Management of Asthma and Chronic Obstructive Pulmonary Disease Exacerbations
November 1, 2021
Reprints
AUTHORS
Zachary Freedman, MD, Emergency Medicine Resident, New York-Presbyterian, New York, NY
Osman R. Sayan, MD, Associate Professor of Emergency Medicine, Columbia University Medical Center, New York, NY
PEER REVIEWER
Steven M. Winograd, MD, FACEP, Attending Emergency Physician, Keller Army Community Hospital, West Point, NY
EXECUTIVE SUMMARY
- Asthma is a disease that most often develops in children and generally is reversible. While many children are brought to the emergency department (ED) once audible wheezing in heard, chronic cough often precedes the wheezing and usually is the first symptom of an exacerbation.
- Chronic obstructive pulmonary disease (COPD) most often develops over years as a result of smoking and generally is not totally reversible. Patients generally present with cough, shortness of breath, and increased sputum production.
- As with any ED patient, patients with asthma or COPD should always be evaluated for emergent intubation. This is a clinical decision and should not wait for laboratory evaluation.
- Pneumothorax can cause a severe presentation and even death in patients with asthma or COPD. The pneumothorax does not need to be large to cause symptoms.
Given the regularity with which we see patients with asthma and chronic obstructive pulmonary disease (COPD), it is important to have a framework and understand the extent, etiology, diagnosis, and treatment of these conditions. This article will establish such a framework, with a focus on the management of patients with asthma or COPD in the emergent setting.
This article will discuss emergent management of patients with asthma and COPD exacerbations, as well as the epidemiology, etiology, and pathophysiology of each condition. Next, the clinical features and diagnostic parameters will be discussed, followed by a comprehensive discussion on the best way to manage these patients.
Introduction
Classically, asthma is thought to be a disease associated with childhood, while COPD is more commonly seen in older adults. The differences extend beyond just an age range: Asthma typically has reversibility in symptoms, while the symptoms of COPD tend to persist. However, one important feature that the illnesses share is that they can present with exacerbations.
Despite best efforts, patients with asthma and COPD will experience some exacerbations in their lifetime. A recent study concluded that 12.5% of asthma patients in the United States will experience at least one exacerbation in a 12-month period, and 2.5% will experience two or more exacerbations in that same period.1 Estimates surrounding exacerbations of COPD are considerably higher: 44.3% experienced at least one exacerbation in a 24-month period, and 26.3% experienced at least two episodes in that period.2 These percentages indicate that there is a high number of exacerbations of airway disease.
Epidemiology
There is no doubt that the burden of these two diseases combined is staggering, both worldwide and in the United States. Worldwide, there are an estimated 262 million people with asthma.3 In the United States, about 25 million people have asthma, which represents about 7.1% of the population (8% of adults and 7% of children have the disease).4 There are more than 1.5 million emergency department (ED) visits each year because of new-onset or exacerbations of asthma, with more than 10% (176,000) of those visits resulting in an admission. Further, on average nearly 10 Americans each day die from this disease.5
The numbers for COPD are comparable. Worldwide, between 210 million and 600 million individuals have COPD. (There is a lot of uncertainty because many people are undiagnosed.) In the United States, there are 15 million COPD patients, making it the third leading cause of disease in this country.6 A study in 2015 examining self-reported ED visits by COPD patients older than 35 years of age found that more than 77% of these patients went to the ED for a COPD exacerbation in the past 12 months, and nearly 20% of those were admitted to the hospital for further management.7
These large numbers make it inevitable that ED physicians will treat patients with one of these diseases with high frequency, making the task of closing the gap between what practitioners are doing and what they should be doing even more important.
Etiology
Although asthma and COPD both are chronic diseases, the exacerbations seem to be most problematic. Understanding what causes patients to have these worsening episodes may help to decrease their frequency.
Asthma. The underlying etiology of asthma is multifactorial and hard to define. Genetics, maternal age and diet, maternal prenatal smoking history, and mode of birth (cesarean vs. vaginal delivery) all are thought to be risk factors for the disease.8
Respiratory infections, particularly rhinovirus, influenza, and human metapneumovirus, have long been associated with acute asthma exacerbations. A study published in 2017 showed a plausible link between the aforementioned viruses and asthma exacerbations, but, interestingly, failed to show any clinical evidence that they lead to an exacerbation.9 Another study from 2018 evaluated the relationship between human rhinovirus (hRV) and exacerbations of asthma in children.10 The authors concluded that hRV was not an independent risk factor for a severe exacerbation.
Another common risk factor for asthma exacerbations is allergens, particularly inhaled allergens from pet hair, dust mites, indoor mold, or outdoor plant allergens such as pollen.11 The most common risk factors for asthma exacerbations probably are irritants, including cigarette smoke, cannabis smoke, and outdoor pollution. Exposure to cigarette smoke, either through actively smoking or through secondhand exposure, is known to increase both the frequency and the severity of asthma exacerbations.12,13 Exercise, once thought to worsen asthma exacerbations, now is known to decrease the inflammation associated with episodes if the disease is well controlled in the individual. A Brazilian study from 2015 followed 58 patients, divided into an exercise group and a control group, for three months and collected data on inflammatory marker levels and clinical symptoms.14 The results demonstrated that aerobic exercise decreases levels of inflammatory cytokines and improves the quality of life of patients with severe asthma exacerbations. Finally, there are several medications that can increase the likelihood of an exacerbation. The most common of these include aspirin and nonsteroidal anti-inflammatory drugs.
COPD. Risk factors for COPD overlap those for asthma to some degree. Smoking is the greatest risk factor for the development of COPD and the recurrence of exacerbations, as determined by a longitudinal study from Copenhagen.15 Other factors, such as increased airway responsiveness, environmental exposures, and atopy, also increase the occurrence of COPD. Interestingly, having childhood asthma also is associated with COPD in adulthood. Lastly, there are molecular risk factors for COPD. Some of these risk factors include gene polymorphisms, such as transforming growth factor (TGF) beta 1, antioxidant-related enzymes such as glutathione S-transferases, or excess elastase. A detailed discussion of these risk factors is beyond the scope of this report.
Pathophysiology
The pathophysiology of asthma and COPD are somewhat different.
Asthma. There are two parallel schools of thought regarding asthma. The first focuses on airway inflammation and the second deals with epithelial cell remodeling of the airway.
The airway inflammation model is very similar to the response from a severe allergic reaction. There is an early phase involving mast cells and immunoglobulin E (IgE) antibodies and a late phase several hours later involving more innate immune cells.16 In the early phase, there is nearly immediate smooth muscle-mediated bronchoconstriction; the late phase involves recruitment of eosinophils, neutrophils, and other pro-inflammatory cells to the bronchioles.
The second model, called the epithelial-mesenchymal contribution model, involves a structural remodeling scenario. It is believed that structural cells, such as epithelial cells and smooth muscle, release cytokines that cause remodeling of the airway.17 This new architecture of the airway has a significantly increased subbasement thickness, directly contributing to the reduced airflow in the bronchioles. Both models ascribe to the contraction of airway smooth muscle as the underlying process that causes a deterioration in airflow.
COPD. There is no single pathologic process related to COPD because it is an umbrella term for multiple underlying diseases, including emphysema, chronic bronchitis, and even asthma. Therefore, the pathology of the specific disease explains the pathology of COPD for a given patient. Chronic bronchitis, for example, is characterized by chronic inflammation with an increase in the number of neutrophils and lymphocytes. Alternatively, emphysema is a disease of the lung parenchyma destruction resulting in respiratory bronchioles and alveoli permanently dilated and a loss of alveolar surface area.
Clinical Features
The overlap in clinical presentations of asthma and COPD is not surprising: Both diseases involve poorly functioning airways. In fact, asthma-COPD overlap is a suitable diagnosis when symptoms of both diseases are present. In most cases, there are enough subtle differences in symptomology that the entities are distinguishable.
Asthma. Asthma is commonly characterized by cough and wheezing. Patients, especially children, typically present with either a nocturnal cough or a persistent dry cough that lasts several weeks. One study indicates that the most likely etiology of persistent cough is asthma.18 Wheezing, the second most common symptom associated with asthma, can be thought of as a marker of severity of a given exacerbation. A patient with milder symptoms exhibits only an expiratory wheeze that is present only when the patient exhales. As the symptoms become more intense, the wheezing begins to be heard even as the patient inhales (inspiratory wheezing). Eventually, as the symptoms worsen, wheezing is heard without a stethoscope throughout the entire breath.
In asthma, the most common chief complaint is a cough and/or shortness of breath, whether for an initial diagnosis or an exacerbation. Other presenting symptoms of asthma include breathlessness, inability to talk in full sentences, and varying levels of mental alertness. The degree of breathlessness is on a spectrum from only occurring during heavy exertion (mild end of the spectrum) to occurring at rest (severe). Likewise, the inability to talk also is on a continuum, from being able to speak in full sentences to only being able to speak one-syllable words. The progression of mental alertness during an asthma exacerbation follows this course: As the severity of the attack increases, so does agitation and restlessness; this trend continues until the patient is so hypoxic that they become drowsy or stuporous. Signs that the typical patient exhibits are respiratory distress, tachypnea, often with accessory muscle use, tachycardia, and hypoxemia with or without cyanosis. Again, the degree of abnormality of these indicators depends on the episode severity. When evaluating an individual patient, it is important that the provider determine the following: previous doctor or ED visits, previous hospitalizations, history of endotracheal intubations for asthma, and medications being used.19
COPD. As mentioned, the symptoms of COPD seem to overlap those of asthma, as shown in Figure 1.
Figure 1. Symptom Overlap for Asthma and Chronic Obstructive Pulmonary Disease |
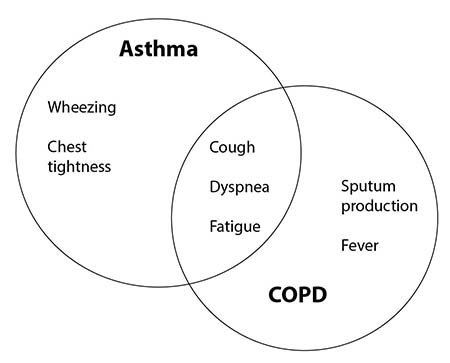 |
In fact, the three most common presenting symptoms of COPD are dyspnea, cough, and sputum production. Where the disease symptomology differs is with wheezing and chest tightness, which typically are less common in COPD.20 Commonly, patients will present with symptoms of fatigue, unaware that the underlying cause is dyspnea on exertion. This happens more often in less active patients in whom the dyspnea becomes progressively more severe over time. It also is common for patients to present with a chronic cough productive of green sputum. This cough typically is more intense in the morning and resolves throughout the day. Patients also can present with a constellation of the symptoms mentioned earlier, with dyspnea plus cough plus breathlessness plus wheezing, etc. With or without fever, securing a COPD diagnosis with such a presentation can be difficult, and the differential diagnosis list can be quite long.
Asthma-COPD Overlap (ACO) Syndrome. ACO is a rather complicated subject and will be discussed briefly here. It is identified in the literature as a syndrome with restricted airflow that shares many typical features of both asthma and COPD. The pathophysiology is multifaceted. Some patients with this condition may have had asthma and began smoking and, thus, became progressively short of breath and developed COPD over time. Alternatively, other patients may have underlying COPD and then developed hypersensitivity to an allergen and developed asthma. ACO is a condition that seems to have features of both asthma and COPD, yet there still are many unanswered questions regarding the exact etiology and diagnosis of the condition.21
Diagnostic Studies
Asthma. The diagnosis of asthma requires the presence of typical symptoms, such as cough and wheezing, and abnormal pulmonary tests. The second component of the diagnosis also has two subparts: abnormal expiratory flow of air and variability in airway function.
Determining whether the expiratory airflow is normal or limited is best done with spirometry.22 Spirometry is commonly known to test the ratio of the forced expiratory volume in one second (FEV1) to the forced vital capacity (FVC), known as the FEV1/FVC. Values less than 0.70 in adults and less than 0.90 in children are indicative of obstructive lung disease. Older studies have shown that the greater the variability of the test results (if multiple tests are performed), the stronger the indication that asthma is the etiology.
Once it has been established that a patient has obstructive lung disease, it is necessary to establish that the disease in question is asthma. This can be done in one of several ways. The most common way is with bronchodilation treatment. The patient is treated with a bronchodilator, such as albuterol, and the spirometry is performed again. The diagnosis of asthma is confirmed if the patient has an increase in FEV1 of greater than 12% or 200 mL.
Another common way of being fairly confident of an asthma diagnosis is with provocative testing. This test involves treating the patient with a known bronchoconstrictor, such as methacholine or histamine, and determining the extent of the drop in FEV1. A drop of greater than 20% is diagnostic. This diagnostic pathway is outlined in Figure 2.
Figure 2. Asthma Diagnosis |
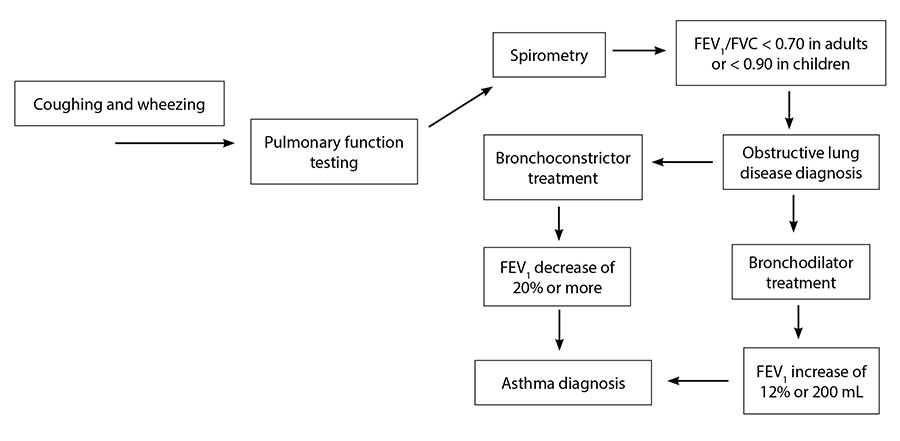 |
Other confirmatory tests include an anti-inflammatory treatment test (Does the FEV1 improve after four weeks of anti-inflammatory medications?) and exercise challenge testing (Does exercising lead to a significant drop in FEV1?). It should be noted that there are several populations in which diagnosing asthma is somewhat difficult. These include older adults, obese patients, and those with any smoking history.
COPD. As in asthma, the diagnosis of COPD depends on spirometry. The first step is to determine if the patient has an obstructive condition. This is defined as an FEV1/FVC fraction of less than 0.70. Next, the patient is treated with a bronchodilator, such as albuterol (0.4 mg is the standard dose), and the FEV1 ratio is measured a second time. If the new value still is less than 0.70, COPD can be diagnosed. The Global Initiative for Chronic Obstructive Lung Disease (GOLD) further classifies the severity of COPD based on the percent predicted FEV1 value (predictions are based on the individual’s age, sex, and height).23
Differential Diagnosis
Asthma. Considering alternative diagnoses for a patient diagnosed with asthma may be necessary, especially for pediatric patients who are not responding well to traditional asthma treatments. This differential diagnosis list should include all conditions with asthma-like symptoms (note, this could be extensive). This section will discuss when it is appropriate to consider other possible diagnoses.
It was mentioned earlier that persistent cough is highly associated with asthma. However, there are other etiologies that should be considered in patients with a chronic cough who are not responding to traditional asthma therapies.24 If a patient has a long-term cough that is associated with frequent upper respiratory infections, then cystic fibrosis should be considered, particularly if the symptoms were present since birth. Other possible diagnoses include a ciliary dyskinesia or an immunodeficiency.
If the patient has a wet cough and seemingly responds well to antibiotics, then chronic bacterial bronchitis is a consideration. Alternatively, if there are gastro-enteral-esophageal symptoms alongside a chronic cough, then there should be a concern for aspiration or swallowing issues. An inspiratory stridor with the cough would suggest a tracheal or laryngeal disorder, such as croup. It should be noted that some conditions, particularly ciliary disorders, lead to childhood asthma, yet it still is important to not miss the underlying cause. A persistent cough with a postnasal drip would suggest seasonal allergies. Lastly, a chronic cough associated with a sore throat and acid reflux indicates gastroesophageal reflux disease (GERD). Figure 3 shows which conditions should be added to the differential diagnosis based on other symptoms that are present.
Figure 3. Asthma Differential Diagnosis |
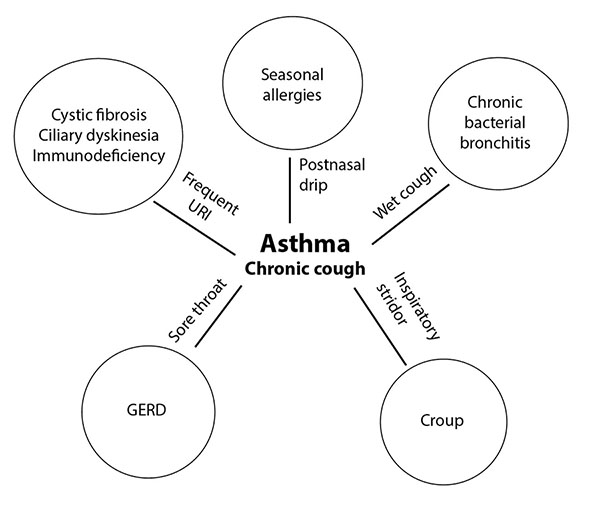 |
GERD: gastroesophageal reflux disease; URI: upper respiratory infection |
COPD. It also is important to consider the differential diagnosis for COPD because COPD can mimic other diseases. Probably the most commonly missed diagnosis is heart failure.25 This condition must be considered whenever a patient presents with dyspnea, chest tightness, and wheezing — symptoms that look very much like COPD. As in COPD, airflow also may be limited in heart failure (albeit in a more restrictive pattern as opposed to obstructive). However, heart failure will have certain symptoms that are not seen in COPD, such as lower extremity edema and crackles on lung auscultation, but both conditions can appear similar.
Tuberculosis is another condition that can mimic COPD. In fact, one study showed that more than 30% of tuberculosis patients have airflow obstruction. Bronchiectasis also should be suspected when a patient has a condition with exacerbations associated with dyspnea and productive cough. In this case, a computed tomography (CT) scan will show bronchial wall thickening and dilation of the airway lumen, which ultimately differentiates it from COPD.26
An important mimic of COPD and, more importantly, COPD exacerbation, is pneumothorax. Patients typically present with hypoxia and sudden-onset unilateral chest pain. Even a small pneumothorax can lead to significant symptoms. Therefore, the chest X-ray should be checked on patients with a COPD exacerbation.
Lastly, pulmonary embolism (PE) should be considered for all patients with persistent hypoxia, especially if it is associated with tachycardia and pleuritic chest pain. There has been extensive research recently on the prevalence of PE in patients with a COPD exacerbation. In a meta-analysis involving 17 studies and more than 3,000 patients to determine the prevalence of PE in such patients, investigators found that, while the aggregate percentage of COPD patients with PEs was 17%, there was significant variability among the patient groups.27 Another study from 2021 found the prevalence of PE to be closer to 12% and found that the prevalence varied based on how the PE was worked up (when the CT scan was performed).28
A third study examined the utility of a D-dimer level in COPD patients for detecting PE.29 This study found that while D-dimer alone was not useful in detecting PE in patients with COPD exacerbations, when combined with Wells criteria, PE could be detected reliably, with a sensitivity and specificity of 48% and 88%, respectively. Figure 4 illustrates appropriate differential diagnoses to consider for COPD.
Figure 4. Chronic Obstructive Pulmonary Disease Differential Diagnosis |
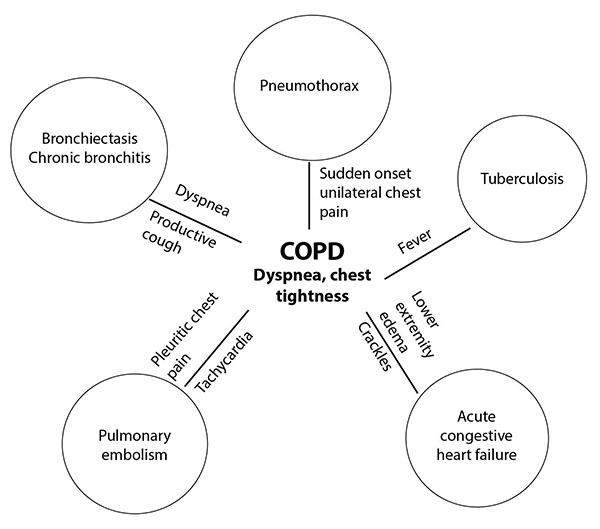 |
COPD: chronic obstructive pulmonary disease |
Management
Asthma. Acute severe asthma can be managed at home or in a medical care setting (either a primary care provider’s office or the ED). Appropriate at-home management of an exacerbation, also referred to as a written asthma action plan, can reduce the risk of a mild exacerbation becoming severe by as much as two-thirds.30 These written asthma action plans include instructions for when patients should adjust their medication doses based on new symptoms. They also include directives on when the patient should return to their primary care provider or report to the ED.
Most patients receive a prescription for either an inhaled short-acting beta-agonist (SABA) or an inhaled corticosteroid (ICS) plus a long-acting beta-agonist (LABA) for as-needed relief of symptoms, with the SABA option being more common.31 Despite the SABA option being more common, current guidelines recommend patients increase doses of ICS + LABA when they develop worsening symptoms. Patients are advised to double, or even quadruple, their doses of this medication combination, if needed. The maximum dose advised is 72 mcg of budesonide-formoterol or 48 mcg of beclometasone-formoterol in a 24-hour period. This strategy of significantly increasing doses of ICS + LABA has been shown to be more effective than increasing doses of SABAs in preventing an exacerbation from requiring hospitalization. Further guidance for managing exacerbations at home include detailed instructions on when a patient should commence oral corticosteroids (most patients will have a supply on hand).
The typical criteria for a patient to begin oral corticosteroids (OCS) are if they satisfy any of the following: not responding to an increase in either SABA or ICS + LABA dosing as described earlier for three days; rapid deterioration; or a history of severe exacerbations. Meeting any of these would prompt the patient to begin a short course of OCS, usually 40 mg to 50 mg per day for about a week. After that, the patient should see their prescribing doctor in two weeks for follow-up. If the patient has trialed the written asthma action plan and has persistent symptoms, they must go to primary care or the ED.
In a lower-acuity setting, the initial treatment for a moderate to severe exacerbation includes repeat administration of a SABA. Currently, guidelines recommend that the mode of administration be a pressurized metered dose inhaler (pMDI) with a spacer. The dose is 4-10 puffs every 20 minutes for an hour. Additionally, an oral steroid, such as prednisolone 40 mg, should be added. Finally, the patient should be provided oxygen (O2) with a goal saturation of 93% to 95%.32 After one hour, the patient should be reassessed. If there is no improvement or only minimal improvement, the patient should be transferred to a setting that can provide a higher level of care (e.g., ED).
On arrival to the ED, a brief history and physical exam should be performed. The exam should look for signs of severe exacerbation, such as tachypnea or inability to talk in full sentences. In addition, the exam should evaluate for complications, such as anaphylaxis or a pneumothorax. Lastly, the exam should attempt to exclude other etiologies, such as heart failure or a foreign body. The need for intubation should be guided by the severity of the presentation, not a particular measured arterial blood gas (ABG). Common indicators for intubation include decreased level of consciousness, inability to speak more than one syllable, and rapidly worsening symptoms despite treatment. It should be noted that, once intubated, the patient will still require aggressive bronchodilator treatment and steroids. If there is no immediate indication for intubation, but the patient is having severe symptoms, the patient should be given supplemental oxygen through nasal cannula to sustain a saturation of 88% to 93%. When considering the need for ventilation, noninvasive ventilation is superior to invasive ventilation. The decision to initiate invasive methods (i.e., intubation) must be based on the patient’s wishes and the reversibility of the underlying cause.
The most recent study investigating the usefulness of noninvasive ventilation (NIV) is from 2017.33 Osadnik et al compiled 17 randomized controlled trials and compared treatment of COPD exacerbation with NIV plus usual therapies to just the usual therapies. They found that adding NIV decreased the risk of mortality by 46% and, more encouraging, decreased the need for intubation by 65%. Other studies investigating this topic are at least a decade old. Based on the existing research, old and new, the indications for placing a patient on NIV are fairly intuitive: the patient has respiratory acidosis defined as a pH < 7.35 and PaCO2 > 45, the patient has severe dyspnea on nasal cannula and exhibits signs of increased work of breathing with effort that is not sustainable, or the patient has a persistent inability to adequately oxygenate. If any one of those is present, NIV has been shown to have substantial benefit in the patient’s outcome.
Once the exam is complete and the patient does not need acute airway support, some pieces of objective data need to be collected to properly manage the patient. If possible, before treatment is started, a PEF or FEV1 should be measured. Lung function should continue to be measured at intervals through the stay in the ED to ensure improvement. Oxygen saturation ideally should be measured with pulse oximetry before oxygen therapy is started. ABG measurements are only recommended for patients with an initial FEV1 of less than 50% of predicted or for those who are not improving. Routine ABGs are not indicated. Likewise, chest X-rays typically are not indicated unless the patient is not responding to treatment or there is concern for a complicating etiology.
Guidelines indicate that treatment in the ED is very similar to treatment at a primary care setting. Initially the patient should be provided oxygen via a nasal cannula or, if this mode is not sufficient, with a nonrebreather mask. It is not recommended to use high-flow nasal cannula unless absolutely necessary. Oxygen still can be provided to the patient even if there is not continuous pulse oximetry available.
The initial pharmacological intervention is an inhaled SABA, with dosing repeated until symptoms improve. The literature indicates that the most efficient mode of administration of the SABA is with a pMDI. A study by Colacone et al showed that albuterol given via a pMDI is equally effective and just as safe as wet nebulized albuterol in promoting bronchodilation.34 A second study by Burger at al from 2021 indicated that providing nebulized albuterol contributed to significantly more muscle weakness in pediatric patients compared with patients who took albuterol with a pMDI.35 Currently there is limited research comparing the use of continuous nebulizers to intermittent nebulizers, and most of the studies were published decades ago.
Intravenous (IV) beta-agonist administration is not routinely recommended for patients. Additionally, intramuscular epinephrine is indicated only for patients with anaphylaxis but is not widely used in situations where there is no anaphylaxis.
The criteria for adding systemic corticosteroids in the ED are slightly different than the criteria for adding them in the primary care setting. In the ED, systemic steroids should be added to virtually all exacerbations.36,37 Patients who meet any of the following criteria especially will need steroid therapy:
• if the SABA treatment does not provide lasting improvement in symptoms;
• if the current exacerbation occurred while the patient was already on a course of steroids; or
• if the patient has previously required corticosteroids during an exacerbation.
The mode of corticosteroid administration is largely at the discretion of the physician. Research indicates that oral steroids are as effective as intravenous steroids. The oral route should be avoided when the patient’s respiratory status prevents the ability to safely swallow, if the patient has an altered mental state, or if the patient is vomiting. Prednisone is the most common steroid for asthma exacerbations, and the most studied daily dose is 0.5 mg/kg.38 The most effective duration of steroid treatment was believed to be 10-14 days; however, more recent studies have shown that a course half as long (five to seven days) is equally efficacious. This shorter course may avoid the need for a steroid taper.
It is worthwhile to discuss the utility of ICS. Current guidelines state that if patients are not taking systemic steroids at the time of the exacerbation, then ICS given within an hour of presentation can reduce the risk of hospitalization.39 However, if the patient is taking steroids, the usefulness of ICS is unclear. (Note, in children, the evidence suggests that both systemic steroids and ICS are beneficial.) A recent Norwegian study argued that inhaled steroids are not necessarily helpful for patients having exacerbations, especially if they are already using ICS at home.40 Specifically, the authors argue that there are no studies to support the British guidelines recommending dose doubling of ICS for patients experiencing an acuity in symptoms. In fact, the authors cite several studies showing no benefit to increased doses of ICS in the emergent setting. In summary, the Global Initiative on Asthma (GINA) is somewhat vague about using ICS in the ED, so it is left up to the physician’s discretion.32
Albuterol probably is the most commonly administered medicine in the treatment of acute asthma exacerbation. Yet, evidence demonstrates albuterol can be more effective in terms of improving lung function as well as reducing hospitalizations if it is given with ipratropium bromide, an anticholinergic that often is nebulized.41 Interestingly, there does not seem to be a benefit from ipratropium bromide once the patient is admitted, particularly in children.
Magnesium is another medication that should be considered for patients with worsening asthma. The indication for adding magnesium sulfate in the ED for an acutely ill patient is if they fail to improve with traditional treatment and have persistent hypoxemia. In some patients, the literature hints that adding 2 g of IV magnesium sulfate has been shown to reduce the need for admission, yet in mild to moderate asthma exacerbations, adding this medication has been shown to be as beneficial as a placebo. Note, this does not apply to severe exacerbations, wherein adding magnesium has been shown to be more beneficial than a placebo.42 The evidence also suggests that the mode of administration may be important: nebulized magnesium sulfate is less efficacious than the IV formulation, although the data on that are nearly a decade old. The mechanism for how magnesium sulfate works to improve airway function is unclear, yet there are several proposed mechanisms, such as directly relaxing smooth muscle or having some anti-inflammatory effect. Figure 5 illustrates these interventions.
Figure 5. Management of Asthma Exacerbation at Home and in the Emergent Setting |
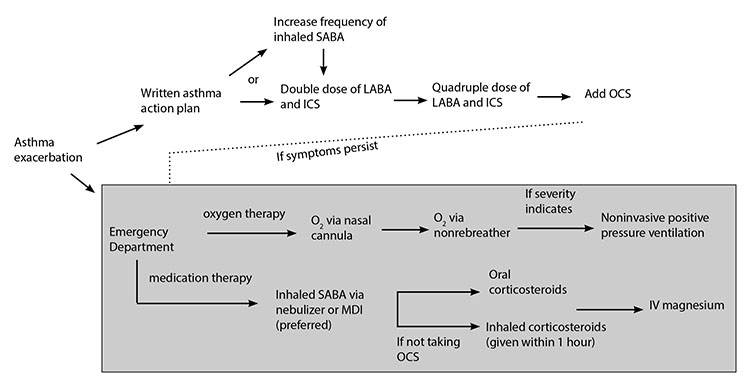 |
SABA: short-acting beta-agonist; LABA: long-acting beta-agonist; ICS: inhaled coritcosteroid; OCS: oral corticosteroid; O2: oxygen; MDI: metered dose inhaler; IV: intravenous |
Phosphodiesterase inhibitors, such as aminophylline and theophylline, are not recommended because of their safety profile in the setting of SABAs and anticholinergic drugs. Aminophylline, when given IV, can have very serious side effects and has not been shown to improve patient outcomes.43 Despite its limited effectiveness, it still is an approved treatment in Japanese guidelines.44
Leukotriene receptor antagonists (LTRA) are another class of medications that have almost no utility in asthma exacerbations, and there is only a small amount evidence indicating they are helpful at all. LTRAs are not generally advised for exacerbations.
Helium oxygen therapy, commonly referred to as Heliox, is not standard of care for most acute exacerbations. There may be some benefit in severe cases, yet its availability tends to be limited in EDs and, thus, it typically is not used.
COPD. Management of COPD in the ED depends on the severity of the exacerbation and whether the exacerbation can be managed on an outpatient or inpatient basis. The goal of managing these episodes is to lessen the impact of the exacerbation and to prevent poor downstream effects and outcomes.45 The general approach to controlling exacerbations includes:
• administration of bronchodilators and other medications;
• possible invasive or noninvasive mechanical ventilation; and
• treatment of underlying medical condition.
The three main medication classes are bronchodilators, steroids, and antibiotics. As in asthma exacerbations, the most commonly ordered bronchodilator for a COPD exacerbation is a short-acting beta-agonist, such as albuterol. Interestingly, although there is a paucity of evidence supporting this treatment, it is the recommended first-line medication. Beta-agonists may or may not be paired with an anticholinergic agent, such as ipratropium. The delivery route of this medicine seems to have little effect on the improvement in FEV1 between before and after treatment. The delivery method usually is either with an MDI or, more typically, with a nebulizer. Recommendations state that if the medication is nebulized, it should be air-driven and not oxygen-driven because of the concern for suppressing the respiratory drive and causing hypercapnia.
Data supporting the use of corticosteroids in COPD exacerbation are roughly 20 years old, yet, despite the lack of recent data, use of this medication still is supported by the guidelines. It is commonly accepted that corticosteroids shorten recovery time, improve FEV1, and improve oxygenation. Further, the data suggest that steroids, when used appropriately, decrease the risk of treatment and decrease the length of indicated hospitalization.45 Recommendations regarding the dose and course of corticosteroids seem to be ever evolving, with shorter courses becoming more standard.
A Danish study from 2019 investigated the outcomes for COPD exacerbation with a five-day course of prednisone compared to a 10-day course.46 More than 10,000 patients were included in this study, and the primary outcomes were development of pneumonia after the exacerbation and mortality after the exacerbation. The results showed that the patients receiving a 10-day course of steroids had higher rates of pneumonia and all-cause mortality than the patients receiving the shorter course within 12 months of the exacerbation. This study was largely responsible for the current guidelines recommending a five-day course of 40 mg of prednisone. Note, no taper is required with this regimen. In the ED, there is no benefit to providing IV corticosteroids. Steroids should be given orally unless the patient cannot tolerate anything by mouth because of mental status changes, severe tachypnea, or vomiting.
The efficacy of antibiotics during a COPD exacerbation remains to be determined, since there are multiple conflicting reports. However, when there are clinical signs of a concurrent bacterial pneumonia, the data are clearer regarding the benefit of antibiotics. There is even some evidence that sputum color may be highly sensitive for detecting an associated bacterial pneumonia.47 A systematic review from more than a decade ago revealed that antibiotics can reduce the length of hospitalization and reduce sputum production.48 Although this is an older study, it supports the use of antibiotics for severely ill patients; no more-recent studies support this.
There have been some studies suggesting the use of a positive procalcitonin level as a prompt to initiate antibiotics. The data merely suggest that, while this method works to reduce antibiotic use, it has little effect on outcome measures, such as length of hospitalization and mortality. The most comprehensive guidelines suggest using antibiotics only if the patient has all of the following: dyspnea, increased sputum production, and purulent sputum, or if they require invasive or noninvasive ventilation (the data supporting this are more than five years old).
The choice of antibiotic has not been studied recently, but older studies suggest that the chosen antibiotic depends on the frequency of exacerbations for a particular patient.49 If the patient tends to have less frequent exacerbations, then a macrolide or a penicillin would be appropriate. However, if the patient has more frequent episodes or requires intubation during their exacerbations, then coverage for Pseudomonas would be appropriate, usually with piperacillin-tazobactam.
Finally, the underlying cause should be treated. This may involve providing antibiotics for a pneumonia, diuresing a patient with a congestive heart failure exacerbation, or removing irritants to which the patient may have been exposed. This arm of management often is beyond the scope of the ED and is best managed on hospital admission. The three arms of COPD management in the ED are illustrated in Figure 6.
Figure 6. Management of Chronic Obstructive Pulmonary Disease in the Emergent Setting |
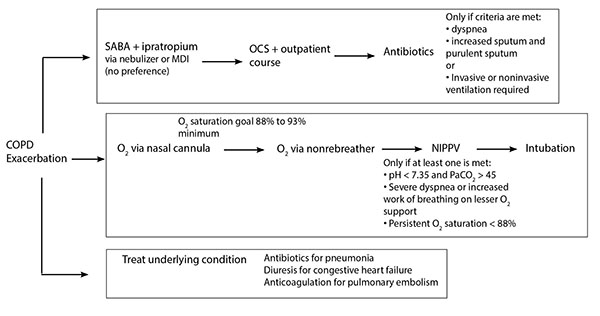 |
OCS: oral corticosteroids; COPD: chronic obstructive pulmonary disease; SABA: short-acting beta-agonist; NIPPV: noninvasive positive pressure ventilation; ICS: inhaled corticosteroid: O2: oxygen; MDI: metered dose inhaler |
Practice Gaps
It is important to note that, while the guidelines are up to date regarding best practices, much of the evidence supporting the guidelines is more than five years old. This suggests the need for new research that investigates the efficacy of some of the more controversial aspects of treatment, such as corticosteroids or antibiotics.
Summary
This article has explained that the burden of disease of asthma and COPD are extensive, both in the United States and across the globe. The risk factors for asthma seem to be more complicated and less understood than the risk factors for COPD, for which long-term smoking is the main risk factor. Diagnosing either condition depends on a high degree of suspicion coupled with spirometry measurements. Although both diseases commonly present to the emergent setting, it is necessary to keep the differential diagnosis broad so as not to miss other common etiologies of cough and dyspnea. Finally, asthma and COPD are two distinct entities that often have similar appearing exacerbations. The subtle differences in clinical presentation can make managing these diseases in the ED somewhat challenging. Further complicating treatment is the scarcity of recent research and data supporting conventional treatments recommended by current guidelines.
REFERENCES
- Suruki RY, Daugherty JB, Boudiaf N, et al. The frequency of asthma exacerbations and healthcare utilization in patients with asthma from the UK and USA. BMC Pulm Med 2017;17:74.
- Dhamane AD, Moretz C, Zhou Y, et al. COPD exacerbation frequency and its association with health care resource utilization and costs. Int J Chron Obstruct Pulmon Dis 2015;10:2609-2618.
- World Health Organization. https://www.who.int/news-room/fact-sheets/detail/asthma
- Centers for Disease Control and Prevention. National Center for Health Statistics. 2019 National Health Interview Survey. U.S. Department of Health & Human Services. https://www.cdc.gov/nchs/nhis/index.htm
- National Center for Health Statistics. National Hospital Ambulatory Medical Care Survey (2010-2018). U.S. Department of Health & Human Services, Centers for Disease Control and Prevention. https://www.cdc.gov/nchs/ahcd/index.htm
- Centers for Disase Control and Prevention. Chronic obstructive pulmonary disease among adults — United States, 2011. MMWR Morb Mortal Wkly Rep 2012;61:938-943.
- Kumbhare SD, Beiko T, Wilcox SR, Strange C. Characteristics of COPD patients using United States emergency care or hospitalization. Chronic Obstr Pulm Dis 2016;3:539-548.
- Martinez FD, Wright AL, Holberg CJ, et al. Maternal age as a risk factor for wheezing lower respiratory illnesses in the first year of life. Am J Epidemiol 1992;136:1258-1268.
- Rudd PA, Thomas BJ, Zaid A, et al. Role of human metapneumovirus and respiratory syncytial virus in asthma exacerbations: Where are we now? Clin Sci 2017;131:1713-721.
- Lambert KA, Prendergast LA, Dharmage SC, et al. The role of human rhinovirus (HRV) species on asthma exacerbation severity in children and adolescents.J Asthma 2018;55:596-602.
- National Asthma Education and Prevention Program: Expert panel report III: Guidelines for the diagnosis and management of asthma. National Heart, Lung, and Blood Institute, 2007. (NIH publication no. 08-4051) www.nhlbi.nih.gov/guidelines/asthma/asthgdln.htm
- Siroux V, Pin I, Oryszczyn MP, et al. Relationships of active smoking to asthma and asthma severity in the EGEA study. Epidemiological study on the Genetics and Environment of Asthma. Eur Respir J 2000;15:470-477.
- Morkjaroenpong V, Rand CS, Butz AM, et al. Environmental tobacco smoke exposure and nocturnal symptoms among inner-city children with asthma. J Allergy Clin Immunol 2002;110:147-153.
- França-Pinto A, Mendes FA, de Carvalho-Pinto RM, et al. Aerobic training decreases bronchial hyperresponsiveness and systemic inflammation in patients with moderate or severe asthma: A randomised controlled trial. Thorax 2015;70:732-739.
- Løkke A, Lange P, Scharling H, et al. Developing COPD: A 25 year follow up study of the general population. Thorax 2006;61:935-939.
- Liu MC, Hubbard WC, Proud D, et al. Immediate and late inflammatory responses to ragweed antigen challenge of the peripheral airways in allergic asthmatics. Cellular, mediator, and permeability changes. Am Rev Respir Dis 1991;144:51-58.
- Knight DA, Lane CL, Stick SM. Does aberrant activation of the epithelial-mesenchymal trophic unit play a key role in asthma or is it an unimportant sideshow? Curr Opin Pharmacol 2004;4:251-256.
- Johnson D, Osborn LM. Cough variant asthma: A review of the clinical literature. J Asthma 1991;28:85-90.
- Delbridge, T, Domeier R, Key CB. Prehospital asthma management. Prehosp Emerg Care 2003;7:42-47.
- Vogelmeier CF, Román-Rodríguez M, Singh D, et al. Goals of COPD treatment: Focus on symptoms and exacerbations. Respir Med 2020;166:105938.
- Hikichi M, Hashimoto S, Gon Y. Asthma and COPD overlap pathophysiology of ACO. Allergol Int 2018;67:179-186.
- Rothe T, Spagnolo P, Bridevaux P, et al. Diagnosis and management of asthma — The Swiss guidelines. Respiration 2018;95:364-380.
- Duffy SP, Criner GJ. Chronic obstructive pulmonary disease: Evaluation and management. Med Clin North Am 2019;103:453-461.
- Ullmann N, Mirra V, Di Marco A, et al. Asthma: Differential diagnosis and comorbidities. Front Pediatr 2018;6:276.
- Güder G, Störk S. COPD and heart failure: Differential diagnosis and comorbidity. Herz 2019;44:502-508.
- Martin C, Regard L, Chassagnon G, Burgel P-R. Diagnostic étiologique d’une dilatation des bronches [Bronchiectasis in adults: Etiological diagnosis]. [Article in French]. Rev Pneumol Clin 2018;74: 292-298.
- Fu X, Zhong Y, Xu W, et al. The prevalence and clinical features of pulmonary embolism in patients with AE-COPD: A meta-analysis and systematic review. PLoS One 2021;16:e0256480.
- Wang J, Ding YM. Prevalence and risk factors of pulmonary embolism in acute exacerbation of chronic obstructive pulmonary disease and its impact on outcomes: A systematic review and meta-analysis. Eur Rev Med Pharmacol Sci 2021;25:2604-2616.
- Sadeghi S, Emami Ardestani M, Raofi E, Esfandabadi AJ. Diagnostic value of D-dimer in detecting pulmonary embolism in patients with acute COPD exacerbation. Tanaffos 2020;19:371-379.
- O’Byrne PM, FitzGerald JM, Bateman ED, et al. Inhaled combined budesonide-formoterol as needed in mild asthma. N Engl J Med 2018;378:1865-1876.
- Bateman ED, Reddel HK, O’Byrne PM, et al. As-needed budesonide-formoterol versus maintenance budesonide in mild asthma. N Engl J Med 2018;378:1877-1887.
- Global Initiative for Asthma. 2021 GINA Report, Global Strategy for Asthma Management and Prevention. https://ginasthma.org/gina-reports/
- Osadnik CR, Tee VS, Carson-Chahhoud KV, et al. Non-invasive ventilation for the management of acute hypercapnic respiratory failure due to exacerbation of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2017;7:CD004104.
- Colacone A, Afilalo M, Wolkove N, Kreisman H. A comparison of albuterol administered by metered dose inhaler (and holding chamber) or wet nebulizer in acute asthma. Chest 1993;104:835-841.
- Burger C, Vendiola DF, Arnold DH. Nebulized albuterol delivery is associated with decreased skeletal muscle strength in comparison with metered-dose inhaler delivery among children with acute asthma exacerbations. J Am College Emerg Phys Open 2021;2:e12422:
- Littenberg B, Gluck EH. A controlled trial of methylprednisolone in the emergency treatment of acute asthma. N Engl J Med 1986;314:150-152.
- Schneider SM, Pipher A, Britton HL, et al. High-dose methylprednisolone as initial therapy in patients with acute bronchospasm. J Asthma 1988;25:189-193.
- Reddel HK, Barnes DJ, Exacerbation Advisory Panel. Pharmacological strategies for self-management of asthma exacerbations. Eur Respir J 2006;28:182-199.
- Edmonds ML, Camargo CA Jr, Pollack CV Jr, Rowe BH. Early use of inhaled corticosteroids in the emergency department treatment of acute asthma. Cochrane Database Syst Rev 2003;3:CD002308.
- Grønseth IM, Nag T, Roland PH. [No increase in inhaled corticosteroids in asthma exacerbation]. [Article in Norwegian]. Tidsskr Nor Laegeforen 2019;139. doi: 10.4045/tidsskr.18.0537.
- Agnihotri NT, Saltoun C. Acute severe asthma (status asthmaticus). Allergy Asthma Proc 2019;40:406-409.
- Conway J, Friedman B. Intravenous magnesium sulfate for acute asthma exacerbation in adults. Acad Emerg Med 2020;27:1061-1063.
- Nair P, Milan SJ, Rowe BH. Addition of intravenous aminophylline to inhaled beta(2)-agonists in adults with acute asthma. Cochrane Database Syst Rev 2012;12:CD002742.
- Nakamura Y, Tamaoki J, Nagase H, et al. Japanese guidelines for adult asthma 2020. Allergol Int 2020;69:519-548.
- Viniol C, Vogelmeier CF. Exacerbations of COPD. Eur Respir Rev 2018;27:170103.
- Sivapalan, P, Ingebrigtsen TS, Rasmussen DB, et al. COPD exacerbations: The impact of long versus short courses of oral corticosteroids on mortality and pneumonia: Nationwide data on 67 000 patients with COPD followed for 12 months. BMJ Open Respir Res 2019;6:e000407.
- Stockley RA, O’Brien C, Pye A, Hill SL. Relationship of sputum color to nature and outpatient management of acute exacerbations of COPD. Chest 2000;117:1638-1645.
- Ram FS, Rodriguez-Roisin R, Granados-Navarrete A, et al. Antibiotics for exacerbations of chronic obstructive pulmonary disease. Cochrane Database Syst Rev 2006;(2):CD004403.
- Miravitlles M, Espinosa C, Fernández-Laso E, et al. Relationship between bacterial flora in sputum and functional impairment in patients with acute exacerbations of COPD. Study Group of Bacterial Infection in COPD. Chest 1999;116:40-46.
This article discusses emergent management of patients with asthma and chronic obstructive pulmonary disease exacerbations, as well as the epidemiology, etiology, and pathophysiology of each condition
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
