Strangulation and Related Injuries
January 1, 2022
Reprints
AUTHORS
Caleb P. Canders, MD, Department of Emergency Medicine, UCLA Ronald Reagan Medical Center, Los Angeles, CA
Anna Nguyen, DO, Department of Emergency Medicine, UCLA Ronald Reagan Medical Center, Los Angeles, CA
Eugenie F. Como, MD, Department of Emergency Medicine, UCLA Ronald Reagan Medical Center, Los Angeles, CA
PEER REVIEWER
Catherine A. Marco, MD, FACEP, Professor, Emergency Medicine and Surgery, Wright State University, Dayton, OH
EXECUTIVE SUMMARY
- Strangulation is defined as external pressure to the neck that causes sustained impairment of air or blood flow.
- Obstruction of venous return is the main cause of death from strangulation.
- Victims of strangulation may not present until days or weeks after the event.
- In awake and alert patients, symptoms of potential serious strangulation injuries include reported loss of consciousness, voice changes, difficulty swallowing, facial petechiae, and ligature marks on the neck.
- Computed tomography angiography is the preferred imaging modality for patients with findings of serious strangulation events.
- Initial treatment of carotid artery dissection is with unfractionated heparin infusion with conversion to oral anticoagulants for six months.
- Strangulation has a strong association with intimate partner violence (IPV), so victims of IPV should be asked about strangulation events, and victims of strangulation should be asked about IPV.
Introduction
Strangulation accounts for approximately 1% of violent deaths in the United States.1 The prevalence of non-fatal strangulation, estimated to be 10% in all women and nearly 70% in women experiencing intimate partner violence, is increasing over time.2-4 Most survivors of strangulation do not seek medical care. Those who do present to the emergency department (ED) may not do so immediately or may be hesitant to disclose information. In addition, many survivors of strangulation are asymptomatic initially, and most do not have visible signs of injury.2,5,6 However, approximately 1% of strangulation survivors will have immediate or delayed-onset injuries, some of which are life-threatening.2,7 In addition, survivors of strangulation are more likely to eventually die by homicide.8 Therefore, it is important for emergency providers to be able to identify injuries associated with strangulation, to prevent its devastating sequelae, and to provide safety planning and resources.
Despite increasing recognition of strangulation as a traumatic injury with serious consequences, there is little evidence to guide the workup and management of survivors of strangulation who present to the ED. Some of the controversies that exist, such as the appropriate diagnostic imaging in survivors of strangulation and the optimal management of carotid artery dissections, will be reviewed in this paper. In addition, this article will briefly review some injuries related to strangulation that may be encountered by emergency providers.
Definitions
Strangulation is defined as the sustained impairment of air or blood flow through the neck caused by external pressure.9 Strangulation can result in asphyxia (any process that deprives the brain of oxygen) and should be distinguished from the layperson’s term “choking,” which medically refers to an internal airway obstruction.10 Strangulation can be categorized further by the mechanism of external neck compression. For example, manual strangulation, or “throttling,” occurs when an assailant uses a body part (usually his/her hands or knees) to apply direct pressure to the victim’s neck. It is the most common method of strangulation in intimate partner violence.6,11,12 Ligature strangulation, or “garroting,” involves the use of any cord-like object that is tightened around the victim’s neck. Some other forms of asphyxiation that will be reviewed include hanging, which refers to external compression of the neck caused by a person’s own weight, and mechanical asphyxia, which refers to restriction of lung expansion by external compression or the positioning of one’s own body.
Pathophysiology of Strangulation
External pressure applied to the neck induces pain, anxiety related to difficulty breathing, and rapid loss of consciousness, usually within 10 seconds.2 Incontinence of urine and feces typically occurs within 15 and 30 seconds, respectively.2,13 Four mechanisms have been proposed as possible causes of death from strangulation, which likely play variable roles that depend on the location, magnitude, and direction of force applied to the neck.2,14 (See Table 1.)
Table 1. Proposed Mechanisms of Death Caused by Strangulation |
|
Venous congestion: Obstruction of cerebral venous return, not airway occlusion, is the main cause of death in most fatal strangulations.15 Only 2 kg of external pressure is required to compress the jugular veins, which lie superficial in the neck.16 Occlusion of venous outflow from the brain results in cerebral congestion and loss of consciousness. The resulting decreased muscle tone ultimately leads to arterial compression and cerebral anoxia.
Arterial obstruction: Depending on the direction that the force is applied, 2-10 kg of external pressure is adequate to obstruct flow through the carotid arteries.16 Complete arterial occlusion of the carotid arteries results in rapid cerebral anoxia and death.2
Airway occlusion: Approximately 15 kg of external pressure is required to occlude the airway.16 Compared to venous congestion and arterial obstruction, airway obstruction takes longer to result in loss of consciousness and death and likely plays a minor role in most fatal strangulations.
Carotid sinus reflex: Continuous force applied directly to the carotid body in the sympathetic ganglion in the neck can lead to vagal stimulation, bradycardia, and subsequent cardiac arrest.17 Given that the force would need to be prolonged and bilateral, it likely plays little to no role in most fatal strangulations.12
ED Presentation Following Strangulation
Emergency providers may face challenges when assessing survivors of strangulation. Survivors of strangulation often present days to weeks after the incident, may be ashamed or afraid to disclose information, and may not recall details about the event because of loss of consciousness or concurrent substance use.2,18 If occurring in the context of intimate partner violence, it may be especially difficult to interview a survivor of strangulation if the assailant is present. However, emergency providers should take all reports of strangulation seriously, since asymptomatic patients and those without signs of trauma still can have life-threatening injuries.2
Initial Assessment
As with other traumatic injuries, emergency providers should first assess the airway, breathing, and circulation (i.e., “the ABCs”) in survivors of strangulation. A difficult airway should be anticipated in any person reporting neck trauma, although it is rare for strangulation to cause injuries that impede intubation.15 Spinal fractures and associated ligamentous injuries also are exceedingly rare following strangulation and, if a difficult airway is encountered, it may be necessary and acceptable to remove a patient’s cervical collar.15
Symptoms Following Strangulation
Less than half of survivors of strangulation who seek medical evaluation do so on the day of the incident, partly because many are asymptomatic initially.2,6,19 Neck pain is reported in 50% to 60% of survivors of strangulation.2,11,20 Survivors of strangulation often report voice changes, which may not be appreciable to the emergency provider and can be secondary to laryngeal injuries.11 Swallowing that is painful (odynophagia) or difficult (dysphagia) often develops weeks after a strangulation and can be secondary to soft tissue swelling, hematomas, or fractures of the hyoid bone or of the cricoid or thyroid cartilage.10 Painful tongue movement may indicate an injury to the epiglottis.21
Roughly 10% of survivors of strangulation report respiratory symptoms, which emergency providers may mistakenly attribute to hyperventilation or anxiety, but which also can be the result of aspiration, laryngeal injury, or postobstructive edema.2 Therefore, any complaint of neck pain, voice change, difficult/painful swallowing, or changes in breathing may signal impending airway compromise and should be investigated.15 In addition, loss of consciousness, reported in up to 40% of survivors of strangulation, is considered a sign of a potentially life-threatening strangulation.11,19,22-24
Association with Intimate Partner Violence
Strangulation often is an attempt of the assailant to exert control over, rather than kill, the victim, and more often occurs in the context of intimate partner violence than sexual assault.3,22,25 It also is a gendered crime; women are 13 times more likely to be strangled by an intimate partner than men, and an estimated 3% to 10% of women report having been strangled by an intimate partner.7,23,26 Female survivors of strangulation often report multiple prior strangulation events.23,27 With repeated episodes of strangulation, injuries typically escalate in severity, and respiratory and neurologic injuries are more common in women who have been strangled multiple times.6,28 Female survivors of strangulation are seven times more likely to be killed by an intimate partner.8 Therefore, emergency providers should ask specifically about strangulation in women who report or screen positive for intimate partner violence.29
Physical Findings
Half of survivors of strangulation lack visible injuries on initial examination, which may lead some emergency providers to discount their complaints.2,6,16 However, it should be noted that 40% of persons who die by strangulation have no external signs of injury.2,22 It is important for emergency providers to document all identified injuries, since less than 15% of external injuries caused by strangulation are adequately photographed to count as evidence in a trial, and the presence of documented injuries may persuade survivors to file complaints, lawyers to press charges, and juries to convict assailants.5,29,30 Table 2 lists physical findings suggestive of a strangulation event.
Table 2. Physical Exam Findings Suggestive of Strangulation |
|
Petechiae
Petechiae form when uninterrupted external pressure on the neck compresses veins, typically for at least 15 seconds, leading to venous congestion and leakage of blood into the soft tissue.2,16 Petechiae are reported most frequently on the face or conjunctivae following strangulation, but also can develop in the oral mucosa, palate, neck, and ear canal.16,21 (See Figure 1.) All survivors of strangulation should be examined closely for petechiae, which may persist for weeks, since their presence is considered a sign of a life-threatening strangulation.2,12
Figure 1. Petechiae on the Face |
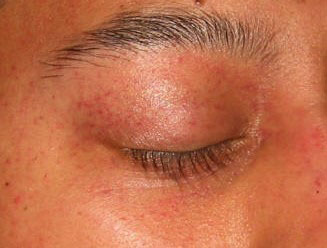
Image courtesy of J. Stephan Stapczynski, MD |
Other Skin Findings
In addition to petechiae, pressure against the skin incurred during strangulation can lead to abrasions and ecchymosis, which may not be visible on initial inspection.11 Abrasions from fingernails may be caused by the assailant or the victim trying to release the assailant’s grip. Identification of skin findings may be obscured by cervical collars, poor lighting, or in patients with dark skin.6 However, the detection and documentation of these findings are important because ligature marks are considered by some to be signs of life-threatening strangulations. (See Figures 2 and 3.)
Figure 2. Ligature Mark |
Image courtesy of J. Stephan Stapczynski, MD |
Figure 3. Ligature Mark |
Image courtesy of J. Stephan Stapczynski, MD |
Hyoid, Cricoid, and Thyroid Cartilage Fractures
Dislocations and fractures of the hyoid bone and cricoid and thyroid cartilages occur in half of fatal strangulations but are rare in non-fatal strangulations.2,12 Given their low prevalence in survivors of strangulation, these injuries are frequently missed by emergency providers.16 Normally, the hyoid bone provides mobility for the tongue and maintains patency of the pharynx during swallowing and respiration.
Patients with fractures of the hyoid bone or cricoid or thyroid cartilages may be asymptomatic or complain of neck pain, dyspnea, dysphagia, or hoarseness.2 A palpable fracture or subcutaneous emphysema may be present.31 While some injuries heal spontaneously, others can lead to laryngeal bleeding or edema, with subsequent airway compromise. All patients who are found to have fractures of the hyoid bone or cricoid or thyroid cartilages should be admitted for observation and otolaryngological consultation.
Respiratory Sequelae
Pharyngeal and laryngeal edema that leads to airway compromise can develop immediately or days after a strangulation.2,14,21 Injuries to the laryngopharynx that occur during strangulation can cause leakage of air into the chest cavity, resulting in pneumothoraces, pneumomediastinum, and pneumopericardium.32 Pulmonary edema, seen more commonly in survivors of strangulation who arrive comatose to the ED, can result from anoxic injury to the central nervous system (i.e., neurogenic pulmonary edema) or from aggressive attempts to inspire against an occluded airway (i.e., postobstructive pulmonary edema).2 Pulmonary edema and pneumonia are the most common causes of in-hospital death following strangulation.2
Anoxic Encephalopathy
Survivors of strangulation are at risk of developing neurologic sequelae related to hypoxic brain injuries. Immediate and delayed ischemic cerebrovascular accidents (CVAs), due to transient low cerebral blood flow, can occur following strangulation, without injury to the cerebral vessels.19 In such cases, neurons in regions of the brain that are especially sensitive to hypoxia, such as the hippocampus, cerebellum, and striatum, undergo delayed death.19 Delayed-onset blindness, choreoathetosis, pseudobulbar paralysis, and parkinsonism all have been reported following strangulation.2
Similar to athletes who sustain multiple concussions, survivors of repeated strangulations also can develop chronic traumatic encephalopathy.19,33 The prognoses of survivors of strangulation who present with neurologic symptoms often are unpredictable. Full recovery has been reported in patients who initially presented comatose, and there are reports of patients who initially were asymptomatic but later developed irreversible brain damage following strangulation.2
Mental Health
Survivors of strangulation often report anxiety, nightmares, and other symptoms of post-traumatic stress disorder.6 Depressive symptoms also are common.34 It is thought that some of these psychiatric symptoms result from anoxic changes in the limbic system, which is particularly sensitive to hypoxia.2
Other complications of strangulation that have been reported include tracheal perforation, thyroid storm, Horner’s syndrome, and cerebral venous thrombosis.19,35-37 Strangulation also is associated with increased risks of miscarriage and premature birth in pregnant women.5,28
Carotid Artery Dissection Due to Strangulation
Pathophysiology
Carotid artery dissections are estimated to occur in 1% of all survivors of strangulation, although this may be underestimated because of the underreporting of strangulations.2,20,38 Strangulation can lead to carotid artery dissection via multiple proposed mechanisms: 1) neck hyperextension during rotatory movement in strangulation may stretch and tear the arterial walls; 2) an anterior force applied to the carotid artery may compress it against the transverse processes of the cervical vertebrae, causing mechanical obstruction, vasospasm, or tearing; 3) a direct blow to the carotid artery may cause it to dissect.2 Cases of bilateral carotid artery dissection following non-fatal strangulation have been reported.2 Extracranial carotid dissections are more common than intracranial carotid dissections, and vertebral artery injuries are rare following strangulation.39 The damage to the medial or intimal layers of a dissected carotid artery can lead to carotid stenosis, transection of the carotid artery, pseudoaneurysm formation, or the creation of a thrombus at the dissection site, which then can dislodge and cause an embolic CVA.19,40,41
Approximately 20% to 30% of patients with carotid artery dissections develop embolic CVAs, which typically occur within 24 hours of a strangulation but can develop years later.2,19,42 The role of computed tomography angiography (CTA), which has high sensitivity in detecting carotid artery dissections and is readily available to most emergency providers, will be discussed later. Among patients with embolic CVAs resulting from carotid artery dissections secondary to any blunt trauma, mortality is 20% to 30%, and half of the survivors develop severe permanent neurologic deficits.43 Given that 10% to 25% of CVAs in persons younger than 45 years of age are caused by carotid artery dissections, emergency providers should specifically ask young patients with stroke symptoms about strangulation events.2,41
Diagnostic Imaging
Imaging of the neck is obtained in more than half of survivors of strangulation who present to the ED, most commonly to assess for carotid artery dissection.11,20 However, there is little evidence to guide when and which type of imaging should be performed, and the workup often depends on details of the strangulation event, availability of imaging modalities, institutional policies, the provider’s clinical judgment, and the patient’s demographics and preferences.
One group of experts on strangulation, the Training Institute on Strangulation Prevention, recommends performing imaging of the neck in any survivor of strangulation who has one of the findings listed in Table 3, which demonstrates a conservative approach intended to not miss any carotid artery dissections.44 On the other hand, recent studies have found an incidence of less than 1% of clinically important injuries on CTA in adult survivors of strangulation presenting to the ED, despite high rates of CTA imaging.20,38,45 This suggests that a more selective approach to imaging may be acceptable in alert, asymptomatic survivors of strangulation.
Of note, some radiologic findings, such as lymph node hemorrhages, are undetectable on physical examination but can be seen on computed tomography (CT) and magnetic resonance imaging (MRI), offering forensic evidence of a life-threatening strangulation.46,47
Table 3. Features of Strangulation that Warrant Radiographic Investigation, as Proposed by the Training Institute on Strangulation Prevention |
|
Plain radiography: Plain radiographs of the chest may be useful in survivors of strangulation with respiratory complaints to identify pulmonary edema or aspiration pneumonitis. On the other hand, plain radiographs of the neck are not routinely performed, since they rarely reveal subcutaneous emphysema or hyoid fractures.
CTA: Nearly half of survivors of strangulation who present to the ED receive CTA imaging of the neck.20,45 CTA has a sensitivity and specificity of nearly 98% and 100%, respectively, in detecting traumatic carotid artery dissections.48,49 In addition to the classic finding of a narrow lumen with a dissection flap surrounded by a mural thrombus, CTA may demonstrate an enlarged or abnormally shaped carotid artery in patients with dissections. (See Figure 4.) Advantages of CTA are that it is readily available in most EDs, it is rapid to perform, and it can be combined with other imaging in an initial trauma evaluation. Disadvantages include its use of contrast, which can be harmful to patients with kidney disease, and its associated exposure to radiation.
Figure 4. Computed Tomography Angiography of Strangulation Survivor |
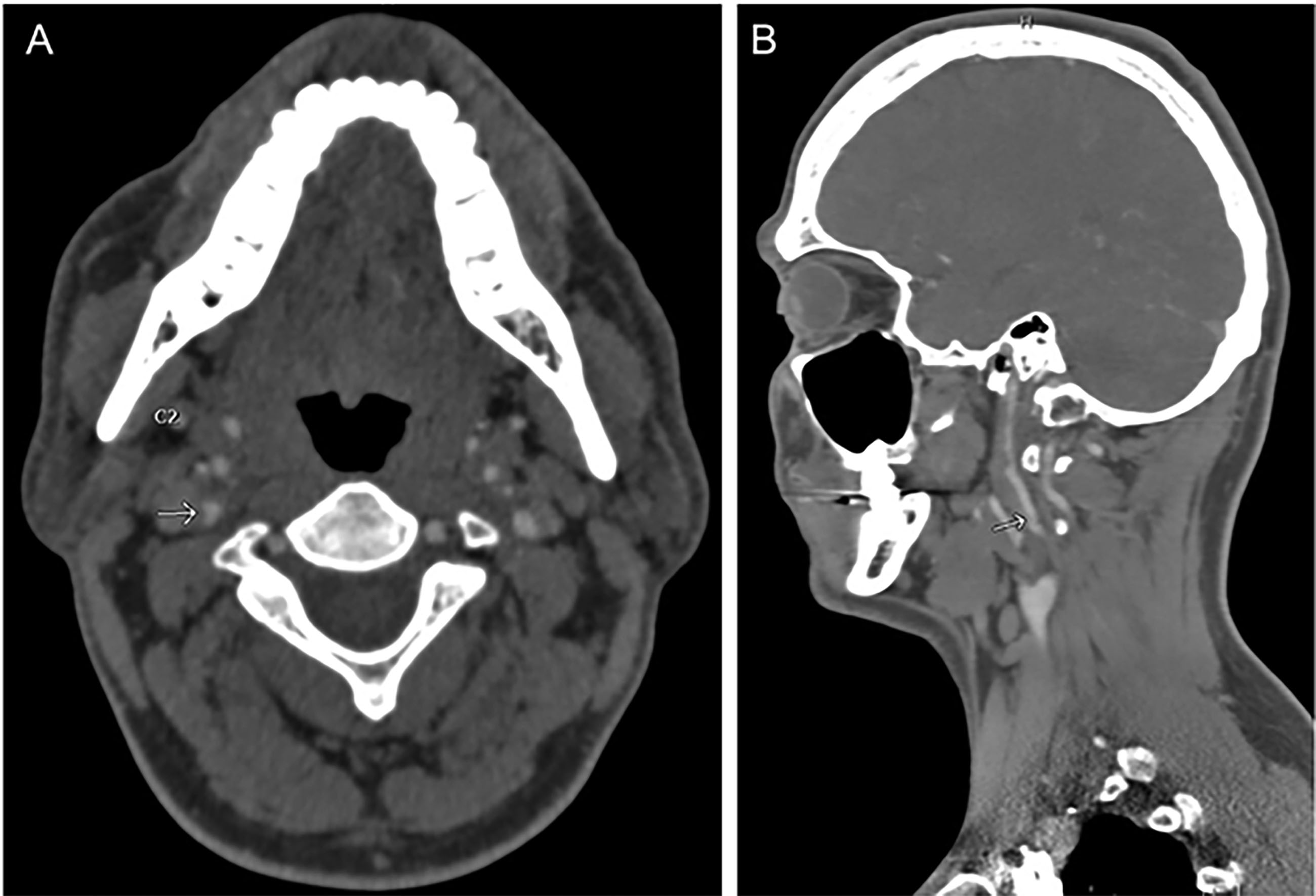
A) Computed tomography angiography of the neck in a survivor of strangulation demonstrates stenosis of the right internal carotid artery (arrow) on transverse view. B) On sagittal view, a dissection flap (arrow) with partial thrombosis of the carotid artery is seen, consistent with carotid artery dissection. |
MRI: MRI is the most sensitive imaging modality to detect soft tissue, laryngeal, vascular, and lymphatic injuries in the neck.47 However, both MRI and magnetic resonance angiography (MRA) of the neck are less sensitive than CTA for the assessment of carotid artery injuries.40 In addition, MR is relatively unavailable to most emergency providers, and survivors of strangulation may be resistant to entering an enclosed space or wearing an MRI neck coil.
Doppler ultrasound: Carotid artery Doppler ultrasound, which is radiation-free and can be performed at the bedside, is able to detect intimal injuries and intraluminal thrombosis.48 However, it is only 86% sensitive for the detection of carotid artery dissection, and it does not adequately evaluate the internal carotid or vertebral arteries, limiting its use in the evaluation of strangulation injuries.40,49
Cerebral angiography: Cerebral angiography, although considered to be the gold standard in the diagnosis of carotid artery dissection secondary to blunt trauma, is invasive and risks causing iatrogenic dissection. It has largely been supplanted by other imaging modalities. The classic finding of carotid artery dissection on cerebral angiography is the “string sign,” which refers to prolonged narrowing of the artery. Other angiographic findings include the “double lumen” sign, tapering stenosis of the vessel with distal dilatation, and occlusion of the artery.48
Management of Carotid Artery Dissection Following Strangulation
The acute management of carotid artery dissections identified in survivors of strangulation depends on the presence or absence of a concurrent embolic CVA. If signs of acute embolic CVA are present, standard stroke management should be followed, including the identification of candidates for reperfusion therapy. The same indications for systemic thrombolysis and/or mechanical thrombectomy apply, and the presence of a carotid dissection is not a contraindication to either therapy.50,51 If thrombolytics are given, anticoagulant and antiplatelet medications should be withheld for 24 hours.
In the absence of signs of an embolic CVA, survivors of strangulation with carotid artery dissections should be started on antithrombotic medications, which have been shown to decrease the risks of embolic CVAs and death.42 However, there is no clear consensus on the optimal medication regimen. Trauma society guidelines recommend starting unfractionated heparin as a weight-based infusion of 15 units/kg per hour, without a loading dose, with the goal of achieving an activated partial thromboplastin time (aPTT) of 40-50 seconds.42,43
At discharge, patients with carotid artery dissections who lack neurologic sequelae typically are started on an oral anticoagulant, such as warfarin, which is more effective at preventing embolic CVAs than an antiplatelet, such as aspirin or clopidogrel.52 In those patients with carotid artery dissections complicated by CVA, oral anticoagulants and antiplatelets have been shown to be equally effective at preventing recurrent CVAs.41
Since most carotid artery dissections heal within six months and rarely recur, treatment with oral therapies generally is recommended for six months.53 Endovascular stenting is usually not performed in survivors of strangulation with carotid artery dissections, since in-stent thrombosis can lead to embolic CVA.42
ED Disposition Following Strangulation
Admission to the hospital is recommended for survivors of strangulation who are found to have neurologic injuries or signs of a life-threatening strangulation, such as facial petechiae. Survivors of strangulation who report hoarseness, dyspnea, or odynophagia, as well as those with neck swelling or other signs of airway compromise, should be evaluated for underlying laryngeal or vocal cord injuries.14,40 In such cases, otolaryngologic consultation for direct/fiberoptic laryngoscopy or flexible nasopharyngoscopy is recommended.14,15
If a survivor of strangulation is asymptomatic, alert, and has no signs of a life-threatening strangulation, then there is growing evidence that imaging of the neck can be deferred, and the person can be discharged.20,38,45,54 Some experts recommend observing these asymptomatic survivors for at least six hours after the strangulation.2,7 A safe discharge plan should be established with the patient, including education about potential delayed respiratory and neurologic sequelae and strict return precautions.
When appropriate, social work and psychiatry should be consulted. No states specifically require mandatory reporting of strangulation; however, emergency providers should be aware of their individual state and federal laws regarding intimate partner violence reporting. As of 2021, strangulation occurring in the context of intimate partner violence is a felony in at least 48 U.S. states, and survivors of strangulation should be offered the opportunity to speak with law enforcement.55
Identification of High-Risk Populations
Since EDs often are the initial healthcare access points for survivors of strangulation, emergency providers potentially can identify at-risk persons. Several screening tools for intimate partner violence have been validated in the ED, including the Partner Violence Screen, which has a specificity of 80% to 94% for detecting intimate partner violence.56 (See Table 4.) Specifically asking about strangulation, multiple strangulations, and loss of consciousness in persons who screen positive for intimate partner violence may further help to identify persons at risk for strangulation injuries.23 Screening measures should be undertaken in a nonjudgmental manner, ideally in a private and confidential setting without intimate partners present.10
Table 4. The Partner Violence Screen Is a Three-Question Screening Tool for Intimate Partner Violence |
1. Have you been hit, kicked, punched, or otherwise hurt by someone within the past year? If so, by whom? 2. Do you feel safe in your current relationship? 3. Is there a partner from a previous relationship who is making you feel unsafe now? |
Actions shown to improve the health of persons who screen positive for intimate partner violence include providing continued access to healthcare, addressing immediate safety concerns, and educating about available resources.57 Therefore, persons who screen positive for intimate partner violence should be educated about the health risks of strangulation and offered social work consultation, resources for women’s shelters, and the opportunity to speak with law enforcement or state social services. Routine screening for intimate partner violence is associated with improved patient satisfaction and feelings of safety among survivors of intimate partner violence.10
Strangulation-Like Injuries
Hanging
Hanging is the second most common means of completed suicide in the United States, after firearms.58 It can be complete, in which the person is fully suspended by a constricting band around his or her neck, or partial, in which a portion of the person’s body remains in contact with the undersurface.40 In general, the force applied to the neck in a hanging is greater than that applied during other strangulation injuries. As a result, hyoid bone, thyroid cartilage, and cervical spine fractures, as well as cervical dislocations (typically at C2-C3), are more common in hangings than other forms of strangulation.59,60 Approximately 5% of hanging victims have carotid artery injuries.2 Hanging patients who survive to ED arrival are more likely to present with decreased levels of consciousness compared to survivors of strangulation.61 As with strangulation, it is rare for hanging patients to have injuries that impede intubation. However, a difficult airway should always be anticipated, and in-line stabilization of the cervical spine should be maintained if an unstable cervical fracture is suspected. If hanging was a self-harm attempt, other methods of self-harm should be investigated (e.g., toxic ingestions).
Autoerotic Asphyxiation
Autoerotic asphyxiation refers to sexual activity in which a person uses a device, typically a ligature, to self-strangle or hang themselves, with the goal of temporarily inducing cerebral hypoxia to heighten sexual pleasure. The activity occurs almost exclusively in young and middle-age men and can lead to accidental death by asphyxiation, typically when ligature strangulation or hanging is involved.62 Less commonly, hypoxia may be caused by covering the head with a plastic bag, wrapping the body in plastic, or inhaling volatile gases.63 Persons who engage in autoerotic asphyxia typically try to hide the activity. Emergency providers therefore should be alerted to the possibility of autoerotic asphyxiation by certain findings, such as hyoid bone or thyroid cartilage fractures.64
The “Choking Game”
The “choking game” refers to a practice by children and adolescents in which the participant intentionally self-strangulates, either manually or with a ligature, to induce cerebral hypoxia and a subsequent euphoria.65 The lifetime prevalence of participation in the choking game is 7% to 10% in middle school students.65,66 Videos of adolescents engaging in the choking game exist on YouTube and other social media platforms, which public health experts fear may normalize the activity and promote its spread.67
Short- and long-term complications of the choking game include chronic headaches, behavioral changes, memory loss, recurrent syncope, seizures, retinal hemorrhages, chronic visual changes, neurologic damage, and death.68 In addition, adolescents who engage in the choking game are more likely to report suicidal ideation and suicide attempts.65 Therefore, emergency providers should ask children and adolescents who present with headaches, petechiae, or other signs of strangulation about participation in the choking game, given its associated morbidity and mortality.
Martial Arts and Sports-Related Injuries
Approximately 40% of injuries sustained by mixed martial arts (MMA) and Taekwondo athletes involve the head and neck.69 Chokeholds performed during these and other contact sports mimic strangulations and can lead to similar injuries, including hyoid bone fractures, anoxic brain damage, and carotid artery dissections.70-72 Similar to survivors of repeated strangulation, MMA fighters who sustain repeated chokeholds are at risk of developing chronic traumatic encephalopathy.73,74 Given the increasing popularity of MMA, emergency providers should be aware of potential strangulation-related injuries and provide appropriate counseling to at-risk athletes.
Mechanical Asphyxia
Mechanical asphyxia, also referred to as positional, compressive, and restraint asphyxia, is the result of external airway obstruction caused by abnormal body positioning, restricted chest wall expansion, or other external mechanical factors not related to strangulation or hanging.75 Examples include intoxicated persons who “pass out” in abnormal positions, persons crushed by crowds or collapsed structures, and persons physically restrained by law enforcement officers.76-79 An estimated 25% of persons who die of opioid overdoses are found in airway-compromising positions, suggesting that mechanical asphyxia may play a role in the deaths.78 Most victims of mechanical asphyxia do not survive to ED arrival. However, emergency providers should consider the use of harm reduction strategies in vulnerable patients, such as those with dementia, limitations in mobility, or substance use.
Conclusion
Strangulation and related incidents are common, especially in women experiencing intimate partner violence. It is crucial for emergency providers to recognize strangulation as a unique form of violence, with its own specific injuries, to identify and document subtle physical findings, perform appropriate diagnostic testing, and provide adequate treatment and resources to patients who are at high risk for poor health outcomes and death. Emergency providers should keep in mind that the presence or absence of visible injuries in survivors of strangulation may not correlate with the development of life-threatening injuries, which can be delayed in onset.
Carotid artery dissections, although rare overall following strangulation, are of special concern, given their high rates of morbidity and mortality if left untreated. Therefore, emergency providers should have a low threshold to investigate any alarming symptoms in survivors of strangulation, employ shared decision-making with patients, and err on the side of caution when deciding whether to perform CTA imaging of the neck. However, emergency providers also should be aware of the emerging literature, which suggests that alert and asymptomatic survivors of strangulations can be discharged safely after a period of observation, without imaging of the neck.
Further research is needed to guide imaging protocols in the assessment of alert survivors of strangulation presenting to the ED.
REFERENCES
- Centers for Disease Control and Prevention. 20 leading causes of violence-related injury death, United States. WISQARS Leading Causes of Death Visualization Tool. https://www.cdc.gov/injury/wisqars/index.html
- De Boos J. Non-fatal strangulation: Hidden injuries, hidden risks. Emerg Med Australas 2019;31:302-308.
- Bendlin M, Sheridan L. Nonfatal strangulation in a sample of domestically violent stalkers: The importance of recognizing coercively controlling behaviors. Crim Justice Behav 2019;46:1528-1541.
- Cannon LM, Bailey JM, Ernst SD, et al. Examining trends in non-fatal strangulation among sexual assault survivors seeking Sexual Assault Nurse Examiner care from 2002 to 2017. Int J Gynaecol Obstet 2020;149:106-107.
- Douglas H, Fitzgerald R. Women’s stories of non-fatal strangulation: Informing the criminal justice response. Criminol Crim Justice 2020. doi:10.1177/1748895820949607
- Patch M, Anderson JC, Campbell JC. Injuries of women surviving intimate partner strangulation and subsequent emergency health care seeking: An integrative evidence review. J Emerg Nurs 2018;44:384-393.
- Jacob B, Cullen N, Haag HL, et al. Assault by strangulation: Sex differences in patient profile and subsequent readmissions. Can J Public Health 2020;111:492-501.
- Spencer CM, Stith SM. Risk factors for male perpetration and female victimization of intimate partner homicide: A meta-analysis. Trauma Violence Abuse 2020;21:527-540.
- Pritchard AJ, Reckdenwald A, Nordham C. Nonfatal strangulation as part of domestic violence: A review of research. Trauma Violence Abuse 2017;18:407-424.
- Monahan K, Bannon S, Dams-O’Connor K. Nonfatal strangulation (NFS) and intimate partner violence: A brief overview. J Fam Viol 2020; https://doi.org/10.1007/s10896...
- MacDonald Z, Eagles D, Yadav K, et al. Surviving strangulation: Evaluation of non fatal strangulation in patients presenting to a tertiary care sexual assault and partner abuse care program. CJEM 2021;23:762-766.
- Wahlsten P, Eriksson A. Asphyxia homicides in Finland, 1983-2012. J Forensic Sci 2020;65:1548-1556.
- Midttun D. Involuntary loss of bowel-control in sexual assault with non-fatal strangulation: A case report. Forensic Sci Int 2021;3:100200.
- Armstrong M, Strack GB. Recognition and documentation of strangulation crimes: A review. JAMA Otolaryngol Head Neck Surg 2016;142:891-897.
- Bean AS. Trauma to the Neck. In: Tintinalli JE, Ma O, Yealy DM, et al, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide, 9e. McGraw Hill; 2020.
- Payne-James JJ, Stark MM, Nittis M, Sheasby DR. Chapter 4: Injury assessment, documentation, and interpretation. In: Stark MM, ed. Clinical Forensic Medicine: A Physician’s Guide. Springer Nature; 2020:143.
- Saukko P, Knight B. Fatal pressure on the neck. In: Knights’ Forensic Pathology, 4th ed. CRC Press Taylor & Francis Group;2016:369-397.
- Pritchard AJ, Reckdenwald A, Nordham C, et al. Improving identification of strangulation injuries in domestic violence: Pilot data from a researcher-practitioner collaboration. Fem Criminol 2018;13:160-181.
- Bichard H, Byrne C, Saville CWN, Coetzer R. The neuropsychological outcomes of non-fatal strangulation in domestic and sexual violence: A systematic review. Neuropsychol Rehabil 2021;12:1-29.
- Matusz EC, Schaffer JT, Bachmeier BA, et al. Evaluation of nonfatal strangulation in alert adults. Ann Emerg Med 2020;75:329-338.
- Rozzi HV, Riviello R. How to evaluate strangulation. ACEP Now 2019;38. https://www.acepnow.com/article/how-to-evaluate-strangulation
- Zilkens RR, Phillips MA, Kelly MC, et al. Non-fatal strangulation in sexual assault: A study of clinical and assault characteristics highlighting the role of intimate partner violence. J Forensic Leg Med 2016;43:1-7.
- Messing JT, Campbell J, AbiNader MA, Bolyard R. Accounting for multiple nonfatal strangulation in intimate partner violence risk assessment. J Interpers Violence 2020;886260520975854.
- Mcquown C, Frey J, Steer S, et al. Prevalence of strangulation in survivors of sexual assault and domestic violence. Am J Emerg Med 2016;34:1281-1285.
- McKee GB, Gill-Hopple K, Oesterle DW, et al. New perspectives on risk factors for non-fatal strangulation and post-assault imaging. J Interpers Violence 2020;886260520966673.
- Stansfield R, Williams KR. Coercive control between intimate partners: An application to nonfatal strangulation. J Interpers Violence 2021;36:NP5105-NP5124.
- Vella SA, Miller MM, Lambert JE, Morgan ML. “I felt close to death”: A phenomenological study of female strangulation survivors of intimate terrorism. J Fem Family Therapy 2017;29:171-188.
- Messing JT, Patch M, Sullivan Wilson J, et al. Differentiating among attempted, completed, and multiple nonfatal strangulation in women experiencing intimate partner violence. Womens Health Issues 2018;28:104-111.
- Reckdenwald A, Mandes CL, Fernandez K. The effectiveness of a coordinated response toward nonfatal strangulation in facilitating evidence-based prosecution. Criminal Justice Policy Review 2021;32:816-840.
- Douglas H, Fitzgerald R. Proving non-fatal strangulation in family violence cases: A case study on the criminalisation of family violence. Int J Evid Proof 2021;25:350-370.
- Keerthi R, Quadri A. Hyoid bone fracture: Associated with head and neck trauma — a rare case report. J Maxillofac Oral Surg 2016;15(Suppl 2):249-252.
- Jung MH, Kim SE, Lee DH, et al. Cervical emphysema and pneumomediastinum following ‘light strangulation’ injury.” Hong Kong J Emerg Med 2017;24:90-92.
- Campbell JC, Anderson JC, McFadgion A, et al. The effects of intimate partner violence and probable traumatic brain injury on central nervous system symptoms. J Womens Health (Larchmt) 2018;27:761-767.
- Mittal M, Resch K, Nichols-Hadeed C, et al. Examining associations between strangulation and depressive symptoms in women with intimate partner violence histories. Violence Vict 2018;33:1072-1087.
- De Boos J. Tracheal perforation from non-fatal manual strangulation. J Forensic Leg Med 2019;66:1-3.
- von Hohenberg CC, Kerl U, Sartorius A, Schwarz S. Cerebral venous thrombosis following strangulation. Prim Care Companion CNS Disord 2018;20:17l02198.
- Lanham T, Sullivan A, Lanham E, Donato A. Strangulation-induced thyrotoxicosis in a patient with undiagnosed underlying Graves’ disease. Case Rep Endocrinol 2020;2020:7986581.
- Zuberi OS, Dixon T, Richardson A, et al. CT angiograms of the neck in strangulation victims: Incidence of positive findings at a level one trauma center over a 7-year period. Emerg Radiol 2019;26:485-492.
- Le Blanc-Louvry I, Papin F, Vaz E, Proust B. Cervical arterial injury after strangulation — different types of arterial lesions. J Forensic Sci 2013;58:1640-1643.
- Dunn RJ, Sukhija K, Lopez RA. Strangulation injuries. In: StatPearls [Internet]. StatPearls Publishing; 2021.
- Markus HS, Levi C, King A, et al. Antiplatelet therapy vs anticoagulation therapy in cervical artery dissection: The Cervical Artery Dissection in Stroke Study (CADISS) randomized clinical trial final results. JAMA Neurol 2019;76:657-664.
- Kim DY, Biffl W, Bokhari F, et al. Evaluation and management of blunt cerebrovascular injury: A practice management guideline from the Eastern Association for the Surgery of Trauma. J Trauma Acute Care Surg 2020;88:875-887.
- Biffl WL, Burley CC, Moore EE. Blunt cerebrovascular injury: Treatment and outcomes. UpToDate.com.
- Smock BS, Sturgeon S. Recommendations for the Medical/Radiographic Evaluation of Acute Adult, Non-fatal Strangulation. San Diego, CA: Training Institute on Strangulation Prevention; 2015.
- Williamson F, Collins S, Dehn A, Doig S. Vascular injury is an infrequent finding following non-fatal strangulation in two Australian trauma centres. Emerg Med Australas 2021;doi:10.1111/1742-6723. [Online ahead of print].
- Bruguier C, Genet P, Zerlauth JB, et al. Neck-MRI experience for investigation of survived strangulation victims. Forensic Sci Res 2019;5:113-118.
- Gascho D, Heimer J, Thali MJ, Flach PM. The value of MRI for assessing danger to life in nonfatal strangulation. Forensic Imaging 2020;22:200398.
- Hakimi R, Sivakumar S. Imaging of carotid dissection. Curr Pain Headache Rep 2019;23:2.
- Nagpal P, Policeni BA, Bathla G, et al. Blunt cerebrovascular injuries: Advances in screening, imaging, and management trends. AJNR Am J Neuroradiol 2017;39:406-414.
- Tsivgoulis G, Zand R, Katsanos AH, et al. Safety and outcomes of intravenous thrombolysis in dissection-related ischemic stroke: An international multicenter study and comprehensive meta-analysis of reported case series. J Neurol 2015;262:2135.
- Li S, Zi W, Chen J, et al. Feasibility of thrombectomy in treating acute ischemic stroke because of cervical artery dissection. Stroke 2018;49:3075.
- Hanna K, Douglas M, Asmar S, et al. Treatment of blunt cerebrovascular injuries: Anticoagulants or antiplatelet agents? J Trauma Acute Care Surg 2020;89:74.
- Urasyanandana K, Songsang D, Aurboonyawat T, et al. Treatment outcomes in cerebral artery dissection and literature review. Interv Neuroradiol 2018;24:254-262.
- Subramanian M, Hranjec T, Liu L, et al. A case for less workup in near hanging. J Trauma Acute Care Surg 2016;81:925-930.
- Department of Justice. U.S. Attorney’s Office, District of Columbia. Statement of U.S. Attorney’s Office for the District of Columbia Before D.C. Council Regarding Measures to Strengthen Protections for Victims-Survivors of Domestic Violence. May 13, 2021. https://www.justice.gov/usao-dc/pr/statement-us-attorneys-office-district-columbia-dc-council-regarding-measures-strengthen
- Vonkeman J, Atkinson P, Fraser J, et al. Intimate partner violence documentation and awareness in an urban emergency department. Cureus 2019;11:e6493.
- Lizdas K, O’Flaherty A, Durborow N, et al. Compendium of state and U.S. territory statutes and policies on domestic violence and health care. 4th ed. Futures Without Violence; 2019. https://www.futureswithoutviolence.org
- National Center for Health Statistics. Suicide and self-harm injury. 2014. https://www.cdc.gov/nchs/fastats/suicide.htm
- Zátopková L, Janík M, Urbanová P, et al. Laryngohyoid fractures in suicidal hanging: A prospective autopsy study with an updated review and critical appraisal. Forensic Sci Int 2018;290:70-84.
- Amadasi A, Buschmann CT, Tsokos M. Complex fracture patterns in hanging associated with a fall from height. Forensic Sci Med Pathol 2020;16:359-361.
- Berke DM, Helmer SD, Reyes J, Haan JM. Injury patterns in near-hanging patients: How much workup is really needed? Am Surg 2019;85:549-555.
- Lohner L, Sperhake JP, Püschel K, Schröder AS. Autoerotic deaths in Hamburg, Germany: Autoerotic accident or death from internal cause in an autoerotic setting? A retrospective study from 2004-2018. Forensic Sci Int 2020;313:110340.
- Bäckström B, Johansson B, Eriksson A. Death from nitrous oxide. J Forensic Sci 2015;60:1662-1665.
- Eckhardt M, Shah K, Bois M, et al. Healed fracture of superior horn of thyroid cartilage in autoerotic asphyxia: An indication of prior activity? A case report utilizing 3D scanning and printing of the larynx. Acad Forensic Pathol 2018;8:170-179.
- Michel G, Garcia M, Aubron V, et al. Adolescent mental health and the choking game. Pediatrics 2019;143:e20173963.
- Busse H, Harrop T, Gunnell D, Kipping R. Prevalence and associated harm of engagement in self-asphyxial behaviours (‘choking game’) in young people: A systematic review. Arch Dis Child 2015;100:1106-1114.
- Defenderfer EK, Austin JE, Davies WH. The choking game on YouTube: An update. Glob Pediatr Health 2016;3:2333794X15622333.
- Re L, Birkhoff JM, Sozzi M, et al. The choking game: A deadly game. Analysis of two cases of “self-strangulation” in young boys and review of the literature. J Forensic Leg Med 2015;30:29-33.
- Thomas RE, Thomas BC. Systematic review of injuries in mixed martial arts. Phys Sportsmed 2018;46:155-167.
- Jensen AR, Maciel RC, Petrigliano FA, et al. Injuries sustained by the mixed martial arts athlete. Sports Health 2017;9:64-69.
- Demartini Z Jr, Rodrigues Freire M, Lages RO, et al. Internal carotid artery dissection in Brazilian Jiu-Jitsu. J Cerebrovasc Endovasc Neurosurg 2017;19:111-116.
- Knapik DM, Royan SJ, Salata MJ, Voos JE. Hyoid dislocation following subacute fracture in an American high school football athlete. Orthop J Sports Med 2018;6:2325967117753594.
- Schlegel P, Novotny M, Valis M, Klimova B. Head injury in mixed martial arts: A review of epidemiology, affected brain structures and risks of cognitive decline. Phys Sportsmed 2021;49:371-380.
- Lim LJH, Ho RCM, Ho CSH. Dangers of mixed martial arts in the development of chronic traumatic encephalopathy. Int J Environ Res Public Health 2019;16:254.
- Kroll MW, Brave MA, Kleist SR, et al. Applied force during prone restraint: Is officer weight a factor? Am J Forensic Med Pathol 2019;40:1-7.
- Nolan JP, Soar J, Cary N, et al. Compression asphyxia and other clinicopathological findings from the Hillsborough Stadium disaster. Emerg Med J 2021;38:798-802.
- Rutty GN. Traumatic, crush and compression asphyxia including ‘burking.’ In: Madea B. Asphyxiation, Suffocation, and Neck Pressure Deaths. CRC Press;2020:222-231.
- deJong JL, Lee J, Grande A, et al. Positional asphyxia in opioid-related deaths: Is it being overlooked? J Forensic Sci 2020;65:2008-2012.
- Karch SB. The problem of police-related cardiac arrest. J Forensic Leg Med 2016;41:36-41.
It is important for emergency providers to be able to identify injuries associated with strangulation, to prevent its devastating sequelae, and to provide safety planning and resources.
Subscribe Now for Access
You have reached your article limit for the month. We hope you found our articles both enjoyable and insightful. For information on new subscriptions, product trials, alternative billing arrangements or group and site discounts please call 800-688-2421. We look forward to having you as a long-term member of the Relias Media community.
