Is This Wellens’ Syndrome?
By Ken Grauer, MD
Professor Emeritus in Family Medicine, College of Medicine, University of Florida
The ECG in the figure below is from a young adult man known to have a bicuspid aortic valve. He presented to the ED following a presyncopal episode. The patient has not experienced chest pain recently. Does this patient have Wellens’ syndrome?
There is sinus arrhythmia at a fairly slow rate. The PR interval is a little short (0.11 to 0.12 seconds in duration), although this is not necessarily an abnormal finding for a young adult. QRS duration, the QTc interval, and the frontal plane axis all are normal.
QRS amplitude often is increased in younger adults. Voltage criteria for left ventricular hypertrophy probably are satisfied nonetheless, considering the tall R waves in leads II and V5, and especially considering the extremely deep anterior S waves (well over 20 mm in lead V2, and so deep that S waves are cut off in lead V3).
Deeper-than-usual Q waves are seen in each inferior lead, as well as in lateral chest lead V6 (with a tiny q wave in lead V5). In addition, there are prominent anterior forces (an R wave in lead V1 of ~9 mm, followed by a huge R wave of 24 mm in anterior lead V2). These two features should suggest the possibility of hypertrophic cardiomyopathy.
That said, the most remarkable ECG finding is anterior ST-segment coving with slight elevation, followed by a steep downsloping of the T wave (especially in lead V2) that ends in terminal T wave inversion. The ST-T wave picture in the anterior leads of this tracing resembles the changes seen with Wellens’ syndrome, in which there is a high-grade stenosis of the proximal left anterior descending coronary artery. Nevertheless, there are several clinical and ECG features in this case that suggest this patient does not have Wellens’ syndrome.
The patient is a younger adult; therefore, he is likely to be in a lower prevalence group for coronary disease. A history of recent chest pain that has resolved by the time the ECG is obtained is expected with Wellens’ syndrome, yet there was no history of chest pain in this case. The QTc interval is normal here, but, typically, it is prolonged with Wellens’ syndrome. There is early transition, with extremely prominent anterior R waves in this case, whereas there usually is loss of anterior forces with Wellens’ syndrome. Finally, there is markedly increased QRS amplitude, which often makes recognition of Wellens’ syndrome problematic.
Further evaluation of this patient suggested no underlying coronary disease. Echo ruled out chamber enlargement and hypertrophic cardiomyopathy. By exclusion, clinicians believed this patient was living with a repolarization variant, which can (especially in a young adult) produce the ECG pattern of increased voltage, early transition, and ST-T wave changes similar to those seen in the figure.
For more information about and further discussion of this case, please click here.
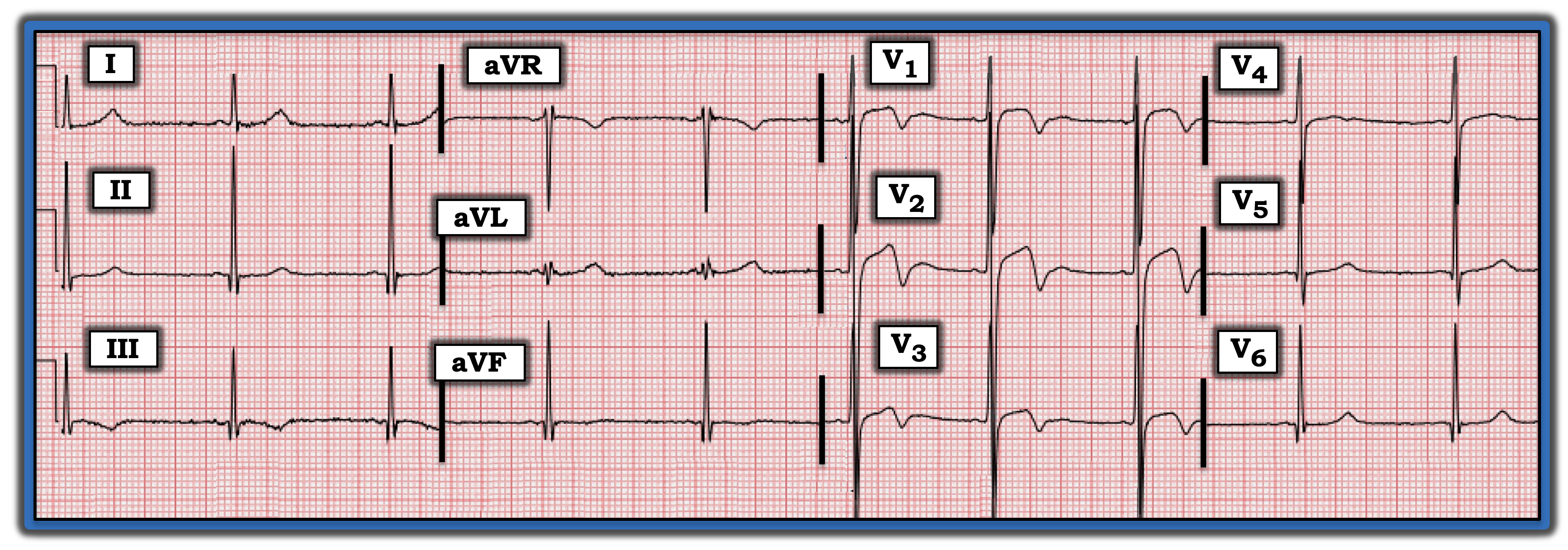
The ECG in the figure is from a young adult man known to have a bicuspid aortic valve. He presented to the ED following a presyncopal episode. The patient has not experienced chest pain recently. Does this patient have Wellens’ syndrome?
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
