E, et al. Predictors of mortality, limb loss, and discharge disposition at admission among patients with necrotizing skin and soft tissue infections. J Trauma Acute Care Surg 2020;89:186-191.
- Wallace HA, Perera TB. Necrotizing fasciitis. In: StatPearls [Internet]. StatPearls Publishing; 2021. Updated Nov. 20, 2020.
- Kalaivani V, Hiremath BV, Indumathi VA. Necrotising soft tissue infection-risk factors for mortality. J Clin Diagn Res 2013;7:1662-1665.
- Zhao JC, Zhang BR, Shi K, et al. Necrotizing soft tissue infection: Clinical characteristics and outcomes at a reconstructive center in Jilin Province. BMC Infect Dis 2017;17:792.
- Giuliano A, Lewis F, Hadley K, et al. Bacteriology of necrotizing fasciitis. Am J Surg 1977;134:52-57.
- Morgan MS. Diagnosis and management of necrotizing fasciitis: A multiparametric approach. J Hosp Infect 2010;75:249-257.
- Cywes C, Wessels MR. Group A Streptococcus tissue invasion by CD44-mediated cell signalling. Nature 2001;414:648-652.
- Schrager HM, Albertí S, Cywes C, et al. Hyaluronic acid capsule modulates M protein-mediated adherence and acts as a ligand for attachment of group A Streptococcus to CD44 on human keratinocytes. J Clin Invest 1998;101:1708-1716.
- Nizet V, Beall B, Bast DJ, et al. Genetic locus for streptolysin S production by group A streptococcus. Infect Immun 2000;68:4245-4254.
- Edwards RJ, Taylor GW, Ferguson M, et al. Specific C-terminal cleavage and inactivation of interleukin-8 by invasive disease isolates of Streptococcus pyogenes. J Infect Dis 2005;192:783-790.
- Hamilton SM, Bryant AE, Carroll KC, et al. In vitro production of panton-valentine leukocidin among strains of methicillin-resistant Staphylococcus aureus causing diverse infections. Clin Infect Dis 2007;45:1550-1558.
- Anaya DA, Patchen Dellinger E. Necrotizing soft-tissue infection: Diagnosis and management. Clin Infect Dis 2007;44:705-710.
- Wang YS, Wong CH, Tay YK. Staging of necrotizing fasciitis based on the evolving cutaneous features. Int J Dermatol 2007;46:1036-1041.
- Headley AJ. Necrotizing soft tissue infections: A primary care review. Am Fam Physician 2003;68:323-328.
- Madsen MB, Arnell P, Hyldegaard O. Necrotizing soft-tissue infections: Clinical features and diagnostic aspects. Adv Exp Med Biol 2020;1294:39-52.
- Stevens DL, Bisno AL, Chambers HF, et al; Infectious Diseases Society of America. Practice guidelines for the diagnosis and management of skin and soft tissue infections: 2014 update by the Infectious Diseases Society of America. Clin Infect Dis 2014;59:e10-e52.
- Wong CH, Khin LW, Heng KS, et al. The LRINEC (Laboratory Risk Indicator for Necrotizing Fasciitis) score: A tool for distinguishing necrotizing fasciitis from other soft tissue infections. Crit Care Med 2004;32:1535-1541.
- Hsiao CT, Chang CP, Huang TY, et al. Prospective validation of the Laboratory Risk Indicator for Necrotizing Fasciitis (LRINEC) score for necrotizing fasciitis of the extremities. PLoS One 2020;15:e0227748.
- Neeki MM, Dong F, Au C, et al. Evaluating the Laboratory Risk Indicator to differentiate cellulitis from necrotizing fasciitis in the emergency department. West J Emerg Med 2017;18:684-689.
- Wu PH, Wu KH, Hsiao CT, et al. Utility of modified Laboratory Risk Indicator for Necrotizing Fasciitis (MLRINEC) score in distinguishing necrotizing from non-necrotizing soft tissue infections. World J Emerg Surg 2021;16:26.
- Borschitz T, Schlicht S, Siegel E, et al. Improvement of a clinical score for necrotizing fasciitis: ‘Pain out of proportion’ and high CRP levels aid the diagnosis. PLoS One 2015;10:e0132775.
- Wu H, Liu S, Li C, Song Z. Modified Laboratory Risk Indicator for Necrotizing Fasciitis (m-LRINEC) score system in diagnosing necrotizing fasciitis: A nested case-control study. Infect Drug Resist 2021;14:2105-2112.
- Stevens DL, Bisno AL, Chambers HF, et al; Infectious Diseases Society of America. Practice guidelines for the diagnosis and management of skin and soft-tissue infections. Clin Infect Dis 2005;41:1373-1406.
- Stevens DL, Badour LM. Necrotizing soft tissue infections. UpToDate. Updated Aug. 25, 2021.
- Sartelli M, Guirao X, Hardcastle TC, et al. 2018 WSES/SIS-E consensus conference: Recommendations for the management of skin and soft-tissue infections. World J Emerg Surg 2018;13:58.
- Kobayashi L, Konstantinidis A, Shackelford S, et al. Necrotizing soft tissue infections: Delayed surgical treatment is associated with increased number of surgical debridements and morbidity. J Trauma 2011;71:1400-1405.
- Okoye O, Talving P, Lam L, et al. Timing of redébridement after initial source control impacts survival in necrotizing soft tissue infection. Am Surg 2013;79:1081-1085.
- Eckmann C, Montravers P. Current management of necrotizing soft-tissue infections. Curr Opin Infect Dis 2021;34:89-95.
- Kruppa C, Hutter DJ, Königshausen M, et al. Necrotizing fasciitis and the midterm outcomes after survival. SAGE Open Med 2019;9:2050312119842433.
- Stevens DL, Bryant AE. Necrotizing soft-tissue infections. N Engl J Med 2017;377:2253-2265.
- Parks T, Wilson C, Curtis N, et al. Polyspecific intravenous immunoglobulin in clindamycin-treated patients with streptococcal toxic shock syndrome: A systematic review and meta-analysis. Clin Infect Dis 2018;67:1434-1436.
- Bruun T, Rath E, Madsen MB, et al; INFECT Study Group. Risk factors and predictors of mortality in streptococcal necrotizing soft-tissue infections: A multicenter prospective study. Clin Infect Dis 2021;72:293-300.
- Levett D, Bennett MH, Millar I. Adjunctive hyperbaric oxygen for necrotizing fasciitis. Cochrane Database Syst Rev 2015;1:CD007937.
- Faunø Thrane J, Ovesen T. Scarce evidence of efficacy of hyperbaric oxygen therapy in necrotizing soft tissue infection: A systematic review. Infect Dis (Lond) 2019;51:485-492.
- Zens Y, Barth M, Bucher HC, et al. Negative pressure wound therapy in patients with wounds healing by secondary intention: A systematic review and meta-analysis of randomised controlled trials. Syst Rev 2020;9:238.
- Orgill DP, Manders EK, Sumpio BE, et al. The mechanisms of action of vacuum assisted closure: More to learn. Surgery 2009;146:40-51.
- Huang C, Leavitt T, Bayer LR, Orgill DP. Effect of negative pressure wound therapy on wound healing. Curr Probl Surg 2014;51:301-331.
- Chen SJ, Chen YX, Xiao JR, et al. Negative pressure wound therapy in necrotizing fasciitis of the head and neck. J Oral Maxillofac Surg 2019;77:87-92.
- Lamb MM, Lloyd A. Necrotizing soft-tissue infection: Disease overview and updated treatment strategies. US Pharm 2017;42:HS16-HS20.
- Bassetti M, Castaldo N, Carnelutti A, et al. Tedizolid phosphate for the treatment of acute bacterial skin and skin-structure infections: An evidence-based review of its place in therapy. Core Evid 2019;14:31-40.
- Bulger EM, May AK, Robinson BRH, et al; ACCUTE Study Investigators. A novel immune modulator for patients with necrotizing soft tissue infections (NSTI): Results of a multicenter, phase 3 randomized controlled trial of Reltecimod (AB 103). Ann Surg 2020;272:469-478.
- Bulger EM, Maier RV, Sperry J, et al. A novel drug for treatment of necrotizing soft-tissue infections: A randomized clinical trial. JAMA Surg 2014;149:528-536.
- Endorf FW, Klein MB, Mack CD, et al. Necrotizing soft-tissue infections: Differences in patients treated at burn centers and non-burn centers. J Burn Care Res 2008;29:933-938.
Necrotizing soft tissue infections (NSTIs) produce an intensive inflammatory state that can injure and necrose the skin and subcutaneous tissues.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
